Abstract
In spastic paresis, stretch applied to the antagonist increases its inappropriate recruitment during agonist command (spastic co-contraction). It is unknown whether antagonist stretch: (1) also affects agonist recruitment; (2) alters effort perception. We quantified voluntary activation of ankle dorsiflexors, effort perception, and plantar flexor co-contraction during graded dorsiflexion efforts at two gastrocnemius lengths. Eighteen healthy (age 41 ± 13) and 18 hemiparetic (age 54 ± 12) subjects performed light, medium and maximal isometric dorsiflexion efforts with the knee flexed or extended. We determined dorsiflexor torque, Root Mean Square EMG and Agonist Recruitment/Co-contraction Indices (ARI/CCI) from the 500 ms peak voluntary agonist recruitment in a 5-s maximal isometric effort in tibialis anterior, soleus and medial gastrocnemius. Subjects retrospectively reported effort perception on a 10-point visual analog scale. During gastrocnemius stretch in hemiparetic subjects, we observed: (1) a 25 ± 7 % reduction of tibialis anterior voluntary activation (maximum reduction 98 %; knee extended vs knee flexed; p = 0.007, ANOVA); (2) an increase in dorsiflexion effort perception (p = 0.03, ANCOVA). Such changes did not occur in healthy subjects. Effort perception depended on tibialis anterior recruitment only (βARITA = 0.61, p < 0.01) in healthy subjects (not on gastrocnemius medialis co-contraction) while it depended on both tibialis anterior agonist recruitment (βARITA = 0.41, p < 0.001) and gastrocnemius medialis co-contraction (βCCIMG = 0.43, p < 0.001) in hemiparetic subjects. In hemiparesis, voluntary ability to recruit agonist motoneurones is impaired—sometimes abolished—by antagonist stretch, a phenomenon defined here as stretch-sensitive paresis. In addition, spastic co-contraction increases effort perception, an additional incentive to evaluate and treat this phenomenon.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tardieu has postulated that the major factor limiting active movement in spastic paresis is the antagonist (Tardieu 1966). It has been suggested in particular that the responsiveness of agonist motoneurones to descending commands may be impacted by the stretch imposed on the antagonist (Gracies 2005). In healthy subjects, motoneurone output is known to be sensitive to agonist stretch, depending on whether contraction is eccentric or concentric (Abbruzzese et al. 1994; Sekiguchi et al. 2001, 2003). The primary question addressed here was thus whether antagonist stretch might impede the ability to activate the agonist motoneurones in hemiparesis.
The second objective of this study was to determine whether effort perception (not the sense of the force achieved) (McCloskey et al. 1983) during agonist recruitment might also depend on antagonist stretch. Beyond feedforward information on the centrally generated command (McCloskey et al. 1974; Gandevia and McCloskey 1977a, b; Jones and Hunter 1983; Jones 1986; Cafarelli and Bigland-Ritchie 1979), feedback from peripheral receptors (Roland and Ladegaard-Pedersen 1977; Jones and Hunter 1985) may also contribute to effort perception, which is typically increased in disorders, of central origin (Gandevia and McCloskey 1977b; Jones and Hunter 1983; Simon et al. 2009; Holmes 1917; Solomon and Robin 2005). Whether a specific peripheral situation such as antagonist stretch might also impact on effort perception during agonist recruitment is unknown in spastic paresis. Finally, in the light of the impact of spastic co-contraction on motor weakness particularly when the co-contracting muscle is stretched (Gracies et al. 1997; Gracies 2005; Bourbonnais and Vanden Noven 1989; el-Abd et al. 1993; Dewald et al. 1995; Ikeda et al. 1998; Kamper and Rymer 2001; Vinti et al. 2013), we also aimed to explore the specific role of co-contraction in the effort perception in hemiparesis.
We have used a model of graded dorsiflexion efforts with or without gastrocnemius stretch (knee extended or flexed), positions that did not alter the length of the agonist dorsiflexors. Our primary hypothesis was that stretch in a contractured antagonist (i.e. a muscle with reduced length and reduced passive extensibility) such as the gastrocnemius might diminish the ability of the motor command to recruit agonist dorsiflexor motoneurones in hemiparesis. Further, we hypothesized an influence of spastic co-contraction on the perceived effort, suggesting that, in addition to limiting active movements, spastic co-contraction might also participate in the perception of weakness. A first part of the data using this paradigm but focusing on torques and co-contraction has previously been published (Vinti et al. 2013).
