Abstract
Delirium is a common complication seen after surgery and anesthesia, in particular in older patients. Although the etiology of postoperative delirium is only incompletely understood, various lines of evidence suggest that proinflammatory signaling from the peripheral site of inflammation to central nervous system results in a decrease of cerebral acetylcholine (ACh) levels thereby inducing neuroinflammation. To corroborate this theory, we applied an animal model for characterization of the neuroinflammatory response after partial hepatectomy (HPx). In this model, the surgery-induced decrease in cerebral ACh levels can be prevented by intraoperative application of physostigmine. Thus, ACh-associated changes in the expression and secretion of inflammation-related compounds can be assessed by comparing the results obtained after surgery, in physostigmine-treated and untreated controls. This way we were able to show that the decrease of cerebral ACh triggers increased secretion of IL-1β, IL-6, TNFα, MIP-2 (CCL3), RANTES, MCP1, IFNgamma, and IP-10. A gene array covering the expression of 370 inflammation-related genes indicated 13 candidates that are induced upon cerebral ACh decrease after HPx. Quantification of the changes in the expression of these candidates by the comparative CT method revealed a significant increase (> 1.5-fold) in the expression of IL-1β, IL-6, TNFα, MIP2, RANTES, MCP1, TLR2, TLR4, HMGB1, TNFSF6, TNFSF12, IL1R1 and ILR6. Thus, our results suggest that peripheral surgery induces a reduction of cerebral ACh levels which trigger a complex neuroinflammatory response. From a clinical point of view, manipulating cerebral ACh levels by procholinergic drugs such as physostigmine could become an option to therapeutically target this kind of neuroinflammation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Postoperative delirium (POD) is a form of delirium that manifests in patients who have undergone surgical procedures and anesthesia, usually peaking between 1 and 3 days after their operation (Whitlock et al. 2011). Postoperative delirium (POD) rates vary widely, ranging from 9 to 87% depending on the age of patients and the type of surgery (Maldonado 2008). The etiology of POD is not yet fully understood and is probably multifactorial. However, the brain’s reaction to a peripheral inflammatory process, as induced by surgery, is considered to be a pathophysiological key element (Steiner 2011). Also animal experiments indicate that surgery-induced inflammation rather than anesthesia may be the major cause of POD-associated reactions in the brain (Plaschke et al. 2014, 2016). Since an inflammatory response to intra- or postoperative stress as well as the induction of structural changes in brain vascular cells by anesthetics can affect the permeability of the blood brain barrier, proinflammatory cytokines generated in the periphery may reach the brain, thereby also causing proinflammatory signaling to the central nervous system (CNS) (Acharya et al. 2015; Rudolph et al. 2008). As a result, neuroinflammation with expression of proinflammatory cytokines and inflammatory mediators in the CNS is induced. These neuroinflammatory changes induce neuronal and synaptic dysfunction and subsequent neurobehavioural and cognitive symptoms, which may finally result in the development of delirium (Cerejeira et al. 2010; Cortese and Burger 2017). Peripheral inflammation as well as neuroinflammation is under the control of the vagus nerve-based inflammatory reflex (Pavlov and Tracey 2015). According to this, peripheral inflammation is signaled to the brain via afferent cholinergic vagus signaling to the brain where the afferent signal is integrated with efferent vagus nerve-mediated immunoregulatory output back to the periphery (Chavan et al. 2017). Likewise cholinergic modulation of microglial activation (Shytle et al. 2004) has been shown to attenuate neuroinflammation that was primarily induced by peripheral inflammation (Terrando et al. 2014). Accordingly, reduced cholinergic inhibition of microglia was suggested as a major cause of severe neuroinflammation and resulting delirium (van Gool et al. 2010). In a recent study applying partial hepatectomy (HPx) in rats to investigate the effects of surgery-induced systemic inflammation on cholinergic activity in the CNS, a significant decrease of acetylcholine (ACh) levels in brain was detected in response to surgical stress. Physostigmine, an inhibitor of the acetylcholinesterase (AChE) that easily penetrates the blood–brain barrier, effectively prevented the surgery-induced decrease of ACh levels in the brain (Plaschke et al. 2016). Thus, this appears to be a suitable model to investigate the role of cholinergic signaling in surgery-induced neuroinflammation. In line with this, the model was already successfully applied to show that cholinergic signaling controls the secretion of the inflammation marker IL-1β in the brain after surgery induced stress (Plaschke et al. 2014). However, a detailed analysis of the influence of cholinergic signaling on the cytokine production and secretion pattern in the CNS has not been conducted yet. We, therefore, now applied the HPx animal model for in-depth analysis of the action of altered ACh levels on the expression and secretion of inflammation-related compounds. To this end, we analyzed the effects of HPx with and without concomitant physostigmine treatment on the expression of 370 inflammation-related genes in rat brains and measured the levels of inflammatory cytokines in the rats’ cerebrospinal fluid by multiplex immunoassay.
