Abstract
Purpose
The goal of this study was to compare the accuracy of a novel intraoperative cone beam computed tomography (CBCT) imaging technique with that of conventional computed tomography (CT) scans for assessment of pedicle screw placement and breach detection.
Methods
Three hundred and forty-eight pedicle screws were inserted in 58 patients between October 2013 and March 2016. All patients had an intraoperative CBCT scan and a conventional CT scan to verify the placement of the screws. The CBCT and CT images were reviewed by two surgeons to assess the accuracy of screw placement and detect pedicle breaches using two established classification systems. Agreement on screw placement between intraoperative CBCT and postoperative CT was assessed using Kappa and Gwet’s coefficients. Using CT scanning as the gold standard, the sensitivity, specificity, positive predictive value, and negative predictive value were calculated to determine the ability of CBCT imaging to accurately evaluate screw placement.
Results
The Kappa coefficient was 0.78 using the Gertzbein classification and 0.80 using the Heary classification, indicating a substantial agreement between the intraoperative CBCT and postoperative CT images. Gwet’s coefficient was 0.94 for both classifications, indicating almost perfect agreement. The sensitivity, specificity, positive predictive value and negative predictive value of the CBCT images were 77, 98, 86, and 96%, respectively, for the Gertzbein classification and 79, 98, 88, and 96%, respectively, for the Heary classification.
Conclusions
Intraoperative CBCT provides accurate assessment of pedicle screw placement and enables intraoperative repositioning of misplaced screws. This technique may make postoperative CT imaging unnecessary.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Placement of pedicle screws, because of their biomechanical properties, has become a widely used procedure for spinal fusion in the treatment of various pathologies, including trauma, scoliotic deformities, infection, and degenerative and malignant diseases [1, 2]. An ideally placed screw is fully contained within the pedicle without any breach. However, variations in the size and shape of spinal vertebrae can increase the risk of misplacement. Pedicle screw placement has been the subject of many studies evaluating accuracy and surgical complications. Indeed, incorrect screw placement with pedicle breach can lead to spinal cord, visceral and vascular injuries, with complications in terms of patient survival and fixation instability [3, 4].
Many techniques have been described for detection of pedicle breach. Standard techniques are direct visualization and manual wall inspection with a ball-tipped probe [5, 6]; however, it is not possible to detect a breach after screw insertion [5]. Other options include imaging techniques. The CT scan is the clinical standard for assessing the correct position of pedicle screws and the spinal fusion between the instrumented vertebrae [7,8,9,10]. This technique can provide three-dimensional (3D) information instead of the two-dimensional (2D) images from a plain radiograph [10, 11]. Rao et al. concluded that CT scanning provides adequate in vitro and in vivo assessment of screw position [9]. Unfortunately, CT scans are seldom available intraoperatively, and screw position is assessed postoperatively, so that intraoperative repositioning of misplaced screws is not possible.
Several intraoperative 3D-imaging techniques have been adapted to enable direct pedicle breach determination, including intraoperative CT [12] and intraoperative 3D-fluoroscopy called cone beam computed tomography (CBCT) [7, 8, 13]. These techniques have the clinically important advantage of enabling direct repositioning of misplaced screws, thereby potentially reducing the re-operation rate and the number of postoperative CT scans required [12,13,14].
A new intraoperative CBCT imaging technique consisting in a robotic system (Artis zeego, Siemens Healthcare, Forchheim, Germany) is now available. Unlike the O-arm originally designed to support orthopedic surgery [15], the Artis zeego was firstly developed in interventional angiography for transfemoral aortic valve implantation, percutaneous coronary intervention [16], transarterielle chemo-perfusion [17], or liver segmentation [18]. It has recently been adapted for spinal surgery, as described by Richter et al. [19] and Raftopoulos et al. [20]. The purpose of this new imaging technique is to assist the surgeon in the placement of pedicle screws, as well as to assess pedicle screw placement intraoperatively.
The goal of this retrospective study was to assess the efficacy of this new CBCT technique for intraoperative assessment of pedicle screw insertion and pedicle breach determination, and to compare it with conventional postoperative CT scans.
