Abstract
Objectives
Lactate as a key regulator of the glycolytic phenotype has been recently described in fueling tumor growth and metastatic spread in head and neck squamous cell carcinoma (HNSCC). However, in context of tumor recurrence following adjuvant radiation, the underlying mechanisms remain uncertain. We therefore investigate the role of lactate towards radioresistance in HNSCC in this prospective study for the first time in vivo.
Materials and methods
Herein, we analyzed biopsies of primary squamous cell carcinoma after surgery and adjuvant irradiation in 17 patients. Tumor tissue levels of ATP, glucose, and lactate were detected using induced metabolic bioluminescence imaging (imBI) and correlated with clinical data within an observation period of up to 15 years.
Results
High amounts of lactate levels in tumors of HNSCC are significantly negatively correlated with overall patient survival. Moreover, high expression of lactate in a primary tumor site is significantly correlated with tumor recurrence post radiation, whereas ATP and/or glucose showed no such correlation.
Conclusion
Lactate can be seen not only as a waste product of altered glycolytic metabolism but also as a key master of malignancy as well as resistance mechanism towards irradiation.
Clinical relevance
High expression of lactate levels in tumor tissue, obtained by metabolic bioluminescence imaging, may therefore serve as a predictor for overall and recurrence-free survival and could represent a future biomarker in the validation of adjuvant irradiation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With an estimated annual incidence of approximately 633,000 cases per annum, head and neck squamous cell carcinoma (HNSCC) represents the sixth most common cancer diagnosed worldwide that causes a global number of over 300,000 deaths per year. It can therefore be seen as a significant global health burden [1, 2]. Despite advances in the multidisciplinary treatment of this cruel disease, no major improvement of the generally poor 5-year-survival rate between 50 and 60 % could be made in the past 20 years [3–6]. Consequently, recent investigations focus on the molecular mechanism as well as the underlying metabolic features that drive the resistance of the neoplasia to adjuvant chemotherapy and/or radiation.
The distribution of metabolites in physiological tissues differs fundamentally from that in solid tumors with a malignant phenotype of energy metabolism, such as HNSCC. This difference is mainly due to the unlimited cell proliferation potential and to an inadequate and heterogeneous blood supply in malignancies. The carcinogenesis-related switch in essential processes fueling cell growth and division was postulated for the first time in the early 1920s by Otto Warburg and is nowadays seen as an emerging hallmark of cancer [7–9]. Warburg hypothesized that tumor development is associated with a shift from oxidative to glycolytic energy production [10] which leads to the phenomenon of aerobic glycolysis even in the presence of oxygen (“Warburg effect”) [11]. Thus, namely driven by an overexpression of glycolytic genes and subsequent activation of glycolytic enzymes and membrane transporters [11–13], cancer cells are able to avoid oxidative phosphorylation, the main source of ATP under physiological conditions that normally reduces the glycolytic flux in normoxic tissues (“Pasteur effect”) [14, 15]. Instead, via the conversion of pyruvate into lactate by LDH-A, NADH+H+ can efficiently be recycled to NAD+, which is the key reaction that makes glycolysis self-sufficient by further generation of ATP without feeding the TCA cycle [16].
As a consequence, these metabolic alterations lead to an immense accumulation of lactate that is widely accepted as a unique phenotype of cancer [13, 17, 18]. In this context, previously published investigations of our own working group [10, 11, 19, 20] and others [3, 21, 22], showing a statistical significant negative correlation between increased lactate amounts and outcome of patients with HNSCC, strengthen the hypothesis that lactate mirrors tumor malignancy [10]. Additionally, there is growing evidence that lactate is positively correlated with radioresistance of HNSCC, as shown in in vitro studies and human tumor xenografts [12, 13, 23].
Therefore, the aim of this study was to investigate the possible role of lactate as a modifier of radiosensitivity of HNSCC in patients. Hence, we analyzed cryobiopsies of primary squamous cell carcinoma after surgery and adjuvant irradiation in 17 patients. Tumor tissue levels of ATP, glucose, and lactate were detected using induced metabolic bioluminescence imaging (imBI). Moreover, we correlated these results with clinical data such as overall survival and recurrence-free survival within an observation period of up to 15 years, so as to point out lactate as a possible biomarker for tumor recurrence post radiation.
