Abstract
Background
Dipeptidyl peptidase-4 inhibitor (DPP4-I) is clinically used as a new oral antidiabetic agent. Although DPP4 is reportedly associated with the progression of chronic liver diseases, the effect of DPP4-I on liver fibrosis development is still obscure. This study was designed to elucidate the effect of DPP4-I on liver fibrosis development in conjunction with the activated hepatic stellate cells (Ac-HSCs).
Methods
The antifibrotic effect of DPP4-I was assessed in vivo and in vitro using porcine serum-induced experimental liver fibrosis model. DPP4-I, sitagliptin, at a clinically comparable low dose was administered by gavage daily.
Results
DPP4-I significantly attenuated liver fibrosis development along with the suppression of hepatic transforming growth factor (TGF)-β1, total collagen, and tissue inhibitor of metalloproteinases-1 in a dose-dependent manner. These suppressive effects occurred almost concurrently with the attenuation of HSCs activation. Our in vitro studies showed that DPP4-I inhibited platelet-derived growth factor-BB-mediated proliferation of the Ac-HSCs as well as upregulation of TGF-β1 and α1(I)-procollagen at magnitudes similar to those of the in vivo studies. The inhibitory effects of DPP4-I against HSCs proliferation and fibrogenic gene expression are mediated through the inhibition of the phosphorylation of ERK1/2, p38 and Smad2/3, respectively.
Conclusions
DPP4-I markedly inhibits liver fibrosis development in rats via suppression of HSCs proliferation and collagen synthesis. These suppressive effects are associated with dephosphorylation of ERK1/2, p38 and Smad2/3 in the HSCs. Since DPP4-I is widely used in clinical practice, this drug may represent a potential new therapeutic strategy against liver fibrosis in the near future.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Liver cirrhosis can be defined as the end stage of chronic liver diseases, and hepatic failure due to liver cirrhosis is caused by progressive fibrosis that ultimately results in nodular regeneration with loss of function [1]. Liver fibrosis is a common feature of chronic liver diseases regardless of their etiology, such as hepatitis B, hepatitis C, autoimmune disorders, alcohol abuse and nonalcoholic steatohepatitis (NASH), characterized by excessive accumulation of extracellular matrix (ECM) and activated hepatic stellate cells (Ac-HSCs) [2, 3]. Because liver fibrosis progresses and the status of chronic liver disease progress over a long period, therapies should be tolerable and safe over decades, with good targeting to the liver and few adverse effects on other organs. However, no antifibrotic agent has been approved in clinical practice yet [4]. Thus, an alternative approach may be to find a clinically used compound that also shows antifibrotic activity until new drugs become widely available [5]. It has been reported that several drugs used in different clinical liver diseases might exert a suppressive effect on liver fibrosis, targeting Ac-HSCs. For example, blockers of the renin–angiotensin–aldosterone system, such as the angiotensin-converting enzyme inhibitor, angiotensin-II receptor blocker and selective aldosterone blocker, which are commonly used as antihypertensive agents, can reportedly suppress the progression of hepatic fibrosis [6–9]. Moreover, recent reports have demonstrated that imatinib mesylate, an inhibitor of specific protein kinases such as Bcr-Abl fusion protein expressed in chronic myeloid leukemia and c-KIT in gastrointestinal stromal tumors, could attenuate liver fibrosis development via inhibition of the platelet-derived growth factor receptor (PDGFR) in an experimental animal model [10, 11].
Dipeptidyl peptidase 4 inhibitors (DPP4-I) have been recently developed as a new viable option for treatment of type-2 diabetes mellitus (DM) [12–14]. DPP4-I can exert an antidiabetic action due to the enhancement of the function of incretin, including glucagon-like peptide 1 (GLP-1). GLP-1, a prominent active compound of the incretin family, is a gut-derived peptide secreted in a nutrient-dependent manner from the small intestine and stimulates glucose-dependent insulin production and secretion via specific receptors expressed on the islet β cells [14–17]. It potentiates insulin synthesis and secretion, inhibits glucagon secretion, increases islet cell proliferation, and decreases cell apoptosis. Although GLP-1 contributes to improve hyperglycemia, its functions are rapidly inactivated in serum because of the degradation of GLP-1 by DPP4. Therefore, continuous inhibition of DPP4 by DPP4-I can enhance the effects of GLP-1, and consequently may lower the serum glucose [12, 14].
Besides its key role in the regulation of incretin, DPP4 has multiple the functions in various organs [18, 19]. In the liver, DPP4 also plays a role in fibronectin-mediated interaction of hepatocytes with ECM [18, 20, 21]. Moreover, it has been noted that DPP4 is possibly involved in several liver diseases, such as chronic hepatitis C (CHC), primary biliary cirrhosis (PBC), chronic cholestasis and hepatocellular carcinoma (HCC) [22–26]. Previous reports revealed that DPP4 is expressed on the surface of reactive fibroblasts including Ac-HSCs [27–29]. However, the effect of DPP4-I against liver fibrosis development has yet to be clarified.
In the current study, we examined the direct effect of DPP4-I against liver fibrosis induced in rats by porcine serum to evaluate the feasibility of future clinical applications of DPP4-I. We also attempted to investigate the related mechanisms possibly involved therein.
Materials and methods
Animals and reagents
Male Fischer 344 rats, aged 6 weeks, were purchased from Japan SLC, Inc. (Hamamatsu, Shizuoka, Japan). They were housed in stainless steel, mesh cages under a controlled temperature (23 ± 3 °C) and relative humidity (50 ± 20 %), with 10–15 air changes per hour and illumination for 12 h a day. The animals were allowed access to tap water ad libitum throughout the experimental periods. Sitagliptin (DPP4-I) and porcine serum were purchased from Merck & Co., Inc. (Whitehouse Station, NJ, USA) and Life Technologies Japan Ltd. (Tokyo, Japan), respectively.
