Abstract
Levodopa-induced dyskinesias (LID) in Parkinson’s disease (PD) are frequent complications, and the endocannabinoid system has a role on its pathophysiology. To test the hypothesis that the functioning of the endocannabinoid system would be altered in PD and in LID by measuring plasma and CSF levels of α-N-arachidonoylethanolamine (AEA) and 2-arachidonoyl-glycerol (2-AG) in patients with PD with and without LID and in healthy controls. Blood and CSF samples were collected from 20 healthy controls, 23 patients with PD without LID, and 24 patients with PD with LID. The levels of AEA and 2-AG were measured using a highly sensitive column switching ultrahigh-performance liquid chromatography–tandem mass spectrometry method. When pooled together, patients with PD had lower plasma and CSF levels of 2-AG and higher CSF levels of AEA compared to healthy controls (Mann–Whitney statistics = 303.0, p = 0.02). Patients with PD without LID had lower CSF levels of 2-AG (Kruskal–Wallis statistics = 7.76, p = 0.02) and higher CSF levels of AEA levels than healthy controls (Kruskal–Wallis statistics = 8.81, p = 0.01). The findings suggest that the endocannabinoid system participates in the pathophysiology of PD symptoms, but its role in the pathophysiology of LID is still unclear.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a neurodegenerative condition, and after few years of levodopa therapy, motor complications occur, including motor fluctuations and levodopa-induced dyskinesias (LID) (Poewe et al. 2017). LID have a major impact in the quality of life of patients, especially in the intermediate phase of the disease (Perez-Lloret et al. 2017). LID pathophysiology is not completely understood but is believed to involve the endocannabinoid system (ECS) (Espay et al. 2018; Chaudhuri et al. 2018; Cenci et al. 2020).
The ECS seems to play an important role in the modulation of the basal ganglia (Mechoulam and Parker 2013), mainly through interaction with the dopaminergic transmission based on control of neuronal activity and terminal dopamine release (Covey et al. 2017; Ferreira-Junior et al. 2020). Anandamide (α-N-arachidonoylethanolamine—AEA) and 2-arachidonoyl-glycerol (2-AG) are the two main neurotransmitters of the ECS, which has two known specific receptors named cannabinoid receptors type 1 (CB1R) and type 2 (CB2R) (Mechoulam and Parker 2013; Garcia et al. 2016; Baggelaar et al. 2018). There are evidences of the role of the ECS in PD and in LID (van der Stelt et al. 2005; Wang et al. 2014, 2018; Sierra et al. 2015; Rojo-Bustamante et al. 2018), with increased ECS activity and increased density of CB1R in the basal ganglia of dopamine deficiency animal models of PD, which can be reversed by dopaminergic therapy (Di Marzo et al. 2000; Maccarrone et al. 2003; Pisani et al. 2005; Giuffrida and McMahon 2010). Findings also show that LID are associated with adaptive changes in the functioning of the ECS (Ferrer et al. 2003; van der Stelt et al. 2005; Dos-Santos-Pereira et al. 2016).
Furthermore, few clinical studies reported elevated levels of AEA in the CSF of untreated patients with PD, but no studies have evaluated endocannabinoid levels and their association with LID onset (Pisani et al. 2005, 2010). In this study, we tested the hypothesis that the functioning of the ECS would be altered in PD and in LID by measuring plasma and CSF levels of AEA and 2-AG in patients with PD and healthy controls.
Materials and methods
Study design and participants
We conducted an observational cross-sectional study to analyze 2-AG and AEA levels in the plasma and CSF of patients with PD with and without LID and in healthy controls. Patients with PD were recruited from the Movement Disorders Unit of Ribeirão Preto Medical School, Brazil, between October 2015 and May 2017. All patients were diagnosed with PD according to the UK PD Society Brain Bank diagnostic criteria (Hughes et al. 1993). We invited healthy controls to participate between the companions and caregivers of patients who attended the same hospital. Patients and healthy controls were consecutively invited to participate in the study according to the convenience of using a 1:1 ratio matching for sex and age at evaluation within four years. Patients with PD with and without LID were also stratified per age at evaluation and sex. Our goal was to include at least 20 individuals in each group. We defined the presence of LID by a score ≥ 1 in item 4.1 (time spent with dyskinesias) of the International Parkinson and Movement Disorders Society—Unified Parkinson’s Disease Rating Scale (MDS-UPDRS), in addition to clinical confirmation of the presence of LID in the ON-state (Goetz et al. 2008a, b). Only patients in treatment with levodopa were included.
