Abstract
Purpose
Kyphosis of the cervical spine has been reported in patients with adolescent idiopathic scoliosis (AIS). However, few reports have compared sagittal spine alignment of AIS patients with that of the normal population. The purposes of this study were (1) to analyze the characteristics of sagittal alignment, including the cervical spine, in AIS patients with a single thoracic curve (Lenke type 1) compared with the age-matched normal population and (2) to quantify the changes in sagittal alignment of the cervical spine and thoracic kyphosis following posterior spinal fusion.
Methods
In study 1, pre- and postoperative X-ray were measured for the following sagittal plane parameters: lumbar lordosis angle (L1–S1; LL), thoracic kyphosis angle (Th5-12; TK), sacral slope (SS), C7 plumb line (C7PL), cervical lordosis angle (C2–C7 angle; CL), and T1 slope. These measurements were then evaluated with CL and other parameters using spearman rank correlation coefficient between two groups. Comparison was made with the sagittal plane parameters from preoperative 42 AIS (AIS group) with main thoracic curve and 24 normal populations (Control group). In study 2, 38 operative AIS patients had at least 1-year follow-up. These patients (38 AIS patients after the correction surgery) were enrolled. We collected for each patient on pre- and postoperative sagittal plane parameters of X-ray.
Results
In study 1, LL and C7PL did not differ significantly between the groups. Although CL was observed in 10 of the 24 patients (41.7 %) in the Control group, the CL was smaller in the AIS group, with 6 of 42 patients (14.3 %). The CL correlated significantly with T1 slope (r = 0.634), C7PL (r = 0.684), and TK (r = 0.311) in the AIS group, and with T1 slope (r = 0.681) and C7PL (r = 0.451) in the Control group. No correlations were observed with respect to the TK. In study 2, the mean CL improved significantly from 7.2° kyphosis preoperatively to 0.1° kyphosis postoperatively. Interestingly, Spearman correlation analysis showed that the postoperative CL correlated significantly with postoperative TK (r = 0.607), postoperative T1 slope (r = 0.701), and postoperative C7PL (r = 0.373).
Conclusions
There were no effects of scoliosis on sagittal spine parameters such as LL and C7PL in AIS patients with a main thoracic curve. Cervical spine alignment was affected by the thoracic deformity in the sagittal plane, as shown by the reduction in the CL after the operation. These findings suggest that TK may be a cause of cervical kyphosis in AIS patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adolescent scoliosis, also termed adolescent idiopathic scoliosis (AIS), occurs in around 2–3 % of the general population [1]. AIS is a three-dimensional deformity of the spine [2]. Deformity of spine has been recently characterized in the coronal and sagittal planes in AIS patients. Many radiographic parameters have been described to assess the sagittal alignment and the importance of considering the sagittal spinal and pelvic alignments for the treatment of spinal pathologies [3]. However, the sagittal spine alignment of AIS is poorly described in the literature compared with adult spinal deformities. In patients with thoracic scoliosis, coronal deformity is often associated with sagittal alignment. Flattening or kyphosis of the cervical and thoracic spines has been reported in AIS patients [4, 5]. Generally, a decrease in cervical lordosis and thoracic kyphosis is commonly associated with AIS [6]. Some studies have reported that a hypokyphotic thoracic spine coexists with kyphosis in the cervical spine in AIS patients. Using sagittal plane X-rays, Hilibrand et al. were the first to confirm a relationship between the thoracic and cervical spines in AIS patients. They reported a straight (lordosis <5°) or kyphotic cervical alignment in 34 of 39 patients (89 %) and concluded that patients with idiopathic scoliosis develop lordosis within the thoracic spine and compensatory kyphosis within the cervical spine [7]. Canavese et al. also found that 34.4 % of patients with AIS had an average of 11° cervical kyphosis with thoracic kyphosis and that the reduction of cervical lordosis was proportional to the reduction of thoracic kyphosis [8]. Based on this background, Hu et al. used morphological classification to analyze the relationship between the cervical spine and global spinal–pelvic alignment in AIS patients and reported that cervical kyphosis was a part of the cervicothoracic sagittal deformity in AIS patient and was correlated with global sagittal alignment [9]. Clement et al. analyzed the relationship between lumbar lordosis and thoracic kyphosis [10] and found that decreased thoracic kyphosis is associated with decreased lumbar lordosis in AIS patients.
