Abstract
Aims
To address questions regarding onset and progression of types 1 and 2 diabetes (T1D/T2D), surrogate imaging biomarkers for beta cell function and mass are needed. Here, we assess the potential of GPR44 as a surrogate marker for beta cells, in a direct comparison with clinically used biomarker VMAT2.
Methods
GPR44 surface availability was assessed by flow cytometry of human beta cells. RNA transcription levels in different pancreas compartments were evaluated. The density of GPR44 receptor in endocrine and exocrine tissues was assessed by the radiolabeled GPR44 ligand [3H]AZD 3825. A direct comparison with the established beta cell marker VMAT2 was performed by radiolabeled [3H]DTBZ.
Results
GPR44 was available on the cell surface, and pancreatic RNA levels were restricted to the islets of Langerhans. [3H]AZD 3825 had nanomolar affinity for GPR44 in human islets and EndoC-βH1 beta cells, and the specific binding to human beta cells was close to 50 times higher than in exocrine preparations. The endocrine-to-exocrine binding ratio was approximately 10 times higher for [3H]AZD 3825 than for [3H]DTBZ.
Conclusion
GPR44 is a highly beta cell-specific target, which potentially offers improved imaging contrast between the human beta cell and the exocrine pancreas.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
There is considerable interest in development of novel surrogate biomarkers for beta cells, due to the fact that current blood markers correlate to beta cell function rather than mass. Proposed novel plasma markers of beta cell death and function may alleviate this issue, but these will in the best case still constitute an indirect measure of beta cell mass [1–3]. Molecular imaging of the pancreas has been proposed as a solution for this clinical need. Positron emission tomography (PET) is a quantitative and essentially noninvasive technique with the sensitivity required for clinical in vivo imaging of beta cell mass.
The anatomical localization of the beta cells in humans sets strict requirements on putative beta cell imaging biomarkers. The beta cells constitute approximately 60 % of the islets of Langerhans, cell clusters of varying size (5–500 µm) which are distributed heterogeneously within the exocrine parenchyma. Additionally, there are pancreatic beta cells not embedded in islets of Langerhans. Clinical PET scanners have sufficient resolution (approximately 3 mm) to image the whole or parts of the pancreas, but not individual islets. Therefore, the aim is to measure the integrated pancreatic signal of a beta cell biomarker, which potentially correlates to the present beta cell mass in the individual.
Consequently, imaging biomarkers (for example a receptor) must combine high expression in beta cells with low expression in exocrine and other endocrine cells. Additionally, a suitable PET ligand must have high affinity to the target receptor, combined with low-to-negligible non-target interactions. Several target receptors and enzymes have previously been suggested as suitable biomarkers, most notably the vesicular monoamine transporter 2 (VMAT2) [4], the glucagon-like peptide-1 receptor (GLP-1R) [5] and DOPA decarboxylase [6]. However, despite promising preclinical data only few clinical studies on imaging of beta cells in T1D and the healthy condition have yet been published—two employing analogues of the VMAT2 high-affinity ligand dihydrotetrabenazine (DTBZ) [7, 8], one using Indium-111 labeled Exendin4 [9] and one using the serotonin precursor [11C]5-Hydroxy-Tryptophan [10]. Unexpectedly high radiotracer uptake was found in the beta cell-deficient T1D pancreas in each of these clinical studies, raising doubt on the beta cell selectivity of the respective target. Novel imaging targets are therefore required in order to increase the imaging contrast between the beta cells and the remaining pancreatic tissue [11, 12].
Recently the G coupled protein GPR44 that bind endogenous Prostaglandin D2 (PGD2) has been identified as a beta cell-specific biomarker through proteomic screening [13]. GPR44 is also designated as the prostaglandin D2 receptor 2 (PTGDR2), chemoattractant receptor-homologous expressed on Th2 lymphocytes receptor (CRTH2) or CD294. Here, we have quantified the density of the GPR44 receptor in endocrine (isolated human islets and human and rodent beta cell lines) and exocrine tissues by the radiolabeled GPR44 ligand AZD 3825. To assess the potential of GPR44 as a surrogate marker for beta cells, we performed a direct comparison with radiolabeled DTBZ.