Material and methods
Study population
All patients (n = 17) with newly histopathological diagnosis of HNSCC underwent surgery between 1999 and 2000 at the Department of Oral and Maxillofacial Surgery, University of Mainz, Medical Center, due to valid guidelines [24]. Written informed consent of all patients was given to participate in this study. At the time of surgery, average patient’s age was 56 years (±13.2). After surgery, staging of the disease was performed by independent pathologists due to the current version of TNM classification [25]. Herein, 11 patients (64 %) showed far advanced T status (T4), 88 % (15 patients) were presented with at least one or more lymph node metastases (N1–3). Furthermore, in 3 patients (17 %), distant metastases were detectable. Every patient received R0 resection of the primary tumor site. As a result of these pathophysiologically findings, all 17 patients were therefore regarded as high-risk profile for locoregional tumor recurrence. Consequently, all 17 patients received adjuvant irradiation with 60 Gy in 30 fractions over a 6-week period, and 15 patients obtained an combined chemoradiotherapy with addition of cisplatin or 5-fluoracil. Clinical data were analyzed within an observation period up to 15 years, wherein 11 patients (64 %) demonstrated a histopathological confirmed tumor recurrence. The local ethics committee (Landesärztekammer Rheinland-Pfalz) approved the following experiments (Ethikvotum 837.837.11 (7924)) in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki.
Biopsy excision
During the surgical tumor resection, a separate biopsy was taken from each patient at the tumor border and was instantly snap frozen in liquid nitrogen. This procedure is crucial for the proper cryopreservation of the momentary metabolic status of the tissue. Any severe disturbance of the tissue microcirculation before removal of the biopsy and any time delay before the immersion of the biopsy into liquid nitrogen have to be strictly avoided. This may be sometimes challenging in clinical routine, but numerous patient studies applying imBI in the clinical setting have demonstrated the feasibility of this approach. The biopsies can be kept in −80 °C until using them for imBI measurements. For long-term cryopreservation of the metabolome, biopsies have to be transferred into liquid nitrogen (−180 °C), where metabolite concentrations remain unaffected for at least 10 years.
Induced metabolic bioluminescence imaging (imBI)
Mueller-Klieser and coworkers have developed and refined the imBI technique in the early 1990s for measuring the spatial contribution of metabolites such as ATP, glucose, and lactate inter alia in cryosections of tumor origin [26]. Briefly, serial cryosections with a thickness of 15 μm were made from the frozen biopsies. Since each metabolite can only be assessed separately in one section, registration of different metabolites in adjacent sections reflects metabolic measurements at quasi-identical locations in the tissue. Including a further serial section for histological staining (hematoxylin and eosin) allows for the assessment of metabolites in relation to the histological structure of the tissue, such as viable tumor regions, necrosis, or stromal areas. The development of a specific puncture technique (s. below) warrants an exact overlay of the serial cryosections and the 2D metabolite distributions, respectively. For metabolic imaging, each section has to be processed in an identical manner. The experimental setup is schematically shown in Fig. 1 [26]. The cryosection is adherent to a cover glass which is placed upside-down on a glass block with a casting mold containing a specific enzyme solution. This solution biochemically links the metabolite of interest within the tissue section to the emission of light by bacterial (for glucose and lactate) or firefly (for ATP) luciferase. The reaction sandwich is then transferred to a thermostated microscope chamber being adjusted to 22 °C. The 2D bioluminescence low light emission is registered with an ultrasensitive cooled CCD camera connected to the microscope. The metabolite distributions within the tissue sections can then be calibrated as tissue concentrations in units of micromole per gram tissue using appropriate standards. These concentration distributions are routinely displayed in a color-coded manner. Interactive computerized overlay of selected histological areas obtained from the H & E-stained sections with metabolite distributions makes it possible to evaluate metabolite concentrations in specific tumor regions, such as viable tumor cell accumulations or stromal areas. A representative documentation of structure-associated color-coded metabolite distributions within a solid tumor is displayed in Fig. 2 [27]. Further methodological details can be obtained from a comprehensive and detailed documentation of the imBI technique that has been published recently (s. references).
