Abstract
Alterations in hippocampus frequently occur following bacterial meningitis, despite antibiotic treatment. We investigated the cognitive performance in rats submitted to bacterial meningitis after 10, 30, and 60 days. To this aim, we utilized male Wistar rats submitted to either sham (control) or meningitis by Streptococcus pneumoniae, and followed by the initiation of the antibiotic treatment at 16 h after inoculation. The animals underwent six behavioral tasks 10, 30 and 60 days after surgery. We demonstrated that some of the learning and memory impairment, demonstrated 10 days after the induction of meningitis, persists up to 30 days, but not 60 days after induction.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bacterial meningitis caused by Streptococcus pneumoniae is a common disease worldwide consisting of a severe infection of the central nervous system, and remains associated with high mortality and morbidity rates despite the advances made in antimicrobial therapy over the past decades (Schuchat et al. 1997; Merkelbach et al. 2000). The estimated annual incidence of bacterial meningitis is 4–6 per 100,000 adults (Hoogma et al. 2007). Moreover, impairment of learning and memory occur in up to 50% of the survivors (Weisfelt et al. 2006a, b; Hoogma et al. 2007).
In addition, patients after pneumococcal meningitis have a higher rate of cognitive dysfunction (Hoogma et al. 2007). One of the consequences of the massive inflammatory reaction in the experimental pneumococcal meningitis is the occurrence of neuronal apoptosis in the hippocampus and cortex (Braun et al. 1999; Grandgirard et al. 2007a, b), and the extent of hippocampal apoptosis correlates with the extent of learning dysfunction. For this reason, memory, learning, and alterations in the hippocampus were studied in animal model of pneumococcal meningitis and humans survivors (Grimwood et al. 1995; Nau et al. 1999; Braun et al. 1999; Wellmer et al. 2000; Leib et al. 2001; van de Beek et al. 2006). In humans, clinical studies assessing long-term outcome after bacterial meningitis indicate the importance of an impaired function of the hippocampal formation: in a retrospective survey on patients surviving bacterial meningitis 31% reported disturbances of attention and 24% memory deficits, which affected their ability to work (Bohr et al. 1984). In animal models, experimental pneumococcal meningitis in mice leads to long-term spatial learning deficits, thereby resembling the human disease (Wellmer et al. 2000).
However, there were not studies that evaluated the cognitive deficits, depression- and anxiety-like behavior during any time after induction aiming to verify time-dependent recovery on several cognitive deficits. Thus, we here present data regarding a time-dependent recovery on several cognitive deficits, and depression- and anxiety-like behavior in meningitis survivor rats.
Materials and methods
Animals
Male Wistar rats (3–4 months, 220–310 g) were obtained from our breeding colony (UNESC). The animals were housed five in a cage with food and water available ad libitum and maintained on a 12-h light/dark cycle (lights on at 7:00 a.m.). All experimental procedures involving animals were performed in accordance with the NIH Guide for the Care and Use of Laboratory Animals and the Brazilian Society for Neuroscience and Behavior (SBNeC) recommendations for animal care and with the approval of Ethics Committee from Universidade do Extremo Sul Catarinense, UNESC, through the protocol number 210/2008.
Meningitis model
All surgical procedures and bacteria administrations were performed under anesthesia consisting of an intraperitoneal (i.p.) administration of ketamine (6.6 mg/kg), xylazine (0.3 mg/kg), and acepromazine (0.16 mg/kg) (Irazuzta et al. 2002). S. pneumoniae (ATCC 6303) was cultured overnight in 10 mL Todd Hewitt broth medium, and grow for another 6 h (35°C, CO2 5.5%) and grown to logarithmic phase. The culture was centrifuged for 10 min at 5,000×g, and resuspended in sterile saline to the desired concentration and used for intracisternal injection (Irazuzta et al. 2002; Grandgirard et al. 2007a), containing 5 × 109 cfu/mL (Irazuzta et al. 2008; Barichello et al. 2009a, b, c). On day 1, the rats underwent a basilar cistern tap with a 23-gauge needle. The position of the needle was verified by the free flow of clear cerebrospinal fluid. Cerebrospinal fluid was withdrawn and the animals received either 10 µL of sterile saline as a control (sham) or an equivalent volume of the S. pneumoniae. At the time of inoculation, meningitis was documented by a quantitative culture of 5 µL of CSF obtained by puncture of the cisterna magna and cultured quantitatively on sheep blood agar plates. The number of bacteria in the CSF was determined by plating serial dilutions of CSF on blood agar plates at 18 h after inoculation and followed by the initiation of the antibiotic treatment in the groups described below (ceftriaxone 100 mg/kg twice a day, i.p.) (Leib et al. 2003; Grandgirard et al. 2007b) for 7 days.