Materials and methods
We retrospectively reviewed all spinal instrumentation performed by two orthopedic surgeons at Clinique universitaires Saint-Luc, Brussels, Belgium, between October 2013 and March 2016.
Patient selection
Among the spinal interventions performed by the two surgeons on this period, we have selected only the patient who had an intraoperative CBCT scan after screws insertion and a CT scan after the surgery to assess the screw position. The CT scans included 18 postoperative CT made directly after the surgery. Half of them were made for the surgery follow-up (radiculopathy, pain), the other half were made for other reasons (respiratory symptoms, abdominal dysfunction). The other patients (40/58) had a CT scan at least one month after the surgery for osseous fusion (18/40), for pain symptoms during consultation (11/40), for cancer follow-up (5/40), for respiratory or urology symptoms (4/40), for control of fall (2/40), for coxofemoral arthropathy (1/40) and infection after abdominal surgery (1/40). A total of 38 (66%) CT scans were made for the spine surgery follow-up. The average interval between the surgery and the postoperative CT scan was 3 months.
Surgical technique
All patients were placed in the prone position during standard posterolateral fusion surgery. The surgeon checked the surgical level using 2D-fluoroscopy and made a mark on the skin. The skin was then disinfected and covered with sterile drapes. Skin incision and soft tissue dissection were made at the corresponding levels. A drill was used to make a hole in the cancellous bone of the pedicle for screw insertion. After all the screws had been inserted, a CBCT scan was performed.
CBCT imaging technique
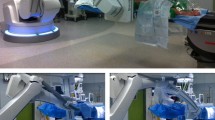
The intraoperative 3D-imaging device consists of a floor-mounted multi-axis robotic C-arm “Artis zeego” system (Fig. 1a) equipped with “syngo DynaCT” software (Siemens Healthcare, Forchheim, Germany). This system can operate as standard 2D-fluoroscopy and as a rapid 3D-fuoroscopy CT-like imaging system. Equipped with a large flat panel detector (size 300 × 400 mm), the system acquires 3D volumetric data by rotating isocentrically around the patient through 200° (Fig. 1b–e). In our institution, the default mode for 3D acquisition in spinal surgery acquires 397 projection images during a 6-s spin (6sDCT). During this acquisition, the surgeon and medical staff step out of the operating room to reduce their personal X-ray exposure. The acquired images are then automatically transferred to a dedicated workstation (syngo X Workplace, Siemens Healthcare) where they are reconstructed to volumetric data with an isotropic voxel-size of 0.5 mm using a filtered backprojection algorithm. The volumetric data can be visualized intraoperatively as multi-planar reformattations (MPR) in any desired plane orientation or as a volume rendering technique (VRT). Figure 2 shows examples of the MPR and VRT images that could be used intraoperatively to check screw positions.
Illustrations of the Artis zeego imaging system and simulated intraoperative use. a Intraoperative setup with the Artis zeego system positioned prior to image acquisition. b–e The Artis zeego system moves around the patient, continuously acquiring fluoroscopic images. White arrows represent direction of X-rays
Assessment of screw position
All the screws were assessed using intraoperative CBCT and CT scan images, and then graded using two established classifications: Gertzbein and Heary (Table 1).
The Gertzbein classification uses five grades from 0 to 4: screws fully contained within the pedicle are graded 0; medial breaches of <2 mm are graded 1; medial breaches of 2–4 mm are graded 2; medial breaches of >4 mm are graded 3; lateral and other breaches are graded 4.
The Heary classification uses five grades from I to V: screws entirely contained within the pedicle are graded I; In-out-in screws with a lateral breach but with the screw tip entirely contained within the vertebral body are graded II; screws with a tip that penetrated the anterior or lateral vertebral body are graded III; medial or inferior pedicle breaches are graded IV; screws that endanger the spinal cord, nerve root, or great vessels, and that require immediate revision are graded V.
