Abstract
Chronic relapsing multifocal osteomyelitis (CRMO) is a rare condition. It commonly affects the clavicle and pelvis. Rarely it can affect the spine. Spinal deformity due to CRMO is rare. We report a case of acute scoliosis due to CRMO. A 10-year-old girl with CRMO presented with acute painful scoliosis of her spine. She was neurologically intact. Imaging suggested a neoplastic process involving T10, L2 and L3. Further imaging and subsequent biopsy was performed and a diagnosis of CRMO was established. Spinal involvement with deformity is uncommon. It is commonly misdiagnosed as infection or a neoplasm and unnecessary aggressive surgical and antibiotic therapy instituted. A high index of suspicion is needed to diagnose this disease and thus manage it appropriately. This patient with a previously normal spine had a long right sided thoracic scoliosis. We think that the particular pattern of scoliosis was a protective mechanism to offload the right sided T10 vertebral pedicle. Prognosis is generally good although the disease can relapse and remit over many years. At 9 months follow up, the lesions were resolving and the deformity had resolved. CRMO presenting as acute scoliosis is rare and to our knowledge this is the second recognised case in the reported world literature.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Chronic relapsing multifocal osteomyelitis (CRMO) was first described by Giedion in 1972 as “sub acute and chronic symmetrical osteomyelitis” [13]. Gamble and Rinsky [12] described it as CRMO.
It is a non-pyogenic inflammatory bone disease of unknown aetiology with an unpredictable course. It is characterised by exacerbations and spontaneous remissions [17]. It predominantly occurs during childhood and adolescence. The various etiological hypotheses postulated are: genetic [6], infectious, and autoimmunity [19].
The skeletal manifestations of CROM are most often seen in tubular bones, the clavicle, and less frequently the spine and pelvic bones [16]. It has been known to cause skeletal features of sclerosis, premature epiphyseal fusion, long bone deformity, growth arrest and progressive kyphosis [19]. CRMO presenting as acute onset scoliosis is a rare thing and only one such case has been reported before [30].
We present a case of a young girl presenting with acute onset scoliosis with mild backache. On investigation it turned out to be a case of CRMO involving multiple vertebrae.
Case report
A 10-year-old girl presented to the Accident and Emergency Department with complaint of sudden onset backache and stiffness over the last 2 weeks. Over the last 1 week her parents noticed progressive deformity of her back in the thoracic region. She did not have any history of trauma. Her sleep was not disturbed. Her appetite and weight were normal. There was no history of fever. She had not travelled abroad recently and neither did she have any other skeletal or joint complaints. She was systemically well. She was a full term normally delivered baby who had normal milestones. She did not suffer from any major medical problems apart from mild eczema, which was well controlled. She had no allergies. There was no family history of skeletal problems.
Examination showed normal vital signs. Respiratory, cardiovascular and abdominal examination was normal. Nervous system examination revealed normal higher functions, cranial nerves and cerebellar functions. She had full power and sensations in all her limbs and trunk. Reflexes were all present and normal.
Examination of her back and spine revealed a marked thoracic scoliosis with convexity to the right. There was mild bony midline tenderness over the T9 and T10 vertebrae. She had significantly restricted rotation and flexion/extension of her thoracic spine. Cervical and lumbosacral spine was clinically normal.
Full blood count, all inflammatory markers including CRP were normal (CRP 4). Blood cultures were negative for pyogenic organisms, mycobacteria and fungi.
X-ray of her spine revealed slight collapse of the body of T10 with a little sclerosis. There was a right convex scoliosis with the apex of the curve at the level of T10. The curve was 22° as measured by the Cobb angle method. Ultrasound examination of the abdomen and pelvis was normal.
Urgent MRI revealed abnormal marrow signal (low signal on T1, high on T2 and STIR) in T10, L2 and L3 vertebral bodies, with some compression of T10 body and extension into the right pedicle. The discs were of normal appearance. There was no intra-spinal or extra-osseous component. The spinal cord was normal. There was no para-aortic lymphadenopathy and liver, spleen and kidneys looked normal.
Isotope bone scan revealed increased uptake on the late films in C2, C3, T10, L2 and L3 vertebrae.
CT scan revealed lytic lesions of the right side of body and right pedicle of T10, bodies of L2 and L3.