We excluded participants if they had (1) acute or chronic infections, severe systemic conditions, autoimmune disorders or other neurological diseases; (2) kidney or chronic liver diseases or regular alcohol intake (over 80 g/day for 6 months); and (3) healthy controls if they had neurological or psychiatric disorders. Additionally, we excluded patients with PD if they had (1) dementia according to MDS diagnostic criteria (Emre et al. 2007); or (2) mild psychosis defined as a score > 1 on item 1.2 of the MDS-UPDRS Part I (hallucinations and psychosis).
For the analyses, participants were divided into three groups: healthy controls (HC), patients with PD without LID (PD-ND) and patients with PD with LID (PD-D). The study was approved by institutional review board of the Ribeirão Preto Medical School (Number 3.036.243), and each participant provided written informed consent to participate.
Evaluations
All patients with PD were evaluated by the same movement disorders specialist (B.L.S.L.) using a standardized assessment comprising clinical and epidemiological data, including a definition of levodopa therapy duration and levodopa equivalent daily doses (LEDD), the Hoehn and Yahr stage, the MDS-UPDRS, and the Unified Dyskinesia Rating Scale (UDysRS) (Hoehn and Yahr 1967; Goetz et al. 2008a, b; Tomlinson et al. 2010). All patients were evaluated in the ON-state. For the UDysRS, we analyzed Part 1B (effect of LID on usual activities described by patients), Part 3 (intensity of LID in seven regions of patient’s body during each of four observed tasks—communication, drinking, dressing and ambulation) and Part 4 (global disability caused by LID during each of these four observed tasks), historical subscore, objective subscore and total UDysRS score. The evaluation sessions of patients with PD with LID were recorded on video for later scoring of the UDysRS objective score.
Collection, processing and storage of biologic samples
For each participant, we collected peripheral blood and CSF on the same day, between 08:00 and 10:00 AM, without fasting. The samples were placed on ice immediately after collection. All patients were instructed to take their regular morning dose of dopaminergic drugs.
Peripheral blood was collected into Vacutainer tubes (BD Diagnostics, Plymouth, UK) with anticoagulant (EDTA) by venipuncture, and whole blood was centrifuged at 4 °C and 1600 g for 15 min. Supernatant plasma samples were aliquoted into 1-mL cryotubes, coded, and stored at − 80 °C until analysis.
CSF was collected through lumbar puncture immediately after the collection of peripheral blood in the lateral recumbent position, using a traumatic Quincke (0.7 mm × 63 mm) needle at the L3/L4 or L4/L5 level. We separated 1–2 mL of CSF for routine analysis (cell counts, glucose, proteins). All remaining CSF (10–12 mL) was collected in polypropylene tubes and gently mixed to avoid gradient effects, centrifuged at 4 °C at 4000g for 10 min to remove cells, aliquoted into 1-mL cryotubes, coded, and stored at − 80 °C until use without preservatives added. CSF samples contaminated with blood (CSF red cells > 500 per mm3) were excluded.
Lipid extraction and UHPLC–MS/MS conditions
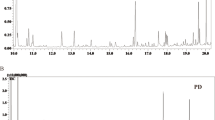
For lipid extraction, CSF was mixed with acetone (2:1, v/v) in the presence of AEA-d4 and 2-AG-d5 as internal standards. The supernatant was mixed with toluene for liquid–liquid extraction and the organic phase was dried and analyzed (Marchioni et al. 2017, 2018). This procedure was based on the method described previously (Leweke et al. 2007). For plasma samples, the procedure was a simple precipitation of proteins with acetonitrile, as described elsewhere (Marchioni et al. 2017).
UHPLC–MS/MS analysis was performed with a two-dimensional Waters® UHPLC–MS/MS system (Waters Corporation, Milford, MA, USA) coupled with a Xevo® TQ-D triple-quadrupole operating in positive electrospray ionization (ESI +) mode with multiple reaction monitoring (MRM). Plasma samples (100 µL) were injected into a first RP-8 ADS column (25 mm × 4 mm × 25 μm) and then into a Kinetex C18 core–shell column (100 mm × 2.1 mm × 1.7 μm) in the second dimension (Marchioni et al. 2017). RP-8 ADS was used for enrichment with traces of endocannabinoids and macromolecular matrix size exclusion, while the core–shell column was used for chromatographic separation. The prepared CSF samples (10 µL) were injected directed into the second column (Kinetex C18 core–shell) (Marchioni et al. 2017).