Methods
Subjects
This study was approved by the local ethics committee—Comité de Protection des Personnes Ile-de-France IX. Eighteen subjects with hemiparesis (8 women, age 54 ± 12, mean ± SD) from the Neurorehabilitation clinic of Henri Mondor University Hospitals (Créteil, France) and 18 healthy subjects (9 women, age 41 ± 13) underwent isometric dynamometric evaluation. Inclusion criteria for hemiparetic subjects were (1) vascular or traumatic brain injury-induced hemiparesis at least 6 months prior, and (2) a range of passive ankle dorsiflexion of at least 90° (Tardieu Scale, Gracies et al. 2010) with knee flexed or extended. Exclusion criteria consisted of intercurrent disease affecting ability to participate, cognitive dysfunction—in particular neglect—and major proprioceptive impairment, the latter two based on clinical examination including line bisection tests and determination of the joint perception thresholds using a goniometer. Inclusion criteria for healthy subjects were (1) absence of neurological disorder and (2) age <75.
Experimental procedures
Clinical examination in hemiparetic subjects included a 10-m ambulation speed and plantar flexor spasticity angle and grade using the Tardieu Scale (Gracies et al. 2010).
Measurements of torque and effort perception
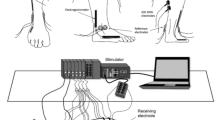
The precise methodology has been previously described (Vinti et al. 2013). In brief, isometric evaluation of ankle torque was performed using a dynamometric apparatus (Contrex™, CMV AG, Switzerland). Subjects were comfortably semi-seated with the tested ankle strapped to a rotating footplate, fixed at 90° of dorsiflexion, in one of two knee positions: extended and flexed at 90°. The hip was kept around 80°–100° flexion throughout the procedures. The axis between the two malleoli was used as the landmark for matching the ankle joint with the axis of rotation of the resistance adapter. The knee-extended position was arranged to place the trans-joint gastrocnemius muscle in maximally stretched position. The level of torque at each effort was recorded; considering measurement errors at low torques, only dorsiflexor torque levels greater than 2 Nm were considered “positive” in terms of capacity to help initiate foot dorsiflexion. The same investigator carried out all procedures.
After a few slow passive movements at low speed (10°/sec) from minimally to maximally stretched position of the plantar flexors to make the subject familiar with the apparatus, the ankle was positioned back at 90° dorsiflexion and the subject was asked to perform one maximal isometric dorsiflexion (“lift up your foot as hard as possible”) and one maximal isometric plantar flexion (“push down your foot as hard as possible”) to become familiarized with the feeling associated with a maximal contraction.
Then the subject was asked to produce three dorsiflexion efforts, one at light intensity (approximately 10–20 % maximum), one at medium intensity (approximately 50–60 %) and again one at maximal intensity, in that order. While different subjects could interpret “light” and “medium” efforts differently, producing some variability in the actual percent of maximum, each subject attempted to reproduce those same effort levels with the knee flexed and extended. Each effort was to be sustained for 5 s, and this was verified using EMG monitoring and encouraged verbally.
Immediately after each effort, subjects were asked to quantify the perception of the effort produced using a Visual Analog Scale of Perceived Effort (VASPE), much as in pain measurements (Huskisson 1974). At one end of a straight 100-mm line the number zero indicated a sensation of no effort, and at the other end the number 10 indicated a sensation of maximal effort. Subjects placed a check on the line at the point that would best reflect the intensity of their effort. In addition to quantifying subjective impression of the effort achieved, this served as a quality control of the three prescribed intensity levels.
EMG measurements
Muscle activity was assessed by surface EMG simultaneously from ankle dorsiflexors (tibialis anterior, TA) and plantar flexors (soleus, SO and medial gastrocnemius, MG) with pairs of surface electrodes (ARBO H135TSG, device ME 6000 from MEGA Electronics system, Cambridge, UK). The skin was cleansed and abraded with alcohol before electrode application. Electrode positioning followed the recommendations of Basmajian and Blumenstein (1980). The EMG signal was sampled at 2000 Hz, amplified (gain = 1000), filtered using a bank of anticausal notch filters to remove the power line interference (50 Hz) and its harmonics. Each notch filter was centered at the frequency of 50 × i Hz, with i ranging from 1 to 9, and had a bandwidth of 4 Hz. Filtered signals were rectified. All computations were performed by a custom-written Matlab program (version 7.1, Natick, Massachusetts, USA). From these processed surface EMG measurements, we derived in each knee position: (1) The agonist Root Mean Square (RMS) of ankle dorsiflexor/plantar flexor EMG during maximal isometric ankle dorsiflexion/plantar flexion, measured over the 500 ms around the recruitment peak. The timing of the agonist peak recruitment within the 5 s was not specifically monitored. (2) The Agonist Recruitment Index (ARI), i.e. the ratio of the RMS of a muscle acting as an agonist during a given period to its largest RMS value observed during the 500 ms around its agonist recruitment peak. (3) The Co-contraction Index (CCI), defined as the ratio of the RMS of the EMG of the muscle when it was antagonist to the intended effort (i.e. opposing the intended direction of the effort) to the RMS of its EMG when acting as an agonist during the 500 ms around its recruitment peak.
