Abstract
Purpose
Seventeen thousand patients receive treatment with radical pelvic radiotherapy annually in the UK. Up to 50% develop significant gastrointestinal symptoms. The National Cancer Survivorship Initiative has identified access to specialist medical care for those with complications after cancer as one of their four key needs. We aimed to determine the current practice of British gastroenterologists with regards to chronic gastrointestinal symptoms after pelvic radiotherapy.
Methods
A questionnaire was developed and sent up to a maximum of five times to all UK consultant gastroenterologists.
Results
Eight hundred sixty-six gastroenterologists were approached and 165 (20%) responded. Sixty-one percent saw one to four patients annually with bowel symptoms after radiotherapy. Eighteen percent rate the current treatments as effective “often” or “most of the time”. Forty-seven percent of gastroenterologists consider themselves “confident with basic cases”, with 11% “confident in all cases”. Fifty-nine percent thinks a gastroenterologist with a specialist interest should manage these patients. Although only 29% thinks a specific service is required for these patients, 34% rates the current service as inadequate. The ideal service was considered to be gastroenterology-led, multidisciplinary and regional. Low referral rates, poor evidence-base and poor funding are cited as reasons for the current patchy services.
Conclusions
The low response rate contrasts with that from a parallel survey of clinical oncologists. This may reflect the opinion that radiation-induced bowel toxicity is not a significant issue, which may be because only a small proportion of patients are referred to gastroenterologists. The development of new, evidence-based gastroenterology-led services is considered the optimal way to meet the needs of these patients.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Seventeen thousand patients per year are treated with radical pelvic radiotherapy in the UK [1]. Survival is improving [2–4]. In parallel to improved survival and cure, there has been an increase in chronic side effects of treatment, including gastrointestinal damage [5, 6]. The chronic side effects of radiotherapy also include bladder, bone and sexual dysfunction, but bowel symptoms have the greatest impact on quality of life [7].
The published incidence varies from 2% to 30% for rectal toxicity [8] and 5% to 15% for chronic radiation damage to the GI tract outside the rectum [9, 10], although recent published data suggest that radiation injury is rarely focal and often involves much more extensive changes than are frequently described [11]. The true extent of chronic gastrointestinal toxicity is underestimated [12]. Up to 90% of patients develop a permanent change in bowel habit after pelvic radiotherapy and in 50% of patients this adversely affects quality of life [13].
Bowel symptoms after pelvic radiotherapy do not necessarily equate to late radiation toxicity, with one third of patients having a diagnosis unrelated to the previous radiotherapy [14]. Twelve percent have either a recurrent malignancy or a new secondary tumour [14]. More than half of patients have two or more separate diagnoses causing their symptoms [14]. The underlying diagnoses are often easily treatable, e.g. lactose intolerance, bile acid malabsorption, small bowel bacterial overgrowth, drug-induced diarrhoea or thyroid dysfunction [13]. In fact, gastroenterological assessment of these patients alters diagnosis in 64%, with curative therapy available for 27% of patients [15].
The UK Cancer Plan (2000) raised the standards of cancer treatment on a national level and improved outcomes for patients diagnosed with cancer through a multidisciplinary structured approach. Unfortunately, this has not been extended to patients with chronic, often complex, complications of their cancer treatment. The National Cancer Survivorship Initiative (2008) and the Survivorship Vision (2010), part of the Cancer Reform Strategy (2007), has identified access to specialist care for complications of cancer treatment as one of the four key needs of cancer survivors. However, these patients continue to receive suboptimal care due to a combination of poor patient reporting [16], poor clinician recognition [17], lack of GI specialists or expertise [11] and therapeutic nihilism [18].
We aimed to determine the current practice and opinion of British gastroenterologists with respect to the management of and services available to patients who develop chronic bowel symptoms, defined as symptoms which are present at least 6 months following pelvic radiotherapy. This group was chosen as gastroenterologists are not routinely involved in the management of acute gastrointestinal symptoms related to cancer treatments.
Methods
A questionnaire was developed with input from gastroenterologists and clinical oncologists with expertise in chronic side effects of radiotherapy. It comprised five sections including demographic data, referral patterns, management strategy, confidence in management and service provision. This was sent to all consultant gastroenterologists in the UK who are members of the British Society of Gastroenterology. Those who were exclusively academic or those with a purely hepatological practice were excluded.
Survey participants were divided into two groups: those with email addresses (701) and those without email addresses (165). Those with email addresses were sent the survey electronically using survey monkey by sending an email with the survey link. If the recipient did not respond, the email was sent again up to a maximum of three times. If there was still no response, the survey was posted out up to a maximum of two times. Those without an email address were sent a paper questionnaire with a stamped addressed envelope up to a maximum of two times. The time period between each time the survey was sent out was 15–20 days. The survey was conducted between December 2009 and April 2010.