Statistical analysis
To compare clinical and epidemiological data between groups, we performed the Mann–Whitney and Kruskal–Wallis tests followed by Dunn’s test for multiple comparisons for continuous variables, and the chi-square test for categorical variables. To compare the levels of endocannabinoids between groups, we used the Mann–Whitney and Kruskal–Wallis tests followed by Dunn’s test for multiple comparisons. To compare two continuous variables, we performed Spearman’s Rho correlation test. All analyses were performed using SPSS for Windows version 23.0 (SPSS Inc., Chicago, USA) and figures were created using GraphPrism for Windows version 5.0 (GraphPad Software Inc., La Jolla, USA).
Results
Clinical and demographic data
Sixty-seven participants fulfilled the inclusion and exclusion criteria. We were unable to collect CSF from four patients with PD (one with LID and three without LID) due to technical problems during the lumbar puncture. The clinical and demographic data of participants are summarized in Table 1.
Men predominated in the PD-ND (62.5%) and PD-D (78.3%) groups, and women in the HC group (70%). There were no significant age differences across groups. Patients with PD with LID had an earlier onset of disease, longer disease duration, longer levodopa therapy, and higher LEDD intake compared to patients with PD with LID patients (Table 2) .
Plasma and CSF AEA and 2-AG levels
The endocannabinoid levels of 2-AG and AEA in the plasma and CSF samples of patients with PD and healthy controls are presented in Fig. 1.
Endocannabinoid plasma and CSF levels in patients with Parkinson’s disease and healthy controls. A: Plasma 2-AG in HC and all patients with PD; B: CSF 2-AG in HC and all patients with PD; C: Plasma AEA in HC and all patients with PD; D: CSF AEA in HC and all patients with PD; E: CSF 2-AG in HC, PD-ND and PD; F: CSF AEA in HC, PD-ND and PD; G: Plasma 2-AG in HC, PD-ND and PD; H: Plasma AEA in HC, PD-ND and PD. 2-AG 2-arachidonoyl-glycerol, AEA anandamide, HC healthy controls, PD-D Patients with PD with levodopa-induced dyskinesias, PD-ND Patients with PD without levodopa-induced dyskinesias
The comparative analysis of the groups of patients with PD and HC showed that patients with PD had lower plasma and CSF levels of 2-AG (plasma: Mann–Whitney statistics = 303.0, p = 0.02; CSF: Mann–Whitney statistics = 286.0, p = 0.03) (Fig. 1a, b), and higher CSF levels of AEA than HC (plasma: Mann–Whitney statistics = 460.5, p = 0.9; CSF: Mann–Whitney statistics = 234.0, p = 0.003) (Fig. 1c, d).
The comparative analysis considering the presence of LID showed that patients of the PD-ND group had lower CSF levels of 2-AG and higher CSF levels of AEA than HC (2-AG: Kruskal–Wallis statistics = 7.76, p = 0.02, difference in rank sum = − 15.95, p < 0.05; AEA: Kruskal–Wallis statistics = 8.81, p = 0.01, difference in rank sum = 16.35, p < 0.05) (Fig. 1e, f). There were no differences between groups in the plasma levels of endocannabinoids (2-AG: Kruskal–Wallis statistics = 5.24, p = 0.07; AEA: Kruskal–Wallis statistics = 2.16, p = 0.33) (Fig. 1g, h).
Correlations between endocannabinoid levels and clinical variables
With respect to endocannabinoid levels in the CSF, body weight was associated with AEA levels (Spearman’s ρ = − 0.41, p = 0.006, n = 43) and MDS-UPDRS Part 1 score was associated with AEA and 2-AG and AEA levels (2-AG: Spearman’s ρ = 0.35, p = 0.02, n = 43; AEA: Spearman’s ρ = − 0.34, p = 0.02, n = 43). Regarding plasma, advanced Hoehn & Yahr stages were associated with lower AEA levels (Spearman’s ρ = − 0.36, p = 0.01, n = 47), but increased time spent with dyskinesias (item 4.1 of the MDS-UPDRS) in PD patients with LID was associated with higher AEA levels (Spearman’s ρ = 0.45, p = 0.02, n = 24).
