Abstract
Background: Twiddler’s syndrome consists of rotation or manipulation of an implantable pulse generator (IPG) in its subcutaneous pocket by a patient, thus causing hardware malfunction. Methods: This syndrome is being reported more frequently in patients treated with deep brain stimulation (DBS). Results: We report the case of a woman who had received bed nucleus of stria terminalis (BNST) electrodes for obsessive-compulsive disorder (OCD) and developed twiddler’s syndrome a few months after surgery, causing hardware malfunction due to obsessive manipulation of the IPG. Conclusion: The patient did not have compulsions related to touching objects at admission, thus making it difficult to foresee and prevent TS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Deep brain stimulation (DBS) is an accepted surgical treatment for a large variety of movement, neurological, pain and psychiatric disorders. It works through the electrical stimulation of specific structures in the basal ganglia or their related structures. The electrical current is delivered into the targeted structure through multi-contact electrodes. The intracranial electrodes, secured to the skull, are connected by extension wires to a pulse generator implanted in a subcutaneous pocket on the chest or in the abdomen. Several sites exist where this circuit can be interrupted, thus possibly leading to hardware failure, the most common location being the extracranial portion of the DBS electrode and the extension wires [4, 6].
The so-called “twiddler’s syndrome” (TS) consists of rotation or manipulation of the implanted pulse generator (IPG) in its subcutaneous pocket by the patient, causing damage and malfunction of the extension leads and even the DBS electrode [14]. This problem may result from the intentional obsessive manipulation of the IPG and the connecting cables [6].
Here we present a case of TS occurring in a patient who received DBS for obsessive-compulsive disorder (OCD).
Case report
The patient is a 51-year-old unemployed overweight female who has suffered from OCD since the age of 15 years and has comorbid major depression disorder. The patient was treated by several psychiatrists and received numerous medications, including several serotonin-reuptake inhibitors, clomipramine and flurazepam, and augmentation with atypical antipsychotics. She underwent cognitive-behavioral therapy, electroconvulsive therapy and cycles of transcranial magnetic stimulation with little benefit. Her main symptoms at the baseline evaluation revealed contamination obsessions, aggressive thoughts towards children and fear of sharp objects, animals, dead people and religious figures such as priests and nuns. Her compulsions included cleaning and avoidance rituals. This patient’s behavior resulted in so much impairment that she became dependent on her family in activities of daily living.
The patient was referred to us in 2016 as a candidate for DBS. She met the criteria of severity and treatment resistance for surgical eligibility; thus, in November 2016 she underwent bilateral bed nucleus of stria terminalis (BNST) DBS; the electrodes were connected to a single-channel non-rechargeable pulse generator (Activa SC, Medtronic) implanted in the infraclavear region. Postoperative CT confirmed the correct positioning of the intracerebral electrodes. After discharge, she presented a slow but evident clinical improvement of both obsessive-compulsive symptoms and general functioning. Her stimulation parameters were adjusted in follow-up evaluations. Due to the high voltage of stimulation needed, the left IPG had been exhausted in May 2017, while the right one had a low battery charge at the same time. This finding matched a worsening in her clinical presentation; therefore, we decided to position two rechargeable IPGs (Activa RC, Medtronic). At surgery, the left extension lead appeared extensively coiled on itself, probably because of rotation of the IPG in the loose connective tissue of the infraclavear pocket (Fig. 1).
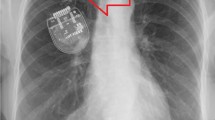
At the postoperative check, impedance was within the normal range on the right side, whereas high impedances of the DBS system were detected on all contacts on the left electrode, suggesting a fracture or malfunction of the implanted hardware. Plain x-ray examinations of the patient’s chest, neck and head were then obtained, revealing also the braiding and fraying of the distal part of the intracranial electrode (Fig. 2).
DBS surgery was then repeated on the left side, with replacement also of the extension cable. Intraoperatively, measurement of the impedances was carried out in all the electrode combinations. High impedance with a low stimulation current was observed in all of the circuit nodes. At this time, the rechargeable IPG (Activa RC, Medtronic) was secured to the muscle fascia at two points with non-absorbable silk sutures to prevent further rotation of the system and recurrence of TS. A postoperative CT showed the correct electrode insertion. At the 6-month follow-up no more TS had occurred.
Discussion
Hardware-related adverse DBS events are reported to affect 8.7% of all patients, the most common being infections (2.4%), system malfunctioning (1%), premature loss of battery power (0.9%) and acute failure of the stimulator (0.8% each) [15].
