Abstract
Purpose
A detailed morphometry of the Hill–Sachs lesion and quantification of its volume was studied in 71 patients with traumatic anterior shoulder instability with radiographs and computerized arthrotomography.
Methods
The accuracy of the conventional radiographs and Bernageau view to visualize the humeral and the glenoid lesion was also assessed. This study also analysed the depth of the Hill–Sachs lesion (D) and the humeral head radius (R) from conventional radiograph and its location from the computerized arthrotomography. All the findings were analysed and correlated with the outcome of the arthroscopic stabilization procedure.
Results
Sensitivity for demonstrating the Hill–Sachs lesion for the 45° internal rotation anteroposterior radiograph was 84%, whereas sensitivity for demonstrating the glenoid lesion for the comparative Bernageau view was 68%. The mean D/R ratio, the lateralization angle and the volume of the Hill–Sachs lesion were 16.2%, 188° and 1,019 mm³, respectively. The mean Hill–Sachs lesion volume represented 2.28% of the total humeral head volume. The D/R ratio, the lateralization angle and the volume of the Hill–Sachs lesion were significantly high in the recurrent dislocation group, whereas the D/R ratio and the lesion volume were also significantly high in the group that did not perform well following the stabilization procedure. The recurrence rate in this study was 16.6%, majority being from the recurrent dislocation group.
Conclusion
This study confirms the interest as risk factor for a simple and reproducible radiographic quantitative measure of the Hill–Sachs lesion: D/R.
Level of evidence
II.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Traumatic anterior shoulder instability is routinely seen in younger patients and its immediate post-reduction complication is relatively low; however, it is known to re-dislocate in 30–90% of young patients [1–3]. In spite of the isolation of the risk factors and the selection of the patients for nonoperative treatment [4], it persists an important rate of after primary anterior shoulder dislocation.
Malgaigne was the first surgeon to describe the humeral bony lesion in shoulder dislocation in 1855 [5]. However, H.A. Hill and M.D. Sachs [6] in 1940 gave a detailed description of this posterolateral humeral bony.
Various radiographic studies [7–9] described different projections to visualize the Hill–Sachs lesion with an accuracy of 90–100%. In the last one, Ito [10] used a new X-ray to achieve an undistorted radiographic view of the notch. Recently, MRI (Magnetic Resonance Imagery) and CT (Computer Tomography) arthrography has also been used increasingly as a precise and reproducible diagnostic tool for a detailed three-dimensional evaluation of the soft tissue and bony lesion following anterior shoulder instability [11]. Roger [12] demonstrated the superiority of CT arthrography for the detection of Hill–Sachs lesion compared to the X-rays. However, these modalities are routinely implemented in combination with the pre-operative planning of the shoulder stabilization procedure.
It has long been recognized that both open and arthroscopic shoulder stabilization procedures leads to good functional outcome. The reported arthroscopic failure rate with different repair technique varies from 49 to 7% [13, 14] and is much higher as compared to the open surgical procedures [15].
In the aim to reduce this high recurrence rate, some studies [16–22] isolated numerous predisposing factors. All these data of the literature are summarized in Table 1.
For many authors [4, 16, 17, 19, 23–26], the Hill–Sachs lesion is an important risk factor and its ignorance or its negligence into pre-operative planning could be a reason for arthroscopic procedures failure.
It persists a semantics problem to considerate this humeral bone defect. H.A. Hill and M.D. Sachs [6] classified as small, medium and large on the basis of its diameter. Burkhart [23] described the Hill–Sachs lesion into engaging and nonengaging lesion. For Rowe [26] and Boileau [17], a higher post-surgical failure rate associated with ‘large’ Hill–Sachs lesion, and for Balg [16], one of the criteria to calculate the instability severity index score is an Hill–Sachs lesion ‘visible on external rotation’ on anteroposterior X-ray view. All these definition are subjective and rough.
Kaar [27], in a cadaveric study, found with increasing size of Hill–Sachs defects glenohumeral stability decreasing.
These conclusions raised the problem of quantification and location of Hill–Sachs lesion. In spite of some dedicated articles [4, 24, 25], there is no standard reference.
Hence, the purpose of this study was to assess the influence of the Hill–Sachs lesion on the long-term success of the arthroscopically stabilized unstable shoulder. We hypothesized that the importance of the Hill–Sachs lesion has a predictive value for the result of arthroscopic stabilization procedure and could be used as a selection criteria along with glenoid lesion to choose between arthroscopic and open technique. We, finally, looked for a simple and reproducible radiographic measure to quantify the Hill–Sachs lesion and a value threshold by making a precise risk factor for failure after an arthroscopic stabilization procedure.