The studies described above evaluated sagittal alignment in the same AIS patients, and no full comparison of the sagittal alignment of AIS patients with that of the normal populations has been reported. To our knowledge, Upasani et al. have reported the only study comparing the sagittal profiles of patients with AIS with age-matched controls [11]. In this study, we retrospectively examined the characteristics of sagittal alignment, including the cervical spine, in AIS patients with a main thoracic curve. The first purpose of this study was to compare the sagittal alignment in AIS patients with a main thoracic curve with that of a normal age-matched control population (study 1). A better understanding of the sagittal changes of the spinal column and their effects on other parts of the body and the operative outcomes is still needed. Despite the report on surgical correction of the thoracic and lumbar spines in AIS patients inducing significant changes in the sagittal spinopelvic profile, the effect on the detail of sagittal parameters, including the cervical spine, has not been reported. Thus, the second purpose of this study was to quantify the changes in the sagittal alignment of the cervical spine, thoracic kyphosis, and other parameters following posterior spinal fusion using multisegmented hook and screw instrumentation in AIS patients (study 2).
Materials and methods
Ethics statement
The Committee on Ethics and the Institutional Review Board of Tokai University School of Medicine approved the study protocol (Approval number: 15R-164). This investigation was designed as a single-center retrospective comparative study of AIS patients.
Participants
Between March 2010 and March 2015, 58 patients (52 females) with thoracic AIS (Lenke type 1–4) who had undergone posterior fusion with hybrid constructs were reviewed at our institute retrospectively. The inclusion criteria were an admission diagnosis of AIS with no other pathological conditions, age between 12 and 21 years, and no previous spine surgery. The Cobb angles of any structural curves were measured, and the proximal thoracic curve, main thoracic curve, and thoracolumbar/lumbar curve were measured as described by Lenke et al. [12]. We focused on AIS patients with the main thoracic curve type. Based on the Lenke classification, 42 had a type 1 curve, 7 had a type 2 curve, 8 had a type 3 curve, and 1 had a type 4 curve. The first purpose of this study was to analyze the characteristics of sagittal alignment, including the cervical spine, in AIS patients with a single thoracic curve (Lenke type 1) (called AIS group in this paper) compared with the age-matched normal population. Thus, a total of 42 patients were enrolled in study 1. The mean patient age at surgery was 15.1 years (range 12–21 years). The primary Cobb angle in the AIS group was 49.8° ± 11.9°.
All patients were evaluated preoperatively and at the last follow-up. Postoperative values were measured on radiographs obtained at the last follow-up visit; therefore, the clinical follow-up was equivalent to the radiographic follow-up in this series. A minimum of 1-year follow-up was required, and 38 AIS patients attended at least the 1-year follow-up (mean follow-up, 31 ± 15 months). These 38 AIS patients after the correction surgery were enrolled in study 2.
Control patients
For comparison, 24 patients (20 females) with a coronal Cobb angle of <10° were also included in study 1 as the control group (control group). The mean patient age was 14.7 years (range 12–18 years). These people were matched for age and sex with the patients in the AIS group.
Radiologic analysis
All 66 patients (AIS group and control group, 58 females and 8 males) had a full-spine radiological assessment. X-ray evaluation involved examination of standing erect whole-spine posteroanterior and lateral full-spine radiographs. Coronal flexibility of the curves or the primary and compensatory curves was assessed based on bending radiographs and traction radiographs. Flexibility radiographs have been recommended to help determine the surgical technique and the levels to be selected in the correction of scoliosis. Flexibility of both the thoracic and lumbar curves was determined from Cobb measurements on the preoperative standing and supine bending radiographs. Frontal assessment included measurement of the coronal Cobb angle of the main coronal curvature. For the lateral films, the patients stood with their knees locked, the feet shoulder-width apart, looking straight ahead, and with their elbows bent and knuckles in the supraclavicular fossa bilaterally [13].
