Abstract
Background
The development of a supportive diagnostic method has long been required to differentially diagnose ulcerative colitis (UC) and Crohn’s disease (CD). Several antibodies circulate in the sera of patients with inflammatory bowel disease. We previously identified the high mobility group box 1 and box 2 non-histone chromosomal proteins (HMGB1 and HMGB2) as novel antigens of perinuclear type anti-neutrophil cytoplasmic antibodies (pANCA) and discovered anti-HMGB1/HMGB2 antibodies in sera from patients with UC. Here, we evaluated the ability of anti-HMGB1/HMGB2 antibodies combined with anti-Saccharomyces cerevisiae antibodies (ASCA) to differentially diagnose UC and CD.
Methods
We measured titers of anti-HMGB1/HMGB2 antibodies and ASCA in the sera of 213 patients with UC and 93 with CD, using enzyme-linked immunosorbent assays.
Results
Among the patients with UC, 26.8% were positive for anti-HMGB1/HMGB2 antibodies, with 85.0% specificity towards CD and a positive predictive value of 80.3%. Corticosteroids significantly suppressed the titer of anti-HMGB1/HMGB2 antibodies. Among the patients with CD, 24.7% were positive for ASCA, with 96.2% specificity towards UC and a positive predictive value of 74.2%. Interestingly, the positivity rate of anti-HMGB/HMGB2 antibodies was higher (35.7%) in patients with the ileitis type of CD than in patients with CD in the colon (6.2%; significant difference, P < 0.01). The specificity of anti-HMGB1/HMGB2 antibodies in UC for CD in the colon was 93.8%.
Conclusions
CD in the colon and UC can be differentially diagnosed using anti-HMGB/HMGB2 antibodies combined with ASCA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) with unknown etiology. Autoimmune mechanisms might play an important role in the pathogenesis of UC, and various autoantibodies have been identified in sera from patients with UC [1–3]. Anti-neutrophil cytoplasmic antibodies (ANCA) are directed against the cytoplasmic components of neutrophils and can be identified as cytoplasmic (cANCA) and perinuclear (pANCA) types by indirect immunofluorescence (IIF). pANCA are often recognized in sera from patients with UC [4] and are thus useful in UC screening, along with corresponding antigens such as myeloperoxidase (MPO) [5], cathepsin G [6], and elastase [7].
Recently, we identified high mobility group box 1 and box 2 non-histone chromosomal proteins (HMGB1 and HMGB2) as novel antigens of pANCA and discovered anti-HMGB1/HMGB2 antibodies in sera from patients with UC [8].
Both HMGB1 and HMGB2 have strong base domains and are commonly distributed not only in the nuclei but also in the cytoplasm of eukaryotic cells, having an amino acid sequence homology of approximately 81% [9, 10].
HMGB1 and HMGB2 can be assumed to play important roles based on the high homology observed among species and on their likely involvement in transcription, cell proliferation, and cell differentiation [11–14].
Though formally called HMG1 and HMG2, they are also known as HMGB1 and HMGB2 (“B” is an abbreviation for “box”), because they share a common DNA binding domain called an “HMG box” [15]. We developed an enzyme-linked immunosorbent assay (ELISA) to detect anti-HMGB1/HMGB2 antibodies and found their frequency to be 89% in autoimmune hepatitis (AIH) and 70% in primary biliary cirrhosis (PBC) [16]. Moreover, anti-HMGB1/HMGB2 antibodies were also detected at rates between 41 and 48% among patients with rheumatoid arthritis (RA), systemic lupus erythematosus (SLE), Sjögren’s syndrome, and progressive systemic sclerosis (PSS) [17, 18]. Anti-HMGB1/HMBG2 antibodies were detected in 35% of UC patients, all of whom had higher disease activity, extensive disease in the colon, and shorter periods of disease than those who were negative for these antibodies [19].
Also of interest, because the prevalence of Crohn’s disease is high among bakers [20], the yeast Saccharomyces cerevisiae has been investigated as an etiologic factor of CD. In fact, titers of anti-Saccharomyces cerevisiae antibody (ASCA) are significantly elevated in the sera of patients with Crohn’s disease [21]. ASCA is highly specific against the cell-wall mannan of Saccharomyces cerevisiae [22] and is used to diagnose CD [23].
Observations of clinical symptoms and endoscopic and pathological findings are usually required to differentiate UC and CD. A supportive differential diagnostic method has long been required, and it remains difficult to precisely diagnose many patients. Because a definitive diagnosis of IBD based solely on the presence of a single antibody is difficult, efforts are underway to differentiate UC and CD using both pANCA and ASCA [24]. Therefore, combined antibody assays would enhance the accuracy of clinical diagnoses. We therefore examined the value of anti-HMGB1/HMGB2 antibodies combined with ASCA in the sera of IBD patients to differentiate UC and CD. Moreover, we also evaluated the relationship between these antibodies and the extent of disease or disease activity.
