Abstract
Purpose
Peroneus longus tendon (PLT) autograft has been successfully used for isolated anterior cruciate ligament (ACL) or posterior cruciate ligament (PCL) reconstruction cases. Being a powerful evertor and flexor of great toe, there might be associated ankle morbidity with this autograft option. However, there are only a few studies exploring whether the ankle morbidity is significant or not. This study aims to assess the functional outcomes, donor site morbidity, and ankle strength after harvesting ipsilateral peroneus longus autograft for ACL reconstruction in revision ACL and multi-ligament injury cases.
Methods
This was a prospective case series. All of the patients were evaluated by clinical examination for knee for laxity, ankle joint stability, and using visual analog scale (VAS) for pain, International Knee Documentation Committee (IKDC) score, and Lysholm score, preoperatively and postoperatively at two-year follow-up. Morbidity of donor ankle was assessed using American Orthopedic Foot and Ankle Society (AOFAS) score, bilateral evertors, and first ray plantarflexion strength measurement using an isometer (Innovative Design Orthopedics) at two-year follow-up.
Results
Ipsilateral PLT graft was used in ten patients of revision ACL reconstruction and 27 patients of the multi-ligament knee injury. The mean length of PLT harvested (cm) was 26.2 (standard deviation 2.6, range 22–31), and mean diameter of the doubled graft (mm) was 7.9 (standard deviation 0.68, range 7.5–8.5). There was a significant improvement in VAS score for pain, Lysholm, and IKDC scores (p = < 0.001) at two -year follow-up. There were no cases of graft failure, superficial, or deep infection. Ankle dorsiflexion(p = 0.32), ankle plantarflexion (p = 0.19), eversion strength(p = 0.6), first ray plantarflexion strength(p = 0.52), and AOFAS score(p = 0.29) were found to be comparable to the normal side in all patients.
Conclusions
Peroneus longus autograft can be considered as a potential autograft option for ACL reconstruction in multi-ligament knee injuries and revision ACL reconstruction. No significant donor site morbidity was noted at follow-up.
Level of evidence
Level IV.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Several options for tendon grafts exist in anterior cruciate ligament (ACL) reconstruction surgeries. The most popular autografts used are quadrupled hamstring graft and bone-patellar tendon-bone (BPTB) graft [1, 2]. The choice of an appropriate autologous graft becomes difficult in cases of revision ACL surgeries or multi-ligament reconstructions, where more than one tendon may be needed. Allografts can be used in such situations but they are not easily available, and carry a small but definite risk of transmission of blood-borne infections and a higher rate of graft rupture [3]. Thus, other options for a suitable tendon autograft are being studied.
None of the commonly used autografts can be considered as the ideal graft for anterior cruciate ligament (ACL) reconstruction. The hamstring tendon graft is one of the most commonly used graft in an anterior cruciate ligament (ACL) reconstruction. It would be worthwhile to mention here that hamstrings are strong agonists of ACL function in preventing anterior translation of the tibia [4]. Despite showing excellent mechanical strength, it has been said to have disadvantages of knee flexion weakness [5,6,7,8], poor predictability of length and diameter [4, 9], and injury to infrapatellar branches of the saphenous nerve [10, 11]. The second most commonly used graft, BPTB, carries a risk of anterior knee pain and patellar fracture [12, 13]. Contralateral hamstring tendons have been used in revision ligament reconstructions and multi-ligament injuries [14]. But it subjects the normal limb to an additional surgical procedure, delays rehabilitation, and thus, may not easily be acceptable to patients [5, 6].
Recently, peroneus longus tendon (PLT) harvested from the ankle has been used in knee ligament surgeries [15,16,17,18,19,20,21,22]. The use of peroneus longus tendon as a graft is not new and has been used previously for other indications [23]. The half-thickness of the tendon has been used variably in knee ligament surgery before [18, 24, 25]. PLT is gaining popularity as a graft option in primary ACL reconstruction surgeries with studies showing tensile strength [26] and clinical outcomes [19] comparable to quadrupled hamstring grafts. Peroneus longus is a powerful evertor of the foot and flexor of the great toe. Loss of this function is an important concern in the use of this graft, but this donor site morbidity has not been adequately evaluated in most of the studies [15,16,17,18,19, 22]. To the best of our knowledge, there are no studies to date showing clinical outcomes of using PLT autograft in multi-ligament injuries or revision anterior cruciate ligament surgeries.
