Abstract
The purpose of this study is to develop a scale (Perinatal Anxiety Screening Scale, PASS) to screen for a broad range of problematic anxiety symptoms which is sensitive to how anxiety presents in perinatal women and is suitable to use in a variety of settings including antenatal clinics, inpatient and outpatient hospital and mental health treatment settings. Women who attended a tertiary obstetric hospital in the state of Western Australia antenatally or postpartum (n = 437) completed the PASS and other commonly used measures of depression and anxiety. Factor analysis was used to examine factor structure, and ROC analysis was used to evaluate performance as a screening tool. The PASS was significantly correlated with other measures of depression and anxiety. Principal component analyses (PCA) suggested a four-factor structure addressing symptoms of (1) acute anxiety and adjustment, (2) general worry and specific fears, (3) perfectionism, control and trauma and (4) social anxiety. The four subscales and total scale demonstrated high to excellent reliabilities. At the optimal cutoff score for detecting anxiety as determined by ROC analyses, the PASS identified 68 % of women with a diagnosed anxiety disorder. This was compared to the EPDS anxiety subscale which detected 36 % of anxiety disorders. The PASS is an acceptable, valid and useful screening tool for the identification of risk of significant anxiety in women in the perinatal period.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
There has been increasing recognition of the high prevalence and impact of anxiety symptoms and disorders in the perinatal period. The prevalence of anxiety disorders in the antenatal period ranges from 6.6 (Andersson et al. 2004) to 21.7 % (Borri et al. 2008; Grant et al. 2008). Research suggests that anxiety disorders are more common than depressive disorders in the perinatal period (Matthey et al. 2003). In addition, elevated anxiety (not meeting diagnostic criteria) is common during pregnancy and postnatally. Heron et al. (2004) in a community sample of 8,323 women found that approximately 15 % of women reported elevated anxiety in the antenatal period, and rates were comparable postnatally (13 %). Despite variations in the published prevalence rates, the prominence of anxiety in the perinatal period is evident.
There is also mounting evidence of the detrimental effects and sequelae of maternal anxiety on mothers and infants. Elevated untreated anxiety in pregnancy may impact negatively on the developing baby (Glasheen et al. 2010; Grant et al. 2008; Ibanez et al. 2012). Antenatal anxiety may have long-term negative effects on the child’s cognitive (Bergman et al. 2010), emotional and behavioural development (O’Connor et al. 2002). Antenatal anxiety can also be detrimental to maternal health during pregnancy (Johnson and Slade 2003) and postnatally (Matthey et al. 2003; Milgrom et al. 2008). In the postnatal period, mothers presenting with a generalised anxiety disorder have been described as less responsive and less engaged during interaction with their infants, who are more likely to be withdrawn and show less positive emotional tone than infants from non-anxious mothers (Stein et al. 2012). This supports previous findings on the association between maternal anxiety and insecure attachment in young children (Stevenson-Hinde et al. 2011). The risk of postnatal depression has been found to be three times higher for women with anxiety disorders during pregnancy (Sutter-Dallay et al. 2004). Antenatal anxiety is one of the strongest predictors of postnatal depression (Milgrom et al. 2008). Furthermore, postnatal anxiety appears to be preceded by antenatal anxiety in two thirds of women (Heron et al. 2004). Given this, the detection of problematic anxiety via the use of an effective screening tool may be important in screening for risk, prevention, early intervention and treatment in the field of perinatal mental health.
Clinical presentations of perinatal anxiety are varied. Ross and McLean’s (2006) review found that the prevalence rates of panic disorder (1.3 to 2.0 %), post-traumatic stress disorder (PTSD, 0.6 to 7.7 %), generalised anxiety disorder (GAD, 8.5 %) and obsessive compulsive disorder (OCD, 0.2 to 3.9 %) in the perinatal period were the same as or higher than in the general population. Phillips et al. (2007) found that 30.5 % of their sample of women attending a residential unit for complex early parenting difficulties met the diagnostic criteria for an anxiety disorder, with panic disorder, social phobia, specific phobias and OCD all represented. Anxiety disorder not otherwise specified (ADNOS) was identified as the most common anxiety diagnosis during pregnancy (Andersson et al. 2004), with prevalence rates as high as 10.8 % (Phillips et al. 2007). In their follow-up study, Phillips et al. (2009) found that women diagnosed with ADNOS were experiencing excessive and uncontrollable worry confined to their baby and/or motherhood, which they termed ‘maternally focused worry’. These findings suggest that screening for perinatal anxiety should include a broad range of anxiety presentations across the various anxiety disorders and specific maternal and pregnancy-focused anxieties.
Current Australian National Postnatal Depression Initiative (NPDI) guidelines advocate for universal perinatal screening including depression and psychosocial risk (Austin and Highet 2011). Whilst it is recognised amongst clinicians and researchers that screening for perinatal anxiety is warranted, effective screening remains limited due to the measures currently available. General anxiety measures (i.e. measures of anxiety developed for other populations and used with perinatal women) are most commonly used to detect anxiety in perinatal populations (Meades and Ayers 2011). However, several problems arise from this reliance on general measures. Firstly, general anxiety measures may include questions about physical symptoms of anxiety common in pregnancy. Items such as “I can sit at ease and feel relaxed” (HADS; Zigmond and Snaith 1983), “I feel rested” and “I feel comfortable” (STAI; Spielberger et al. 1983) and those which ask about symptoms such as ‘discomfort in abdomen’, ‘difficulty breathing’, ‘feeling faint’ or ‘flushed’ (Beck Anxiety Inventory; Beck and Steer 1993) may inflate anxiety scores and result in identification of false positives (Swallow et al. 2003) in perinatal populations. Secondly, the cutoff scores indicative of problematic anxiety for some general measures have not been validated in perinatal samples (e.g. the STAI; Field et al. 2010; Grant et al. 2008; Moss et al. 2009). Finally, anxiety disorders in pregnancy and the postnatal period may not be optimally defined when using general measures. Pregnancy-specific anxieties, such as fear of childbirth, intrusive ego-dystonic thoughts of the baby being harmed or dying, losing control in labour or not coping with the pain of labour or as a parent, may be relatively distinct problematic anxiety presentations in the perinatal period that are not relevant in the general population (Huizink et al. 2004) and not included in screening for anxiety using general anxiety measures. Therefore, the use of general anxiety measures may limit the accurate detection of perinatal anxiety. Given the limitations of using general anxiety measures with perinatal women, a review of measures that have been developed to screen for anxiety specific to the perinatal period is warranted.
