Abstract
In this study, the quotients (Q) between metal concentrations in cerebrospinal fluid (CSF) and plasma were studied in subjects with Alzheimer’s disease (AD) and referents to investigate if the leakage through the blood–CSF barrier (BCB) increased with increased duration and severity of the disease. Concentrations of 18 metals (Mg, Ca, Mn, Fe, Co, Ni, Cu, Zn, Se, Rb, Sr, Mo, Cd, Sn, Sb, Cs, Hg, and Pb) were determined by ICP-MS in plasma and cerebrospinal fluid in 264 patients with AD, and in 54 healthy referents. The quotients Q Mn, Q Rb, Q Sb, Q Pb and Q Hg were significantly lower (p ≤ 0.003) and Q Co significantly higher (p ≤ 0.001) in subjects with AD as compared with the controls. Subjects in a subgroup with more severe AD, showed the same pattern. The metal leakage into CSF did not increase with increased duration and/or severity of the disease. The permeability of BCB varied considerably between the studied metals with low median quotients (Q ≤ 0.02) for Cd, Cu, Sb, Se and Zn and higher median quotients for Ca (Q ~ 0.5) and Mg (Q ~ 1.3), probably partly depending on differences in size and lipophilicity of metal–carrier complexes and specific carrier mechanisms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The blood–CSF barrier (BCB) has an important role in CNS for maintaining homeostasis. The lipophilicity and the size of the substance are of importance for the passage through the barrier, so also facilitated diffusion and specific carrier mechanisms (Zheng et al. 2003). The choroidal epithelium is part of the blood–CSF barrier and forms a monolayer between the choroidal blood flow and the CSF flow (Szmydynger-Chodobska et al. 1994). Several transporter mRNAs seem to be expressed in choroid plexus (Choudhuri et al. 2003). Some metals such as mercury and cadmium may directly harm the choroid plexus structure. Another point of attack is by impairment of specific regulatory pathways that are critical to brain development and function, e.g., manganese interaction with iron in the choroid plexus. Thirdly, metals like iron, silver, and gold may be sequestered by the choroid plexus as an essential CNS defense mechanism (Zheng 2001).
A number of essential metals are needed for optimal CNS function, e.g., calcium, copper, magnesium, manganese, iron, zinc, cobalt, and molybdenum. A series of active or receptor-mediated transport systems serve to control the transport of these metals into the brain. These membrane transporters are often quite substrate-specific.
Transporters seem to mediate the influx of the Mn2+ ion, Mn citrate and Mn Tf. The effect of Mn uptake is influenced by dietary iron intake and stores since these two metals compete for transferrin in serum and subsequent transport systems. The lateral plexus choroideus sequesters mercury, and also Cd, As, and Pb. This is probably an important mechanism to protect the CSF and the brain from fluxes of heavy metals in the blood (Zheng et al. 1991).
In a previous study, the CSF concentrations of about 20 metals were determined in CSF in subjects with Alzheimer’s disease (AD) and Alzheimer’s disease with minor vascular components (ADMV) (Gerhardsson et al. 2008). A comparison with healthy controls was made. In CSF, the levels of vanadium, manganese, rubidium, antimony, cesium, and lead were significantly lower among subjects with AD (p ≤ 0.010) and ADMV (p ≤ 0.047) than in controls. In a following study, the metal concentrations in CSF were related to the levels of well-known Alzheimer markers in CSF such as Aβ, total-tau (T-tau) and phosphorylated-tau (P-tau). In subjects with severe AD, CSF-Aβ showed strong positive correlations with CSF-Cs, while CSF-P-tau and CSF-T-tau both showed strong negative correlations with CSF-Cs (Gerhardsson et al. 2009).
The aim of this study is to investigate the quotients between metal concentrations in CSF versus plasma in subjects with AD, who are compared with healthy controls. An increased quotient with increased length and severity of the disease may implicate an increased leakage through the BCB, as the disease aggravates.
Methods
Subjects
The study group comprised 264 patients with a clinical diagnosis of AD (n = 264; 85 males, 179 females) from the Malmo Alzheimer study. These 264 subjects had no medical history of kidney disease and could not be classified as having either vascular dementia according to the DSM-IV criteria or mixed dementia. They did not display an abnormal executive control function that was severe enough to interfere with social or occupational functioning. At the time of the lumbar puncture, none of the patients was treated with cholinesterase inhibitors or memantine.