Method and materials
Chemicals
[3H]AZD 3825 (specific activity 22.2 Ci/mmol) and unlabeled AZD 3825 were synthesized by AstraZeneca, Mölndal, Sweden. [3H]DTBZ (specific activity 20 Ci/mmol) was purchased from American Radiolabeled Chemicals (St Louis, MO, USA). Tetrabenazine (TBZ) was obtained from Biotrend AG (Zurich, Switzerland). [3H]PGD2 (160 Ci/mmol) was obtained from PerkinElmer Life Sciences (Boston, MA, USA).
Cell culture
The human beta cell line EndoC-βH1 [14] was obtained from Endocells (Paris, France) and cultured according to the provider in DMEM low glucose supplemented with 2 % BSA fraction V (Roche Diagnostics, Indianapolis, IN), 50 µM 2-mercaptoethanol (Sigma-Aldrich, St Louis, MO), 10 mM nicotinamide (VWR), 5.5 µg/ml transferrin and 6.7 ng/ml sodium selenite.
The rat insulinoma cell line INS-1 was obtained from Dr Hans Hohmeier (Duke University Medical Center, Durham, NC) and cultured in RPMI 1640 supplemented with 10 % FBS, 2 mM l-glutamine, 10 mM HEPES, 1 mM sodium pyruvate and 50 µM 2-mercaptoethanol.
Homogenized Human Embryonic Kidney (HEK) 293 cells overexpressing GPR44 were used for a [3H]PGD2 binding assay as described previously [15].
All cell culture reagents were from Life Technologies (Carlsbad, CA, USA) except when stated otherwise.
Human tissue
The use of human tissue was approved by the Uppsala Ethical Review Board (#2011/473, #Ups 02-577). Isolated pancreatic islets and exocrine tissue were obtained within the Nordic network for Clinical islet Transplantation laboratory in Uppsala, Sweden. Isolation procedures and culturing conditions have been described previously [15–17]. Fresh frozen tissue including two pancreatic samples with normal histology was obtained from Uppsala Biobank.
RNA analysis
RNA preparation and analysis were conducted within the Human Protein Atlas project [18].
Preparation of tissue
Fresh frozen tissue was imbedded in OCT compound (Sakura Finetek, Alphen aan den Rijn, the Netherlands) and used as source of RNA. Six sections of 10 µm each were cut using a cryotome and put into ice-cold RLT buffer (Qiagen, Hilden, Germany) and mixed by vortex. RNA from the islet and exocrine preparations was extracted without imbedding. Samples were stored in −70 °C until RNA extraction.
RNA was extracted using the RNeasy mini kit (Qiagen) according to the manufacturer’s instructions. Disruption was conducted using a 3-mm steel grinding ball (VWR, Radnor, PA) and vortexing. Concentration and RNA integrity (RIN) were determined by Qubit 2.0 Fluorometer (Life Technologies) and Agilent 2100 Bioanalyzer (Agilent Technologies, Santa Clara, CA), respectively. Purity of the samples was confirmed by an A260/A280 value over 2.0 using Nanodrop (Thermo Scientific, Wilmington, DE). Samples with RIN values above 7.5 were sequenced by Illumina HiSeq 2000 and 2500 (Illumina, San Diego, CA) using the standard Illumina RNA-Seq protocol with a read length of 2 × 100 bases.
Analysis of data
The raw reads obtained from the sequencing system were trimmed for low-quality ends with the software sickle [19], using a phred quality threshold of 20. All reads shorter than 54 bp after the trimming were discarded. The processed reads were mapped to the GRCh37 version of the human genome with Tophat v2.0.3 [20]. Potential PCR duplicates were eliminated using the MarkDuplicates module of Picard 1.77 [21]. To obtain quantification scores for all human genes, FPKM (fragments per kilobase of exon model per million mapped reads) values were calculated using Cufflinks v2.0.2 [22], which corrects for transcript length and the total number of mapped reads from the library to compensate for different read depths for different samples. The gene models from Ensembl build 69 [23] were used in Cufflinks. In addition to Cufflinks, HTSeq v0.5.1 was run to calculate read counts for each gene, which were used for analyses of differentially expressed genes using the DESeq package [24]. All data were analyzed using R Statistical Environment [25] with the addition of package ‘gplots’ [26]. For analyses performed in this study where a log2-scale of the data was used, pseudocounts of +1 were added to the data set.
