Abstract
Background
Obesity is an important health issue, the prevalence of which is increasing in childhood. The aim of this study was to examine urinary renal injury markers in order to determine the renal effect of obesity and its comorbidities in a pediatric population.
Methods
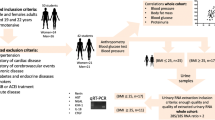
Eighty-four obese children and 64 healthy control subjects were enrolled in the study. We checked their urine using N-acetyl-beta-d-glucosaminidase (NAG), neutrophil gelatinase-associated lipocalin (NGAL), kidney injury molecule-1 (KIM-1), and microalbumin as renal injury markers. Associations of renal damage markers with hypertension, an impaired glucose tolerance test, and insulin resistance were assessed.
Results
Obese individuals had higher urinary NAG and KIM-1 values compared to those of healthy controls (p = 0.027, p = 0.026). There was no difference in urinary NGAL between obese and lean subjects (p = 0.885). Urinary renal injury markers were not statistically different in the obese group when checked for impaired glucose tolerance, insulin resistance, and hypertension (p > 0.05).
Conclusions
This study shows that urinary NAG and KIM-1 could be used as a screening method for detection of early renal damage in obese children.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Childhood obesity has become a global epidemic and is related to essential hypertension and type 2 diabetes mellitus (DM), the most important causes of end-stage renal disease [1]. With the increase in obesity, the prevalence of end-stage renal disease has also risen dramatically in the last decade [2]. One screening method used to identify high-risk patients is detection of microalbuminuria, which has been defined as an early predictor of hypertensive or diabetic nephropathy [3, 4]. Urinary albumin excretion is primarily a result of glomerular damage, but renal tubular injury and dysfunction also plays a critical role in the early increase of albumin in the urine. Recent studies indicate a growing interest regarding the contribution of renal tubulointerstitium in the pathophysiology of diabetic nephropathy. Reports in the literature show that tubular changes such as hypertrophy, reduced ion transport, and thickening of the basement membrane are already apparent before the onset of proteinuria [5, 6].
Proximal tubular cells are vulnerable to various metabolic and hemodynamic factors. Urinary enzymes are used to assess renal tubular injury [7–11]. One of the most commonly used markers is N-acetyl-beta-d-glucosaminidase (NAG), a lysosomal enzyme found in many tissue types. Its high molecular weight prevents it from passing into the glomerular ultrafiltrate and expressed urinary NAG has a renal proximal tubular origin. Urinary NAG is used to determine the extent of tubular damage caused by proteinuria, nephrolithiasis, hyperglycemia, kidney transplants, and nephrotoxic drugs [9–11].
In recent years, neutrophil gelatinase-associated lipocalcin (NGAL) and kidney injury molecule-1 (KIM-1) have emerged as promising biomarkers of acute and chronic renal injury. NGAL is a small protein belonging to the lipocalcin family and KIM-1 is a type 1 cell membrane glycoprotein. Levels of both increase in response to renal proximal tubular cell injury. These tubular damage markers have been extensively used to assess proteinuric, toxic, and ischemic kidney diseases [7, 8, 12–14].
We performed a cross-sectional study to determine the levels of these tubular markers in obese children and healthy controls. We also investigated the correlation between the renal injury markers NAG, NGAL, and KIM-1, and comorbidities of obesity including insulin resistance, impaired glucose tolerance, and hypertension. In addition, serum and urine electrolytes and microalbuminuria were checked. We specifically focused on a pediatric population to determine early renal effects of obesity. Identifying these early markers may help to assist in determining high-risk individuals and point to specific interventions to delay or prevent the development of nephropathy.