All morphologic data were archived using picture archiving and communication systems (PACS). The films were retrieved and measured using the PACS on 17-inch diagonal screens with a resolution of 75 dpi. The main curve was determined as the most rigid curve with the greatest rotation of the apical vertebra and curve angle. We used Lenke’s classification system to determine the types of deformities [12].
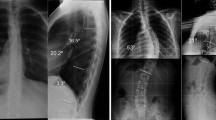
The X-rays were assessed for the following sagittal plane parameters (Fig. 1): lumbar lordosis angle (L1–S1, LL), the angle between the superior endplate of L1 and the superior endplate of S1; thoracic kyphosis angle (T5–T12, TK), the subtending angle between the superior endplate of T5 and the inferior endplate of T12; sacral slope (SS), the angle subtended by the superior endplate of S1 and the horizontal; C7 plumb line (C7PL), the horizontal distance between the posterosuperior angle of S1 and a vertical line through the middle of the C7 inferior endplate; cervical lordosis angle (C2–C7 angle, CL), the angle between the lower endplate of C2 and the inferior endplate of C7; T1 slope, the angle between the horizontal and the superior endplate of T1 in the standing lateral radiograph. These measurements with the CL or TK and other parameters were then compared between the two groups using the Spearman rank correlation coefficient. The cervical alignment was further classified into four types—kyphosis, straight, sigmoid, and lordosis—as described by Yu et al. [14].
Operative procedure
All patients in the AIS group underwent posterior spinal fusion and instrumentation using hybrid constructs. Fusion levels of 38 AIS patients were selected following the same criteria during the entire study period. The upper instrumented vertebra was in T3–T5 (T3, n = 14; T4, n = 19; T5, n = 5) and the lowest instrumented vertebra (LIV) varied according to the location of the stable and neutral vertebra in L1–L3 (L1, n = 4; L2, n = 19; L3, n = 15). Intraoperative spinal cord monitoring was performed routinely. After exposure of the posterior elements of the spine, removal of the inferior facet joints to be fused (in all cases) and Ponte osteotomy at the apical and juxta-apical segments with a rigid structural curve were performed. Pedicle screws were inserted bilaterally using a navigation system. In particular, a two-dimensional optical localizer (StealthStation Tria Plus Surgical Navigation; Medtronic, Minneapolis, MN, USA) and the Mach 4.0™ graphical user interface (Medtronic), which provides target-centric accuracy and color 3D guidance, were used with additional attachment of some lamina and transverse process hooks. All procedures were performed by the same surgical team.
Statistical analysis
Statistical analysis was performed using SPSS software (version 20.0; IBM Corp., Armonk, NY, USA). All values are expressed as mean ± standard deviation. Analyses of variance with a post hoc test (Mann–Whitney U test) and Student’s t test were used for comparisons. Normally distributed variables were compared using Student’s t test, and non-normally distributed variables were compared using the Mann–Whitney U test. For the variables sex and age, the numbers and percentages were compared between groups using Student’s t test. The relationships between the CL, TK, and other parameters were analyzed using Spearman’s product-moment correlation coefficients. For all statistical analyses, type 1 error was set at 5 % and p < 0.05 was considered significant.
Results
First study: comparative study of the sagittal alignment in the control and the AIS patients with main thoracic curve
A total of 66 patients (42 AIS patients and 24 normal controls) were enrolled in study 1. The measurements obtained from the radiological assessments are reported in Table 1A. Preoperatively, the average and standard deviations for sagittal parameters in the AIS group were −8.9 ± 16.1 for CL, 11.4 ± 9.4 for T1 slope, 13.4 ± 9.4 for TK, 46.9 ± 9.6 for LL, 37.8 ± 7.3 for SS, and −7.4 ± 28.0 for C7PL. The values in the Control group were 2.5 ± 15.0 for CL, 17.8 ± 7.9 for T1 slope, 21.3 ± 7.6 for TK, 40.9 ± 11.8 for LL, 28.5 ± 8.3 for SS, and 2.8 ± 36.9 for C7PL. The differences in LL and C7PL between the two groups were not significant (p = 0.066 and p = 0.252, respectively). The differences in CL, T1 slope, TK, and SS between groups were significant (p < 0.05).