Flow cytometry
Surface expression of GPR44 on EndoC-βH1 cells was analyzed by flow cytometry. Cells were harvested enzymatically using accutase. Cells in suspension were stained by a rabbit polyclonal GPR44 antibody (HPA14259, Atlas Antibodies, Stockholm, Sweden) for 30 min at +4 °C. Staining of HLA-I (GTX61891, GeneTex, Irvine, CA) was used as a positive control of the detection antibody. An alexa-488 conjugated goat anti-rabbit antibody was used for detection (Life Technologies). Cells were analyzed on a BD FACSCanto II flow cytometer (BD Biosciences, San Jose, CA).
Preparation of tissue for in vitro binding studies
50–100 mg isolated endocrine (75–95 % islet purity) and exocrine tissues as well as EndoC-βH1 cells were homogenized in ice-cold 0.32 M sucrose by hand using a Dounce glass homogenizer to a final concentration of 6 mg/ml. 50–100 mg INS-1 was homogenized using a polytron tissue homogenizer (Polytron® PT 3000, Kinematica AG, Littay-Luzern, Switzerland) in ice-cold 0.32 M sucrose at a concentration of 6 mg/ml and then by hand using a Dounce glass homogenizer. Protein concentration was determined using Bio-Rad Protein Assay (Bio-Rad Laboratories, Hercules, CA) with bovine serum albumin as standard. Aliquots of the homogenates were stored at −80 °C until used.
AZD 3825 binding to GPR44
Potency of binding of AZD 3825 to GPR44 was determined by a [3H]PGD2 displacement assay on membrane fractions from HEK 293 cells overexpressing GPR44, over a range of concentrations as described previously [15]. The assay readout was the concentration of AZD 3825 giving 50 % of maximum inhibitory effect (IC50) on [3H]PGD2 binding.
In vitro binding assays for [3H]AZD 3825 and [3H]DTBZ
Two milligrams of homogenized endocrine, exocrine and insulinoma tissue, and 1 mg of homogenized EndoC-βH1 cells were incubated for 3 h in room temperature with 4 nM [3H]AZD 3825 (dissolved in ethanol, final concentration 1 %) and 50 mM TRIS (pH7.4) in a final incubation volume of 1 ml. Twenty micrograms of unlabeled AZD 3825 dissolved in ethanol (final concentration 0.5 %) was added for determination of non-specific binding. The samples were filtered using a Brandel M-48 cell harvester with Whatman GF/C filter (presoaked with 50 mM TRIS) and washed four times with 3 ml 50 mM TRIS (room temperature). Filters were put into scintillation vials and dried for 30 min before adding 10 ml Ultima Gold scintillation fluid (Perkin Elmer, Waltham, MA). The filters were shaken for 90 min and then counted in a β-counter (Packard Scintillator Tri-Carb 2100TR). Similar experiments with 4 nM [3H]DTBZ in ethanol were performed using 20 µM TBZ to estimate the non-specific binding. The Kd and Bmax values for [3H]AZD 3825 and [3H]DTBZ binding were determined using concentrations of the tritiated ligand from 1 to 15 nM. The specific binding was calculated by subtracting the non-specific binding from the total binding, and expressed as fmol/mg protein. All measurements were performed in triplicates. The binding data were analyzed with curve-fitting software (GraphPad Prism version 5.04) to obtain Kd and Bmax values.
Statistical analysis
When reported on group level, results are given as mean ± SEM. Differences between groups were assessed by nonparametric Mann–Whitney rank test using a 95 % confidence level.
Results
RNA analysis
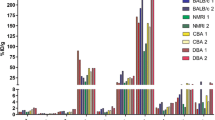
RNA analysis of different pancreas compartments shows higher transcripts levels of GPR44 in islets (5.2 FPKM) compared to exocrine tissue (0.2 FPKM) (Table 1). Similar levels as in islets were observed in small intestine and colon, while stomach had a slightly higher RNA expression of 8.2 FPKM. Transcript levels in other tissues were generally below 1 FPKM. Taken together, RNA analysis of a large panel of human tissues shows that there is a selective transcriptional expression of GPR44 restricted to islets in the pancreas and some cells in the gastrointestinal tract.