This study aims to assess the functional outcomes, donor site morbidity, and ankle strength after harvesting ipsilateral peroneus longus autograft for anterior cruciate ligament (ACL) reconstruction in revision ACL and multi-ligament injury cases.
Methodology
In this prospective observational study conducted over a time period of 1 year (December 2017 to November 2018), all patients aged between 16 and 50 years undergoing ACL reconstruction surgery as a part of multi-ligament reconstruction or revision surgery using PLT autografts were included. The diagnosis of ligament injury was made based on history, clinical examination, and magnetic resonance imaging (MRI). Any patient with history of injury or any surgery or disability affecting strength of ipsilateral ankle were excluded from the study. Patients with associated fractures around knee were also excluded. Informed consent was obtained from all patients. The ethical clearance was obtained from institutional ethical committee (AIIMS/IEC/18/189).
All of the patients were evaluated clinically by Lachman test, anterior drawer test, and pivot shift tests for anterior laxity, and functional evaluation was done using visual analog scale (VAS) for pain (0–10 cm scale), International knee documentation committee (IKDC) score, and Lysholm score, preoperatively at presentation to the hospital. The activity level of all of the patients was also noted. The preoperative workup also included assessment of the cause of failure in revision ACL reconstruction cases by computed tomography scans and MRI.
Surgical technique
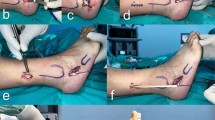
For harvesting the PLT, a 3-cm-skin incision was given 1 cm behind the lateral malleolus. Any branches of the cutaneous nerve in this area were carefully protected. Peroneal tendons were identified after incising the superficial fascia and the superior peroneal retinaculum. The PLT was differentiated from peroneus brevis tendon by thicker size, superficial location, and absence of any muscle fibers attached to it. The PLT was marked and divided behind the lateral malleolus. The distal part of the tendon was stitched to the peroneus brevis tendon in end-to-side fashion. Whipstitch was made at the proximal free end of PLT with Ethibond #2 suture, and a closed tendon stripper was used to harvest the tendon keeping the tendon stripper at least 5 cm away from fibular head (Fig. 1). Dimensions of the tendon graft were noted, and the tendon was prepared on a graft preparation board. The graft was doubled in all of the cases, and ends secured with a whipstitch.
In multiple ligament injuries, ipsilateral PLT was used for reconstructing ACL, ipsilateral semitendinosus tendon grafts were preferred for any other ligament reconstruction if needed (ACL + PCL or Medial collateral ligament or posterolateral corner). If three ligaments were reconstructed (ACL + PCL + Medial collateral ligament or posterolateral corner) contralateral semitendinosus graft was also harvested. PLT graft was used to reconstruct ACL in all revision ACL reconstruction cases.
All cases were performed by the single arthroscopic surgeon under spinal anesthesia and pneumatic tourniquet. Standard vertical anterolateral portal and horizontal antero-medial portal, were used for instrumentation and femoral tunnel preparation. The femoral socket was drilled from antero-medial portal at the position of native ACL footprint. The graft was fixed on the femoral side using a cortical suspensory device (Stryker Procinch adjustable loop) and on the tibial side with a bio-absorbable tibial interference screw (Stryker).
For revision ACL reconstruction cases, the tunnels were aimed to be anatomically placed avoiding any tunnel convergence. All of the revision ACL reconstruction procedures were single staged.
Rehabilitation protocol
Isometric quadriceps exercises and closed-chain knee flexion exercises were started from the first postoperative day. Patients with cruciate reconstructions and revision ACL reconstruction were kept on the partial weight-bearing protocol for three weeks, followed by full weight-bearing. Patients with collateral reconstructions were kept on a non-weight-bearing mobilization plan for six weeks. The hinged knee brace was used for six weeks in cases of multi-ligament injury patients. Open-chain quadriceps exercises were started at 6–8 weeks. Hamstring exercises were started after the surgery unless ipsilateral hamstring tendon was harvested. A compression bandage was used for the ankle for two weeks. Ankle range of motion was started soon after pain relief, and no specific rehabilitation changes were made for PLT harvest. Proprioceptive training, quadriceps strengthening was started at eight weeks.