To perform memory experiments, 140 animals underwent sham operation and the survival in this group was 100%. A total of 360 animals were submitted to meningitis; around 60% of these animals survived to perform behavioral tests. The death of the animals was within the first 5–7 days after meningitis, and those that survived were free from infection after 10 days with normal motor activity (data not shown).
Behavioral tests
The animals separately underwent six behavioral tasks: habituation to an open field, step-down inhibitory avoidance, continuous multiple trials step-down inhibitory avoidance task, object recognition, elevated plus-maze, and forced swimming test at 10, 30, and 60 days after induction. Thus, using this design, we do not assess time-dependent memory, but memory over time (with new training at each test session). All behavioral procedures were conducted between 01:00 and 04:00 p.m. in a sound-isolated room, and a single animal performed only one behavior test in only one time point after surgery. All behavioral tests were recorded by the same person who was blind to the animal group.
Habituation to an open field task
This task evaluates motor performance in the training section and non-associative memory in the retention test session. Habituation to an open field was carried out in a 40 × 60 cm open field surrounded by 50 cm high walls made of brown plywood with a frontal glass wall. The floor of the open field was divided into 12 equal rectangles by black lines. The animals were gently placed on the left rear quadrant and left to explore the arena for 5 min (training session). Immediately following this, the animals were taken back to their home cage and 24 h later submitted again to a similar open-field session (test session). Crossing of the black lines and rearing performed in both sessions were counted. The decrease in the number of crossings and rearings between the two sessions were taken as a measure of the retention of habituation (Tuon et al. 2008).
Step-down inhibitory avoidance task
This task evaluates aversive memory. The apparatus and procedures have been described in previous reports (Tuon et al. 2008). Briefly, the training apparatus was a 50 × 25 × 25 cm acrylic box (Albarsch, Porto Alegre, Brazil) whose floor consisted of parallel caliber stainless steel bars (1 mm diameter) spaced 1 cm apart. A 7 cm wide, 2.5 cm high platform was placed on the floor of the box against the left wall. In the training trial, animals were placed on the platform and their latency to step down on the grid with all four paws was measured with an automatic device. Immediately after stepping down on the grid, the animals received a 0.4 mA, 2.0 s foot shock and returned to their home cage. A retention test trial was performed 24 h after training (long-term memory). The retention test trial was procedurally identical to training, except that no foot shock was presented. The retention test step-down latency (maximum 180 s) was used as a measure of inhibitory avoidance retention.
Reactivity to the foot shock was evaluated in the same apparatus used for inhibitory avoidance, except that the platform was removed. Each animal was placed on the grid and allowed a 1-min habituation period prior to the start of a series of shocks (0.5 s) delivered at 10-s intervals. Shock intensities ranged from 0.1 to 0.5 mA in 0.1 mA increments. The adjustments in shock intensity were made in accordance to each animal’s response. The intensity was raised by 1 unit when no response occurred and lowered by 1 unit when a response was made. A “flinch” response was defined as withdrawal of one paw from the grid floor, and a “jump” response was defined as rapid withdrawal of three or four paws. Two measurements of the “flinch” threshold were made and then two measurements of the “jump” threshold were made. For each animal, the mean of the two scores for the flinch and the jump thresholds were calculated.
