Abstract
Background
The COVID19 lockdown has altered the dynamics of living. Its collateral fallout on head injury care has not been studied in detail, especially from low- and middle-income countries, possibly overwhelmed more than developed nations. Here, we analyze the effects of COVID19 restrictions on head injury patients in a high-volume Indian referral trauma center.
Methods
From the prospective trauma registry, clinico-epidemiological and radiological parameters of patients managed during 190 days before and 190 days during COVID19 phases were studied. As an indicator of care, the inpatient mortality of patients with severe HI was also compared with appropriate statistical analyses.
Results
Of the total 3372 patients, there were 83 head injury admissions per week before COVID19 restrictions, which decreased to 33 every week (60% drop) during the lock phases and stabilized at 46 per week during the unlock phases. COVID19 restrictions caused a significant increase in the proportion of patients arriving directly without resuscitation at peripheral centers and later than 6 h of injury. Though the most common mechanism was vehicular, a relative increase in the proportion of assaults was noted during COVID19. There was no change in the distribution of mild, moderate, and severe injuries. Despite a decrease in the percentage of patients with systemic illnesses, severe head injury mortality was significantly more during the lock phases than before COVID19 (59% vs. 47%, p = 0.02).
Conclusions
COVID19 restrictions have amplified the already delayed admission among patients of head injury from north-west India. The severe head injury mortality was significantly greater during lock phases than before COVID19, highlighting the collateral fallout of lockdown. Pandemic control measures in the future should not ignore the concerns of trauma emergency care.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
With the World Health Organization declaring the COVID19 pandemic in March 2020, there have been various strategies to cut off the viral transmission [8, 22, 40, 44]. Of these, lockdown and social distancing have been the major ones. Post lockdown, a global change in admission pattern and patient care, has been noted across multiple medical domains [1, 4, 17, 32, 36]. Neurosurgical patients remain no exception, and COVID19 has impacted all facets of neurosurgery, including neurotrauma [3, 19, 21, 23, 25, 28, 32]. The latter, however, has been less evaluated. While a few studies on the Western population have attempted to look upon the COVID19 influence on neurotrauma patterns, the comparable data from low- and middle-income countries (LMIC) is minimal [16, 26, 37]. This assumes importance, as there is a considerable difference in head injury epidemiology between high-income and LMIC [18, 30, 39]. Therefore, understanding the sectoral changes in neurotrauma following COVID19 could better prepare for the ongoing pandemic and an unprecedented catastrophe in the future. Many European nations have already started experiencing the COVID19 second wave [27].
The COVID19 viral surge in India was relatively late; however, the volume has exponentially escalated to approximately 9.7 million, with the country emerging as a significant epicenter [6, 33]. As of this writing, although the spread of the contagion seems to be stabilized with a reducing trend in the number of new active cases, the effect of forthcoming winters on the viral spread is currently uncertain [2, 15, 33]. Soon after 11 Mar 2020, when the World Health Organization declared COVID19 as a pandemic and with few sporadic cases reported in the country, the Indian Government, on 25 Mar, imposed a strict nationwide lockdown. This was staged in 4 phases with gradual unlock in sequence. Neurotrauma trends have likely changed during these periods due to more extraordinary travel restrictions. Besides, the COVID19 pandemic has forced a reshuffle of the existing resources to focus mainly on COVID19 patients [3, 28, 32]. The care may have consequently altered for a non-COVID cohort such as neurotrauma. We intended to perform a comparative analysis on the effect of COVID19 on the volume and admission patterns of head injury (HI) in our level 1 tertiary trauma care center and compare the mortality for severe HI, which can act as a surrogate indicator of the collateral fallout of COVID19 restrictions.
Methods and materials
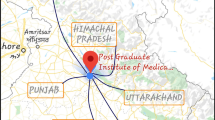
This comparative study of prospectively acquired data was carried out in our level 1 central tertiary referral trauma center catering to north-west India (Fig. 1). The overall study data represent approximately 12-month HI admissions between 16 Sept 2019 and 30 Sept 2020.