Materials and methods
The study group consisted of 84 obese individuals who were recruited from the endocrinology outpatient clinic whose ages ranged from 4 to 16 years (mean, 11.73 ± 2.3). Obesity is based on a body mass index (BMI) equal to or greater than the 95th percentile for gender and age, BMI %, and BMI standard deviation [15]. Children whose obesity was the result of a syndromal problem (Prader Willi, Laurence-Moon Biedle syndrome, etc.) were excluded, as were those whose obesity had an endocrinal cause such as Cushing’s syndrome or hypothyroidism. Those with systemic disease including liver disease, malignancy, drug use, etc., were also excluded. Standing height was measured to the nearest 0.1 cm with a Harpenden fixed stadiometer. Body weight (kg) was measured on a SECA balance scale to the nearest 0.1 kg, with each subject dressed in a light T-shirt and shorts. BMI was calculated by dividing weight in kilograms by height in meters squared (kg/m2). The control group consisted of 64 age- and gender-matched lean, normotensive healthy children who were recruited from the pediatric outpatient clinic of the same hospital and who were free of acute or chronic inflammatory illnesses. Both study and control groups were randomly selected. Fresh second-morning urine samples were collected in order to assess urine phosphorus, sodium, calcium, creatinine, albumin, NAG, NGAL, and KIM 1. Also at the same time, blood samples were collected for use in measuring fasting glucose, insulin, phosphorus, sodium, and creatinine. All tests were measured within 4 h of the sample collections, except for urinary NAG, NGAL, and KIM-1, where urine samples were centrifuged (3,000 rpm for 10 min) and stored at –80 °C until measurement. Estimated glomerular filtration rate (GFR) was calculated according to the Schwartz formula [16]. The fractional excretion of sodium (FENa) and tubular phosphorus reabsorption ratio (TPR) were calculated with standard formulas.
Oral glucose tolerance tests (OGTT) were performed on 37 obese children following overnight fasting of 12–14 h. After subjects ingested a simple carbohydrate solution equivalent to 75 g glucose, blood samples were obtained at 0, 30, 60, and 120 min. Impaired glucose tolerance was defined according to WHO criteria, i.e., a condition in which fasting blood glucose levels in venous plasma drop to <140 mg/dl and 2 h later glucose administration is maintained between 140 and 200 mg/dl [17]. Insulin resistance was estimated from fasting plasma measurements using HOMA-IR (insulin (mU/l) × glucose (mmol/l)/22.5) [18]. Insulin resistance criteria were HOMA-IR >2.5 for prepubertal children and HOMA-IR >4.0 for adolescents [19]. Hypertension was defined as blood pressure above the 95th percentile for age and height according to the National Health and Nutrition Examination Survey [20].
Urinary NGAL and KIM-1 were measured by ELISA methods (Aviscera Bioscience, Santa Clara, CA, USA) and the intra-assay precision was 4–6 and 4–8 %, respectively. The results are expressed as ng/mg creatinine. Urinary NAG was analyzed using the photometric method (Diazyme Labs, USA with autoanalyzer, Cobbas 8000) with results expressed as U/g creatinine. Urinary enzyme levels could be affected by urine flow rate, so in order to minimize this effect, the level of enzymuria is expressed as the ratio of enzyme activity to urinary creatinine level.
Clinical characteristics are presented as mean ± standard deviation (SD). Comparison between groups was performed using Student’s t tests and between subgroups with Mann–Whitney U tests. A p value of <0.05 was regarded as significant. Categorical data were evaluated using the Chi-square test. Pearson’s correlation coefficient analysis was used for comparing biochemical variables. All statistics were performed using the IBM SPSS statistics 17.0 software program. The study was approved by the hospital ethics committee and informed consent was obtained from all subjects and their parents before the start of the study.
Results
The clinical and biochemical data of obese and control subjects are summarized in Tables 1 and 2, respectively. The two groups were well matched in terms of age and gender (p = 0.398 and p = 0.723, respectively), but systolic and diastolic blood pressures were significantly higher in the obese group (p < 0.001). Serum creatinine values were all within normal limits and all patients had normal GFR according to the Schwartz formula. Fasting glucose levels were <126 mg/dl and second-hour glucose levels were <200 mg/dl.
Obese subjects had significantly higher urinary NAG/Cr (17.39 ± 19.9 vs. 11.91 ± 6.0 U/g creatinine, p = 0.027) and urinary KIM1/Cr (0.87 ± 1.16 vs. 0.56 ± 0.29 ng/mg creatinine, p = 0.026) compared with the lean subjects, however no significant difference was found in urinary NGAL/Cr values between the two groups (195.66 ± 205.57 vs. 191.51 ± 101.55 ng/mg creatinine, p˃0.05) (Figs. 1 and 2). No statistically significant differences were found in serum creatinine, sodium, phosphorus, GFR, FENa, TPR, urine calcium/creatinine ratio, NGAL/creatinine, and urine microalbumin/creatinine (Table 2).