Materials and methods
Seventy-one consecutive patients (49 men and 22 women), with traumatic anterior shoulder instability who had arthroscopic stabilization procedure at our institution, were included in this study. The mean age of the patient at the time of arthroscopic procedure was 29 years, and the dominant shoulder was involved in 27% of the cases. The mean follow-up was 68 months (32–100 months).
Forty-two patients (59%) were involved in sports, with twenty-two (31%) participated in high risk sports with or without cocked position of the arm, thirteen (18%) involved in overhead sports and the remaining seven (10%) participated at competitive level.
The patients were assigned to three groups on the basis of their symptoms and physical examination finding: Recurrent dislocation group, patients with 2 or more episodes of dislocation requiring close reduction (41 patients); recurrent subluxation group, patients with recurrent subluxation with spontaneous reduction (21 patients) and painful unstable shoulder group, patients with history of pain and instability following trauma but without dislocation or subluxation (9 patients).
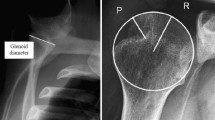
All the patients were subjected to standard anteroposterior radiographs in neutral rotation, 45° external rotation and 45° internal rotation as well as a comparative Bernageau view pre-operatively. Next transparent circular gauges in 1-mm increment were fitted on the humeral head on the 45° internal rotation anteroposterior radiograph, and a best fit circle was used to measure the radius (R) of the humeral head and the depth (D) of the lesion (D) (Fig. 1). Because of the variation in the magnification and to reflect the true size of the notch on the X-ray, a ratio between the depth of the lesion and the radius of the humeral head (D/R) was determined.
A double-contrast computerized arthrotomography of the affected shoulder joint was also carried out for accurate evaluation of the Hill–Sachs lesion. The computed tomography scan was made with a 3-mm slice thickness after injection of 1 mL (millilitre) of contrast medium and 19 mL of room air into the glenohumeral joint.
The CT scans were evaluated by an independent observer to measure the following parameters on the humeral head (Fig. 2).
-
1.
Humeral head diameter (HD): represents the maximum anteroposterior distance, determined by a best fit circle along the circumference of the humeral head which also gives us the centre of the circle.
-
2.
Width of the lesion (W): represents the distance between the medial and lateral edge of the lesion, determined by two trajectories projected from the centre of the humeral head along the edges of the lesion.
-
3.
Depth of the lesion (De): represents the distance between the apex and bottom of the lesion along the best fit circle.
-
4.
Length of the Hill–Sachs lesion (L): represents the distance between the initial and the last CT slice where the lesion is visualized.
-
5.
Lateralization angle: measured for precise location of the lesion and determined by a best fit circle on the humeral head and by an intersection of an anteroposterior axis through the centre of the humeral head and another extending from the centre of the circle to the centre of the lesion (Fig. 3). This method of measurement was described by Richards et al. [28] on shoulder MRI.
Assuming the Hill–Sachs lesion as an irregular geometrical body and for the purpose of calculation, we applied the formula of an ellipsoid for calculating the Hill–Sachs lesion volume.
The arthroscopic stabilization procedure was carried out as a day case in a lateral decubitus position under general anaesthesia and interscalene block. Most of the patients had transglenoïd fixation, and 23% of patients also had a capsular shift with Bankart repair. Post-operative recovery was uneventful. The patients were managed with the arm in a sling in internal rotation for 4 weeks. Passive pendulum exercises were started on the day after surgery. Shoulder rehabilitation with a physiotherapist was commenced after a month. External rotation was limited to 45º until 45 days. Re-creational and over-head sports were allowed after 3 and 4 months, respectively.
The post-operative functional results were evaluated by an independent observer with the Duplay group clinical score.
Statistical analysis
To evaluate the reliability of X-ray measurements, 10 orthopaedic surgeons independently measured the depth of the lesion and the radius of the humeral head in 10 patients on the anteroposterior X-ray in 45° internal rotation. Inter-Observer reliability of the measurement was tested by calculation of the intra-class correlation coefficient (ICC).
We used the student’s t test, Tukey’s post-test, ANOVA (ANalysis Of Variance), Chi-square test and Mann–Whitney test. The level of significance was set at P < 0.05. Data were analysed with Statview 5.0 (SAS institute, Cary, North Carolina).
Results
Fifty-nine patients were available for final follow-up review. The mean follow-up was 68 months (32–100 months). The functional results were classified as excellent (24 patients), good (14 patients), fair (7 patients) and poor (14 patients). For statistical purpose, the first two and the last two functional groups were combined. Nine patients from the poor group had previous open Bankart procedure, 7 for recurrence of dislocation and 2 for recurrence of subluxation. There was no significant difference in patient demographics between the combined excellent and good group (38/59) and the fair and poor group (21/59).
