Abstract
Objectives
Radial head replacement by using a bipolar prosthesis is frequently used when unable to reconstruct fractures of the radial head. The GUEPAR© implant is a metallic bipolar prosthesis. The authors describe an uneventful complication of this implant. Four patients have sustained an acute disassembling of the GUEPAR© implant after an important grip effort. A biomechanical study was performed in order to explain this disassembling.
Method
The retention system of the GUEPAR implant has been tested at different temperatures: 4, 20 and 37°C. The stem and the cup were cemented in a support. Disassembling was achieved using a dynamometer.
Results
The study has shown that the theoretical grip strength leading to disassembling is 145.65 kg at 4°C and 51.45 kg at 37°C.
Discussion
The polyethylene of the floating head of the implant appears to be very influenced by the temperature. The authors state that the association of a cam effect between the floating cup and the stem with an important grip might lead to the disassembling of the GUEPAR prosthesis. This study shows that the conception of a bipolar implant is very demanding in terms of retention of the floating head on the stem.
Résumé
Introduction
La mise en place d’une prothèse à cupule mobile représente actuellement une solution adaptée face aux fractures non reconstructibles de la tête radiale. L’implant bipolaire permet une meilleure congruence de la prothèse avec le capitellum lors des mouvements du coude. Les auteurs rapportent une séquelle non encore décrite faisant suite à l’implantation d’une prothèse de tête radiale à cupule mobile: le désassemblage aigu. Le phénomène a eu lieu chez quatre patients après un effort de poigne inhabituel, entraînant une impotence douloureuse. L’expulsion extra articulaire spontanée de la cupule prothétique a entraîné une sédation immédiate des douleurs. Les patients ayant subi cette complication ont bénéficiés une fois d’un réassemblage avec modification de la taille de la cupule, deux fois d’une résection simple de la tête radiale. Dans un cas le patient a refusé toute reprise chirurgicale. Une étude biomécanique a été réalisée afin de comprendre ce phénomène.
Methode
le système de rétention à été testé à trois températures différentes: 4, 20 et 37 degrés celsius. La tige et la cupule flottante ont été scellées dans du ciment. Le seuil de désassemblage a été mesuré à l’aide d’un dynamomètre. Un calcul a permis d’évaluer l’effort de poigne théorique conduisant au désassemblage.
Resultats
l’étude a montré que l’effort de poigne théorique conduisant au désassemblage de l’implant à la température de 4 degrés est de 145 kilogrammes, alors qu’il est de 51 kilogrammes à 37 degrés.
Discussion
le système de rétention de l’implant est fortement influencé par la température ambiante. L’existence d’une platine prenant appui sur la cupule entraîne un effet de came favorisant le désassemblage de la prothèse. Ces éléments doivent être connus lors de l’établissement du cahier des charges d’une prothèse de tête radiale à cupule mobile.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Radial head replacement for comminuted fractures of the radial head is nowadays widely accepted [1]. The poor outcome of radial head resection has convinced more and more surgeons to maintain a lateral complex of the elbow joint either by open reduction and internal fixation (ORIF) or by radial head replacement [2–7].
Although silicone rubber implants gave encouraging results [8, 9], these implants have fallen out of favour because of severe complications and the inability to restore elbow stability [10–12]. Metallic prosthesis give better results in terms of stability and durability of the implant [7, 13, 14]. Recent modular and bipolar prostheses allow better stability and matching to the anatomy of the proximal radius. The surgical procedure however remains as demanding as any other prosthesis implantation.
In 1995, Judet et al. [15] described a bipolar prosthesis with a mobile head, with good initial results. Alnot et al. [16] in 2003, described a similar implant, the GUEPAR© (Depuy™) radial head implant (Fig. 1). The use of a floating implant improves the contact between the cup and the capitellum during elbow motion. We describe an uneventful complication of this implant which has disassembled in situ in four patients.
Case series
Between April 2004 and November 2005, we have treated four patients for an acute disassembling of a GUEPAR implant. There were three women and one man. Mean age was 52 (46–58). All patients had initially sustained an unreconstructible fracture of the radial head (Table 1).
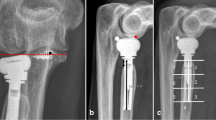
The average time to the disassembling was 40 days (5–120). All the patients describe an acute pain around the elbow following an important grip effort (Fig. 2). After a short time, the pain dramatically decreased, followed by the appearance of a subcutaneous mass at the level of the proximal radius (Fig. 3). The patients underwent various treatments, related in Table 1. The first patient refused any revision surgery and was satisfied with the result at follow up 33 months post operation. Patient 2 had revision surgery to change the implant 3 days after disassembling. Revision was completed with a cast held in 90° of flexion and neutral forearm rotation for 3 weeks. A total of 12 months after revision, clinical and radiological results are good, but the patient still has a disability allowance. Patients 3 and 4 underwent a simple removal of the whole implant. Subjective results at the last review are good for patient 3, and mild for patient 4.
