Abstract
Background
Several different techniques exist to treat degenerative lumbar foraminal stenosis. Failure to adequately decompress the lumbar foramen may lead to failed back surgery syndrome. However, wide decompression often causes spinal instabilities or may require an additional fusion surgery. The aim of this study was to report the outcomes of endoscopic partial facetectomy (EPF) performed on patients with degenerative lumbar foraminal stenosis.
Methods
Between 2012 and 2014, 25 consecutive patients (12 women and 13 men) who underwent EPF were included in the study. The patients were assessed before surgery and followed-up regularly during outpatient visits (preoperatively and 1, 3, 6, 12, and 24 months postoperatively). The clinical outcomes were evaluated using the visual analog scale (VAS), Oswestry Disability Index (ODI), and Short Form-36 (SF-36) outcome questionnaire. The radiological outcome was measured using the lumbar Cobb angle, disc wedging angle, lumbar lordosis (LL), slip percentage, and disc height index (DHI) in plain standing radiographs.
Results
The VAS, ODI, and SF-36 scores significantly improved at 1 month of follow-up compared with the baseline mean values and were maintained within the 2-year follow-up period. There was no radiologic progression in the lumbar Cobb’s angle, disc wedging angle, LL, slip percentage, and DHI between preoperatively and 2 years postoperatively. In addition, the EPF with discectomy group and the EPF group were not significantly different in terms of clinical and radiological outcomes.
Conclusions
EPF is an effective option in decompressing the lumbar exiting nerve root without causing spinal instabilities for the treatment of patients with lumbar foraminal stenosis.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Degenerative lumbar foraminal stenosis is a condition in which a nerve root or spinal nerve is entrapped in a narrowed lumbar foramen in degenerative lumbar spinal disorders [9, 13, 20]. The circumferential narrowing of the space available for the exiting nerve root leads to back pain and radicular symptoms. Impingement of the foraminal canal has also been implicated as a cause of failed back surgery syndrome due to an unrecognized or possibly inadequate treatment of foraminal stenosis [5]. Therefore, it is an important pathology in recognizing outcomes both clinically and radiographically in the treatment of patients with radicular pain. However, the preferred surgical treatment to relieve the compression on the exiting nerve root has not been established yet. Several different techniques for degenerative lumbar foraminal stenosis have been described, including foraminotomy, facetectomy, partial pediculectomy, fusion, and distraction instrumentation. Traditionally, decompression with a spinal fusion is utilized as a primary treatment in patients with degenerative lumbar foraminal stenosis, even in the absence of a gross instability, partly because of the limitations of the effective decompression tools. To solve these problems, several authors reported that a paraspinal approach [21, 27] and various minimally invasive techniques have been developed [15, 22, 24, 29]. We performed endoscopic partial facetectomy (EPF) using an endoscopic osteotome for degenerative lumbar foraminal stenosis. The purpose of this study is to describe the EPF procedure and report its clinical and radiological outcomes.
Materials and methods
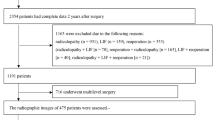
Between January 2012 and January 2014, EPF was performed on 32 patients. The patients underwent relevant clinical and radiological investigations, and an adequate follow-up was possible in 25 patients. Seven patients were excluded owing to an incomplete follow-up. One patient was lost to follow-up because she had undergone a revision fusion surgery in another hospital due to severe radicular symptoms by our phone request information. Six patients were also lost to follow-up because they did not come to the hospital despite our phone requests for the postoperative follow-up. A total of 25 consecutive patients (12 women and 13 men) who underwent EPF were retrospectively reviewed. The inclusion criteria of this study were degenerative lumbar foraminal stenosis with unilateral radicular symptoms. Patients with clear instabilities, central canal stenosis, and/or bilateral symptoms were excluded. All patients underwent a continuous conservative treatment, including medicine, physical therapy, and selective nerve root block therapy for a minimum of 6 weeks before surgery. The radiographic indications were moderate to severe foraminal stenosis with perineural fat obliteration or nerve root collapse based on the Wildermuth grading system [26]. All patients were assessed before surgery and followed-up regularly during outpatient visits (preoperatively and 1, 3, 6, 12, and 24 months postoperatively). The study was approved by the Clinical Research Ethics Committee of Pusan National University Hospital.