The pedicle screw assessment was done on the intraoperative CBCT and on CT scan images separately by each of the two experienced surgeons who inserted the screws. The surgeons reviewed the images for screw placement assessment independently, at separate times and locations according to their availabilities. They systematically started by the CBCT images at first, and reviewed the CT images afterwards. A third joint session was made to discuss the discrepancies on the grading to reach a consensus. Figure 3a and b illustrates the comparison between screw placement assessment using intraoperative CBCT and conventional CT scan images.
Operative characteristics: radiation and operative time
During surgery, the patient was exposed to radiation. We investigated radiation exposure using the total dose area product (DAP, Gy cm2), to estimate the stochastic effects (e.g., cancer and genetic mutation), and the total skin dose (SD, mGy), to estimate the deterministic effects (e.g., skin injuries, cataract) and calculated from DAP by the system [21,22,23,24]. These parameters were automatically generated by the exam protocol of the CBCT system, which is an excerpt of the X-ray Radiation Dose Structured Report (RDSR). These data were reported using medians and interquartile ranges (IQ).
Operative time was investigated by the review of anesthesia and surgery protocols. We used the total time in operative room (from entrance to exit of the patient) and the surgical time (from surgical incision to closure), both expressed in minutes (min). These data were reported using means and standard deviations (SD).
Statistical analysis
Analyses were performed using the Statistical Package for Social Sciences (SPSS) version 23.0 software package and a free software R version 3.0.3. Reliability tests computing Cohen’s Kappa coefficients [25] and Gwet’s coefficients [26] were performed to compare the ability of the CBCT imaging technique to assess screw placement and determine pedicle breach with that of conventional postoperative CT scans. Gwet’s coefficient is an alternative to the Kappa statistic because the Kappa coefficient is influenced by prevalence and hardly comparable across studies. A coefficient value close to 1 indicates almost perfect agreement and a value close to 0 indicates poor agreement. We used the Landis and Koch standards for the strength of agreement [27] with <0.00 indicating poor agreement, 0.00–0.20 slight agreement, 0.21–0.40 fair agreement, 0.41–0.60 moderate agreement, 0.61–0.80 substantial agreement, and >0.81 almost perfect agreement.
Sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) of the CBCT imaging technique to assess screw placement were computed, using postoperative CT scans as the gold standard. Values of Kappa coefficient, Gwet’s coefficient, sensitivity, specificity, PPV, and NPV are presented with their 95% confidence intervals (CI). The analyses were performed in R version 3.0.3 (with the customized R code available upon request from the authors).
Results
Demographic results
From October 2013 to March 2016, 348 pedicle screws were inserted in 58 patients who had CBCT and CT scan images. The mean patient age was 61.5 years; 153 (44%) screws were inserted in male patients and 195 (56%) in female patients. Thirty-eight of the patients (65.5%) had surgery for degenerative disease, 8 (13.8%) for trauma, 6 (10.3%) for malignancy, 4 (6.9%) for infection, and 2 (3.4%) for scoliosis. Of the 348 screws, 135 (38.8%) were inserted at the thoracic level (from T1 to T12), 193 (55.5%) at the lumbar level (L1 to L5), and 20 (5.7%) at the first sacral level (S1).
Assessment of screw position
Using the Gertzbein classification, 19 of the 348 screws (5.5%) were graded differently using the CBCT and conventional CT scans (Table 2). Eleven screws were graded 0 with no breach with the CBCT technique, while the conventional CT technique revealed six breaches of <2 mm (grade 1) and five screws with lateral breaches (grade 4). Seven screws were graded 1 with a medial breach <2 mm with the CBCT imaging technique, while the conventional CT technique revealed five screws with no breach (grade 0) and two screws with a medial breach of 2–4 mm (grade 2). Finally, one screw was graded 4 on CBCT imaging, while the conventional CT revealed no breach (grade 0).
Using the Heary classification, 18 of the 348 screws (5.2%) were graded differently (Table 3). Twelve screws were graded I without any breach with CBCT, while the conventional CT revealed five screws with in-out-in breach (grade II), one screw with anterior breach (grade III), and six screws with medial breach (grade IV). One screw was graded II with CBCT, while the conventional CT revealed no breach (grade I). Finally, five screws were graded IV with medial breaches on CBCT, but with no breach on postoperative CT (grade I).