Surface expression of GPR44 in EndoC-βH1
To verify surface expression of GPR44, EndoC-βH1 was stained with an antibody against GPR44 and evaluated by flow cytometry. The majority of the cells were detected by the GPR44 antibody (Fig. 1). As a positive control, HLA-I was used, which gave a slightly higher positivity than GPR44, 84 % compared to 71 %. The secondary fluorescent antibody gave negligible background signal. This demonstrates that GPR44 is expressed in and available at the cell surface of EndoC-βH1.
Surface expression of GPR44 on EndoC-βH1 cells evaluated by flow cytometry. The majority of the cells were positive for GPR44 (upper histogram), slightly less than the HLA-1 control (middle histogram). The lower histogram shows the negative control represented by the secondary detection antibody alone
AZD 3825 binding to GPR44
AZD 3825 inhibited [3H]PGD2 binding on membrane fractions from HEK 293 cells overexpressing GPR44. The AZD 3825 displayed high potency for interacting with human GPR44 through competing with [3H]PGD2, with an IC50 of 0.98 nM (Table 2).
Initial experiments for optimizing in vitro binding of [3H]AZD 3825 and of [3H]DTBZ
Initial experiments with [3H]AZD 3825 and [3H]DTBZ in homogenates from endocrine tissue were performed to find optimal incubation time and amount of tissue needed. Binding reached a maximum between 150 and 180 min with [3H]AZD 3825 and after 90 min with [3H]DTBZ (data not shown). An incubation time of 180 min was chosen for all experiments. There was a linear increase in specific [3H]AZD 3825 and [3H]DTBZ binding using 0.5–2 mg tissue (r = 0.997 and 0.976, respectively). Binding to homogenates corresponding to 2 mg tissue was used in the final experiments. In comparison with different tissues (endocrine, exocrine, EndoC-βH1 cells and INS-1 insulinoma), a concentration of 4 nM [3H]AZD 3825 and [3H]DTBZ was chosen.
Comparison of [3H]AZD 3825 and [3H]DTBZ binding to endocrine and exocrine pancreatic tissues and EndoC-βH1 cells
For both [3H]AZD 3825 and [3H]DTBZ, there was higher amount of displaceable binding in endocrine compared to exocrine pancreatic tissue (p < 0.001, Fig. 2a).
[3H]AZD 3825 and [3H]DTBZ evaluated for specific and non-displaceable with binding at 4 nM ligand concentration. Non-displaceable binding was assessed by co-incubation with unlabeled ligand in excess. a Specificity of [3H]AZD 3825 and [3H]DTBZ in human pancreatic endocrine and exocrine preparations. b Amount of receptor bound [3H]AZD 3825 or [3H]DTBZ per mg protein in endocrine and exocrine preparations. c Comparison of endocrine-to-exocrine and EndoC-βH1-to-exocrine uptake ratio between [3H]AZD 3825 and [3H]DTBZ. d Amount of receptor bound [3H]AZD 3825 or [3H]DTBZ per mg protein in human EndoC-βH1 and rodent INS-1 cells
The specificity in endocrine tissue was not significantly different between [3H]AZD 3825 and [3H]DTBZ at 4 nM (56 ± 3 and 49 ± 5 %, respectively, Fig. 2a). In exocrine tissue, the percentage-specific binding was approximately 3 times lower for [3H]AZD 3825 compared to [3H]DTBZ (6.3 ± 2 and 22 ± 2 %, respectively, Fig. 2a). Specific binding of 4 nM [3H]AZD 3825 was almost 20 times higher in endocrine tissue compared to exocrine tissue (Fig. 2b, p < 0.001), while the specific binding of 4 nM [3H]DTBZ was only 2.2 times higher in endocrine tissue compared to exocrine tissue (Fig. 2b, p < 0.05). Accordingly, the important endocrine-to-exocrine uptake ratio was approximately 10 times higher for [3H]AZD 3825 (Fig. 2c). The absolute specific binding of [3H]DTBZ was significantly higher than binding of [3H]AZD 3825 in both endocrine (p < 0.001) and exocrine (p < 0.05) tissue. The specific binding of 4 nM [3H]AZD 3825 in EndoC-βH1 cells was significantly higher (p < 0.05) in comparison with endocrine tissue, whereas the specific binding of 4 nM [3H]DTBZ was similar in endocrine tissue and in EndoC-βH1 cells (Fig. 2d). The uptake ratio of [3H]AZD 3825 between the pure beta cells and the exocrine tissue was in excess of 90 (Fig. 2c). Very low or non-existent specific binding of [3H]AZD 3825 (0.88 ± 0.18 fmol/mg protein) and [3H]DTBZ (9.70 ± 1.55 fmol/mg protein) was detected in homogenates of INS-1 insulinoma xenografts (Fig. 2d).