CT guided trans-pedicular biopsy of T10 and X-ray guided trans-pedicular biopsy of her L2 vertebra provided tissue which did not grow any organism on culture. Histopathological examination revealed “loose textured fibrous tissue with a prominent plasma cell population” which was highly suggestive of CRMO. There was no evidence of neoplasia.
The patient was not started on any antibiotics as there were no obvious clinical signs suggestive of infection, inflammatory markers were normal and no organism could be cultures from blood or the biopsy material. She needed only minimal analgesics in the form of NSAIDs and paracetamol for pain relief. The patient is being monitored clinically and radiologically to detect any worsening of the scoliosis and potential cord compromise at the earliest. The lesions have not progressed and the patient is symptomatically improving at a follow up of 10 months. The scoliosis has improved uneventfully.
Discussion
CRMO is a rare entity. Its incidence is 2–5% of all osteomyelitis cases. It primarily affects young girls, with a female/male ratio of 5:1 [7]. The median age of onset is 10 years with a reported range of 4–14 years [15]. It affects all races equally [31]. There are still many unsolved questions about the aetiology. Infectious and autoimmune theories have been put forth, but none has been proven [19]. There have been suggestions of a genetic link, but no definite evidence exists for this [6].
CRMO has been associated with various other overlapping disease entities. Palmoplantar pustulosis has been described with CRMO [4, 11, 25, 31]. Psoriasis has also been described with CRMO [25]. CRMO is now considered as part of the synovitis, acne, palmoplantar pustulosis, hyperostosis, and osteitis (SAPHO) syndrome [27]. Diffuse sclerosing osteomyelitis of Garre may be a limited presentation of CRMO [29]. SAPHO syndrome and CRMO are considered types of seronegative spondyloarthropathies [3, 18, 19, 24, 28].
In contrast to haematogenous osteomyelitis, the onset of CRMO is rarely abrupt, high fever is unusual and the isolation of a responsible infectious agent is unsuccessful.
Various diagnostic criteria for CRMO have been suggested.
King et al. [19] suggest the following criteria:
-
Multifocal, i.e. two or more bony lesions: clinically or radiographically diagnosed.
-
A prolonged course over 6 months characterized by varying activity of disease and with most patients being healthy between recurrent episodes of pain, swelling and tenderness.
-
Lack of response to antimicrobial therapy given for at least 1 month.
Manson et al. [22] suggested the following diagnostic criteria:
-
Two radiographically confirmed bone lesions.
-
At least 6 months of remissions and exacerbations of signs and symptoms.
-
Radiographic and bone scan evidence of osteomyelitis.
-
Lack of response to antimicrobial therapy at least 1 month in duration.
-
Lack of an identifiable cause.
Essentially, it is a diagnosis of exclusion. The presentation, radiographic, and nuclear scintigraphic findings can mimic acute haematogenous osteomyelitis, neoplasia, eosinophilic granuloma, osteoblastoma, and osteoid osteoma. It is common to see a delay in diagnosis and appropriate treatment. Patients usually are treated with systemic antibiotics at initial presentation; however, cultures of bone are typically negative [19, 28].
Plain radiographs usually reveal non-specific features suggestive of osteomyelitis, such as osteolysis, sclerosis and new bone formation. X-ray changes are quite subtle initially and often missed [5, 9].
Radioisotope bone scans assist in establishing the diagnosis and in identifying initially silent lesions [21].
Magnetic resonance imaging scans are highly sensitive. They can provide data on the involvement of adjacent joints and soft tissue and are helpful in disease monitoring [10, 14, 17, 20, 23]. MRI appearance of CRMO lesions in tubular bones and the spine is often rather characteristic showing high signal on T2 and low signal on T1 images. With quiescence, T2 images show decreased intensity [16].
Biopsy is done mainly to exclude neoplasia. Histologically, early lesions show acute and chronic inflammatory infiltrate i.e. polymorphonuclear cells. Later lymphocytes and plasma cells predominate. Some multinucleated giant cells and non-caseating granulomata can also be seen. Older lesions reveal necrosis, fibrosis and new bone formation [19, 28].
There have been no controlled trials on this condition and all the treatments tried are empirical.