The pedicle screws that were graded differently using the CBCT and CT images were the same for the Gertzbein and Heary classifications, except for three screws (two of them were graded differently only for Gertzbein and one only for Heary classification).
Using the Gertzbein classification, agreement on screw placement between the intraoperative CBCT and the CT scans was substantial, with a Kappa coefficient of 0.78 (CI 0.68–0.88) and almost perfect, with a Gwet coefficient of 0.94 (CI 0.91–0.97). The sensitivity of the CBCT imaging technique was 0.77 (CI 0.62–0.88), the specificity 0.98 (CI 0.96–0.99), the PPV 0.86 (CI 0.71–0.95), and the NPV 0.96 (CI 0.94–0.98). Using the Heary classification, agreement on screw placement was substantial, with a Kappa coefficient of 0.80 (CI 0.71–0.89) and almost perfect, with a Gwet of 0.94 (CI: 0.89–0.96). The sensitivity was 0.79 (CI 0.66–0.88), the specificity 0.98 (CI 0.96–0.99), the PPV 0.88 (CI 0.76–0.95), and the NPV 0.96 (CI 0.93–0.98). Table 4 summarizes all the results for each classification used and Fig. 4 shows the ROC curve for sensibility and specificity for the Gertzbein and Heary classifications.
Radiation and operative time
Concerning the radiation exposure for patient during standard posterolateral fusion surgery, we measured a total DAP (Gy cm2) of 81.56 (IQ 43.41–122.2) and a total SD (mGy) of 267.20 (IQ 148.7–409.35). The results for operative time showed a total time in operative room of 391 ± 155 min and a surgical time of 272 ± 131 min.
Discussion
This study compared the efficacy of a new intraoperative CBCT imaging technique with that of conventional postoperative CT scans for assessment of pedicle screw placement and breach detection. The accuracy of the CBCT imaging system was similar to that of conventional CT scans for breach detection and grading of pedicle screw placement.
In terms of sensitivity, specificity, PPV, and NPV, postoperative CT images are considered as the gold standard with values of 100% for each parameter. Using the Gertzbein classification, the sensitivity of the CBCT images was 77%, indicating that if a breach is detected on the CT scan, it will be detected on the CBCT images in 77% of cases. Similarly, using the Heary classification, the sensitivity of 79% indicates that if a breach is detected on the CT scan, it will be detected on the CBCT images in 79% of cases. A specificity of 98%, with the Gertzbein and Heary classifications, indicates that when there is no breach on the CT scan, a breach will be detected on the CBCT images in only 2% of cases. The results in terms of sensitivity and specificity—the specificity, close to 1 (98%), is higher than the sensitivity—suggest that CBCT-based assessment tends to slightly underestimate pedicle breach occurrence compared to CT-based assessment. However, none of the patients with a difference in pedicle grades between the two imaging techniques required surgical revision.
A PPV of 86% with the Gertzbein classification indicates that, for all the breaches identified using the CBCT images, 86% were correctly classified. With the Heary classification, the PPV was 88%, indicating that 88% of the breaches identified using the CBCT images were correctly classified. An NPV of 96%, with the Gertzbein and Heary classifications, indicates that 96% of the screws identified as being correctly placed on the CBCT images were correctly classified; this classification was incorrect in just 4% of the cases.
Our observations agree with those of previous studies that have investigated the efficacy of intraoperative fluoroscopy for pedicle breach determination. Santos et al. [8] compared the efficacy of O-arm images with that of direct visualization on cadavers as gold standard for pedicle breach detection. They reported sensitivity, specificity, PPV, and NPV of 76, 71, 74, and 72%, respectively. The study of Wang et al. used the direct inspection for the pedicles as gold standard and showed a sensitivity of 0.716 with the 3-D fluoroscopy, and a sensitivity of 0.608 with conventional CT. Garber et al. [13] compared the efficacy of intraoperative O-arm (Medtronic, Minneapolis, MN, USA) fluoroscopic images with that of postoperative CT images for pedicle breach detection in a series of 73 pedicle screws inserted under O-arm guidance. They reported a Kappa coefficient of 0.79 and sensitivity, specificity, PPV, and NPV of 85, 97, 82, and 98%, respectively.