Animal treatment
To validate the effect of DPP4-I against liver fibrosis development in vivo, we employed a model of liver fibrosis; namely, the porcine serum model [30]. The experimental period of all experiments was 8 weeks. The rats were randomly divided into 4 groups (n = 10, in each group). Groups 1–3 (G1–3) were given 0.5 ml of porcine serum intraperitoneally twice weekly for 8 weeks. G1 received distilled water by gavage daily as the positive control group. G2 was treated with DPP4-I by gavage daily at 100 mg/kg, as the low-dose DPP4-I-treated group. G3 was treated with DPP4-I at 300 mg/kg, as the high-dose DPP4-I-treated group. Group 4 (G4) was injected with PBS and received distilled water by gavage. At the end of the experiments, all rats were anesthetized and several indices were examined. All animal procedures were approved by our Institutional Animal Care Committee, and conducted in accordance with the Nara Medical University Guidelines for the Care and Use of Laboratory Animals.
Histological and immunohistochemical analyses
In all experimental groups, 5-μm-thick sections of formalin-fixed and paraffin-embedded livers were processed routinely for Sirius-red (S-R) staining to determine the development of liver fibrosis. Immunohistochemical staining techniques of α-smooth muscle actin (α-SMA) (DAKO, Kyoto, Japan) were performed as described previously [6]. Semi-quantitative analyses of fibrosis development and the immunopositive cell area of α-SMA were carried out with Adobe Photoshop software and National Institute of Health image software in 6 microscopic visual fields (magnification ×40) per specimen in 10 rats as described previously with minor modifications [6].
Several indices in the liver
The hepatic hydroxyproline content was determined as described previously using 200 mg of frozen liver samples. After equalization of the protein contents, the total collagen and TGF-β1 in the liver were determined by Sircol Soluble Collagen Assay (Biocolor Ltd., Newtownabbey, Northern Ireland) and TGF-β1 ELISA kit (Bender MedSystems GmbH, Vienna, Austria), respectively, according to the manufacturer’s instructions. We also examined tissue inhibitor of metalloproteinase (TIMP)-1 and monocyte chemotactic protein (MCP)-1 by ELISA kit (R&D Systems, Tokyo, Japan) according to the manufacturer’s instructions. We also evaluated the effects of DPP4-I on the production of total collagen and TGF-β1 in PDGF-BB-mediated Ac-HSCs (n = 8 per group) as described for measurement of the whole liver.
Quantitative real-time RT-PCR
The total RNA was extracted by RNeasy mini kit (QIAGEN, Tokyo, Japan) according to the manufacturer’s instructions. The total RNA (2 μg) from each sample was reverse-transcribed to complementary DNA (cDNA) using a High Capacity RNA-to-cDNA kit (Applied Biosystems Inc., Foster City, CA, USA) according to the manufacturer’s instructions. The mRNA expressions of TGF-β1 and α1(I)-procollagen were estimated by quantitative real-time PCR using the StepOnePlus real-time PCR system (Applied Biosystems) with Fast SYBR Green master mix (Applied Biosystems). The relative gene expression was measured using glyceraldehyde-3-phosphate dehydrogenase (GAPDH) as an internal control. The relative amount of target mRNA in each sample was determined by applying the threshold cycle to the standard curve. The primer sequences were as follows: TGF-β1-forward, 5′-CGG CAG CTG TAC ATT GAC TT-3′ and reverse, 5′-AGC GCA CGA TCA TGT TGG AC-3′; α1(I)-procollagen-forward, 5′-AAA GCA GAA ACA TCG GAT TTG G-3′ and reverse, 5′-CGT GTC ATC CCT TGT GCC GCA-3′; GLP-1-forward, 5′-CAG AAG TTG GTC GTG AGG CA-3′ and reverse, 5′-GCC TTT CAC CAG CCA AGC AA-3′; DPP4-forward, 5′-CTC CAG AGG ACA ACC TTG AC-3′ and reverse, 5′-GGA CAA GTG TGC TCT TGA GT; GAPDH-forward, 5′-GTA TGA CTC TAC CCA CGG CAA GT-3′ and reverse, 5′-TTC CCG TTG ATG ACC AGC TT-3′.
Cell isolation and culture
The primary HSCs were isolated from the liver of F344 rats, as described previously, with minor modifications [31]. The cell viability was over 95 %, as determined by the Trypan blue exclusion test. The freshly isolated HSCs were plated at a density of 5 × 105 cells/ml on uncoated plastic dishes. After a 5-day culture period, the HSCs became myofibroblast-like with reduced lipid vesicles and increased immunoreactive α-SMA. After 7-day plating, all cells were well spread and α-SMA positive.