Statistical analysis
After a descriptive analysis deriving average values and standard deviations of all continuous variables, we performed two-factor (group × position) and (group × effort) ANOVAs with repeated measures to detect changes in RMSTA, ARITA and the perceived effort (VASPE) across the three-graded efforts (light, medium and maximal) in both populations, first whichever the position and second whichever the effort. We then compared the relative influence of potential predictors (ARITA, CCI and Torque) on the dependent variable VASPE in each population, using standardized regression coefficients obtained from multiple regression analysis. Significance was set at p < 0.05.
Results
Patient characteristics
As reported in a previous paper using the same experimental paradigm (Vinti et al. 2013), the 18 patients included 9 cases of left hemiparesis. Ten-meter ambulation velocity was 0.64 ± 0.17 m/s (mean ± SEM) at comfortable speed and 0.84 ± 0.24 at maximal safe speed. In soleus, spasticity angle was 12.7° ± 6.8° and spasticity grade was 2.4 ± 0.8. In gastrocnemius, spasticity angle was 7.5° ± 4.5° and spasticity grade was 2.1 ± 0.8 (Gracies et al. 2010). During torque and EMG measurements all subjects were able to maintain effort (agonist EMG activation) for the full 5 s upon verbal encouragement. Torques for all contractions were close to three times higher in healthy subjects than in subjects with hemiparesis, as has been reported previously (Vinti et al. 2013).
Agonist tibialis anterior recruitment
Illustrations of typical EMG responses during the different levels of voluntary effort in each group have been previously provided (Vinti et al. 2013).
Effect of position
Whatever the effort, there was a major interaction between group (hemiparetic or healthy) and position (knee flexed or extended) for the raw agonist RMS of tibialis anterior (RMSTA, F 2,206 = 32.85, p < 0.0001) with a 25 ± 7 % (up to 98 %) reduction of RMSTA from knee flexed to extended in hemiparetic subjects, across all effort grades (p = 0.007), not seen in healthy subjects (p = 0.95; Fig. 1a). Averaging each effort grade separately in hemiparetic subjects, the difference knee flexed–knee extended for RMSTA was significant during the maximal efforts only (mean reduction 28 ± 8 %; p = 0.002; Fig. 1b, c). In individual patients, however, RMSTA reduction from knee flexed to knee extended was greater than 80 % in three subjects for light efforts, one subject for medium efforts and one subject for maximal efforts. These subjects with major inhibitory impact of the knee-extended position on agonist TA recruitment seemed more spastic in the plantar flexors (mean spasticity angle 19.3° ± 5.1° in soleus and 9.5° ± 1.5° in gastrocnemius) and slower walkers (mean 10-m ambulation velocity 0.60 ± 0.05 m/s at comfortable speed and 0.72 ± 0.07 m/s at maximal safe speed) than the rest of the group. The interaction between group and position for raw agonist recruitment (RMSTA) was lost when considering agonist recruitment indices only (ARITA; Fig. 2a, b).
Effect of effort
RMSTA increased from light to maximal efforts in healthy (F 2,102 = 40.87, p < 0.0001) and hemiparetic subjects (F 2,96 = 13.13, p < 0.0001) whatever the knee position (Fig. 1b, c). In parallel, ARITA also increased across the graded efforts in both groups (p < 0.0001; Fig. 2a, b). In both joint positions there was a trend for an interaction between group and effort for ARITA (F 2,201 = 2.58, p = 0.08). This interaction was highly significant for maximal efforts, where ARITA was greater in healthy subjects than in hemiparetic subjects (0.90 ± 0.01 vs 0.82 ± 0.02, p < 0.0001, ANOVA).
Plantar flexor co-contraction
Plantar flexor co-contraction and torque data have been reported in a previous article (Vinti et al. 2013). In brief: (1) CCIs were abnormally high for the three dorsiflexion effort levels in hemiparetic subjects; (2) whatever the dorsiflexion effort, there was a strong interaction between position and group for the soleus (F 2,196 = 9.37, p < 0.001) and for medial gastrocnemius (F 2,196 = 21.91, p < 0.0001): the knee-extended position was associated with an increase in soleus CCI in hemiparetic subjects (p < 0.001) but not in healthy subjects and with reduced medial gastrocnemius co-contraction in healthy subjects but maintained levels in hemiparetic subjects; (3),in hemiparesis the increased co-contraction associated with gastrocnemius stretch was sufficient to reverse or cancel the intended dorsiflexor torque in 26 % of cases (Vinti et al. 2013).