Methods
Patients and healthy human volunteers
The subjects of this study were all the patients (except for those who refused to be enrolled in the study) who were definitely diagnosed as having IBD at the Department of Internal Medicine of the Keio University Hospital or the Department of Internal Medicine, St. Marianna University School of Medicine, during the period from February 2002 to December 2004. The diagnoses were based on clinical symptoms, laboratory data, and histopathological findings. Serum samples were obtained from 306 patients. All serum samples were separated by centrifugation within 1 h of collection and stored frozen at −70°C. Written, informed consent was obtained from each participant under a protocol approved by our Hospital Committee on Clinical Investigation in accordance with the Declaration of Helsinki. All serum samples were assayed in a blinded fashion.
The clinical characteristics of the patients were as follows (Table 1). UC or CD was diagnosed, based on clinical, radiographic, endoscopic, and histological findings, by established criteria [25, 26]. A total of 213 patients had UC (pancolitis type in 90, left-sided type in 82, proctitis in 37, right-sided type in 1, pouchitis in 1, and unidentified locations in 2). Eighty-six of the patients had active disease; active disease was defined as a Lichtiger score [27] of more than 4. The mean duration of the disease was 9.4 years (range 0.2–30.2 years). Forty-six patients were receiving corticosteroid treatment at the time of blood sampling.
Of the 93 patients with CD (ileitis type in 28, colitis type in 14, and ileocolitis type in 51), 26 had active disease (Crohn’s disease activity index; CDAI score more than 220) [28] and the remaining 67 were in clinical and endoscopic remission. The mean duration of disease was 9.6 years (range 0.0–41.3 years). Sixteen patients were being treated with corticosteroids at the time of blood sampling.
None of the patients had any evidence of liver disease. We also examined anti-HMGB1/2 antibodies and ASCA levels in 164 healthy human volunteers (mean age 45.8; range 18–81 years; M/F 82/82).
Indirect immunofluorescence (IIF) assay to detect ANCA
Neutrophils were isolated from peripheral blood obtained from healthy human volunteers by Ficoll density gradient centrifugation. ANCA activity was determined by IIF assay as described by Wiik [29] using the Fluoro-ANCA test (MBL, Nagoya, Japan). Briefly, cytospin preparations of human neutrophils fixed with 99% ethanol at 4°C for 5 min were incubated with sera diluted 1:10 at room temperature for 20 min and stained with fluorescein isothiocyanate (FITC)-conjugated rabbit anti-human IgG F(ab’)2 antibodies (Serotec, Oxford, UK). The slides were evaluated by fluorescence microscopy. All samples positive for perinuclear staining were retested using neutrophils fixed in formalin, instead of ethanol, to distinguish ANCA from antibodies to neutrophil nuclei [30]. Neutrophils were fixed with phosphate-buffered paraformaldehyde (4%) for 10 min and permeabilized with 99% ethanol for 2 min at room temperature. Perinuclear or nuclear staining of ethanol-fixed neutrophils and cytoplasmic staining of formalin-fixed neutrophils indicated pANCA positivity.
ELISA to detect anti-HMGB1/2 antibodies and ASCA
Anti-HMGB1/2 antibodies
We detected anti-HMGB1/2 antibodies using ready-for-use HMG-1,-2 mixture (code No. 080-07041; NIPPON GENE, Tokyo, Japan) from calf thymus, as described previously [16, 18, 19]. Briefly, HMGB-1,-2 (100 μl; 5 μg/ml in 0.1 M NaPB, pH 7.4) was placed in microtiter plates (Nunc-Immuno BreakApart Modules, Nalge Nunc International, New York, NY, USA) and incubated at 4°C overnight. Non-specific binding was blocked with 5% bovine serum albumin (BSA) in phosphate-buffered saline (PBS). Serum samples were diluted 1:51 in 0.1% BSA, and binding was detected using peroxidase-conjugated F(ab’)2 goat anti-human IgG (code No. 208; MBL). All samples were incubated at room temperature for 1 h, and the plates were washed 4 times with PBS containing 0.13% Tween 20. Antibody titers were expressed as an index, as follows: (A450 of serum − A450 of negative standard)/(A450 of positive standard − A450 of negative standard) × 100]. A level of >2 standard deviations (SD) above the mean for normal sera was regarded as positive. Anti-HMG antibody specificity was determined by competitive inhibition in an ELISA using soluble HMGB1/HMGB2. Appropriate dilutions of anti-HMG1/2 antibody-positive sera were incubated with equal volumes of HMG-1,-2 mixture (100 μg/ml) for 30 min at room temperature. Ovalbumin (100 μg/ml) was used as the control. A reduction in the optical density (OD) value of at least 30% compared to controls was considered significant inhibition.