The subjects were all outpatients at the Neuropsychiatric Clinic, Malmo University Hospital, Malmo, Sweden. They had all gone through a clinical investigation of dementia during the time-period 1999–2003. Diagnostic criteria used were NINCDS–ADRDA (McKhann et al. 1984) for probable Alzheimer’s disease and Diagnostic and Statistical Manual of Mental Disorders from 1994 by American Psychiatric Association (DSM-IV) for vascular dementia (American Psychiatric Association 1994). None fulfilled the stricter NINDS–AIREN diagnostic criteria for vascular dementia (Roman et al. 1993). Only AD patients showing mild and moderate disease and with a complete investigation including sampling of cerebrospinal fluid (CSF) were selected to participate in the study. Other forms of dementia and psychiatric diseases explaining the cognitive decline were not included. Lumbar function was seldom performed during the investigation of subjects with severe AD. Accordingly, these patients were not included in the study population, as they did not fulfill the inclusion criteria. The diagnosis was given prospectively as part of a clinical routine by different doctors employed at the neuropsychiatric clinic, and later reviewed by the study doctors (EL, LM). Of the 274 original patients, 10 patients diagnosed as having Lewy body dementia were not included in the study. The other 264 patients diagnosed as having Alzheimer’s disease participated in our study.
The normal healthy controls (n = 54; 18 males, 36 females) were recruited through advertisements at senior clubs and among relatives to health care personnel. No matching was performed regarding education and/or premorbid IQ. The first selection was made through telephone interviews. Volunteers went through physical examination and cognitive testing. They had no medical history of kidney disease. Inclusion criteria were a Mini-Mental State Examination (MMSE) (Folstein et al. 1975) test result of 28 or above and an Alzheimer’s Disease Assessment Scale (ADAS-cog) (Mohs et al. 1983) test result of 12 or below. Controls showing mild cognitive impairment, e.g., cognitive complaints from the patients or their families, decline in cognitive functioning during the last year, cognitive disorders, activities of daily living preserved, absence of dementia (Tian et al. 2008), dementia or other mental or physical illness, which could affect the cognitive status, did not pass the inclusion criteria. Accordingly, they were not included in the reference population (Stomrud et al. 2007).
The complete investigation included anamnestic data, physical and neuropsychiatric examination, tests of cognitive function, blood and CSF sampling, computerized tomography (CT), regional cerebral blood flow (rCBF), electrocardiogram (ECG), blood pressure measurements and routine laboratory tests, including the determination of apolipoprotein E (ApoE) genotype and albumin CSF/serum ratio.
Sampling of blood and cerebrospinal fluid
Lumbar puncture was performed in the sitting position in all patients. The CSF samples were obtained by lumbar puncture in the L3/L4 or L4/L5 interspace. The first mL of CSF was thrown away, 1 mL was sent for cell analysis, and 10 mL was collected in plastic (polypropylene) tubes. All CSF samples were mixed gently to avoid possible gradient effects. No CSF sample contained more than 500 erythrocytes/μL. The CSF samples were centrifuged at 2,000×g at 4°C for 10 min to eliminate cells and other insoluble material, and were then immediately deep frozen and stored at −80°C pending biochemical analyses. At the same time, the plasma and serum samples were collected. For plasma, blood was collected in tubes containing EDTA (B-D Vacutainer System, Franklin Lakes, NJ, USA), and centrifuged at 2,000×g at 4°C for 10 min. The aliquots were immediately frozen at −80°C and stored until assayed. The study was approved by the ethics committee of Lund University.
Metal analysis
Analytical methods
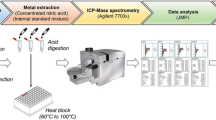
All metals, but mercury, in plasma and cerebrospinal fluid were determined by inductively coupled plasma-mass spectrometry (ICP-MS; Thermo X7; Thermo Elemental, Winsford, UK). The samples were diluted five times with an alkaline solution according to Bárány et al. (1997). External matrix-matched calibration samples were used for the element quantification.
All samples were analyzed in peak jump mode. Interference corrections were made for 114Cd for the spectral overlap of 114Sn. The limits of detection (LOD) were calculated as three times the standard deviation (SD) for the blank (Gerhardsson et al. 2008). To ensure the accuracy of the analytical methods and results, quality control (QC) samples were analyzed along with the collected samples. In the ICP-MS analysis, Seronorm Trace Elements Serum Lot MI0181 (Nycomed Pharma, Oslo, Norway) was used. The obtained values for the QC samples showed good agreement with the recommended concentrations.