Cell proliferation and signaling assay
The effects of DPP4-I (0.5–10 μM) on PDGF-BB (10 nM)-induced in vitro proliferation of Ac-HSCs were determined by tetrazolium, 3-(4, 5-dimethylthiazol-2,5-yl)-2,5-diphenyltetrazolium bromide (MTT) assay as described previously (n = 8 per group) [10]. This assay was performed following incubation of the Ac-HSCs with PDGF-BB and DPP4-I for 24, 48, and 72 h, respectively. The effects of DPP4-I on PDGF-BB-induced phosphorylation of mitogen-activated protein kinase (MAPK), including ERK1/2, p38, and JNK in Ac-HSCs were measured by ELISA (RayBiotech, Inc., Norcross, GA, USA). It has been reported that the PDGF-BB (10 nM)-induced maximum phosphorylation of ERK1/2, p38, JNK was achieved at 10–15 min after treatment of the Ac-HSCs [10, 32]. Moreover, the effect of DPP4-I on PDGF-BB-induced phosphorylation of Smad2/3 was evaluated by ELISA (R&D Systems, Inc., Minneapolis, MN USA). The Ac-HSCs were incubated with PDGF for 15 min. The cell lysate in each experiment was prepared after PDGF-BB stimulation with or without 0.5–10 μM DPP4-I. The total and phosphorylated ERK1/2, p38, JNK and Smad2/3 were measured by ELISA according to the manufacturer’s instructions (n = 8 in each group).
Western blotting
Both the total- and phospho-PDGF receptor (PDGFR)-β levels in the Ac-HSC were evaluated by a Western blotting assay as described previously [10]. The cell lysate was prepared after PDGF-BB stimulation with or without 0.5–10 μM DPP4-I. The proteins were separated by SDS-PAGE and then transferred to PVDF membranes. The membranes were blocked with PBS-T (PBS, 0.05 % Tween-20) containing 10 % skim milk and were then incubated with 1:1000 diluted total-PDGFR-β antibody and phospho-PDGFR-β (Tyr751) antibody (Cell Signaling Technology, Inc., Danvers, MA, USA) in PBS-T containing 5 % skim milk for 1 h at room temperature. After washing, the membranes were incubated with horseradish peroxidase-conjugated antibody (1:1000) for 1 h at room temperature.
Statistical analyses
To assess the significance of differences in the quantitative data between groups, Bonferroni’s multiple comparison test was used after one-way ANOVA. This was followed by Bartlett’s test to determine the homology of variance.
Results
General findings
The general findings of the rats at the age of 14 weeks are shown in Table 1. No significant differences in the final body weights could be observed. The relative liver weights of the PS-treated rats (G1–G3) were higher than those of the PBS-treated rats (G4), whereas no significant differences were observed among G1–G3. Regarding the serological data, no significant differences in the levels of alanine aminotransferase (ALT), albumin (Alb) and total bilirubin (T-Bil) could be observed. The levels of serum glucose, plasma insulin and glucagon were not altered by treatment with DPP4-I at the current dose. Similarly, there were no significant differences among G1G4 in the levels of the expression of hepatic GLP-1 mRNA (data not shown), indicating that local GLP-1 alteration was not involved in the antifibrotic effects of DPP4-I.
Effects of DPP4-I on liver fibrosis development
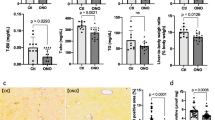
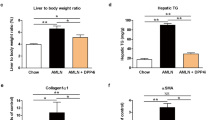
We first examined the effects of DPP4-I on liver fibrosis induced by administration of porcine serum. As shown in Fig. 1a and b, liver fibrosis development was significantly suppressed by treatment with a low-dose DPP4-I (G2) as compared to the control group (G1). The high-dose DPP4-I (G3) exerted a more potent inhibitory effect than the low-dose treatment. No fibrosis development could be observed in the PBS-treated control rats (G4). We next carried out an immunohistochemical analysis of α-SMA to examine the effects of DPP4-I on HSCs activation during liver fibrosis development. The α-SMA immunopositive Ac-HSCs drastically decreased by treatment with DPP4-I (Fig. 2a). Computer-assisted semiquantitative analysis showed that α-SMA-positive cells in the DPP4-I-treated groups significantly decreased in comparison with the control group (Fig. 2b). We also found that DPP4-I markedly suppressed the hepatic TGF-β1, total collagen and hydroxyproline contents in comparison with the control group (Fig. 3a, b and c, respectively). These inhibitory effects closely correlated with the changes in mRNA expressions of TGF-β1 and α1(I)-procollagen (Fig. 4a and b, respectively). We also examined the PDGF-BB and PDGFR-β mRNA expression levels in the liver. As shown in Fig. 4c and d, PDGF-BB and PDGFR-β mRNA expression levels were elevated in the porcine serum-induced fibrotic liver, whereas DPP4-I did not significantly suppress both augmentations. We also measured the protein levels of hepatic TIMP-1 and MCP-1 by ELISA. As shown in Fig. 3d, hepatic TIMP-1 increased in G1, and this increase was suppressed by treatment of high dose of DPP4-I. The MCP-1 expression level was also increased in the liver of PS-treated rats. However, this increase was not significantly suppressed in the DPP4-I-treated rats, indicating that the DPP4-I did not regulate the MCP-1 production in the current experimental model (Fig. 3e).