There were no correlations between the levels of endocannabinoids in plasma or CSF and age at onset of PD, disease duration, levodopa therapy duration and dose at evaluation, LEDD, and MDS-UPDRS total and sub-item scores, initial motor symptoms, and clinical motor phenotype. Also, there were no correlations between endocannabinoid levels and UDysRS scores.
When patients and controls were pooled together, we found no correlations between plasma levels of AEA and 2-AG (Spearman’s ρ = 0.156, p = 0.206, n = 67), but CSF levels of AEA and 2-AG tend to be in opposite directions (Spearman’s ρ = − 0.221, p = 0.08, n = 63). Plasma and CSF levels of 2-AG had inverse patterns in their levels (Spearman’s ρ = − 0.295, p = 0.01, n = 63).
Longer intervals between sample collection and freezing were associated with higher plasma 2-AG levels (Spearman’s ρ = 0.46, p = < 0.001, n = 61) (Fig. 2a), longer plasma storage times were associated with lower plasma AEA levels (Spearman’s ρ = -0.52, p = < 0.001, n = 67), and longer CSF storage times were associated with higher CSF 2-AG levels (Spearman’s ρ = 0.33, p = 0.007, n = 63) (Fig. 2b). Covariance analyses did not show a significant effect of these variables on the measurements of endocannabinoid levels in the three groups. There was no correlation between CSF 2-AG and AEA levels and cell counts, proteins, glucose, and chloride levels in CSF.
Discussion
In our study, we found elevated CSF levels of AEA and decreased CSF and plasma levels of 2-AG in patients with PD, in comparison to healthy controls. These CSF alterations in endocannabinoid levels were observed only in patients with PD without LID, but not in those with LID.
There are few clinical studies on CSF AEA levels in patients with PD. The first study reported higher levels of AEA in the CSF of patients with PD compared to healthy controls (Pisani et al. 2010). Later, the same group demonstrated that CSF levels of AEA were elevated in patients with PD without dopaminergic therapy, and that chronic dopaminergic replacement restored CSF levels of AEA to normal levels (Ferrer et al. 2003). The authors suggested that elevated CSF AEA levels would be part of the compensatory mechanisms induced by striatal dopaminergic loss, and that treatment with dopaminergic drugs would restore AEA levels to normal (Ferrer et al. 2003; Pisani et al. 2010, 2011). No previous studies analyzed 2-AG CSF levels in patients with PD. Our findings are consonant with these original observations showing increased CSF AEA levels in patients with PD, but additionally revealed that 2-AG levels are reduced in the CSF of these patients. This shows that the CSF levels of the two major endocannabinoids follow an inverse relationship in patients with PD.
Many experimental observations suggested that the functioning of the ECS is altered in PD. Preliminary studies reported alterations in endocannabinoid levels in the basal ganglia in animal models of PD. There were increased levels of endocannabinoids in basal ganglia of rats treated with reserpine, but especially noted a sevenfold elevation in the levels of 2-AG in the globus pallidus. They suggested that, in the parkinsonian state, increased levels of 2-AG in the globus pallidus would be a consequence of increased activity in the indirect pathway (Di Marzo et al. 2000). Posteriorly, two studies described increased levels of AEA in the striatum of 6-OHDA-lesioned rats, but not of 2-AG (Gubellini et al. 2002; Maccarrone et al. 2003), and in non-human primates, elevated levels of AEA and 2-AG in the basal ganglia of MPTP-lesioned primates were described (van der Stelt et al. 2005). A recent study also supported the increase of AEA in untreated parkinsonian animals based on alteration of AEA synthesizing/degrading enzymes in external globus pallidus (Rojo-Bustamante et al. 2018). In these studies, treatment with dopaminergic drugs promoted a significant reduction in the levels of endocannabinoids in these basal ganglia (Di Marzo et al. 2000; Maccarrone et al. 2003). These observations suggest that changes in the ECS might result from the development of compensatory modifications induced by a reduction in striatal dopamine levels, which would be characterized by increases in the levels of endocannabinoids in the basal ganglia. The findings available also indicate that dopamine play a modulatory role in the ECS activity and that dopaminergic therapy in PD would restore the normal functioning of this system and reduce the abnormally elevated endocannabinoid levels (Di Marzo et al. 2000; Maccarrone et al. 2003).