Biomechanical study
Materials and methods
The retention system of the floating head of the GUEPAR implant was evaluated on two prosthesis. Implant 1 was composed by a short stem and a head of 16 mm wide, 12 mm height. Implant 2 was composed by a short stem and a head of 14 mm wide, 12 mm height. The head of the implant was cemented in a support. The stem was cemented in a 17.2 cm long tube. A dynamometer (Pesola®) was attached at the distal extremity of the tube. Forces were applied perpendicularly to the tube in order to reproduce the dislocation (Fig. 4).
The limit of disassembling was measured at three different temperatures: 4 (refrigerator temperature), 20 (ambient temperature), and 37 (body temperature) degrees Celsius. For each test, the cemented implants were placed at the predetermined temperature for 6 h. For each temperature, three tests were done on each implant.
For each temperature and implant, the torque (Nm) of disassembling was calculated.
Knowing that the in vivo mechanism of implant disassembling might be an axial pressure on the floating cup with a cam effect, an extrapolation was calculated in order to provide the theoretical grip strength leading to disassembling. According to Shaaban et al. [17], the mean axial forces through the radius are about 60% of the grip strength between 30° and 60°degrees of pronation.
Results
Results are shown in Table 2.
Discussion
The surgical management of comminuted radial head fractures remains controversial. Nevertheless, radial head replacement in face of unreconstructible fractures of the radial head may be superior to simple resection [5–7], especially when combined lesions [18] occur or when the patient are manual workers.
Several types of prosthesis have been used since early 1940s. Swanson et al. in 1968, presented a silicone rubber implant which initially gave good results [8, 9]. Long-term follow-up and biomechanical studies have shown that this type of implant is not adapted to radial head replacement [5, 7]. Metallic prosthesis provide a better stability to the elbow joint and can be very well tolerated on long-term [14].
Judet, in 1996 [15], published the initial results of a new type of prosthesis, which presented a mobile head (Tornier™, St Ismier, France). The mobile head increases the contact between the implant and the capitellar surface in order to achieve a better stability of the implant among the elbow joint. In addition, the neck of the stem presents a 15°degrees angulation that reproduces the anatomy of the proximal radius. This implant is widely used to replace the radial head and many reports have shown good results [15, 19, 20]. However, it remains technically demanding: the resection has to be wide enough to avoid a proud position of the prosthesis, and the angulation of the stem has to be perfectly placed otherwise the implant might have detrimental effects on the elbow function [21–23].
Alnot et al. in 2003 [16], presented a similar implant with a mobile head, the GUEPAR© (Depuy™, France) implant. Compared to the Judet prosthesis, the GUEPAR© implant is shorter, avoiding large resection of the neck. In this way the design does not require any angulation, given that the short resection respects the neck-shaft angle of the proximal radius. Thus the GUEPAR© prosthesis enables bone sparing and the straight shape of the stem makes it very simple to implant.
Silicone rubber implants have fallen out of favour since the end of 1980s because of various problems. Metallic implants are however, not free from complications. Friction between metal and capitellum, especially in a context of preoperative cartilaginous traumatic lesions and furthermore when the prosthesis is too proud, may lead to early capitellar erosion causing pain and stiffness [21–23]. The use of other materials such as pyrolytic carbon will perhaps limit these phenomenons [24, 25].
All of the four patients described in this study have initially sustained an unreconstructible fracture of the radial head, leading the surgeon to replace the radial head with a GUEPAR implant. The initial outcome of surgery was good and initial radiographs did not show any problem around the prosthesis.
For the four patients, an acute pain occurred while grasping with the injured side. This phenomenon is probably due to a disassembling of the head of the implant, entrapped in the humero radial space. A relief of the pain has constantly appeared with a lateral swelling of the elbow a few hours after. This is explained by the expulsion of the head of the implant out of the humero radial space, in the postero lateral subcutaneous zone.
For the biomechanical study, two implants were used. Implant 1 has been taken out of patient 4’s elbow. It did not demonstrate any macroscopic wear or damage of the polyethylene. Implant 2 has never been implanted. The results show that there is no difference between these two implants in terms of retention.
Obviously, temperature has an important impact on the retention system. To us, dilatation of polyethylene increases the weakness of the retention system of the GUEPAR© prosthesis.