ASCA
ASCA was quantified using ASCA IgG, IgA screen ELISA kits (lot ASCA-Ig G: 202-01, ASCA-IgA: 304-02; D-tek, Mons, Belgium). Serum (100 μl) diluted 1/51 in ready-for-use diluent was added to 96-well microtiter plates coated with S. cerevisiae mannan. The plates were covered and incubated for 30 min at room temperature. Free serum components were removed and the plates were washed 3 times with 200 μl of washing buffer before the addition of anti-human IgA or IgG antibodies conjugated with horseradish peroxidase (100 μl), which were reacted with antibodies bound specifically to the antigen. After incubation for 30 min at 37°C, free conjugates were removed and the plates were washed 5 times with 300 μl of washing buffer. Thereafter, 100 μl of substrate (3,3′,5,5′-tetramethylbenzidine in citrate buffer with hydrogen peroxide) was added and the plates were incubated for 10 min at room temperature in the dark. The enzyme reaction was stopped with 100 μl of stop solution (0.25 M sulfuric acid for IgA; 1 M sulfuric acid for IgG). The plates were read at 450 nm using a microplate reader (Tosoh, Tokyo, Japan). Diluted human sera provided by the manufacturer served as an internal control. Four calibrators (20, 40, 70, 300 U/ml), and three control samples (ASCA IgG-positive control, ASCA IgG-negative control, ASCA IgG cut-off control) were included in the IgA and IgG assays, respectively. The binding index (BI = ODsample/ODcut-off control) was calculated for quantitative evaluations. The cut-off control for the IgA assay was the 20 U/ml calibrator. The sample was considered positive at a BI ≥1.0. Additionally, IgA was quantified after calculating a standard curve from the four calibrators. Samples were considered positive at values of ≥20 U/ml. All samples were assayed in duplicate.
Statistical analysis
Sensitivity for anti-HMGB1/2 antibodies was defined as the probability of a positive result in a patient diagnosed with CD. Specificity for anti-HMGB1/2 antibodies was defined as the probability of a negative result in a patient diagnosed with UC. Sensitivity for ANCA was defined as the probability of a positive result in a patient with UC. Specificity for ANCA was defined as the probability of a negative result in a patient with CD. The positive predictive value (PPV) was defined as the proportion of patients with positive results in the disease group. The disease prevalence in the population under investigation was determined by a formula based on the Bayes’ theorem of conditional probability with the assumption that the ratios of UC and CD incidence are equivalent to prevalence. The relationships between test results and clinical parameters were evaluated using the χ2 test and the Mann–Whitney U-test. Significance was assigned to probability values of less than 0.05. Data analysis was conducted using the Statistical Package for the Biosciences (COMWORKS, Saitama, Japan).
Results
Detection of anti-HMGB1/HMGB2 antibodies
The mean and SD values of the anti-HMGB1/HMGB2 antibody titer index in the 164 healthy human volunteers were 5.0 and 5.4, respectively (6 positive, 158 negative). Therefore, the cut-off value was set at 16 (mean + 2 SD). Applying this index value to data for UC patients resulted in a sensitivity of 26.8% (57/213), specificity of 85.0%, and PPV of 80.3% (Table 2). The mean titer of anti-HMGB1/HMGB2 antibodies for 86 patients with active UC was 16.7, SD was 29.3, and the antibody positivity rate was 30% (Fig. 1). These findings did not significantly differ from those for patients in remission (15.4, 23.1, and 24%, respectively). The mean titer of anti-HMGB1/HMGB2 antibodies for 26 patients with active CD was 7.4; the SD was 5.9. For patients in remission, these values were 11.3 and 14.4, respectively (Fig. 1). These data also did not differ between patients with active disease and those in remission.