However, other experimental studies suggested that changes in ECS function in the basal ganglia following dopaminergic striatal denervation seem to be more complex. One study using an MPTP mouse model of PD showed that, following MPTP administration, the levels of 2-AG in the ventral midbrain increased significantly for two days after administration; however, these levels were almost back to control levels seven days after treatment. On the other hand, there was a slow decline in the level of 2-AG in the striatum, reaching significantly lower values at seven days until 21 days after treatment with MPTP (Mounsey et al. 2015). In another study using unilaterally 6-OHDA-lesioned rats, AEA levels reduced considerably in the caudate-putamen ipsilateral to the lesion; however, neither acute nor chronic levodopa treatment affected the levels of endocannabinoids in these animals (Ferrer et al. 2003).
Regarding the preclinical data of role of the ECS in LID, the current evidences are not clear yet. On the measurement of endocannabinoids in basal ganglia, parkinsonian primates with dyskinesias in chronic levodopa therapy did not show distinct levels in AEA and 2-AG in the basal ganglia compared to parkinsonian animals not using levodopa or parkinsonian animals in acute levodopa therapy (van der Stelt et al. 2005), but recent studies explored the expression of genes and metabolites in the striatum of 6-OHDA-lesioned rats and found a dysregulation in the retrograde endocannabinoid pathway in rats with LID (Wang et al. 2014, 2018). On the evaluation of cannabinoid receptors in basal ganglia, new data showed a decreased expression of CB1R and CB2R in the pallidothalamic neurons in LID animals (Sierra et al., 2015), and for CB1R, the dyskinetic state seems to modulate its expression: CB1R mRNA is downregulated in the basal ganglia of LID animals but not exhibiting acute dyskinesias (OFF state), and is upregulated during the active phase of LID (ON-state) (Rojo-Bustamante et al., 2018).
Our findings agree with studies that reported increased levels of AEA in the CSF/brain of patients with PD and animal models of PD (Gubellini et al. 2002; Maccarrone et al. 2003; van der Stelt et al. 2005; Pisani et al. 2010; Rojo-Bustamante et al. 2018), and with experimental studies that reported altered levels of 2-AG (Di Marzo et al. 2000; Mounsey et al. 2015). We found increased CSF AEA levels in PD patients using dopaminergic therapy. As dopaminergic treatment has been reported to reduce CSF AEA levels back to normal, we expected that endocannabinoid levels were influenced by the intake of dopaminergic drugs in our study. Unfortunately, we could not explore this association, as a drug-näive group of patients with PD was not included, as our aim was to verify changes in the ECS associated with the development of LID. Therefore, we cannot rule out the possibility that endocannabinoid levels could be different if patients were not on dopaminergic drug therapy. Also, fasting can increase the plasma AEA (Piccolo et al. 2020), but as all participants were instructed to eat as usual before sample collection, we believe it would not interfere with our results.
The reasons for the differences observed in the endocannabinoid levels of our patients with and without LID are unclear. PD-D group presented higher LEDD intake and longer levodopa therapy than PD-ND group; however, we found no significant correlations between endocannabinoid levels and LEDD intake and duration of levodopa therapy. Based on these findings, we are unable to conclude whether endocannabinoid levels vary according to the dose and duration of dopaminergic therapy.
Another interesting finding was that changes in AEA and 2-AG levels in the CSF of patients with PD tend to take opposite directions. There is evidence that AEA inhibits the metabolism and physiological actions of 2-AG in the striatum, which could explain these findings (Morgese et al. 2007; Maccarrone et al. 2008). However, we found no significant correlations between AEA and 2-AG levels in the CSF as could be expected based on this hypothesis.
With respect to plasma, we found no significant alterations in the levels of endocannabinoids across groups, and there were no essential correlations between plasma and CSF endocannabinoid levels; therefore, it is possible to assume that the change in plasma endocannabinoid levels was presumably of central origin.
Our findings support the hypothesis that the physiology of the ECS is altered in PD. However, the association between the human plasma and CSF endocannabinoid levels and LID in PD is still unclear. The role of the ECS in the pathophysiology of LID seems to be complex, since endocannabinoids act in retrograde signaling in many circuits of the basal ganglia and could modulate different neurotransmitter systems as glutamate, adenosine, but especially dopamine transmission (Kano 2014).
Our study has limitations, among which we highlight the low sample size and the absence of a drug-näive group of patients with PD, which would allow us to investigate variations in the endocannabinoid levels of untreated patients. Together, these findings suggest that the endocannabinoid system participates in the pathophysiology of PD symptoms, but its role in the pathophysiology of LID is still unclear.