Modificated schematic overview shows simplified experimental setup of the bioluminescence imaging and photon counting. For further information, see text or previously published description in the literature [26]
Exemplary series of sections through an HSNCC biopsy and display of the metabolite accumulation via bioluminescence imaging [27]. For further details, see text
Statistics
Data were presented as the mean ± SD (standard deviation). For statistical analysis, SPSS 22 (Ehningen, Germany) and Microsoft Office Excel (Unterschließheim, Germany) was used to perform Student’s t test, Spearman’ s rank correlation, Chi-square test, ANOVA regression analysis as well as log rank test for Kaplan-Meier survival curve. For descriptively analysis, results were shown in boxplots (black bar in the middle: mean, whiskers: valid minima and maxima). A p value <0.05 was determined as statistically significant.
Results
High-lactate tumors of HNSCC are significantly negative correlated with overall patient survival
In our study population, patients with high amounts of lactate in primary tumor tissue of HNSCC (>average level of 10.3 μmol/g; “high-lactate tumors”) showed a significantly reduced overall survival compared to patients with “low-lactate tumors”, as clearly demonstrated by the result of a respective Kaplan-Meier analysis (p = 0.04) (Fig. 3). Median survival time for the low-lactate group was 1827 months vs. 428 months for the high-lactate group within the total observation time of 15 years.
Kaplan-Meier analysis of the overall survival in the patient cohort within the 15-year follow-up. High-lactate tumor (>average concentration of 10.3 μmol/g) showed statistically significant worse outcome with a median survival time of 428 months vs. 1827 months in the low-lactate group (<10.3 μmol/g) (p = 0.04)
Post radiation tumor recurrence is significantly correlated with increased levels of lactate in the primary site of HNSCC
All patients of this study population underwent surgical tumor resection and received adjuvant irradiation. Eleven patients (64 %) established tumor recurrence within the follow-up.
Figure 4 represents graphically the correlation between the investigated metabolites ATP, glucose, as well as lactate with the reappearance of HNSCC. Herein, ATP (mean 1.19 ± 0.5 μmol/g for non-recurrence vs. 1.14 ± 0.59 μmol/g for positive recurrence) and glucose (1.89 ± 1.3 μmol/g vs. 1.28 ± 0.8 μmol/g) showed no significantly correlation (p = 0.78 for ATP respectively 0.30 for glucose after Student’s t test analysis). In contrast, lactate showed a statistically significant correlation (8.82 ± 3.7 μmol/g for non-recurrence vs. 12.37 ± 5.1 μmol/g). Student’s t test analysis resulted in p = 0.02. To strengthen this result, we conducted a multivariate analysis that ruled out dependency of the tumor recurrence for T, N, and M status, as well as patient’s gender and the risk factors alcohol and/or nicotine consumption. Lactate can therefore be seen as an independent prognostic marker for tumor recurrence with p = 0.048 in ANOVA analysis. Furthermore, Kaplan-Meier analysis (Fig. 5) was used to demonstrate the influence of lactate on timing of tumor recurrence. High-lactate tumors (>average concentration of 10.3 μmol/g) showed herein a significantly earlier and more frequent tumor recurrence (p = 0.019). Additionally, Chi-square test revealed a strong tendency (p = 0.086) for an overexpression of lactate in the early recurrence group (date of recurrence within 1 year after tumor resection) compared to the late recurrence cohort.
Boxplots visualize the correlation between tumor recurrence and increased ATP, glucose, and lactate level in the 15-year follow-up. Student’s t test shows statistical significance for lactate (p = 0.02 marked by asterisk), i. e., primaries which later on recurred contained significantly higher lactate concentrations compared to non-recurring primaries
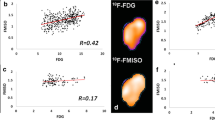
Interestingly, spearman’s rank correlation analysis demonstrated a weak but significant inverse correlation between intratumoral glucose and lactate concentrations in patients without (R = 0.30) or with (R = 0.29) tumor recurrence, as shown in Fig. 6.
