Abstract
Purpose
Meta-analysis was conducted to estimate whether MiTLIF could reduce the complication rate while maintaining the similar clinical result to that of open procedures.
Methods
A search of the literature was conducted on pubmed or EMBASE. A database including patient clinical information was created. A systematic review of eligible studies with multivariate regression analysis was performed to quantitatively review the correlation of VAS improvement rate and the performance of MiTLIF.
Results
Fourteen articles with a minimum of 12-month follow-up met our inclusion criteria. The hypothesis of homogeneity could be accepted. The fixed-effects model was used to calculate the summary risk ratio (odds ratio). In the pooled analysis, the summary risk ratio (odds ratio) in patients with MiTLIF against those with open procedure for fusion rate, complication rate and revision/readmission rate was 0.99 (p = 0.36), 1.15 (p = 0.5) and 2.59 (p = 0.003), respectively, suggesting that MiTLIF was a risk factor for revision/readmission. Multivariate regression analysis showed that the percentage of male patients and the length of surgery exert a significant impact on VAS improvement rate. The selection of MiTLF was not significant.
Conclusion
Fusion rate and complication rate for both open and MiTLIF were similar. Moreover, the MiTLIF group tended to have a higher revision/readmission rate, which might be associated with the deep learning curve. Therefore, to achieve the level of surgical skill required of an MiTLIF surgeon, many years of training and experience are necessary. Otherwise, MiTLIF may yield unsatisfactory result upon patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Posterior lumbar interbody fusion (PLIF) and transforaminal lumbar interbody fusion (TLIF) are commonly utilized to treat lumbar degenerative disease, spondylolisthesis and other diseases that need stabilization. TLIF has gained more popularity because of the innovative surgical concepts. In TLIF, decompression and cage placement are performed through a unilateral approach, which provides exposure of the disc space while minimizing the retraction of dural sac and nerve root. However, extensive dissection of muscles on the back in the open procedures results in more trauma with the disadvantages including the postoperative pain, massive blood loss, lengthier hospitalization and lower quality of life, which have aroused more attention [1]. Therefore, the avoidance of excessive muscle retraction and stripping in the posterior open approaches can contribute to good postoperative back muscle functions.
A minimally invasive transforaminal lumbar interbody fusion surgery (MiTLIF) using percutaneous posterior fixation (approved by FDA of USA) of the lumbar spine has been described to reduce the iatrogenic soft tissue injury that occurs with retraction of paraspinal muscles during conventional spinal exposure [2–4]. Several studies have tried to investigate the difference between MiTLIF and traditional open approaches on complication rate and the clinical result, fusion rate and revision/readmission rate (due to serious complication) in treating lumbar diseases, but no consensus on this has been reached, and different studies have yielded conflicting results [3, 5–17]. But whether differences in the literature have been mostly due to the limitation of sample size or genuine heterogeneity is unknown.
In this study, we sought to conduct a systematic review and meta-analysis from published studies to estimate whether MiTLIF could reduce the complication rate and revision rate while maintaining fusion rate and clinical results similar to or even better than that of open procedures.
Patients and methods
Search strategy
The primary sources of the reviewed studies were PubMed and Embase. The search included literature exclusively in English published through Nov 4, 2014 with no lower date limit on the search results. Searches included the terms “lumbar fusion”, “minimally invasive”, “mini-open”, “percutaneously” and “percutaneous pedicle screw” to explore all the possible relevant articles. The computer search was reinforced with manual searches for reference lists of all retrieved articles. In studies where there were overlapping patients, of which criteria included study period, hospital and treatment information, we retained only the largest one to avoid duplication of information.
Eligibility of relevant trials
Studies that met the following criteria were eligible for inclusion in this meta-analysis: (1) studies comparing the clinical result or complication rate or fusion rate that was confirmed by radiograph or computed tomography scan between the MiTLIF and open procedures; (2) cases were medically confirmed of lumbar disease that needs surgical intervention; (3) studies reported outcome measures with visual analog scale (VAS); (4) a follow-up time exceeded 1 year. Studies that met the following criteria were excluded: studies only reported MiTLIF or open surgery without control group; studies reported anterior lumbar interbody fusion (ALIF) or extreme lateral interbody fusion (XLIF) or other types of minimally invasive surgery (MIS) which were totally different from PLIF/TLIF. All the potentially relevant papers were reviewed and extracted independently by two investigators (Q. JT. and T. Y) and disagreements were resolved by discussion until consensus was finally reached.