Characteristics of [3H]AZD 3825 and [3H]DTBZ binding to endocrine and exocrine pancreatic tissue
Saturation experiments with 1–15 nM [3H]AZD 3825 and [3H]DTBZ were performed with homogenates of endocrine, exocrine tissue and EndoC-βH1 cells (representative graphs are shown in Supplementary Fig. 1). Nonlinear regression analysis of data for [3H]AZD 3825 binding to endocrine and exocrine tissue gave average Kd values of 1.39 and 1.87 nM and Bmax values of 31.9 and 5.0 fmol/mg protein, respectively (Table 3). The affinity of [3H]DTBZ to endocrine and exocrine tissue was approximately 6 and 9 times lower than that for [3H]AZD 3825, while the Bmax values were approximately 7 and 97 times higher in endocrine and exocrine tissues, respectively (Table 3). Kd obtained from saturation experiments with EndoC-βH1 cells was 1.18 nM for [3H]AZD 3825, which was similar to the value estimated for endocrine tissue, whereas Bmax was approximately 7 times higher in the EndoC-βH1 cells (Table 3).
Discussion
Efforts to find a biomarker for beta cell mass that can be targeted and studied noninvasively by imaging have yielded a few potential candidates. Analogues of DTBZ were the first PET ligands putatively targeting beta cells that were evaluated in prospective clinical studies aimed at visualizing native pancreatic beta cell mass. VMAT2 that DTBZ targets is, however, not completely restricted to beta cells as demonstrated in subjects with long-standing T1D where a decrease in binding of the ligand of not more than 15 % was observed [7]. Naively, one would expect receptor-specific radioligand binding to be decreased by close to 100 % in T1D, accompanying the near total loss of beta cells. Similarly when targeting the GLP-1R, a large overlap between groups of non-diabetic subjects and subjects with T1D was seen [9]. Assessment of serotonergic biosynthesis by DOPA decarboxylase in pancreas by PET could differentiate between non-diabetic subjects and subjects with T1D without overlap, but the serotonergic metabolic pathway is present in all pancreatic endocrine tissue and therefore not beta cell specific [10].
Herein, we have therefore quantified the expression and density of the recently identified beta cell biomarker GPR44 in pancreatic tissue [13], in order to investigate its potential future use for radionuclide imaging.
RNA analysis of a panel of human tissues showed that GPR44 is specific at the transcriptional level for endocrine cells in pancreas. Similar levels were observed in stomach and intestines, and further protein profiling using immunohistochemistry showed weak staining in stomach, negative staining in intestines whereas the staining of islet cells were strong (data not shown). We therefore believe that other organs in the abdominal tract will not interfere with signals from the pancreas in imaging applications. The same antibody was used to verify surface availability of the target in the recently established human beta cell line EndoC-βH1 [14] by flow cytometry. Since the majority of the cells were positive in this setting, it is likely that GPR44 is targetable at the surface, i.e., internalization of ligands is unnecessary.
Binding assays using the tritiated GPR44 ligand AZD 3825 shows preferential accumulation in the human endocrine pancreas, with minor binding to exocrine preparation. The affinity to endocrine and exocrine preparations did not differ, indicating a structurally similar or identical target protein. This is in contrast to DTBZ binding which could be found in high density mainly in endocrine, but also exocrine pancreatic preparations. Furthermore, the affinity in exocrine tissue was higher, indicating displaceable interactions to target proteins other than VMAT2. For example, [18F]FP-DTBZ has been shown to interact with Sigma receptors with low affinity but high capacity especially in the rat exocrine pancreas [27]. We previously found similar results when assessing two Fluorine-18 labeled DTBZ analogues for beta cell specificity [28, 29]. These observations, and those of other reports [30, 31], may partially explain the difficulties encountered in visualizing human beta cells by targeting VMAT2.