Perception of dorsiflexion effort
Effect of effort
From light to medium and maximal efforts, perception increased in both healthy (F 2,202 = 354, p < 0.0001; Fig. 3a) and hemiparetic subjects (F 2,202 = 236, p < 0.0001; Fig. 3b) for both knee positions. The three-way ANOVA (group × position × effort) revealed a significant interaction, group × effort (p = 0.002) across both knee positions, whereby light efforts were perceived as lighter by healthy subjects (95 % CI VASPE [1.76–2.60]) than by hemiparetic subjects (95 % CI [2.67–3.49]), and maximal efforts were perceived as stronger by healthy subjects (95 % CI VASPE [8.52–9.36]) than by hemiparetic subjects (95 % CI [7.89–8.71]; Fig. 3a, b).
Effect of position
Whatever the effort, knee position had an impact on the dorsiflexion effort perception in hemiparetic subjects, which was on average 7 % greater in the extended than in the flexed position (5.6 vs 5.2, p = 0.03, ANCOVA; Fig. 3b). This effect was greatest for light efforts, where effort perception increased by 20 % when the knee was extended (2.8 vs 3.4, p < 0.05). In contrast, healthy subjects displayed no difference in the effort perception between the two knee positions, whatever the effort.
Effect of agonist contraction and antagonist co-contraction
When the knee was flexed, in healthy subjects the perception of dorsiflexion efforts (VASPE) was related to tibialis anterior activation only (standardized regression coefficient βARITA = 0.67, p < 0.0001), with no impact of medial gastrocnemius co-contraction or the torque produced (βCCIMG = 0.14, NS; βtorque = 0.11, NS). In hemiparetic subjects, however, effort perception was related to both tibialis anterior activation and gastrocnemius antagonist co-contraction (βARITA = 0.42, p < 0.002; βCCIMG = 0.39, p < 0.001; Fig. 4a, b).
Determinants of dorsiflexor effort perception. Standardized regression coefficients (β) of three potential predictors of effort perception in healthy (a) and hemiparetic (b) subjects knee flexed (left) and extended (right). Bars 95 % confidence intervals. In hemiparetic subjects knee extended, plantar flexor co-contraction becomes the strongest predictor
When the knee was extended, the perception of effort by healthy subjects was related to tibialis anterior activation (βARITA = 0.54, p < 0.01) and the resulting torque (p < 0.01), with again no impact of antagonist co-contraction (βCCIMG = 0.12, p = 0.40; Fig. 4a). In hemiparesis, however, plantar flexor co-contraction was the strongest predictor of effort perception (βCCIMG = 0.45, p < 0.001), together with tibialis anterior activation (βARITA = 0.40, p < 0.001) and the torque (p < 0.05; Fig. 4b).
Discussion
This study demonstrates an increase in dorsiflexor paresis (reduced output from dorsiflexor motoneurones—sometimes virtually cancelled) with antagonist muscle stretch, a phenomenon defined here as stretch-sensitive paresis. The study also reports an increase in dorsiflexion effort perception with gastrocnemius stretch in spastic paresis, probably related to both antagonist stretch itself and the associated spastic co-contraction increase.
Impact of antagonist position on agonist recruitment: stretch-sensitive paresis
A previous paper already demonstrated and quantified the increase in plantar flexor co-contraction and the decrease in dorsiflexor torque at three dorsiflexion effort levels in hemiparetic subjects when the knee was in extended position (Vinti et al. 2013). Here, we demonstrate for the first time that the reduction in agonist torque with antagonist stretch is not only due to the increase in plantar flexor co-contraction (Levin et al. 2000; Knutsson and Mårtensson 1980) but also to a decrease in agonist motoneuroneal recruitment, which we were able to measure. The phenomenon of decreased agonist recruitment with antagonist stretch thus goes over and above the classically described spastic restraint, which merely corresponded to torque limitation due to passive and active antagonist resistance (Kamper et al. 2003; Dietz et al. 1981; Koo et al. 2003; Hu et al. 2006; Gracies et al. 1997; Tardieu 1966; Vinti et al. 2013; Ikeda et al. 1998; Kamper and Rymer 2001). This study helps explain torque reduction during antagonist stretch by a decrease in agonist EMG.