Data extraction
Abstracts of all articles were read by two independent reviewers (Q. JT. and T. Y). Articles that could not be excluded from our study based on title and abstract alone were retrieved for full-text review independently by the same two reviewers. The required information extracted from all primary studies included: (1) demographic data in each study, (2) follow-up time, (3) complication rate, (4) revision rate/readmission rate (as serious complication such as serious surgical site infection, intraoperative durotomy, incisional cerebrospinal fluid leak and hardware failure that needs unscheduled surgery or readmission), (5) length of hospital stay, (6) intraoperative blood loss, (7) variables including number of patients analyzed, the operative time, source of the patients (developed area or not) and fusion rate.
Quality assessment
We assessed the methodological quality of included studies based on Newcastle–Ottawa Scale (NOS) for quality of case–control and cohort studies [18]. A star system of the NOS (range 0–9 stars) has been developed for the evaluation. The highest value for quality assessment was nine stars (Table 1).
Statistical analysis
If fusion rate, complication rate and revision rate of patients were found to have fine homogeneity, a fixed-effect model was used for analysis. If not, a random-effect model was used. Review Manager 5.2 (Version 5 for Windows, Cochrane Collaboration, Oxford, UK) and SAS 8.0 were used for statistical analysis to estimate the pooled RR or OR of fusion rate, complication rate and revision/readmission rate associated with MiTLIF against open surgery. For the quantitative combination of the effect value, fusion rate and their 95 % confidence intervals (CIs) were aggregated. VAS improvement rate of each study as one of the clinical outcomes was calculated as follows: (preoperative average VAS score−postoperative average VAS score)/(preoperative average VAS score) × 100 %. The final VAS score was obtained by calculating the average of VAS of back pain and leg pain, if both available in a study. When VAS score failed to provide the aggregated value using meta-analysis based on the improvement rate, statistics were reinforced by multivariate regression analyses of the collected variables, which were suspected to cause inconsistency in all researches, to examine the association between variables of each study and the VAS improvement rate. Publication bias was assessed using the STATA procedure of “Metabias”, which was based on two different approaches, Begg’s and Egger’s tests.
Result
Identification of relevant studies
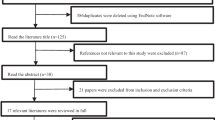
A total of 357 articles were identified. We excluded 343 articles that did not meet the selection criteria. Figure 1 shows a flow diagram of the selection process for relevant studies, and 14 studies were finally considered to be eligible for inclusion in our analysis [3, 5–17].
Characteristics of studies
Characteristics of the 14 studies with long enough follow-up are presented in Table 2. All the demographic information, intraoperative and postoperative parameters were listed. The overall quality of the included studies was adequate. The mean value was 7.8 out of 9 stars (Table 1).
Overall association of MiTLIF conditions with the risk of fusion, complication and revision/readmission
An assessment of heterogeneity of 14 studies included for the meta-analysis was performed in terms of fusion rate, complication rate and revision/readmission rate. The hypothesis of homogeneity could be accepted (p ≥ 0.7, Figs. 2, 3, 4) which indicated few confounding factors in the meta-analysis. And the fixed-effects model was used to calculate the summary risk ratio (odds ratio). In the pooled analysis (Figs. 2, 3, 4), the summary risk ratio associated with MiTLIF in comparison with open surgery in fusion rate, complication rate and revision/readmission rate was 0.99 (95 % CI 0.97–1.01, p = 0.36), 1.15 (95 % CI 0.76–1.74, p = 0.5), and 2.59 (95 % CI 1.37–4.90, p = 0.003), respectively, suggesting that MiTLIF was a risk factor for revision/readmission. Sensitivity analysis showed that the pooled result after excluding either of the study did not change substantially (data not shown).