These complications deserve attention, as they may require surgical correction or removal of the system, with a decrease or loss of benefit and significant economic burden [4].
TS was first described in 1968 [2], becoming a well-recognized cause of malfunction in patients with cardiac pacemakers and defibrillators, but it has only rarely been reported as a hardware-related adverse event in DBS patients. Only a few case reports and small series dealing with this complication exist in the present literature, mostly in patients submitted to DBS for Parkinson’s disease or essential tremor [3, 4, 6], even if its occurrence has also been reported in patients affected by epilepsy [10], dystonia [1, 7, 12] and, in one case, OCD [9].
TS is most commonly diagnosed within the first year following DBS surgery. As for other hardware-related complications, the usual clinical presentation consists of sudden loss of efficacy from DBS, with the return of the pre-existing symptomatology [4, 10].
This syndrome is more likely to occur in elderly women, who tend to have loose subcutaneous tissue, but several other risk factors have been described to facilitate its development: inadequate fixation of the IPG to the muscular fascia, excessive enlargement of the subcutaneous pocket, increasing age, female gender, obesity and, in particular, neurological and psychiatric disorders [10, 11]. Because of the latter, since medically refractory OCD is becoming a more frequent indication for DBS, the possibility of TS in this subset of patients must be considered when a system malfunction is identified, because the obsessive behaviors could facilitate its occurrence [6]. In the present case, in fact, the patient and her relatives reported frequent manipulation of the device at both the thoracic and cranial (at the connector position) locations. Compulsive manipulation of the device is a feature observed in OCD patients and could also lead to wound complications and infections [4]. Touching and checking compulsions are often performed with the dominant hand, making the right-hand dominance of our patient a possible explanation for the monolateral manipulation of the device.
To rule out a fracture in the DBS system, skull and thorax x-ray are advisable. TS can be radiologically evident as a double-helix or braided pattern in the extension cable [3] or in the DBS lead.
The treatment of TS (when necessary) consists of replacing the malfunctioning or fractured part(s) of the system. The removal of the DBS electrode and implantation of a new one carry a risk of intracranial hemorrhage [4, 14]. To recognize the site of malfunction and lessen the surgical risk coming from a further stereotactic procedure, neurophysiological intraoperative checking of the electrode’s impedance is necessary.
Some technical precautions have been proposed in the literature to avoid TS, including anchoring of the IPG and wires to the thoracic muscular fascia with non-absorbable sutures as well as placement of the IPG into fixable polyester pouches within the infrapectoral region, in a sub-fascial position [10] or in the upper back [5]. In our patient, we decided to anchor the IPG to the muscle fascia with multiple silk sutures. This precaution prevents IPG rotation and caudal migration in the subcutaneous tissue, which, especially in a fat patient, could hinder the reload of a rechargeable IPG because of excessive subcutaneous tissue being interposed between the IPG and recharger. A difficult recharge may also trigger the manipulation of the device. Moreover, the patient underwent a psychiatric consultation, which ascertained that she was aware of the benefit of DBS and was motivated to avoid further touching of the IPG area. Her relatives assured us they would help her.
Our patient is overweight, which could have played a role in the rotation of the IPG in the abundant subcutaneous tissue. Moreover, she is affected by OCD and reported frequent manipulation of the IPG at multiple sites, predisposing her to develop TS. TS may develop either spontaneously or as the result of intentional compulsive manipulation, with the latter occurrence being described as either a “de novo” compulsion in patients not affected by OCD or a new compulsion in an OCD patient [6, 9]. Considering the small number of patients treated for OCD worldwide, and the even scarcer reporting of TS in those patients, it is impossible to identify predictive factors for this complication. We could only hypothesize that, in a specific subpopulation of patients with OCD, the presence of a DBS system could be a trigger for the development of new compulsions. Further studies have to be done to confirm our hypothesis and determine specific risk factors.
OCD has various presentations. Symptoms are different among patients, and they can also change or multiply over time in the same subject [8, 11, 13]. A meticulous assessment of the patient’s symptoms (in our case performed using the y-BOCS V checklist) is mandatory in the evaluation of eligibility for DBS. An examination of each compulsion and the possibly adjustment over time could be useful to identify those patients who may need a more intensive schedule of postoperative evaluations. Patients with touching or checking compulsions and those with a history of rapidly modifying symptoms could be selected for in-depth analysis for the development of TS. As we said before, more studies with larger samples are needed to confirm our hypothesis and findings. Indeed, one could hypothesize that the presence of compulsions related to touching objects may play a determining role in this complication.