The binding studies were performed on islet and exocrine homogenates. This assay does not rule out also binding to exposed intracellular epitopes. Repetition of these studies using intact viable human islets could rule out this possibility.
Furthermore, the endocrine pancreas also contains nervous tissue such as Schwann cells. The assay using homogenates of endocrine pancreatic homogenates does not exclude the presence of receptors also on non-islet nervous tissue. However, the IHC staining in the HPA database was negative for GPR44 in most CNS tissue including glial cells [32]. Quantitative in vitro autoradiography using AZD 3825 labeled by a positron emitting nuclide, with corresponding insulin staining of consecutive sections, must be performed in order to verify the extent of overlap between tracer receptor binding and the Islets of Langerhans.
Only minor uptake of AZD 3825 was observed in the rat cell line INS-1. This can have several explanations; first, the amino acid sequences of GPR44 have 79 % similarity between human and rat (according to BLAST) which means that the ligand could target a sequence that is dissimilar; second, the INS-1 cells are derived from insulinoma that implicates that many genes might have altered expression levels. Similarly, low binding of DTBZ was observed in the rodent-derived INS-1 cell line. These “false negatives” in DTBZ and AZD3825 binding (in relation to human islets) underline the importance of utilizing humanized animal models or human beta cell lines such as EndoC-βH1 in the preclinical evaluation of imaging agents in diabetic research.
A further requirement for a reliable and accurate biomarker of beta cell mass is low variability in expression between individual beta cells within an individual, as well as between beta cells in different individuals. The receptor densities shown in Table 3 are all acquired from islet preparations from different individuals. This indicates quite low variation of GPR44 between individuals both in their endocrine and exocrine pancreatic tissues. However, since these are tissue homogenates, it does not yield information on the variability between individual beta cells. This must be further explored by, for example, quantitative autoradiography using a positron emitting GPR44 ligand.
The major issue in visualizing biological processes or receptors by molecular imaging is that of contrast. In the case of beta cell imaging, the contrast requirements are immense due to the volumetric difference between the beta cells and the non-endocrine pancreatic parenchyma. Here we show that GPR44 is highly preferential for the endocrine pancreas and the beta cell in particular. The contrast between human beta cells and human exocrine preparations was 45.2 (Bmax ratio) or 59.1 [Binding Potential (BP) ratio]. This is in contrast to VMAT2 or other molecular entities targeted by DTBZ that were found in both endocrine and exocrine pancreatic preparations.
Our ability to visualize and quantify a receptor by in vivo molecular imaging is interplay between ligand affinity and receptor density. We have here demonstrated excellent in vitro affinity to GPR44 by the tritiated ligand AZD 3825, as well as improved contrast for the endocrine pancreas compared to DTBZ. GPR44 was expressed in relatively low densities compared to VMAT2 in the endocrine pancreas, which potentially limits the possibilities of generating a strong enough signal. However, the binding potential, or the receptor density divided by the dissociation constant, was similar to that of DTBZ (approximately 30 % lower). Given that the entire DTBZ binding in pancreas in vivo is displaceable and therefore receptor specific [33] and readily quantifiable in primates and humans, we foresee no insurmountable problems in quantifying the GPR44 in the endocrine pancreas as soon as a PET ligand is available.
A final criterion, which applies to PET tracers in general, is that the agent should be pharmacologically neutral, i.e., the tracer molecule itself should not induce a physiological response even at high doses. This is preferred but not an absolute requirement, as pharmacologically active agonists have been successfully employed in clinical imaging research such as [11C]Carfentanil [34] or radiolabeled Exendin4 [9]. Therefore, the pharmacological effect of GPR44 agonism or antagonism must be further explored before selecting a GPR44 binder for PET labeling with the aim of clinical translation.
Conclusion
The GPR44 protein has been confirmed as beta cell restricted by proteomics, transcriptomics as well as by a radiolabeled small molecule ligand. Given the development of a suitable PET ligand, this target potentially offers improved contrast between endocrine and exocrine pancreas compared to currently available biomarkers.