Methods
Animal experiments
The studies were performed on adult male Wistar-HAN rats (n = 30, JANVIER, Elevage Janvier, Le Genest St. Isle, France) weighing between 190 and 270 g. Rats were housed in a temperature-controlled room at 22 ± 0.5 °C with a reversed day–night cycle (12 h:12 h, light on at 7 p.m.). Free access to food (Altromin, standard no. 1320, Lage, Germany) and water was allowed throughout the experimental period. The experimental protocol was approved by the appropriate review committee of the Medical Faculty of the University of Heidelberg (Germany) and complied with the guidelines of the responsible government agency and with international standards.
All three groups received sevoflurane (3.5 vol% and 30% oxygen/70% N2O) for the experimental period using a rat-adapted mask. Partial liver resection (HPx, n = 10) was performed as described previously (Plaschke et al. 2016). Control rats (n = 10) did not undergo any surgical intervention. Injections of physostigmine (n = 10) or placebo were applied once, at 5 min before the end of the 30-min surgery period to the vena femoralis. Physostigmine (anticholium™, Dr. Franz Köhler Chemie GmbH, Bensheim, Germany) was prepared freshly before application in HPx rats and dissolved in nonpyrogenic sterile saline (0.9% NaCl). The drug was administered slowly intravenously at a dose of 0.04 mg kg−1 body weight (0.01 mg in 240 µl 0.9% sterile NaCl solution saline) under the same conditions of anesthesia as described above. As placebo, a volume-adapted 0.9% sterile NaCl solution was given. At 120 min after physostigmine, rats were anesthetized again using 4 vol% sevoflurane in combination with 30% oxygen and 70% N2O. Cerebrospinal fluid (CSF) (40–90 µl per rat, n = 10) was taken after preparation of the membrane atlantooccipitalis via the suboccipitale puncture of the second cervical vertebra, and was immediately frozen at − 80 °C. For tissue preparation, rats were decapitated. Rats’ brains were rapidly removed and the right and left hemispheres were prepared. Fronto-parietal cortical tissue of n = 3 was separated, frozen on dry ice for 5–10 min, and stored at − 80 °C.
Acetylcholine determination
The concentration of ACh in the CSF supernatant (n = 10) was determined after dilution with a specific reaction buffer to prevent ACh hydrolysis using the Amplex Red Assay kit (Molecular Probes; Invitrogen, Karlsruhe, Germany). The Amplex® Red Acetylcholine/Acetylcholinesterase Assay Kit provides an ultrasensitive method for detecting ACh and also AChE activity in a fluorescence microplate reader or fluorometer. This, the kit detects ACh levels as low as 0.3 µM using excess AChE with a range of detection from 0.3 to 100 µM ACh. In detail, AChE activity is monitored indirectly using 10-acetyl-3,7-dihydroxyphenoxazine (Amplex® Red reagent), a sensitive fluorogenic probe for hydrogen peroxide. AChE converts the ACh substrate to choline, which is then oxidized by choline oxidase to betaine and hydrogen peroxide. In the presence of horseradish peroxidase, hydrogen peroxide reacts with the Amplex® Red reagent in a 1:1 stoichiometric ratio to generate the highly fluorescent product resorufin.