Continuous multiple trials step-down inhibitory avoidance task
This task evaluates aversive memory in the test section and learning when analyzing the number of training trials required for the acquisition criterion (see below). It was performed in the same step-down inhibitory avoidance apparatus; however, in the training session, the animal was placed on the platform and immediately after stepping down on the grid, received a 0.3 mA, 2.0 s foot shock. This procedure continued until the rat remained on the platform for 50 s. The animal was then returned to the home cage. The number of training trials required to reach the acquisition criterion of 50 s on the platform was recorded. The retention test was performed 24 h later (long-term memory) (Tuon et al. 2008).
Object recognition
This task evaluates non-aversive, non-spatial memory. The apparatus and procedures for the object recognition task have been described elsewhere (Tuon et al. 2008). Briefly, the task took place in a 40 × 50 cm open field surrounded by 50 cm high walls made of plywood with a frontal glass wall. The floor of the open field was divided into 12 equal rectangles by black lines. All animals were submitted to a habituation session where they were allowed to freely explore the open field for 5 min. No objects were placed in the box during the habituation trial. Crossings of the black lines and rearings performed in this session were evaluated as locomotors and exploratory activity, respectively. Different times after habituation, training was conducted by placing individual rats for 5 min in the field, in which two identical objects (objects A1 and A2, both being cubes) were positioned in two adjacent corners, 10 cm from the walls. In a short-term recognition memory test given 1.5 h after training, the rats explored the open field for 5 min in the presence of one familiar (A) and one novel (B, a pyramid with a square-shaped base) object. All objects had similar textures (smooth), colors (blue), and sizes (weight 150–200 g), but distinctive shapes. A recognition index calculated for each animal is reported as the ratio TB/(TA + TB) (TA = time spent exploring the familiar object A; TB = time spent exploring the novel object B). In a long-term recognition memory test given 24 h after training, the same rats were allowed to explore the field for 5 min in the presence of the familiar object A and a novel object C (a sphere with a square-shaped base). Recognition memory was evaluated as done for the short-term memory test. Exploration was defined as sniffing (exploring the object 3–5 cm away from it) or touching the object with the nose and/or forepaws.
Elevated plus-maze
The apparatus used in animal models for anxiety has been described in detail elsewhere (Tuon et al. 2008). Briefly, the apparatus consisted of two open arms (50 × 9 × 10 cm) and two closed arms (50 × 9 × 10 × 9 × 40 cm) arranged in such a way that the two arms of each type were opposite to each other, with a central platform (5 × 9 × 5 cm). The maze’s height was 50 cm and the tests were conducted under dim red light. Animals were exposed for 5 min to the red light in their own home cages before the testing procedure. Next, they were placed individually on the central platform of the plus-maze facing an open arm. During a 5-min test period, the following measurements were recorded by two observers: the number of entries, the time spent in the open and closed arms, and the total number of arm entries.
Forced swimming test
The test was conducted according to the previous reports (Tuon et al. 2008), and was used as a model for depressive behavior. Briefly, the test involves two exposures to a cylindrical water tank in which rats cannot touch the bottom or from which they cannot escape. The tank is made of transparent plexiglass, 80 cm tall, 30 cm in diameter, and filled with water (22–23°C) to a depth of 40 cm. Water in the tank was changed for each rat. For the first exposure, the rats were placed in the water for 15 min (pre-test session). After 24 h, the rats were placed in the water again for a 5-min session (test session). The periods of immobility were analyzed. The rats were judged to be immobile whenever they stopped swimming and remained floating in the water, with their head just above water level.
Statistical analysis
Data for the elevated plus-maze and forced swimming tests are reported as mean ± SD, and were analyzed by the Student’s t test. Unpaired t tests were performed on the flinch and jump scores, comparing the sham and meningitis groups. Data from the inhibitory avoidance task, object recognition task and the number of training trials from continuous multiple trials step-down inhibitory avoidance are reported as median and interquartile ranges, and comparisons among groups were performed using Mann–Whitney U tests. The within-individual groups were analyzed by Wilcoxon’s tests. In all comparisons, p < 0.05 indicated statistical significance.
Results
In the behavior tests that did not present impairments on 10 or 30 days after meningitis, we did not perform the 60-day analyses (to avoid unnecessary use of experimental animals).
