Abstract
Cell-derived decellularized matrices are promising cell culture substrates for tissue engineering and regenerative medicine. However, it is required that cell-derived decellularized matrices are fabricated as desirably-shaped three-dimensional (3D) scaffolds for these applications because they do not retain macrostructures of tissue and organs. To fabricate cell-derived decellularized matrices as 3D scaffolds, 3D template scaffolds have been employed. Recently, 3D-printing techniques have been widely used to construct 3D scaffolds. Thus, 3D-printed scaffolds are available to fabricate cell-derived decellularized matrices as desirably-shaped 3D scaffolds. In this study, cell-derived decellularized matrices were prepared on 3D-printed poly (D, L-lactic acid) (PLA) scaffolds. HT-1080 fibrosarcoma cells were seeded on 3D-printed PLA scaffolds and were cultured to deposit extracellular matrix components beneath the cells. After the culture, the cells were removed from cell-scaffold constructs. Additionally, deposited fibronectin was detected on the surface of 3D-printed PLA scaffolds. These results indicate that cell-derived decellularized matrices were successfully prepared as desirably-shaped 3D scaffolds with the aid of 3D-printed scaffolds. Moreover, the matrices exhibited cell adhesiveness. These results indicate that 3D-printing techniques will aid fabrication of cell-derived decellularized matrices as desirably shaped 3D scaffolds. Improved production of such desirably-shaped 3D scaffolds of cell-derived decellularized matrices will expand the applications in tissue engineering and regenerative medicine.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Extracellular matrix (ECM) is an adhesive substrate for the cells in our body. ECM can regulate various cell functions, including cell adhesion, survival, proliferation, differentiation, migration, and responses to growth factors (Hynes 2009; Giancotti and Ruoslahti 1999). ECM plays a key role in regenerative medicine and tissue engineering. ECM is composed of numerous types of proteins and carbohydrates, and its composition depends on tissue types as well as developmental and pathological states (Manabe et al. 2008; Larsen et al. 2006; Ioachim et al. 2002). Thus, the reconstitution of native ECM in vitro is difficult with conventional chemical and physical methods. Decellularization has been widely used to reconstitute native ECM in vitro (Badylak 2007; Crapo et al. 2011; Hoshiba et al. 2010). Decellularization is a technique to specifically remove cells from cell-ECM constructions. Decellularized matrices, which are reconstituted ECM by decellularization, are mainly derived from two sources: (1) ECM in tissues and organs and (2) ECM deposited on substrates by cultured cells (Hoshiba et al. 2010, 2016; Hoshiba 2017). Each source has both advantages and disadvantages. Specifically, cell-derived decellularized matrices can mimic native ECM located in limited regions, such as the stem cell niche, which is a big advantage over tissue-/organ-derived decellularized matrices (Hoshiba et al. 2016; Hoshiba 2017). Conversely, it is difficult for cell-derived decellularized matrices to mimic macro-structures of tissues and organs, whereas decellularized matrices derived from tissues/organs maintain their micro-structures (Hoshiba et al. 2016; Hoshiba 2017). Thus, fabrication of cell-derived decellularized matrices into desirably-shaped three-dimensional (3D) scaffolds which mimic the shapes of tissues and organs is highly desirable for future tissue and organ substitutions.
To fabricate cell-derived decellularized matrices as 3D scaffolds, cells are seeded for culture upon 3D template scaffolds with various materials to facilitate deposition of ECM components on the surface of the scaffolds (Liao et al. 2010; Pham et al. 2008). Thus, cell-derived decellularized matrices may be fabricated as desirably-shaped 3D scaffolds through the use of 3D templates. There are many methods to construct 3D scaffolds. Recently, 3D-printers have been used to construct desirably-shaped scaffolds (Guvendiren et al. 2016). In this study, we sought to fabricate cell-derived decellularized matrices as desirably-shaped 3D scaffolds with the aid of 3D-printed biodegradable polymer scaffolds. Additionally, we tested whether prepared matrices possess the cell adhesiveness. It is expected that cell-derived decellularized matrices may be fabricated as desirably-shaped 3D scaffolds using 3D-printed templates.