Gene expression array
Total RNA was extracted from the brain cortical tissue samples using the RNeasy Mini Kit (Quiagen, Hilden, Germany) according to the manufacturer’s instructions. RNA yield and purity were assessed using a spectrophotometer. One microgram of total RNA was converted into cDNA using SuperScript™ II reverse transcriptase (Invitrogen, Dreieich, Germany) and oligo dT Primer (Invitrogen) according to the manufacturer’s protocol. Production was controlled by amplifying the transcript of a housekeeping gene (glyceraldehyde-3-phosphate dehydrogenase; GAPDH). cDNA was analyzed by a RT2 Profiler PCR Array (Quiagen, Hilden, Germany) on a ABI StepOnePlus according to the manufacturer’s protocol.
Multiplex immunoassay
The concentrations of cytokines and chemokines in CSF were analyzed by a commercial Luminex immunoassay kit (Cytokine & Chemokine 22-Plex Rat ProcartaPlex™ Panel, Thermo Fisher Scientific, Dreieich, Germany) according to the manufacturer’s instructions.
Statistical analysis
All measurements were performed by an independent investigator blinded to the experimental conditions. Differences within normally distributed data (acetylcholine) were subjected to one-way analysis of variance (ANOVA) using SPSS v22.0 (SPSS IBM, Chicago, USA) followed by post hoc Fisher’s LSD test. Results were considered significant at p ≤ 0.05. Data were presented as mean values + standard deviation (SD).
Results
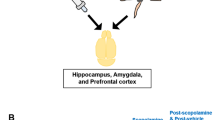
To emulate conditions of a major surgery in an animal model, HPx was performed in Wistar rats and cholinergic signaling in the CNS was manipulated by the blood–brain barrier penetrating AChE inhibitor physostigmine. The whole experimental design of the study is schematically summarized in Fig. 1.
No significant differences between the groups in intraoperative blood gas parameters were determined for the following parameters: pH value, pCO2, pO2, bicarbonate (HCO3−), base excess (BE), hematocrit (Hk), hemoglobin (Hb), potassium (K+), glucose (Glu), and lactate (Lac) concentrations (data not shown). Thus, all these measured parameters were in the physiological range.
Measurement of ACh levels in the CSF obtained from the rats 120 min after surgery indicated a decrease of the neurotransmitter in the CNS in response to HPx. Infusion of a single physostigmine injection at the end of the surgical intervention counteracted this effect (Fig. 2). Since this observation points to an influence of the surgery-induced inflammatory reaction in the periphery on cholinergic signaling in the CNS, we applied this animal model to study the role of cholinergic activities in the induction of a neuroinflammatory response. CSF is a particularly suited matrix to measure neuroinflammation-related secretion of cytokines in the CNS. It freely communicates with the brain interstitial fluid thereby reflecting biochemical changes in the brain. Therefore, we choose this matrix for screening of neuroinflammation-related release in the CNS. Since the amount of CSF that can be taken from a rat is very limited, we applied a multiplex assay procedure to concomitantly measure 22 inflammation-relevant cytokines/chemokines in sample. The list of these analytes is given in supplementary table S1. Nine cytokines were found altered after HPx and eight of these alterations were influenced by manipulating the ACh levels in the brain (Fig. 3). In detail, for IL-1β, IL-6, TNFα, MIP-2 (CCL3), RANTES, MCP1 and IP10, a marked increase was observed which was attenuated by physostigmine. IFNγ was only moderately increased while an exaggerated increase was induced by physostigmine. Also secretion of IL-10 was triggered by HPx, but was not influenced by physostigmine. The other cytokines were not detectable in the CSF (detection limits given in supplementary table S1).
ACh levels in CSF. CSF was sampled 120 min after HPx as shown in Fig. 1. ACh levels (n = 30) were determined the Amplex Red Assay kit. Results are the median (IQR inter quartile range) of ten rats per group ±. HPx partial liver resection, physo physostigmine
Besides the secretion of inflammation-controlling cytokines also changes in the expression of other inflammation-related proteins including cytokine receptors, enzymes of cytokine metabolism, and regulators of cytokine production and inflammation, are an integral feature of the inflammatory response in the brain. To screen for such changes, we applied a gene expression array targeting 380 genes involved in the inflammation process. A list of all screened mRNAs is given in supplementary table S2. Among these, 13 genes were found altered by HPx and their alterations influenced by physostigmine. The comparative CT method (Schmittgen and Livak 2008) was applied to quantify the effects of HPx and physostigmine on the expression of these genes (Fig. 4).