Patient cohort
In India, the lockdown was imposed in phases from 25 Mar 2020, with the following timeline: phase 1 (25 Mar–14 Apr), phase 2 (15 Apr–3 May), phase 3 (4–17 May), and phase 4 (18–31 May). Similarly, the phases of unlocking were as follows: unlock 1.0 (1–30 June), unlock 2.0 (1–31 July), unlock 3.0 (1–31 August), and unlock 4.0 (1–30 September) [35]. The study cohort involved three distinct periods in analyzing the significant change in trends and patient characteristics. The patients admitted with HI during the lock phases (68 days, 25 Mar to 31 May) and unlock phases (122, 1 Jun to 30 Sept) were compared to those admitted during 190 days from 16 Sept to 24 Mar, an equivalent time frame just before COVID19 restrictions. The latter served as a control group before the onset of the COVID19 pandemic. The data were evaluated in each phase of the lockdown and unlock period.
Data collection
The basic clinico-demographics, mechanism of injury, hospital arrival time since the time of injury, admission Glasgow coma scale (GCS), significant computed tomography (CT) imaging findings, and surgical intervention were prospectively entered into a pre-planned database. The mortality among patients with severe HI was compared during the pre-COVID period and lock phases.
Statistical analysis
The pre-COVID and post-COVID groups were compared using standard descriptive measures such as percentages and the mean number. The chi-square method tested significance for categorical variables, while the independent samples t test tested the difference in means for continuous variables. p < 0.05 was considered significant.
Results
Head injury admissions
The trends in number and pattern of head injury admissions are detailed in Fig. 2 and Table 1. Overall, the study identified 3372 HI admissions (2259 in pre-COVID19, 320 in lock phases, and 720 during unlocking phases of COVID19). There were 83 head injury admissions per week before COVID19. The numbers decreased to 33 per week during the lock phases (60% less). Although the unlock period saw a rise in the number of patients (46 per week), it was still only 55% of the pre-COVID19 period.
Demography and referral
After COVID19 restrictions, there was a significant increase in the proportion of patients arriving directly without initial resuscitation at peripheral centers (15% vs. 11%, p = 0.002). Though the patients’ mean age did not change, more female admissions were noted post restrictions.
Time of arrival
After COVID19, the proportion of patients reaching later than 6 h increased significantly from 66 to 74% (p < 0.001) (Table 1). Interestingly, it showed a continuing trend from lock phases to even the unlock phases (Fig. 3).
Mode and severity of injury
Regarding the mechanism of injury, motor vehicular accidents remained the most common cause overall. There was a significant rise in admissions secondary to assault (4.5% vs. 8%) after the onset of COVID19. The percentage of fall exceeded vehicular accidents (48% vs. 42%). Despite lockdown measures, vehicular accidents in the later phases contributed to almost 50% of injuries, increasing up to 71% in the last phase. Though the percentage of vehicular accidents returned to pre-COVID19 status during unlocks phases, assaults were still relatively high. During the COVID19 period, there was a significant decrease in HI under alcohol influence (21% vs. 17%, P=0.02) and with comorbid illnesses (10% vs. 2%, p < 0.001). The proportions of patients with associated ophthalmic and faciomaxillary injuries were lower with COVID19. However, according to GCS, there was no change in patients’ distribution as mild, moderate, and severe head injury (Table 1).
Neuroimaging, treatment, and mortality
The common imaging findings were contusions, subdural hematoma (SDH), skull fractures, subarachnoid hemorrhage (SAH), and pneumocephalus in decreasing order of frequency. The proportion of SDH, SAH, and pneumocephalus decreased during COVID19, compared to the pre-COVID19 period (p < 0.05). There was, however, a marginal increase in concurrent spinal injuries (Table 1). The majority of the patients were managed conservatively. Operative intervention was undertaken among 27% and 29% of patients before and during COVID19, respectively. The severe head injury mortality was significantly more during the lock phases than before COVID19 (59% vs. 47%, p = 0.02).
Discussion
Head injury like any acute brain insult, initiates a cascade of secondary pathophysiological events, potentially influenced by the COVID19 constraints, possibly widening the economic divide between the developed and LMIC [9, 12, 13, 43]. By contrast to the cancelation of non-emergency admissions, our neurotrauma wing has been functioning throughout COVID19, offering its regular services, amidst a tight situation of these pandemic-related constraints. We considered the following perspectives for this study: First, how the pandemic has influenced the HI epidemiology in LMIC trauma center, and second, has there been any difference in care because of the significant ongoing rearrangement of health resources. As of this writing, India has experienced substantial COVID19 case-volume and its consequences [6, 33]. Therefore, it is imperative to understand the changes in the HI profile from the standpoint of LMIC.