In conclusion, TS must be carefully considered when trying to explain or rule out a cause of hardware malfunction in patients with psychiatric pathologies (especially OCD). A specific warning about the risks of IPG manipulation and connection wires should be given to all patients.
Moreover, when rechargeable IPGs are positioned in patients with abundant subcutaneous tissue, it could be useful to fix them properly in a more superficial location to facilitate the recharge and avoid migration and continuous manipulation, which could cause rotation until TS.
Abbreviations
- DBS:
-
Deep brain stimulation
- OCD:
-
Obsessive-compulsive disorder
- TS:
-
Twiddler’s syndrome
- IPG:
-
Implantable pulse generator
References
Astradsson A, Schweder PM, Joint C, Green AL, Aziz TZ (2011) Twiddler’s syndrome in a patient with a deep brain stimulation device for generalized dystonia. J Clin Neurosci 18:970–972
Bayliss CE, Beanlands DS, Baird RJ (1968) The pacemaker-twiddler’s syndrome: a new complication of implantable transvenous pacemakers. Can Med Assoc J 99:371–373
Burdick AP, Okun MS, Haq IU, Ward HE, Bova F, Jacobson CE, Bowers D, Zeilman P, Foote KD (2009) Prevalence of twiddler’s syndrome as a cause of deep brain stimulation hardware failure. Stereotact Funct Neurosurg 88:353–359
Carvallo JFD, Simpson R, Jankovic J (2011) Diagnosis and treatment of complications related to deep brain stimulation hardware. Mov Disord 8:1398–1406
Garg A, Mohan AL, Garell PC (2010) Placement of the internal pulse generator for deep brain stimulation in the upper back to prevent fracture of the extension wire due to generator rotation: case report. Park Dis 8
Machado AG, Hiremath GK, Salazar F, Rezai A (2005) Fracture of subthalamic nucleus deep brain stimulation hardware as a result of compulsive manipulation: case report. Neurosurgery 57:1318
Menghetti C, Zekaj E, Saleh C, Porta M, Servello D (2014) How to avoid twiddler’s syndrome in deep brain stimulation for dystonia. Neuromodulation 17:198–199
Mataix-Cols D, Rauch SL, Baer L, Eisen JL, Shera DM, Goodman WK, Rasmussen SA, Jenike MA (2002) Symptom stability in adult obsessive-compulsive disorder: data from a naturalistic two-year follow-up study. Am J Psychiatry 159(2):263–268
Moliz N, Katati MJ, Ianez B, Garcia A, Yagui E, Horcajadas A (2015) A twiddler's syndrome in a patient with obsessive-compulsive disorder treated with deep brain stimulation. Neurocirurgia 26(4):196–199
Penn DL, Wu C, Skidmore C, Sperling MR, Sharan AD (2012) Twiddler’s syndrome in a patient with epilepsy treated with deep brain stimulation. Epilepsia 53(7):e119–e121
Rufer M, Grothusen A, Mass R, Peter H, Hand I (2005) Temporal stability of symptom dimensions in adult patients with obsessive-compulsive disorder. J Affect Disord 88(1):99–102
Samuelsson J, Blomstedt P (2014) Twiddler’s syndrome in a patient with dystonic tremor treated with DBS. Open J Mod Neurosurg 4:193–195
Skoog G, Skoog I (1999) A 40-year follow-up of patients with obsessive compulsive disorder. Arch Gen Psychiatry 56:121–127
Sobstyl MR, Zabek M, Brzuszkiewicz-Kuzmicka G, Pasterski T (2017) Dual anchor internal pulse generator technique may lower risk of twiddler’s syndrome: a case series and literature review. Neuromodulation 9
Videnovic A, Verhagen Metman L (2008) Deep brain stimulation for Parkinson’s disease: prevalence of adverse events and need for standardized reporting. Mov Disord 3:343–349
Contributors
AF and GM contributed to the conception and design of the article, data acquisition, analysis and interpretation. All the authors were involved in critically drafting/revising the article for important intellectual content. Finally, they all gave final approval of the version to be published.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None
Consent
The patient has consented to submission of this case report to the journal.
Rights and permissions
About this article
Cite this article
Franzini, A., Ranieri, R., Gambini, O. et al. Manipulating an internal pulse generator until twiddler’s syndrome in a patient treated with deep brain stimulation for obsessive-compulsive disorder. Acta Neurochir 160, 389–392 (2018). https://doi.org/10.1007/s00701-017-3412-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3412-9