The determination of total mercury (T-Hg; inorganic Hg + organic Hg) was made in acid-digested samples by cold vapor atomic fluorescence spectrometry (Sandborg-Englund et al. 1998). The LOD calculated as three times the SD for the blanks were 0.21 μg/L. The analytical accuracy was checked against reference material. The results obtained were 1.8 ± 0.27 μg/L (mean ± SD), n = 38 versus the recommended range 1.7–2.4 μg/L (Seronorm; batch OK0336, Nycomed Pharma, Oslo, Norway).
Statistics
As most of the variables showed a skewed distribution (checked by Normal Probability Plots), non-parametric statistical processing was applied (Kruskal–Wallis one-way analysis of variance, Mann–Whitney’s U test, Spearman’s correlation coefficients) (Altman 1991). A value of p < 0.05 was regarded as statistically significant (two-tailed tests).
The flexibility and power of parametric methods were used to further analyze the material. We used stepwise multiple regression to find the best subset of variables to jointly explain the severity of the disease as expressed by ADAS-cog and MMSE-figures. The p values used to include of exclude the variables in the stepwise process were 0.05 and 0.10, respectively. All calculations were performed using the Statistical Package for the Social Sciences (SPSS v 18.0).
Results
Median values and ranges of the quotients between metal concentrations in CSF and plasma are presented in Table 1. The quotients Q Mn, Q Rb, Q Sb, Q Pb and Q Hg were significantly lower in subjects with AD (p ≤ 0.003) as compared with the controls. Q Co was the only quotient that was significantly higher in subjects with AD (p < 0.001) as compared with healthy controls.
When selecting subjects with more severe AD, patients with ADAS-cog subscale 70 (ADAS-cog 70) ≥ 18 and APOε4/4 were chosen. This AD subgroup (N = 20) showed basically the same pattern as for the total material with significantly lower (p ≤ 0.024) Q Mn, Q Rb, Q Sb, Q Pb and Q Hg than the healthy controls. As for the total material, this subgroup had a significantly higher (p = 0.003) Q Co than the reference group. The albumin quotient (CSF-albumin/serum albumin × 1,000) did not differ significantly between subjects with AD or subjects within the AD subgroup on the one hand and healthy controls on the other (c.f. Table 1).
Correlation coefficients
To avoid the multicomparison problem, only the quotients that differed significantly between AD cases and healthy controls were used for further analyses. The strongest correlations in the total AD material was observed between Q Pb and Q Mn (r s = 0.30; p < 0.001), Q Pb and Q Sb (r s = 0.27; p < 0.001) and between Q Mn and Q Rb (r s = 0.25; p < 0.001). Weaker correlations were observed between Q Co and Q Sb, Q Co and Q Pb and between Q Mn and Q Sb (r s = 0.13–0.16; p ≤ 0.039). In the AD subgroup, considerably stronger correlation coefficients were observed between, e.g., Q Pb and Q Rb (r s = 0.53; p = 0.018), Q Pb and Q Sb (r s = 0.52; p = 0.019), Q Mn and Q Rb (r s = 0.63; p = 0.003; Fig. 1, R 2 linear = 0.26), and Q Mn and Q Co (r s = 0.58; p = 0.007).
Regression analysis
In a next step, multiple linear regression analyses were performed with ADAS-cog (70) or MMSE as dependent variables and with age at time of the study, duration of the disease, gender, APOE and metal quotients (Q Mn, Q Co, Q Sb, Q Rb, Q Hg or Q Pb) as independent variables. None of the metal quotients, however, were included in the models. The outcome was similar when using ADAS-cog (70) or MMSE as dependent variables. Thus, the metal quotients investigated did not make a significant contribution to the model when looking at the severity of the disease.
Discussion
In a previous study (Gerhardsson et al. 2008), the CSF concentrations of vanadium, manganese, rubidium, antimony, cesium, and lead were significantly lower in subjects with AD (N = 264; p ≤ 0.007) as compared with the healthy controls. In analogy with these findings, the corresponding quotients between the metal concentrations in CSF versus plasma of manganese, rubidium, antimony, and lead, as well as Q Hg were significantly lower in subjects with AD as compared with controls. On the other hand, the CSF/plasma quotient for cobalt showed an increase in subjects with AD as compared with healthy controls.
In a next step, subjects with a more severe AD (AD subgroup) were selected. The pattern of the corresponding quotients in this subgroup (N = 20), however, was very similar to the pattern in the total material, with significantly lower quotients for manganese, rubidium, antimony, lead and mercury and with a significantly higher quotient for cobalt (Table 1). This consistency reduces the risk of making a type I error.