Outcome evaluation
All the patients were followed up at regular intervals upto a minimum of two years and any assessed any complications. None of the patients were lost to follow-up. The postoperative function assessment included clinical examination to assess laxity and noting the similar functional scores (VAS scale, IKDC and Lysholm scores) at two-year follow-up period. Morbidity of donor ankle was assessed using the American Orthopedic Foot and Ankle Society (AOFAS) score, measurement of ankle range of motion and bilateral evertor and first ray plantarflexion strength using an isometer (Innovative Design Orthopedics, Redditch, UK) at two -year follow-up visit. Ankle range of motion was measured with patient lying supine on couch with hip and knee extended, while keeping the goniometer’s pivot centered over lateral malleolus, with one arm parallel to the axis of tibia and fibula and another arm along the axis of 5th metatarsal. Evertor strength (in Kgs) was measured with the patient lying in lateral decubitus position with the leg touching the bed and hip and knee flexed at 30 degrees, keeping the tape of isometer at the base of 5th metatarsal, and first ray plantarflexion strength (in Kgs) was measured in the prone position with knee flexed at 90 degrees and the measurement tape at the level of the base of the great toe (Fig. 2). The evertor and plantarflexion strength measurements were noted by two independent, blinded observers with a gap of 7 days between observations.
Statistical analysis
Statistical analysis was done using SPSS 24.0. Data were assessed for normal distribution by Kolmogorov–Smirnov test. Continuous variables are expressed as mean ± standard deviation. A paired T-test or wilcoxon signed rank test was used to calculate the improvement between preoperative and postoperative functional outcome scores as per distribution of the data. A paired T-test or wilcoxon signed rank test was used to compare between AOFAS score, evertor power, and first ray plantarflexion power of affected and unaffected sides as per distribution of the data. Intra-observer and inter-observer reliability were tested by repeat measurements of all the parameters. They were expressed as intraclass correlation coefficients (ICC) with its 95% confidence interval (CI).
Results
Ipsilateral PLT graft was used for ACL reconstruction in 10 patients of revision ACL reconstruction and 27 patients of multi-ligament knee injury (17 patients of ACL, PCL, and MCL injury and 10 patients with ACL and PCL injury). Among the revision ACL cases, four patients had graft intrasubstance or femoral attachment tear with minimal to no tunnel widening, five patients had femoral tunnel malposition, and four patients had tibial tunnel malposition with widening (range 10–12 mm). Tunnel malposition was managed by placement of tunnels in anatomical position avoiding any tunnel convergence with suspensory fixation at femoral and aperture fixation at tibial side. Age, sex, side, mechanism, and duration since the injury have been summarized in Table 1. The data were found to be normally distributed.
The mean length of PLT harvested was 26.2 cm (Standard Deviation 2.6, range 22–31), and the mean diameter of the doubled graft (mm) was 7.9 ± 0.68 (Standard Deviation 0.68, range 7.5–8.5). None of the patients had any anterior laxity at two years follow-up. There was a significant improvement in pain scores (VAS), Lysholm, and IKDC scores (p < 0.001) at two -year follow-up (Table 2). Ankle range of motion, eversion strength, first ray plantarflexion strength, and AOFAS score were found to be comparable to the normal side in all patients (Table 3). None of the patients complained of hypoaesthesia around the graft harvest site on clinical examination. Ankle range of motion was comparable on both sides.
None of the patients had any surgical site infections. However, two patients aged 41 and 54 years, with ACL, PCL and MCL injury had progression of osteoarthritis and underwent total knee replacement after 2 and 1.5 years after surgery consecutively. Although tunnel widening was noted in one revision ACL reconstruction patient at 2 year’s follow-up, none of the patients had any clinically significant laxity in the knee joint. However, none of the postoperative radiographs at follow-up visits reveal any subluxation of tibia or abnormal opening up of the knee joint. Six patients developed knee stiffness in the early postoperative period (4 patients with ACL, PCL and MCL injury, 2 patients with ACL and PCL injury). Three among them gained full range of motion after regular physiotherapy and rest three patients needed manipulation under anesthesia. Overall, the postoperative knee range of motion was comparable to the normal side (Table 2). The intra-observer reliability was noted to be 0.951 (95% CI:0.891−0.978), 0.963 (95% CI:0.918–0.983) for eversion strength measurements, and 0.915 (95% CI:0.817–0.962), 0.929 (95% CI:0.846–0.968) for plantarflexion strength measurements for observer 1 and observer 2, respectively. Whereas the inter-observer reliability was 0.911 (95% CI:0.808–0.960) and 0.938 (95% CI:0.864–0.972) for eversion strength and plantarflexion strength, respectively.