Statistical methods
Data was analysed using SPSS version 16. The majority of the results are expressed as simple frequencies, with percentages quoted as part of the whole group (n = 165), or as part of a subgroup as stated. Qualitative data are reported by identifying key themes and reporting direct quotes.
As this was a survey of clinicians’ views, there were no ethical implications, and as such, ethics committee approval was not sought.
Results
Eight hundred sixty-six gastroenterologists were identified in the UK. One hundred sixty-five responses (20%) were received.
Background data
One hundred fifty-six respondents (96%) reported that they treat luminal gastrointestinal disease. Twenty-six (16%) do not see any patients with radiation-induced symptoms. The reported number of patients seen annually with GI symptoms following pelvic radiotherapy is shown in Fig. 1. Of note, only five (3%) gastroenterologists report being referred more than 20 such patients per year.
Referral patterns and management strategy
Gastroenterologists receive referrals from numerous sources. Seventy-one (43%) receive referrals from oncologists and 111 (67%) receive them directly from GPs. Referrals are also reported from colorectal surgeons by 71 (43%), urologists by 28 (17%) and gynaecologists by 53 (32%). The most frequent referral symptoms are stool frequency (116, 70%), rectal bleeding (115, 70%), urgency (108, 66%), loose stool (87, 53%) and faecal incontinence (74, 45%). The symptoms these patients have when referred is shown in Fig. 2.
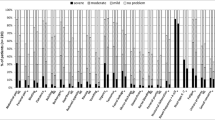
The investigations requested by gastroenterologists are shown in Fig. 3. A wide variety of treatments are prescribed by gastroenterologists to treat bowel symptoms in this patient population (Fig. 4). Only 22 (13%) rate currently available treatments as effective “often” and 8 (5%) “most of the time”. Ninety-six (58%) think the treatments are effective sometimes with 12 (7%) only considering them effective “rarely”.
Confidence in management
Gastroenterologists were asked to choose the statement that best described their confidence in managing patients with late-onset bowel symptoms after pelvic radiotherapy. Forty (24%) stated that they were “somewhat confident, but have minimal experience”. Seventy-seven (47%) consider themselves “confident with basic cases, but would need sub-speciality advise with more complex cases”, with 19 (11%) “confident in all cases” and considered themselves to have a specialist interest in this area. Five (3%) felt they were “not at all confident with no experience”.
Service provision
Ninety-seven (59%) respondents think that a gastroenterologist with a specialist interest should ideally manage these patients. Thirty-one (19%) stated that they should be managed by a general gastroenterologist and 10 (6%) stated that they should be managed by a GI surgeon with a specialist interest. However, only 31 (19%) have a gastroenterologist or GI surgeon with a specialist interest in their area.
Forty-eight (29%) think that a specific service is required for this patient group, with 65 (39%) stating that they do not know whether or not one is required. Seventy (42%) gastroenterologists rate the current service as “adequate”, whereas 56 (34%) rate it as “poor” or “fails to meet the needs of patients”. Only 12 (7%) think the service is “good”.
The ideal components of a service
The key themes emerging from this open question regarding the ideal components of a service are listed in Table 1. Table 2 shows direct quotations.
Most of those surveyed felt there should be a multidisciplinary service led by a gastroenterologist with a specialist interest, with specialist nurse and dietician support and good links to clinical oncologists, colorectal surgeons and a nutrition team. Many felt that this should be a regional, tertiary service to enable rapid access to the whole range of diagnostic and therapeutic modalities required. It should disseminate information on management and be a hub of expertise, education and research. They also specifically mentioned the need for adequate resources to fund the service.
Care and management of patients
The key themes emerging from this open question about the current care and management of this patient group are listed in Table 1. Table 2 shows direct quotations.
The current care and management is felt by many to be poor and inconsistent, with a lack of awareness of the importance and significance of this clinical scenario amongst gastroenterologists. Many state that, although there is a large cohort of patients affected, they think that chronic GI side effects of pelvic radiotherapy are not reported, recognised or referred. This may explain why some responding gastroenterologists report that they do not feel it is a significant issue. They also report that paucity of evidence and emphasis on the symptom of rectal bleeding may be compromising the standard of management for this patient group. One respondent stated that they had tried to set up a specific service to improve the management of these patients, but no funding was provided.