Discussion
Following major surgery, many patients experience problems that originate from the brain, such as postoperative cognitive dysfunction and POD. Initiation of neuroinflammation is considered one of the central mechanisms in the development of such cerebral dysfunction (Cerejeira et al. 2010). Since the mechanisms that are involved in the development of neuroinflammation and cerebral dysfunction following major surgery are still poorly understood, also robust clinical strategies to prevent POD are lacking. This can be mainly attributed to the complex multifactorial nature of POD. Animal models can be shaped to help unraveling such complexity by focusing on single but potentially basic mechanisms of POD development, like the role of cerebral ACh signaling in neuroinflammation.
Our model demonstrates that surgery is associated with a postoperative reduction of cerebral ACh levels. Thus, our results are in line with the cholinergic deficiency hypothesis in delirium (Hshieh et al. 2008). We selected a time point of 120 min in accordance with our previous data (Plaschke et al. 2014, 2016) showing an induction of cytokines at 120 min after surgery. In addition, 120 min after surgery is a typical time point of postoperative deteriorations, e.g. for POD. Our previous investigations suggest that a surgery-triggered increase of cerebral AChE activity might contribute to the postoperative reduction of cerebral ACh levels. A potential mechanism could be the AChE gene activation by cholinergic neurotransmission via a feedback mechanism, leading to increased formation of AChE protein and accelerated degradation of ACh at cholinergic synapses (Nitsch et al. 1998). Also a reduction of ACh release has been suggested to conduce to neuroinflammation-associated hypocholinergic activity in the brain (Rada et al. 1991; Taepavarapruk and Song 2010). Such decrease of the ACh level in brain is associated with an increase of proinflammatory cytokines. IL-1β, known to be one of the most potent inducers of neuroinflammation (Basu et al. 2004), is not detectable in CSF of the control animals, but high concentrations of this “master regulator of neuroinflammation” (Basu et al. 2004) are found in the HPx animals. The point of view that IL-1β plays a dominating role in neuroinflammation is corroborated by the observation that reduction of ILR1 in the brain alleviates neuroinflammatory reactions thereby conferring neuroprotection (Lazovic et al. 2005). However, our multiplex assay indicates that besides IL-1β the concerted action of several cytokines may contribute to the full-blown picture of surgery-induced neuroinflammation. In particular, IL-6 and TNFα are also considered to be at the top of the hierarchy of inflammation-regulatory processes. Autocrine activation of microglia by TNFα can orchestrate a complex proinflammatory microglial reaction (Kuno et al. 2005). The important role of IL-6 as important inducer of neuroinflammation is exemplified in a recent study showing that intracisternal administration of an IL-6 antagonist attenuates surgery-induced cognitive impairment by inhibition of neuroinflammatory responses in laparatomized rats (Jiang et al. 2015). Interestingly, IL-1β was also shown to serve as a long-lasting stimulus for MIP-2 expression. Thus IL-1β-dependent induction of MIP-2 (CXCL2), as also indicated by our present study, may play a role in sustaining neuroinflammation (Shaftel et al. 2007). RANTES (CCL5) was initially described as a potent chemoattractant guiding leukocytes to sites of inflammation and injury (Schall 1991). However, in the CNS it was also suggested to exert neurotrophic and neuroprotective activities (Bolin et al. 1998; Tripathy et al. 2010). Yet, the functions of CCL5 in the brain are multifaceted, since it can bind to different receptors that are restricted to certain regions in the brain. Even a function of CCL5 in neuronal/glial communication was suggested (Lanfranco et al. 2017). Increase of MCP-1 (CCL2) has been associated with several neuroinflammatory conditions (Conductier et al. 2010). Based on a clinical study in hip fracture patients in which a significant association between increased MCP-1 levels and the development of delirium in the postoperative face was found, a role of MCP-1 in the pathogenesis was hypothesized (Skrede et al. 2015). Our results, indicating an ACh-induced reduction of MCP-1 in the CNS of HPx-treated animals, support this hypothesis. HPx had only a moderate effect on IFNγ levels in CSF which was augmented by physostigmine-induced increase of ACh. The role of IFNγ is difficult to pin down since both neuroprotective/neuroregulatory as well as proinflammatory functions are effective. Such opposing role of IFNγ appears to depend on dose, disease phase, and cell development stage (Ottum et al. 2015). Elevated levels of IP-10 (CXCL10) during neuroinflammation, as also found in our study, can alter neuronal excitability and calcium signaling in hippocampal neurons. In particular, changes in neuronal excitability induced by IP-10 may contribute to the cognitive dysfunction (Cho et al. 2009; Nelson and Gruol 2004). Since IL-10 is known as an effective anti-inflammatory cytokine, its striking increase after HPx can be considered a counterregulation to the strong inflammatory stimulus by the other cytokines. Physostigmine had no effect on its secretion after HPx indicating that the cholinergic system is not directly involved in its release under these conditions.