In the study group, 78 subjects had HOMA-IR values and 59 of them had insulin resistance (HOMA-IR mean ± SD = 6.4 ± 3.9). Among these obese subjects, seven had impaired glucose tolerance. Those with impaired glucose tolerance did not have significantly higher urinary NAG/Cr (22.8 ± 21.7 vs. 16.15 ± 13.71 U/g creatinine, p = 0.252), NGAL/Cr (249.94 ± 238.38 vs. 175.21 ± 116.37 ng/mg creatinine, p = 0.509) and KIM-1/Cr (1.05 ± 1.11 vs. 0.80 ± 0.58 ng/mg creatinine) compared to those with a normal glucose tolerance test.
Renal injury markers of obese patients with or without insulin resistance were compared and no significant differences were found in urinary NAG/Cr (17.18 ± 21.44 vs. 15.78 ± 14.57 U/g creatinine, p = 0.798), NGAL/Cr (189.27 ± 215.47 vs. 182.49 ± 165.33 ng/mg creatinine, p = 0.904) and KIM-1/Cr (0.88 ± 1.29 vs. 0.74 ± 0.72 ng/mg creatinine, p = 0.653).
Urinary NAG/Cr, NGAL/Cr, and KIM-1/Cr did not correlate with fasting blood glucose level or 120-min glucose levels in the OGTT (p > 0.05). Urinary NAG/Cr, NGAL/Cr, and KIM-1/Cr correlated well with each other (p < 0.005).
In the obese subjects, 30.9 % (n = 26) of them were hypertensive; 7.1 % (n = 6) were found to be in stage 1 (BP levels range from the 95th percentile to 5 mmHg above the 99th percentile) and 23.8 % (n = 20) were found to be in stage 2 (BP levels more than 5 mmHg above the 99th percentile), as well as 14.2 % (n = 12) who were prehypertensive (BP levels between 90th and 95th percentile) (Table 3). Urinary injury markers in different categories of hypertension are also presented in Table 3. When we compared obese subjects with lean controls, blood pressure percentiles were significantly higher in obese subjects (p < 0.001).
We also analyzed obese subjects for effects of hypertension on urinary injury markers. Obese subjects with hypertension did not have significantly higher urinary NAG/Cr (21.04 ± 29.36 vs. 15.19 ± 12.63 U/g creatinine, p = 0.323), NGAL/Cr (222.36 ± 296.06 vs. 184.60 ± 138.95 ng/mg creatinine, p = 0.528) or KIM-1/Cr (1.09 ± 1.83 vs. 0.73 ± 0.57 ng/mg creatinine, p = 0.301) compared to obese patients with normal blood pressure (Table 4).
Discussion
As many as 250 million people worldwide are obese. It is a consequence of increasingly sedentary lifestyles and more energy-dense diets [21]. In Turkey, obesity and overweight prevalence studies have been done in different parts of the country, with results ranging between 1.6 and 8.9 % and 8.3 and 11.1 % [22–25]. In the second half of the 20th century, the obvious increase of type 2 DM correlates with the growing prevalence of obesity that now affects 6 % of the world’s population [26, 27]. Excess weight gain accounts for as much as 65–75 % of the risk for essential hypertension [28]. Diabetes and hypertension both increase the risk of end-stage renal disease [1, 2, 28].
Nowadays, an increasingly popular hypothesis is that a tubular phase of diabetic disease precedes the manifestations of classic glomerular lesions. Several biomarkers have been used to support this hypothesis [29–33], urinary NAG being the most relevant parameter, but urinary NGAL and KIM-1 have also been studied [12, 29, 31, 32]. A recent study conducted by Savino et al. [34] revealed that serum and urinary nitric oxide—an important modulator of renal function and morphology—and its metabolites (nitrite and nitrate) were significantly lower, and urinary PGF-2α (an oxidative stress marker) was significantly higher, in obese children and adolescents compared with lean age- and gender-matched subjects.
In our study, we wanted to determine if renal tubular damage starts before the development of diabetes and diabetic nephropathy. We showed that urinary NAG and KIM-1 were elevated in obese children compared to those markers in lean age- and gender-matched controls. No patients in the study group had microalbuminuria or diabetes.