Forest plots of included studies reporting comparative fusion rate were shown on the right. The summary risk ratio for fusion rate comparison between patients with MiTLIF versus patients with open procedure was generated on the fourth column. The “event” meant the number of patients who had successful fusion at the last follow-up
Forest plots of included studies reporting comparative complication rate were shown on the right. The summary odds ratio for complication rate comparison between patients with MiTLIF versus patients with open procedure was generated on the fourth column. The “event” meant the number of patients who had complication during the follow-up
Forest plots of included studies reporting comparative revision/readmission rate were shown on the right. The summary odds ratio for revision/readmission rate comparison between patients with MiTLIF versus patients with open procedure was generated on the fourth column. The “event” meant the number of patients who had revision/readmission during the follow-up
Multivariate regression analysis was used to identify the potential sources of heterogeneity among these studies and the result of the analysis is shown in Table 3. After stepwise selection, the percentage of male patients and the length of surgery were shown to exert a significant impact on the VAS improvement rate. The selection of MIS was not significant.
Publication bias
Publication bias analysis indicated no publication bias among these studies regarding risk ratio of fusion rate (Begg’s p = 0.881, Egger’s p = 0.712). Odds ratio of complication rate (Begg’s p = 0.652, Egger’s p = 0.753) and revision/readmission rate (Begg’s p = 0.602, Egger’s p = 0.545) also showed no publication bias. The funnel plot was largely symmetric (not shown). These results suggest a possibility that publication bias may not have played a role in the observed effect, which implies that the results here are largely reliable.
Discussion
Meta-analysis was conducted to estimate whether MiTLIF could reduce the complication rate while maintaining the similar clinical result to that of open procedures. In our paper, the aggregated fusion rate and complication rate for both open and MiTLIF were similar. But the MiTLIF group tended to have a higher revision/readmission rate.
The goal of the MiTLIF approach is to reduce blood loss, decrease postoperative pain, shorten the length of stay (LOS) and improve appearance. And it indeed has reached it in the short term as we can see from Table 2. TLIF and other posterior procedures can lead to the denervation and atrophy of muscles, which results in a higher risk of “fusion disease”, a term used for patients having a successful fusion radiographically but with a poor clinical outcome [19, 20], and the incidence of the fusion disease is not low [21]. So efforts have been made to develop better treatments to reduce these adverse effects without compromising the clinical outcome.
Theoretically, trauma of paraspinal soft tissue in the open posterior procedures has an adverse effect on adjacent segments and reduces the blood supply for fusion. So complications such as adjacent segment degeneration, infection and pseudoarthrosis may occur [22]. But in our study, fusion rate and complication rate showed no significant difference between open procedures and MiTLIF. Furthermore, we found a significantly higher aggregated revision/readmission rate in patients who underwent MiTLIF, of which the pooled odds ratio of the occurrence of revision/readmission in the “MiTLIF” group against the “OPEN” group was 2.59, which suggests a 2.59-fold increased risk for patients who underwent MiTLIF to have serious complications that need reoperation or readmission for treatment.
“Pain” is the most common complaint of patients with lumbar disease, which can seriously affect the quality of life [3]. The iatrogenic muscle injury from traditional open procedures can cause long-term problems that can negate the beneficial effects of the surgery itself. So we took the “VAS improvement rate” as an indicator of clinical outcome. Eleven studies were considered in the multivariate regression analysis [6–9, 11–17], the result of which showed that the lower percentage of male patients and the shorter length of surgery are protective factors on the VAS improvement rate; however, to our surprise, the selection of MiTLIF meant little in the clinical outcome, only a trend towards protective factor in clinical result investigation. The multivariate analysis, to some extent, reduced the information bias of this meta-analysis by combining all the relative studies that contained the eight variables listed in Table 3. We could also learn from Table 3 that the female patients had relatively high VAS improvement rate, which might be explained by the fact that male patients had higher muscle mass leading to more damage to the paraspinal muscles due to stronger retraction and more extensive stripping.
But patients undergoing MIS tended to lose less blood and leave the hospital sooner than their open counterparts, which was verified in this study and in a systemic review by Goldstein [23]. All the included studies presented consistent conclusion.