The distribution of the four subtypes groups according to the Yu classification [14] revealed that the incidence of cervical kyphosis was 59.5 % (25/42) in the AIS group and 41.7 % (10/24) in the Control group. Interestingly, significant differences in the incidence of CL were found between the curve types of the two groups (14.3 vs. 41.7 %) Table 1B).
We next investigated the correlations between the CL and other parameters in both groups. The results of the Spearman correlation analysis of CL are summarized in Table 2A. Significant correlations were found between the CL and the T1 slope (r = 0.634), C7PL (r = 0.684), and TK (r = 0.311) in the AIS group, and between the CL and the T1 slope (r = 0.681) and C7PL (r = 0.451) in the Control group. No correlation was observed between the CL and TK in the Control group. TK correlated with the CL (r = 0.311) and T1 slope (r = 0.646) in the AIS group. However, TK did not correlate significantly with any parameters in the Control group (Table 2B). This result suggested that the TK was related to the CL in the AIS patients and that the TK seemed to be causally related to cervical kyphosis in these patients.
Second study: quantification of the changes in sagittal alignment following posterior spinal fusion in AIS patients
The characteristics of the 38 patients are presented in Table 3A. The mean number of fused motion segments was 10.6 ± 1.0 (range 8–12). The incidence of cervical kyphosis was 52.6 %. The average operative time was 291 ± 62 min. Intraoperative complications were not reported. In particular, no significant change in the monitored somatosensory/motor-evoked potentials was recorded during correction surgery. Early infections (within 45 days after the operation) were found in 4 of the 38 patients (10.3 %) after a mean infection-free interval of 29.3 days (±6.2); no late surgical site infections occurred after the surgery.
Table 3B summarizes the mean pre- and postoperative radiological values for the 38 AIS patients. Cervical lordosis was considered as positive and cervical kyphosis as negative. Thoracic kyphosis was considered as positive and thoracic lordosis as negative. The mean preoperative coronal Cobb angle was 49.0° in the MT group, and the last follow-up postoperative coronal Cobb angle was significantly reduced to 15.8° (p < 0.001), which corresponded to an average correction of 67.2 ± 12.6 %. The mean CL improved significantly from 7.2° kyphosis preoperatively to 0.1° kyphosis postoperatively (p < 0.05) (Fig. 2).
The mean TK increased significantly from 13.7° preoperatively to 19.3° postoperatively (p < 0.001). However, the LL (46.5° to 45.0°, p = 0.404) and C7PL (−5.0 mm to −5.3 mm, p = 0.967) did not change between the pre- and postoperative evaluations. Interestingly, the Spearman correlation analysis showed that the postoperative CL correlated significantly with the postoperative TK (r = 0.607), postoperative T1 slope (r = 0.761), and postoperative C7PL (r = 0.373) (Table 4).
Discussion
Several studies have already explored the spinopelvic sagittal alignment in patients with AIS. The findings of the current study confirmed the results of previous studies [7, 15]. Recently, Pesenti et al. analyzed 29 AIS patients with <20° preoperative hypothoracic kyphosis in a retrospective study. They reported T1 slope was increased after correction surgery and is a good indicator of postoperative changes for regional (cervical lordosis and thoracic kyphosis) and global sagittal parameters [16]. However, few studies have evaluated the sagittal alignment of the spine and pelvis in these patients according to their coronal curve type [6, 17]. Thus, we focused on the sagittal alignment in AIS patients affected by idiopathic thoracic scoliosis (Lenke type 1) before and after a posterior surgery.
The TK in this study was smaller than that of the normal population. We evaluated the relationships between various sagittal parameters and found that reduction of the CL was proportional to the reduction of TK in AIS patients. We also found that thoracic hypokyphosis and cervical kyphosis, which are observed in AIS, improved after the correction surgery.
