Abstract
Aims
To compare high-sensitivity C-reactive protein (hs-CRP) and white blood cell count (WBC) as a predictor of incident diabetes in a population where obesity is not prevalent.
Methods
This is a retrospective 6-year follow-up study in a Japanese health screening population including 1874 men and 1094 women. Using Cox regression methods, hazard ratios (HRs) of incident diabetes for hs-CRP and WBC adjusting for fasting plasma glucose (FPG), hemoglobin A1c (HbA1c) and other confounders were calculated, and using areas under receiver operating characteristic curve (AUCs), diabetes-predicting abilities of hs-CRP and WBC were compared. Diabetes was defined as FPG ≥ 126 mg/dL and HbA1c ≥ 6.5 % or use of antidiabetic medication.
Results
During the 6-year follow-up period (mean ± SD, 4.8 ± 1.7 years), 71 men (3.8 %) and 19 women (1.7 %) developed incident diabetes. The fully adjusted HRs [95 % confidence intervals (CIs)] of incident diabetes for each 1 SD increase in log hs-CRP and WBC were 1.20 (0.92–1.56) (p = 0.174) and 1.01 (0.78–1.30) (p = 0.946), respectively. The fully adjusted HRs (95 % CIs) of incident diabetes for the highest tertile of hs-CRP and WBC compared with the lowest tertile were 2.57 (1.05–6.27) (p = 0.039) and 1.20 (0.53–2.70) (p = 0.665), respectively. The AUCs (95 % CIs) of hs-CRP and WBC for the discrimination of incident diabetes were 0.73 (0.68–0.77) and 0.67 (0.62–0.72), respectively.
Conclusions
Hs-CRP, but not WBC, was independently associated with incident diabetes in a Japanese health screening population where obesity is not prevalent.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Growing evidence shows that obesity-related inflammation [1–3] may play a crucial role in the pathogenesis of metabolic syndrome (MetS) [4, 5] and type 2 diabetes [6]. Accumulating data suggest that inflammatory biomarkers including high-sensitivity C-reactive protein (hs-CRP) are associated with the incidence of type 2 diabetes [7–19]. An acute-phase plasma protein, hs-CRP, is synthesized by the liver in response to interleukin-6 (IL-6) and other proinflammatory cytokines secreted by macrophages, T cells and adipocytes [6]. The stability of this protein during long-term frozen blood storage and the availability of inexpensive, precise and standardized assays have assisted studies of hs-CRP [20]. While hs-CRP is known as an independent risk factor for cardiovascular disease (CVD) [20, 21], white blood cell count (WBC) is also a routinely measured marker of systemic inflammation and reported to be a predictor of CVD mortality [22, 23] and incident MetS [24, 25]. Previously, the authors of a cross-sectional study reported that hs-CRP was superior to WBC as an inflammatory component of MetS [26]. However, a longitudinal study conducted in a healthy Japanese population, where obesity was not prevalent, showed that these two inflammatory markers equally predicted incident MetS [27]. Recently, WBC was also reported to be a predictor of incident diabetes [28]. However, there have been no studies which compared the ability to predict incident diabetes between hs-CRP and WBC, both of which are routinely measured markers of systemic inflammation in clinical as well as epidemiological studies. Inflammation was shown to be linked to incident diabetes in a Japanese population where obesity was not prevalent [16]. Previously, the author reported that very low levels of hs-CRP were significantly related to other metabolic risk factors in a Japanese health screening population [29]. The aim of the present study was to compare hs-CRP and WBC as a predictor of incident diabetes in a Japanese health screening population where obesity defined as body mass index (BMI) of ≥30 kg/m2 was not prevalent (1.9 %) and the mean (SD) BMI was 22.6 (0.3) kg/m2.