In spastic paresis, reduced EMG signals may reflect at least in part decreased excitatory drive to agonist motoneurones, contributing to reduced force or movement (Dietz et al. 1981; Koo et al. 2003; Hu et al. 2006; Sahrmann and Norton 1977; Knutsson and Richards 1979; Inman et al. 1952; Woods and Bigland-Ritchie 1983; Bourbonnais et al. 1989; Visser and Aanen 1981). In the face of triceps surae co-contraction, the net torque associated with dorsiflexion efforts could then become negligible or even be reversed into plantar flexion (Vinti et al. 2013; Levin et al. 2000). This effect was higher during strong efforts but was also major during light or medium efforts in individual cases.
The classically altered EMG–force relationship in spastic paresis (Dietz et al. 1981; Bourbonnais et al. 1989; Dewald et al. 1995; Canning et al. 2000) was not a critical issue here as our conclusions rely mostly on quantitative EMG measures, and because the observed decrease in agonist tibialis anterior EMG paralleled that in dorsiflexion torque (Vinti et al. 2013). These findings are also not due to muscle or skin conformation changes because tibialis anterior length and skin stretch on the anterior aspect of the leg are not affected by knee position changes. Accordingly, tibialis anterior EMG was not different in healthy subjects when knee position was changed (Fig. 1a), which confirmed previous evidence (Cafarelli and Bigland-Ritchie 1979; Komi and Buskirk 1972; Marsh et al. 1981; Newman et al. 2003).
Rather, the reduction of dorsiflexor recruitment by gastrocnemius stretch in hemiparesis might involve reciprocal inhibition from triceps surae (Cody et al. 1987; Simonetta-Moreau et al. 1999; Marque et al. 2001). Tonic gastrocnemius stretch could exert a post-synaptic inhibitory effect on tibialis anterior motoneurones, making them less able to respond to descending voluntary drives (Simonetta-Moreau et al. 1999; Marque et al. 2001). This effect would further diminish the ability of a weakened descending command to bring motoneurones to firing threshold, sufficiently to completely abolish voluntary dorsiflexors EMG in some patients. The larger effects in maximal efforts (Fig. 1) and the loss—or rather masking—of these inhibitory effects when looking only at agonist recruitment indices (Fig. 2) might involve preferential effects of such reciprocal inhibition on the latest recruited motoneurones therefore on the high-threshold motoneurones. However, while some studies mention various sensitivities of motoneurones of different sizes to Ia reciprocal inhibition or Group II inputs, no quantification is available to our knowledge (Henneman 1985; Marchand-Pauvert et al. 2000; Pierrot-Deseilligny and Burke 2005). Finally, Ia reciprocal inhibition effects would certainly increase from muscles with higher spindle sensitivity, which is the case of the most contractured muscles (Gioux and Petit 1993). Even though the present study was not designed to study reciprocity in stretch-sensitive paresis (the position knee extended or knee flexed altered only the length of gastrocnemius and not of tibialis anterior), we would speculate that this increased paresis might thus affect particularly the less contractured of two muscles around a joint when its more contractured antagonist is stretched, a phenomenon termed stretch-sensitive paresis (Gracies 2005).
Effect of antagonist position—and of spastic co-contraction—on the perception of agonist effort
This study showed increased dorsiflexor effort perception with gastrocnemius stretch in hemiparetic subjects, but not in healthy subjects. It may appear paradoxical that effort perception would increase in the position knee extended, while agonist recruitment decreased in that condition, even though effort perception partially depended on agonist recruitment (Fig. 4). Such paradox could be explained by an increased magnitude of the dependence of effort perception on antagonist co-contraction, as shown in Fig. 4. Here, increased dorsiflexor effort perception with the knee extended has to do with the associated increased plantar flexor co-contraction in that situation (Vinti et al. 2013), rather than with plantar flexor stretch per se (the degree of gastrocnemius stretch was similar in all patients with the knee extended but plantar flexor co-contraction and sense of effort vastly differed). To further establish this hypothesis might require pure motor blocks (e.g. using curare) to filter out the effects of antagonist co-contraction from those of antagonist stretch on agonist effort perception. The study otherwise confirmed increased effort perception with the isometric force exerted (Stevens and Cain 1970; Eisler 1962; Cain and Stevens 1971) at least with the knee extended, for both healthy and hemiparetic subjects (Fig. 4).