Abnormal spinopelvic balance and pelvic morphology with flattened sagittal contours are common in AIS patients [4]. Most studies of the LL and TK have failed to include the cervical column in their analysis, but some authors have reported an associated loss of the CL [7, 18]. The changes in cervical alignment are compensatory mechanisms that occur in response to the abnormal thoracic alignment to allow maintenance of vision parallel to the horizontal [6]. These preoperative observations are consistent with radiographic measurements obtained by Hilibrand et al. [7]. The TK appears to be smaller in patients with thoracic AIS compared with age-matched controls [11]. Upsani et al. have reported that the preoperative TK of patients with AIS was smaller than that in nonscoliotic controls (18.9 ± 11.5 vs. 27.9 ± 7.9). The reason may be that the TK may be smaller when seen from a true lateral view at the apex because of vertebral rotation and wedging in patients with a main thoracic curve. We also studied TK from T5–T12 in this study because this corresponds to the region of the typical main thoracic curve and is most reliably assessed on lateral radiographs. We found a smaller TK compared with that in the normal control population (13.4 ± 9.4 vs. 21.3 ± 7.6, respectively; p < 0.001), whereas the LL did not differ significantly between groups (46.9 ± 9.6 vs. 40.9 ± 11.8, respectively).
Some of the goals of AIS surgery are to restore optimal coronal and sagittal alignment, and to reduce the incidence of adjacent segment degeneration and junctional malalignment. The relationships between postoperative thoracic, lumbar, and pelvic sagittal parameters have been characterized extensively, and most studies have reported difficulty in correcting both scoliosis in the frontal plane and thoracic hypokyphosis with hooks or all-pedicle screw constructs.
In this study, hybrid constructs used in the treatment of AIS patients had a powerful hypokyphotic effect on the thoracic spine. A reduction in TK may predispose to cervical spine decompensation into a kyphotic alignment. The surgical treatment of AIS patients with a main thoracic curve using all-pedicle screw constructs has a significant hypokyphotic effect on the thoracic sagittal plane alignment. If postoperative TK is decreased excessively, the cervical spine may decompensate into significant kyphosis. In this study, we found that the CL (C2–C7) and TK (T5–T12) were significantly increased after the correction surgery. This increase in thoracic alignment was associated with a significant decrease in cervical kyphosis in the postoperative period.
Hwang et al. evaluated the relationship between postoperative thoracic kyphosis and sagittal cervical alignment in patients with AIS treated with all-pedicle screw constructs [19]. They reported that the sagittal profile of the thoracic spine is related to that of the cervical spine. Some studies have also shown that the use of pedicle screw constructs and the number of implanted screws correlate significantly with hypokyphosis of the thoracic spine. Thus, there are reports that decreased TK is associated with decreased CL. However, other authors have reported that corrective surgery can significantly modify the sagittal alignment of the cervical spine, but this effect can vary depending on the underlying configuration of the preoperative sagittal thoracic spine [6]. Certainly, our results may not be observed consistently in all AIS patients because sagittal alignment can differ between AIS patients with different curve severity and because there are multiple types of scoliosis, each caused by a variety of different factors. The cause of AIS is unknown, and it is generally considered to be multifactorial in origin and to have separate factors for curve initiation and progression [20, 21]. Therefore, it is unclear in this study why the same surgical maneuvers used in AIS patients produced different corrective effects in the sagittal alignment depending on whether the thoracic spine was hypo- or normokyphotic, but we hypothesize that the coupled motions produced by these maneuvers may be responsible.