Discussion
The most important findings of the present study were that PLT autograft had sufficient length and diameter while using in ACL reconstruction. There was significant improvement in postoperative knee functional outcome without any clinical laxity. PLT harvesting didn’t affect the ankle range of motion and evertor or first ray plantarflexion strength at two years follow-up.
The choice of the graft is one of the most crucial steps in ligament reconstruction surgeries. Peroneus longus tendon has been used for other orthopedic surgeries for a long time [23, 25]. Biomechanical studies have shown peroneus longus to have a tensile strength similar to quadrupled hamstring autograft [24, 26] and significantly better tensile strength than quadriceps tendon or patellar tendon [27]. PLT graft has also been shown to have sufficient length and diameter for ligament reconstruction surgeries [28], which is larger than the dimensions of semitendinosus graft. Mean length of 26.2 ± 2.6 cm and doubled diameter of 7.9 ± 0.68 mm were observed in this study, which is comparable to previous studies [19, 29].
Thus, PLT may be a very useful tendon graft for ligament reconstruction. However, its use is not very popular. One of the main reasons behind its underutilization in knee ligament reconstruction is apprehension about the ankle stability and function and altered foot mechanics after harvesting this graft. We found no functional deficits in any of the 37 patients included in this study. Ankle range of motion and stability were unaffected. Functional outcome scores for the ankle joint were unaffected after harvest of this graft. This concern of ankle morbidity after the PLT harvest is not substantiated by this study.
Multi-ligament injuries and revision ACL reconstruction present a dilemma of a suitable graft choice. The allograft is not available readily, and it has its risks of infection and early failure compared to autografts [30]. This study shows that PLT graft can be a very useful autograft in these situations. Peroneus longus acts as an evertor and plantar flexor of the first ray with the role of maintaining the longitudinal arch of the foot [31]. However, harvesting peroneus longus has shown not to affect the gait pattern or ankle stability [28]. This can probably be explained by the compensatory activity of other muscles of the foot like the peroneus brevis, which is a more powerful evertor than peroneus longus [32]. A study by Angthong et al. [21] revealed peak torque of inversion and eversion to be significantly lower after harvesting PLT graft. However, the study evaluated only ten patients for isokinetic testing at seven months follow-up. The evertor strength (p = 0.13) and first ray plantarflexion strength (p = 0.26) was found to be comparable to the normal side in our study, which is similar to a study conducted by Rhatomy et al. [20]. Mean AOFAS score was 98.9 ± 1.6 in the affected side and 99.3 ± 0.7 on the normal side in our study. Similar findings were seen by Rhatomy et al. [20] (98.71 ± 3.03) and Shi et al. [15] (96.0 ± 9.6). None of the patients complained of ankle pain or stiffness in the follow-up period.
PLT graft has been used in isolated ACL [15, 16, 18,19,20,21,22] or PCL [17] reconstruction before with excellent outcomes. However, use of PLT may be more justified in Multi-ligament injury or revision ACL cases where there is a dilemma about the choice of autograft. Most of these studies lack evaluation of ankle morbidity by both subjective and objective measurements [15,16,17,18,19, 22]. Incorporating assessment of the ankle strength after tendon harvest is an important strength of this study. A follow-up of two years is sufficient to comment on the functional outcomes of the knee as well as the donor site. Yet a longer follow-up of graft function and survival is desirable preferably with a control group with different grafts. Another limitation of this study is that patients with multiple ligament injuries receiving different ligament reconstructions with different autografts were included. Thus, the assessment of the functional outcomes of patients may be influenced by the heterogeneity of the study population.
Conclusion
Peroneus longus graft can be considered as a potential autograft option for ACL reconstruction in multi-ligament knee injuries and revision ACL reconstruction with favorable functional outcomes. The range of motion and muscle strengths were comparable to contralateral ankle.