Surgical technique
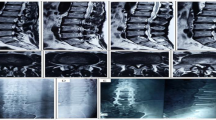
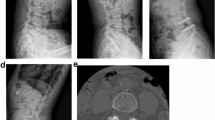
The EPF procedure was performed under local anesthesia. As a premedication, midazolam (0.05 mg/kg) was injected intramuscularly 30 min before surgery. Dexmedetomidine (1 µg/kg within 10 min for the loading dose and 0.2–0.7 µg/kg/h for the maintenance dose) was intravenously administered during surgery. The patients were placed in the prone position on a radiolucent table. The skin entry point was located on the lateral edge of the paravertebral back muscle (about 8–13 cm lateral to the midline, depending on the patient’s waist size), and local anesthesia was administered to the intervertebral foramen and facet joint. The target point of initial needling was the surface of the facet joint, with the needle firmly engaged into the facet joint and then replaced by a guidewire under a lateral fluoroscopic control. A tapered obturator was inserted over the guidewire not to the intervertebral foramen but to the facet joint, which prevents an exiting nerve root damage and enables a safe working space without a direct contact on the exiting nerve root (Fig. 1). After the correct placement of the obturator on the facet surface, a beveled working cannula was introduced over the obturator. After the obturator was withdrawn, an endoscope was inserted. Initially, the surgeon can view the surface of the facet joint via an endoscopic visualization. After the soft tissue, capsule, and cortical bone of the facet joint were removed using an endoscopic burr and a low-energy bipolar radiofrequency, the cancellous bone of the facet joint was exposed (Fig. 2a and b). Once the joint was identified via endoscopic visualization, osteotomy of the superior articular process was performed using several custom-made endoscopic osteotomes (Fig. 3a and b). Although the superior articular process can be mobilized after osteotomy, removal of the bony fragments may be difficult. Because the capsule and ligament were firmly attached to the facet, the bony fragments can be removed by manipulating with a beveled obturator engaged to the osteotomy site (Fig. 3c and d). After the hypertrophied superior articular process was removed, the intraforaminal structures, such as the foraminal ligament, ligament flavum, perineural fat, and disc surface should appear clearly. Thereafter, the hypertrophied ligament flavum and osteophyte around the exiting nerve root were removed using endoscopic forceps and punch. A flexible probe under endoscopic view was used to confirm an adequate decompression by mobilizing the exiting nerve root (Fig. 4a and b). After all instruments were removed, direct closure of the skin was performed. No drainage was required. All patients were compared in terms of the extent of decompression via magnetic resonance imaging preoperatively and 1 day postoperatively (Fig. 5a and b), discharged within 5 days after surgery, and provided with a back brace for 2 weeks.
a Once the joint is identified via endoscopic visualization, osteotomy of the superior articular process is performed using an endoscopic osteotome. b Osteotomized superior articular process on an intraoperative endoscopic view. c Because the capsule and ligament are firmly attached to the facet, the bony fragments can be removed by manipulating with a beveled obturator engaged to the osteotomy site. d After the hypertrophied superior articular process is removed, the articular cartilage in the facet joint is seen on an intraoperative endoscopic view
Illustrated case of a 70-year-old male patient. a Preoperative magnetic resonance (MR) image showing foraminal stenosis with disc herniation at the right L5/S1 level. b Postoperative MR image showing decompression of the stenotic foramen and visualization of the exiting nerve root 1 day after surgery
Measurements of the clinical and radiological outcomes
At each visit, the patients were asked to complete an outcome questionnaire, and plain radiographs were obtained. The clinical outcomes were evaluated using the visual analog scale (VAS), Oswestry Disability Index (ODI), and Short Form-36 (SF-36) outcome questionnaire (preoperatively and 1, 3, 6, 12, and 24 months postoperatively). The radiological parameters were measured preoperatively and 1 and 2 years postoperatively. The radiological outcome was measured using the lumbar Cobb angle, disc wedging angle, lumbar lordosis (LL), slip percentage, and disc height index (DHI) in plain standing radiographs. Plain standing radiographs were obtained in all patients, and changes in the radiographs were evaluated in terms of the lumbar Cobb angle and disc wedging angle at the affected level on the anteroposterior view. The LL, slip percentage, and DHI were checked at the affected level on the lateral plain radiograph. The slip percentage, which is the degree of slip as a percentage of the anteroposterior diameter of the superior margin of the lower vertebra, was calculated using the Taillard method [25]. The DHI, which is the ratio of the mean of the disc height (three-point disc height at each operated level) to the mean sagittal diameter of the consecutive vertebra, was calculated from the midvertebral level using the modified Inoue method [11] (Fig. 6). Radiological progression was defined as ≥5° Cobb angle progression, ≥3° disc wedging progression, ≥5% slip percentage progression, and/or ≥2 mm disc height (≥5% DHI) progression [29]. All measurements were performed twice independently by three spine surgeons with an interval of 2 weeks between the two measurements to decrease intraobserver (Pearson correlation coefficient, 0.919; range, 0.884–0.940) and interobserver errors (Pearson correlation coefficient, 0.910; range, 0.873–0.930).