References
Akirav EM, Lebastchi J, Galvan EM et al (2011) Detection of β cell death in diabetes using differentially methylated circulating DNA. Proc Natl Acad Sci USA 108:19018–19023
Kanak MA, Takita M, Shahbazov R et al (2015) Evaluation of MicroRNA375 as a novel biomarker for graft damage in clinical islet transplantation. Transplantation 99:1568–1573
Locke JM, Lango Allen H, Harries LW (2014) A rare SNP in pre-miR-34a is associated with increased levels of miR-34a in pancreatic beta cells. Acta Diabetol 51:325–329
Souza F, Simpson N, Raffo A et al (2006) Longitudinal noninvasive PET-based beta cell mass estimates in a spontaneous diabetes rat model. J Clin Investig 116:1506–1513
Gotthardt M, Lalyko G, van Eerd-Vismale J et al (2006) A new technique for in vivo imaging of specific GLP-1 binding sites: first results in small rodents. Regul Pept 137:162–167
Eriksson O, Selvaraju RK, Johansson L et al (2014) Quantitative imaging of serotonergic biosynthesis and degradation in the endocrine pancreas. J Nucl Med 55:460–465
Goland R, Freeby M, Parsey R et al (2009) 11C-dihydrotetrabenazine PET of the pancreas in subjects with long-standing type 1 diabetes and in healthy controls. J Nucl Med 50:382–389
Normandin MD, Petersen KF, Ding YS et al (2012) In vivo imaging of endogenous pancreatic beta-cell mass in healthy and type 1 diabetic subjects using 18F-fluoropropyl-dihydrotetrabenazine and PET. J Nucl Med 53:908–916
Brom M, Woliner-van der Weg W, Joosten L et al (2014) Non-invasive quantification of the beta cell mass by SPECT with 111In-labelled exendin. Diabetologia 57:950–959
Eriksson O, Espes D, Selvaraju RK et al (2014) Positron emission tomography ligand [11C]5-hydroxy-tryptophan can be used as a surrogate marker for the human endocrine pancreas. Diabetes 63:3428–3437
Karlsson F, Antonodimitrakis P, Eriksson O (2015) Systematic screening for islet biomarkers: retrospective evaluation of clinically available neuroendocrine positron emission tomography tracers. Nucl Med Biol 42:762–769
Moran BM, Abdel-Wahab YH, Vasu S, Flatt PR, McKillop AM (2015) GPR39 receptors and actions of trace metals on pancreatic beta cell function and glucose homoeostasis. Acta Diabetol. doi:10.1007/s00592-015-0781-5
Lindskog C, Korsgren O, Pontén F, Eriksson JW, Johansson L, Danielsson A (2012) Novel pancreatic beta cell-specific proteins: antibody-based proteomics for identification of new biomarker candidates. J Proteom 75:2611–2620
Ravassard P, Hazhouz Y, Pechberty S et al (2011) A genetically engineered human pancreatic beta cell line exhibiting glucose-inducible insulin secretion. J Clin Investig 121:3589–3597
Royer JF, Schratl P, Carrillo JJ et al (2008) A novel antagonist of prostaglandin D2 blocks the locomotion of eosinophils and basophils. Eur J Clin Investig 38:663–671
Goto M, Eich TM, Felldin M et al (2004) Refinement of the automated method for human islet isolation and presentation of a closed system for in vitro islet culture. Transplantation 78:1367–1375
Friberg AS, Stahle M, Brandhorst H, Korsgren O, Brandhorst D (2008) Human islet separation utilizing a closed automated purification system. Cell Transplant 17:1305–1313
Fagerberg L, Hallström BM, Oksvold P et al (2014) Analysis of the human tissue-specific expression by genome-wide integration of transcriptomics and antibody-based proteomics. Mol Cell Proteom 13:397–406
Sickle (2012) A windowed adaptive trimming tool for FASTQ files using quality. https://github.com/najoshi/sickle. Accessed November 2013
Trapnell C, Pachter L, Salzberg SL (2009) TopHat: discovering splice junctions with RNA-Seq. Bioinformatics 25:1105–1111
Picard (2012) http://picard.sourceforge.net/. Accessed November 2013
Trapnell C, Williams BA, Pertea G et al (2010) Transcript assembly and quantification by RNA-Seq reveals unannotated transcripts and isoform switching during cell differentiation. Nat Biotechnol 28:511–515
Flicek P, Amode MR, Barrell D et al (2012) Ensembl 2012. Nucleic Acids Res 40:D84–D90