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Baggelaar MP, Maccarrone M, van der Stelt M (2018) 2-Arachidonoylglycerol: a signaling lipid with manifold actions in the brain. Prog Lipid Res 71:1–17
Cenci MA, Riggare S, Pahwa R, Eidelberg D, Hauser RA (2020) Dyskinesia matters. Mov Disord 35:392–396
Covey D, Mateo Y, Sulzer D, Cheer JF, Lovinger DM (2017) Endocannabinoid modulation of dopamine neurotransmission. Neuropharmacology 124:52–61
Di Marzo V, Hill MP, Bisogno T, Crossman AR, Brotchie JM (2000) Enhanced levels of endogenous cannabinoids in the globus pallidus are associated with a reduction in movement in an animal model of Parkinson's disease. FASEB J 14:1432–1438
Dos-Santos-Pereira M, da-Silva CA, Guimaraes FS, Del-Bel E (2016) Co-administration of cannabidiol and capsazepine reduces L-DOPA-induced dyskinesia in mice: possible mechanism of action. Neurobiol Dis 94:179-195
Emre M, Aarsland D, Brown R, Burn DJ, Duyckaerts C, Mizuno Y, Broe GA, Cummings J, Dickson DW, Gauthier S, Goldman J, Goetz C, Korczyn A, Lees A, Levy R, Litvan I, McKeith I, Olanow W, Poewe W, Quinn N, Sampaio C, Tolosa E, Dubois B (2007) Clinical diagnostic criteria for dementia associated with Parkinson's disease. Mov Disord 22:1689–1707
Espay AJ, Morgante F, Merola A, Fasano A, Marsili L, Fox SH, Bezard E, Picconi B, Calabresi P, Lang AE (2018) Levodopa-induced dyskinesia in Parkinson disease: Current and evolving concepts. Ann Neurol 84:797–811
Ferreira Junior NC, Dos-Santos-Pereira M, Guimarães FS, Del Bel E (2020) Cannabidiol and cannabinoid compounds as potential strategies for treating Parkinson's disease and L-DOPA-induced dyskinesia. Neurotox Res 37:12–29
Ferrer B, Asbrock N, Kathuria S, Piomelli D, Giuffrida A (2003) Effects of levodopa on endocannabinoid levels in rat basal ganglia: implications for the treatment of levodopa-induced dyskinesias. Eur J Neurosci 18:1607–1614
Garcia C, Palomo-Garo C, Gomez-Galvez Y, Fernandez-Ruiz J (2016) Cannabinoid-dopamine interactions in the physiology and physiopathology of the basal ganglia. Br J Pharmacol 173:2069–2079
Giuffrida A, McMahon LR (2010) In vivo pharmacology of endocannabinoids and their metabolic inhibitors: therapeutic implications in Parkinson's disease and abuse liability. Prostaglandins Other Lipid Mediat 91:90–103
Goetz CG, Tilley BC, Shaftman SR, Stebbins GT, Fahn S, Martinez-Martin P, Poewe W, Sampaio C, Stern MB, Dodel R, Dubois B, Holloway R, Jankovic J, Kulisevsky J, Lang AE, Lees A, Leurgans S, LeWitt PA, Nyenhuis D, Olanow CW, Rascol O, Schrag A, Teresi JA, van Hilten JJ, LaPelle N (2008a) Movement Disorder Society-sponsored revision of the Unified Parkinson's Disease Rating Scale (MDS-UPDRS): scale presentation and clinimetric testing results. Mov Disord 23:2129–2170
Goetz CG, Nutt JG, Stebbins GT (2008b) The Unified Dyskinesia Rating Scale: presentation and clinimetric profile. Mov Disord 23:2398–2403
Gubellini P, Picconi B, Bari M, Battista N, Calabresi P, Centonze D, Bernardi G, Finazzi-Agrò A, Maccarrone M (2002) Experimental parkinsonism alters endocannabinoid degradation: implications for striatal glutamatergic transmission. J Neurosci 22:6900–6907
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression, and mortality. Neurology 17:427–442
Hughes AJ, Daniel SE, Blankson S, Lees AJ (1993) A clinicopathologic study of 100 cases of Parkinson's disease. Arch Neurol 50:140–148
Kano M (2014) Control of synaptic function by endocannabinoid-mediated retrograde signaling. Proc Jpn Acad Ser B Phys Biol Sci 90:235–250
Leweke FM, Giuffrida A, Koethe D, Schreiber D, Nolden BM, Kranaster L, Neatby MA, Schneider M, Gerth CW, Hellmich M, Klosterkötter J, Piomelli D (2007) Anandamide levels in cerebrospinal fluid of first-episode schizophrenic patients: impact of cannabis use. Schizophr Res 94:29–36