Radiologic measurement of DHI at the affected level. A, B (white line): sagittal diameter from the midvertebral level of the consecutive vertebra; 1 (black line): the line between the anterior/superior corner of the upper vertebra and anterior/inferior corner of the lower vertebra; 2 (black line): the line between the middle/superior point of the upper vertebra and middle/inferior point of the lower vertebra; 3 (black line): the line between the posterior/superior corner of the upper vertebra and posterior/inferior corner of the lower vertebra; a, b, c measured disc height on lines 1, 2, and 3. Disc height index (DHI) measured using the modified Inoue method was calculated using the following formula: DHI (%) = {[(a + b + c)/3]/[(A + B)/2]} × 100
Statistical analysis was performed using the SPSS 21 software for Windows (SPSS, Chicago, IL, USA). Data were expressed as means ± standard deviations. The clinical and radiological outcomes were compared using the ANOVA test and t-test, if appropriate. The post-test was used to analyze individual differences. A P < 0.05 was regarded as statistically significant.
Results
Adequate clinical and radiological follow-ups were available for 25 patients. The average age at the time of surgery was 66.1 (48–82) years. Twelve patients were women, and 13 patients were men. Four patients had surgery at two levels (L3/4/5 in one case and L4/5/S1 in three cases), and 21 patients had surgery at a single level (L2/3 in two cases, L3/4 in one case, L4/5 in nine cases, and L5/S1 in nine cases). Of the EPF performed, 15 cases were left-sided, and 10 cases were right-sided. We performed EPF with an additional discectomy (EPF with discectomy group) in 11 patients and only EPF without discectomy (EPF group) in 14 patients.
The clinical outcomes were evaluated using the VAS, ODI, and SF-36 outcome questionnaire (preoperatively and 1, 3, 6, 12, and 24 months postoperatively). The baseline preoperative mean values of the VAS, ODI, and SF-36 were 74.6, 48.1, and 34.4, respectively. Compared with the baseline mean values, the 1- and 3-month follow-up values showed significant improvements. Similar results were observed for the 2-year follow-up scores (Table 1). The EPF with discectomy group and the EPF group were not significantly different in terms of VAS, ODI, and SF-36 scores (Table 2).
The radiological parameters were measured preoperatively, and 1 and 2 years postoperatively (Table 3). There were no significant differences in the lumbar Cobb angle, disc wedging angle, LL, and slip percentage preoperatively, and 1 and 2 years postoperatively. The DHIs decreased during the follow-up periods compared with the preoperative baseline values; however, there was no statistical significance. In addition, the preoperative and 1- and 2-year postoperative DHIs did not significantly differ between the EPF with discectomy group and the EPF group (Table 4).
In the present study, there were four patients with transient postoperative dysesthesia, which improved during the follow-up with medications and selective nerve root block. There were no other serious complications in our study. Follow-up images on dynamic X-ray showed no instability at the operated or any adjacent segments.
Discussion
Loss of intervertebral disc height secondary to degeneration allows the superior articular process of the inferior vertebra to subluxate anteriorly and superiorly, diminishing the foraminal area. Lumbar exiting nerve roots may be compressed in anteroposterior and/or craniocaudal directions [13, 19]. Anteroposterior foraminal stenosis attributes to transverse compression between the superior articular facet and posterior vertebral body. Craniocaudal foraminal stenosis is caused by a protrusion of the posterolateral osteophytes from the vertebral endplates into the foramen with a laterally bulging disc, compressing the nerve root against the superior pedicle [29]. The L5 nerve root may also be compressed by the L5 transverse process, sacral ala, or lumbosacral ligament in the extraforaminal zone [18, 28]. Moreover, dynamic factors contribute to foraminal stenosis [7, 12].