Discussion
Since the first description of an altered metabolism in solid tumors by Warburg et al. in the early 1920s [8], tumor glycolysis as well as lactate metabolism has become an aspiring research field in exploration of tumor development. Nowadays, these unique pathways of cancer metabolism are fundamentally used in routine clinical practice for prognosis and diagnosis of solid tumors, for example within the 18FDG-PET-Scan [28]. As previously described, among others by Gatenby et al., the glycolytic phenotype is now seen as a “crucial component of the malignant phenotype and confers a significant proliferative advantage during somatic evolution of cancer” [14]. Firstly shown in biopsies of cervical cancer by Schwickert et al. in 1995 using bioluminescence imaging and photon counting [29], Walenta et al. from our working group could for the first time find a statistically significant correlation between increase lactate expression in HNSCC with high risk of metastatic spread [30]. Our results confirm data obtained in subsequent studies investigating the overall survival, among others, of patients with HNSCC and point out increased lactate levels as a possible marker of patient’s predeceasing [20, 22]. However, the underlying mechanisms remain unclear and therefore represent an on-going challenge in the current literature: In early state of tumorigenesis, the glycolytic switch could be initiated by hypoxia (meditated by the transcription factor hypoxia-inducible factor 1-alpha (HIF-1α)) that itself is a product of restricted blood perfusion due to increasing heterogeneity in vascular pattern. Subsequently, the oxidation of lactate via LDH-B seems to be able to stabilize HIF-1α through an inhibition of the HIF-PHD (prolylhydroxylase) that normally tags HIF-1α for degradation in the proteasomes [31]. Thus, adaption to hypoxia by switching to glycolytic metabolism could be seen as a survival advantage of cancer cells in the hostile tumor environment [14, 26, 32]. Afterwards, an upregulation of multiple genetic alterations, among them PI3K/Akt/mTOR pathway or c-Myc transcription factor, is nowadays recognized as master regulators in controlling the persistent glycolytic switch that is then fueling the unlimited proliferation [16]. In addition, lactate seems to increase the expression of VEGF, henceforth resulting in angiogenesis and further tumor growth [31].
Interestingly, recent investigations challenging the traditional view of a homogenous tumor mass, but focus on metabolic compartmentalization leading to heterogeneity in neoplasia [31, 33, 34]. Lately demonstrated for oral squamous cell carcinoma (OSCC), cancer-associated fibroblasts (CAF) in the tumor stroma were identified to fuel well-oxygenated cancer cells with metabolic nutrition as lactate via specific lactate shuttles (monocarboxylate transporter MCT-1/4) [33]. This parasitic-like relationship between microenvironment and cancer cells is termed the reverse Warburg Effect and is mainly driven by glycolytic metabolism [17, 35]. In this context, our corresponding results, showing only a weak inverse correlation between glucose uptake and lactate concentration in tumor tissue, could be interpreted regarding this reverse effect. Our data therefore provides a slight hint in supporting the hypothesis of compartmentalization in solid tumors, such as HNSCC.
Furthermore, a multitude of proton export systems including vacuolar-type ATPases represent an evolutionary strategy for escape from those self-created hostile conditions. [15]. As a consequence, these mentioned alterations lead to a “reversed pH gradient” combining an acidic microenvironment with an alkaline cytosol which was recently described as a mechanism to suppress anticancer immune response as well as crucial for multidrug and radioresistance [15, 36]. In this context, a lately published analysis by Federici et al. demonstrated microenvironmental acidity in human melanoma cells as a highly efficient mechanism of chemoresistance against cisplatin [37]. Just recently, another study by Sun et al. could confirm these conclusions for HNSCC by demonstrating LDH-B as a prognostic factor for OSCC in general as well as predictive marker for the response to neoadjuvant chemoradiotherapy. However, LDH-B seems to specifically affect the sensitivity of cancer cells to taxol but not to cisplatin [3]. Therefore, the underlying mechanisms seem to be not fully understood yet. Since 15 patients in our small sample size received a combined chemoradiotherapy with cisplatin, we also present a first indication that lactate, possibly due to the reversed pH gradient, may drive resistance to adjuvant cisplatin therapy in HNSCC. As a consequence, the precise mechanisms beyond this effect may be of great interest for subsequent investigations. Regarding head and neck squamous cell carcinoma’s resistance towards radiation, results of this study demonstrate a statistically significant correlation between lactate and tumor recurrence after radiation. Increased lactate levels, in turn, showed weak correlation to the glucose uptake of tumor cells in the altered glycolytic metabolism.
These results confirm evidence of previously published in vitro studies using HNSCC tumor models in which lactate was demonstrated as a possible marker for radiosensitivity [12, 13, 23]. The potential underlying mechanism of this effect could be seen at least in part in the potential of lactate (and pyruvate) as an antioxidant agent [20, 38]. Thus, lactate could be able to reduce the oxidative stress that radiation is therapeutically exerting via accumulation of reactive oxygen species (ROS) essentially mediating radiation-induced DNA damage [20, 39].