Habituation to an open-field task
In the open-field task, there were no differences in the number of crossings and rearings between groups in the habituation to the open-field training session (p > 0.05) demonstrating no difference in motor and exploratory activity between groups. In the test session, there was a significant reduction in both crossings and rearings of the sham group as compared to the meningitis group at 10 (crossing t = 9.649, df = 9, p = 0.0001; rearings t = 6.680, df = 9, p = 0.0001) and 30 days (crossing t = 3.061, df = 9, p = 0.008; rearings t = 4.594, df = 9, p = 0.0001) (suggesting memory impairment), but not 60 days after meningitis (Fig. 1).
Habituation to an open-field test. Animals were submitted to either meningitis or sham. They underwent the training test on the open-field task 10, 30, and 60 days after induction, and were tested 24 h later. Data are presented as mean ± SEM, n = 10 rats per group. # p < 0.05 versus sham and *p < 0.05 versus training
The step-down inhibitory avoidance
In the step-down latency in the test session, 10 days (Z = −1.474, p = 0.140), but not 30 days after meningitis, there was no significant difference between training and test in the meningitis group (Fig. 2), suggesting impaired aversive memory. Because meningitis could affect sensory processing during training, such as the rats’ reactivity to the foot shock, rather than memory, we evaluated the effects of meningitis on foot shock sensitivity, and there were no significant differences between groups in the flinch or the jump nociceptive thresholds showing that meningitis did not affect the animal’s reactivity to the foot shock (data not shown).
The step-down inhibitory avoidance task. Animals were submitted to either meningitis or sham. They underwent the training test the step-down inhibitory avoidance task 10 and 30 days after induction, and were tested 24 h later. Data are presented as median and interquartile ranges, n = 10 rats per group. *p < 0.05 versus training
Continuous multiple trials step-down inhibitory avoidance task
In the continuous multiple trials step-down inhibitory avoidance, 10 but not 30 days after meningitis, we demonstrated a significant increase in the number of training trials (t = 3.536, df = 18.541, p = 0.002) required to reach the acquisition criterion (50 s on the platform) in the meningitis group as compared to the sham group (Fig. 3a). The results of this task suggest that the meningitis group required approximately two times more stimulus to reach the acquisition criterion when compared with the sham group 10 days after meningitis, indicating learning impairment. In the retention test, there was no difference between groups for all the times tested (Fig. 3b).
Continuous multiple trials step-down inhibitory avoidance task. Animals were submitted to either meningitis or sham. They underwent the training test on the continuous multiple trials stepdown inhibitory avoidance task 10 and 30 days after induction, and were tested 24 h later. a Training trials required to reach the acquisition criterion (50 s on the platform). Data are presented as mean ± SEM, n = 10 rats per group. *p < 0.05 versus sham. b Retention in the test section. Data are presented as median and interquartile ranges, n = 10 rats per group
Object recognition
At 10 and 30, but not 60 days after meningitis, the animals presented impairment of novel object recognition memory, i.e., they did not spend a significantly higher percentage of time exploring the novel object. After 10 days, the animals present memory impairment only during short term (Z = −3.395, p = 0.713), but not in the long term (Z = −2.562, p = 0.011). After 30 days, they did not spend a significantly higher percentage of time exploring the novel object during short term (Z = −0.685, p = 0.512) and long term (Z = −0.125, p = 0.902) retention test sessions in comparison to the training trial (Fig. 4). In addition, meningitis group (10 and 30 days) presented a significant reduction in the recognition index in short- and long-term recognition retention tests as compared to the sham group (Fig. 4).
Object recognition test. Animals were submitted to either meningitis or sham. They underwent the training test on the object recognition task 10, 30, and 60 days after induction, and were tested 1.5 h (short-term memory, STM) or 24 h (long-term memory, LTM) later. Data are presented as median and interquartile ranges, n = 10 rats per group, *p < 0.05 versus training
Elevated plus-maze task
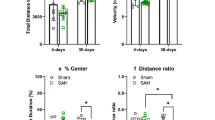
There were no statistically significant differences in the number of entries (t = −0.929, df = 34, p = 0.359), but there were statistically significant differences in the time spent (t = −2.128, df = 34, p = 0.041) in the arms between groups at 10, but not 30 days after surgery, suggesting that meningitis survivors present anxiety-like symptoms after 10 days induction (Fig. 5).