The Hill–Sachs lesion was seen as a notch in fifty patients (84%) on the anteroposterior radiograph with the arm in 45° internal rotation (Fig. 1), whereas on Bernageau view, glenoïd pathology was seen in forty patients (68%). Glenoïd surface abrasion was seen in 29 patients (49.15%), nine patients (15.25%) had an antero-inferior glenoïd fracture with a detached bone fragment and two patients (3.38%) had amputation (defect) of the anterior glenoïd surface. The following Table 2 shows different glenoïd pathology in the two functional groups. This glenoïd lesions had no statistically significant influence on the overall surgical result except in three patients (5%) with recurrence of instability, a significant antero-inferior glenoïd lesion (two amputations and one fracture) was present but on the humeral side a small Hill–Sachs lesion with a volume was less than 500 mm³ was present.
The mean D/R ratio was 16.2% (3–34%). Tukey’s post-test showed a significantly high D/R ratio in recurrent dislocation versus the subluxation group (Table 3). This ratio was also statistically significant in the two functional groups (Table 4). The inter-observer correlation coefficient values for the depth of the lesion and the radius of the humeral head were 0.67 and 1.31 mm, respectively, which was statistically insignificant.
The mean Hill–Sachs lesion volume was 1019 mm³ (0–4,792 mm³). This lesion volume represented 2.28% of the head volume (range 0–10.5%). The lesion volume variation in the 3 patient groups was statistically significant (ANOVA P = 0.001) (Table 3). This volume was also significantly high in the fair and poor functional group (Table 4). The mean lesion/head volume ratio (VR) in the two functional groups was 1.5% (0–8.4%) and 4.9% (0.6–10.5%), respectively.
The lateralization angle measured to precisely locate the lesion ranged from 165° to 218° with a mean of 188° in the excellent and good group and 193° in the fair and poor group that was statistically insignificant. However, this angle was significantly different in the three symptomatic groups with much higher angle in the recurrent dislocation group.
The instability recurred in ten patients (16.9%) following arthroscopic stabilization procedure, which were later revised with open coracoid transplantation. Majority of the recurrences were from the recurrent dislocation group with significantly high D/R and volume of the Hill–Sachs lesion.
Discussion
This study found that arthroscopic stabilization procedure in patients with high volume of the Hill–Sachs lesion led to a post-operative recurrence of instability in 16.9% of patients with a mean follow-up of 68 months. This result is comparable to those found in the other similar studies [18]. Few authors reported lower failure rate but they had a less important average follow-up [16, 17, 21, 22], and or the radiographic lesions (glenoïd and Hill–Sachs) were criteria of exclusion [22]. The long mean follow-up of our series was essential because it was recently clearly proved [19] the importance of this risk factor in the analysis of the results of this surgery.
The most important finding from this study was a simple measure on conventional X-rays and reproducible in the daily clinical practice: D/R. When the D/R ratio threshold was more than 15%, the failure rate was 56% contrary to only 16% failure when the D/R ratio was less than 15%. Patients who had a high D/R ratio as seen in the recurrent dislocation group had significantly higher rate of recurrence of instability.
At the same time, the Hill–Sachs volume was significantly high in patients with history of recurrent dislocation leading to 37% recurrence in this group. When the lesion volume was compared in the two post-operative functional groups, we found it to be significantly high in the group which performed poorly. When the lesion volume threshold was considered to be 1,000 mm³, the surgical failure rate below this threshold was 7.7% and dropped to 2.5% on exclusion of the cases with glenoïd fractures and amputations.
Even if recently Kaar [27] proved glenohumeral joint stability decreases with increasingly larger humeral head defects and Cetik [24] correlated the number of dislocations and the extent and depth of the Hill–Sachs lesions; nobody of them gave morphometric details of the Hill–Sachs lesion.
Ito [25] first, on X-ray described by himself [10], and Kralinger [4], on anteroposterior with 60° of internal rotation, tried to quantify the humeral bon defect. In their analysis, they did not take into account the radiographic magnification, which always exists and did not show any relationship between the Hill–Sachs lesion and the incidence of recurrence after arthroscopic stabilization procedure.
As Saito [29], we thought that not only the size but also the location of the Hill–Sachs lesion determined the risk factor for recurrence. This angle was significantly much higher in the recurrent dislocation group but no statistically significant difference could be found between combined excellent/good group and combined fair/poor group. It can be explained by the fact that only one computerized arthrotomography slice showing the deepest position of the notch was taken into account while measuring this angle, possibly giving a false position of the notch. However, if we had measured this angle on all the slices showing the lesion would have given the obliqueness of the notch and may have given a different lateralization angle.