Methods
Subjects
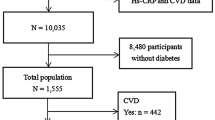
Between April 2008 and March 2009, 2435 men and 1437 women visited our Medical Check-up Center for general health screenings and gave written informed consent to use their data for epidemiological studies. The visitors were required to fill out a questionnaire prepared by the Japanese Ministry of Health, Labor, and Welfare for the purpose of the Specific Health Examination and Instruction, including questions about histories of coronary heart disease and stroke, smoking, alcohol consumption, physical activity, antihypertensive, antidiabetic and antihyperlipidemic medications. Among them, 139 men and 33 women presented diabetes at baseline. By excluding these individuals, 2296 men and 1414 women remained as candidate subjects for the follow-up study. Among them, 1874 men and 1094 women revisited our Medical Check-up Center between April 2009 and March 2015 and were included in this study. The first diagnosis with incident diabetes in the annual health screenings was ascertained as the outcome, and subjects without the outcome were censored at their last visits. Diabetes was defined as fasting plasma glucose (FPG) ≥ 126 mg/dL and hemoglobin A1c (HbA1c) ≥ 6.5 % or use of antidiabetic drugs. The protocol for this study was approved by the ethics committee of Tachikawa Medical Center, and the study procedures were in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Measurements
After an overnight fast, blood samples were obtained to measure blood levels of routine medical checkup tests including FPG, HbA1c, triglycerides, total cholesterol, high-density lipoprotein (HDL) cholesterol, low-density lipoprotein (LDL) cholesterol, hs-CRP, uric acid, aspartate aminotransferase (AST), alanine aminotransferase (ALT), creatinine and WBC. The chemical measurements were all taken at BML Nagaoka (Nagaoka, Japan) with routine laboratory methods except for hs-CRP which was measured at BML General Laboratory (Tokyo, Japan) with nephelometry using N-latex CRP-2 (Siemens Healthcare Japan, Tokyo, Japan). The measurement limit of hs-CRP was 0.02 mg/L, and the value of hs-CRP less than the measurement limit was considered to be 0.01 mg/L. HbA1c was measured with latex aggregation immunoassay using Determiner HbA1c (Kyowa Medex, Tokyo, Japan). LDL cholesterol was measured using a direct surfactant method with Choletest-LDL (Sekisui Medical Inc, Tokyo, Japan). The directly measured LDL cholesterol was used in the present study because subjects with triglycerides of ≥400 mg/dL were excluded from those with the calculated LDL cholesterol using Friedewald’s equation, and the directly measured LDL cholesterol and the calculated one were very strongly correlated (r = 0.966). The estimated glomerular filtration rate (eGFR) was calculated using the following equation according to the recommendation from the Japanese Society of Nephrology: eGFR (mL min−1/1.73 m2) = 194 × creatinine−1.094 × age−0.287 in men and 194 × creatinine−1.094 × age−0.287 × 0.739 in women [30]. Blood pressure was automatically measured with MPV-3301 (NIHON KODEN Inc., Tokyo, Japan). An average systolic blood pressure (SBP) and diastolic blood pressure (DBP) were calculated from two measurements in sitting position after a 5-min rest period. Body weight was measured with the light clothes provided by our center, and the weight of the clothing was subtracted from the measured body weight. Body mass index (BMI) was calculated as the weight in kilograms divided by the square of height in meters.
Statistical analysis
The baseline data of potential candidates and actually followed subjects were compared. Then, the baseline data of subjects who developed diabetes and those who did not were compared. Means were compared by two-tailed t tests, and percentages were compared by Chi-squared tests. Hs-CRP and triglycerides were compared after log transformation because their distributions were highly skewed.
The incidence of developing diabetes was calculated for each tertile of hs-CRP and WBC, and linear trends of the incidence of diabetes along the tertiles of hs-CRP and WBC were examined by logistic regressions.