Although used less frequently perinatally than general anxiety measures, self-report questionnaires which have been developed specifically to screen for aspects of perinatal anxiety include the Pregnancy Anxiety Scale (PAS; Levin 1991), the Pregnancy-Related Anxiety Questionnaire (PRAQ; Van den Bergh 1989) and the Pregnancy-Related Anxiety Scale (PRAS; Wadhwa et al. 1993). These measures assess fears related to the birth (PAS, PRAQ, PRAQ-R and PRAS), the pregnancy (PAS), the baby’s health and safety (PRAS; e.g. bearing a physically or mentally handicapped child; PRAQ), the mother’s concerns about her physical appearance (PRAQ-R), the health-care providers (PRAS), the problems in the mother-child relationship (PRAQ) and the changes in the mother’s personal life and relationship with her partner (PRAQ). However, these measures, whilst relevant to the perinatal period, have narrow domains and are not a broad screen for the range of problematic anxiety symptoms that may be of concern. They do not indicate the risk of significant clinical levels of anxiety or specific anxiety disorders. Therefore, elevated symptoms of a range of anxiety disorders in perinatal women may go undetected with the use of these as screening instruments.
The NPDI recommends screening using the Edinburgh Postnatal Depression Scale (Cox et al. 1987) which is the most widely used and recommended screening scale for perinatal depression. The EPDS contains three anxiety-related items, but it does not distinguish whether reported anxiety symptoms are a feature of depression or a separate clinical entity (Ross et al. 2003). Thus, the Edinburgh Postnatal Depression Scale detects but does not distinguish anxiety disorders from depression in mothers of infants and is therefore limited as a perinatal anxiety screening tool (Matthey et al. 2013; Muzik et al. 2000; Rowe et al. 2008). Recently, O’Hara et al. (2012) concluded that anxiety can be detected with very few items based on the finding that the combination of three items that assessed symptoms of panic, restlessness and problems with sleeping estimated the prevalence of GAD most accurately. However, this measure did not screen for the broad range of problematic anxiety and was restricted to the postnatal period. O’Hara et al. acknowledged that their measure may be a useful screen for problematic anxiety that may be then followed up with a more comprehensive measure.
To the authors’ knowledge, a screening tool for perinatal anxiety that detects symptoms across a broad range of anxiety presentations that is not confounded with common physiological pregnancy symptoms and is sensitive to perinatal anxiety presentations and concerns is not yet available. Accordingly, the aims of this study were twofold. Firstly, to develop and validate a screening scale designed to screen for a broad range of problematic anxiety symptoms that is sensitive to how anxiety presents in perinatal women. The secondary aim was for the Perinatal Anxiety Screening Scale (PASS) to provide clinicians and researchers with an effective tool to screen for problematic perinatal anxiety with cutoff scores maximising sensitivity and specificity in a perinatal population with some indication of the nature of anxiety symptoms being experienced. To evaluate the PASS, the factor structure, comparison with other screening scales, validity, reliability, acceptability and performance as a case finder for anxiety disorders was examined.
Materials and method
Research setting and overview of questionnaire development
The research was conducted at King Edward Memorial Hospital (KEMH), the largest public tertiary obstetric hospital and neonatal intensive care unit in Western Australia. Australian citizens or permanent residents are able to obtain free treatment via the universal publicly funded health-care scheme. Obstetrically complex patients as well as those who do not have or cannot afford private health insurance cover are managed at KEMH. This is in contrast to the private hospital system which is available to patients who have private health insurance. Over 6,000 births are managed at KEMH each year. Care is provided for routine pregnancies and births as well as specialised services for women with obstetrically high-risk pregnancies and other groups of women with increased risk of perinatal complications such as women with substance use issues, diabetes and serious mental illness. KEMH also incorporates an eight-bed Mother Baby Unit (MBU) which provides statewide inpatient perinatal mental health services.
Mental health services to the general hospital are provided by the Department of Psychological Medicine to inpatients and outpatients of the hospital. The department receives over 2,000 referrals each year, most of which are from obstetrics for perinatal women.
Participants
Participants included antenatal and postnatal English speaking and literate adult (18 years and over) women up to 6 months post-partum who attended KEMH antenatal clinics (both high risk and routine clinics), the Department of Psychological Medicine or were hospitalised at the MBU. The aim was to include as broad a range of obstetric, general community and mental health presentations as possible. Women in the acute stages of psychiatric or obstetric presentations or who experienced a current pregnancy loss, stillbirth or neonatal death were not recruited to participate.
Measures
The Edinburgh Postnatal Depression Scale (EPDS; Cox et al. 1987) is a 10-item self-report questionnaire administered to screen for depressive symptoms in the antenatal and postnatal periods (Murray and Cox 1990). The EPDS has high reliability (0.87) and sensitivity as a screen for depression (95 %; Harris et al. 1989). Three items (item 3, “blamed myself unnecessarily when things go wrong”; 4, “been anxious or worried for no good reason”; 5, “felt scared or panicky for no good reason”) have been found to cluster together on an anxiety factor (EPDS-A) with an optimum cutoff score of 6 or more to indicate probable anxiety (Matthey 2008).
