Abstract
Studies have demonstrated that cyclin-dependent kinase inhibitors (CDKI) that inhibit cell-cycle progression have a protective effect against acute kidney injury (AKI). Most studies have focused on the CIP/KIP family members of CDKI; only a few have explored the role of INK4 family members in AKI. Because INK4 family members block the G1-S transition, we postulated that they should have protective effects against AKI. The most conserved INK4 member is p18, so we selected it to explore its effects on cisplatin-induced renal cell injury. We overexpressed p18 in renal tubular epithelial cells (LLC-PK1) by transient transfection and investigated its effects on the cell cycle and proliferation. After transfection, cell injury was induced by cisplatin (100 μM) incubation for 24 h in a standard medium. The effect of p18 was assayed by assessing cell necrosis and apoptosis in transfected cells. The endoplasmic reticulum stress (ERS) pathway was evaluated to interpret the possible mechanism of p18 action in cisplatin-induced renal cell injury. Overexpression of p18 arrested cell cycle progression in the G1 phase and inhibited proliferation. Compared with vehicle transfection, p18 overexpression did not affect cisplatin-induced necrosis, but it reduced the percentage of apoptotic cells significantly. The severity of ERS induced by cisplatin was also decreased by p18 overexpression. P18 protects against cisplatin-induced renal cell injury. The mechanism of p18 protection may lie in its effect on the cell death pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although recent advances have improved our understanding of acute kidney injury (AKI), the mortality from AKI remains high, especially in patients in the intensive care unit, where mortality is higher than 50% [1]. The pathogenesis of AKI is complex, involving inflammation, cytokines, and multiple cell-death pathways [2–10]. AKI is thus a challenging clinical syndrome, although renal replacement therapy provides an effective supportive treatment for AKI patients.
Necrosis and apoptosis are the main manifestations of AKI in both kidney injury in vivo and renal cell injury in vitro. Activation of cell-death pathways and the actions of cell-cycle regulatory proteins eventually decide the final fate of injured renal cells: proliferation, hypertrophy or apoptosis [11–13]. Cyclins bind to cyclin-dependent kinases (CDK) to form a complex that promotes cell-cycle progression [14], while cyclin-dependent kinase inhibitors (CDKI) block cell-cycle progression by inhibiting the activities of CDK [15]. Cell-cycle arrest is beneficial because it allows damaged DNA to be repaired and, thus, reduces the severity and teratogenicity of the injury [16]. For this reason, CDKI have been investigated intensively and shown to have cell protective properties in AKI [17–24]. It is therefore thought that cell cycle regulation might be a potential component in the treatment of AKI.
Based on sequence and the inhibitory effects they exert on CDK, the seven CDKI are divided into two families. The CIP/KIP family includes p21, p27, and p57, which act with multiple CDK and extensively inhibit the cell cycle [25]. The INK4 family includes p16, p15, p18, and p19, which interact only with CDK4/6 and specifically arrest the cell cycle in the early G1 phase [26]. CDKI studies in AKI have mainly focused on the CIP/KIP family, especially p21, but few studies have investigated the members of the INK4 family. INK4 family members were long thought to be tumor-suppressor genes because they are frequently defective or mutated in tumors [27]. However, more recent studies have shown that INK4 family members also play many other novel biological roles, such as in DNA damage response and apoptosis [28]. We therefore postulated that INK4 family members have additional protective actions in AKI.
The members of the INK4 family share approximately 40% amino acid sequence identity. Compared with p15, p16, and p19, p18 is relatively well conserved. Both human and murine p18 contain 168 amino acids, of which only seven residues in the C-terminal domains differ [29, 30]. Therefore, we selected p18 as the focus of this study to investigate its actions in cisplatin-induced renal cell injury.
Materials and methods
Cell culture and experiments in vitro
LLC-PK1 cells, purchased from American Type Culture Collection (CL-101), were maintained in Dulbecco’s modified Eagle’s medium (DMEM) supplemented with 10% FBS in an atmosphere of 95% air/5% CO2 at 37°C. The plasmid pCMV-sport-6-murine-p18 and the vehicle were a generous gift from Professor Xing-zhen Chen of Alberta University in Canada. The plasmid pVAX1/LacZ was purchased from Invitrogen.