Elevated plus-maze test. Animals were submitted to either meningitis or sham. They underwent the elevated plus-maze task 10 and 30 days after induction. a Number of entries on the closed and open arms. b Time spent on the closed and open arms. Data are presented as mean ± SEM, n = 10 rats per group, *p < 0.05 versus sham
Forced swimming test
In the test session (5 min), we observed a significant increase in the immobility time in the meningitis group as compared to the sham group 10 (t = 3.739, df = 28.350, p = 0.001) and 30 (t = −3.704, df = 28.350, p = 0.001) days after surgery (Fig. 6), suggesting depressive-like behavior. In contrast, there were no statistically significant differences between groups after 60 days (Fig. 6).
Discussion
Our results demonstrate that meningitis animals 10 days after the surgery presented memory and learning deficits, anxiety-like and depressive-like behavior. These impairments were time-dependent, since after 30 days of meningitis the rats presented a normal performance on the step-down inhibitory avoidance, continuous multiple trials step-down inhibitory, and elevated plus-maze test, whereas after 60 days, the animals presented a normal performance in all behavior tests performed.
Cognitive impairment occurs frequently after bacterial meningitis (Grimwood et al. 1995; Braun et al. 1999; Wellmer et al. 2000; Leib et al. 2001; van de Beek et al. 2006). In comparison to healthy control persons, Merkelbach et al. (2000) found a high proportion of persisting cognitive deficits (more than 70%) resembling subcortical cognitive impairment. van de Beek et al. (2002) also reported cognitive slowing in patients after bacterial meningitis, especially in patients after S. pneumoniae meningitis. In experimental meningitis, one of the consequences of the massive inflammatory reaction in the meninges and subarachnoid space is the occurrence of neuronal apoptosis in the hippocampus (Braun et al. 1999). Hippocampal damage has been related to learning and memory deficits in humans and in animal models (Leib et al. 2001; Loeffler et al. 2001).
Other studies suggested that loss of cognitive speed might be partially reversible in time (Weisfelt et al. 2006b). This might well be explained by the longer time interval between meningitis and neuropsychological evaluation in this study compared with those previous studies (median 8 years range, 30 months to 12 years) (Weisfelt et al. 2006a) versus 14 months (range 7–25 months) (van de Beek et al. 2002) and 17 months (range 6 months to 4 years) (Weisfelt et al. 2006a). Other findings imply that neuropsychological impairment improves in the first years after bacterial meningitis and becomes relatively stable with time (Weisfelt et al. 2006a).
Additionally to hippocampus apoptosis, other alterations in the brain may be involved. Recently, it was verified that creatine kinase activity was altered at 24 h after the induction of the bacterial meningitis for S. pneumoniae in prefrontal cortex, hippocampus, and cortex (Barichello et al. 2009a). In other recent study, we found an increase in TNF-α levels at 6 h after induction of the meningitis in the hippocampus, frontal cortex, and CSF (Barichello et al. 2009b). The death or any alteration of these cells (apoptosis) appears to be responsible for the learning and memory deficits in patients who survive the disease (Nau et al. 1999; Leib et al. 2001).
Nowadays, few experimental strategies that aimed to decrease late cognitive impairment after meningitis were published. The early application of hypothermia or dexamethasone modulates the inflammatory reaction by improving short-term neurologic outcome (Irazuzta et al. 2002, 2005); caspase activation secondary to inflammatory reaction is probably central to the development of late cognitive impairment, since the pharmacologic caspase inhibition by bocaspartyl abolished cognitive impairment after meningitis in animal models (Irazuzta et al. 2008). In this context, the use of bactericidal antibiotic regimens can cause a burst of meningeal inflammation during experimental meningitis (Grandgirard et al. 2007a), and could be associated with worsening long-term outcome. Using a simple and feasible strategy, we demonstrated that early antibiotic administration (8 h after inoculation) when compared with late antibiotic administration (16 h after inoculation) prevents cognitive impairment induced by pneumococcal meningitis in rats after 10 days (Barichello et al. 2009c).