To understand how diabetes causes renal tubular damage without microalbuminuria, its relationship with blood glucose levels was investigated. Recent studies in adults have revealed that urinary NAG is found to correlate with blood glucose levels, and decreases to normal levels when the blood glucose level is well controlled [35, 36]. Fujita et al. [31] have shown that NAG is elevated in patients with impaired glucose tolerance, a preliminary state of diabetes. Among patients with impaired glucose tolerance test, 19–61 % proceed to DM within 5–10 years [37]. Kordonouri et al. [29] demonstrated that NAG is correlated with HbA1c and that tubular enzymuria is more prevalent in patients with poorer metabolic control. The Diabetes Control and Complications Trial has recently shown that NAG is positively correlated with 120-min blood glucose levels in OGTT. With these results, postprandial hyperglycemia was thought to be an independent factor that causes renal damage [38]. In the current study, however, we found that urinary injury markers did not differ when we compared patients for insulin resistance and impaired glucose tolerance nor were these values correlated with fasting and postprandial glucose values. This may be due to the small sample size of our study. Increasing the number of individuals in the obese group might have resulted in statistically significant values.
Obesity is associated with hypertension and glomerular hyperfiltration. Increased glomerular hyperfiltration is expected to raise postglomerular oncotic pressure and to increase proximal tubular sodium reabsorption. Salt retention is the major cause of hypertension in obesity [39]. Hypertension is closely related to kidney dysfunction. Limited data in the childhood period revealed that GFR, the prevalence of hypertension, and stage II hypertension were associated with obesity. In a recent paper, Duzova et al. found that rates of children with eGFR <90 and <75 ml/min/1.73 m2 were higher in obese children, but did not reach statistical significance. Also, they showed that the obese group had a higher ratio of hypertension than the healthy population (11.4 vs. 5.6 %) [40]. When we compared our study with Duzova’s [40] study, none of the obese children had decreased eGFR values and the percentage of hypertension was 30 %. The difference between these two studies might be related to the study populations: Duzova et al.’s [40] study was a population-based field study, whereas our cases were selected from an outpatient endocrinology clinic. Some studies that investigated the relationship between NAG and hypertension in diabetic patients have found that urinary NAG levels are not related to blood pressure [41, 42], results which support our current work. In our study, urinary NAG, NGAL, and KIM-1 were not significantly increased in hypertensive patients. To the best of our knowledge, KIM-1 has not previously been studied in obese and non-obese subjects who have hypertension.
We also evaluated whether the electrolyte transport system could be affected in obese patients. In poorly controlled diabetic patients, increased urinary phosphate excretion was observed. In juvenile diabetic patients, significantly increased urinary sodium excretion was found in relation to body surface area [43]. Hyperinsulinemia is also associated with reduced urinary sodium excretion. Whether the principal site of this action is the proximal or distal tubule remains somewhat controversial [29, 44]. In this study, we showed that in early stages of obesity fractional excretion of sodium and tubular phosphorus reabsorption rates were unchanged.
We acknowledge that the current study has some limitations. First, it has a cross-sectional design and renal injury markers should be investigated in long-term, prospective, observational studies. Second, having a larger number of patients would have allowed us to analyze different specific subgroups, i.e., children with impaired glucose tolerance or type 2 DM but without microalbuminuria. The strengths of this study are that we measured a wide range of kidney injury markers.
In conclusion, we found that two tubular damage markers—urinary NAG and KIM-1—were elevated in obese patients compared to healthy lean controls. Longitudinal observational studies are needed to analyze early renal effects of obesity and its comorbidities in individual patients. Treatment would then be optimized in order to prevent nephropathy.