For IL1β, IL6, TNFα, MIP2, RANTES and MCP1, in addition to the increased ACh-dependent secretion, also an induction of their gene expression was found, indicating that their synthesis was also induced. Likewise the synthesis of HMGB1 was induced. HMGB1 is considered to prime microglia for an inflammatory response thereby potentiating to action of proinflammatory cytokines in the brain (Fonken et al. 2016; Frank et al. 2015). Members of the tumor necrosis factor (TNFSF) superfamily are considered central mediators of the extrinsic apoptotic pathway. Thus, the induction of TNFSF6 and TNFSF12 expression after HPx and the alleviating effect of physostigmine hint to an ACh-dependent proapoptotic signaling (Sonar and Lal 2015). Besides the increase of IL-1β and IL-6 expression and secretion in the CNS also an induction of their receptors IL1R1 and ILR6 was observed. IL-1R1 has been localized widely in the CNS. Notably, there is strong evidence that IL1R1 and IL6R are expressed in neurons and these receptors play an important role in neuroinflammation-induced neurodegeneration (Guo et al. 2007; Holmes et al. 2004; Kempuraj et al. 2016). To investigate functional changes after HPx and physostigmine application, psychometric investigations relating spatial cognition, also in more aged rats, actually are under the way. In conclusion, our study substantiates the point of view that a decrease of cholinergic signaling in the CNS after peripheral surgery triggers a complex proinflammatory reaction in the brain that is considered to play a pivotal role in the development of delirium. This reaction can be extenuated by medication with physostigmine which restores the cerebral ACh levels. Although the kinetic half-life of physostigmine is only about 16–20 min, its anti-inflammatory action was sustained until 120 min. This is in line with the observation that during single-dose conditions the dynamic half-life of the drug is substantially longer (Asthana et al. 1995). Correspondingly, a recent case report refers a single dose of physostigmine as a successful therapeutic intervention in a patient who developed severe POD (Zujalovic and Barth 2015).
Abbreviations
- ACh:
-
Acetylcholine
- CNS:
-
Central nervous system
- CSF:
-
Cerebrospinal fluid
- HPx:
-
Partial hepatectomy
- POD:
-
Postoperative delirium
References
Acharya NK, Goldwaser EL, Forsberg MM, Godsey GA, Johnson CA, Sarkar A, DeMarshall C, Kosciuk MC, Dash JM, Hale CP et al (2015) Sevoflurane and isoflurane induce structural changes in brain vascular endothelial cells and increase blood–brain barrier permeability: possible link to postoperative delirium and cognitive decline. Brain Res 1620:29–41
Asthana S, Greig NH, Hegedus L, Holloway HH, Raffaele KC, Schapiro MB, Soncrant TT (1995) Clinical pharmacokinetics of physostigmine in patients with Alzheimer’s disease. Clin Pharmacol Ther 58:299–309
Basu A, Krady JK, Levison SW (2004) Interleukin-1: a master regulator of neuroinflammation. J Neurosci Res 78:151–156
Bolin LM, Murray R, Lukacs NW, Strieter RM, Kunkel SL, Schall TJ, Bacon KB (1998) Primary sensory neurons migrate in response to the chemokine RANTES. J Neuroimmunol 81:49–57
Cerejeira J, Firmino H, Vaz-Serra A, Mukaetova-Ladinska EB (2010) The neuroinflammatory hypothesis of delirium. Acta Neuropathol 119:737–754
Chavan SS, Pavlov VA, Tracey KJ (2017) Mechanisms and therapeutic relevance of neuro-immune communication. Immunity 46:927–942