Using Cox regressions in which years were used as a unit of the survival variable, the first diagnosis with incident diabetes in the annual health screenings was ascertained as the outcome, and subjects without the outcome were censored at their last visits; the hazard ratios and their 95 % confidence intervals [HRs (95 %CIs)] of incident diabetes for each 1 SD increase in log hs-CRP and WBC as well as for the higher tertiles of hs-CRP and WBC compared with the lowest tertile were calculated adjusting for sex, age, current smoking, daily alcohol drinking, physical activity, use of antihypertensive and antihyperlipidemic medications and history of coronary heart disease and stroke (model 1), further adjusting for the above covariates plus BMI, FPG and HbA1c (model 2), and further adjusting for the covariates in model 2 plus SBP, log triglycerides, HDL cholesterol, LDL cholesterol, AST, ALT, uric acid and eGFR (model 3). DBP was excluded from the covariates to avoid multicollinearity because SBP and DBP were strongly correlated (r = 0.93).
The areas under receiver operating characteristic curve (AUCs) and the optimal cutoff points with their sensitivities and specificities of hs-CRP and WBC for the discrimination of incident diabetes were calculated. An optimal cutoff point was defined as a point at which the sum of its sensitivity and specificity is maximal.
Statistical analyses were performed using the Dr SPSS-2 software (IBM Japan, Tokyo, Japan). P values lower than 0.05 were considered to be statistically significant.
Results
The comparison of baseline data between the potential candidates and the actually followed subjects is shown in Table 1. There was no significant difference in the baseline data between the candidates and the actually followed subjects. The comparison of baseline data between diabetes developers and non-developers is shown in Table 2. The age, BMI, SBP, DBP, FPG, HbA1c, hs-CRP, WBC, triglycerides, LDL cholesterol and uric acid were significantly higher, while HDL cholesterol and eGFR were significantly lower in the diabetes developers than in non-developers. Male sex, antihypertensive drug use, antihyperlipidemic drug use and current smoking were significantly more frequent in the diabetes developers than in non-developers.
Among the 1874 men aged 24–82 (mean ± SD, 51.6 ± 9.4) years and 1094 women aged 30–82 (mean ± SD, 51.8 ± 9.5) years, diabetes developed in 71 men (3.8 %) and 19 women (1.7 %) during the 6-year follow-up period (mean ± SD, 4.8 ± 1.7 years). The incidence of diabetes stratified by the tertiles of hs-CRP and WBC is presented in Table 3. There were significant increasing trends of the incidence of diabetes along the tertiles of hs-CRP and WBC.
The HRs (95 % CI) of incident diabetes for each 1 SD increases in log hs-CRP and log WBC as well as for the higher tertiles of hs-CRP and WBC compared with the lowest tertile are shown in Table 4. Only the highest tertile of hs-CRP was significantly associated with incident diabetes in model 2 [HR (95 % CI), 2.76 (1.19–6.41)] and model 3 [HR (95 % CI), 2.57 (1.05–6.27)] although each 1 SD increase in hs-CRP as well as WBC and the higher tertiles of hs-CRP as well as WBC was all significantly associated with incident diabetes in model 1.
The AUCs and the optimal cutoff points with their sensitivities and specificities of hs-CRP and WBC for the discrimination of incident diabetes are shown in Table 5. The diabetes-discriminating AUCs (95 % CIs) of hs-CRP and WBC were 0.73 (0.68–0.77) and 0.67 (0.62–0.72), respectively.
Discussion
The present study found that hs-CRP, but not WBC, was independently associated with incident diabetes and that the AUCs (95 % CIs) of hs-CRP and WBC for the discrimination of incident diabetes were 0.73 (0.68–0.77) and 0.67 (0.62–0.72), respectively, in a Japanese health screening population where obesity was not prevalent.