Effect of lockdown/COVID on neurotrauma patterns
Regional variations in the HI profile are established [18, 30]. For instance, while fall predominates the HI etiology in high-income countries secondary to a growing geriatric population and better adaptation of traffic practices, vehicular accidents remain the most typical cause of HI in LMIC [18, 24, 30, 34]. After COVID19 and lockdown began, reports across countries have documented a decrease in overall hospital admissions [17, 23, 25, 28, 32, 36]. This trend owes restricted freedom of movement consequent to lockdown, social distancing, and possibly a COVID19 fear with hesitancy in reaching hospital premises. However, the neurotraumatological aspects have been relatively less studied.
As evident from this study and others from developed nations, the lockdown has changed HI patterns and care [16, 26, 37]. The proportion of vehicular HI decreased, while the relative percentage secondary to assault rose during COVID19. In contrast to the pre-COVID19 period, when vehicular accidents were the most common, the injury after fall and vehicular accidents were nearly the same during the first phase of lockdown. Less commutation, traffic, and strict vigilance during the initiation of the lockdown explain this change. With more people residing at home and a few hailing from hilly terrains of the hospital catchment area has possibly led to the rise in fall-associated HI. However, in the subsequent lockdown phases, vehicular accidents showed an increasing trend, suggesting lockdown fatigue and perhaps complacency. The psychosocial stress of staying at home, interpersonal conflict, and financial crisis has been implicated in increased assault-related injuries [16, 26, 37]. Interestingly, the percentage of female HI also increased after COVID19. This could be due to an increase in the non-vehicular mode of injuries than pre-COVID conditions when males were more frequently involved in a substantial proportion of road traffic accidents.
After the COVID19 outbreak, the percentage of patients referred to our center after resuscitation has decreased. With a rise in direct admissions, this is possibly due to fewer intermediate hospitals fully functional or effectively delivering early care during this pandemic. Some have suggested a higher proportion of severe HI after COVID19 due to mild HI patients’ reluctance to attend hospitals. However, we observed that mild HI continued to occupy a significant share of our hospital admissions. Despite being a tertiary referral center, our institute has continuously been overburdened due to a higher proportion of mild HI that can be effectively managed at peripheral centers. Although this demand could be met by stretching the hospital resources during the standard pre-COVID19 period, at this point, with the pandemic taking the upper hand and with significant infrastructure shifted towards COVID19 care, this trend appears to sustain excess stress on the limited resources. A lack of fall in the proportion of mild HI (approximately 50% in both periods) hints that peripheral facilities are less prepared to manage this cohort of neurotrauma. Upgrading these intermediate facilities with a long-term outlook may permit better care for patients who legitimately require advanced care while avoiding strain on health resources.
Timely transportation to an appropriate trauma care facility is an essential component that affects the final HI outcomes [14, 20, 29, 41]. We noted that during COVID19, the proportion of patients who reached our hospital within optimal time has decreased. This can be explained by factors such as hindrance in arranging transport and transfer-related delays due to disruption of the routine transfer services compared to that of typical time frame. The findings imply that interhospital transfer coordination is a domain that needs a relook.
With the gradual lifting of lockdown restrictions, the absolute volume of HI admissions demonstrated a rising trend. Also, few authors have noted the emergency neurosurgical load remained the same despite the ongoing pandemic [3]. While the COVID19 may continue to stay longer, our findings hint that it is time to reconsider mobilizing sufficient health resources for treating non-COVID conditions such as neurotrauma, which has a significant social and economic impact. As expected, owing to the initial fall in admissions, the surgical volume of neurotrauma decreased during the lockdown.
After COVID19, some positive effects were noticed, such as decreased HI patients under alcohol influence. Lockdown restrictions with restricted access to alcohol availability can explain this trend. A decline in HI patients with comorbid illness was also seen after this pandemic. With the awareness that comorbidities constitute a significant risk factor for COVID19 infection, there is probably a natural tendency for persons with preexisting illnesses not to venture out of the home during COVID19.
Mortality of severe HI
We attempted to evaluate whether the COVID19 outbreak has influenced the overall HI patient care. Hence the mortality of severe HI was chosen as a proxy variable. In a severe HI cohort, there are many determinants such as prehospital resuscitation, timely transfer, and dedicated nursing care that influence the hypoxemic morbidity after head injury [5, 20, 42]. While improvements in services have been shown to result in better neurosurgical outcomes in LMICS, COVID19 has caused a redistribution of resources, with less emphasis on non-COVID19 cases [10, 11, 38]. These patients likely received care that is less optimal than during the pre-COVID19 period. Apprehensions among healthcare workers to care for the airway and breathing could also have contributed to poorer outcomes.