Titer of anti-high mobility group box 1 and box 2 non-histone chromosomal proteins (HMGB1/2) antibodies (Abs) in ulcerative colitis (UC) patients with active or quiescent disease state. Among 86 patients with active UC, the titer and the positivity rate of anti-HMGB1/HMGB2 antibodies did not differ significantly compared to these features in UC patients in a quiescent disease state. CD Crohn’s disease
For 22 patients with active UC treated with corticosteroid, the mean titer of anti-HMGB1/HMGB2 antibodies was 9.9, the SD was 6.4, and the positivity rate was 27% (Fig. 2), representing a significant decrease from the values for 64 patients not receiving corticosteroid treatment (19.0, 33.7, and 39%, respectively). For CD patients, corticosteroid treatment produced a significantly lower mean antibody titer (4.8; SD = 2.4) than that for the untreated patients (11.3 and 13.7, respectively; Fig. 2). These results indicate that immunosuppressive agents reduce the titers of anti-HMGB1/HMGB2 antibodies in patients with IBD, although we should have assessed the changes of the titers before and after the treatment with corticosteroids. Subsequently, we examined the consistency of pANCA positivity among patients who were positive for the anti-HMGB1/HMGB2 antibodies and found consistency in 49.1% (28 of 57 patients) of patients with UC, but in only 7.1% (1 of 14 patients) of those with CD (data not shown).
Among 22 patients with active UC who were administered corticosteroid (prednisolone; PSL), the titers of HMGB1/2 antibodies were significantly decreased compared to those in the 64 UC patients without corticosteroid treatment (left). Among 16 patients with CD who were administered corticosteroid, the titers of HMGB1/2 antibodies were significantly decreased compared to those in the 77 CD patients without corticosteroid treatment (right)
Detection of ASCA
The mean antibody titer of ASCA-IgG was 10.6 U/ml (SD was 7.1) in the healthy human volunteers (5 positive, 159 negative). The cut-off for the controls (mean + 2 SD) was 25 U/ml, which matched the detection limit (=25 U/ml) in the manufacturer’s instructions. This cut-off value gave a sensitivity for CD of 24.7%, specificity of 96.2%, and PPV of 74.2% (Table 2). In 26 patients with active disease, the mean antibody titer of ASCA was 28.6, the SD was 45.6, and the positivity rate was 22%, values which did not significantly differ from the values for 67 patients in remission (24.2, 51.0, and 26.5%, respectively; data not shown).
Evaluation of HMG and ASCA antibody positivity in various types of IBD
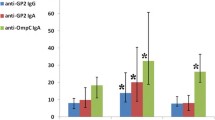
The positivity rate of anti-HMGB1/HMGB2 antibodies in UC was 27.8% in the pancolitis type, 26.8% in the left-sided type, and 21.6% in the proctitis type, indicating that the types could not be distinguished in this manner (Fig. 3). On the other hand, for CD, the positivity rate for these antibodies was 35.7% in the ileitis type, 7.1% in the colitis type, and 5.9% in the ileocolitis type. These data indicated that the positivity rate in CD patients with ileitis type (35.7%; 10 of 28 patients) was higher than that for the CD patients with ileocolitis type grouped together with those with colitis type (6.2%; 4 of 65 patients), with a significant difference of P < 0.001. The various types of CD did not show significant differences with respect to the ASCA antibody titer or with respect to the positivity rate of ASCA antibody (25.0, 21.4, and 25.5% in the ileitis type, the colitis type, and ileocolitis type, respectively) (Fig. 3). Furthermore, our studies revealed that the sensitivity, specificity, and PPV of UC with anti-HMG antibodies(+) ASCA(−) were 25.4, 87.1, and 81.8%, respectively. The sensitivity, specificity, and PPV of CD with anti-HMG antibodies(−) ASCA(+) were 22.6, 97.7, and 80.8%, respectively (Table 3).
Analysis of anti-HMGB1/HMGB2 antibodies and anti-Saccharomyces cerevisiae antibodies (ASCA) in various clinical types of inflammatory bowel disease (IBD). The positivity rates of anti-HMGB1/HMGB2 antibodies in various types of UC were 27.8, 26.8, and 21.6% in pancolitis, left-sided, and proctitis types, respectively (left). On the other hand, the positivity rates of anti-HMGB/HMGB2 antibodies in various types of CD were 35.7, 7.1, and 5.9% in the ileitis, colitis, and ileocolitis types, respectively (right). The relationships between various types of CD and ASCA findings did not differ significantly
Differential diagnosis of IBD in the colon
Of the 65 patients with CD in the colon (alternatively, colitis and ileocolitis type), 4 were positive for anti-HMGB1/HMGB2 antibodies (positivity rate of 6.2%) (Fig. 3). As a consequence, the sensitivity for anti-HMGB1/HMGB2 antibodies in UC was 26.8% and the specificity for CD in the colon was 93.8%. Moreover, of the 65 patients with CD in the colon, 16 were positive for ASCA-IgG (positivity rate of 24.6%) (Fig. 3), and the specificity for UC was 96.2%. Furthermore, of the 213 patients with UC, 54 patients were positive for anti-HMGB1/HMGB2 antibodies and negative for ASCA-IgG (positivity rate of 25.4%) (Table 4), and of the 65 patients with CD in the colon, 3 patients were positive for anti-HMGB1/HMGB2 antibodies and negative for ASCA-IgG (positivity rate of 4.6%) (Table 4). Therefore, anti-HMGB1/HMGB2 antibody positivity and ASCA-IgG negativity were significantly higher in UC patients than in patients with CD in the colon. Of the 213 UC patients, 5 patients were positive for ASCA-IgG and negative for anti-HMGB1/HMGB2 antibodies (positivity rate of 2.3%) (Table 4), and in contrast, of the 65 patients with CD in the colon, 15 patients (23.1%) were positive for ASCA-IgG and negative for anti-HMGB1/HMGB2 antibodies (Table 4). Therefore, a significantly higher percentage of patients with CD in the colon showed ASCA-IgG positivity and anti-HMGB1/HMGB2 antibodies negativity than those with UC. In addition, in the differential diagnosis of UC and CD with colitis, the sensitivity, specificity, and PPV of UC with anti-HMG antibodies(+) ASCA(−) were 25.4, 95.4, and 94.7%, and the sensitivity, specificity, and PPV of CD with anti-HMG antibodies(−) ASCA(+) were 23.1, 97.7, and 75.0, respectively (Table 4).