In general, our study suffers from some limitations: First, major weakness may be seen in the small sample size. Nevertheless, the firstly presented in vivo results confirm findings of other in vitro essays in the current literature. Furthermore, we did not reanalyzed tumor tissue levels of ATP, glucose, and lactate in the recurrent tumor mass. Considering our hypothesis of lactate as a key player in radioresistance however, this objective may be of great interest of subsequent analyses in order to help defining the exact molecular mechanisms.
In summary, we present in this study an in vivo analysis of the underlying metabolic alterations in 17 HNSCC biopsies via bioluminescence imaging. Subsequently, we demonstrated a statistically significant inverse correlation between lactate and the overall as well as the recurrence-free survival after surgery and radiation in the ensuing 15-year follow-up. Therefore, we hypothesize that lactate can be seen not only as a waste product of altered glycolytic metabolism but also as a key master of resistance mechanism and therefore a reliable prognostic biomarker in adjuvant therapy such as radiation. A recently published investigation strengthens this postulate and presents combined inhibition of lactate metabolism with radiation therapy as an effective new therapeutic strategy in targeting solid tumors [40]; nevertheless, more in vivo analyses are required to gain much needed information of the still unclear underlying metabolic processes.
References
Rassouli A, Saliba J, Castano R, Hier M, Zeitouni AG (2015) Systemic inflammatory markers as independent prognosticators of head and neck squamous cell carcinoma. Head & Neck 37(1):103–110. doi:10.1002/hed.23567
Rampias T, Sasaki C, Psyrri A (2014) Molecular mechanisms of HPV induced carcinogenesis in head and neck. Oral Oncol 50(5):356–363. doi:10.1016/j.oraloncology.2013.07.011
Sun W, Zhang X, Ding X, Li H, Geng M, Xie Z, Wu H, Huang M (2015) Lactate dehydrogenase B is associated with the response to neoadjuvant chemotherapy in oral squamous cell carcinoma. PLoS One 10(5):e0125976. doi:10.1371/journal.pone.0125976
Bose P, Brockton NT, Dort JC (2013) Head and neck cancer: from anatomy to biology. International Journal of Cancer Journal International du Cancer 133(9):2013–2023. doi:10.1002/ijc.28112
Chai RC, Lambie D, Verma M, Punyadeera C (2015) Current trends in the etiology and diagnosis of HPV-related head and neck cancers. Cancer Medicine. doi:10.1002/cam4.424
Grimm M, Alexander D, Munz A, Hoffmann J, Reinert S (2013) Increased LDH5 expression is associated with lymph node metastasis and outcome in oral squamous cell carcinoma. Clinical & Experimental Metastasis 30(4):529–540. doi:10.1007/s10585-012-9557-2
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144(5):646–674. doi:10.1016/j.cell.2011.02.013
O. Warburg KP, E. Negelein (1924) Über den Stoffwechsel der Carcinomzelle. Biochem Z 152:pp. 319–344
Vegran F, Boidot R, Michiels C, Sonveaux P, Feron O (2011) Lactate influx through the endothelial cell monocarboxylate transporter MCT1 supports an NF-kappaB/IL-8 pathway that drives tumor angiogenesis. Cancer Res 71(7):2550–2560. doi:10.1158/0008-5472.CAN-10-2828
Walenta S, Mueller-Klieser WF (2004) Lactate: mirror and motor of tumor malignancy. Semin Radiat Oncol 14(3):267–274. doi:10.1016/j.semradonc.2004.04.004
Ziebart T, Walenta S, Kunkel M, Reichert TE, Wagner W, Mueller-Klieser W (2011) Metabolic and proteomic differentials in head and neck squamous cell carcinomas and normal gingival tissue. J Cancer Res Clin Oncol 137(2):193–199. doi:10.1007/s00432-010-0875-y