Several authors [11, 12] found 3D (Dimension) CT reconstruction of the glenohumeral joint useful to visualize the Hill–Sachs lesion and calculate its volume, whereas Hammar [30] used ultrasound scan for measuring the volume. Saito [29] thinks the CT scan may overestimate the Hill–Sachs lesion because it is sometimes difficult to distinguish from the bare area.
Various methods like capsuloplasty, mosaïcplasty and proximal humeral osteotomy have been advocated to reduce the incidence of surgical failure secondary to Hill–Sachs lesion. However, capsuloplasty is not an acceptable procedure in a young population with high functional demand as it leads to limitation in the range of glenohumeral external rotation. Mosaïcplasty has limited indication and is reserved for large defects. Proximal humeral rotation osteotomy described by Weber leads to subscapularis and capsular shortening and is also associated with complications like pseudarthrosis, implant failure and axillary nerve injury.
Hence, stabilization procedures like Bankart repair open or arthroscopic are the preferred methods to deal with anterior shoulder instability. Although the incidence of failure is high with arthroscopic stabilization procedure, it is still developing and hopefully in future the recurrence of instability will be much lower.
Conclusion
The results from this study suggest that pre-operative radiological assessment of the Hill–Sachs lesion can predict success of arthroscopic surgical repair. Arthroscopic stabilization procedure should be reserved for Hill–Sachs lesion with a D/P less than 16% but any associated glenoïd lesions should also be quantified.
High volume Hill–Sachs lesion and glenoïd bony defects clearly compromise the success of arthroscopic stabilization procedure, and hence, the management of anterior shoulder instability must include proper patient selection.
References
Arciero RA, Wheeler JH, Ryan JB, McBride JT (1994) Arthroscopic bankart repair versus nonoperative treatment for acute, initial anterior shoulder dislocations. Am J Sports Med 22(5):589–594
Brooks JH, Fuller CW, Kemp SP, Reddin DB (2005) Epidemiology of injuries in english professional rugby union: part 1 match injuries. Br J Sports Med 39(10):757–766. doi:10.1136/bjsm.2005.018135
Hovelius L, Olofsson A, Sandstrom B, Augustini BG, Krantz L, Fredin H, Tillander B, Skoglund U, Salomonsson B, Nowak J, Sennerby U (2008) Nonoperative treatment of primary anterior shoulder dislocation in patients forty years of age and younger. A prospective twenty-five-year follow-up. J Bone Joint Surg Am 90 (5):945–952. doi:10.2106/JBJS.G.00070
Kralinger FS, Golser K, Wischatta R, Wambacher M, Sperner G (2002) Predicting recurrence after primary anterior shoulder dislocation. Am J Sports Med 30(1):116–120
Malgaigne (1855) Traité des fractures et des luxations. Paris
Hill HA, Sachs MD (1940) The grooved defect of the humeral head: a frequently unrecognized complication of dislocations of the shoulder joint. Radiology 35:690–700
Danzig LA, Greenway G, Resnick D (1980) The hill-sachs lesion. An experimental study. Am J Sports Med 8(5):328–332
Didiée J (1930) Le radiodiagnostic dans la luxation récidivante de l’épaule. J Radiol Electrol 14:209–218
Garth WP, Jr., Slappey CE, Ochs CW (1984) Roentgenographic demonstration of instability of the shoulder: the apical oblique projection. A technical note. J Bone Joint Surg Am 66(9):1450–1453
Ito H, Shirai Y, Takayama A, Shibasaki T (1996) A new radiographic projection for the posterolateral notch in cases of recurrent dislocation of the shoulder. Nippon Ika Daigaku Zasshi 63(6):499–501
Workman TL, Burkhard TK, Resnick D, Goff WB II, Balsara ZN, Davis DJ, Lapoint JM (1992) Hill-sachs lesion: Comparison of detection with mr imaging, radiography, and arthroscopy. Radiology 185(3):847–852
Roger B, Skaf A, Hooper AW, Lektrakul N, Yeh L, Resnick D (1998) Imaging findings in the dominant shoulder of throwing athletes: comparison of radiography, arthrography, ct arthrography, and mr arthrography with arthroscopic correlation. AJR Am J Roentgenol 172(5):1371–1380