Discussion
Here, we evaluated a new procedure for differentially diagnosing IBD through the measurement of anti-HMGB1/HMGB2 antibodies and ASCA-IgG in the sera of IBD patients. The results indicate that CD can be differentiated from UC using the combination of measuring serum levels of anti-HMGB/HMGB2 and ASCA-IgG. This study suggests that this approach would be valuable for reducing many interventional endoscopic and/or double-contrast X-ray examinations that are used to differentially diagnose these diseases. However, it should be noted that this approach may be appropriate for the differential diagnosis of CD and UC, but not for screening patients with IBD, as the sensitivity of this approach was quite low.
The serum autoantibody, pANCA, is effective in UC screening. However, pANCA antigens are heterogeneous and many target antigens might be involved with various IBD pathogeneses; therefore, we considered that a specific pANCA would be required to establish the significance of pANCA in IBD. Therefore, we focused on HMGB1 and HMGB2, which are the target antigens of ANCA [19], and we examined the presence of anti-HMGB1/HMGB2 antibodies and ASCA in Japanese patients with IBD. As a consequence, we obtained a higher PPV by the present approach, using the combination of measuring anti-HMGB1/HMGB 2 antibodies and ASCA, as compared to previous studies [23]. However, only one patient with pouchitis was enrolled in this study, and patients with total colectomy and without pouchitis were not enrolled. Therefore, we could not determine the impact of surgical resection in this study. Further study will be needed to address this issue.
We found that the the positivity rates of anti-HMGB1/HMGB2 antibodies and ASCA-IgG were 26.8 and 3.8%, respectively, in patients with UC, compared to 15.1 and 25% in those with CD. The positivity rates for ASCA-IgG and the antibody titer in Japanese CD patients were lower than those in CD patients in western countries (positive rate of about 60%). The antigen for ASCA-IgG is mannan-peptose, a membranous polysaccharide found on the surface of the yeast cell membrane. Because glycoproteins are also present in humans, the immunogen for ASCA might be something other than mannan-peptose [22]. However, mannan is antigenic even when ingested as food, because polysaccharides remain stable after heating. A diet free of mannan is essential to maintaining the remission stage of Crohn’s disease, which suggests that mannan polysaccharide is the cause of CD [23, 31]. The fact that the Japanese, who typically eat rice rather than bread, have lower ASCA titers than westerners [32] is noteworthy, and suggests that food ingredients are critical in the management of IBD.
Though the positivity rate of ASCA-IgG was not high in our Japanese CD patients, we surmised that this test might efficiently diagnose CD due to the high positive predictive value of 74.2% and superior specificity toward CD.
The positivity rate of anti-HMGB/HMGB2 antibodies in UC patients in our study was lower than that of pANCA (positivity rate of pANCA, 36%) [1, 33]. This is because the target antigens of pANCA are heterogeneous, and HMGB1/HMGB2 are only two of many target antigens. Moreover, steroid treatment may have decreased the antibody titer of anti-HMGB1/HMGB2 antibodies in our patients with active CD and UC (Fig. 2).