Our mechanical study of the GUEPAR© implant highlights the difficulty of designing a reliable bipolar prosthesis. Indeed, although the load required to dislocate the floating head is important at low temperatures, it reaches about 50 kg of theoretical grip strength at 37°. The association of a cam effect and an important grip can lead to the post-operative disassembling of the GUEPAR implant. This study shows that the conception of a bipolar implant is very demanding in terms of retention of the floating head upon the stem. Concerning the treatment of this phenomenon, we favour a revision surgery, either to replace the implant properly if necessary or to simply reassemble a new head. Knowing the potential consequences of a radial head resection, we think that early revision is mandatory in order to avoid important damages to the capitellum
References
Morgan JW (2001) Fractures of the radial head. J Am Soc Surg Hand 4(1):225–235
Ikeda M, Oka Y (2000) Function after early radial head resection for fracture. Acta Orthop Scand 71(2):191–194
Ikeda M, Sugiyama K, Kang C, Tagagaki T, Oka Y (2005) Comminuted fractures of the radial head: comparison of resection and internal fixation. J Bone Joint Surg 87A:76–84
Janssen RPA, Vegter J (1998) Resection of the radial head after Mason type III fractures of the elbow. J Bone Joint Surg 80B:231–233
King GJW, Zarzour Z, Rath D, Dunning C, Patterson S, Johnson J (1999) Metallic radial head arthroplasty improves valgus stability of the elbow. Clin Orthop 368:114–125
King GJW (2004) Management of radial head fracture with implant arthroplasty. J Am Soc Surg Hand 4(1):11–26
Obert L, Lepage D, Huot F, Givry F, Clappaz P, Garbuio P, Tropet Y (2005) Fractures de tête radiale non synthésables: resection, implant de Swanson ou prothèse? Etude retrospective comparative. Chir Main 24:17–23
Carn RM, Medige J, Curtain D, Koenig A (1986) Silicone rubber replacement of the severely fractured radial head. Clin Orthop 209:259–269
Swanson AB, Jaeger SH, La Rochelle D (1981) Comminuted fractures of the radial head : the role of silicon-implant arthroplasty. J Bone Joint Surg 63A:1039–1049
Worsing RA, Engber WD, Lange TA (1982) Reactive synovitis from particulate silastic. J Bone Joint Surg 64A:581–585
Mayhall WS, Tiley FT, Paluska DJ (1981) Fractures of silastic radial head prosthesis. J Bone Joint Surg 63A:459–460
Gordon M, Bullough PG (1982) Synovial and osseous inflammation in failed silicone-rubber prostheses. J Bone Joint Surg 64A:574–580
Miller JH, Kaye JC, Amis AA (1986) Vitallium replacement of the radial head in trauma. J Bone Joint Surg 68B:665–666
Harrington IJ, Sekiyi-Out A, Barrington T, Evans DC, Tuli V (2001) The functional outcome with metallic radial head implants in the treatment of unstable elbow fractures: a long term review. J Trauma 50:46–52
Judet T, de Loubresse C, Garreau C, Piriou P, Charnley G (1996) A floating prosthesis for radial head fractures. J Bone Joint Surg 78B(2):244–249
Alnot J-Y, Katz V, Hardy P, le GUEPAR (2003) La prothèse de tête radiale GUEPAR dans les fractures récentes et anciennes. Rev Chir Orthop 89:304–309
Shaaban H, Giakas G, Bolton M, Williams R, Wick Ps, Scheker LR, Lees VC (2006) The load-bearing characteristics of the forearm: pattern of axial and bending force transmitted through ulna and radius. J Hand Surg [Br] 31(3):274–279
Pugh D, Wild LM, Schemitsch E, King GJW, Mc Kee D (2004) Standard surgical protocol to treat elbow dislocations with radial head and coronoid fractures. J Bone Joint Surg 86A(6):1122–1130
Popovic N, Gillet P, Rodriguez A, Lemaire R (2000) Fracture of the radial head with associated elbow dislocation: results of treatment using a floating radial head prosthesis. J Orthop Trauma 14(3):171–177
Smets S, Govaers K, Jansen N, Van Riet R, Schaap M, Van Glabbek F (2000) The floating radial head prosthesis for comminuted radial head fractures: a multicentric study. Acta Orthop Belg 66(4):353–358
Van Glabbeek F, Van Riet R, Baumfeld JA, Neale P, O’Driscoll SW, Morrey BF, An KN (2004) The kinematic importance of radial neck length in radial head replacement. Med Eng 16(3):114–121
Van Glabbeek F, Van Riet R, Baumfeld JA, Neale P, O’Driscoll SW, Morrey BF, An KN (2004) Detrimental effects of overstuffing or understuffing with radial head replacement in the medial collateral ligament deficient elbow. J Bone Joint Surg 86A(12):2629–2635
Van Riet R, Van Glabbeek F, Verbogt O, Gielen J (2004) Capitellar erosion caused by a metal radial head prosthesis. J Bone Joint Surg 86A(5):1061–1064
Cook SD, Thomas KA, Kester MA (1989) Wear characteristics of the canine acetabulum against different femoral prostheses. J Bone Joint Surg 71B:189–197
Allieu Y, Winter M, Péquignot JP, De Mourgues Ph (2006) Radial head replacement with a pyrocarbon head prosthesis: preliminary results of a multicentric prospective study. Eur J Orthop Surg Traumatol 16(1):1–9
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Winter, M., Pelegri, C., Balaguer, T. et al. Acute bipolar radial head prosthesis disassembling. Eur J Orthop Surg Traumatol 18, 101–105 (2008). https://doi.org/10.1007/s00590-007-0269-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-007-0269-2