In our study, the sensitivity of 77 and 79% for Gertzbein and Heary classifications, respectively, might be explained by the number of the false negative in each classification. The sensitivity decreases with the number of false negative (11 screws in Gertzbein classification and 12 screws in Heary classification). However, all these breaches were minors (perforation of medial wall less than 2 mm) or were “in-out-in” screws which can be consider as accurate for theirs mechanical stability [28]. Furthermore, many studies have demonstrated sensitivity from 67 to 94% for the conventional postoperative CT scan [9, 29,30,31]. Our results are in these ranges.
The metallic artifact due to the screws could complicate the review of the images, particularly in the small pedicles and could explain the two underestimated breach on the CBCT images (Gerzbein grade 1-Heary grade IV on CBCT images and Gertezbein grade 2-Heary grade IV on the CT images) which were in thoracic segment. There was no complication after the surgery for these screws.
The degree of radiation exposure was also investigated using the total DAP and the total SD. The results showed a total DAP of 81.56 Gy cm2 and a total SD of 267.20 mGy. The recent study of Kaminski et al. [32] showed a total DAP of 82.8 Gy cm2 (9.17–286.8) and a SD of 273 (31.0–1031) using the Artis zeego for thoracic and lumbar spine fusion. Harstall et al. [33] studied radiation with fluoroscopy during vertebroplasty and showed a mean total DAP of 27.72 Gy cm2. Using thermoluminescence dosimeters, Gebhard et al. [34] studied intraoperative radiation in 38 patients for spine surgery. They reported a median of 1091 mGy for standard procedure, 432 mGy for CT-based surgery, 664 mGy in C-arm-based surgery, and 152 mGy for Iso-C3D C-arm-based surgery.
Our results were higher than 2D-fluoroscopy as expected, but lower than the radiation exposure with the intraoperative CT.
Regarding the operative time, our results were consistent with those of Ling et al. [35], showing a mean operative time of 325 min with the O-arm coupled with navigation system and of 314 min with fluoroscopy control group. Laine et al. [36] showed a mean operative time of 160 ± 73 (range 47–360) min in conventional pedicle screw insertion and of 179 ± 74 (range 95–425) min in computer-assisted navigation group. In their study, Jin et al. [37] found a mean operative time of 268 ± 21 min in O-arm group and 257 ± 13 min in fluoroscopy group. The operative time with intraoperative 3D-imaging system seems to be more time consuming than conventional systems. In our study, this difference could be partly explained by the systematic intraoperative CBCT scan performs at the end of the surgery which is time consuming.
In conclusion, this study compares the efficacy of a new CBCT system with that of conventional postoperative CT scans for determination of pedicle breach. Intraoperative CBCT images seem to allow accurate assessment of pedicle screw placement. The surgeon can therefore assess screw position or detect breaches intraoperatively on the 3D images and decide to reposition the screw if necessary with relative consequences in terms of operative time. Use of this new system for screw assessment does not expose the patient to extra radiation compared to other systems. This technique could potentially reduce the re-operation rate and decrease the number of postoperative CT scans required with benefits in terms of morbidity and patient cost.
Further studies should be performed to account for additional factors that may impact the overall quality of pedicle screw assessment and breach detection using the new intraoperative CBCT imaging system. These factors include, among others, image quality depending on the protocol used, time necessary to manipulate and review the images, and use of a navigation system.