2 Materials and methods
2.1 Fabrication of biodegradable polymer scaffolds with 3D printer
A honeycomb 3D model was created with free 3D modeling software from Autodesk 123D Design (Autodesk Inc., USA), then the digital 3D model was saved in STL format and sent to a fused deposition modeling (FDM) type 3D printer from UP Mini (Japan 3D printer Co., Ltd, Tokyo, Japan). Real honeycomb scaffolds were built up on UP Mini layer-by-layer from the bottom up by heating and extruding thermoplastic poly (D, L-lactic acid) (PLA) filament (Japan 3D printer Co., Ltd, Tokyo, Japan).
2.2 Cell culture
HT-1080 cells (Japanese Collection of Research Bioresources Cell Bank, Osaka, Japan) were maintained in Dulbecco’s Modified Eagle/Nutrient F-12 Mixture (1:1) medium (Gibco, Carlsbad, CA, USA) supplemented with 10% fetal bovine serum (FBS, Equitech-Bio, Kerrville, TX, USA) (serum medium) in tissue culture polystyrene (TCPS) flasks (Greiner Bio-One GmbH, Kremsmünster, Austria). Prior to the experiments, the cells were harvested by treatment with 0.25% trypsin/EDTA solution (Gibco).
2.3 Preparation of cell-derived decellularized matrices on 3D printed scaffolds
The scaffolds were sterilized by soaking in 70% ethanol for 15 min and washed with PBS twice. The cells were suspended in serum medium at a concentration of 500,000 cells/mL. The scaffolds were then immersed in 2 mL of this cell suspension and were incubated for 6 h at 37 °C in 15 mL tubes. After incubation, cell suspensions were removed and the scaffolds were immediately immersed in 2 mL of freshly prepared cell suspension in 15 mL tubes. The scaffolds were then incubated at 37 °C overnight to ensure firm cell adhesion on the scaffolds. After incubation, the cell-scaffold constructs were transferred into a 6-well tissue culture plate cast-coated with 360 μL/well of 0.2% poly (2-methacryloyloxyethyl phosphorylcholine-co-butyl methacrylate) (30:70 mol%, generously provided by NOF, Tokyo, Japan). Transferred cell-scaffold constructs were further cultured in serum medium for 10 days to deposit ECM components by the cells.
2.4 Decellularization
Decellularization was performed with the method described previously (Hoshiba et al. 2012; Hoshiba and Tanaka 2016). Briefly, the cell-scaffold constructs were incubated in PBS containing 0.5% Triton X-100 and 20 mM NH4OH for 5 min at 37 °C. After incubation, the constructs were incubated in PBS containing 100 μg/mL of DNase I (Roche Applied Science, Penzberg, Germany) and RNase A (Nacalai Tesque, Kyoto, Japan) for 1 h at 37 °C. After incubation, the constructs were incubated in 0.1% glutaraldehyde containing PBS for 6 h at 4 °C to fix the deposited ECM components. After fixation, the constructs were treated with 0.1 M glycine containing PBS at 4 °C overnight to quench unreacted aldehyde groups. The decellularized matrices were stored at 4 °C until use.
2.5 Confirmation of cell removal
After the culture of cell-scaffold constructs for 10 days, the cells were fixed with 0.1% glutaraldehyde for 6 h at 4 °C without decellularization. Decellularized matrices and cell-scaffold constructs without decellularization were treated with 1% Triton X-100 containing PBS for 2 min at room temperature to permeabilize cell membranes. The samples were then incubated with Alexa 488-conjugated phalloidin (Invitrogen, Carlsbad, CA, USA) for 1 h at 37 °C to visualized actin filaments. After incubation, the samples were incubated in 10 μg/mL Hoechst 33258 (Wako) for 5 min at 37 °C to visualize cell nuclei. The samples were observed with fluorescence microscope.
2.6 Immunocytochemical analysis of fibronectin
The decellularized matrices were incubated in Blocking One (Nacalai Tesque) for 30 min at 37 °C to block non-specific antibody reactions. After the blocking process, the samples were treated with primary anti-fibronectin antibody (Sigma, St Louis, MO, USA) for 2 h at 37 °C. The samples were incubated with corresponding secondary antibody conjugated with peroxidase (Dako, Carpinteria, CA, USA) for 1 h at 37 °C. Finally, the samples were incubated with 3, 3′-diaminobenzidine (DAB) solution (Dako), a colorimetric substrate used to visualize peroxidase-labeled proteins. Gross appearance of the samples was recorded with a digital camera (Panasonic, Osaka, Japan). The samples were observed using an optical microscope with a light emitting diode (LED), lighting from the lower side of the sample instead of the lighting equipped with the microscope.