References
West RV, Harner CD (2005) Graft selection in anterior cruciate ligament reconstruction. J Am Acad Orthop Surg 13(3):197–207. https://doi.org/10.5435/00124635-200505000-00006
Romanini E, D’Angelo F, De Masi S et al (2010) Graft selection in arthroscopic anterior cruciate ligament reconstruction. J Orthop Traumatol 11:211–219
Lobo Gajiwala A (2003) Tissue banking in India: gamma-irradiated allografts. Cell Tissue Bank 4:203–211. https://doi.org/10.1023/B:CATB.0000007022.91458.00
Goyal T, Paul S, Das L, Choudhury AK (2020) Correlation between anthropometric measurements and activity level on length and diameter of semitendinosus tendon autograft in knee ligament surgery: a prospective observational study. SICOT-J. https://doi.org/10.1051/sicotj/2020007
Armour T, Forwell L, Litchfield R et al (2004) Isokinetic evaluation of internal/external tibial rotation strength after the use of hamstring tendons for anterior cruciate ligament reconstruction. Am J Sports Med 32:1639–1643. https://doi.org/10.1177/0363546504263405
Ohkoshi Y, Inoue C, Yamane S et al (1998) Changes in muscle strength properties caused by harvesting of autogenous semitendinosus tendon for reconstruction of contralateral anterior cruciate ligament. Arthroscopy 14:580–584. https://doi.org/10.1016/s0749-8063(98)70053-2
Tashiro T, Kurosawa H, Kawakami A et al (2003) Influence of medial hamstring tendon harvest on knee flexor strength after anterior cruciate ligament reconstruction: a detailed evaluation with comparison of single- and double-tendon harvest. Am J Sports Med 31:522–529. https://doi.org/10.1177/31.4.522
Goradia VK, Grana WA, Pearson SE (2006) Factors associated with decreased muscle strength after anterior cruciate ligament reconstruction with hamstring tendon grafts. Arthrosc - J Arthrosc Relat Surg 22:80.e1-80.e15. https://doi.org/10.1016/j.arthro.2005.10.012
Charlton WP, Randolph DA Jr, Lemos S, Shields CL Jr (2003) Clinical outcome of anterior cruciate ligament reconstruction with quadrupled hamstring tendon graft and bioabsorbable interference screw fixation. Am J Sports Med 31(4):518–521. https://doi.org/10.1177/03635465030310040701
Sanders B, Rolf R, McClelland W, Xerogeanes J (2007) Prevalence of saphenous nerve injury after autogenous hamstring harvest: an anatomic and clinical study of sartorial branch Injury. Arthrosc - J Arthrosc Relat Surg 23:956–963. https://doi.org/10.1016/j.arthro.2007.03.099
Ruffilli A, De Fine M, Traina F et al (2017) Saphenous nerve injury during hamstring tendons harvest: does the incision matter? A systematic review. Knee Surg Sport Traumatol Arthrosc 25:3140–3145
Sherman OH, Banffy MB (2004) Anterior cruciate ligament reconstruction: Which graft is best? Arthrosc J Arthrosc Relat Surg 20:974–980. https://doi.org/10.1016/j.arthro.2004.08.001
Hardy A, Casabianca L, Andrieu K et al (2017) Complications following harvesting of patellar tendon or hamstring tendon grafts for anterior cruciate ligament reconstruction: systematic review of literature. Orthop Traumatol Surg Res 103:S245–S248
Goyal T, Paul S, Banerjee S, Das L (2021) Outcomes of one-stage reconstruction for chronic multiligament injuries of knee. Knee Surg Relat Res. https://doi.org/10.1186/s43019-020-00083-y
Shi F-D, Hess DE, Zuo J-Z et al (2019) Peroneus longus tendon autograft is a safe and effective alternative for anterior cruciate ligament reconstruction. J Knee Surg 32:804–811. https://doi.org/10.1055/s-0038-1669951
Ertoğrul R, Sezer HB, Armağan R et al (2017) Comparison of clinical outcomes after anterior cruciate ligament reconstruction with autogenous hamstring tendons and peroneus longus allograft. Orthop J Sport Med. https://doi.org/10.1177/2325967117S00042
Setyawan R, Soekarno NR, Asikin AIZ, Rhatomy S (2019) Posterior cruciate ligament reconstruction with peroneus longus tendon graft: 2-years follow-up. Ann Med Surg 43:38–43. https://doi.org/10.1016/j.amsu.2019.05.009
Bi M, Zhao C, Zhang S et al (2018) All-inside single-bundle reconstruction of the anterior cruciate ligament with the anterior half of the peroneus longus tendon compared to the semitendinosus tendon: a two-year follow-up study. J Knee Surg 31:1022–1030. https://doi.org/10.1055/s-0038-1627466