DPP4-I ameliorates liver fibrosis development induced by treatment of porcine serum. a An extensive fibrosis development was observed in the vehicle-treated control group (G1). Treatment with DPP4-I at 100 mg/kg/day (G2) showed significant inhibitory effect against liver fibrosis. Treatment with DPP4-I at 300 mg/kg/day (G3) exerted a stronger inhibitory effect than in G2. No fibrosis development was observed in the PBS-treated rats (G4) (original magnification ×40). b Semi-quantitative analysis confirmed histological findings. The data represent the mean ± SEM (bars n = 10). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
α-SMA immunopositive Ac-HSCs were attenuated by administration of DPP4-I. a: The α-SMA immunopositive cells significantly decreased following administration of DPP4-I in the 100 mg/kg/day-treated group (G2) as compared with the control group (G1). A more potent inhibitory effect was observed in the 300 mg/kg/day-treated group (G3). No α-SMA immunopositive cells were observed in the PBS-treated rats (G4) (original magnification ×40). b Semi-quantitative analysis confirmed that the α-SMA immunopositive cells decreased in the DPP4-I-treated-groups in parallel with the reduction of liver fibrosis (original magnification ×40). The data represent the mean ± SEM (bars n = 10). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
DPP4-I inhibited several fibrotic markers in the liver. a The TGF-β1 level increased in the vehicle-treated control group (G1) as compared with the PBS-treated group (G4). This increase was significantly suppressed by DPP4-I in the 100 mg/kg/day-treated group (G2) and 300 mg/kg/day-treated group (G3). The suppression of TGF-β1, total collagen, hydroxyproline with treatment of DPP4-I was of similar magnitude to the inhibition of liver fibrosis and α-SMA positive cells (b and c, respectively). d The hepatic TIMP-1 was increased in G1 when compared to the PBS-treated group (G4), and this increase was suppressed by DPP4-I treatment (G3). e The MCP-1 was increased in the liver of PS-treated rats (G1), but this increment was not significantly suppressed in the DPP4-I-treated rats (G2 and G3). The data represent the mean ± SEM (bars n = 10). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
DPP4-I inhibited TGF-β1 and α1(I)-procollagen mRNA expression in the liver. The TGF-β1 (a) and α1(I)-procollagen (b) mRNA expression significantly increased in the vehicle-treated control group (G1) as compared with the PBS-treated group (G4). Treatment with DPP4-I at 100 mg/kg/day (G2) markedly suppressed the expressions of both TGF-β1 and α1(I)-procollagen in comparison with G1. More potent suppressive effects were observed in DPP4-I at 300 mg/kg/day-treated group (G3). PDGF-BB (c) and PDGFR-β (d) mRNA expression levels were elevated in the porcine serum-induced fibrotic liver (G1) when compared to the PBS-treated group (G4). DPP4-I did not significantly suppress both augmentations (G2 and G3). The data represent the mean ± SEM (bars n = 10). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
Effects of DPP4-I on proliferation, TGF-β1, and total collagen of the Ac-HSCs
To elucidate the possible mechanisms, we examined the effects of DPP4-I on the Ac-HSCs from several aspects. First, we examined the effect of DPP4-I on PDGF-BB-induced proliferation of the Ac-HSCs in vitro. As shown in Fig. 5a, DPP4-I significantly attenuated PDGF-BB-induced proliferation of the Ac-HSCs in a dose-dependent manner. Moreover, we examined the effects of DPP4-I on the protein production of TGF-β1 and total collagen in Ac-HSCs. We observed that the protein levels of both TGF-β1 and total collagen increased by stimulation with PDGF-BB, and these increased levels were reduced in the presence of DPP4-I (Fig. 5b). Similar to the relation of α-SMA-positive cells in the liver, the suppressive effect of DPP4-I on the Ac-HSCs proliferation closely correlated with the reduction of TGF-β1 and total collagen production in vitro. In addition to protein production, we investigated the effects of DPP4-I on PDGF-BB-stimulated TGF-β1 and α1(I)-procollagen mRNA expressions of the Ac-HSCs. We found that both TGF-β1 and α1(I)-procollagen mRNA expressions stimulated by PDGF-BB were downregulated in the presence of DPP4-I in a dose-dependent manner (Fig. 6a and b, respectively). Moreover, we noticed that this downregulation of these genes in vitro was of similar magnitude to the reduction of both mRNA levels in the in vivo fibrotic liver.
Treatment of DPP4-I attenuated the PDGF-BB-stimulated proliferation and production of TGF-β and total collagen in the Ac-HSCs. a PDGF-BB-stimulated HSCs proliferation was suppressed by treatment with DPP4-I in a dose-dependent manner. b Similar to the changes in the cell proliferation, the production of TGF-β1 and total collagen in the Ac-HSCs was suppressed by treatment with DPP4-I. Each bar represents the mean ± SEM (n = 8). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01). Filled square PDGF-BB only, filled triangle PDGF-BB and 0.5 μM DPP4-I, open square PDGF-BB and 1 μM DPP4-I, open rectangle PDGF-BB and 10 μM DPP4-I, filled circle untreated
DPP4-I inhibited PDGF-BB-stimulated TGF-β1 and α1(I)-procollagen mRNA expressions in the Ac-HSCs. Both TGF-β1 (a) and α1(I)-procollagen (b) mRNA expressions stimulated by PDGF-BB were downregulated in the presence of DPP4-I in a dose-dependent manner. This downregulation was of similar magnitude to reduction of both mRNA levels in the in vivo fibrotic liver. Each bar represents the mean ± SEM (n = 8). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
Effects of DPP4-I on the phosphorylation of ERK1/2, p38 and Smad2/3 in the Ac-HSCs
We firstly examined whether or not DPP4-I directly inhibited the phosphorylation of PDGF receptor (PDGFR)-β. As shown in Fig. 7a, the phosphorylated PDGFR-β level was not altered by treatment of DPP4-I, indicating that the DPP4-I is not an antagonist of PDGFR-β. We next examined the effects of DPP4-I on the MAPK and Smad2/3 pathway in the Ac-HSCs. As shown in Fig. 7b–d, ERK1/2, p38 and JNK phosphorylation was markedly upregulated by PDGF-BB. DPP4-I treatment significantly suppressed the ERK1/2 phosphorylation in a dose-dependent manner (Fig. 7b). The p38 phosphorylation was only suppressed by a high dose (10 μM) of DPP4-I (Fig. 7c). On the other hand, phosphorylation of JNK was not affected by DPP4-I treatment even at a dose of 10 μM (Fig. 7d). Figure 7e shows that Smad2/3 phosphorylation induced by PDGF-BB was attenuated by DPP4-I in a dose-dependent manner.