CRMO is characterised by its refractory nature despite treatment with extended regimens of anti-inflammatory and antibiotic medications. Hence prompt diagnosis of CRMO will allow patients to avoid the risks associated with lengthy courses of antibiotic therapy and repeat bone biopsies [7]. Intermittent treatment of acute relapses is as effective as long-term therapy [8]. Antimicrobial agents have been shown to be ineffective and indeed this has suggested to be used as a criterion for diagnosis [2, 12, 28]. Some studies have found oral corticosteroids beneficial [2, 19].
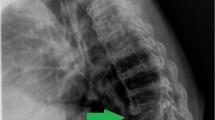
Bony complications include sclerosis, premature epiphyseal fusion, long bone deformity, growth arrest and progressive kyphosis [5, 19]. Spinal involvement has been reported from the mid-cervical spine to the sacrum. This occurs in the form of “migratory spondylitis” or “saltatory spondylitis” [26]. X-ray picture is predominantly of the chronic sclerosing type. Vertebral deformity due to compression and total collapse (vertebra plana) is rare [26]. Spondylodiscitis only develops as secondary destruction following the spondylitis, thus helping in differentiating from the spondyloarthropathies. Spinal cord compression is extremely rare and till date only one case of severe kyphosis, due to CRMO has been reported which needed anterior decompression and fusion [1]. Vertebra plana has been described as a complication of CRMO [32]. Scoliosis is commonly seen in female patients of the adolescent age group. In case of acute painful onset, the possibility of CRMO needs to be kept in mind. Our patient (who had a previous chest X-ray prior to this episode with no evidence of scoliosis; Fig. 1) had a long C-shaped thoracic scoliosis which was convex to the right. The apex of the curve was at T10 and the magnitude of the curve was 22° as measured by the Cobb angle method. We think that the particular pattern of scoliosis was a protective mechanism to offload the right sided T10 vertebral pedicle. Prognosis is generally good, most lesions healing with sclerosis, although the disease can relapse and remit over many years [2, 9, 12, 19] (Figs. 2–8).
CRMO is a diagnosis of exclusion. It needs appropriate treatment and support for the patient and his/her family. Spinal involvement is silent in many cases hence true incidence is unknown.
References
Baulot E, Bouillien D, Giroux EA, Grammont PM (1998) Chronic recurrent multifocal osteomyelitis causing spinal cord compression. Eur Spine J 7(4):340–343
Bjorksten B, Boquist L (1980) Histopathological aspects of chronic recurrent multifocal osteomyelitis. J Bone Joint Surg Br 62(3):376–380
Bjorksten B, Gustavson KH, Eriksson B, Lindholm A, Nordstrom S (1978) Chronic recurrent multifocal osteomyelitis and pustulosis palmoplantaris. J Pediatr 93(2):227–231
Brand CU, Yawalkar N, Ballmer-Weber B, Braathen LR (1996) Pustulosis palmoplantaris associated with chronic recurrent multifocal osteomyelitis of the mandible. Br J Dermatol 134:977–979
Brown T, Wilkinson RH (1988) Chronic recurrent multifocal osteomyelitis. Radiology 166(2):493–496
Byrd L, Grossmann M, Potter M, Shen-Ong GLC (1991) Chronic multifocal osteomyelitis, a new recessive mutation on chromosome 18 of the mouse. Genomics 11:794–798
Chun CS (2004) Chronic recurrent multifocal osteomyelitis of the spine and mandible: case report and review of the literature. Pediatrics 113(4):e380–e384
Coinde E, David L, Cottalorda J et al (2001) Chronic recurrent multifocal osteomyelitis in children: a report of 17 cases [in French]. Arch Pediatr 8:577–583
Cyrlak D, Pais MJ (1986) Chronic recurrent multifocal osteomyelitis. Skeletal Radiol 15(1):32–39
Dawson JS, Webb JK, Preston BJ (1994) Case report: chronic recurrent multifocal osteomyelitis with magnetic resonance imaging. Clin Radiol 49:133–136