References
Henegar JR, Bigler SA, Henegar LK, Tyagi SC, Hall JE (2001) Functional and structural changes in the kidney in the early stages of obesity. J Am Soc Nephrol 12:1211–1217
Ross WR, McGill JB (2006) Epidemiology of obesity and chronic kidney disease. Adv Chronic Kidney Dis 13:324–335
Tagle R, Gonzalez F, Acevedo M (2012) Microalbuminuria and urinary albumin excretion in clinical practice. Rev Med Chil 140:797–805
Redon J, Martinez F (2012) Microalbuminuria as surrogate endpoint in therapeutic trials. Curr Hypertens Rep 14:345–349
Thomas MC, Burns WC, Cooper ME (2005) Tubular changes in early diabetic nephropathy. Adv Chronic Kidney Dis 12:177–186
Brito PL, Fioretto P, Drummond K, Kim Y, Steffes MW, Basgen JM, Sisson-Ross S, Mauer M (1998) Proximal tubular basement membrane width in insulin-dependent diabetes mellitus. Kidney Int 53:754–761
Soni SS, Cruz D, Bobek I, Chionh CY, Nalesso F, Lentini P, de Cal M, Corradi V, Virzi G, Ronco C (2010) NGAL: a biomarker of acute kidney injury and other systemic conditions. Int Urol Nephrol 42:141–150
Han KW, Bailly V, Abichandani R, Thadhani R, Bonventre JV (2002) Kidney injury molecule-1(KIM-1): a novel biomarker for human renal proximal tubule injury. Kidney Int 62:237–244
Adiyanti SS, Loho T (2012) Acute kidney injury (AKI) biomarker. Acta Med Indones 44:246–255
Kavukçu S, Soylu A, Türkmen M (2002) The clinical value of urinary N-acetyl-β-d-glucosaminidase levels in childhood age group. Acta Med Okayama 56:7–11
Mohammadi-Karakani A, Asgharzadeh-Haghighi S, Ghazi-Khansari M, Hosseini R (2007) Determination of urinary enzymes as a marker of early renal damage in diabetic patients. J Clin Lab Anal 21:413–417
Nielsen SE, Schjoedt KJ, Astrup AS, Tarnow L, Lajer M, Hansen PR, Parving HH, Rossing P (2010) Neutrophil gelatinase-associated lipocalcin (NGAL) and kidney injury molecule 1 (KIM1) in patients with diabetic nephropathy: a cross-sectional study and the effects of lisinopril. Diabet Med 27:1144–1150
Bonvente JV (2009) Kidney injury molecule-1 (KIM-1): a urinary biomarker and much more. Nephrol Dial Transplant 24:3165–3168
Cowland JB, Sorensen OE, Sehested M, Borregaard N (2003) Neutrophil gelatinase-associated lipocalcin is up-regulated in human epithelial cells by IL-1β, but not TNF-α. J Immunol 171:6630–6639
Barlow SE, Committee E (2007) Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics 120:164–192
Schwartz GJ, Brion LP, Spitzer A (1987) The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children, and adolescents. Pediatr Clin N Am 34:571–590
Alberti KG, Zimmet PZ (1998) Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of WHO consultation. Diabet Med 15:539–553
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Valerio G, Licenziati MR, Iannuzzi A, Franseze A, Siani P, Riccardi G, Rubba P (2006) Insulin resistance and impaired glucose tolerance in obese children and adolescents from southern Italy. Nutr Metab Cardiovasc Dis 16:279–284
National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents (2004) The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics 114:555–576
Siedell JC (2000) Obesity, insulin resistance and diabetes—a worldwide epidemic. Br J Nutr 83:5–8
Yuca SA, Yilmaz C, Cesur Y, Dogan M, Kaya A, Basaranoglu M (2010) Prevalence of overweight and obesity in children and adolescents in eastern Turkey. J Clin Res Pediatr Endocrinol 2:159–163
Krassas GE, Tsametis C, Baleki V, Constantinidis T, Unluhizarci K, Kurtoglu S, Kelestimur F (2004) Balkan group for the study of obesity. Prevalence of overweight and obesity among children and adolescents in Thessaloniki-Greece and Kayseri-Turkey. Pediatr Endocrinol Rev 3:460–464
Ercan S, Dallar YB, Onen S, Engiz O (2012) Prevalence of obesity and associated risk factors among adolescents in Ankara, Turkey. J Clin Res Pediatr Endocrinol 4:204–207
Soylemezoglu O, Duzova A, Yalcinkaya F, Arınsoy T, Suleymanlar G (2012) Chronic renal disease in children aged 5-18 years: a population-based survey in Turkey, the CREDIT-C study. Nephrol Dial Transplant 27:146–151