PDGF-BB-stimulated phosphorylation of ERK1/2, p38 and Smad2/3 in the Ac-HSC was inhibited in the presence of DPP4-I. a Effect of DPP4-I on the phosphorylation of PDGF receptor (PDGFR)-β. The level of phosphorylated PDGFR-β was upregulated in the presence of PDGF-BB, while this up-regulation was not influenced by DPP4-I. b ERK1/2 phosphorylation stimulated by PDGF-BB was downregulated in the presence of DPP4-I in a dose-dependent manner. c p38 MAPK phosphorylation was suppressed only by treatment of 10 μM DPP4-I. d JNK phosphorylation was not affected by treatment with DPP4-I. e Smad2/3 phosphorylation was suppressed by DPP4-I in a dose-dependent manner. Each bar represents the mean ± SEM (n = 8). Asterisk indicates a statistically significant difference between the indicated experimental groups (p < 0.01)
Discussion
DPP4 is identical to CD26 (DPP4, EC 3.4.14.5), a molecule of 110-kDa membrane-associated sialoglycoprotein with serine protease activity that catalyzes the release of N-terminal dipeptides from peptides and proteins with proline, hydroxyproline and alanine at the penultimate position. In humans, DPP4 is present in several organs including the liver [33]. Furthermore, DPP4 is expressed in various cell types such as the capillary endothelial cells [34, 35]. It has been assumed that DPP4 may play an important role in the control of proliferation and growth of these cell types through regulation of the extracellular concentration of biologically active peptides, and that DPP4 contributes to various physiological and pathological events such as cancer, angiogenesis, and organ fibrosis development [28, 36, 37]. In clinical practice, DPP4 is now commonly recognized as a target of therapy for hyperglycemia due to its function of inhibiting incretin [12–14].
In the current study, we firstly demonstrated that DPP4-I could exert an antifibrotic effect on the experimental hepatic fibrosis in rats. It has been reported that the serum DPP4 activity was augmented in tetrachloromethane-induced cirrhotic rats [38]. In humans, the serum DPP4 activity was suppressed by treatment with interferon in patients with CHC [25]. Furthermore, it has also been stated that the serum DPP4 activity might be an indicator of the severity and progression of PBC [24]. DPP4 also participates in the fibroblast activation, and plays a role in hepatocyte-ECM interactions [20, 21]. Fibroblast activation protein (FAP), which is a cell surface protein exhibiting DPP4, is expressed by the Ac-HSCs, indicating that the high DPP4 level may contribute to the Ac-HSCs-induced ECM accumulation in the liver [27–29]. Interestingly, we observed the DPP4 mRNA expression in the Ac-HSCs, but not in the quiescent HSCs (data not shown). This observation was consistent with the results of a previous report showing that the DPP4 could only express on the Ac-HSCs [27]. Our in vivo studies showed that DPP4-I inhibited liver fibrosis development and production of both hepatic TGF-β1 and total collagen, along with the attenuation of the α-SMA positive Ac-HSCs. These results indicate that the antifibrotic effect of DPP4-I may be achieved by suppression of the function of the Ac-HSCs. Furthermore, our in vitro studies confirmed that DPP4-I could repress the function of the Ac-HSCs. The proliferation of the Ac-HSCs induced by PDGF-BB was significantly attenuated by treatment with DPP4-I in a dose-dependent manner. Several reports have demonstrated that inhibition of DPP4 suppressed the activation of ERK1/2 [39, 40]. The inhibitors of DPP4-like activity could attenuate phosphorylation of ERK stimulated by TGF-β in the normal and keloid-derived skin fibroblasts [39]. In our study, we found that DPP4-I induced the dephosphorylation of ERK1/2 in the Ac-HSCs, and the magnitude of this suppressive effect was almost parallel to the antiproliferative effect. Consequently, these results suggest that the inhibitory effect of DPP4-I on the Ac-HSCs proliferation is mainly associated with suppression of ERK1/2 phosphorylation. DPP4-I also inhibited the TGF-β-Smad2/3 signaling pathway in the Ac-HSCs, and led to suppression of collagen synthesis. TGF-β1 is the most potent stimulus to hepatic fibrogenesis through the TGF-β1-Smad signaling pathway [41]. The activated TGF-β receptors stimulate the phosphorylation of the receptor-regulated Smad2 and Smad3 proteins (R-Smads), which in turn form complexes with Smad4. This complex translocates from the cytoplasm into the nucleus, where the Smads regulate the transcription of target genes including α1(I)-procollagen [41, 42]. In our current study, we showed that treatment with DPP4-I inhibited α1(I)-procollagen expression induced by PDGF-BB in the Ac-HSCs, along with the attenuation of TGF-β expression and phosphorylation of Smad2/3, indicating that the antifibrotic effect of DPP4-I is, at least partially, associated with prevention of this signaling pathway as well as the ERK1/2 pathway. We also found that DPP4-I could interfere with p38 MAPK phosphorylation in the Ac-HSCs. A recent study has revealed that p38 MAPK regulates the α1(I)-collagen gene expression and increases the α1(I)-collagen mRNA stability in the HSCs [43]. These actions of DPP4-I on p38 phosphorylation are also likely to be involved in the inhibitory effect against liver fibrosis in the current study. However, in the current study, we only observed the possible correlations between DPP4-I and several signaling cascades, and not the direct interaction. DPP4-I could suppress Smad2/3 and ERK1/2 that are known to be important molecules in TGF-β and proliferation signaling pathways. Since the suppression of TGF-β pathway by DPP4-I was not likely to ameliorate all other intra-cellular signaling cascades including proliferation, we presume that DPP4-I would suppress each cascade independently although the exact mechanism is still obscure at this time. Further detailed studies, such as binding assay is required in the future.