Cho J, Nelson TE, Bajova H, Gruol DL (2009) Chronic CXCL10 alters neuronal properties in rat hippocampal culture. J Neuroimmunol 207:92–100
Conductier G, Blondeau N, Guyon A, Nahon JL, Rovere C (2010) The role of monocyte chemoattractant protein MCP1/CCL2 in neuroinflammatory diseases. J Neuroimmunol 224:93–100
Cortese GP, Burger C (2017) Neuroinflammatory challenges compromise neuronal function in the aging brain: postoperative cognitive delirium and Alzheimer’s disease. Behav Brain Res 322:269–279
Fonken LK et al (2016) The alarmin HMGB1 mediates age-induced neuroinflammatory priming. J Neurosci 36:7946–7956
Frank MG, Weber MD, Watkins LR, Maier SF (2015) Stress sounds the alarmin: the role of the danger-associated molecular pattern HMGB1 in stress-induced neuroinflammatory priming. Brain Behav Immun 48:1–7
Guo W, Wang H, Watanabe M, Shimizu K, Zou S, LaGraize SC, Wei F, Dubner R, Ren K (2007) Glial-cytokine-neuronal interactions underlying the mechanisms of persistent pain. J Neurosci 27:6006–6018. https://doi.org/10.1523/jneurosci.0176-07.2007
Holmes GM, Hebert SL, Rogers RC, Hermann GE (2004) Immunocytochemical localization of TNF type 1 and type 2 receptors in the rat spinal cord. Brain Res 1025:210–219
Hshieh TT, Fong TG, Marcantonio ER, Inouye SK (2008) Cholinergic deficiency hypothesis in delirium: a synthesis of current evidence. J Gerontol Ser A 63:764–772
Jiang P, Ling Q, Liu H, Tu W (2015) Intracisternal administration of an interleukin-6 receptor antagonist attenuates surgery-induced cognitive impairment by inhibition of neuroinflammatory responses in aged rats. Exp Ther Med 9:982–986
Kempuraj D, Thangavel R, Natteru PA, Selvakumar GP, Saeed D, Zahoor H, Zaheer S, Iyer SS, Zaheer A (2016) Neuroinflammation induces neurodegeneration. J Neurol Neurosurg Spine 1:1003
Kuno R, Wang J, Kawanokuchi J, Takeuchi H, Mizuno T, Suzumura A (2005) Autocrine activation of microglia by tumor necrosis factor-alpha. J Neuroimmunol 162:89–96
Lanfranco MF, Mocchetti I, Burns MP, Villapol S (2017) Glial- and neuronal-specific expression of CCL5 mRNA in the rat brain. Front Neuroanat 11:137
Lazovic J, Basu A, Lin HW, Rothstein RP, Krady JK, Smith MB, Levison SW (2005) Neuroinflammation and both cytotoxic and vasogenic edema are reduced in interleukin-1 type 1 receptor-deficient mice conferring neuroprotection. Stroke 36:2226–2231
Maldonado JR (2008) Delirium in the acute care setting: characteristics, diagnosis and treatment. Crit Care Clin 24:657–722
Nelson TE, Gruol DL (2004) The chemokine CXCL10 modulates excitatory activity and intracellular calcium signaling in cultured hippocampal neurons. J Neuroimmunol 156:74–87
Nitsch RM, Rossner S, Albrecht C, Mayhaus M, Enderich J, Schliebs R, Wegner M, Arendt T, von der Kammer H (1998) Muscarinic acetylcholine receptors activate the acetylcholinesterase gene promoter. J Physiol Paris 92:257–264
Ottum PA, Arellano G, Reyes LI, Iruretagoyena M, Naves R (2015) Opposing roles of interferon-gamma on cells of the central nervous system in autoimmune neuroinflammation. Front Immunol 6:539
Pavlov VA, Tracey KJ (2015) Neural circuitry and immunity. Immunol Res 63:38–57
Plaschke K, Muller AK, Kopitz J (2014) Surgery-induced changes in rat IL-1beta and acetylcholine metabolism: role of physostigmine. Clin Exp Pharmacol Physiol 41:663–670