References
Boos N, Webb JK (1997) Pedicle screw fixation in spinal disorders: a European view. Eur Spine J 6(1):2–18
Mobbs RJ, Sivabalan P, Li J (2011) Technique, challenge and indications for percutaneous pedicle screw fixation. J Clin Neurosci 18(6):741–749
Jutte PC, Castelein RM (2002) Complications of pedicle screws in lumbar and lumbosacral fusion in 105 consecutive primary operations. Eur Spine J 11(6):594–598
Li G, Lv G, Passias P et al (2010) Complications associated with thoracic pedicle screws in spinal deformity. Eur Spine J 19(9):1576–1584
Donohue ML, Moquin RR, Singla A, Calancie B (2014) Is in vivo manual palpation for thoracic pedicle screw instrumentation reliable? J Neurosurg Spine 20:492–496
Lehman RA, Potter BK, Kuklo TR, Chang AS (2004) Probing for thoracic pedicle screw tract violation(s): is it valid? J Spinal Disord Tech 17(4):227–283
Sembrano JN, Polly DW Jr, Ledonio CG, Santos ER (2016) Intraoperative 3-dimensional imaging (O)arm for assessment of pedicle screw position: does it prevent unacceptable screw placement? Int J Spine Surg 6:49–54
Santos ER, Ledonio CG, Castro CA, Truong WH, Sembrano JN (2012) The accuracy of intraoperative O-arm images for the assessment of pedicle screw position. Spine (Phila Pa 1976) 37(2):E119–E125
Rao G, Brodke DS, Rondina M, Dailey AT (2002) Comparison of computerized tomography and direct visualization in thoracic pedicle screw placement. J Neurosurg (Spine 2) 97:223–226
Faber GL, Place HM, Mazur RA et al (1995) Accuracy of pedicle screw placement in lumbar fusions by plain radiographs and computed tomography. Spine (Phila Pa 1976) 20(13):1494–1499
Steinmann JC, Herkowitz HO, El-Kommos H, Wesolowski DP (1993) Spinal pedicle fixation: confirmation of an image-based technique for screw placement. Spine (Phila Pa 1976) 18:1856–1861
Scheufler KM, Franke J, Eckardt A, Dohmen H (2011) Accuracy of image-guided pedicle screw placement using intraoperative computed tomography-based navigation with automated referencing. Part II: thoracolumbar spine. Neurosurgery 69(6):1307–1316
St Garber, Bisson EF, Schmidt MH (2012) Comparison of three-dimensional fluoroscopy versus postoperative computed tomography for the assessment of accurate screw placement after instrumented spine surgery. Global Spine J 2(2):95–98
Ling JM et al (2014) Routine spinal navigation for thoraco-lumbar pedicle screw insertion using the O-arm three-dimensional imaging improves placement accuracy. J Clin Neurosci 21:493–498
Zhang J, Weir V, Fajardo L, Lin J, Hsiung H, Ritenour R (2009) Dosimetric characterization of cone-beam O-arm™ imaging system. J X-ray Sci Technol 17:305–317. doi:10.3233/XST-2009-0231
Boland J, Wang L, Love B, Christofi M, Muller D (2016) Impact of new-generation hybrid imaging technology on radiation dose during percutaneous coronary interventions and trans-femoral aortic valve implantations: a comparison with conventional flat-plate angiography. Hurt Lung Circ 25:668–675
Vogl J, Naguib N, Nour Eldin N, Lehnert T, Mbalisike E (2009) Transarterielle Chemo-perfusion und-embolisation thorakaler Neoplasmen mittels C-Arm-CT. Der Radiol 49:837–841. doi:10.1007/s00117-009-1863-6
Diana M, Liu Y, Pop R, King S et al (2016) Superselective intra-arterial hepatic injection of indocyanine green (ICG) for fluorescence image-guided segmental positive staining: experimental prof of the concept. Surg Endosc 3:1451–1460. doi:10.1007/s00464-016-5136-y
Richter PH, Yarboro S, Kraus M, Gebhard F (2015) One year orthopaedic trauma experience using an advanced interdisciplinary hybrid operating room. Injury 46(Suppl 4):S129–S134
Raftopoulos C, Waterkeyn F, Fomekong E, Duprez T (2012) Percutaneous pedicle screw implantation for refractory low back pain: from manual 2D to fully robotic intraoperative 2D/3D fluoroscopy. Adv Tech Stand Neurosurg 38:75–93
Stecker S et al (2009) Guidelines for patient radiation dose management. J Vasc Interv Radiol 20:S263–S273