DPP4-I is now recognized as a new agent providing beneficial effects for diabetic patients [12–14]. DM plays an important role in development of some liver diseases, such as NASH [44]. Several reports have recently demonstrated that antidiabetic agents might exert beneficial effects for patients with NASH [45–47]. Moreover, it has recently been reported that GLP-1 receptor agonism could improve biochemical and histopathological indices in the experimental NASH model [48]. In the current study, we observed that DPP4-I suppressed liver fibrosis development, while both the concentrations of serum glucose, insulin and glucagon and the hepatic GLP-1 expression level showed no differences among the experimental groups. These results indicate that the antifibrotic effect of DPP4-I was independent of the improvement of DM or upregulation of hepatic GLP-1 in this study. Further studies are needed to elucidate whether the antifibrotic effect of DPP4-I could take place under the condition of DM in the future.
Noteworthy was the finding that the inhibitory effects of DPP4-I were achieved at clinically comparable low doses. A dose of 50–100 mg/body/day of sitagliptin (DPP4-I) is commonly used for treatment of type-2 DM. When DPP4-I is administered to man at 100 mg/body/day continuously, the Cmax level is about 1 μM. In the current study, we employed a dose of 500 nM to 10 μM including 1 μM for the in vitro studies. Accordingly, we assume that the dose of DPP4-I in the current study was comparable to that used in clinical practice. Similarly, in some recent studies, sitagliptin was administered to rats at the dose of 100–400 mg/kg/day to examine the antidiabetic effect [49–51]. Furthermore, we also observed that sitagliptin did not cause any adverse effect at a dose of 300 mg/kg/day, which was consistent with a previous report using 500 mg/kg/day (Merck & Co., Inc. personal communication). We also observed that DPP4-I could suppress the liver fibrosis development in the CCl4-induced, as well as porcine serum-induced (under the condition of insulin resistance) models of liver fibrosis. These results indicated that the anti-fibrotic effect of DPP4-I was not model-specific, and demonstrated not only its preventive effect on the liver fibrosis development, but also the therapeutic potential (data not shown).
In summary, we could herein show that treatment with a clinically used DPP4-I markedly inhibited liver fibrosis development along with suppression of proliferation and collagen synthesis in the Ac-HSC. These suppressive effects possibly involved the suppression of several intracellular signaling pathways including ERK1/2, p38 and Smad2/3. It is noteworthy that the inhibitory effects of DPP4 against liver fibrosis development could be achieved at a clinically comparable low dose. Since DPP4-I has already been proved clinically useful for type-2 DM and is safe and widely used, this drug may represent a potential new therapeutic strategy against liver fibrosis in the near future.
Abbreviations
- Ac-HSCs:
-
Activated hepatic stellate cells
- CHC:
-
Chronic hepatitis C
- DM:
-
Diabetes mellitus
- DPP4-I:
-
Dipeptidyl peptidase-4 inhibitor
- ECM:
-
Extracellular matrix
- ERK1/2:
-
Extracellular-signal regulated kinase 1/2
- FAP:
-
Fibroblast activation protein
- GAPDH:
-
Glyceraldehyde-3-phosphate dehydrogenase
- GLP-1:
-
Glucagon-like peptide 1
- HCC:
-
Hepatocellular carcinoma
- JNK:
-
c-Jun N-terminal kinase
- MAPK:
-
Mitogen-activated protein kinase
- MTT:
-
Tetrazolium 3-(4, 5-dimethylthiazol-2,5-yl)-2,5-diphenyltetrazolium bromide
- NASH:
-
Nonalcoholic steatohepatitis
- PBC:
-
Primary biliary cirrhosis
- PDGF:
-
Platelet-derived growth factor
- α-SMA:
-
α-Smooth muscle actin
- TGF-β1:
-
Transforming growth factor-β1
References
Bataller R, Brenner DA. Liver fibrosis. J Clin Invest. 2005;115:209–18.
Guo J, Friedman SL. Hepatic fibrogenesis. Semin Liver Dis. 2007;27:413–26.
Friedman SL. Mechanisms of hepatic fibrogenesis. Gastroenterology. 2008;134:1655–69.
Friedman SL. Liver fibrosis – from bench to bedside. J Hepatol. 2003;38(Suppl 1):S38–53.
Fallowfield JA. Therapeutic targets in liver fibrosis. Am J Physiol Gastrointest Liver Physiol. 2011;300:G709–15.
Yoshiji H, Kuriyama S, Yoshii J, Ikenaka Y, Noguchi R, Nakatani T, Tsujinoue H, et al. Angiotensin-II type 1 receptor interaction is a major regulator for liver fibrosis development in rats. Hepatology. 2001;34:745–50.
Debernardi-Venon W, Martini S, Biasi F, Vizio B, Termine A, Poli G, Brunello F, et al. AT1 receptor antagonist Candesartan in selected cirrhotic patients: effect on portal pressure and liver fibrosis markers. J Hepatol. 2007;46:1026–33.
Matono T, Koda M, Tokunaga S, Sugihara T, Ueki M, Murawaki Y. The effects of the selective mineralocorticoid receptor antagonist eplerenone on hepatic fibrosis induced by bile duct ligation in rat. Int J Mol Med. 2010;25:875–82.