Transporters through the choroidal epithelium for major essential metals such as calcium, iron, and zinc can also mediate the transport of non-essential metals (Bressler et al. 2007). One example is the intestinal iron transporter divalent metal transporter 1 that also mediates the uptake of lead and cadmium. The levels of essential metals are strictly regulated by these transporters to prevent injuries that could result from oxidative damage induced by an increased uptake of, e.g., iron, zinc, and copper (Bressler et al. 2007).
Metals can affect the choroid plexus in different ways. Metals like mercury and cadmium may directly damage the choroid plexus. Another point of attack is a selective choroid plexus toxicant that can impair specific regulatory pathways that are critical to brain function, e.g., the lead-induced alteration in transthyretin production and secretion. Thirdly, a sequestered choroid plexus toxicant, such as iron, silver, or gold, may be sequestered by the choroid plexus as an essential CNS defense mechanism (Zheng 2001).
Several protective mechanisms at the BCB-level may prevent an individual from increased exposures to heavy metals and other toxicants. These gatekeepers may be subject to harmful attacks from heavy metals, thereby increasing the risk for metal-induced neurotoxicity. Presumably, a degradation of these barriers would increase the influx of potentially toxic metals to the CSF as well as to the brain. In this study however, only the quotient CSF-Co/P-Co was significantly higher in of AD subjects as compared to the healthy controls. The other quotients were of the same magnitude in AD subjects and healthy controls with the exception of the quotients for manganese, rubidium, antimony, lead and mercury that were significantly lower among the cases. This is in accordance with a previous study (Gerhardsson et al. 2008) showing significantly lower CSF concentrations of, e.g., manganese, rubidium, antimony, and lead in AD subjects as compared with controls.
The publication of CSF-metal data in literature is limited. Recently, however, Nischwitz et al. (2008) studied serum and CSF concentrations of manganese, iron, copper, zinc, magnesium, and calcium in 29 patients with unspecified neurological complaints, e.g., headache, dizziness, and sensory symptoms, at a neurology department in München. The mean CSF–serum metal ratios in their study were 0.7 for Mn, 0.02 for Fe, 0.02 for Cu, 0.03 for Zn, 1.3 for Mg and 0.5 for Ca, which are comparable to the figures in our study. The findings indicate that the permeability of the BCB varies considerably for different metals. Copper, zinc and iron seem to be retained by the barrier to prevent the brain from excessive exposure. Calcium and magnesium, which are required in higher amounts for optimal brain function, seem to pass the BCB easier. Differences in the lipophilicity of the metals after complex-binding to carriers and specific carrier mechanisms may explain part of the differences in metal transports through the BCB. For manganese, the influx of Mn-compounds seems to be mediated by transporters while the efflux seems to be mediated by diffusion. Accordingly, repeated and increased Mn exposure may cause accumulation in the brain of Mn over time (Yokel 2006). Another example is methyl mercury (MeHg), which can bind to the amino acid cysteine. The MeHg–cysteine complex is then treated as an amino acid analog, which can pass the barrier by the L system carrier for neutral amino acids (Aschner and Clarkson 1988).
The metal concentrations in SCF and plasma in our control group were of the same magnitude as the values observed in a reference group that was used in a study by Forte et al. (2004) comparing metal concentrations of, e.g., Ca, Cu, Fe, Mg, Mn, and Zn in CSF and serum in patients with Parkinson’s disease with the levels in age-matched controls.
Conclusion
In summary, the CSF/plasma quotients for Mn, Rb, Sb, Pb, and Hg were significantly lower in subjects with AD as compared with the healthy controls. The CSF/plasma ratio for Co was the only quotient that was significantly higher among the cases. The same pattern was observed in subjects in the subgroup with more severe AD. In this subgroup, the strongest correlation coefficients were noted between Q Pb and Q Rb, Q Pb and Q Sb, Q Mn and Q Rb, and Q Mn and Q Co. Thus, we did not observe an increased leakage of these metals into CSF with increased duration and/or severity of AD. In analogy with this finding, the albumin quotients were of the same magnitude when comparing subjects with AD or the subgroup with more severe AD with healthy controls.
Furthermore, the permeability of BCB seems to vary considerably between the studied metals. Low quotients were noted for antimony, copper, zinc, selenium, and cadmium, while higher quotients were observed for, e.g., calcium and magnesium. Homeostatic mechanisms for essential metals, differences in size and lipophilicity of metal–carrier complexes, and specific carrier mechanisms can explain some of these differences.