Reduced range of effort perception in spastic paresis
The correspondence between the prescribed level of effort (Fig. 3, X axis) and the level of effort retrospectively estimated (Y axis) suggests gross capacity of subjects (healthy and hemiparetic) to appropriately follow the light, medium and maximal effort levels. However, the range of available effort perceptions appeared reduced in hemiparesis, raising the question of a dampened effort perception (Fig. 3). Alternatively, the striking parallelism to the reduced range of agonist recruitment indices (Fig. 2) suggests a correlation between effort perception and agonist recruitment index, demonstrated in Fig. 4, the effort perception itself being adequate in hemiparesis. On the high end of the range, reduction of maximal agonist recruitment index over 5 s efforts could reveal higher fatigability of large muscle fibers in paresis, explaining short tolerance to strong efforts (Dietz et al. 1981, 1986; Edström 1970 ). On the low end, changes in recruitment gain of motoneurone pools with non-uniform distribution of synaptic effects to low- and high-threshold motor units could explain previously reported sustained tonic motoneurone firing with little or no synaptic input in spastic paresis, especially in low-threshold units (Hultborn et al. 2004; Heckmann et al. 2005; Mottram et al. 2009). Yet, reduced proprioception in hemiparesis may also contribute to a reduced range of effort perceptions but patients with major sensory impairment were not included in this study (see “Methods”) (Carey et al. 1996; Tyson et al. 2013).
Study limitations
Exact knee angles were not verified with goniometry, thus the two knee positions might not have been comparable for the two groups, as hamstrings shortening might have limited ability to obtain full knee extension in the paretic group. However, significant hamstring shortening is rare with adult-acquired brain lesions, as opposed to infant-acquired lesions (Van Reeth et al. 2013a, b). More importantly, the exact knee angle in the situation “knee extended” was not relevant here, rather the fact that the knee was maximally extended in that situation, thus providing maximal gastrocnemius stretch. Another potential limitation is the slightly—but not significantly—different age between the two groups.
Conclusions/implications
This study first showed the existence of a direct link between the degree of paresis—measured by the agonist motoneurone output—and the antagonist in the spastic paresis context. As plantar flexors are almost invariably contractured in chronic adult hemiparesis (Kwah et al. 2012), decreased dorsiflexor recruitment when the antagonist plantar flexor is stretched suggests that this phenomenon may occur with any pair of muscles around a joint in spastic paresis, when one is far more contractured than the other (e.g. finger flexors and extensors, pronators and supinators, etc.). If such a generalization proves true in future studies, there is additional incentive for clinicians to ascribe higher priority to desensitizing spindles by lengthening contractured muscles. Antagonist lengthening might thus both decrease its spastic co-contraction and increase voluntary agonist recruitment.
References
Abbruzzese G, Morena M, Spadavecchia L, Schieppati M (1994) Response of arm flexor muscles to magnetic and electrical brain stimulation during shortening and lengthening tasks in man. J Physiol 481:499–507
Basmajian JV, Blumenstein R (1980). Electrode placement in EMG biofeedback. Williams & Wilkins, Baltimore
Bourbonnais D, Vanden Noven S (1989) Weakness in patients with hemiparesis. Am J Occup Ther 43:313–319
Bourbonnais D, Vanden Noven S, Carey KM, Rymer WZ (1989) Abnormal spatial patterns of elbow muscle activation in hemiparetic human subjects. Brain 112:85–102
Cafarelli E, Bigland-Ritchie B (1979) Sensation of static force in muscles of different length. Exp Neurol 65:511–525
Cain WS, Stevens JC (1971) Effort in sustained and phasic handgrip contractions. Am J Psychol 84:52–65
Canning CG, Ada L, O’Dwyer NJ (2000) Abnormal muscle activation characteristics associated with loss of dexterity after stroke. J Neurol Sci 176:45–56
Carey LM, Oke LE, Matyas TA (1996) Impaired limb position sense after stroke: a quantitative test for clinical use. Arch Phys Med Rehabil 77:1271–1278
Cody FW, Richardson HC, MacDermott N, Ferguson IT (1987) Stretch and vibration reflexes of wrist flexor muscles in spasticity. Brain 110:433–450
Dewald JP, Pope PS, Given JD, Buchanan TS, Rymer WZ (1995) Abnormal muscle coactivation patterns during isometric torque generation at the elbow and shoulder in hemiparetic subjects. Brain 118:495–510