Serious life events, such as meningitis can have a critical long-term impact on psychic and mood stability (Bremner et al. 2004; Twamley et al. 2004), and can induce depression- and anxiety-like symptoms (Penick et al. 1994). Utilizing the Beck’s depression index, a study showed that there were not differences between survivor bacterial meningitis and healthy patients (Schmidt et al. 2006). Differently from what was shown in this study, meningitis survivor rats presented depressive-like symptoms up to 30 days of induction. In this report, anxiety-like symptoms were observed and these alterations persisted up to 30 days after induction. However, there were not studies that showed anxiety-like symptoms in neither humans nor animal model of meningitis.
In our model, we did not study all these potential mechanisms responsible for human long-term alterations, but only the isolated effect of meningitis on neurocognitive impairment and this may explain why our animals had a full recovery, differing from that observed in humans. In addition, the concept of sickness behavior could help in elucidating some of the mechanisms associated with cognitive (dys)function after meningitis. The presented model could be a useful tool in studying cognitive impairment, depression, and anxiety after meningitis, and thus the mechanisms associated with the recovery of these functions.
References
Barichello T, Silva GZ, Savi GD, Torquato JM, Batista AL, Scaini G, Rezin GT, Santos PM, Feier G, Streck EL (2009a) Brain creatine kinase activity after meningitis induced by Streptococcus pneumoniae. Brain Res Bull 28:85–88
Barichello T, dos Santos I, Savi GD, Florentino AF, Silvestre C, Comim CM, Feier G, Sachs D, Teixeira MM, Teixeira AL, Quevedo J (2009b) Tumor necrosis factor alpha (TNF-alpha) levels in the brain and cerebrospinal fluid after meningitis induced by Streptococcus pneumoniae. Neurosci Lett 467:217–219
Barichello T, Silva GZ, Batista AL, Savi GD, Feier G, Comim CM, Quevedo J, Dal-Pizzol F (2009c) Early antibiotic administration prevents cognitive impairment induced by meningitis in rats. Neurosci Lett 1:71–73
Bohr V, Paulson OB, Rasmussen N (1984) Pneumococcal meningitis, late neurologic sequelae and features of prognostic impact. Arch Neurol 41:1045–1049
Braun JS, Novak R, Herzog K-H, Bodner SM, Cleveland JL, Tuomanen EI (1999) Neuroprotection by a caspase inhibitor in acute bacterial meningitis. Nat Med 5:298–302
Bremner J, Vermetten E, Afzal N, Vythilingamm M (2004) Deficits in verbal declarative memory function in women with childhood sexual abuse related posttraumatic stress disorder. J Nerv Ment Dis 192:643–649
Grandgirard D, Steiner O, Täuber MG, Leib SL (2007a) An infant mouse model of brain damage in pneumococcal meningitis. Acta Neuropathol 114:609–617
Grandgirard D, Schürch C, Cottagnoud P, Leib SL (2007b) Prevention of brain injury by the nonbacteriolytic antibiotic daptomycin in experimental pneumococcal meningitis. Antimicrob Agents Chemother 51:2173–2178
Grimwood K, Anderson VA, Bond L, Catroppa C, Hore RL, Keir EH, Nolan T, Roberton DM (1995) Adverse outcomes of bacterial meningitis in school-age survivors. Pediatrics 95:646–656
Hoogma M, Beek DV, Weisfelt M, Gans J, Schmand B (2007) Cognitive outcome in adults after bacterial meningitis. J Neurol Neurosurg Psychiatry 78:1092–1096
Irazuzta J, Pretzlaff RK, Zingarelli B, Xue V, Zemlan F (2002) Modulation of nuclear factor-B activation and decreased markers of neurological injury associated with hypothermic therapy in experimental bacterial meningitis. Crit Care Med 30:2553–2559