Discussion
Although up to 50% of patients treated with pelvic radiotherapy develop significant chronic bowel symptoms, which equates to twice the number of patients diagnosed annually with Crohn’s disease [11], this survey of British gastroenterologists had a low response rate. This is in contrast to a high response rate (61%) from a parallel survey of clinical oncologists [18] and may reflect the opinion amongst some gastroenterologists that this is not common or relevant clinical scenario.
Only a small proportion of affected patients are referred for gastroenterological evaluation and many gastroenterologists do not feel confident in managing them. This may reflect the lack of established routes of referral, lack of services and available expertise and poor communication. Treatments known to be ineffective are often prescribed, and investigations for common diagnoses following radiotherapy are not often used. This may reflect poor access to the necessary diagnostic tools and treatments in clinical practice, and may contribute to the opinion that treatments are ineffective. Low referral rates may also be compounding the perception that this is not a widespread or significant clinical problem.
The most common symptoms that gastroenterologists report as a reason for referral are frequency, urgency, loose stool and rectal bleeding. Tests for bile acid malabsorption, lactose intolerance and small bowel bacterial overgrowth are not commonly used despite the fact that these are common causes for these symptoms following pelvic radiotherapy [14, 18–23]. The most commonly used treatments are anti-diarrhoeal agents. Whilst this medication does have a role in symptomatic treatment, it should not replace systematic investigation to identify underlying GI diagnoses. Other commonly used treatments are rectal steroids and 5ASAs, for which there is no good evidence for use in the management of radiation-related GI injury [24–26].
The management practice elicited from this survey raises the issue of training for both clinical oncologists and gastroenterologists. Education could raise the standards of management generally and greater emphasis on the consequences of cancer treatments during higher specialist training would comprehensively address this shortfall in knowledge in the future. This is particularly important given there are two million cancer survivors in the UK and this number is increasing at a rate of 3% per annum [27].
Many gastroenterologists consider that specialist gastroenterology-led multidisciplinary services are required to meet the needs of this patient group and are dissatisfied with the quality of current services:
There is a large group of patients out there who do not even get referred to the right people and their suffering goes unrecognised and their needs remain unmet
This is in keeping with British clinical oncologists, as demonstrated in a parallel survey, which showed that 75% of oncologists think that a gastroenterologist with a specialist interest should manage these patients, 65% think a specific service is required and 52% rate the current service as inadequate [18].
In comparison to a survey of British gastroenterologists in 2003 [15] which had a 50% response rate, the findings concurred in many respects. Most gastroenterologists surveyed in 2003 saw a median of 3 patients per year and only 18% felt they could often help patients. Whilst this may initially seem disheartening, there is an increasing momentum at a national level with the National Cancer Survivorship Initiative (2008), increasing recognition amongst clinical oncologists and the development of local patient user groups.
This survey focuses specifically on the management of gastrointestinal symptoms following pelvic radiotherapy. There are very few services available currently in the UK for consequences of pelvic radiotherapy and several potential models could be implemented. It is likely that the model of care used would need to be tailored to regional need. One of the few designated services for pelvic radiation disease in the UK is based at the Royal Marsden Hospital, but it is unlikely that this model of care could be effectively exported to a more rural region of the UK. There is also a paucity of services for other consequences of pelvic radiotherapy including bladder dysfunction. Patients with urological malignancies often have follow-up with urological surgeons, but otherwise there are few models of care on which to base a new gastroenterology service.
Whilst this survey begins to highlight some of the issues regarding the current management of patients who develop chronic gastrointestinal symptoms following pelvic radiotherapy, several questions remain. The current literature clearly demonstrates that the quality of life and social functioning of patients is adversely affected by GI symptoms following pelvic radiotherapy [13, 28, 29]. It has also been demonstrated that patients do not always volunteer information about symptoms, often considering them inevitable consequences of treatment or age and that there is nothing that can be done [16, 30]. However, the effect of improved gastroenterological services to manage these symptoms on patients’ quality of life and patient satisfaction has not yet been adequately addressed. Also, we do not currently have clear criteria to identify which patients require gastroenterology assessment. Whilst it is likely that all patients with GI symptoms would benefit from specialist evaluation, this may not be realistic in the current economic climate. Further work is needed to identify which patients should be referred and methods of risk stratification. Other models of providing services for this patient group are currently being investigated, including the possibility of care being provided by specialist nurses alongside physicians [31].