There is increasing evidence that obesity-related adipose tissue inflammation [1–3] is closely involved in the pathogenesis of type 2 diabetes [6]. Wang et al. reviewed prospective studies on the associations of elevated levels of IL-6 and hs-CRP with increased risk of diabetes [19]. Their meta-analysis, including 10 prospective studies with a total of 19,709 participants and 4480 cases, detected a significant dose–response association of IL-6 levels with diabetes risk [relative risk (RR) (95 % CI), 1.31 (1.17–1.46)] [19]. For hs-CRP, a meta-analysis involving 22 cohorts with a total of 40,735 participants and 5753 cases showed that elevated hs-CRP levels were significantly associated with increased risk of diabetes [RR (95 % CI), 1.26 (1.16–1.37)] [19]. An association between WBC and diabetes risk has been recently suggested by Twig et al. They assessed whether WBC was an independent risk factor for incident diabetes in 24,897 young men (mean ± SD age, 30.8 ± 5.36 years) during a mean follow-up period of 7.5 years and concluded that WBC was an independent risk factor for diabetes [28]. The HRs (95 % CI) of incident diabetes for the highest quintile (WBC 7801–12,000/L−6) was 1.52 (1.06–2.18) (p = 0.02) adjusted for age, BMI, family history, smoking status, FPG and triglycerides [28]. In contrast, Ford reported in an approximately 20-year follow-up study including 8352 participants that the HRs (95 % CI) of incident diabetes for WBC of ≥9100/L−6 compared with WBC of ≤5700/L−6 were 1.33 (0.81–2.19) in men and 1.68 (1.21–2.34) in women after adjusting for age, smoking status, SBP, cholesterol, use of antihypertensive medication, physical activity, alcohol use and BMI [31]. He did not include FPG in the adjusting covariates and suggested that inflammatory markers might be limited as predictors of diabetes [31].
The present study compared hs-CRP and WBC as a predictor of incident diabetes in a population where obesity was not prevalent (1.9 %) and found that hs-CRP was independently associated with diabetes, but WBC was not. Inflammation was reported to be associated with incident diabetes in a Japanese population where obesity was not prevalent [16]. Previously, the author reported that very low levels of hs-CRP were significantly related to other metabolic risk factors in a Japanese health screening population [29]. The means (SDs) of FPG for the first (lowest), second, third, fourth and fifth quintile of hs-CRP were 5.14 (0.66), 5.26 (0.72), 5.21 (0.61), 5.37 (0.74) and 5.42 (0.90) mmol/L, respectively, in men, while 4.82 (0.45), 4.93 (0.48), 4.92 (0.54), 4.96 (0.48) and 5.12 (0.88) mmol/L, respectively, in women [29]. In the present study, the correlation coefficients between end point FPG and baseline hs-CRP and WBC were 0.133 (p < 0.001) and 0.134 (p < 0.001), respectively, in subjects with baseline BMI of <25 kg/m2 who did not use antidiabetic drugs at end point (n = 2368). Animal studies indicated that the infiltration of activated macrophages into adipose tissue and accompanied inflammation, but not increased adipose tissue mass, adipocyte size, or visceral adipose tissue mass per se, was crucial for the metabolic consequences of obesity including insulin resistance and glucose status [32–35]. Therefore, it is reasonable to think that inflammation may be associated with glucose status even in non-obese humans. Beyond traditional risk factors, measurement of inflammatory markers contributed relatively little additional value in clinical diabetes risk prediction in a multiethnic cohort of postmenopausal women [36]. Although recent studies have linked plasma markers of inflammation to incident diabetes [6–23, 28], the utility of these inflammatory biomarkers for risk prediction of diabetes remains uncertain.
Limitations
The subjects of the present study were not from a general population but from a relatively health-conscious population, and the follow-up period was relatively short. Therefore, the cumulative number of cases was only 71 for men and 19 for women so that gender-stratified analysis could not find statistically significant associations between hs-CRP or WBC and incident diabetes (Online Supplementary Tables s1 and s2). However, both hs-CRP and WBC were associated with incident diabetes in men (Online Supplementary Tables s1). Information about family history, diet and demographic background was not available so that residual confounders might influence the study results.