Previous reports indicate that the positivity rates of ASCA are higher in patients with ileocolitis and ileitis than in patients with colitis [24, 34, 35], but we demonstrated that the positivity rates of ASCA in the ileocolitis, ileitis, and the colitis types of CD did not differ. Classifying UC and CD patients into subgroups according to the extent of disease to evaluate therelationship of disease extent with anti-HMGB1/HMGB2 antibodies and ASCA showed a relatively high rate of anti-HMGB1/HMGB2 antibodies in the ileitis type of CD (35.7%) and an extremely low rate in the colitis and ileocolitis types (6.2%). This is the first report to show a clear difference in the rates of anti-HMGB1/HMGB2 antibodies detected in CD patients with different disease types. Further, the IgG ASCA binding index was reported to be significantly lower in patients with CD who were taking mesalazine than in those not taking the drug [36]. It was previously reported that ASCA was present in 31.3% of CD patients before clinical diagnosis [37]. Indeterminate colitis is defined as a case in which a definitive diagnosis of UC or CD cannot be made at colonoscopy, in colonic biopsies, or in the colectomy specimen. Furthermore, we have previously confirmed that, in 17 patients with other colitis (infectious colitis, diverticulitis, and intestinal Behcet’s disease), anti-HMGB1/HMGB2 antibodies and ASCA were not detectable.
Estimated range of the corresponding antigens is IF-ANCA (immunofluorescence assay) ≥ pANCA (immunofluorescence assay) ≥ anti-HMGB1/HMGB2 antibodies. We found that the positivity rate followed this order for all UC disease types (data not shown) and for patients with CD in the colon. However, the positivity rate of anti-HMGB1/HMGB2 antibodies was higher than those of IF-ANCA and pANCA in the ileitis type of CD, suggesting a unique distribution. We therefore calculated the consistency of the positive ANCA rates in all samples that were positive for anti-HMGB1/HMGB2 antibodies. The results showed that in UC and CD patients positive for anti-HMGB/HMGB2 antibodies, consistency with pANCA was 49.1 and 7.1%, respectively (data not shown).
While UC and CD are completely different diseases, distinguishing them in the clinical setting can be difficult when the disease is located in the colon. Cytapheresis or surgery for difficult UC cases, and an elemental diet for CD, using amino acids or infliximab (an anti-tumor necrosis factor [TNF]-α antibody), are frequently used for patients in Japan. Relying on conventional diagnostic methods such as endoscopic and pathological findings to determine a treatment plan at an early stage does not yield optimal results. Thus, a new procedure to support differential diagnosis has been required. Our proposed assay for the presence of anti-HMGB1/HMGB2 antibodies combined with ASCA-IgG can support the differential diagnosis of UC and CD and thus has significant clinical potential. For CD, the specificity of anti-HMGB1/HMGB2 was 85.0%; for UC, the specificity of ASCA was 96.2%. The prevalence of patients with anti-HMGB1/HMGB2 antibodies (+) and ASCA-IgG(−) for UC was effective for distinguishing between UC and CD, especially for CD in the colon. The prevalence of patients with anti-HMGB1/HMGB2 antibodies(−) and ASCA-IgG(+) for CD was also effective in distinguishing these diseases. Thus, anti-HMGB1/HMGB2 antibodies combined with ASCA may be an effective diagnostic marker for discriminating between CD in the colon and UC.
One study has shown that pANCA cross-reacts with Bacteroides caccae and Escherichia coli [38] and that the production of pANCA might be associated with an abnormal immune response to bacteria in the intestinal tract. Moreover, patients who are positive for pANCA are more likely to be difficult to treat or to have serious symptoms, and patients with UC together with high pANCA levels have a higher probability of developing pouchitis after colectomy compared to those who are negative for pANCA [39].
The role of HMGB1/HMGB2 in the pathogenesis of IBD has not been demonstrated and requires further investigation. Anti-HMGB1/HMGB2 antibodies combined with ASCA could be a candidate diagnostic marker for discriminating between CD in the colon and UC.
References
Hibi T, Ohara M, Kobayashi K, Brown WR, Toda K, Takaishi H, et al. Enzyme linked immunosorbent assay (ELISA) and immunoprecipitation studies on anti-goblet cell antibody using a mucin producing cell line in patients with inflammatory bowel disease. Gut. 1994;35:224–30.
Takaishi H, Ohara S, Hotta K, Yajima T, Kanai T, Inoue N, et al. Circulating autoantibodies against purified colonic mucin in ulcerative colitis. J Gastroenterol. 2000;35:20–7.
Das KM, Dasgupta A, Mandal A, Geng X. Autoimmunity to cytoskeletal protein tropomyosin. A clue to the pathogenetic mechanism for ulcerative colitis. J Immunol. 1993;150:2487–93.
Duerr RH, Targan SR, Landers CJ, Sutherland LR, Shanahan F. Anti-neutrophil cytoplasmic antibodies in ulcerative colitis. Comparison with other colitides/diarrheal illnesses. Gastroenterology. 1991;100:1590–6.