Limitations
There was a low response rate to this survey, despite sending it up to five times in both paper and electronic form. This raises the potential for systematic bias, particularly non-respondent bias, i.e. those who responded are likely to be those most interested in this subject and may not accurately reflect the opinions of all British gastroenterologists. However, the opinions expressed in the survey were not uniform and included a minority of people who do not feel that chronic bowel symptoms after pelvic radiotherapy are a significant or relevant problem. Another issue may have been the initial questions on the survey regarding personal details of the respondents. Although this was optional, it may have raised concerns in some potential respondents regarding anonymity.
The questionnaire was developed with input from clinical oncologists and gastroenterologists with expertise in the side effects of radiotherapy. It is, however, not a validated tool and was developed specifically to gauge current practice and opinion. Given that this is not a prospective study reporting actual practice, it is a survey establishing reported practice, it is possible that some of the results may reflect what gastroenterologists think is happening, as opposed to what is actually happening.
Conclusions
Gastroenterological assessment is necessary to effectively manage patients who develop gastrointestinal symptoms after pelvic radiotherapy [11]; however, currently services and specialist expertise are sparse. Better communication between clinical oncologists and gastroenterologists will enable appropriate services to be developed which satisfy the needs of both clinicians and this often overlooked patient group.
References
West CML, Davidson SE (2009) Measurement tools for gastrointestinal symptoms in radiation oncology. Curr Opin Support Palliat Care 3(1):36–40
Vale CL, Tierney JF, Davidson SE, Drinkwater KJ, Symonds P (2010) Substantial improvement in UK cervical cancer survival with chemoradiotherapy: results of a royal college of radiologists’ audit. Clin Oncol 22(7):590–601
Ryu H-S, Chun M, Chang K-H, Chang H-J, Lee J-P (2005) Postoperative adjuvant concurrent chemoradiotherapy improves survival rates for high-risk, early stage cervical cancer patients. Gynecol Oncol 96(2):490–495
Green JA, Kirwan JM, Tierney JF, Symonds P, Fresco L, Collingwood M, Williams CJ (2001) Survival and recurrence after concomitant chemotherapy and radiotherapy for cancer of the uterine cervix: a systematic review and meta-analysis. Lancet 358(9284):781–786
Creutzberg CL, van Putten WLJ, Koper PCM, Lybeert MLM, Jobsen JJ, Wárlám-Rodenhuis CC, De Winter KAJ, Lutgens LCHW, van den Bergh ACM, van de Steen-Banasik E, Beerman H, van Lent M (2000) Surgery and postoperative radiotherapy versus surgery alone for patients with stage-1 endometrial carcinoma: multicentre randomised trial. Lancet 355(9213):1404–1411
Landoni F, Maneo A, Colombo A, Placa F, Milani R, Perego P, Favini G, Ferri L, Mangioni C (1997) Randomised study of radical surgery versus radiotherapy for stage Ib-IIa cervical cancer. Lancet 350(9077):535–540
Bergmark K, AVall-Lundqvist E, Dickman PW, Henningsohn L, Steineck G (2002) Patient-rating of distressful symptoms after treatment for early cervical cancer. Acta Obstet Gynecol Scand 81(5):443–450
Denham JW, O'Brien PC, Dunstan RH, Johansen J, See A, Hamilton CS, Bydder S, Wright S (1999) Is there more than one late radiation proctitis syndrome? Radiother Oncol 51(1):43–53
DeCosse JJ, Rhodes RS, Wentz WB, Reagan JW, Dworken HJ, Holden WD (1969) The natural history and management of radiation induced injury of the gastrointestinal tract. Ann Surg 170(3):369–384
Schofield PF, Holden D, Carr ND (1983) Bowel disease after radiotherapy. J R Soc Med 76(6):463–466
Andreyev HJN, Wotherspoon A, Denham JW, Hauer-Jensen M (2010) Defining pelvic-radiation disease for the survivorship era. Lancet Oncol 11(4):310–312
Davidson SE, Trotti A, Ataman ÖU, Seong J, Lau FN, da Motta NW, Jeremic B (2007) Improving the capture of adverse event data in clinical trials: the role of the International Atomic Energy Agency. Int J Radiat Oncol Biol Phys 69(4):1218–1221
Andreyev J (2007) Gastrointestinal symptoms after pelvic radiotherapy: a new understanding to improve management of symptomatic patients. Lancet Oncol 8(11):1007–1017