The Depression, Anxiety and Stress Scale 21 (DASS 21; Lovibond & Lovibond 1995) is a 21-item self-report questionnaire that consists of three subscales measuring current (‘over the past week’) symptoms of depression, anxiety and stress on a four-point Likert scale. Subscale scores are calculated by adding the rating scores of the seven items of each scale, with higher scores indicative of more severe depression, anxiety or stress. The DASS 21 is well-validated and demonstrates high internal consistency and construct validity (Osman et al. 2012).
The Spielberg State-Trait Anxiety Inventory (STAI; Spielberger et al. 1983) is a 40-item self-report questionnaire with separate subscales to measure situational (state) and stable (trait) levels of anxiety. Patients respond on a four-point Likert scale, with higher scores indicative of higher anxiety. The STAI is a reliable and valid measure used with clinical and non-clinical populations (Spielberger et al. 1983) and in perinatal samples (Grant et al. 2008). Scores above 45 (Figueiredo and Conde 2011) and 48 (Field et al. 2007) have been used to indicate risk of problematic anxiety in perinatal samples.
The Beck Depression Inventory-II (BDI; Beck et al. 1996a, b) measures the severity of 21 symptoms of depression experienced during the past 2 weeks for clinical and non-clinical samples. Higher total scores indicate more severe depressive symptoms. The BDI-II is a psychometrically sound measure with high test–retest reliability (Beck et al. 1996a, b) and internal consistency (Beck et al. 1996a, b).
A Social Circumstances Checklist was developed by the authors to provide further demographic information on the study sample about the presence of psychosocial stressors as rated by respondents which may be associated with symptoms of anxiety, such as difficulties during the pregnancy, significant events (e.g. car accident, planning a wedding), personal abuse or trauma (e.g. victim or witnessed violence and abuse), loss of support, relationship difficulties, accommodation problems (e.g. homeless) and financial issues (see Appendix A in Electronic Supplementary Material). Participants were asked to indicate whether they had experienced each psychosocial stressor in the past 12 months. The checklist provided information about the total number and nature of stressors.
General demographic information
Information on demographics (e.g. age, marital status and occupation), prior and current pregnancies and births (e.g. mode of delivery, pregnancy complications and history of miscarriage), medication use including psychotropic medications, current or past psychiatric problems or other substance misuse pertaining to participants, was obtained from patient medical records in the same way for all participants. Categories of background information are recorded in patient medical records which are set out in the same sections, and the same demographic data is routinely collected by admissions officers and midwives from patients at admission and entered into the medical record. To facilitate consistency in the extraction and coding of the variables for all study participants, only two research officers reviewed patient medical records and a pro forma was developed for data extraction.
Skills level of occupation for the study sample and comparison with the Australian population was derived from the index published by the Australian and New Zealand Standard Classification of Occupation (ANZSCO Version 1.2), which is based on census variables including household income and employment. This index assigns a value of one (highest skill level, e.g. university degree or higher qualification) to five (lowest skill level, e.g. minimum Australian compulsory education level) to each occupation based on the amount and level of formal education, occupational experience and on the job training required.
PASS questionnaire development
The PASS questionnaire was developed by a panel of five experienced, specialist perinatal psychologists in the Department of Psychological Medicine at KEMH. The experience in how to effectively ask perinatal women about their anxiety in assessment and therapy interviews was incorporated into the wording of scale items.
Stage 1: item generation
Development of the screening scale items was informed by clinical practice, reviewing validated anxiety questionnaires and the wording used in nationally disseminated anxiety information sheets and online websites generated by Beyondblue (2013) and the Australian National Postnatal Depression Initiative (Austin and Highet 2011). The questions were developed to systematically encompass DSM and ICD-10 symptoms and diagnostic criteria for the various anxiety disorders including GAD, panic disorder, OCD, social anxiety, PTSD, adjustment disorder and phobias. Two screening questions for dissociative disorder were also included given their relevance to trauma and PTSD in the perinatal period. Women who have had previous sexual abuse or traumatic birth experiences may present over the course of perinatal experiences with symptoms of dissociation (Beck 2004; Zambaldi et al. 2011) which can be problematic during delivery and routine perinatal care.
Thirty-eight items were generated to screen for anxiety disorders and formatted as a self-report questionnaire with a four-point Likert scale assessing the frequency of the symptoms with consistent descriptors (from 0 = ‘Not at all’ to 3 = ‘All the time’). Seven items were reversed as positive statements to avoid response set bias. The timeframe for rating frequency of symptoms was limited to over the past month in order to limit the length required of retrospective memory recall. Symptoms were rated for longer than the past week to avoid responses being mainly in terms of short-term reactions to situational stressors. The design and presentation of the scale were extensively reviewed to ensure it was streamlined and easy to respond to. The Likert scale with consistent response options for each item was used to facilitate ease of completion as the respondent would not be required to rethink each item. The wording of items was subjected to a computer literacy check (Flesch-Kincaid Grade Level test) as being understandable for someone with 5 years of education or a 10-year-old child (Kincaid et al. 1975). The preliminary PASS scale was reviewed via a standard feedback questionnaire by a focus group of 15 perinatal women from the general community for acceptability. The feedback from these women was incorporated into the questionnaire wording, design, presentation and format.
Stage 2: pilot study
A pilot study was conducted with 50 women recruited from the KEMH antenatal clinics to assess comprehensibility of language and phrasing, ease of administration and responding and any other implementation issues. An examination of the answer patterns for the PASS scale suggested that participants were reluctant to endorse ‘All the time’; therefore, this option was reformulated as ‘Almost all the time’ (see Table 5 for wording of retained items).
