Background:
Background:
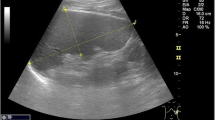
The aim of this study was to evaluate the hemodynamics of gastric varices.
Methods:
We evaluated the detection rates of gastric varices, inflowing vessels to gastric varices, and outflowing vessels from gastric varices in 24 patients with gastric varices, using color Doppler sonography, and compared these findings with computed tomography findings. Eighteen patients had F2-type varices and 6 had F3-type, classified according to the Japanese Research Society for Portal Hypertension. Fourteen patients had fundal varices, and 10 had cardiac and fundal varices.
Results:
The detection rates of collateral veins using color Doppler sonography were as follows: gastric varices were detected in all 24 patients (100%); inflowing vessels, in 21 of the 24 patients (87.5%); and outflowing vessels, in 18 of the 24 patients (75.0%). The detection rates of collateral veins, using computed tomography, were: gastric varices were detected in all 24 patients (100%); inflowing vessels, in all 24 patients (100%); and outflowing vessels, in 21 of the 24 patients (87.5%). The color Doppler findings agreed perfectly with the computed tomography findings in 13 of the 24 patients (54.2%).
Conclusions:
Although color Doppler sonography is a useful, noninvasive modality for evaluating the hemodynamics of gastric varices, it falls short in visualizing the detailed hemodynamics of the inflowing and outflowing vessels of gastric varices in half of the patients when compared with computed tomography.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Author information
Authors and Affiliations
Additional information
Received: September 13, 2001 / Accepted: December 14, 2001
Rights and permissions
About this article
Cite this article
Sato, T., Yamazaki, K., Toyota, J. et al. Color Doppler findings of gastric varices compared with findings on computed tomography. J Gastroenterol 37, 604–610 (2002). https://doi.org/10.1007/s005350200096
Issue Date:
DOI: https://doi.org/10.1007/s005350200096