Lassoued S, Sixou L, Oksman F, Pages M, Fournie A. Antineutrophil cytoplasmic antibodies and antibodies to myeloperoxidase in rheumatoid arthritis. Arthritis Rheum. 1991;34:1069–70.
Halbwachs-Mecarelli L, Nusbaum P, Noel LH, Reumaux D, Erlinger S, Grunfeld JP, et al. Antineutrophil cytoplasmic antibodies (ANCA) directed against cathepsin G in ulcerative colitis, Crohn’s disease and primary sclerosing cholangitis. Clin Exp Immunol. 1992;90:79–84.
Goldschmeding R, van der Schoot CE, ten Bokkel Huinink D, Hack CE, van den Ende ME, Kallenberg CG, et al. Wegener’s granulomatosis autoantibodies identify a novel diisopropylfluorophosphate-binding protein in the lysosomes of normal human neutrophils. J Clin Invest. 1989;84:1577–87.
Sobajima J, Ozaki S, Osakada F, Uesugi H, Shirakawa H, Yoshida M, et al. Novel autoantigens of perinuclear anti-neutrophil cytoplasmic antibodies (P-ANCA) in ulcerative colitis: non-histone chromosomal proteins, HMG1 and HMG2. Clin Exp Immunol. 1997;107:135–40.
Lotze MT, Tracey KJ. High-mobility group box 1 protein (HMGB1): nuclear weapon in the immune arsenal. Nat Rev Immunol. 2005;5:331–42.
Muller S, Ronfani L, Bianchi ME. Regulated expression and subcellular localization of HMGB1, a chromatin protein with a cytokine function. J Intern Med. 2004;255:332–43.
Waga S, Mizuno S, Yoshida M. Chromosomal protein HMG1 removes the transcriptional block caused by the cruciform in supercoiled DNA. J Biol Chem. 1990;265:19424–8.
Shirakawa H, Tsuda K, Yoshida M. Primary structure of non-histone chromosomal protein HMG2 revealed by the nucleotide sequence. Biochemistry. 1990;29:4419–23.
Melloni E, Sparatore B, Patrone M, Pessino A, Passalacqua M, Pontremoli S. Extracellular release of the ‘differentiation enhancing factor’, a HMG1 protein type, is an early step in murine erythroleukemia cell differentiation. FEBS Lett. 1995;368:466–70.
Passalacqua M, Zicca A, Sparatore B, Patrone M, Melloni E, Pontremoli S. Secretion and binding of HMG1 protein to the external surface of the membrane are required for murine erythroleukemia cell differentiation. FEBS Lett. 1997;400:275–9.
Weir HM, Kraulis PJ, Hill CS, Raine AR, Laue ED, Thomas JO. Structure of the HMG box motif in the B-domain of HMG1. EMBO J. 1993;12:1311–9.
Sobajima J, Ozaki S, Uesugi H, Osakada F, Inoue M, Fukuda Y, et al. High mobility group (HMG) non-histone chromosomal proteins HMG1 and HMG2 are significant target antigens of perinuclear anti-neutrophil cytoplasmic antibodies in autoimmune hepatitis. Gut. 1999;44:867–73.
Andersson U, Erlandsson-Harris H. HMGB1 is a potent trigger of arthritis. J Intern Med. 2004;255:344–50.
Uesugi H, Ozaki S, Sobajima J, Osakada F, Shirakawa H, Yoshida M, et al. Prevalence and characterization of novel pANCA, antibodies to the high mobility group non-histone chromosomal proteins HMG1 and HMG2, in systemic rheumatic diseases. J Rheumatol. 1998;25:703–9.
Sobajima J, Ozaki S, Uesugi H, Osakada F, Shirakawa H, Yoshida M, et al. Prevalence and characterization of perinuclear anti-neutrophil cytoplasmic antibodies (P-ANCA) directed against HMG1 and HMG2 in ulcerative colitis (UC). Clin Exp Immunol. 1998;111:402–7.
Sonnenberg A. Occupational mortality of inflammatory bowel disease. Digestion. 1990;46:10–8.
Main J, McKenzie H, Yeaman GR, Kerr MA, Robson D, Pennington CR, et al. Antibody to Saccharomyces cerevisiae (bakers’ yeast) in Crohn’s disease. BMJ. 1988;297:1105–6.
Sendid B, Colombel JF, Jacquinot PM, Faille C, Fruit J, Cortot A, et al. Specific antibody response to oligomannosidic epitopes in Crohn’s disease. Clin Diagn Lab Immunol. 1996;3:219–26.