2.7 Re-seeding of the cells on the decellularized matrices
Freshly harvested HT-1080 cells were suspended at a concentration of 250,000 cells/mL in serum medium. The matrices were immersed in 2 mL of the suspension and incubated for 6 h at 37 °C in 15 mL tubes. After incubation, non-adherent cells were removed from the cultures and adherent cells were fixed with 0.1% glutaraldehyde containing PBS. The cells were observed by fluorescence microscopy after staining of cell nuclei as described above.
3 Results
3.1 Preparation of cell-derived decellularized matrices on 3D-printed scaffolds
To fabricate cell-derived decellularized matrices as desirably shaped 3D scaffolds, HT-1080 cells were seeded on 3D-printed PLA scaffolds (Fig. 1), and the cells were cultured for 10 days. After the culture, the decellularization was performed. To confirm whether the cells were removed from cell-scaffold constructs, cell nuclei and actin fibers were detected in the samples with Hoechst 33258 and Alexa 488-conjugated phalloidin (Fig. 2). Evident cell nuclei and actin fibers were observed in the samples before decellularization whereas no cell nuclei and actin fibers were observed after decellularization. These results indicated that cells were successfully removed from the cell-scaffold constructs by decellularization.
Additionally, deposited fibronectin was detected to confirm whether ECM components remained even after decellularization (Fig. 3). Deposited fibronectin was labeled by immunocytochemistry and visualized with DAB, which develops a brown deposition after a peroxidase-catalyzed reaction. The decellularized sample was stained brown whereas bare PLA scaffolds were not stained following gross examination (Fig. 3a). Additionally, brown deposition was observed in decellularization samples but not in bare PLA scaffolds following optical microscopic observation (Fig. 3b). These results suggest that ECM components remained even after decellularization and cell-derived decellularized matrices were successfully prepared on 3D-printed PLA scaffolds as templates.
3.2 Cell adhesion on the decellularized matrices
To examine whether cells can adhere on the cell-derived decellularized matrices, freshly harvested HT-1080 cells were seeded on the matrices. After 6 h incubation, adherent cells were detected by the visualization of cell nuclei (Fig. 4). Freshly harvested HT-1080 cells adhered on bare PLA scaffold (Fig. 4, right panel) Additionally, the cells adhered on the cell-derived decellularized matrices (Fig. 4, left panel). This result indicated that the cell-derived decellularized matrices possess the cell adhesiveness even when the matrices were prepared on 3D-printed PLLA scaffolds.
4 Discussion
Cell-derived decellularized matrices are widely used cell culture substrates in tissue engineering and regenerative medicine (Hoshiba et al. 2010, 2016; Hoshiba 2017). However, cell-derived decellularized matrices generally lack tissue- and organ-macrostructure (Hoshiba et al. 2016; Hoshiba 2017). Thus, fabrication of cell-derived decellularized matrices into desirably-shaped 3D scaffolds is required. In this study, we prepared cell-derived decellularized matrices on 3D-printed PLA scaffolds to fabricate matrices in desirably-shaped 3D scaffolds. Preparation of cell-derived decellularized matrices on 3D-printed scaffolds offers a relatively straightforward solution for this problem.
In this study, we demonstrated that cell-derived decellularized matrices can be prepared on 3D-printed scaffolds for fabrication as desirably-shaped 3D scaffolds. However, cells were distributed heterogeneously on PLA scaffolds during the culture for deposition of ECM components (Fig. 2). Deposited fibronectin was also detected as both dense and pale brown regions (Fig. 3). These results indicate that cell-derived decellularized matrices were prepared heterogeneously in this study. To prepare cell-derived decellularized matrices on the 3D scaffolds homogeneously, the homogenous distribution of adherent cells is critical. In this study, the scaffolds were simply immersed in cell suspension and the cells were allowed to adhere. Several cell seeding techniques (e.g., seeding with a low-pressure system, dynamic cell seeding) are available for homogeneous cell seeding (Torigoe et al. 2007; Vitacolonna et al. 2015).