For experiments, the murine p18 plasmid, vehicles or LacZ plasmid was transfected into LLC-PK1 cells in six-well or 6-cm plates. Western blot analysis and β-galactosidase staining were used to evaluate the efficiency of transfection. After transfection, cell cycle and proliferation were analyzed by flow cytometry and methyl thiazolyl tetrazolium (MTT) reduction respectively. The effect of p18 overexpression on CDK2, CDK4, and CDK6 kinase activity was assayed by immunoprecipitation and western blot analysis. Cell injury was induced by cisplatin (100 μM) incubation in complete medium for 24 h, and then cisplatin-induced necrosis and apoptosis were evaluated to investigate the effect of p18 overexpression on the cell injury.
Transient transfection
To perform transfection, LLC-PK1 cells were seeded in 6-cm culture plates or in six-well plates. After growth to 70–80% confluence, the murine p18 plasmid, vehicle or LacZ plasmid was transfected into the cells using Lipofectamine 2000 (Invitrogen). Briefly, 5 μg plasmid and 20 μl Lipofectamine were diluted in 500 μl of incomplete DMEM separately, combined 5 min later, and incubated at room temperature for 20 min. Then, 500 μl or 1,000 μl of the mixture was added to 2.5 ml or 5 ml of complete medium in each well or plate respectively. After 6 h of incubation, cells were treated with complete medium for 18 h, at which point the transfection was completed.
Cell cycle analysis
After transfection, cells in six-well plates were trypsinized and fixed overnight in 70% ethanol at 4°C. For detection, cells were washed with phosphate-buffered saline (PBS), resuspended in binding buffer containing RNase A (10 μg/ml) and propidium iodide (25 μg/ml), and analyzed by flow cytometry on a FACSCalibur flow cytometer (Becton-Dickinson).
Proliferation analysis
Proliferation was assessed in cells transfected with the p18 plasmid or vehicle by MTT assay. After transfection in 6-cm plates, cells were trypsinized and reseeded in 96-well plates, and MTT reduction was detected by spectrophotometry at 490 nm absorbance in a microplate reader (BIO-TEK ELx800) 4 h, 24 h, 48 h, 72 h, and 96 h after cells were reseeded.
CDK assay in vitro
Cyclin-dependent kinase assays were performed as described before [31], but some modifications were made. Transfected cells were extracted and protein concentrations were determined by Bradford assay. A total of 500 μg of protein was used for each immunoprecipitation. CDK2, CDK4, and CDK6 in cell extracts were incubated with a specific antibody (3 μg/reaction) for 1 h at 4°C. 40 μl of protein A/G-agarose (Santa Cruz) was added into the mixture, which was then further incubated for 1 h. Immune complexes were centrifuged at 12,000 rpm for 3 min and the precipitates were washed three times with lysis buffer and once with kinase buffer (50 mM Tris-HCl/pH 7.5, 10 mM MgCl2, 1 mM DTT). CDK assays on histone H1 were performed by mixing the respective immune complexes with 2.5 μg of histone H1 and 50 μM ATP in 30 μl of kinase buffer. CDK assays on retinoblastoma (Rb) were carried out in the same way using 1 μg of full-length Rb protein (QED Bioscience) and 10 μM ATP in 30 μl of kinase buffer. The kinase reaction was performed at 30°C for 15 min (CDK assays on histone H1) or 1 h (CDK assays on Rb) and then terminated with 2× SDS-PAGE sample buffer. The reaction mixtures were resolved by SDS-polyacrylamide gel electrophoresis analysis. The extent of phosphorylation was measured by western blot analysis using the antibodies of phospho-histone H1 (Abcam) and phospho-Rb (CST).
L-lactate dehydrogenase release assay
L-lactate dehydrogenase (LDH) in the medium and in the cellular fraction was measured as an index of lethal membrane injury (necrosis) using an assay kit purchased from Promega and used according to the manufacturer’s specifications. Briefly, at the end of cisplatin incubation, medium was collected, and the adherent monolayer of cells was lyzed at 37°C for 45 min. Then, the mixed substrate was added to the medium and cell plates in the dark for 30 min. The reaction was stopped with stop solution, and the absorbance at 490 nm was measured. The degree of cell injury was expressed as LDH release, which was calculated as the percentage of LDH released into the medium out of the total LDH recovered from both medium and cellular fractions.