This study has several limitations. An important limitation of the study was the use of standard whole-spine posteroanterior and lateral full-spine radiographs, which are suboptimal as a measure of rotational deformity. It is possible that a three-dimensional assessment of lordosis and kyphosis at the cervical and thoracic spine would have altered our categorization of some curves. Second, this was a retrospective study and lacked longer term follow-up with clinical correlates. No previous reports of the long-term surgical outcomes (radiographic correction, pain, and patient satisfaction) are available. In particular, the relationship between the cervical kyphosis and axial pain, which is controversial in the literature, should be explored further. Cochran et al. found that the incidence of neck pain in patients 5–12 years after fusion using Harrington rods was no greater than that in the normal population [4]. In contrast, Moskowitz et al. reported a high incidence of cervical complaints (57 %) at the long-term follow-up (20–32 years) [22]. Third, this study included only radiological data and no functional scores were used to evaluate the patient outcomes. Previously, Youn et al. reported that significant changes in cervical sagittal parameters occur after surgical correction, and they found T1 slope and C2-7 SVA were significant predictors of quality of life (QOL) in AIS patients [23]. However, the relationships established between sagittal parameters and QOL in AIS are lacking. Therefore, future prospective studies should investigate the clinical correlates of neck pain, especially QOL, and their association with sagittal alignment to confirm the effects of cervical kyphosis on clinical outcomes. This information is needed to determine the real benefits of correction surgery to AIS patients. Fourth, we could not examine pelvic parameters such as pelvic tilt and pelvic incidence because of concerns about radiation of the gonads induced by diagnostic X-rays in AIS patients and normal controls. Thus, future research is needed to examine the relationships between cervical spine alignment and pelvic parameters. Fifth, the 42 AIS patients chosen in this study were classified as Lenke type 1. Other scoliotic deformity types were not assessed, and reproducibility of cervical lordosis might be lower on Lenke type 2–4, as the proximal curve induces more rotated vertebral bodies. Finally, the small sample size in our study may have marginalized the relationships between factors, which should be reevaluated in a larger series.
Conclusions
In summary, we focused only on the radiographic findings of the sagittal alignment, including the cervical spine, in AIS patients with a main thoracic curve. The sagittal alignment of the AIS patients with a main thoracic curve was less lordotic and/or more kyphotic than in the normal age-matched population. The coronal scoliotic deformity affects the sagittal contours of the spine by flattening thoracic kyphosis, which has effects on cervical sagittal alignment in AIS patients. The findings of this study suggest that cervical spine alignment is likely a component of the global sagittal alignment, which is strongly affected by TK.
References
Negrini S, Aulisa AG, Aulisa L, Circo AB, de Mauroy JC, Durmala J, Grivas TB, Knott P, Kotwicki T, Maruyama T, Minozzi S, O’Brien JP, Papadopoulos D, Rigo M, Rivard CH, Romano M, Wynne JH, Villagrasa M, Weiss HR, Zaina F (2012) 2011 SOSORT guidelines: orthopaedic and Rehabilitation treatment of idiopathic scoliosis during growth. Scoliosis 7:3. doi:10.1186/1748-7161-7-3
Illes T, Somoskeoy S (2010) Re: Sangole AP, Aubin CE, Labelle H, et al. Three-dimensional classification of thoracic scoliotic curves. Spine 2009;34:91–9. Spine 35:465. doi:10.1097/BRS.0b013e3181cc39b3 (author reply 465–466)
Schwab F, Lafage V, Patel A, Farcy JP (2009) Sagittal plane considerations and the pelvis in the adult patient. Spine 34:1828–1833. doi:10.1097/BRS.0b013e3181a13c08
Cochran T, Irstam L, Nachemson A (1983) Long-term anatomic and functional changes in patients with adolescent idiopathic scoliosis treated by Harrington rod fusion. Spine 8:576–584
Ofiram E, Garvey TA, Schwender JD, Wroblewski JM, Winter RB (2009) Cervical degenerative changes in idiopathic scoliosis patients who underwent long fusion to the sacrum as adults: incidence, severity, and evolution. J Orthop Traumatol Off J Ital Soc Orthop Traumatol 10:27–30. doi:10.1007/s10195-008-0044-0