Stage 3: examination of factor structure and scale validation
Procedure
The research was approved by the Women and Newborn Health Service ethics committee for conducting the research at King Edward Memorial Hospital. Research officers recruited as many women as possible whilst the women waited at the antenatal clinics and the Department of Psychological Medicine for their respective appointments. MBU women were recruited by the nursing staff within 24 h of admission.
Recruitment was conducted by two Ph.D. Psychology graduates or mental health nurses who gauged the women’s eligibility (age, understanding of English) by direct questioning and explained the requirements of participation. Women who were interested in participating were asked to read the information sheet and sign the required consent form which also sought permission to contact them postnatally to obtain postnatal data.
All participants completed the PASS, EPDS, DASS 21, STAI and a social circumstances checklist. In addition, the BDI was completed by participants recruited from the Department of Psychological Medicine and the MBU as part of routine baseline screening measures for patients referred to these mental health facilities.
Ease and acceptability of the PASS were assessed by including an additional question at the end of the PASS for the whole sample: Rate how easy this questionnaire was to complete along a scale from “not at all easy” (0) to “extremely easy” (10). Time to complete the PASS was assessed for a subsample (n = 11) of women recruited from the Department of Psychological Medicine with English as their first language by asking them to record the time they started and finished the PASS prior to their assessment interview.
Women referred to the Department of Psychological Medicine or the MBU were assessed via a diagnostic assessment interview by experienced mental health professionals (psychologists and psychiatrists) who were blind to the PASS scores. The clinicians used a standardised pro forma that included relevant areas for assessment such as presenting symptoms and concerns, social and developmental history and personal and familial psychiatric history (Appendix B in Electronic Supplementary Material). The assessment interview was conducted on the same day and, in most cases, immediately after the questionnaires were completed. The complete assessment was presented at a case presentation meeting and reviewed by a multidisciplinary team of usually five or six clinical staff including psychologists, psychiatrists and mental health nurses blind to the PASS responses to reach a consensus decision on the ICD 10 diagnosis recorded.
Antenatal participants who had consented to being recontacted in the postnatal period were phoned by the research officers between 2 and 6 months following the birth of their baby and invited to complete the questionnaires again. Women were posted the questionnaires and requested to return them using reply-paid envelopes. If the questionnaires were not returned within 6 weeks, the women were contacted (by phone or letter) as a reminder.
Data analyses
Data were summarised using means and frequency distributions for categorical data. When postnatal responses had been provided, antenatal responses from this group of women were excluded from analyses (except for the test–retest analysis) to avoid double representation of participants.
The factor structure of the PASS was analysed using principal components analysis (PCA) with oblique (oblimin) rotation, as recommended for correlated variables (Field, 2009). The convergent and discriminant validity of the PASS were assessed by conducting Pearson product–moment correlations between the PASS global score and the EPDS, DASS 21, STAI and BDI. Test–retest reliability of the PASS was assessed by examining the correlation between total PASS scores in the antenatal and postnatal period for a subsample of participants (n = 35) who completed the PASS antenatally and postnatally.
The subsample of 53 women with an ICD-10 anxiety disorder diagnosis was used to conduct a receiver operating characteristic (ROC) curve analysis to assess the diagnostic accuracy of the PASS and determine a cutoff score that optimally detected cases defined by presence or absence of an ICD-10 diagnosis for an anxiety disorder. The cutoff score is determined by the point at which there is the best tradeoff between sensitivity (percentage of cases correctly identified) and false-positive rates (percentage of cases incorrectly identified). The area under the ROC curve (AUC) describes the discriminative accuracy of cutoff scores in relation to a criterion with a range of 0.5 (poor classification ability) to 1 (perfect classification ability). The discriminative accuracy (i.e. percentage of cases correctly identified as having an anxiety disorder diagnosis) of the PASS cutoff score (as determined by ROC analyses) was compared to the discriminative accuracy of the recommended cutoff scores for the STAI (45; Figueiredo and Conde 2011) and the EPDS-A (6; Matthey 2008). Data analysis was performed using SPSS version 17.0 (SPSS Inc., Chicago, IL) and p values <0.05 were considered statistically significant.
Results
Participants
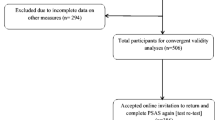
Of the 844 women approached and invited to participate between March 2012 and February 2013, 51.7 % (n = 437) agreed to participate, were eligible and returned the questionnaires. Participants with an incomplete PASS were excluded from analyses (n = 45), resulting in a final sample of 393 (see Fig. 1). Antenatal women comprised 79 % of the sample (please see Table 1 for further information about the sample composition) and on average were 28.5 weeks gestation at the time of participating in the study. There was no difference between the study sample and the Western Australian (WA) population of women giving birth in 2010 for mean age (29 years) and marital status (85 % married) (Joyce and Hutchinson, 2012). Participants’ occupations were most frequently classified as highest skill level (18.6 % of the sample) and second lowest skill level (13.7 %) (see Table 2). The proportion of primiparous women in the study sample (26.5 %) was less than the WA population of women giving birth (42.4 %). Obstetric complications were recorded for 48.7 % of women in the study sample compared to 67.4 % for the WA population. However, obstetric problems were recorded at the time of participation in the study for the sample (on average at 28.5 weeks gestation) compared to at the end of the pregnancy for the WA population (Joyce and Hutchinson, 2012). Of the sample, 7.3 % reported a current medical problem with the baby. Of the study sample, 5.6 % had experienced fertility problems (including difficulties conceiving that may or may not have required fertility treatment) compared to 3.6 % of women who gave birth in WA and required fertility treatment. Overall, the study sample appears to be reflective of the Western Australian population of women giving birth for a number of important variables.