Torchia ME, Caspari RB, Asselmeier MA, Beach WR, Gayari M (1997) Arthroscopic transglenoid multiple suture repair: 2 to 8 year results in 150 shoulders. Arthroscopy 13(5):609–619
Walch G, Boileau P, Levigne C, Mandrino A, Neyret P, Donell S (2005) Arthroscopic stabilization for recurrent anterior shoulder dislocation: results of 59 cases. Arthroscopy 11(2):173–179
Hobby J, Griffin D, Dunbar M, Boileau P (2007) Is arthroscopic surgery for stabilisation of chronic shoulder instability as effective as open surgery? A systematic review and meta-analysis of 62 studies including 3044 arthroscopic operations. J Bone Joint Surg Br 89(9):1188–1196. doi:10.1302/0301-620X.89B9.18467
Balg F, Boileau P (2007) The instability severity index score. A simple pre-operative score to select patients for arthroscopic or open shoulder stabilisation. J Bone Joint Surg Br 89(11):1470–1477. doi:10.1302/0301-620X.89B11.18962
Boileau P, Villalba M, Hery JY, Balg F, Ahrens P, Neyton L (2006) Risk factors for recurrence of shoulder instability after arthroscopic bankart repair. J Bone Joint Surg Am 88(8):1755–1763. doi:10.2106/JBJS.E.00817
Calvo E, Granizo JJ, Fernandez-Yruegas D (2005) Criteria for arthroscopic treatment of anterior instability of the shoulder: a prospective study. J Bone Joint Surg Br 87(5):677–683. doi:10.1302/0301-620X.87B5.15794
Flinkkila T, Hyvonen P, Ohtonen P, Leppilahti J (2010) Arthroscopic bankart repair: results and risk factors of recurrence of instability. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-010-1105-5
Hayashida K, Yoneda M, Nakagawa S, Okamura K, Fukushima S (1998) Arthroscopic bankart suture repair for traumatic anterior shoulder instability: analysis of the causes of a recurrence. Arthroscopy 14(3):295–301
Lafosse L, Iserin A, Kempf JF, Hardy P (2000) Arthroscopic treatment of chronic anterior shoulder instability. Rev Chir Orthop Reparatrice Appar Mot 86(Suppl 1):106–109
Porcellini G, Campi F, Pegreffi F, Castagna A, Paladini P (2009) Predisposing factors for recurrent shoulder dislocation after arthroscopic treatment. J Bone Joint Surg Am 91(11):2537–2542. doi:10.2106/JBJS.H.01126
Burkhart SS, De Beer JF (2000) Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic bankart repairs: significance of the inverted-pear glenoid and the humeral engaging hill-sachs lesion. Arthroscopy 16(7):677–694
Cetik O, Uslu M, Ozsar BK (2007) The relationship between hill-sachs lesion and recurrent anterior shoulder dislocation. Acta Orthop Belg 73(2):175–178
Ito H, Takayama A, Shirai Y (2000) Radiographic evaluation of the hill-sachs lesion in patients with recurrent anterior shoulder instability. J Shoulder Elbow Surg 9(6):495–497. doi:10.1067/mse.2000.106920
Rowe CR, Zarins B, Ciullo JV (1984) Recurrent anterior dislocation of the shoulder after surgical repair. Apparent causes of failure and treatment. J Bone Joint Surg Am 66(2):159–168
Kaar SG, Fening SD, Jones MH, Colbrunn RW, Miniaci A (2010) Effect of humeral head defect size on glenohumeral stability: a cadaveric study of simulated hill-sachs defects. Am J Sports Med 38(3):594–599. doi:10.1177/0363546509350295
Richards RD, Sartoris DJ, Pathria MN, Resnick D (1994) Hill-sachs lesion and normal humeral groove: Mr imaging features allowing their differentiation. Radiology 190(3):665–668
Saito H, Itoi E, Minagawa H, Yamamoto N, Tuoheti Y, Seki N (2009) Location of the hill-sachs lesion in shoulders with recurrent anterior dislocation. Arch Orthop Trauma Surg 129(10):1327–1334. doi:10.1007/s00402-009-0854-4
Hammar MV, Wintzell GB, Astrom KG, Larsson S, Elvin A (2001) Role of us in the preoperative evaluation of patients with anterior shoulder instability. Radiology 219(1):29–34
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Ethical Committee: CPP Ile de France 8, Hôpital Ambroise Paré, 92100 Boulogne, France.
Rights and permissions
About this article
Cite this article
Hardy, P., Lopes, R., Bauer, T. et al. New quantitative measurement of the Hill–Sachs lesion: a prognostic factor for clinical results of arthroscopic glenohumeral stabilization. Eur J Orthop Surg Traumatol 22, 541–547 (2012). https://doi.org/10.1007/s00590-011-0883-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-011-0883-x