Dietz V, Quintern J, Berger W (1981) Electrophysiological studies of gait in spasticity and rigidity. Evidence that altered mechanical properties of muscle contribute to hypertonia. Brain 104:431–449
Dietz V, Ketelsen UP, Berger W, Quintern J (1986) Motor unit involvement in spastic paresis. Relationship between leg muscle activation and histochemistry. J Neurol Sci 75:89–103
Edström L (1970) Selective changes in the sizes of red and white muscle fibres in upper motor lesions and Parkinsonism. J Neurol Sci 11:537–550
Eisler H (1962) Subjective scale of force for a large muscle group. J Exp Psychol 64:253–257
el-Abd MA, Ibrahim IK, Dietz V (1993) Impaired activation pattern in antagonistic elbow muscles of patients with spastic hemiparesis: contribution to movement disorder. Electromyogr Clin Neurophysiol 33:247–255
Gandevia SC, McCloskey DI (1977a) Effects of related sensory inputs on motor performances in man studied through changes in perceived heaviness. J Physiol 272:653–672
Gandevia SC, McCloskey DI (1977b) Sensations of heaviness. Brain 100:345–354
Gioux M, Petit J (1993) Effects of immobilising the cat peroneus longus muscle on the activity of its own spindles. J Appl Physiol 75:2629–2635
Gracies JM (2005) Pathophysiology of spastic paresis. II: emergence of muscle overactivity. Muscle Nerve 31:552–571
Gracies JM, Wilson L, Gandevia SC, Burke D (1997) Stretched position of spastic muscles aggravates their co-contraction in hemiplegic patients. Ann Neurol 42:438–439
Gracies JM, Burke K, Clegg NJ, Browne R, Rushing C, Fehlings D et al (2010) Reliability of the Tardieu scale for assessing spasticity in children with cerebral palsy. Arch Phys Med Rehabil 91:421–428
Heckmann CJ, Gorassini MA, Bennett DJ (2005) Persistent inward currents in motoneurone dendrites: implications for motor output. Muscle Nerve 31:135–156
Henneman E (1985) The size-principle: a deterministic output emerges from a set of probabilistic connections. J Exp Biol 115:105–112
Holmes G (1917) The symptoms of acute cerebellar injuries due to gunshot injuries. Brain 40:461–535
Hu X, Tong K, Tsang VS, Song R (2006) Joint-angle-dependent neuromuscular dysfunctions at the wrist in persons after stroke. Arch Phys Med Rehabil 87:671–679
Hultborn H, Brownstone RB, Toth TI, Gossard JP (2004) Key mechanisms for setting the input-output gain across the motoneurone pool. Prog Brain Res 143:77–95
Huskisson EC (1974) Measurement of pain. Lancet 2:1127–1131
Ikeda AJ, Abel MF, Granata KP, Damiano DL (1998) Quantification of cocontraction in spastic cerebral palsy. Electromyogr Clin Neurophysiol 38:497–504
Inman VT, Ralston HJ, Saunders JB, Feinstein B, Wright EW Jr (1952) Relation of human electromyogram to muscular tension. Electroencephalogr Clin Neurophysiol 4:187–194
Jones LA (1986) Perception of force and weight: theory and research. Psychol Bull 100:29–42
Jones LA, Hunter IW (1983) Effect of fatigue on force sensation. Exp Neurol 81:640–650
Jones LA, Hunter IW (1985) Effect of muscle tendon vibration on the perception of force. Exp Neurol 87:35–45
Kamper DG, Rymer WZ (2001) Impairment of voluntary control of finger motion following stroke: role of inappropriate muscle coactivation. Muscle Nerve 24:673–681
Kamper DG, Harvey RL, Suresh S, Rymer WZ (2003) Relative contributions of neural mechanisms versus muscle mechanics in promoting finger extension deficits following stroke. Muscle Nerve 28:309–318
Knutsson E, Mårtensson A (1980) Dynamic motor capacity in spastic paresis and its relation to prime mover dysfunction, spastic reflexes and antagonist co-activation. Scand J Rehabil Med 12:93–106
Knutsson E, Richards C (1979) Different types of disturbed motor control in gait of hemiparetic patients. Brain 102:405–430
Komi PV, Buskirk ER (1972) Effect of eccentric and concentric muscle conditioning on tension and electrical activity of human muscle. Ergonomics 15:417–434
Koo TK, Mak AF, Hung L, Dewald JP (2003) Joint position dependence of weakness during maximum isometric voluntary contractions in subjects with hemiparesis. Arch Phys Med Rehabil 84:1380–1386
Kwah LK, Herbert RD, Harvey LA, Diong J et al (2012) Passive mechanical properties of gastrocnemius muscles of people with ankle contracture after stroke. Arch Phys Med Rehabil 93:1185–1190
Levin MF, Selles RW, Verheul MH, Meijer OG (2000) Deficits in the coordination of agonist and antagonist muscles in stroke patients: implications for normal motor control. Brain Res 853:352–369