In addition to the homogeneous preparation of cell-derived decellularized matrices on 3D scaffolds, sufficient deposition of ECM components is also critical fully to exert the ability of the matrices for the induction of cell functions. The amounts of deposited ECM components depend many factors, such as cell density and culture period. These factors must be optimized in future studies. Additionally, medium composition can influence the production of ECM components in cells. For example, ascorbic acid promotes the production of collagens and accelerates their deposition (Soucy et al. 2011). Recently, accelerated ECM deposition was reported under macromolecular crowding conditions in the medium (Satyam et al. 2014; Prewitz et al. 2015).
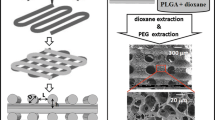
It is possible to fabricate 3D scaffolds with various materials, such as metal, polymers, and inorganic compounds, using a 3D printer (Guvendiren et al. 2016; Frazier 2014; Wu et al. 2011). It is expected that the hybrid scaffolds of cell-derived decellularized matrices with these materials can be prepared and these hybrid scaffolds will helpful to expand the applications, for example, bone and dental tissue engineering. In addition to 3D-printing using these materials, Pati et al., reported that solubilized tissue-derived decellularized matrices could be used as a bio-ink for the 3D-printing of cells (Pati et al. 2014). However, solubilized decellularized matrices lose their microstructures, which can also influence cell functions as well as ECM compositions. We have reported that poly (lactic-co-glycolic acid) (PLGA) scaffolds can be used as template scaffolds, where cell-derived decellularized matrices are prepared. PLGA scaffolds were completely removed after cell-derived decellularized matrices preparation, indicating that PLGA scaffolds can be used as a removable template (Lu et al. 2011a, b). It is expected that cell-derived decellularized matrices can be prepared as desirably-shaped 3D scaffolds without the loss of microstructure using removal scaffolds such as PLGA scaffolds.
5 Conclusions
Cell-derived decellularized matrices can be prepared on 3D-printed scaffolds. The combination with 3D-printing techniques will aid fabrication of cell-derived decellularized matrices as desirably shaped 3D scaffolds. This achievement will expand applications in tissue engineering and regenerative medicine.
References
Badylak SF (2007) The extracellular matrix as a biologic scaffold material. Biomaterials 28:3587–3593
Crapo PM, Gilbert TW, Badylak SF (2011) An overview of tissue and whole organ decellularization processes. Biomaterials 32:3233–3243
Frazier WE (2014) Metal additive manufacturing: a review. J Mater Eng Perform 23:1917–1928
Giancotti FG, Ruoslahti E (1999) Integrin signaling. Science 285:1028–1032
Guvendiren M, Molde J, Soares RMD, Kohn J (2016) Designing biomaterials for 3D printing. ACS Biomater Sci Eng 2:1679–1693
Hoshiba T (2017) Cultured cell-derived decellularized matrices: a review toward the next decade. J Mater Chem B 5:4322–4331
Hoshiba T, Tanaka M (2016) Decellularized matrices as in vitro models of extracellular matrix in tumor tissues at different malignant levels: mechanism of 5-fluorouracil resistance in colorectal tumor cells. BBA-Mol Cell Res 1863:2749–2757
Hoshiba T, Lu H, Kawazoe N, Chen G (2010) Decellularized matrices for tissue engineering. Expert Opin Biol Ther 10:1717–1728
Hoshiba T, Kawazoe N, Chen G (2012) The balance of osteogenic and adipogenic differentiation in human mesenchymal stem cells by matrices that mimic stepwise tissue development. Biomaterials 33:2025–2031