The study sample comprised more women with a psychiatric diagnosis (according to a diagnostic assessment; 39 %) compared to the WA population of women giving birth (6.7 %) which was not surprising given a proportion of the study sample was recruited from mental health services (see Table 3 for information regarding the diagnoses of participants recruited from Psychological Medicine and the MBU).
Participants with a psychiatric diagnosis on average scored in the mild ranges on the EPDS and DASS Stress subscale and in the moderate ranges on the DASS Depression and Anxiety subscales and the BDI (see Table 4). Participants with no known psychiatric diagnosis on average scored below the published cutoff scores for problematic anxiety, depression and stress according to the EPDS, STAI and DASS (see Table 4). These findings support the validity of the diagnoses obtained via assessment interview. Participants reported diverse obstetric histories and psychosocial stressors (see Table 2).
Factor structure of the PASS
Sampling adequacy was excellent (Kaiser-Meyer-Olkin = 0.96). Inter-item correlations were sufficiently large for PCA (Bartlett’s test of sphericity = χ 2 (465) = 7,766.8, p < 0.01). An initial PCA revealed that the seven positively phrased items formed a separate ‘parental confidence’ factor which affected the specificity of the scale. A review of items revealed that a broad range of anxiety symptoms remained covered when the positively phrased items were removed, producing a 31-item scale. The PCA was conducted again excluding the positively phrased items. Four factors were retained based on the results of the scree test (Cattell 1966), the Parallel Analysis test and MAP test (Velicer et al. 2000), which in combination explained 59.37 % of the variance.
An examination of the factor loadings after rotation (see Table 5) suggested that factor 1 (acute anxiety and adjustment) had eight items that addressed symptoms of panic disorder, dissociative disorder and adjustment difficulties; factor 2 (general worry and specific fears) included 10 items covering symptoms of GAD and phobia; factor 3 (perfectionism, control and trauma) had eight items covering symptoms of OCD and PTSD; and factor 4 (social anxiety) had five items that addressed social anxiety. Several items with factor loadings below the 0.4 threshold were retained due to their clinical relevance. These items were the following: “Feeling panicky”, “Feeling agitated”, “Really strong fears about things, e.g., needles, blood, birth, pain, etc.”, “Sudden rushes of extreme fear or discomfort”, “Repetitive thoughts that are difficult to stop or control”, “Difficulty sleeping even when I have the chance to sleep”, “Being ‘on guard’ or needing to watch out for things” and “Upset about repeated memories, dreams or nightmares”.
Cross-loading items (i.e. items, 7, 8, 16, 17 and 26) were retained in the factor showing the highest loading and consistency with clinical anxiety presentations. Items 7 (“feeling panicky”) and 8 (“feeling agitated”) were retained in factor 1 (i.e. acute anxiety and adjustment) due to their consistency with panic disorder items in the same factor. Item 16 (“sudden rushes of extreme fear or discomfort”) was originally developed to address symptoms of panic disorder, but retained in factor 2 (i.e. general worry and specific fears) due to its association with item 15, which is a clinical indicator of phobia (i.e. “Really strong fears about things, e.g., needles, blood, birth, pain, etc.”). Similarly, item 17 (“repetitive thoughts that are difficult to stop or control”), which was developed to address OCD symptoms, was also retained in factor 2 as an indicator of excessive worry.
Item 23 (“feeling jumpy or easily startled”) had similar loadings on factors 1 (i.e. acute anxiety and adjustment) and 3 (i.e. perfectionism, control and trauma). Though this item could address symptoms of panic disorder, it is applicable to the hypervigilance which characterises PTSD along with item 25 (i.e. “being on guard or needing to watch out for things”). Therefore, it was retained in factor 3. Finally, item 26 (“upset about repeated memories, dreams or nightmares”) cross-loaded on factors 2 (i.e. general worry and specific fears) and 3 (i.e. perfectionism, control and trauma) and was retained in factor 3 as an indicator of intrusive, repetitive thoughts and memories associated with PTSD.
The four subscales had high reliabilities (Cronbach’s α ranged from 0.86 to 0.90; see Table 5) and were correlated moderately (r values ranged from 0.4 to 0.51) which supported the internal construct validity of the PASS. The complete scale had also excellent reliability (Cronbach’s α = 0.96).
Acceptability of the PASS
The average score for the ease of completion item on the PASS was 8.56 (median = 8, range = 2–10) with 10 indicative of “extremely easy” to complete. The range of times taken to complete the 31-item PASS was 2 to 10 min (mean completion time = 6 min).
Convergent validity of the PASS
The PASS global score was significantly correlated with the DASS Anxiety and Stress subscales, anxiety subscale of the EPDS, STAI-State and STAI-Trait which are indicative of adequate convergent validity. The PASS global score was also significantly correlated with the BDI and EPDS total score (see Table 6).
Test–retest reliability
The Pearson correlation coefficients were calculated to assess the test–retest reliability of the PASS for a subsample of participants (n = 35) who completed the PASS antenatally and postnatally. The correlation for the PASS global scores was 0.74, indicative of adequate test–retest reliability.
Screening accuracy of the PASS
Analyses revealed that the optimal cutoff PASS score for detecting anxiety was 26, which yielded an AUC of 0.7 (standard error = 0.04) with a sensitivity and specificity of 0.7 and 0.3, respectively (see Fig. 2).
The results revealed that at the recommended cutoff score for the PASS (26), STAI (45) and EPDS-A (6), the PASS performed slightly better than the STAI-S, which detected 68 % (n = 36) and 64 % (n = 34), respectively, of women with an anxiety disorder diagnosis. The EPDS-A identified only 36 % (n = 19) of the cases.