Balter S (2006) Methods for measuring fluoroscopic skin dose. Pediatr Radiol 36:136–140
IEC (2010) Report 60601 medical electrical equipment—part 2–43: particular requirement for the safety of X-ray equipment for interventional procedures, 2nd edn. International Electrotechnical Commission, Geneva
Paul J, Jacobi V, Farhang M, Bazrafshan B, Vogl T, Mbalisike E (2013) Radiation dose and image quality of X-ray volume imaging systems: cone-beam computed tomography, digital subtraction angiography and digital fluoroscopy. Eur Radiol 23:1582–1593. doi:10.1007/s00330-012-2737-2
Sim J, Wright CC (2005) The Kappa Statistics in reliability studies: use, interpretation and sample size requirements. Phys Ther 85(3):257–268
Gwet KL (2014) Handbook of inter-rater reliability: the definitive guide to measuring the extent agreement among multiple raters, 4th edn. Advanced Analytics, LLC, Gaithersburg, USA
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Puvanesarajah V, Liauw J, Lo S, Lina I, v T (2014) Techniques and accuracy of thoracolumbar pedicle screw placement. World J Orthop 5(2):112–123. doi:10.5312/wjo.v5.i2.112
Brooks D, Eskander M, Balsis S, Ordway N, Connolly P (2007) Imaging assessment of lumbar pedicle screw placement. sensitivity and specificity of plain radiographs and computer axial tomography. Spine 32(13):1450–1453
Learch T, Massie J, Pathria M, Ahlgren B, Garfin S (2004) Assessment of pedicle screw placement utilizing conventional radiography and computed tomography: a proposed systematic approach to improve accuracy of interpretation. Spine (Phila Pa 1976) 29(7):767–773
Yoo J, Ghanayem A, Petersilge C, Lewin J (1997) Accuracy of using computed tomography to identify pedicle screw placement in cadaveric human lumbar spine. Spine 22(22):2668–2671
Kaminski L, Cordemans V, Cartiaux O, Van Cauter M (2017) Radiation exposure to the patients in thoracic and lumbar spine fusion using a new intraoperative cone-beam computed tomography imaging technique: a preliminary study. Eur Spine. doi:10.1007/s00586-017-4968-z
Harstall R, Heini PF, Mini RL, Orler R (2005) Radiation exposure to the surgeon during fluoroscopically assisted percutaneous vertebroplasty: a prospective study. Spine 30:1893–1898
Gebhard FT, Kraus MD, Scneider E et al (2006) Does computer-assisted spine surgery reduce intraoperative radiation doses? Spine (Phila Pa 1976) 31:2024–2027
Ling J, Dinesh S, Pang B et al (2014) Routine spinal navigation for thoraco-lumbar pedicle screw insertion using the O-arm three-dimensional imaging system improves placement accuracy. J Clin Neurosci 21:493–498
Laine T, Lund T, Ylikoski M, Lohikoski J, Schlenzka D (2000) Accuracy of pedicle screw insertion with and without computer assistance: a randomised controlled clinical study in 100 consecutive patients. Eur Spine J 9(3):235–240
Jin M, Liu X, Yan H, Han X, Qiu Y, Zhu Z (2015) Doe intraoperative navigation improve the accuracy of pedicle screw placement in the apical region of dystrophic scoliosis secondary to neurofibromatosis type I: comparison between O-arm navigation and free-hand technique. Eur Spine J 25(6):1729–1737. doi:10.1007/s00586-015-4012-0
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Cordemans has received funding from Siemens for this investigation regarding Artis zeego imaging system. Dr. Banse is consultant for Siemens. Dr. Cartiaux is funded by the Brussels Capital Region-Innoviris (Grant BB2B 2012-1-05). Drs. Kaminski and Francq declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Cordemans, V., Kaminski, L., Banse, X. et al. Accuracy of a new intraoperative cone beam CT imaging technique (Artis zeego II) compared to postoperative CT scan for assessment of pedicle screws placement and breaches detection. Eur Spine J 26, 2906–2916 (2017). https://doi.org/10.1007/s00586-017-5139-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5139-y