Irazuzta J, Pretzlaff RK, de Courten-Myers G, Zemlan F, Zingarelli B (2005) Dexamethasone decreases neurological sequelae and caspase activity. Intensive Care Med 31:146–150
Irazuzta J, Pretzlaff RK, Zingarelli B (2008) Caspases inhibition decreases neurological sequelae in meningitis. Crit Care Med 5:1603–1606
Leib SL, Clements JM, Lindberg RL, Heimgartner C, Loeffler JM, Pfister LA, Täuber MG, Leppert D (2001) Inhibition of matrix metalloproteinases and tumour necrosis factor alpha converting enzyme as adjuvant therapy in pneumococcal meningitis. Brain 124:1734–1742
Leib SL, Heimgartner C, Bifrare YD, Loeffler JM, Täauber MG (2003) Dexamethasone aggravates hippocampal apoptosis and learning deficiency in pneumococcal meningitis in infant rats. Pediatr Res 54:353–357
Loeffler JM, Ringer R, Hablützel M, Täuber MG, Leib SL (2001) The free radical scavenger alpha-phenyl-tert-butyl nitrone aggravates hippocampal apoptosis and learning deficits in experimental pneumococcal meningitis. J Infect Dis 183:247–252
Merkelbach S, Sittinger H, Schweizer I, Muller M (2000) Cognitive outcome after bacterial meningitis. Acta Neurol Scand 102:118–123
Nau R, Soto A, Bruck W (1999) Apoptosis of neurons in the dentate gyrus in humans suffering from bacterial meningitis. J Neuropathol Exp Neurol 58:265–274
Penick EC, Powell BJ, Nickel EJ, Bingham SF, Riesenmy KR, Read MR, Campbell J (1994) Co-morbidity of lifetime psychiatric disorder among male alcoholic patients. Alcohol Clin Exp Res 48:1289–1293
Schmidt H, Heimann B, Djukic M, Mazurek C, Fels C, Wallesch CW, Nau R (2006) Neuropsychological sequelae of bacterial and viral meningitis. Brain 129:333–345
Schuchat A, Robinson K, Wenger JD, Harrison LH, Farley M, Reingold AL, Lefkowitz L, Perkins BA (1997) Bacterial meningitis in the United States in 1995 Active Surveillance Team. N Engl J Med 337:970–976
Tuon L, Comim CM, Petronilho F, Barichello T, Izquierdo I, Quevedo J, Dal-Pizzol F (2008) Time-dependent behavioral recovery after sepsis in rats. Intensive Care Med 34:1724–1731
Twamley E, Hami S, Stein M (2004) Neuropsychological function in college students with and without posttraumatic stress disorder. Psychiatry Res 126:265–274
van de Beek D, Schmand B, de Gans J, Weisfelt M, Vaessen H, Dankert J, Vermeulen M (2002) Cognitive impairment in adults with good recovery after bacterial meningitis. J Infect Dis 186:1047–1052
van de Beek D, de Gans J, Tunkel AR, Wijdicks EF (2006) Community-acquired bacterial meningitis in adults. N Engl J Med 354:44–53
Weisfelt M, van de Beek D, Hoogman M, Hardeman C, de Gans J, Schmand B (2006a) Cognitive outcome in adults with moderate disability after pneumococcal meningitis. J Infect 52:433–439
Weisfelt M, Hoogman M, van de Beek D, de Gans J, Dreschler WA, Schmand BA (2006b) Dexamethasone and long-term outcome in adults with bacterial meningitis. Ann Neurol 60:456–468
Wellmer A, Noeskea C, Gerbera J, Munzelb U, Naua R (2000) Spatial memory and learning deficits after experimental pneumococcal meningitis in mice. Neurosci Lett 296:137–140
Acknowledgments
This research was supported by grants from CNPq (TB and JQ), FAPESC (TB and JQ) and UNESC (TB and JQ). JQ is a CNPq Research Fellows. CMC is holder of a CNPq Studentship.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Barichello, T., Silva, G.Z., Generoso, J.S. et al. Time-dependent behavioral recovery after pneumococcal meningitis in rats. J Neural Transm 117, 819–826 (2010). https://doi.org/10.1007/s00702-010-0435-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-010-0435-2