We acknowledge that this is a single-center study, and hence the observations may not be generalized. We have not assessed the long-term functional outcome, influenced by rehabilitation limitations [7, 31]. Yet, the findings, by and large, represent the prevailing scenario in an LMIC trauma center. Hospital referral bias and seasonal bias are some of the other potential concerns. This hospital-based study may not reflect the overall HI prevalence in the community during the COVID19 pandemic. Many mild injured patients may not have been brought to the hospital because of the fear of being infected. Even in severe HI cases, a few might have died before reaching the hospital due to longer transit and suboptimal conditions during the COVID19 lockdown.
Conclusions
In summary, COVID19 has influenced HI care overall. A definitive delay in patient arrival has occurred. The severe head injury mortality was significantly greater during lock phases than before COVID19, highlighting the collateral fallout of lockdown. Pandemic control measures in the future should not ignore the concerns of trauma emergency care.
References
Al-Shamsi HO, Alhazzani W, Alhuraiji A, Coomes EA, Chemaly RF, Almuhanna M, Wolff RA, Ibrahim NK, Chua MLK, Hotte SJ et al (2020) A practical approach to the management of cancer patients during the novel coronavirus disease 2019 (COVID-19) pandemic: an international collaborative group. Oncologist 25(6):e936–e945
Audi A, AlIbrahim M, Kaddoura M, Hijazi G, Yassine HM, Zaraket H (2020) Seasonality of respiratory viral infections: will COVID-19 follow suit? Front Public Health 8:567184. https://doi.org/10.3389/fpubh.2020.567184
Bajunaid K, Alatar A, Alqurashi A, Alkutbi M, Alzahrani AH, Sabbagh AJ, Alobaid A, Barnawi A, Alferayan AA, Alkhani AM et al (2020) The longitudinal impact of COVID-19 pandemic on neurosurgical practice. Clin Neurol Neurosurg 198:106237
Bersano A, Kraemer M, Touzé E, Weber R, Alamowitch S, Sibon I, Pantoni L (2020) Stroke care during the COVID-19 pandemic: experience from three large European countries. Eur J Neurol 3 June:10.1111/ene.14375. https://doi.org/10.1111/ene.14375
Bindu TS, Vyas S, Khandelwal N, Bhatia V, Dhandapani S, Kumar A, Ahuja CK (2017) Role of whole-brain computed tomography perfusion in head injury patients to predict outcome. Indian J Radiol Imaging 27(3):268–273
COVID 19 statewise status, Government of India (2020) https://www.mygov.in/corona-data/covid19-statewise-status. Accessed 28 Sept 2020
Devi Y, Khan S, Rana P, Deepak DM, Ghai S, Gopichandran L, Dhandapani S (2020) Cognitive, behavioral, and functional impairments among traumatic brain injury survivors: impact on caregiver burden. J Neurosci Rural Pract 11(4):629–635
Dhandapani M, Kaur S, Das K, Guru RR, Biswal M, Mahajan P, Koushal V, Puri GD (2020) Enhancing the safety of frontline healthcare workers during coronavirus disease: a novel real-time remote audiovisual aided doffing approach. Infect Dis (Lond) 2:1–3. https://doi.org/10.1080/23744235.2020.1836390
Dhandapani S, Bajaj A, Gendle C, Saini I, Kaur I, Chaudhary I, Jasandeep KJ, Kalyan G, Dhandapani M et al (2018) Independent impact of plasma homocysteine levels on neurological outcome following head injury. Neurosurg Rev 41(2):513–517
Dhandapani S, Singh A, Singla N, Praneeth K, Aggarwal A, Sodhi HB, Pal SS, Goudihalli S, Salunke P, Mohindra S et al (2018) Has outcome of subarachnoid hemorrhage changed with improvements in neurosurgical services? Stroke 49(12):2890–2895
Dhandapani M, Dhandapani S (2020) Challenges posed by COVID-19 and neurosurgical nursing strategies in developing countries. Surg Neurol Int 11:441
Dhandapani SS, Manju D, Mahapatra AK (2012) The economic divide in outcome following severe head injury. Asian J Neurosurg 7(1):17–20