Discussion and conclusion
The results suggest that the PASS is an acceptable and psychometrically sound measure that performed well in screening for anxiety disorders in the perinatal period. It has a four-factor structure described as (1) acute anxiety and adjustment, (2) general worry and specific fears, (3) perfectionism, control and trauma and (4) social anxiety.
The receiver operating characteristics indicated that the PASS performed well at detecting women with an anxiety disorder diagnosis. An optimal balance between sensitivity and specificity occurred when caseness was defined by a score of 26 or above on the PASS. At this cutoff score, 68 % of women with a diagnosis of an anxiety disorder were identified. These results indicate good case-finding abilities of the PASS in samples of perinatal women. Women who score above the threshold may benefit from referral for further psychological assessment.
The internal reliability coefficients of the total scale and all four subscales were good to excellent (George and Mallery 2003). As expected, the PASS total score correlated positively and significantly with measures of anxiety, supporting the convergent validity of the PASS. The PASS was also significantly and positively correlated with measures of depression. This finding is not surprising given the extensive co-morbidity between anxiety and depression which are evident in the literature and the study sample. A recent study indicated that up to 63 % of adults diagnosed with an anxiety disorder met the diagnostic criteria for a depressive disorder (Lamers et al. 2011). Co-morbid depression and anxiety may be more common in pregnant women than independent diagnoses of depression and anxiety (Field et al. 2010). The study sample had 20 % of diagnoses with symptoms characteristic of both anxiety and depression (e.g. adjustment disorder or mixed anxiety and depression). Burns and Eidelson (1998) have accounted for the significant correlations between measures of depression and anxiety by suggesting that they have a shared causal factor. Based on this, these authors suggested that the correlation between any valid and reliable measure of depression and anxiety should be at the 0.70 level. The correlations between the PASS and measures of depression used in the study ranged from 0.77 to 0.83 (Table 3).
The PASS performed better than the EPDS-A at identifying problematic anxiety. The PASS identified almost twice the number of women with an anxiety disorder than the three anxiety questions on the EPDS (EPDS-A). This finding suggests that the current practice of routine screening with the EPDS-A to detect perinatal anxiety may result in a failure to identify a significant number of women with problematic anxiety. It is not surprising that the case-finding ability of the PASS was better than the EPDS-A given that the EPDS anxiety questions do not cover the broad range of anxiety disorders that are included in the PASS. The small number of items on the EPDS-A may also compromise its case-finding ability. The correct identification of clinical cases with instruments with a small number of items may be significantly influenced by the responses to one or two items (Condon and Corkindale 1997). Though this phenomenon may also occur when using longer measures, it is likely that inclusion of more items may buffer the influence of responses to single questions.
The PASS performed only slightly better than the STAI-S at identifying cases of problematic anxiety. However, unlike the STAI-S, the PASS screens for symptoms of anxiety characteristic of the broad range of anxiety disorders as they present for perinatal women (such as fear that harm will come to the baby and fear of birth). Therefore, item analysis of the PASS may be more useful to guide further assessment and referral for perinatal women compared to the STAI-S. Further studies using larger samples are required to explore the benefits associated with the use of the PASS compared to the STAI-S with pregnant and postnatal women.
It may also be beneficial for future research to develop a shortened version of the PASS which may be possible given the high inter-item correlations. This may enhance ease of use in busy community practice settings.
Several limitations warrant consideration. Firstly, the results of this study are limited by the clinical characteristics of the sample. Some participants with anxiety had co-morbidities with other disorders, such as depression. This affected the results regarding the specificity of the PASS. Further, some specific anxiety disorders such as social anxiety, OCD and phobia were not sufficiently represented in the sample. A larger sample representation of these anxiety disorders would be required to determine if the specific subscales of the PASS predict a higher risk of particular anxiety disorders. The fact that the diagnoses were reviewed by a multidisciplinary team of mental health clinicians increased the accuracy of diagnoses. However, the diagnostic assessment did not include a standardised psychometric measure which may limit the level of accuracy of the diagnoses in the study. Future validation studies for the PASS may be strengthened with the use of a standardised diagnostic interview.
Finally, the factor structure of the PASS may be affected by the cross-loading items which were retained. Though these items do not sufficiently discriminate between the components of the PASS, their clinical relevance to the overall screening of heterogeneous anxiety disorders warranted their retention in the scale. Further validation studies in other clinical samples may overcome these limitations.
Despite these limitations, this study has significant clinical and research implications. Due to the possible long-term consequences on infants and mothers, perinatal anxiety requires early detection and treatment, yet its identification has been restricted by the lack of specific screening measures developed for anxiety in perinatal women. The PASS is the first questionnaire to date that screens for a broad range of anxiety disorders in addition to some common fears specific to the perinatal period. The PASS presents as a valid and useful instrument for the identification of pregnant women and new mothers who present with problematic anxiety. It is easy to use and score with a validated recommended clinical cutoff score for screening use in perinatal women. Further validation in clinical populations may confirm its usefulness in identifying the nature of anxiety being experienced with implications for relevant referral pathways, specialist assessment and treatment approaches. The PASS is an important addition to the existing literature on perinatal anxiety and has the potential to provide a significant, more precise and effective complementary choice for practitioners in routine perinatal mental health screening. The PASS also represents an additional option for use in future research targeting perinatal anxiety where there has been a tendency due to lack of more specific perinatal anxiety measures to focus on depression with an assumption of incorporating stress and anxiety.