Flow cytometry
The percentage of apoptotic and necrotic cells was detected using a Vybrant Apoptosis Assay Kit (Invitrogen) by flow cytometry according to the manufacturer’s specifications. Briefly, floating and adherent cells were collected after cisplatin incubation, washed with PBS, and resuspended in binding buffer and Annexin V for 15 min in the dark. Then, 5 μg/ml of propidium iodide (PI) was added to each tube, and the suspensions were analyzed by flow cytometry on the FACSCalibur flow cytometer (Becton-Dickinson).
By staining cells with annexin V-FITC and PI, the percentages of viable cells (lower left quadrant), early apoptotic cells (lower right quadrant), late apoptotic (upper right quadrant) and necrotic cells (upper left quadrant) were quantitatively determined. For statistical analysis, the term "apoptotic cells" refers to early apoptotic cells (lower right quadrant), and "necrotic cells" were the cells located in the upper left quadrant.
Caspase 3 activity
Caspase 3 activity was tested by use of the Caspase Colorimetric Activity Assay Kit (Biovision, China), following the manufacturer’s protocols. After 24 h of cisplatin incubation, cells were collected and lysed in lysis buffer and centrifuged at 10,000 g for 5 min. The supernatants were incubated with caspase 3 substrate (DEVD-pNA) at 37°C for 1 h. The cleaved pNA, with a light emission at 405 nm, was quantified using a microplate reader (BIO-TEK ELx800).
Western blot
Proteins were extracted from cultured cells using the lysis buffer. After a 30-min incubation on ice, the lysates were heated at 100°C for 15 min and centrifuged at 12,000 g for 15 min at 4°C. Lysates containing equal amounts of protein (100 μg) were dissolved in SDS sample buffer, separated on 12% SDS slab gels, and transferred electrophoretically onto polyvinylidene difluoride membranes. Equal protein loading and protein transfer were confirmed by Ponceau S staining. After being blocked with 5% non-fat dry milk in TBST, the membrane was incubated at 4°C overnight with one of the following primary antibodies: mouse anti-GAPDH (1:5,000 dilution; Kangcheng), rabbit anti-β-actin (1:2,000 dilution; CST), rabbit anti-p18 (1:200 dilution; Santa Cruz), rabbit anti-grp78 (1:1,000 dilution; CST), rabbit anti-caspase 3 (1:1,000 dilution; CST), rabbit anti-PARP (1:1,000 dilution; CST), rabbit anti-caspase 12 (1:1,000 dilution; CST), rabbit anti-PERK (1:1,000 dilution; CST), rabbit anti-phospho-PERK (1:1,000 dilution; CST), rabbit anti-eIF2α (1:1,000 dilution; CST) or rabbit anti-phospho-eIF2α (1:1,000 dilution; CST). After the membranes were washed, horseradish peroxidase-conjugated secondary antibody was applied. Proteins that bound to the secondary antibody were visualized using ECL (Amersham Bioscience).
Statistical analysis
Data are presented as means ± SD. Comparisons of experimental values for cisplatin-treated cells with untreated controls were conducted using analysis of variance (ANOVA) or the Kruskal–Wallis rank test. Statistical significance was defined as p < 0.05.
Results
Transfection of p18 plasmid induces p18 overexpression in LLC-PK1 cells
As shown in Fig. 1, p18 expression in LLC-PK1 cells increased markedly 24 h after p18 plasmid transfection, as demonstrated by western blot analysis. Microscopic analysis of β-galactosidase staining showed that 35% of the cytoplasm stained blue 24 h after LacZ plasmid transfection, compared with 0% in pVAX1-transfected cells, which indicated that the transfection efficiency of LLC-PK1 cells was approximately 35%.
Overexpression of p18 in LLC-PK1 cells. a In a β-galactosidase staining assay, the proportion of blue-stained cytoplasm measured under light microscopy, an indication of transfection efficiency, was approximately 35% after LacZ plasmid transfection. b Compared with vehicle transfection, the expression of p18 was markedly increased in p18-transfected cells, as demonstrated by western blot analysis
Overexpression of p18 arrests the cell cycle in G1 and inhibits the proliferation of LLC-PK1 cells
Compared with vehicle transfection, the proportion of G0/G1 cells was increased and that of S-phase cells was decreased significantly by murine p18 plasmid transfection. It was apparent that p18 overexpression arrested LLC-PK1 cells in the G1 phase and prevented cells from entering the phase for DNA synthesis and replication (Table 1).
Accordingly, p18 overexpression also inhibited the proliferation of LLC-PK1 cells (Fig. 2). The greatest difference between the vehicle- and p18-transfected cells was at 48 h after reseeding, based on the p values of statistical analysis at every time-point.