Dhandapani S, Aggarwal A, Srinivasan A, Meena R, Gaudihalli S, Singh H, Dhandapani M, Mukherjee KK, Gupta SK (2015) Serum lipid profile spectrum and delayed cerebral ischemia following subarachnoid hemorrhage: Is there a relation? Surg Neurol Int 6(Suppl 21):S543–8
Dinh MM, Bein K, Roncal S, Byrne CM, Petchell J, Brennan J (2013) Redefining the golden hour for severe head injury in an urban setting: the effect of prehospital arrival times on patient outcomes. Injury 44(5):606–610
Engelbrecht FA, Scholes RJ (2021) Test for Covid-19 seasonality and the risk of second waves. One Health 12:100202. https://doi.org/10.1016/j.onehlt.2020.100202
Figueroa JM, Boddu J, Kader M, Berry K, Kumar V, Ayala V, Vanni S, Jagid J (2020) The effects of lockdown during the SARS-CoV-2 pandemic on neuro-trauma related hospital admissions. World Neurosurg Aug 18:S1878-8750(20)31850-7. https://doi.org/10.1016/j.wneu.2020.08.083
Franchini S, Spessot M, Landoni G, Piani C, Cappelletti C, Mariani F, Mauri S, Taglietti MV, Fortunato M, Furlan F et al (2020) Stranger months: how SARS-CoV-2, fear of contagion, and lockdown measures impacted attendance and clinical activity during February and March 2020 at an urban Emergency Department in Milan. Disaster Med Public Health Prep 27 July:1–23. https://doi.org/10.1017/dmp.2020.265
GBD (2016) Traumatic brain injury and spinal cord injury collaborators (2019) global, regional, and national burden of traumatic brain injury and spinal cord injury, 1990-2016: a systematic analysis for the global burden of disease study 2016. Lancet Neurol 18(1):56–87
Gupta P, Muthukumar N, Rajshekhar V, Tripathi M, Thomas S, Gupta SK, Lal V, Pal P, Abraham M, Behari S et al (2020) Neurosurgery and neurology practices during the novel COVID-19 pandemic: a consensus statement from India. Neurol India 68(2):246–254
Harmsen AM, Giannakopoulos GF, Moerbeek PR, Jansma EP, Bonjer HJ, Bloemers FW (2015) The influence of prehospital time on trauma patients outcome: a systematic review. Injury 46(4):602–609
Hecht N, Wessels L, Werft FO, Schneider UC, Czabanka M, Vajkoczy P (2020) Need for ensuring care for neuro-emergencies-lessons learned from the COVID-19 pandemic. Acta Neurochir 162(8):1795–1801
Issac A, Stephen S, Jacob J, Vr V, Radhakrishnan RV, Krishnan N, Dhandapani M (2020) The pandemic league of COVID-19: Korea versus the United States, with lessons for the entire world. J Prev Med Public Health 53(4):228–232
Jayakumar N, Kennion O, Villabona AR, Paranathala M, Holliman D (2020) Neurosurgical referral patterns during the coronavirus disease 2019 pandemic: a United Kingdom experience. World Neurosurg Sep 2:S1878-8750(20)31931-8. https://doi.org/10.1016/j.wneu.2020.08.162.
Karthigeyan M, Wankhede LS, Singh A, Sahoo SK, Tripathi M, Gendle C, Singla R, Aggarwal A, Singla N, Mohanty M et al (2019) Functioning of neurotrauma center in PGIMER, Chandigarh. Indian J Neurotrauma 16(02/03):120–123
Krenzlin H, Bettag C, Rohde V, Ringel F, Keric N (2020) Involuntary ambulatory triage during the COVID-19 pandemic - a neurosurgical perspective. PLoS One 15(6):e0234956
Lara-Reyna J, Yaeger KA, Rossitto CP, Camara D, Wedderburn R, Ghatan S, Bederson JB, Margetis K (2020) "Staying home"-early changes in patterns of neurotrauma in New York City during the COVID-19 pandemic. World Neurosurg Jul 27:S1878-8750(20)31676-4. https://doi.org/10.1016/j.wneu.2020.07.155
Looi MK (2020) Covid-19: is a second wave hitting Europe? BMJ 371:m4113. https://doi.org/10.1136/bmj.m4113
Lubansu A, Assamadi M, Barrit S, Dembour V, Yao G, El Hadwe S, De Witte O (2020) COVID-19 impact on neurosurgical practice: lockdown attitude and experience of a European academic center. World Neurosurg Sep 3:S1878-8750(20)31937-9. https://doi.org/10.1016/j.wneu.2020.08.168
Luck T, Treacy PJ, Mathieson M, Sandilands J, Weidlich S, Read D (2015) Emergency neurosurgery in Darwin: still the generalist surgeons' responsibility. ANZ J Surg 85(9):610–614