Joossens S, Reinisch W, Vermeire S, Sendid B, Poulain D, Peeters M, Geboes K, Bossuyt X, Vandewalle P, Oberhuber G, Vogelsang H, Rutgeerts P, Colombel JF. The value of serologic markers in indeterminate colitis: a prospective follow-up study. Gastroenterology. 2002;122:1242–7.
Quinton JF, Sendid B, Reumaux D, Duthilleul P, Cortot A, Grandbastien B, et al. Anti-Saccharomyces cerevisiae mannan antibodies combined with antineutrophil cytoplasmic autoantibodies in inflammatory bowel disease: prevalence and diagnostic role. Gut. 1998;42:788–91.
Lennard-Jones JE. Classification of inflammatory bowel disease. Scand J Gastroenterol Suppl. 1989;170:2–6. (discussion 16–9).
Marion JF, Rubin PH, Present DH. Differential diagnosis of chronic ulcerative colitis and Crohn’s disease. In: Kirsner JB, editor. Inflammatory bowel disease. 5th ed. Philadelphia: WB Sauders; 2000.
Lichtiger S, Present DH, Kornbluth A, Gelernt I, Bauer J, Galler G, et al. Cyclosporine in severe ulcerative colitis refractory to steroid therapy. N Engl J Med. 1994;330:1841–5.
Winship DH, Summers RW, Singleton JW, Best WR, Becktel JM, Lenk LF, et al. National Cooperative Crohn’s Disease Study: study design and conduct of the study. Gastroenterology. 1979;77:829–42.
Wiik A. Delineation of a standard procedure for indirect immunofluorescence detection of ANCA. APMIS Suppl. 1989;6:12–3.
Charles LA, Falk RJ, Jennette JC. Reactivity of antineutrophil cytoplasmic autoantibodies with mononuclear phagocytes. J Leukoc Biol. 1992;51:65–8.
Barclay GR, McKenzie H, Pennington J, Parratt D, Pennington CR. The effect of dietary yeast on the activity of stable chronic Crohn’s disease. Scand J Gastroenterol. 1992;27:196–200.
Hisabe T, Matsui T, Sakurai T, Murakami Y, Tanabe H, Matake H, et al. Anti-Saccharomyces cerevisiae antibodies in Japanese patients with inflammatory bowel disease: diagnostic accuracy and clinical value. J Gastroenterol. 2003;38:121–6.
Sugi K, Saitoh O, Matsuse R, Tabata K, Uchida K, Kojima K, et al. Antineutrophil cytoplasmic antibodies in Japanese patients with inflammatory bowel disease: prevalence and recognition of putative antigens. Am J Gastroenterol. 1999;94:1304–12.
Giaffer MH, Clark A, Holdsworth CD. Antibodies to Saccharomyces cerevisiae in patients with Crohn’s disease and their possible pathogenic importance. Gut. 1992;33:1071–5.
Standaert-Vitse A, Jouault T, Vandewalle P, Mille C, Seddik M, Sendid B, et al. Candida albicans is an immunogen for anti-Saccharomyces cerevisiae antibody markers of Crohn’s disease. Gastroenterology. 2006;130:1764–75.
Oshitani N, Hato F, Matsumoto T, Jinno Y, Sawa Y, Hara J, et al. Decreased anti-Saccharomyces cerevisiae antibody titer by mesalazine in patients with Crohn’s disease. J Gastroenterol Hepatol. 2000;15:1400–3.
Israeli E, Grotto I, Gilburd B, Balicer RD, Goldin E, Wiik A, et al. Anti-Saccharomyces cerevisiae and antineutrophil cytoplasmic antibodies as predictors of inflammatory bowel disease. Gut. 2005;54:1232–6.
Cohavy O, Bruckner D, Gordon LK, Misra R, Wei B, Eggena ME, et al. Colonic bacteria express an ulcerative colitis pANCA-related protein epitope. Infect Immun. 2000;68:1542–8.
Fleshner PR, Vasiliauskas EA, Kam LY, Fleshner NE, Gaiennie J, Abreu-Martin MT, et al. High level perinuclear antineutrophil cytoplasmic antibody (pANCA) in ulcerative colitis patients before colectomy predicts the development of chronic pouchitis after ileal pouch-anal anastomosis. Gut. 2001;49:671–7.
Acknowledgments
This work was supported by a grant from MBL Co.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Takaishi, H., Kanai, T., Nakazawa, A. et al. Anti-high mobility group box 1 and box 2 non-histone chromosomal proteins (HMGB1/HMGB2) antibodies and anti-Saccharomyces cerevisiae antibodies (ASCA): accuracy in differentially diagnosing UC and CD and correlation with inflammatory bowel disease phenotype. J Gastroenterol 47, 969–977 (2012). https://doi.org/10.1007/s00535-012-0566-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-012-0566-3