Ginter E, Simko V (2012) Type 2 diabetes mellitus, pandemic in 21st century. Adv Exp Med Biol 771:42–50
Adeghate E, Schattner P, Dunn E (2006) An update on the etiology and epidemiology of diabetes mellitus. Ann N Y Acad Sci 1084:1–29
Wofford MR, Hall JE (2004) Pathophysiology and treatment of obesity hypertension. Curr Pharm Des 10:3621–3637
Kordonouri O, Kahl A, Jörres A, Hopfenmüller W, Müller C, Danne T (1999) The prevalence of incipient tubular dysfunction, but not of glomerular dysfunction, is increased in patients with diabetes onset in childhood. J Diabetes Complications 13:320–324
Bolignano D, Lacquaniti A, Coppolino G, Donato V, Fazio MR, Nicocia G, Buemi M (2009) Neutrophil gelatinase-associated lipocalcin as an early biomarker of nephropathy in diabetic patients. Kidney Blood Press Res 32:91–98
Fujita H, Narita T, Morii T, Shimotomai T, Yoshioka N, Kakei M, Ito S (2002) Increased urinary excretion of N-acetylglucosaminidase in subjects with impaired glucose tolerance. Ren Fail 24:69–75
Golov KG, Va V, Dlu O, Neverov NI, Shestakova MV, Proskurneva FP (1995) Urinary enzymes in the assessment of the early stage of kidney involvement in psoriasis and diabetes mellitus. Ter Arkh 67:80–81
Hsiao PH, Tsai WS, Tsai WY, Js L, Tsau YK, Chen CH (1996) Urinary N-acetyl-beta-d-glucosaminidase activity in children with insulin-dependent diabetes mellitus. Am J Nephrol 16:300–303
Savino A, Pelliccia P, Giannini C, Giorgis T, Cataldo I, Chiarelli F, Mohn A (2011) Implications for kidney disease in obese children and adolescents. Pediatr Nephrol 26:749–758
Nauta FL, Boertien WE, Bakker SJ, van Goor H, van Oeveren W, de Jong PE, Bilo H, Gansevoort RT (2011) Glomerular and tubular damage markers are elevated in patients with diabetes. Diabetes Care 34:975–981
Bastürk T, Altuntaş Y, Kurklu A, Aydin L, Eren N, Unsal A (2006) Urinary N-acetyl-β glucosaminidase as an earlier marker of diabetic nephropathy and influence of low-dose perindopril/indapamide combination. Ren Fail 28:125–128
Hiratsuka N, Shiba K, Nishida K, Lizima S, Kimura M, Kobayashi S (1998) Analysis of urinary albumin, transferring, N-acetyl-β -d-glucosaminidase and β2 microglobulin in patients with impaired glucose tolerance. J Clin Lab Anal 12:351–355
Kern EF, Erhard P, Sun W, Genuth S, Weiss MF (2010) Early urinary markers of diabetic kidney disease: a nested case-control study from the Diabetes Control and Complications Trial(DCCT). Am J Kidney Dis 55:824–834
Chagnac A, Herman M, Zingerman B, Erman A, Rozen-Zvi B, Hirsh J, Gafter U (2008) Obesity-induced glomerular hyperfiltration: its involvement in the pathogenesis of tubular sodium reabsorption. Nephrol Dial Transplant 23:3946–3952
Duzova A, Yalcinkaya F, Baskin E, Bakkaloğlu A, Soylemezoglu O (2013) Prevalence of hypertension and decreased glomerular filtration rate in obese children: results of a population-based field study. Nephrol Dial Transplant 28:166–171
Ouchi M, Suzuki T, Hashimoto M, Motomoya, Ohara M, Suzuki K, Igari Y, Watanabe K, Nakano H, Oba K (2012) Urinary N-acetyl-β-d-glucosaminidase levels are positively correlated with 2-Hr plasma glucose levels during oral glucose tolerance testing in prediabetics. J Clin Lab Anal 26:473–480
Schnoell F, Weitgasser R, Straberger A, Pretsch I (1990) Urinary activity of N-acetyl-β-d-glucosaminidase (NAG) in noninsulin-dependent diabetics. Diabetologia 33:A153
Miltenyi M, Körner A, Tulassay T, Szabo A (1985) Tubular dysfunction in type 1 diabetes mellitus. Arch Dis Child 60:929–931
Quinones-Galvan A, Ferrannini E (1997) Renal effects of insulin in man. J Nephrol 10:188–191
Acknowledgments
We thank S. Delacroix for English editing of the manuscript.
Conflict of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goknar, N., Oktem, F., Ozgen, I.T. et al. Determination of early urinary renal injury markers in obese children. Pediatr Nephrol 30, 139–144 (2015). https://doi.org/10.1007/s00467-014-2829-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-014-2829-0