Maccarrone M, Gubellini P, Bari M, Picconi B, Battista N, Centonze D, Bernardi G, Finazzi-Agrò A, Calabresi P (2003) Levodopa treatment reverses endocannabinoid system abnormalities in experimental parkinsonism. J Neurochem 85:1018–1025
Maccarrone M, Rossi S, Bari M, De Chiara V, Fezza F, Musella A, Gasperi V, Prosperetti C, Bernardi G, Finazzi-Agrò A, Cravatt BF, Centonze D (2008) Anandamide inhibits metabolism and physiological actions of 2-arachidonoylglycerol in the striatum. Nat Neurosci 11:152–159
Marchioni C, de Souza ID, Grecco CF, Crippa JA, Tumas V, Queiroz MEC (2017) A column switching ultrahigh-performance liquid chromatography-tandem mass spectrometry method to determine anandamide and 2-arachidonoylglycerol in plasma samples. Anal Bioanal Chem 409:3587–3596
Marchioni C, de Souza ID, Acquaro VRJ, de Souza Crippa JA, Tumas V, Queiroz MEC (2018) Recent advances in LC-MS/MS methods to determine endocannabinoids in biological samples: Application in neurodegenerative diseases. Anal Chim Acta 1044:12–28
Mechoulam R, Parker LA (2013) The endocannabinoid system and the brain. Annu Rev Psychol 64:21–47
Morgese MG, Cassano T, Cuomo V, Giuffrida A (2007) Anti-dyskinetic effects of cannabinoids in a rat model of Parkinson's disease: role of CB(1) and TRPV1 receptors. Exp Neurol 208:110–119
Mounsey RB, Mustafa S, Robinson L, Ross RA, Riedel G, Pertwee RG, Teismann P (2015) Increasing levels of the endocannabinoid 2-AG is neuroprotective in the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine mouse model of Parkinson's disease. Exp Neurol 273:36–44
Perez-Lloret S, Negre-Pages L, Damier P, Delval A, Derkinderen P, Destée A, Meissner WG, Tison F, Rascol O (2017) L-DOPA-induced dyskinesias, motor fluctuations and health-related quality of life: the COPARK survey. Eur J Neurol 24:1532–1538
Piccolo M, Claussen MC, Bluemel S, Schumacher S, Cronin A, Fried A, Goetze O, Martin-Soelch C, Milos G (2020) Altered circulating endocannabinoids in anorexia nervosa during acute and weight-restored phases: a pilot study. Eur Eat Disorders Rev 28:46–54
Pisani A, Fezza F, Galati S, Battista N, Napolitano S, Finazzi-Agrò A, Bernardi G, Brusa L, Pierantozzi M, Stanzione P, Maccarrone M (2005) High endogenous cannabinoid levels in the cerebrospinal fluid of untreated Parkinson's disease patients. Ann Neurol 57:777–779
Pisani V, Moschella V, Bari M, Fezza F, Galati S, Bernardi G, Stanzione P, Pisani A, Maccarrone M (2010) Dynamic changes of anandamide in the cerebrospinal fluid of Parkinson's disease patients. Mov Disord 25:920–924
Pisani V, Madeo G, Tassone A, Sciamanna G, Maccarrone M, Stanzione P, Pisani A (2011) Homeostatic changes of the endocannabinoid system in Parkinson's disease. Mov Disord 26:216–222
Poewe W, Seppi K, Tanner CM, Halliday GM, Brundin P, Volkmann J, Schrag AE, Lang AE (2017) Parkinson disease. Nat Rev Dis Primers 3:17013
Rojo-Bustamante E, Abellanas MA, Clavero P, Thiolat ML, Li Q, Luquin MR, Bezard E, Aymerich MS (2018) The expression of cannabinoid type 1 receptor and 2-arachidonoyl glycerol synthesizing/degrading enzymes is altered in basal ganglia during the active phase of levodopa-induced dyskinesia. Neurobiol Dis 118:64–75
Sierra S, Luquin N, Rico AJ, Gómez-Bautista V, Roda E, Dopeso-Reyes IG, Vázquez A, Martínez-Pinilla E, Labandeira-García JL, Franco R, Lanciego JL (2015) Detection of cannabinoid receptors CB1 and CB2 within basal ganglia output neurons in macaques: changes following experimental parkinsonism. Brain Struct Funct 220:2721–2738
Tomlinson CL, Stowe R, Patel S, Rick C, Gray R, Clarke CE (2010) Systematic review of levodopa dose equivalency reporting in Parkinson's disease. Mov Disord 25:2649–2653