Rhatomy S, Asikin AIZ, Wardani AE et al (2019) Peroneus longus autograft can be recommended as a superior graft to hamstring tendon in single-bundle ACL reconstruction. Knee Surg, Sport Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05455-w
Rhatomy S, Wicaksono FH, Soekarno NR et al (2019) Eversion and first ray plantarflexion muscle strength in anterior cruciate ligament reconstruction using a peroneus longus tendon graft. Orthop J Sport Med 7:232596711987246. https://doi.org/10.1177/2325967119872462
Angthong C, Chernchujit B, Apivatgaroon A et al (2015) The anterior cruciate ligament reconstruction with the peroneus longus tendon: a biomechanical and clinical evaluation of the donor ankle morbidity. J Med Assoc Thai 98:555–560
Kerimoǧlu S, Aynaci O, Saracoǧlu M et al (2008) Anterior cruciate ligament reconstruction with the peroneus longus tendon. Acta Orthop Traumatol Turc 42:38–43. https://doi.org/10.3944/AOTT.2008.42.1.038
Ellis SJ, Williams BR, Wagshul AD et al (2010) Deltoid ligament reconstruction with peroneus longus autograft in flatfoot deformity. Foot Ankle Int 31:781–789. https://doi.org/10.3113/FAI.2010.0781
Zhao J, Huangfu X (2012) The biomechanical and clinical application of using the anterior half of the peroneus longus tendon as an autograft source. Am J Sports Med 40:662–671. https://doi.org/10.1177/0363546511428782
Xu C, Zhao J, Xie G (2016) Medial patella-femoral ligament reconstruction using the anterior half of the peroneus longus tendon as a combined procedure for recurrent patellar instability. Asia-Pacific J Sport Med Arthrosc Rehabil Technol 4:21–26. https://doi.org/10.1016/j.asmart.2016.03.001
Rudy ME, Phatama KY (2017) Tensile strength comparison between peroneus longus and hamstring tendons: a biomechanical study. Int J Surg Open 9:41–44. https://doi.org/10.1016/j.ijso.2017.10.002
Phatama KY, Hidayat M, Mustamsir E et al (2019) Tensile strength comparison between hamstring tendon, patellar tendon, quadriceps tendon and peroneus longus tendon: a cadaver research. J Arthrosc Jt Surg 6:114–116. https://doi.org/10.1016/j.jajs.2019.02.003
Barzegar M, Hosseini A, Karimi M, Nazem K (2014) Can we use peroneus longus in addition to hamstring tendons for anterior cruciate ligament reconstruction? Adv Biomed Res 3:115. https://doi.org/10.4103/2277-9175.132696
Sasetyo DR, Rhatomy S, Pontoh LA (2017) Peroneus longus tendon: the promising graft for anterior cruciate ligament reconstruction surgery. Asia-Pacific J Sport Med Arthrosc Rehabil Technol 9:25. https://doi.org/10.1016/j.asmart.2017.05.033
Legnani C, Zini S, Borgo E, Ventura A (2016) Can graft choice affect return to sport following revision anterior cruciate ligament reconstruction surgery? Arch Orthop Trauma Surg 136:527–531. https://doi.org/10.1007/s00402-015-2387-3
Riegger CL (1988) Anatomy of the ankle and foot. Phys Ther 68:1802–1814. https://doi.org/10.1093/ptj/68.12.1802
Otis JC, Deland JT, Lee S, Gordon J (2004) Peroneus brevis is a more effective evertor than peroneus longus. Foot Ankle Int 25:242–246. https://doi.org/10.1177/107110070402500408
Funding
There was no funding source.
Author information
Authors and Affiliations
Contributions
TG: Planning of study, patient enrollment, writing of manuscript. SP: Evaluation of functional outcomes, patient enrollment, writing of manuscript, manuscript preparation. AKC: Patient enrollment, Data collection SSS: Patient enrollment, Data collection.
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Consent for publication
The author(s) give consent for publication of this article.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Ethical approval
The institutional ethics committee approved the study (AIIMS/IEC/18/189).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Goyal, T., Paul, S., Choudhury, A.K. et al. Full-thickness peroneus longus tendon autograft for anterior cruciate reconstruction in multi-ligament injury and revision cases: outcomes and donor site morbidity. Eur J Orthop Surg Traumatol 33, 21–27 (2023). https://doi.org/10.1007/s00590-021-03145-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-03145-3