Andreyev HJN, Vlavianos P, Blake P, Dearnaley D, Norman AR, Tait D (2005) Gastrointestinal symptoms after pelvic radiotherapy: role for the gastroenterologist? Int J Radiat Oncol Biol Phys 62(5):1464–1471
Andreyev HJN, Amin Z, Blake P, Dearnaley D, Henry M, Tait D, Vlavianos P (2003) GI symptoms developing after pelvic radiotherapy require gastroenterological review but is this happening in the UK? Clin Oncol 15(2):S12
Faithfull S (1995) ‘Just grin and bear it and hope that it will go away’: coping with urinary symptoms from pelvic radiotherapy. Eur J Cancer Care 4(4):158–165
Putta S, Andreyev HJ (2005) Faecal incontinence: a late side-effect of pelvic radiotherapy. Clin Oncol 17(6):469–477
Henson C, Andreyev HJN, Symonds RP, Peel D, Swindell R, Davidson SE (2011) Late onset bowel dysfunction post-pelvic radiotherapy: a national survey of current practice and opinions of clinical oncologists. Clin Oncol 23:552–557
Ludgate SM, Merrick MV (1985) The pathogenesis of post-irradiation chronic diarrhoea: measurement of SeHCAT and B12 absorption for differential diagnosis determines treatment. Clin Radiol 36(3):275–278
Arlow FL, Dekovich AA, Priest RJ, Beher WT (1987) Bile acids in radiation-induced diarrhea. South Med J 80(10):1259–1261
Danielsson A, Nyhlin H, Persson H, Stendahl U, Stenling R, Suhr O (1991) Chronic diarrhoea after radiotherapy for gynaecological cancer: occurrence and aetiology. Gut 32(10):1180–1187
Ford GA, Preece JD, Davies IH, Wilkinson SP (1992) Use of the SeHCAT test in the investigation of diarrhoea. Postgrad Med J 68(798):272–276
Beer WH, Fan A, Halsted CH (1985) Clinical and nutritional implications of radiation enteritis. Am J Clin Nutr 41(1):85–91
Rougier P, Zimmermann P, Pignon JP, Kac J, Crespon B, Zrihen E, Charbit M, Gerbaulet A, Eschwege F (1992) Radiation proctitis: compared efficacy of two corticosteroids enemas. Med Chir Dig 21(2):91–93
Kochhar R, Patel F, Dhar A, Sharma SC, Ayyagari S, Aggarwal R, Goenka MK, Gupta BD, Mehta SK (1991) Radiation-induced proctosigmoiditis. Prospective, randomized, double-blind controlled trial of oral sulfasalazine plus rectal steroids versus rectal sucralfate. Dig Dis Sci 36(1):103–107
Cavcic J, Turcić J, Martinac P, Jelincić Z, Zupancić B, Panijan-Pezerović R, Unusić J (2000) Metronidazole in the treatment of chronic radiation proctitis: clinical trial. Croat Med Journal 41:314–318
Maddams J, Brewster D, Gavin A, Steward J, Elliott J, Utley M, Moller H (2009) Cancer prevelence in the United Kingdom: estimates for 2008. Br J Cancer 101(3):541–547
De Meerleer G, Vakaet L, Meersschout S, Villeirs G, Verbaeys A, Oosterlinck W, De Neve W (2004) Intensity-modulated radiotherapy as primary treatment for prostate cancer: acute toxicity in 114 patients. Int J Radiat Oncol Biol Phys 60(3):777–787
Henderson A, Ismail AK, Cunningham M, Aldridge S, Loverock L, Langley SE, Laing RW (2004) Toxicity and early biochemical outcomes from 125iodine prostate brachytherapy in the UK. A prospective study. Clin Oncol (R Coll Radiol) 16(2):95–104
Hackett C (2005) Pelvic radiotherapy and GI side effects: Hobson’s choice? Gastrointest Nurs 3:18–24
Benton B, Norton C, Lindsay JO, Dolan S, Andreyev HJ (2011) Can nurses manage gastrointestinal symptoms arising from pelvic radiation disease? Clin Oncol 23:538–551
Acknowledgements
We acknowledge NHS funding to the NIHR Biomedical Research Centre at the Royal Marsden Hospital. The salary of the data manager is paid by a grant from the Research for Patients’ Benefit fund of the NIHR and by the Royal Marsden NHS Foundation Trust Charitable Funds. Dr Caroline Henson is funded by Macmillan Cancer Support. The authors would like to thank Ric Swindell and Mrs Rita Hannon for their help with analysis of the data.
Conflict of interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Appendix 1: Gastroenterologists’ survey
Appendix 1: Gastroenterologists’ survey



Rights and permissions
About this article
Cite this article
Henson, C.C., Davidson, S.E., Lalji, A. et al. Gastrointestinal symptoms after pelvic radiotherapy: a national survey of gastroenterologists. Support Care Cancer 20, 2129–2139 (2012). https://doi.org/10.1007/s00520-011-1323-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-011-1323-5