Maas AIR, Menon DK, Adelson PD, Andelic N, Bell MJ, Belli A, Bragge P, Brazinova A, Büki A, Chesnut RM et al (2017) Traumatic brain injury: integrated approaches to improve prevention, clinical care, and research. Lancet Neurol 16(12):987–1048
Mahak C, Shashi Y, Hemlata MN, Sandhya G, Dheeraj K, Dhandapani M, Dhandapani SS (2018) Assessment of utilization of rehabilitation services among stroke survivors. J Neurosci Rural Pract 9(4):461–467
Mathiesen T, Arraez M, Asser T, Balak N, Barazi S, Bernucci C, Bolger C, Broekman MLD, Demetriades AK, Feldman Z et al (2020) A snapshot of European neurosurgery December 2019 vs. March 2020: just before and during the Covid-19 pandemic. Acta Neurochir 162(9):2221–2233
Ministry of Health and Family Welfare, Government of India (2020) https://covid19.india.gov.in/document-category/ministry-of-health-and-family-welfare/page/2/. Accessed 28 Sept 2020
Mukherjee KK, Dhandapani S, Sarda AC, Tripathi M, Salunke P, Srinivasan A, Tewari MK, Mathuriya SN (2015) Prospective comparison of simple suturing and elevation debridement in compound depressed fractures with no significant mass effect. Acta Neurochir 157(2):305–309
National Disaster Management Authority, Government of India (2020) https://ndma.gov.in/en/mha-orders-guidelines.html. Accessed 28 Sept 2020
Negrini S, Grabljevec K, Boldrini P, Kiekens C, Moslavac S, Zampolini M, Christodoulou N (2020) Up to 2.2 million people experiencing disability suffer collateral damage each day of COVID-19 lockdown in Europe. Eur J Phys Rehabil Med 56(3):361–365
Pinggera D, Klein B, Thomé C, Grassner L (2020) The influence of the COVID-19 pandemic on traumatic brain injuries in Tyrol: experiences from a state under lockdown. Eur J Trauma Emerg Surg 22:1–6. https://doi.org/10.1007/s00068-020-01445-7
Rose DZ, Burgin WS, Renati S (2020) Untreated stroke as collateral damage of COVID-19: "time is brain" versus "stay at home". Neurohospitalist 10(4):291–292
Rubiano AM, Carney N, Chesnut R, Puyana JC (2015) Global neurotrauma research challenges and opportunities. Nature 527(7578):S193–S197
Sahoo SK, Dhandapani S, Singh A, Gendle C, Karthigeyan M, Salunke P, Aggarwal A, Singla N, Singla R, Tripathi M et al (2020) COVID-19: changing patterns among neurosurgical patients from North India, efficacy of repeat testing, and inpatient prevalence. Neurosurg Focus 49(6):E7
Tien HC, Jung V, Pinto R, Mainprize T, Scales DC, Rizoli SB (2011) Reducing time-to-treatment decreases mortality of trauma patients with acute subdural hematoma. Ann Surg 253(6):1178–1183
Tohme S, Delhumeau C, Zuercher M, Haller G, Walder B (2014) Prehospital risk factors of mortality and impaired consciousness after severe traumatic brain injury: an epidemiological study. Scand J Trauma Resusc Emerg Med 22:1
Walker PGT, Whittaker C, Watson OJ, Baguelin M, Winskill P, Hamlet A, Djafaara BA, Cucunubá Z, Olivera Mesa D, Green W et al (2020) The impact of COVID-19 and strategies for mitigation and suppression in low- and middle-income countries. Science 369(6502):413–422
Wong CKH, Wong JYH, Tang EHM, Au CH, Lau KTK, Wai AKC (2020) Impact of national containment measures on decelerating the increase in daily new cases of COVID-19 in 54 countries and 4 epicenters of the pandemic: comparative observational study. J Med Internet Res 22(7):e19904
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The procedures performed were as per the ethical standards of the institutional ethics committee and with the 1964 Helsinki declaration and its later amendments. For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Brain trauma
Rights and permissions
About this article
Cite this article
Karthigeyan, M., Dhandapani, S., Salunke, P. et al. The collateral fallout of COVID19 lockdown on patients with head injury from north-west India. Acta Neurochir 163, 1053–1060 (2021). https://doi.org/10.1007/s00701-021-04723-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-021-04723-4