Noguchi R, Yoshiji H, Ikenaka Y, Kaji K, Shirai Y, Aihara Y, Yamazaki M, et al. Selective aldosterone blocker ameliorates the progression of non-alcoholic steatohepatitis in rats. Int J Mol Med. 2010;26:407–13.
Yoshiji H, Noguchi R, Kuriyama S, Ikenaka Y, Yoshii J, Yanase K, Namisaki T, et al. Imatinib mesylate (STI-571) attenuates liver fibrosis development in rats. Am J Physiol Gastrointest Liver Physiol. 2005;288:G907–13.
Kuo WL, Yu MC, Lee JF, Tsai CN, Chen TC, Chen MF. Imatinib mesylate improves liver regeneration and attenuates liver fibrogenesis in CCL4-treated mice. J Gastrointest Surg. 2012;16:361–9.
Drucker DJ, Nauck MA. The incretin system: glucagon-like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes. Lancet. 2006;368:1696–705.
Ahren B. Dipeptidyl peptidase-4 inhibitors: clinical data and clinical implications. Diabetes Care. 2007;30:1344–50.
Holst JJ, Vilsboll T, Deacon CF. The incretin system and its role in type 2 diabetes mellitus. Mol Cell Endocrinol. 2009;297:127–36.
Toft-Nielsen MB, Damholt MB, Madsbad S, Hilsted LM, Hughes TE, Michelsen BK, Holst JJ. Determinants of the impaired secretion of glucagon-like peptide-1 in type 2 diabetic patients. J Clin Endocrinol Metab. 2001;86:3717–23.
Farilla L, Hui H, Bertolotto C, Kang E, Bulotta A, Di Mario U, Perfetti R. Glucagon-like peptide-1 promotes islet cell growth and inhibits apoptosis in Zucker diabetic rats. Endocrinology. 2002;143:4397–408.
Li Y, Hansotia T, Yusta B, Ris F, Halban PA, Drucker DJ. Glucagon-like peptide-1 receptor signaling modulates beta cell apoptosis. J Biol Chem. 2003;278:471–8.
Lambeir AM, Durinx C, Scharpe S, De Meester I. Dipeptidyl-peptidase IV from bench to bedside: an update on structural properties, functions, and clinical aspects of the enzyme DPP IV. Crit Rev Clin Lab Sci. 2003;40:209–94.
Gorrell MD, Wang XM, Park J, Ajami K, Yu DM, Knott H, Seth D, et al. Structure and function in dipeptidyl peptidase IV and related proteins. Adv Exp Med Biol. 2006;575:45–54.
Piazza GA, Callanan HM, Mowery J, Hixson DC. Evidence for a role of dipeptidyl peptidase IV in fibronectin-mediated interactions of hepatocytes with extracellular matrix. Biochem J. 1989;262:327–34.
Brill S, Zvibel I, Halpern Z, Oren R. The role of fetal and adult hepatocyte extracellular matrix in the regulation of tissue-specific gene expression in fetal and adult hepatocytes. Eur J Cell Biol. 2002;81:43–50.
Stecca BA, Nardo B, Chieco P, Mazziotti A, Bolondi L, Cavallari A. Aberrant dipeptidyl peptidase IV (DPP IV/CD26) expression in human hepatocellular carcinoma. J Hepatol. 1997;27:337–45.
Perner F, Gyuris T, Rakoczy G, Sarvary E, Gorog D, Szalay F, Kunos I, et al. Dipeptidyl peptidase activity of CD26 in serum and urine as a marker of cholestasis: experimental and clinical evidence. J Lab Clin Med. 1999;134:56–67.
Lakatos PL, Firneisz G, Rakoczy G, Selmeci L, Szalay F. Elevated serum dipeptidyl peptidase IV (CD26, EC 3.4.14.5) activity in patients with primary biliary cirrhosis. J Hepatol. 1999;30:740.
Firneisz G, Lakatos PL, Szalay F. Serum dipeptidyl peptidase IV (DPP IV, CD26) activity in chronic hepatitis C. Scand J Gastroenterol. 2001;36:877–80.
Stone SF, Lee S, Keane NM, Price P, French MA. Association of increased hepatitis C virus (HCV)-specific IgG and soluble CD26 dipeptidyl peptidase IV enzyme activity with hepatotoxicity after highly active antiretroviral therapy in human immunodeficiency virus-HCV-coinfected patients. J Infect Dis. 2002;186:1498–502.
Levy MT, McCaughan GW, Abbott CA, Park JE, Cunningham AM, Muller E, Rettig WJ, et al. Fibroblast activation protein: a cell surface dipeptidyl peptidase and gelatinase expressed by stellate cells at the tissue remodelling interface in human cirrhosis. Hepatology. 1999;29:1768–78.
Levy MT, McCaughan GW, Marinos G, Gorrell MD. Intrahepatic expression of the hepatic stellate cell marker fibroblast activation protein correlates with the degree of fibrosis in hepatitis C virus infection. Liver. 2002;22:93–101.
Wang XM, Yu DM, McCaughan GW, Gorrell MD. Fibroblast activation protein increases apoptosis, cell adhesion, and migration by the LX-2 human stellate cell line. Hepatology. 2005;42:935–45.
Bhunchet E, Eishi Y, Wake K. Contribution of immune response to the hepatic fibrosis induced by porcine serum. Hepatology. 1996;23:811–7.
Weiskirchen R, Gressner AM. Isolation and culture of hepatic stellate cells. Methods Mol Med. 2005;117:99–113.