Hoshiba T, Chen G, Endo C, Maruyama H, Wakui M, Nemoto E, Kawazoe N, Tanaka M (2016) Decellularized extracellular matrix as an in vitro model to study the comprehensive roles of the ECM in stem cell differentiation. Stem Cells Int 2016:6397820. doi:10.1155/2016/6397820
Hynes RO (2009) The extracellular matrix: not just pretty fibrils. Science 326:1216–1219
Ioachim E, Charchanti A, Briasoulis E, Karavasilis V, Tsanou H, Arvantis DL, Agnantis NJ, Pavidis N (2002) Immunohistochemical expression of extracellular matrix components tenascin, fibronectin, collagen type IV and laminin in breast cancer: their prognostic value and role in tumor invasion and progression. Eur J Cancer 38:2362–2370
Larsen M, Wei C, Yamada KM (2006) Cell and fibronectin dynamics during branching morphogenesis. J Cell Sci 119:3376–3384
Liao J, Guo X, Grande-Allen KJ, Kasper FK, Mikos AG (2010) Bioactive polymer/extracellular matrix scaffolds fabricated with a flow perfusion bioreactor for cartilage tissue engineering. Biomaterials 31:8911–8920
Lu H, Hoshiba T, Kawazoe N, Chen G (2011a) Autologous extracellular matrix scaffolds for tissue engineering. Biomaterials 32:2489–2499
Lu H, Hoshiba T, Kawazoe N, Koda I, Song M, Chen G (2011b) Cultured cell-derived extracellular matrix scaffolds for tissue engineering. Biomaterials 32:9658–9666
Manabe R, Tsutsui K, Yamada T, Kumura M, Nakano I, Shimono C, Sanzen N, Furutani Y, Fukuda T, Oguri Y, Shimamoto K, Kiyozumi D, Sato Y, Sado Y, Senoo H, Yamashina S, Fukuda S, Kawai J, Sugiura N, Kimata K, Hayashizaki Y, Sekiguchi K (2008) Transcriptome-based systematic identification of extracellular matrix proteins. Proc Natl Acad Sci USA 105:12849–12854
Pati F, Jang J, Ha DH, Kim SW, Rhie JW, Shim JH, Kim DH, Cho DW (2014) Printing three-dimensional tissue analogues with decellularized extracellular matrix bioink. Nat Commun 5:3935. doi:10.1038/ncomms4935
Pham QP, Kasper FK, Baggett LS, Raphael RM, Jansen JA, Mikos AG (2008) The influence of an in vitro generated bone-like extracellular matrix on osteoblastic gene expression of marrow stromal cells. Biomaterials 29:2729–2739
Prewitz MC, Stißel A, Friedrich J, Träber N, Vogler S, Bornhäuser M, Werner C (2015) Extracellular matrix deposition of bone marrow stroma enhanced by macromolecular crowding. Biomaterials 73:60–69
Satyam A, Kumar P, Fan X, Gorelov A, Rochev Y, Joshi L, Peinado H, Lyden D, Thomas B, Rodriguez B, Raghunath M, Pandit A, Zeugolis D (2014) Macromolecular crowding meets tissue engineering by self-assembly: a paradigm shift in regenerative medicine. Adv Mater 26:3024–3034
Soucy PA, Werbin J, Heinz W, Hoh JH, Romer LH (2011) Microelastic properties of lung cell-derived extracellular matrix. Acta Biomater 7:96–105
Torigoe I, Sotome S, Tsuchiya A, Yoshii T, Takahashi M, Kawabata S, Shinomiya K (2007) Novel cell seeding system into a porous scaffold using a modified low-pressure method to enhance cell seeding efficiency and bone formation. Cell Transpl 16:729–739
Vitacolonna M, Belharazem D, Hohenberger P, Roessner ED (2015) Effect of dynamic seeding methods on the distribution of fibroblasts within human acellular dermis. Cell Tissue Bank 16:605–614
Wu C, Luo Y, Cuniberti G, Xiao Y, Gelinsky M (2011) Three-dimensional printing of hierarchical and tough mesoporous bioactive glass scaffolds with a controllable pore architecture, excellent mechanical strength and mineralization ability. Acta Biomater 7:2644–2650
Acknowledgements
This research was supported by a Grant-in-Aid for Challenging Exploratory Research (16K15209) funded by MEXT, Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hoshiba, T., Gong, J. Fabrication of cell-derived decellularized matrices on three-dimensional (3D)-printed biodegradable polymer scaffolds. Microsyst Technol 24, 613–617 (2018). https://doi.org/10.1007/s00542-017-3470-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00542-017-3470-1