Two surgical treatments are available for patients with degenerative lumbar foraminal stenosis: total facetectomy with/without fusion and facet-preserving decompression. Total facetectomy offers sufficient decompression through the nerve root course. However, this often leads to segmental instability and back pain, which may eventually necessitate revision surgeries with fusion [1, 6, 8, 13, 21]. Important structural ligaments that can be affected with conventional facetectomy include the supraspinous, interspinous, and intertransverse ligaments with the superficial thoracolumbar fascia and various interspinous muscles depending on the approach and technique used. Although fusion is usually indicated for preoperative instabilities or deformities, facet-preserving decompression is more desirable as the primary treatment in patients with degenerative lumbar foraminal stenosis in the absence of gross instabilities. Haufe and Mork [10] reported good results in the sagittal rotational or translational motion after unilateral endoscopic total facetectomy for the treatment of severe foraminal stenosis. However, their total facetectomy using the endoscopic system can cause instabilities of the spine. It is well known that the facet joints have an important role in stabilizing the lumbar joints, and the posterior annulus is protected by the facet joint, especially in axial rotation [2, 16, 17]. So a facet-preserving foraminotomy through a paraspinal approach was introduced [21, 27], and many surgeons reported good results using modified methods of this technique [4, 8, 10, 23, 29].
Recently, endoscopic lumbar foraminotomy has been performed, but there is a concern about safety because an endoscopic burr should be used to decompress the stenotic foramen [4]. We performed EPF using an osteotome, which is a more simplified and safe procedure than foraminoplasty using a burr, for degenerative lumbar foraminal stenosis. None of the patients had any statistically significant changes in the radiological parameters, including instability and progression of scoliosis or kyphosis after EPF for 2 years of follow-up. Thus, EPF can be one of the safe and sufficient methods for the treatment of degenerative lumbar foraminal stenosis in selected cases. An advantage of EPF is that it can be safely performed without the need for fusion or instrumentation and preserve the stability of the spine. However, as with other endoscopic surgeries, the inherent disadvantage of EPF is its high exposure to radiation. Ahn et al. [3] compared the radiation dose of percutaneous endoscopic lumbar discectomy (PELD) with open lumbar microdiscectomy and minimally invasive surgery (MIS) microdiscectomy. The mean radiation dose of PELD was much greater than that of MIS microdiscectomy or open microdiscectomy. This implies that a less invasive discectomy technique inevitably results in more radiation exposure for the surgeons, and medical staffs.
Recently, several minimally invasive techniques for the treatment of lumbar foraminal stenosis have been described in the literature with good results [4, 14, 29]. In the present study, the clinical outcomes of VAS, ODI, and SF-36 significantly improved after surgery. Furthermore, the clinical outcomes between the EPF with discectomy group and EPF group were not significantly different. Because an aggressive discectomy may cause an exiting nerve root injury during the EPF procedure and/or loss of disc height at follow-up, only EPF or EPF with a minimal discectomy, as necessary, will be required in patients with degenerative lumbar foraminal stenosis.
This study has several limitations that require consideration. First, the number of subjects tested was relatively small and no control group was used, which diminished the statistical power of the study. Second, because of the relatively short follow-up period, further studies with larger number of patients and long-term outcomes are needed. Third, even though the clinical and radiological outcomes were similar between the EPF with discectomy group and EPF group, we do not know the correlation between the degree of discectomy and outcomes because we did not check the volume, extent, and ratio of the removed disc contents. Fourth, seven patients were excluded owing to an incomplete follow-up. Fifth, we did not distinguish between back pain and leg pain, but overall pain was measured by VAS. Assessment of overall pain using VAS may not accurately reflect radicular problems.
In conclusion, EPF is a safe and effective option in decompressing the lumbar exiting nerve root without causing spinal instabilities for the treatment of patients with lumbar foraminal stenosis.