Goetze K, Meyer SS, Yaromina A, Zips D, Baumann M, Mueller-Klieser W (2013) Glycolysis-related gene induction and ATP reduction during fractionated irradiation. Markers for radiation responsiveness of human tumor xenografts. Strahlentherapie und Onkologie: Organ der Deutschen Rontgengesellschaft [et al] 189(9):782–788. doi:10.1007/s00066-013-0371-9
Sattler UG, Meyer SS, Quennet V, Hoerner C, Knoerzer H, Fabian C, Yaromina A, Zips D, Walenta S, Baumann M, Mueller-Klieser W (2010) Glycolytic metabolism and tumour response to fractionated irradiation. Radiotherapy and Oncology: Journal of the European Society for Therapeutic Radiology and Oncology 94(1):102–109. doi:10.1016/j.radonc.2009.11.007
Gatenby RA, Gillies RJ (2004) Why do cancers have high aerobic glycolysis? Nat Rev Cancer 4(11):891–899. doi:10.1038/nrc1478
Fais S, Venturi G, Gatenby B (2014) Microenvironmental acidosis in carcinogenesis and metastases: new strategies in prevention and therapy. Cancer Metastasis Rev 33(4):1095–1108. doi:10.1007/s10555-014-9531-3
Feron O (2009) Pyruvate into lactate and back: from the Warburg effect to symbiotic energy fuel exchange in cancer cells. Radiotherapy and Oncology: journal of the European Society for Therapeutic Radiology and Oncology 92(3):329–333. doi:10.1016/j.radonc.2009.06.025
Jensen DH, Therkildsen MH, Dabelsteen E (2014) A reverse Warburg metabolism in oral squamous cell carcinoma is not dependent upon myofibroblasts. Journal of Oral pathology & Medicine: Official Publication of the International Association of Oral Pathologists and the American Academy of Oral Pathology. doi:10.1111/jop.12297
Tennant DA, Duran RV, Boulahbel H, Gottlieb E (2009) Metabolic transformation in cancer. Carcinogenesis 30(8):1269–1280. doi:10.1093/carcin/bgp070
Walenta S, Schroeder T, Mueller-Klieser W (2002) Metabolic mapping with bioluminescence: basic and clinical relevance. Biomol Eng 18(6):249–262
Hirschhaeuser F, Sattler UG, Mueller-Klieser W (2011) Lactate: a metabolic key player in cancer. Cancer Res 71(22):6921–6925. doi:10.1158/0008-5472.CAN-11-1457
Curry JM, Tuluc M, Whitaker-Menezes D, Ames JA, Anantharaman A, Butera A, Leiby B, Cognetti DM, Sotgia F, Lisanti MP, Martinez-Outschoorn UE (2013) Cancer metabolism, stemness and tumor recurrence: MCT1 and MCT4 are functional biomarkers of metabolic symbiosis in head and neck cancer. Cell Cycle 12(9):1371–1384. doi:10.4161/cc.24092
Brizel DM, Schroeder T, Scher RL, Walenta S, Clough RW, Dewhirst MW, Mueller-Klieser W (2001) Elevated tumor lactate concentrations predict for an increased risk of metastases in head-and-neck cancer. Int J Radiat Oncol Biol Phys 51(2):349–353
Grotius J, Dittfeld C, Huether M, Mueller-Klieser W, Baumann M, Kunz-Schughart LA (2009) Impact of exogenous lactate on survival and radioresponse of carcinoma cells in vitro. Int J Radiat Biol 85(11):989–1001. doi:10.3109/09553000903242156
S3-Leitlinie Diagnostik und Therapie des Mundhöhlenkarzinoms (2012) Leitlinienprogramm Onkologie der AWMW, Deutschen Krebsgesellschaft e.V. und Deutschen Krebshilfe e.V. http://www.awmf.org/uploads/tx_szleitlinien/007_100OLl_S3_Mundh%C3%B6hlenkarzinom_122012-122015.pdf. Accessed 28.01.2015
Barnes L. EJW, Reichart P., Sdransky D. (2005) World Health Organization classification of tumours. Pathology and genetics of head and neck tumours. IARC Press, Lyon 2005
Mueller-Klieser W, Walenta S (1993) Geographical mapping of metabolites in biological tissue with quantitative bioluminescence and single photon imaging. Histochem J 25(6):407–420
Walenta S, Voelxen N, Sattler U, Mueller-Klieser W (2014) Localizing and quantifying metabolites in situ with luminometry: induced metabolic bioluminescence imaging (imBI). In: Johannes Hirrlinger HSW (ed) Neuromethods 90 (invited review). Special volume “brain energy metabolism” Springer Science and Business Media New York New York. doi:10.1007/ 978-1-4939-1059-5