Conclusions
The present study found that hs-CRP, but not WBC, was independently associated with incident diabetes and that the AUC of hs-CRP for the discrimination of incident diabetes was higher than that of WBC in a Japanese health screening population where obesity was not prevalent. Thus, inflammation was suggested to be associated with incident diabetes even in a non-obese population and that hs-CRP may be superior to WBC as a marker of inflammation.
References
Hotamisligil GS, Shargill NS, Spiegelman BM (1993) Adipose expression of tumor necrosis factor-α: direct role in obesity-linked insulin resistance. Science 259:87–91
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AW Jr (2003) Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest 112:1796–1808
Cinti S, Mitchell G, Barbatelli G et al (2005) Adipocyte death defines macrophage localization and function in adipose tissue of obese mice and humans. J Lipid Res 46:2347–2355
Alberti KG, Eckel RH, Grundy SM et al (2009) Harmonizing the metabolic syndrome. A joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society; and International Association for the Study of Obesity. Circulation 120:1640–1645
Oda E (2012) Metabolic syndrome: its history, mechanisms, and limitations. Acta Diabetol 49:89–95
Donath MY, Shoelson SE (2011) Type 2 diabetes as an inflammatory disease. Nat Rev Immunol 11:98–107
Pradhan AD, Manson JE, Rifai N, Buring JE, Ridker PM (2001) C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA 286:327–334
Barzilay JI, Abraham L, Heckbert SR et al (2001) The relation of markers of inflammation to the development of glucose disorders in the elderly: the Cardiovascular Health Study. Diabetes 50:2384–2389
Freeman DJ, Norrie J, Caslake MJ et al (2002) West of Scotland Coronary Prevention Study. C-reactive protein is an independent predictor of risk for the development of diabetes in the West of Scotland Coronary Prevention Study. Diabetes 51:1596–1600
Han TS, Sattar N, Williams K, Gonzalez-Villalpando C, Lean MEJ, Haffner SM (2002) Prospective study of C-reactive protein in relation to the development of diabetes and metabolic syndrome in the Mexico City Diabetes Study. Diabetes Care 25:2016–2021
Spranger J, Kroke A, Möhlig M et al (2003) Inflammatory cytokines and the risk to develop type 2 diabetes: results of the prospective population-based European Prospective Investigation into Cancer and Nutrition (EPIC)-Potsdam Study. Diabetes 52:812–817
Thorand B, Löwel H, Schneider A et al (2003) C-reactive protein as a predictor for incident diabetes mellitus among middle-aged men: results from the MONICA Augsburg cohort study, 1984–1998. Arch Intern Med 163:93–99
Nakanishi S, Yamane K, Kamei N, Okubo M, Kohno N (2003) Elevated C-reactive protein is a risk factor for the development of type 2 diabetes in Japanese Americans. Diabetes Care 26:2754–2757
Hu FB, Meigs JB, Li TY, Rifai N, Manson JE (2004) Inflammatory markers and risk of developing type 2 diabetes in women. Diabetes 53:693–700
Laaksonen DE, Niskanen L, Nyyssönen K et al (2004) C-reactive protein and the development of the metabolic syndrome and diabetes in middle-aged men. Diabetologia 47:1403–1410
Doi Y, Kiyohara Y, Kubo M et al (2005) Elevated C-reactive protein is a predictor of the development of diabetes in a general Japanese population: the Hisayama Study. Diabetes Care 28:2497–2500
Wannamethee SG, Lowe GDO, Rumley A, Cherry L, Whincup PH, Sattar N (2007) Adipokines and risk of type 2 diabetes in older men. Diabetes Care 30:1200–1205
Wang Z, Hoy WE (2007) C-reactive protein and the risk of developing type 2 diabetes in Aboriginal Australians. Diabetes Res Clin Pract 76:37–43
Wang X, Bao W, Liu J et al (2013) Inflammatory markers and risk of type 2 diabetes: A systematic review and meta-analysis. Diabetes Care 36:166–175
Pearson TA, Mensah GA, Alexander RW et al (2003) Markers of inflammation and cardiovascular disease: application to clinical and public health practice: a statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation 107:499–511