References
Abumi K, Panjabi MM, Kramer KM, Duranceau J, Oxland T, Crisco JJ (1990) Biomechanical evaluation of lumbar spinal stability after graded facetectomies. Spine 15:1142–1147
Adams MA, Hutton WC (1981) The relevance of torsion to the mechanical derangement of the lumbar spine. Spine 6:241–248
Ahn Y, Kim CH, Lee JH, Lee SH, Kim JS (2013) Radiation exposure to the surgeon during percutaneous endoscopic lumbar discectomy: a prospective study. Spine 38:617–625
Ahn Y, Oh HK, Kim H, Lee SH, Lee HN (2014) Percutaneous endoscopic lumbar foraminotomy: an advanced surgical techinique and clinical outcomes. Neurosurgery 75:124–133
Burton CV, Kirkaldy-Willis WH, Yong-Hing K, Heithoff KB (1981) Causes of failure of surgery on the lumbar spine. Clin Orthop Relat Res 157:191–199
Epstein NE (2002) Foraminal and far lateral lumbar disc herniations: surgical alternatives and outcome measures. Spinal Cord 40:491–500
Fujiwara A, An HS, Lim TH, Haughton VM (2001) Morphologic changes in the lumbar intervertebral foramen due to flexion-extension, lateral bending, and axial rotation: an in vitro anatomic and biomechanical study. Spine 26:876–882
Garrido E, Connaughton PN (1991) Unilateral facetectomy approach for lumbar disc herniation. J Neurosurg 74:754–756
Hasegawa T, An HS, Haughton VM, Nowicki BH (1995) Lumbar foraminal stenosis: critical heights of the intervertebral disc and foramina. A cryomicrotome study in cadevera. J Bone Joint Surg Am 77:32–38
Haufe SM, Mork AR (2007) Effects of unilateral endoscopic facetectomy on spinal stability. J Spinal Disord Tech 20:146–148
Inoue H, Ohmori K, Miyasaka K, Hosoe H (1999) Radiographic evaluation of the lumbosacral disc height. Skelet Radiol 28:638–643
Inufusa A, An HS, Lim TH, Hasegawa T, Haughton VM, Nowicki BH (1996) Anatomic changes of the spinal canal and intervertebral formen associated with flexion-extension movement. Spine 21:2412–2420
Jenis LG, An HS (2000) Spine update. Lumbar foraminal stenosis. Spine 25:389–394
Kang K, Rodriguez-Olaverri JC, Schwab F, Hashem J, Razi A, Farcy JP (2014) Partial facetectomy for lumbar foraminal stenosis. Adv Orthop 2014:534658. doi:10.1155/2014/534658
Knight MT, Vajda A, Jakab GV, Awan S (1998) Endoscopic laser foraminoplasty on the lumbar spine—early experience. Minim Invasive Neurosurg 41:5–9
Kunogi J, Hasue M (1991) Diagnosis and operative treatment of intraforaminal and extraforaminal nerve root compression. Spine 16:1312–1320
Natarajan RN, Adnersson GB, Patwardhan AG, Andriacchi TP (1999) Study on effect of graded facetectomy on change in lumbar motion segment torsional flexibility using three-dimensional continuum contact representation for facet joints. J Biomech Eng 121:215–221
Nathan H, Weizenbluth M, Halperin N (1982) The lumbosacral ligament (LSL), with special emphasis on the “lumbosacral tunnel” and the entrapment of the 5th lumbar nerve. Int Orthop 6:197–202
Ploumis A, Transfeldt EE, Gilbert TJ Jr, Mehbod AA, Dykes DC, Perra JE (2006) Degenerative lumbar scoliosis: radiographic correlation of lateral ratatory olisthesis with neural canal dimensions. Spine 31:2353–2358
Porter RW, Hibbert C, Evans C (1984) The natural history of root entrapment syndrome. Spine 9:418–421
Reulen HJ, Pfaundler S, Ebeling U (1987) The lateral microsurgical approach to the “extracanalicular” lumbar disc herniation. I: A technical note. Acta Neurochir (Wein) 84:64–67
Schubert M, Hoogland T (2005) Endoscopic transforaminal nucleotomy with foramnioplasty for lumbar disk herniation. Oper Orthop Traumatol 17:641–661
Sharma M, Langrana NA, Rodriguez J (1995) Role of ligaments and facets in lumbar spinal stability. Spine 20:887–900
Shenouda EF, Gill SS (2002) Laminal fenestration for the treatment of lumbar nerve root foraminal stenosis. Br J Neurosurg 16:494–496
Taillard W (1954) Spondylolisthesis in children and adolescents. Acta Orthop Scand 24:115–144
Wildermuth S, Zanetti M, Duewell S, Schmid MR, Romanowski B, Benini A, Boni T, Hodler J (1998) Lumbar spine: quantitative and qualitative assessment of positional (upright flexion and extension) MR imaging and myelography. Radiology 207:391–398
Wiltse LL, Spencer CW (1988) New uses and refinements of the paraspinal approach to the lumbar spine. Spine 13:696–706
Wiltse LL, Guyer RD, Spencer CW, Glenn WV, Porter IS (1984) Alar transverse process impingement of the L5 spinal nerve: the far-out syndrome. Spine 9:31–41
Yamada K, Matsuda H, Cho H, Habunaga H, Kono H, Nakamura H (2013) Clinical and radiological outcomes of microscopic partial pediculectomy for degenerative lumbar forminal stenosis. Spine 38:E723–E731
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
None
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Youn, M.S., Shin, J.K., Goh, T.S. et al. Clinical and radiological outcomes of endoscopic partial facetectomy for degenerative lumbar foraminal stenosis. Acta Neurochir 159, 1129–1135 (2017). https://doi.org/10.1007/s00701-017-3186-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-017-3186-0