Flygare L, Norderyd J, Kubista J, Ohlsson J, Vallo-Christiansen J, Magnusson B (1997) Chronic recurrent multifocal osteomyelitis involving both jaws. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 83:300–305
Gamble JG, Rinsky LA (1986) Chronic recurrent multifocal osteomyelitis: a distinct clinical entity. J Pediatr Orthop. 6:579–584
Giedion A, Holthusen W, Masel LF, Vischer D (1972) Subacute and chronic “symmetric osteomyelitis” [in French]. Ann Radiol (Paris) 15:329–342
Girschick HJ, Krauspe R, Tschammler A, Huppertz HI (1998) Chronic recurrent osteomyelitis with clavicular involvement in children: diagnostic value of different imaging techniques and therapy with non-steroidal antiinflammatory drugs. Eur J Pediatr 157:28–33
Huber AM, Lam PY, Duffy CM, et al (2002) Chronic recurrent multifocal osteomyelitis: clinical outcomes after more than five years of follow-up. J Pediatr 141:198–203
Jurik AG (2004) Chronic recurrent multifocal osteomyelitis. Semin Musculoskelet Radiol 8(3):243–253
Jurik AG, Egund N (1997) MRI in chronic recurrent multifocal osteomyelitis. Skeletal Radiol 26:230–238
Jurik AG, Helmig O, Ternowitz T, Möller BN (1988) Chronic recurrent multifocal osteomyelitis: a follow-up study. J Pediatr Orthop 8:49–58
King SM, Laxer RM, Manson D, Gold R (1987) Chronic recurrent multifocal osteomyelitis: a noninfectious inflammatory process. Pediatr Infect Dis J 6:907–911
Machiels F, Seynaeve P, Lagey C, Mortelmans LL (1992) Chronic recurrent multifocal osteomyelitis with MR correlation: a case report. Pediatr Radiol 22:535–536
Mandell GA, Contreras SJ, Conard K, Harcke HT, Maas KW (1998) Bone scintigraphy in the detection of chronic recurrent multifocal osteomyelitis. J Nucl Med 39:1778–1783
Manson D, Wilmot DM, King S, Laxer RM (1989) Physeal involvement in chronic recurrent multifocal osteomyelitis. Pediatr Radiol 20:76–79
Martin JC, Desoysa R, O’Sullivan MM, Silverstone E, Williams H (1996) Chronic recurrent multifocal osteomyelitis: spinal involvement and radiological appearances. Br J Rheumatol 35:1019–1021
Paller AS, Pachman L, Rich K, Esterly NB, Gonzalez-Crussi F (1985) Pustulosis palmaris et plantaris: its association with chronic recurrent multifocal osteomyelitis. J Am Acad Dermatol 12(5 Pt 2):927–930
Pelkonen P, Ryoppy S, Jaaskelainen J, Rapola J, Repo H, Kaitila I (1988) Chronic osteomyelitislike disease with negative bacterial cultures. Am J Dis Child 142:1167–1173
Schilling F, Fedlmeier M, Eckardt A, Kessler S. (2002) Vertebral manifestation of chronic recurrent multifocal osteomyelitis (CRMO) [Article in German]. Rofo 174(10):1236–1242
Schilling F, Kessler ST (2001) Chronic recurring multifocal osteomyelitis (CRMO) [in German]. Klin Padiatr 213:271–276
Suei Y, Tanimoto K, Taguchi A et al (1995) Possible identity of diffuse sclerosing osteomyelitis and chronic recurrent multifocal osteomyelitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 80:401–408
Sugimoto H, Tamura K, Fujii T (1998) The SAPHO syndrome: defining the radiographic spectrum of diseases comprising the syndrome. Eur Radiol 8:800–806
Vanhoenacker FM, Baekelandt J, Vanwambeke K, Willemen D, De Schepper AM (1998) Chronic recurrent multifocal osteomyelitis. J Belge Radiol 81(2):84–86
Van Howe RS, Starshak RJ, Chusid MJ (1989) Chronic recurrent multifocal osteomyelitis. Clin Pediatr (Phila) 28:54–59
Yu L, Kasser JR, O’Rourke E, Kozakewich H. (1989) Chronic recurrent multifocal osteomyelitis. Association with vertebra plana. J Bone Joint Surg Am 71(1):105–112
Conflict of interest statement
None of the authors has any potential conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Deogaonkar, K., Ghandour, A., Jones, A. et al. Chronic recurrent multifocal osteomyelitis presenting as acute scoliosis: a case report and review of literature. Eur Spine J 17 (Suppl 2), 248–252 (2008). https://doi.org/10.1007/s00586-007-0516-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-007-0516-6