But in the long term (≥1 year), why does not MiTLIF show its theoretically considerable advantage in this meta-analysis? We think that it is the substantial learning curve that only a proficient surgeon can make MiTLIF give its full play in posterior lumbar fusion. Dissecting, disc space preparation and grafting using tubular retractors are more difficult in MiTLIF than in traditional open procedures, especially for the patients with spondylolisthesis, who are a more challenging group for surgery [24]. So a good and long enough training must be undertaken to make a qualified MiTLIF surgeon who can operate excellently in such a limited working area in MIS. For a particular surgeon, the interacting progressive experience with the open technique may positively influence the learning effect of the percutaneous lumbar fusion technique. So a senior surgeon already skillful at open techniques is recommended to carry out this operation to give full play to the MiTLIF potential. This point was proved in our study that shorter length of surgery could promote VAS improvement rate. Moreover, from Table 2, studies by Zairi et al. [14] and Lee et al. [16], in which the length of surgery in MiTLIF was shorter than in OPEN procedures, showed lower complication rate and higher VAS improvement rate. We commonly know that the length of surgery can be an indicator reflecting the proficiency plateau a surgeon reaches in performing a specific operation. So there is a suggestion that the training to perform the MIS can be enough as long as one can perform the MiTLIF as fast as he can perform the open procedure. And only with this can we maximize the benefit of the MIS and minimize its adverse effect. Another explanation about the length of surgery may be that longer surgeries represent more difficult cases which automatically result in a higher complication rate. But we do not think it is the main cause since there cannot be all difficult cases concentrated in a single hospital which may lead to an increased average length of surgery.
In Wu et al.’s [25] meta-analysis of fusion rate of MiTLIF and open TLIF, they reported similar fusion rates and complication rates with a trend that favored MiTLIF. But articles that did not have a control group were also included in their research, which might cause information bias and made their conclusion less persuasive. Furthermore, clinical outcome was measured using the method aforementioned in our research, which helped us know more about the influencing factors about the clinical outcome.
However, there is a limitation that the sample size might be not large enough to find the possible existing evidence that MiTLIF was superior to open procedures. Till now, the significance of MiTLIF remains unknown based on the limited data available. But the higher aggregated serious complication rate in MiTLIF has raised our awareness of the level of surgical skill required of an MiTLIF surgeon. At last, we still think the future of MIS technique is bright, but to maximize the benefits of MIS technique, many years of training and experience are indispensable. Otherwise, MIS technique may yield unsatisfactory result upon patients.
References
Kalanithi PS, Patil CG, Boakye M (2009) National complication rates and disposition after posterior lumbar fusion for acquired spondylolisthesis. Spine (Phila Pa 1976) 34(18):1963–1969
Tsutsumimoto T, Shimogata M, Ohta H, Misawa H (2009) Mini-open versus conventional open posterior lumbar interbody fusion for the treatment of lumbar degenerative spondylolisthesis: comparison of paraspinal muscle damage and slip reduction. Spine (Phila Pa 1976) 34(18):1923–1928
Rodriguez-Vela J, Lobo-Escolar A, Joven E, Munoz-Marin J, Herrera A, Velilla J (2013) Clinical outcomes of minimally invasive versus open approach for one-level transforaminal lumbar interbody fusion at the 3- to 4-year follow-up. Eur Spine J 22(12):2857–2863
Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ (2011) Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech 24(8):479–484
Schizas C, Tzinieris N, Tsiridis E, Kosmopoulos V (2009) Minimally invasive versus open transforaminal lumbar interbody fusion: evaluating initial experience. Int Orthop 33(6):1683–1688