Mankoff DA, Eary JF, Link JM, Muzi M, Rajendran JG, Spence AM, Krohn KA (2007) Tumor-specific positron emission tomography imaging in patients: [18F] fluorodeoxyglucose and beyond. Clinical Cancer Research: An Official Journal of the American Association for Cancer Research 13(12):3460–3469. doi:10.1158/1078-0432.CCR-07-0074
Schwickert G, Walenta S, Sundfor K, Rofstad EK, Mueller-Klieser W (1995) Correlation of high lactate levels in human cervical cancer with incidence of metastasis. Cancer Res 55(21):4757–4759
Walenta S, Salameh A, Lyng H, Evensen JF, Mitze M, Rofstad EK, Mueller-Klieser W (1997) Correlation of high lactate levels in head and neck tumors with incidence of metastasis. The American Journal of Pathology 150(2):409–415
Sonveaux P, Copetti T, De Saedeleer CJ, Vegran F, Verrax J, Kennedy KM, Moon EJ, Dhup S, Danhier P, Frerart F, Gallez B, Ribeiro A, Michiels C, Dewhirst MW, Feron O (2012) Targeting the lactate transporter MCT1 in endothelial cells inhibits lactate-induced HIF-1 activation and tumor angiogenesis. PLoS One 7(3):e33418. doi:10.1371/journal.pone.0033418
Gillies RJ, Robey I, Gatenby RA (2008) Causes and consequences of increased glucose metabolism of cancers. Journal of Nuclear Medicine: official publication, Society of Nuclear Medicine 49 Suppl 2:24S-42S. doi:10.2967/jnumed.107.047258
Martinez-Outschoorn UE, Lisanti MP, Sotgia F (2014) Catabolic cancer-associated fibroblasts transfer energy and biomass to anabolic cancer cells, fueling tumor growth. Semin Cancer Biol 25:47–60. doi:10.1016/j.semcancer.2014.01.005
Romero IL, Mukherjee A, Kenny HA, Litchfield LM, Lengyel E (2015) Molecular pathways: trafficking of metabolic resources in the tumor microenvironment. Clinical Cancer research: An Official Journal of the American Association for Cancer Research 21(4):680–686. doi:10.1158/1078-0432.CCR-14-2198
Doherty JR, Cleveland JL (2013) Targeting lactate metabolism for cancer therapeutics. J Clin Invest 123(9):3685–3692. doi:10.1172/JCI69741
Choi SY, Collins CC, Gout PW, Wang Y (2013) Cancer-generated lactic acid: a regulatory, immunosuppressive metabolite? J Pathol 230(4):350–355. doi:10.1002/path.4218
Federici C, Petrucci F, Caimi S, Cesolini A, Logozzi M, Borghi M, D'Ilio S, Lugini L, Violante N, Azzarito T, Majorani C, Brambilla D, Fais S (2014) Exosome release and low pH belong to a framework of resistance of human melanoma cells to cisplatin. PLoS One 9(2):e88193. doi:10.1371/journal.pone.0088193
Groussard C, Morel I, Chevanne M, Monnier M, Cillard J, Delamarche A (2000) Free radical scavenging and antioxidant effects of lactate ion: an in vitro study. Journal of Applied physiology (Bethesda, Md: 1985) 89(1):169–175
Hsu HW, Wall NR, Hsueh CT, Kim S, Ferris RL, Chen CS, Mirshahidi S (2014) Combination antiangiogenic therapy and radiation in head and neck cancers. Oral Oncol 50(1):19–26. doi:10.1016/j.oraloncology.2013.10.003
Bola BM, Chadwick AL, Michopoulos F, Blount KG, Telfer BA, Williams KJ, Smith PD, Critchlow SE, Stratford IJ (2014) Inhibition of monocarboxylate transporter-1 (MCT1) by AZD3965 enhances radiosensitivity by reducing lactate transport. Mol Cancer Ther 13(12):2805–2816. doi:10.1158/1535-7163.MCT-13-1091
Acknowledgments
This work was supported by the Deutsche Forschungsgemeinschaft (MU 576/19-1; ZI 1461/2-1) and by the German Federal Ministry of Education and Research („ISIMEP“; 02NUK016A).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Blatt, S., Voelxen, N., Sagheb, K. et al. Lactate as a predictive marker for tumor recurrence in patients with head and neck squamous cell carcinoma (HNSCC) post radiation: a prospective study over 15 years. Clin Oral Invest 20, 2097–2104 (2016). https://doi.org/10.1007/s00784-015-1699-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-015-1699-6