Overexpression of p18 inhibits the proliferation of LLC-PK1 cells as demonstrated by methyl thiazolyl tetrazolium (MTT) assay. Data are from four independent experiments. The most apparent difference between p18- and vehicle-transfected cells occurred at 48 h after reseeding, based on the p values of various time points
Overexpression of p18 inhibits the activity of CDK4 and CDK6
As shown in Fig. 3, CDK4- and CDK6- mediated phosphorylation of Rb protein was lower in p18-transfected cells and no apparent difference existed in CDK2-mediated phosphorylation of histone H1 between the vehicle- and p18- transfected cells. These assays showed that overexpression of p18 in transfected cells only inhibited the activity of CDK4 and CDK6, which was in agreement with previous reports that p18 interacted especially with CDK4 and CDK6.
Overexpression of p18 inhibits the CDK4 and CDK6 kinase activity. Whole cell extracts were prepared from the vehicle- (the left lane) and p18- (the right lane) transfected cells at transfection for 24 h. Equal amounts of the lysates (500 μg) were used for the specific immune complex kinase assay. CDK2 kinase assay was performed using histone H1 as a substrate as described under “Materials and methods.” CDK4 and CDK6 kinase assay was carried out using full-length Rb protein as a substrate. Samples were analyzed by 10% SDS-polyacrylamide gel electrophoresis, the phosphorylated forms of histone H1 and Rb were examined by immunoblotting with histone H1- and Rb- specific antibody. Representative data from three independent experiments are shown. The fold change in the respective kinase activity was analyzed from the straps of each gel slice
Overexpression of p18 protects LLC-PK1 cells against cisplatin-induced injury
As shown in Fig. 4, there was a significant difference in the number of apoptotic cells between the vehicle- and p18-transfected cells after cisplatin (100 μM) administration. The proportion of apoptotic cells in the p18 group was much lower than in the vehicle group (p < 0.05). However, there was no apparent difference between the two groups in the number of necrotic cells after cisplatin (100 μM) treatment (p > 0.05).
Effects of p18 overexpression on LLC-PK1 cell necrosis and apoptosis after cisplatin (100 μM) incubation for 24 h as demonstrated by flow cytometry. Representative FACS plots showed the percentage of viable cells (lower left quadrant), early apoptotic cells (lower right quadrant), late apoptotic cells (upper right quadrant) and necrotic cells (upper left quadrant) in a vehicle-transfected cells and b p18-transfected cells after cisplatin administration. Six independent experiments were analyzed, and statistical analysis showed that there was significant difference in the number of apoptotic cells (early apoptotic cells/lower right quadrant) between the vehicle- and p18-transfected cells after cisplatin administration, while there was no apparent difference in the number of necrotic cells (upper left quadrant) between the two groups. *p < 0.05, comparison between the vehicle- and p18-transfected cells after cisplatin administration
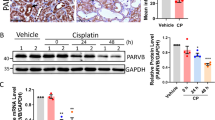
Consistent with the result, caspase 3 activity in the p18 group was much lower than in the vehicle group after cisplatin (100 μM) administration (Fig. 5). The amount of splice fragments of caspase 3 and PARP (a substrate of caspase 3) was much lower in the p18 group after cisplatin (100 μM) administration (Fig. 5). There was no significant difference in LDH release between the two groups after cisplatin (100 μM) treatment (p > 0.05; Fig. 5).
Effect of p18 overexpression on cisplatin-induced apoptosis and necrosis as demonstrated by caspase 3 activity, western blot analysis, and L-lactate dehydrogenase (LDH) release. a Caspase 3 activity: four independent experiments in the four groups were analyzed. Each bar represents the mean ± SD of the absorbance at 405 nm. *p < 0.05, comparison between p18- and vehicle-transfected cells after cisplatin (100 μM) administration. b Overexpression of p18 decreases the cleavage of caspase 3 and PARP in cisplatin-injured LLC-PK1 cells. Equal protein (100 μg) loading of each sample was confirmed by blotting for GAPDH. Three independent experiments were analyzed, and each bar in the figure represents the mean ± SD of the measurements of the ratio of active caspase 3 to pro-caspase 3. The cleavage of PARP in p18-transfected cells after cisplatin administration was lower, so we did not analyze the statistical difference between the p18- and vehicle-transfection groups. *p < 0.05, comparison between p18- and vehicle-transfected cells after cisplatin (100 μM) administration. c LDH release: six independent experiments in between the vehicle- and p18-transfected cells after cisplatin (100 μM) incubation for 24 h were analyzed. Statistical analysis showed that there was no significant difference in LDH release between the two groups
To further investigate the effect of p18 overexpression on necrosis and apoptosis, low (20 μM) and high (500 μM) concentrations of cisplatin were used to induce cell injury in the vehicle- and p18-transfected cells. Results of flow cytometry analysis showed that there was no apparent difference in the number of necrotic cells between the two groups after cisplatin (20 μM) or cisplatin (500 μM) incubation for 24 h. There was a significant difference in the number of apoptotic cells between the two groups after cisplatin (20 μM) administration, but the effect of p18 overexpression on cell apoptosis apparently attenuated after cisplatin (500 μM) administration (Fig. 6).