Anders S, Huber W (2010) Differential expression analysis for sequence count data. Genome Biol 11:R106
R CoreTeam (2013) R: a language and environment for statistical computing. R foundation for statistical computing. http://www.R-project.org/. Accessed November 2013
Gregory RW (2012) Gplots: various R programming tools for plotting data. R package version 2.11.0. http://CRAN.R-project.org/package=gplots. Accessed November 2013
Tsao HH, Skovronsky DM, Lin KJ, Yen TC, Wey SP, Kung MP (2011) Sigma receptor binding of tetrabenazine series tracers targeting VMAT2 in rat pancreas. Nucl Med Biol 38:1029–1034
Jahan M, Eriksson O, Johnström P et al (2011) Decreased defluorination using the novel beta-cell imaging agent [18F]FE-DTBZ-d4 in pigs examined by PET. EJNMMI Res 1:33
Eriksson O, Jahan M, Johnström P et al (2010) In vivo and in vitro characterization of [18F]-FE-(+)-DTBZ as a tracer for beta-cell mass. Nucl Med Biol 37:357–363
Fagerholm V, Mikkola KK, Ishizu T et al (2010) Assessment of islet specificity of dihydrotetrabenazine radiotracer binding in rat pancreas and human pancreas. J Nucl Med 51:1439–1446
Tsao HH, Skovronsky DM, Lin KJ (2011) Sigma receptor binding of tetrabenazine series tracers targeting VMAT2 in rat pancreas. Nucl Med Biol 38:1029–1034
The Human Protein Atlas (2015) http://www.proteinatlas.org/ENSG00000183134-PTGDR2/tissue/cerebral+cortex. Accessed August 2015
Harris PE, Farwell MD, Ichise M (2013) PET quantification of pancreatic VMAT 2 binding using (+) and (−) enantiomers of [(1)(8)F]FP-DTBZ in baboons. Nucl Med Biol 40:60–64
Zubieta JK, Gorelick DA, Stauffer R et al (1996) Increased mu opioid receptor binding detected by PET in cocaine-dependent men is associated with cocaine craving. Nat Med 2:1225–1229
Acknowledgments
The study was supported by grants from JDRF, Diabetesfonden, Barndiabetesfonden, and Tore Nilssons Foundation for Medical Research. O.E.s position was supported by ExoDiab (Excellence of Diabetes Research in Sweden) and O.K.s position was supported by the National Institutes of Health (2U01AI065192-06).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Paul Czernichow is an employee of EndoCells. The remaining authors report no conflicts of interest.
Ethical standard
All work involving human tissue was conducted according to the principles expressed in the Declaration of Helsinki and in the European Council’s Convention on Human Rights and Biomedicine. Consent for organ donation (for clinical transplantation and for use in research) was obtained from the relatives of the deceased donors by the donor’s physicians and documented in the medical records of the deceased subject. The study was approved by the Regional Ethics Committee in Uppsala, Sweden (http://www.epn.se) according to the Act concerning the Ethical Review of Research Involving Humans (2003:460), Permit Number: Dnr 2009/371 (from April 10, 2013).
Human and animal rights disclosure
This article does not contain any studies with human or animal subjects performed by any of the authors.
Informed consent
None.
Additional information
Managed by Antonio Secchi.
Electronic supplementary material
Below is the link to the electronic supplementary material.
592_2015_811_MOESM1_ESM.pdf
Supplementary Fig. 1. Representative saturation binding experiments to assess affinity (Kd) and receptor density (Bmax) of [3H]AZD 3825 (A-C) and [3H]DTBZ (D-E). Homogenized human pancreatic endocrine (A, D) or exocrine (B, E) preparations was used. [3H]AZD 3825 binding to pure human beta cells was assessed by EndoC-βH1 cell homogenates (C). Supplementary material 1 (PDF 55 kb)
Rights and permissions
About this article
Cite this article
Hellström-Lindahl, E., Danielsson, A., Ponten, F. et al. GPR44 is a pancreatic protein restricted to the human beta cell. Acta Diabetol 53, 413–421 (2016). https://doi.org/10.1007/s00592-015-0811-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0811-3