References
Altman DG (1991) Practical statistics for medical research. Chapman & Hall, London
American Psychiatric Association (1994) Diagnostic and statistical manual of psychiatric disorders, 4th edn (DSM IV). American Psychiatric Association, Washington
Aschner M, Clarkson TW (1988) Distribution of mercury 203 in pregnant rats and their fetuses following systemic infusions with thiol-containing amino acids and glutathione during late gestation. Teratology 38:145–155
Bárány E, Bergdahl IA, Schütz A, Skerfving S, Oskarsson A (1997) Inductively coupled plasma mass spectrometry for direct multi-element analysis of diluted human blood and serum. J Anal Atomic Spectrom 12:1005–1009
Bressler JP, Olivi L, Cheong JH, Kim Y, Maerten A, Bannon D (2007) Metal transporters in intestine and brain: their involvement in metal-associated neurotoxicities. Hum Exp Toxicol 26:221–229
Choudhuri S, Cherrington NJ, Li N, Klaassen CD (2003) Constitutive expression of various xenobiotic and endobiotic transporter mRNAs in the choroid plexus of rats. Drug Metab Dispos 31:1337–1345
Folstein MF, Folstein SE, McHugh PR (1975) “Mini mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Forte G, Bocca B, Senofonte O, Petrucci F, Brusa L, Stanzione P et al (2004) Trace and major elements in whole blood, serum, cerebrospinal fluid and urine of patients with Parkinson’s disease. J Neural Transm 111:1031–1040
Gerhardsson L, Lundh T, Minthon L, Londos E (2008) Metal concentrations in plasma and cerebrospinal fluid in patients with Alzheimer’s disease. Dement Geriatr Cogn Disord 25:508–515
Gerhardsson L, Blennow K, Lundh T, Londos E, Minthon L (2009) Concentrations of metals, β-amyloid and tau-markers in cerebrospinal fluid in patients with Alzheimer’s disease. Dement Geriatr Cogn Disord 28:88–94
McKhann G, Drachmann D, Folstein M, Kattzman R, Price D, Stadlan EM (1984) Clinical diagnosis of Alzheimer’s disease: report of the NINCDS–ADRDA Work group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s disease. Neurology 34:939–944
Mohs RC, Rosen WG, Davis KL (1983) The Alzheimer’s disease assessment scale: an instrument for assessing treatment efficacy. Psychopharmacol Bull 19:448–450
Nischwitz V, Berthele A, Michalke B (2008) Speciation analysis of selected metals and determination of their total contents in paired serum and cerebrospinal fluid samples: an approach to investigate the permeability of the human blood–cerebrospinal fluid-barrier. Anal Chim Acta 627:258–269
Roman GC, Tatemichi TK, Erkinjuntti T, Cummings JL, Masdeu JC, Garcia JH et al (1993) Vascular dementia: diagnostic criteria for research studies. Report of the NINDS–AIREN International Workshop. Neurology 43:250–260
Sandborg-Englund G, Elinder CG, Langworth S, Schütz A, Ekstrand J (1998) Mercury in biological fluids after amalgam removal. J Dent Res 77:615–624
Stomrud E, Hansson O, Blennow K, Minthon L, Londos E (2007) Cerebrospinal fluid biomarkers predict decline in subjective cognitive function over 3 years in healthy elderly. Dement Geriatr Cogn Disord 24:118–124
Szmydynger-Chodobska J, Chodobski A, Johanson CE (1994) Postnatal developmental changes in blood flow to choroid plexuses and cerebral cortex of the rat. Am J Physiol 266(5 Pt 2):R1488–R1492
Tian JZ, Shi J, Zhang XQ, Bi Q, Ma X, Wang ZL et al (2008) Guiding principles of clinical research on mild cognitive impairment (protocol). Zhong Xi Yi Jie He Xue Bao 6:9–14 In Chinese
Yokel RA (2006) Blood–brain barrier flux of aluminum, manganese, iron and other metals suspected to contribute to metal-induced neurodegeneration. J Alzheimer’s Disease 10:223–253
Zheng W (2001) Toxicology of choroid plexus: special reference to metal-induced neurotoxicities. Microsc Res Tech 52:89–103
Zheng W, Perry DF, Nelson DL, Aposhian HV (1991) Choroid plexus protects cerebrospinal fluid against toxic metals. FASEB J 5:2188–2193
Zheng W, Aschner M, Ghersi-Egea JF (2003) Brain barrier systems: a new frontier in metal neurotoxicological research. Toxicol Appl Pharmacol 192:1–11
Conflict of interest
Neither my co-authors nor I have any conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gerhardsson, L., Lundh, T., Londos, E. et al. Cerebrospinal fluid/plasma quotients of essential and non-essential metals in patients with Alzheimer’s disease. J Neural Transm 118, 957–962 (2011). https://doi.org/10.1007/s00702-011-0605-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-011-0605-x