Patsenker E, Popov Y, Wiesner M, Goodman SL, Schuppan D. Pharmacological inhibition of the vitronectin receptor abrogates PDGF-BB-induced hepatic stellate cell migration and activation in vitro. J Hepatol. 2007;46:878–87.
Gorrell MD. Dipeptidyl peptidase IV and related enzymes in cell biology and liver disorders. Clin Sci (Lond). 2005;108:277–92.
Koyama T, Gao M, Ueda T, Batra S, Itoh K, Ushiki T, Abe K. Different enzyme activities in coronary capillary endothelial cells. Adv Exp Med Biol. 1997;411:359–64.
Matheeussen V, Baerts L, De Meyer G, De Keulenaer G, Van der Veken P, Augustyns K, Dubois V, et al. Expression and spatial heterogeneity of dipeptidyl peptidases in endothelial cells of conduct vessels and capillaries. Biol Chem. 2011;392:189–98.
Havre PA, Abe M, Urasaki Y, Ohnuma K, Morimoto C, Dang NH. The role of CD26/dipeptidyl peptidase IV in cancer. Front Biosci. 2008;13:1634–45.
Kitlinska J, Lee EW, Li L, Pons J, Estes L, Zukowska Z. Dual role of dipeptidyl peptidase IV (DPP IV) in angiogenesis and vascular remodeling. Adv Exp Med Biol. 2003;524:215–22.
Lakatos PL, Firneisz G, Borcsiczky D, Zalatnai A, Selmeci L, Szalay F. Elevated serum dipeptidyl peptidase IV (CD26, EC 3.4.14.5) activity in experimental liver cirrhosis. Eur J Clin Invest. 2000;30:793–7.
Thielitz A, Vetter RW, Schultze B, Wrenger S, Simeoni L, Ansorge S, Neubert K, et al. Inhibitors of dipeptidyl peptidase IV-like activity mediate antifibrotic effects in normal and keloid-derived skin fibroblasts. J Invest Dermatol. 2008;128:855–66.
Ta NN, Li Y, Schuyler CA, Lopes-Virella MF, Huang Y. DPP-4 (CD26) inhibitor alogliptin inhibits TLR4-mediated ERK activation and ERK-dependent MMP-1 expression by U937 histiocytes. Atherosclerosis. 2010;213:429–35.
Inagaki Y, Okazaki I. Emerging insights into transforming growth factor beta Smad signal in hepatic fibrogenesis. Gut. 2007;56:284–92.
Derynck R, Zhang YE. Smad-dependent and Smad-independent pathways in TGF-beta family signalling. Nature. 2003;425:577–84.
Tsukada S, Westwick JK, Ikejima K, Sato N, Rippe RA. SMAD and p38 MAPK signaling pathways independently regulate alpha1(I) collagen gene expression in unstimulated and transforming growth factor-beta-stimulated hepatic stellate cells. J Biol Chem. 2005;280:10055–64.
Chitturi S, Abeygunasekera S, Farrell GC, Holmes-Walker J, Hui JM, Fung C, Karim R, et al. NASH and insulin resistance: insulin hypersecretion and specific association with the insulin resistance syndrome. Hepatology. 2002;35:373–9.
Belfort R, Harrison SA, Brown K, Darland C, Finch J, Hardies J, Balas B, et al. A placebo-controlled trial of pioglitazone in subjects with nonalcoholic steatohepatitis. N Engl J Med. 2006;355:2297–307.
Torres DM, Jones FJ, Shaw JC, Williams CD, Ward JA, Harrison SA. Rosiglitazone versus rosiglitazone and metformin versus rosiglitazone and losartan in the treatment of nonalcoholic steatohepatitis in humans: a 12-month randomized, prospective, open- label trial. Hepatology. 2011;54:1631–9.
Mazza A, Fruci B, Garinis GA, Giuliano S, Malaguarnera R, Belfiore A. The role of metformin in the management of NAFLD. Exp Diabetes Res;2012:716404.
Trevaskis JL, Griffin PS, Wittmer C, Neuschwander-Tetri BA, Brunt EM, Dolman CS, Erickson MR, et al. Glucagon-like peptide-1 (GLP-1) receptor agonism improves metabolic, biochemical and histopathological indices of nonalcoholic steatohepatitis (NASH) in mice. Am J Physiol Gastrointest Liver Physiol. 2012;302:G762–72.
Matveyenko AV, Dry S, Cox HI, Moshtaghian A, Gurlo T, Galasso R, et al. Beneficial endocrine but adverse exocrine effects of sitagliptin in the human islet amyloid polypeptide transgenic rat model of type2 diabetes: interactions with metformin. Diabetes. 2009;58:1604–15.
Maiztegui B, Borelli MI, Madrid VG, Del Zotto H, Raschia MA, Francini F, et al. Sitagliptin prevents the development of metabolic and hormonal disturbances, increased β-cell apoptosis and liver steatosis induced by a fructose-rich diet in normal rats. Clin Sci (Lond). 2011;120:73–80.
Shang Q, Liu MK, Saumoy M, Holst JJ, Salen G, Xu G. The combination of colesevelam with sitagliptin enhances glycemic control in diabetic ZDF rat model. Am J Physiol Gastrointest Liver Physiol. 2012;302:G815–23.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaji, K., Yoshiji, H., Ikenaka, Y. et al. Dipeptidyl peptidase-4 inhibitor attenuates hepatic fibrosis via suppression of activated hepatic stellate cell in rats. J Gastroenterol 49, 481–491 (2014). https://doi.org/10.1007/s00535-013-0783-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-013-0783-4