Hansson GK (2005) Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med 352:1685–1695
Margolis KL, Manson JE, Greenland P et al (2005) Women’s Health Initiative Research Group: Leukocyte count as a predictor of cardiovascular events and mortality in postmenopausal women: the Women’s Health Initiative Observational Study. Arch Intern Med 165:500–508
Tamakoshi K, Toyoshima H, Yatsuya H et al (2007) White blood cell count and risk of all-cause and cardiovascular mortality in nationwide sample of Japanese. Results from NIPPON DATA90. Circ J 71:479–485
Fadini GP, Marcuzzo G, Marescotti MC, de Kreutzenberg SV, Avogaro A (2012) Elevated white blood cell count is associated with prevalence and development of the metabolic syndrome and its components in the general population. Acta Diabetol 49:445–451
Jung CH, Lee WY, Kim SY et al (2008) The risk of metabolic syndrome according to the high-sensitivity C-reactive protein in apparently healthy Koreans. Int J Cardiol 129:266–271
Oda E, Kawai R (2010) Comparison between high-sensitivity C-reactive protein (hs-CRP) and white blood cell count (WBC) as an inflammatory component of metabolic syndrome in Japanese. Intern Med 49:117–124
Oda E (2013) High-sensitivity C-reactive protein and white blood cell count equally predict development of the metabolic syndrome in a Japanese health screening population. Acta Diabetol 50:633–638
Twig G, Afek A, Shamiss A et al (2013) White blood cells count and incidence of type 2 diabetes in young men. Diabetes Care 36:276–282
Oda E, Kawai R (2009) Very low levels of high-sensitivity C-reactive protein are not bimodally distributed but are significantly related to other metabolic risk factors in Japanese. Intern Med 48:953–958
Matsuo S, Imai E, Horio M et al (2009) Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis 53:982–992
Ford ES (2002) Leukocyte count, erythrocyte sedimentation rate, and diabetes incidence in a national sample of US adults. Am J Epidemiol 155:57–64
Kim JY, Wall E, Laplante M et al (2007) Obesity-associated improvements in metabolic profile through expansion of adipose tissue. J Clin Invest 117:2621–2637
Bains RK, Wells SE, Flavell DM et al (2004) Visceral obesity without insulin resistance in late-onset obesity rats. Endocrinology 145:2666–2679
Cinti S, Mitchell G, Barbatelli G et al (2005) Adipocyte death defines macrophage localization and function in adipose tissue of obese mice and humans. J Lipid Res 46:2347–2355
Kanda H, Tateya S, Tamori Y et al (2006) MCP-1 contributes to macrophage infiltration into adipose tissue, insulin resistance, and hepatic steatosis in obesity. J Clin Invest 116:1494–1505
Chao C, Song Y, Cook N et al (2010) The lack of utility of circulating biomarkers of inflammation and endothelial dysfunction for type 2 diabetes risk prediction among postmenopausal women: the Women’s Health Initiative Observational Study. Arch Intern Med 170:1557–1565
Acknowledgments
The author thanks all subjects who participated in the study, the paramedical staff at our center who assisted with the study and Honorary Prof. Yoshifusa Aizawa at Tachikawa Medical Center for his valuable comments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The sole author, Oda E, received no financial support.
Conflict of interest
The sole author, Oda E, declared that he has no conflict of interest.
Ethical standard
This study was carried out in accordance with the principles of the Declaration of Helsinki of 1975, as revised in 2008.
Human and Animal Rights
All procedures performed in the study were in accordance with the ethical standards of the institutional committee and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Oda, E. High-sensitivity C-reactive protein, but not white blood cell count, independently predicted incident diabetes in a Japanese health screening population. Acta Diabetol 52, 983–990 (2015). https://doi.org/10.1007/s00592-015-0788-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0788-y