References
Andersson L, Sundström-Poromaa I, Wulff M, Åström M, Bixo M (2004) Implications of antenatal depression and anxiety for obstetric outcome. Obstet Gynecol 104:467–476
Austin M, Highet N (2011) Guidelines expert advisory committee: clinical practice guidelines for depression and related disorders—anxiety, bipolar disorder and puerperal psychosis—in the perinatal period. A guideline for primary care professionals. Beyond Blue - The National Depression Initiative, Melbourne
Beck A, Steer R, Ball R, Ranieri W (1996a) Comparison of Beck Depression Inventories—IA and II in psychiatric outpatients. J Pers Assess 67:588–597
Beck A, Steer R, Brown G (1996b) Beck Depression Inventory: second edition manual. Psychological Corporation, San Antonio
Beck AT, Steer RA (1993) Beck Anxiety Inventory Manual. Psychological Association, San Antonio
Beck CT (2004) Post-traumatic stress disorder due to childbirth: the aftermath. Nurs Res 53:216–224
Bergman K, Sarkar P, Glover V, O’Connor TG (2010) Maternal prenatal cortisol and infant cognitive development: moderation by infant-mother attachment. Biol Psychiatry 67:1026–1032
Beyondblue (2013) Anxiety during pregnancy and early parenthood from http://www.beyondblue.org.au/resources/for-me/pregnancy-and-early-parenthood/mental-heath-conditions/anxiety. Accessed 10 Jan 2013
Borri C, Mauri M, Oppo A, Banti S, Rambelli C, Ramacciotti D et al (2008) Axis I psychopathology and functional impairment at the third month of pregnancy: results from the Perinatal Depression-Research and Screening Unit (PND-ReScU) study. J Clin Psychiatry 69:1617–1624
Burns DD, Eidelson RJ (1998) Why are depression and anxiety correlated? A test of the tripartite model. J Consult Clin Psychol 66:461
Cattell RB (1966) The scree test for the number of factors. Multivar Behav Res 1:245–276
Condon JT, Corkindale CJ (1997) The assessment of depression in the postnatal period: a comparison of four self-report questionnaires. Aust N Z J Psychiatry 31:353–359
Cox J, Holden J, Sagovsky R (1987) Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br J Psychiatry 150:782–786
Field A (2009) Discovering statistics using SPSS, 3rd edn. Sage, London
Field T, Diego M, Hernandez-Reif M, Figueiredo B, Deeds O, Ascencio A et al (2010) Comorbid depression and anxiety effects on pregnancy and neonatal outcome. Infant Behav Dev 33:23–29
Field T, Diego M, Hernandez-Reif M, Figueiredo B, Schanberg S, Kuhn C (2007) Sleep disturbances in depressed pregnant women and their newborns. Infant Behav Dev 30:127–133
Figueiredo B, Conde A (2011) Anxiety and depression in women and men from early pregnancy to 3-months postpartum. Arch Wom Ment Health 14:247–255
George D, Mallery M (2003) Using SPSS for Windows step by step: a simple guide and reference. Allyn & Bacon, Boston
Glasheen C, Richardson GA, Fabio A (2010) A systematic review of the effects of postnatal maternal anxiety on children. Arch Wom Ment Health 13:61–74
Grant KA, McMahon C, Austin MP (2008) Maternal anxiety during the transition to parenthood: a prospective study. J Affect Disord 108:101–111
Harris B, Huckle P, Thomas R, Johns S, Fung H (1989) The use of rating scales to identify post-natal depression. Br J Psychiatry 154:813–817
Heron J, O'Connor TG, Evans J, Golding J, Glover V (2004) The course of anxiety and depression through pregnancy and the postpartum in a community sample. J Affect Disord 80:65–73
Huizink AC, Mulder EJH, Robles de Medina PG, Visser GHA, Buitelaar JK (2004) Is pregnancy anxiety a distinctive syndrome? Early Hum Dev 79:81–91
Ibanez G, Charles M, Forhan A, Magnin G, Thiebaugeorges O, Kaminski M, Saurel-Cubizolles M (2012) Depression and anxiety in women during pregnancy and neonatal outcome: data from the EDEN mother–child cohort. Early Hum Dev 88:643–649
Johnson RC, Slade P (2003) Obstetric complications and anxiety during pregnancy: is there a relationship? Psychosom Obstet Gynaecol 24:1–14
Joyce A, Hutchinson M (2012) Western Australia’s Mothers and Babies 2010: Twenty-eighth Annual Report of the Western Australian Midwives’ Notification System. Department of Health, Western Australia
Kincaid J P, Fishburne R P, Rogers R L, Chissom B S (1975) Derivation of New Readability Formulas (Automated Readability Index, Fog Count, and Flesch Reading Ease formula) for Navy Enlisted Personnel. Research Branch Report 8–75. Chief of Naval Technical Training, Naval Air Station Memphis
Lamers F, van Oppen P, Comijs HC, Smit JH, Spinhoven P, van Balkom AJ et al (2011) Comorbidity patterns of anxiety and depressive disorders in a large cohort study: the Netherlands Study of Depression and Anxiety (NESDA). J Clin Psychol 72:341–348
Levin JS (1991) The factor structure of the pregnancy anxiety scale. J Health Soc Behav 32:368–381
Lovibond PF, Lovibond SH (1995) The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav Res Ther 33:335–343
Matthey S (2008) Using the Edinburgh Postnatal Depression Scale to screen for anxiety disorders. Depression Anxiety 25:926–931
Matthey S, Fisher J, Rowe H (2013) Using the Edinburgh postnatal depression scale to screen for anxiety disorders: conceptual and methodological considerations. J Affect Disord 146:224–230
Matthey S, Barnett B, Howie P, Kavanagh DJ (2003) Diagnosing postpartum depression in mothers and fathers: whatever happened to anxiety? J Affect Disord 74:139–147
Meades R, Ayers S (2011) Anxiety measures validated in perinatal populations: a systematic review. J Affect Disord 133:1–15