Roussouly P, Labelle H, Rouissi J, Bodin A (2013) Pre- and post-operative sagittal balance in idiopathic scoliosis: a comparison over the ages of two cohorts of 132 adolescents and 52 adults. Eur Spine J 22(Suppl 2):S203–S215. doi:10.1007/s00586-012-2571-x
Hilibrand AS, Tannenbaum DA, Graziano GP, Loder RT, Hensinger RN (1995) The sagittal alignment of the cervical spine in adolescent idiopathic scoliosis. J Pediatr Orthop 15:627–632
Canavese F, Turcot K, De Rosa V, de Coulon G, Kaelin A (2011) Cervical spine sagittal alignment variations following posterior spinal fusion and instrumentation for adolescent idiopathic scoliosis. Eur Spine J 20:1141–1148. doi:10.1007/s00586-011-1837-z
Hu P, Yu M, Liu X, Zhu B, Liu X, Liu Z (2015) Analysis of the relationship between coronal and sagittal deformities in adolescent idiopathic scoliosis. Eur Spine J. doi:10.1007/s00586-015-3986-y
Clement JL, Geoffray A, Yagoubi F, Chau E, Solla F, Oborocianu I, Rampal V (2013) Relationship between thoracic hypokyphosis, lumbar lordosis and sagittal pelvic parameters in adolescent idiopathic scoliosis. European Spine J 22:2414–2420. doi:10.1007/s00586-013-2852-z
Upasani VV, Tis J, Bastrom T, Pawelek J, Marks M, Lonner B, Crawford A, Newton PO (2007) Analysis of sagittal alignment in thoracic and thoracolumbar curves in adolescent idiopathic scoliosis: how do these two curve types differ? Spine 32:1355–1359. doi:10.1097/BRS.0b013e318059321d
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 83-A:1169–1181
O’Brien MF KT, Blanke KM, Lenke LG (2008) Radiographic measurement manual. Spinal Deformity Study Group
Yu M, Silvestre C, Mouton T, Rachkidi R, Zeng L, Roussouly P (2013) Analysis of the cervical spine sagittal alignment in young idiopathic scoliosis: a morphological classification of 120 cases. Eur Spine J 22:2372–2381. doi:10.1007/s00586-013-2753-1
Pasha S, Aubin CE, Sangole AP, Labelle H, Parent S, Mac-Thiong JM (2014) Three-dimensional spinopelvic relative alignment in adolescent idiopathic scoliosis. Spine 39:564–570. doi:10.1097/brs.0000000000000193
Pesenti S, Blondel B, Peltier E, Choufani E, Bollini G, Jouve JL (2016) Interest of T1 parameters for sagittal alignment evaluation of adolescent idiopathic scoliosis patients. Eur Spine J 25:424–429. doi:10.1007/s00586-015-4244-z
Mac-Thiong JM, Labelle H, Charlebois M, Huot MP, de Guise JA (2003) Sagittal plane analysis of the spine and pelvis in adolescent idiopathic scoliosis according to the coronal curve type. Spine 28:1404–1409. doi:10.1097/01.brs.0000067118.60199.d1
Ilharreborde B, Vidal C, Skalli W, Mazda K (2013) Sagittal alignment of the cervical spine in adolescent idiopathic scoliosis treated by posteromedial translation. Eur Spine J 22:330–337. doi:10.1007/s00586-012-2493-7
Hwang SW, Samdani AF, Wormser B, Amin H, Kimball JS, Ames RJ, Rothkrug AS, Cahill PJ (2012) Comparison of 5-year outcomes between pedicle screw and hybrid constructs in adolescent idiopathic scoliosis. J Neurosurg Spine 17:212–219. doi:10.3171/2012.6.spine1215
Kouwenhoven JW, Castelein RM (2008) The pathogenesis of adolescent idiopathic scoliosis: review of the literature. Spine 33:2898–2908. doi:10.1097/BRS.0b013e3181891751
Wang WJ, Yeung HY, Chu WC, Tang NL, Lee KM, Qiu Y, Burwell RG, Cheng JC (2011) Top theories for the etiopathogenesis of adolescent idiopathic scoliosis. J Pediatr Orthop 31:S14–S27. doi:10.1097/BPO.0b013e3181f73c12
Moskowitz A, Moe JH, Winter RB, Binner H (1980) Long-term follow-up of scoliosis fusion. J Bone Joint Surg Am 62:364–376
Youn MS, Shin JK, Goh TS, Kang SS, Jeon WK, Lee JS (2016) Relationship between cervical sagittal alignment and health-related quality of life in adolescent idiopathic scoliosis. Eur Spine J. doi:10.1007/s00586-016-4488-2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflict of interest directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Hiyama, A., Sakai, D., Watanabe, M. et al. Sagittal alignment of the cervical spine in adolescent idiopathic scoliosis: a comparative study of 42 adolescents with idiopathic scoliosis and 24 normal adolescents. Eur Spine J 25, 3226–3233 (2016). https://doi.org/10.1007/s00586-016-4701-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4701-3