Marchand-Pauvert V, Mazevet D, Nielsen J, Petersen N, Pierrot-Deseilligny E (2000) Distribution of non-monosynaptic excitation to early and late recruited units in human forearm muscles. Exp Brain Res 134:274–278
Marque P, Simonetta-Moreau M, Maupas E, Roques CF (2001) Facilitation of transmission in heteronymous group II pathways in spastic hemiplegic patients. J Neurol Neurosurg Psychiatry 70:36–42
Marsh E, Sale D, McComas AJ, Quinlan J (1981) Influence of joint position on ankle dorsiflexion in humans. J Appl Physiol 51:160–167
McCloskey DI, Ebeling P, Goodwin GM (1974) Estimation of weights and tensions and apparent involvement of a “sense of effort”. Exp Neurol 42:220–232
McCloskey DI, Colebatch JG, Potter EK, Burke D (1983) Judgements about onset of rapid voluntary movements in man. J Neurophysiol 49:851–863
Mottram CJ, Suresh NL, Heckman CJ, Gorassini MA, Rymer WZ (2009) Origins of abnormal excitability in biceps brachii motoneurons of spastic-paretic stroke survivors. J Neurophysiol 102:2026–2038
Newman SA, Jones G, Newham DJ (2003) Quadriceps voluntary activation at different joint angles measured by two stimulation techniques. Eur J Appl Physiol 89:496–499
Pierrot-Deseilligny E, Burke D (2005) The circuitry of the human spinal cord: its role in motor control and movement disorders. Cambridge University Press, Cambridge
Roland PE, Ladegaard-Pedersen H (1977) A quantitative analysis of sensations of tension and of kinaesthesia in man. Evidence for a peripherally originating muscular sense and for a sense of effort. Brain 100:671–692
Sahrmann SA, Norton BJ (1977) The relationship of voluntary movement to spasticity in the upper motor neuron syndrome. Ann Neurol 2:460–465
Sekiguchi H, Kimura T, Yamanaka K, Nakazawa K (2001) Lower excitability of the corticospinal tract to transcranial magnetic stimulation during lengthening contractions in human elbow flexors. Neurosci Lett 312:83–86
Sekiguchi H, Nakazawa K, Suzuki S (2003) Differences in recruitment properties of the corticospinal pathway between lengthening and shortening contractions in human soleus muscle. Brain Res 977:169–179
Simon AM, Kelly BM, Ferris DP (2009) Sense of effort determines lower limb force production during dynamic movement in individuals with poststroke hemiparesis. Neurorehabil Neural Repair 23:811–818
Simonetta-Moreau M, Marque P, Marchand-Pauvert V, Pierrot-Deseilligny E (1999) The pattern of excitation of human lower limb motoneuronees by probable group II muscle afferents. J Physiol 517:287–300
Solomon NP, Robin DA (2005) Perceptions of effort during handgrip and tongue elevation in Parkinson’s disease. Parkinsonism Relat Disord 11:353–361
Stevens JC, Cain WS (1970) Effort in isometric muscular contractions related to force level and duration. Percept Psychophys 8:240–244
Tardieu G (1966) Evaluation et caractères distinctifs des diverses raideurs d’origine cérébrale. In: Association Nationale des IMC (Ed) Chapitre VB1b Les feuillets de l’infirmité motrice cérébrale. Paris, pp 1–28
Tyson SF, Crow JL, Connell L, Winward C, Hillier S (2013) Sensory impairments of the lower limb after stroke: a pooled analysis of individual patient data. Top Stroke Rehabil 20:441–449
Van Reeth C, Pauwels C, Bayle N, Loche CM, Gracies JM (2013a) Predominant factors of motor deficiencies in adult spastic paresis: infant vs adult-acquired lesions. Ann Phys Rehabil Med 56(S1):e385–e386
Van Reeth C, Pauwels C, Bayle N, Loche CM, Gracies JM (2013b) Correlation between muscle length, spasticity and motor weakness in adult spastic paresis: infant vs adult-acquired lesions. Ann Phys Rehabil Med 56(S1):e404–e405
Vinti M, Couillandre A, Hausselle J et al (2013) Influence of effort intensity and gastrocnemius stretch on co-contraction and torque production in the healthy and paretic ankle. Clin Neurophysiol 124:528–535
Visser SL, Aanen A (1981) Evaluation of EMG parameters for analysis and quantification of hemiparesis. Electromyogr Clin Neurophysiol 21:591–610
Woods JJ, Bigland-Ritchie B (1983) Linear and non-linear surface EMG/force relationships in human muscles. An anatomical/functional argument for the existence of both. Am J Phys Med 62:287–299
Conflict of interest
Dr Gracies served as a consultant and received research Grant support from Allergan, Ipsen, and Merz. Drs Vinti, Bayle, Hutin and Burke have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vinti, M., Bayle, N., Hutin, E. et al. Stretch-sensitive paresis and effort perception in hemiparesis. J Neural Transm 122, 1089–1097 (2015). https://doi.org/10.1007/s00702-015-1379-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-015-1379-3