Milgrom J, Gemmill AW, Bilszta JL, Hayes B, Barnett B, Brooks J et al (2008) Antenatal risk factors for postnatal depression: a large prospective study. J Affect Disord 108:147–157
Moss KM, Skouteris H, Wertheim EH, Paxton SJ, Milgrom J (2009) Depressive and anxiety symptoms through late pregnancy and the first year post birth: an examination of prospective relationships. Arch Wom Ment Health 12:345–349
Murray D, Cox JL (1990) Screening for depression during pregnancy with the Edinburgh Depression Scale (EDDS). J Reprod Infant Psychol 8:99–107
Muzik M, Klier CM, Rosenblum KL, Holzinger A, Umek W, Katschnig H (2000) Are commonly used self-report inventories suitable for screening postpartum depression and anxiety disorders? Acta Psychiatr Scand 102:71–73
O’Connor TG, Heron J, Golding J, Beveridge M, Glover V (2002) Maternal antenatal anxiety and children’s behavioural/emotional problems at 4 years. Br J Psychiatry 180:502–508
O’Hara MW, Stuart S, Watson D, Dietz PM, Farr SL, D’Angelo D (2012) Brief scales to detect postpartum depression and anxiety symptoms. J Wom Health 21:1237–1243
Osman A, Wong JL, Bagge CL, Freedenthal S, Gutierrez PM, Lozano G (2012) The Depression Anxiety Stress Scales-21 (DASS21): further examination of dimensions, scale reliability, and correlates. J Clin Psychol 68:1322–1338
Phillips J, Sharpe L, Matthey S (2007) Rates of depressive and anxiety disorders in a residential mother–infant unit for unsettled infants. Aust N Z J Psychiatry 41:836–842
Phillips J, Sharpe L, Matthey S, Charles M (2009) Maternally focused worry. Arch Wom Ment Health 12:409–418
Ross LE, Gilbert Evans SE, Sellers EM, Romach MK (2003) Measurement issues in postpartum depression part 1: anxiety as a feature of postpartum depression. Arch Wom Ment Health 6:51–57
Ross LE, McLean LM (2006) Anxiety disorders during pregnancy and the postpartum period: a systematic review. J Clin Psychiatry 67:1285–1298
Rowe H, Fisher J, Loh W (2008) The Edinburgh Postnatal Depression Scale detects but does not distinguish anxiety disorders from depression in mothers of infants. Arch Wom Ment Health 11:103–108
Spielberger CD, Gorsuch R, Lushene R, Vagg P, Jacobs G (1983) Manual for the State-Trait Anxiety Inventory. Consulting Psychologists, Palo Alto
Stein A, Craske MG, Lehtonen A, Harvey A, Savage-McGlynn E, Davies B et al (2012) Maternal cognitions and mother-infant interaction in postnatal depression and generalized anxiety disorder. J Abnorm Psychol 121:795–809
Stevenson-Hinde J, Shouldice A, Chicot R (2011) Maternal anxiety, behavioral inhibition, and attachment. Attach Hum Dev 13:199–215
Sutter-Dallay A, Giaconne-Marcesche V, Glatigny-Dallay E, Verdoux H (2004) Women with anxiety disorders during pregnancy are at increased risk of intense postnatal depressive symptoms: a prospective survey of the MATQUID cohort. Eur Psychiatry 19:459
Swallow BL, Lindow S, Masson E, Hay D (2003) The use of the General Health Questionnaire (GHQ-28) to estimate prevalence of psychiatric disorder in early pregnancy. Psychol Health Med 8:213–217
Van den Bergh B (1989) De emotionele toestand van de (zwangere) vrouw, obstetrische complicaties en het gedrag en de ontwikkeling van de foetus en van het kind tot de leeftijd van zeven maanden [The emotional state of the (pregnant) woman, obstetrical complications and the behavior and development of fetus and child until seven months after birth] (PhD) Catholic University Leuven, Leuven
Velicer WF, Eaton CA, Fava JL (2000) Construct explication through factor or component analysis: a review and evaluation of alternative procedures for determining the number of factors or components. In: Goffin RD, Helmes E (eds) Problems and solutions in human assessment: honoring Douglas N Jackson at seventy. Kluwer, Boston
Wadhwa PD, Sandman CA, Porto M, Dunkel-Schetter C, Garite TJ (1993) The emotional state of the (pregnant) woman, obstetrical complications and the behavior and development of fetus and child until seven months after birth. Am J Obstet Gynecol 169:858
Zambaldi CF, Cantilino A, Farias JA, Moraes GP, Botelho Sougey E (2011) Dissociative experience during childbirth. J Psychosom Obstet Gynecol 32:204–209
Zigmond AS, Snaith R (1983) The Hospital Anxiety and Depression Scale. Acta Psychiatry Scand 67:361–370
Acknowledgments
The authors wish to thank the women who participated in this research. The authors would also like to thank the late Associate Prof. Jon Rampono, Dr. Jane Fisher, Dr. Janette Brooks, Nadia Cunningham, Maree Brice-Pozzi and the admissions and nursing staff at the Mother and Baby Unit for their input and support. We are grateful to Channel 7 Telethon for funding this project and the Women and Infants Research Foundation for providing research support.
Author information
Authors and Affiliations
Corresponding author
Additional information
The PASS is copyrighted to the Western Australian Department of Health and is available via inquiry at PsychologicalMedicinePASS.WNHSWHCCU@health.wa.gov.au
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 238 kb)
Rights and permissions
About this article
Cite this article
Somerville, S., Dedman, K., Hagan, R. et al. The Perinatal Anxiety Screening Scale: development and preliminary validation. Arch Womens Ment Health 17, 443–454 (2014). https://doi.org/10.1007/s00737-014-0425-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00737-014-0425-8