van der Stelt M, Fox SH, Hill M, Crossman AR, Petrosino S, Di Marzo V, Brotchie JM (2005) A role for endocannabinoids in the generation of parkinsonism and levodopa-induced dyskinesia in MPTP-lesioned non-human primate models of Parkinson's disease. FASEB J 19:1140–1142
Wang Y, Zhang QJ, Wang HS, Wang T, Liu J (2014) Genome-wide microarray analysis identifies a potential role for striatal retrograde endocannabinoid signaling in the pathogenesis of experimental L-DOPA-induced dyskinesia. Synapse 68:332–343
Wang Y, Zhang GJ, Sun YN, Yao L, Wang HS, Du CX, Zhang L, Liu J (2018) Identification of metabolite biomarkers for L-DOPA-induced dyskinesia in a rat model of Parkinson's disease by metabolomic technology. Behav Brain Res 347:175–183
Acknowledgements
We would like to thank Ângela Vieira Pimentel, Larissa Serveli, Manuelina Macruz Capelari and Nathália Novaretti (Ribeirão Preto Medical School, University of São Paulo) for technical support.
Funding
This study was supported by the Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP; 159688/2015–9) and Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq; 2012/17626–7).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. In detail: conceptualization: CM, BLS-L, MECQ, VT; methodology: CM, BLS-L, MECQ, VT; clinical data collection: BLS-L, VT; endocannabinoid analysis: CM, MECQ; formal analysis and investigation: CM, BLS-L, MECQ, JASC, VT; writing—original draft preparation: CM, BLS-L; writing—review and editing: CM, BLS-L, MECQ, JASC, VT; funding acquisition: MECQ, VT; supervision: MECQ, VT.
Corresponding author
Ethics declarations
Conflict of interest
Dr. CRIPPA is co-inventor (Mechoulam R, Zuardi AW, Kapczinski F, Hallak JEC, Guimarães FS, Crippa JA, Breuer A) of the patent ‘Fluorinated CBD compounds, compositions and uses thereof. Pub. No.: WO/2014/108,899. International Application No.: PCT/IL2014/050,023′, Def. US no. Reg. 62,193,296; 29/07/2015; INPI on 19/08/2015 (BR1120150164927). The University of São Paulo has licensed the patent to Phytecs Pharm (USP Resolution No. 15.1.130002.1.1). The University of São Paulo has an agreement with Prati-Donaduzzi (Toledo, Brazil) to ‘develop a pharmaceutical product containing synthetic cannabidiol and prove its safety and therapeutic efficacy in the treatment of epilepsy, schizophrenia, Parkinson’s disease, and anxiety disorders’. Dr. CRIPPA has received travel support from BSPG-Pharm and is a medical advisor of SCBD Centre. Dr. CRIPPA has a grant from University Global Partnership Network (UGPN)–Global priorities in cannabinoid research excellence. Dr. CRIPPA is a member of the international advisory board of the Australian Centre for Cannabinoid Clinical and Research Excellence (ACRE), funded by the National Health and Medical Research Council through the Centre of Research Excellence. Dr. CRIPPA is recipient of CNPq 1A productivity fellowship. Dr. TUMAS received honoraria from Teva Brasil, UCB Biopharma and Ipsen, and travel support for medical conferences from Roche.
Ethics approval
The study was approved by institutional review board of the Ribeirão Preto Medical School (Number 3.036.243), and each participant provided written informed consent to participate.
Consent to participate
Authors declare that informed consents for participation were obtained from all participants. Moreover, informed consents for lumbar pucture examination were also obtained from all participants.
Consent for publication
Authors declare that consent for publication of blinded data was a part of informed consents obtained from participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Marchioni, C., Santos-Lobato, B.L., Queiroz, M.E.C. et al. Endocannabinoid levels in patients with Parkinson’s disease with and without levodopa-induced dyskinesias. J Neural Transm 127, 1359–1367 (2020). https://doi.org/10.1007/s00702-020-02240-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-020-02240-9