Plaschke K, Weigand MA, Fricke F, Kopitz J (2016) Neuroinflammation: effect of surgical stress compared to anaesthesia and effect of physostigmine. Neurol Res 38:397–405
Rada P, Mark GP, Vitek MP, Mangano RM, Blume AJ, Beer B, Hoebel BG (1991) Interleukin-1 beta decreases acetylcholine measured by microdialysis in the hippocampus of freely moving rats. Brain Res 550:287–290
Rudolph JL, Ramlawi B, Kuchel GA, McElhaney JE, Xie D, Sellke FW, Khabbaz K, Levkoff SE, Marcantonio ER (2008) Chemokines are associated with delirium after cardiac surgery. J Gerontol Ser A 63:184–189
Schall TJ (1991) Biology of the RANTES/SIS cytokine family. Cytokine 3:165–183
Schmittgen TD, Livak KJ (2008) Analyzing real-time PCR data by the comparative C(T) method. Nat Protoc 3:1101–1108
Shaftel SS, Carlson TJ, Olschowka JA, Kyrkanides S, Matousek SB, O’Banion MK (2007) Chronic interleukin-1beta expression in mouse brain leads to leukocyte infiltration and neutrophil-independent blood brain barrier permeability without overt neurodegeneration. J Neurosci 27:9301–9309
Shytle RD, Mori T, Townsend K, Vendrame M, Sun N, Zeng J, Ehrhart J, Silver AA, Sanberg PR, Tan J (2004) Cholinergic modulation of microglial activation by alpha 7 nicotinic receptors. J Neurochem 89:337–343
Skrede K, Wyller TB, Watne LO, Seljeflot I, Juliebo V (2015) Is there a role for monocyte chemoattractant protein-1 in delirium? Novel observations in elderly hip fracture patients. BMC Res Notes 8:186
Sonar S, Lal G (2015) Role of tumor necrosis factor superfamily in neuroinflammation and autoimmunity. Front Immunol 6:364
Steiner LA (2011) Postoperative delirium. Part 1: pathophysiology and risk factors. Eur J Anaesthesiol 28:628–636
Taepavarapruk P, Song C (2010) Reductions of acetylcholine release and nerve growth factor expression are correlated with memory impairment induced by interleukin-1beta administrations: effects of omega-3 fatty acid EPA treatment. J Neurochem 112:1054–1064
Terrando N, Yang T, Ryu JK, Newton PT, Monaco C, Feldmann M, Ma D, Akassoglou K, Maze M (2014) Stimulation of the α7 nicotinic acetylcholine receptor protects against neuroinflammation after tibia fracture and endotoxemia in mice. Mol Med 20:667–675
Tripathy D, Thirumangalakudi L, Grammas P (2010) RANTES upregulation in the Alzheimer’s disease brain: a possible neuroprotective role. Neurobiol Aging 31:8–16
van Gool WA, van de Beek D, Eikelenboom P (2010) Systemic infection and delirium: when cytokines and acetylcholine collide. Lancet 375:773–775
Whitlock EL, Vannucci A, Avidan MS (2011) Postoperative delirium. Minerva Anestesiol 77:448–456
Zujalovic B, Barth E (2015) Delirium accompanied by cholinergic deficiency and organ failure in a 73-year-old critically ill patient: physostigmine as a therapeutic option. Case Rep Crit Care 2015:793015
Acknowledgements
The expert technical assistance of Roland Galmbacher, Klaus Stefan and Sigrun Himmelsbach is gratefully appreciated. We also acknowledge financial support by Dr. Franz Köhler Chemie, Bensheim, Germany.
Funding
This study was supported by a research fund from Dr. Franz Köhler Chemie GmbH (Bensheim, Germany).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Plaschke, K., Schulz, S., Rullof, R. et al. In-depth characterization of the neuroinflammatory reaction induced by peripheral surgery in an animal model. J Neural Transm 125, 1487–1494 (2018). https://doi.org/10.1007/s00702-018-1909-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-018-1909-x