Peng CW, Yue WM, Poh SY, Yeo W, Tan SB (2009) Clinical and radiological outcomes of minimally invasive versus open transforaminal lumbar interbody fusion. Spine (Phila Pa 1976) 34(13):1385–1389
Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, Liu J (2010) Comparison of one-level minimally invasive and open transforaminal lumbar interbody fusion in degenerative and isthmic spondylolisthesis grades 1 and 2. Eur Spine J 19(10):1780–1784
Shunwu F, Xing Z, Fengdong Z, Xiangqian F (2010) Minimally invasive transforaminal lumbar interbody fusion for the treatment of degenerative lumbar diseases. Spine (Phila Pa 1976) 35(17):1615–1620
Adogwa O, Parker SL, Bydon A, Cheng J, McGirt MJ (2011) Comparative effectiveness of minimally invasive versus open transforaminal lumbar interbody fusion: 2-year assessment of narcotic use, return to work, disability, and quality of life. J Spinal Disord Tech
Lau D, Lee JG, Han SJ, Lu DC, Chou D (2011) Complications and perioperative factors associated with learning the technique of minimally invasive transforaminal lumbar interbody fusion (TLIF). J Clin Neurosci 18(5):624–627
Park Y, Ha JW (2007) Comparison of one-level posterior lumbar interbody fusion performed with a minimally invasive approach or a traditional open approach. Spine (Phila Pa 1976) 32(5):537–543
Kotani Y, Abumi K, Ito M, Sudo H, Abe Y, Minami A (2011) Mid-term clinical results of minimally invasive decompression and posterolateral fusion with percutaneous pedicle screws versus conventional approach for degenerative spondylolisthesis with spinal stenosis. Eur Spine J
Kim DY, Lee SH, Chung SK, Lee HY (2005) Comparison of multifidus muscle atrophy and trunk extension muscle strength: percutaneous versus open pedicle screw fixation. Spine (Phila Pa 1976) 30(1):123–129
Zairi F, Arikat A, Allaoui M, Assaker R (2013) Transforaminal lumbar interbody fusion: comparison between open and mini-open approaches with two years follow-up. J Neurol Surg A Cent Eur Neurosurg 74(3):131–135
Harris EB, Sayadipour A, Massey P, Duplantier NL, Anderson DG (2011) Mini-open versus open decompression and fusion for lumbar degenerative spondylolisthesis with stenosis. Am J Orthop (Belle Mead NJ) 40(12):E257–E261
Lee KH, Yue WM, Yeo W, Soeharno H, Tan SB (2012) Clinical and radiological outcomes of open versus minimally invasive transforaminal lumbar interbody fusion. Eur Spine J 21(11):2265–2270
Villavicencio AT, Burneikiene S, Roeca CM, Nelson EL, Mason A (2010) Minimally invasive versus open transforaminal lumbar interbody fusion. Surg Neurol Int 1(12)
Stang A (2010) Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605
Zdeblick TA (1998) Laparoscopic spinal fusion. Orthop Clin North Am 29(4):635–645
Sihvonen T, Herno A, Paljarvi L, Airaksinen O, Partanen J, Tapaninaho A (1993) Local denervation atrophy of paraspinal muscles in postoperative failed back syndrome. Spine (Phila Pa 1976) 18(5):575–581
McKinstry CS, Bell KE (1990) The failed back syndrome: the diagnostic contribution of computed tomography. Ulster Med J 59(2):122–130
Harrop JS, Youssef JA, Maltenfort M, Vorwald P et al (2008) Lumbar adjacent segment degeneration and disease after arthrodesis and total disc arthroplasty. Spine (Phila Pa 1976) 33(15):1701–1707
Goldstein CL, Macwan K, Sundararajan K, Rampersaud YR (2014) Comparative outcomes of minimally invasive surgery for posterior lumbar fusion: a systematic review. Clin Orthop Relat Res 472(6):1727–1737
Kim SS, Denis F, Lonstein JE, Winter RB (1990) Factors affecting fusion rate in adult spondylolisthesis. Spine (Phila Pa 1976) 15(9):979–984
Wu RH, Fraser JF, Hartl R (2010) Minimal access versus open transforaminal lumbar interbody fusion: meta-analysis of fusion rates. Spine (Phila Pa 1976) 35(26):2273–2281
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Q. Jin-tao and T. Yu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Jin-tao, Q., Yu, T., Mei, W. et al. Comparison of MIS vs. open PLIF/TLIF with regard to clinical improvement, fusion rate, and incidence of major complication: a meta-analysis. Eur Spine J 24, 1058–1065 (2015). https://doi.org/10.1007/s00586-015-3890-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-3890-5