Effects of p18 overexpression on LLC-PK1 cell necrosis and apoptosis after cisplatin (20 μM and 500 μM) incubation for 24 h as demonstrated by flow cytometry. Representative FACS plots and statistical analysis were shown in the figure. It was apparent that there was no significant effect of p18 overexpression on cisplatin-induced necrosis (the number of necrotic cells located in the upper left quadrant) after cisplatin (20 μM) or cisplatin (500 μM) incubation. However, overexpression of p18 significantly attenuated LLC-PK1 cell apoptosis when it was treated by cisplatin (20 μM), while the protection of p18 overexpression was attenuated when the cells were treated by cisplatin (500 μM). There was no statistical difference in the number of apoptotic cells (early apoptotic cells/lower right quadrant) between the vehicle- and p18-transfected cells after cisplatin (500 μM) treatment
Overexpression of p18 affects the ERS pathway in cisplatin-induced LLC-PK1 cell injury
After cisplatin (100 μM) incubation, the expression of grp78 was upregulated, and caspase 12 was activated in vehicle- and p18 plasmid-transfected cells, which indicates that the ERS pathway was activated in cisplatin-injured LLC-PK1 cells. However, compared with the vehicle group, the degrees of grp78 upregulation and caspase 12 activation in the p18 group were much lower, which indicates that the severity of cisplatin-induced ERS was attenuated by p18 overexpression in LLC-PK1 cells (Fig. 7). As a quick response to ERS, the eIF2α/PERK pathway was also evaluated by western blot analysis. It showed that the extent of phosphorylated eIF2α and PERK was attenuated in p18 plasmid-transfected cells compared with vehicle-transfected cells after cisplatin (100 μM) incubation, which confirmed the effect of p18 overexpression on the ERS pathway in cisplatin-induced LLC-PK1 cell injury (Fig. 7).
Overexpression of p18-attenuated cisplatin-induced ERS severity as demonstrated by western blot analysis. It is apparent that overexpression of p18 in LLC-PK1 cells decreases the upregulation of grp78 and the activation of caspase 12 after cisplatin (100 μM) incubation. The extent of phosphorylated PERK and eIF2α in cisplatin-injured LLC-PK1 cells was also attenuated by the overexpression of p18 in the transfected cells. In this part of the experiments, equal protein (100 μg) loading of each sample was confirmed by blotting for GAPDH. Three independent experiments were analyzed, and each bar represents the mean ± SD of the ratio of the target protein to GAPDH. *p < 0.05, comparison between p18- and vehicle-transfected cells after cisplatin (100 μM) incubation
Discussion
Clinical use of cisplatin is largely limited due to drug resistance and nephrotoxicity [32, 33]. The mechanism by which cisplatin produces its nephrotoxic effect is complex and involves the activation of several signal transduction pathways and cytokine-triggered inflammatory responses [34]. Because the manifestation of cisplatin nephrotoxicity is similar to that of human AKI, it has often been used in the study of AKI. The main forms of cisplatin-induced renal cell injury, which is concentration-dependent, include necrosis and apoptosis. High-concentration cisplatin causes necrosis, whereas low-concentration cisplatin mainly induces apoptosis [35]. For this reason, LLC-PK1 cell injury was induced by cisplatin in our experiments, and different concentrations of cisplatin were used to identify the effects of p18 overexpression on apoptosis and necrosis.
It is true that death pathways must be involved in the mechanism of cisplatin nephrotoxicity. Previous studies have confirmed that in addition to the classical death-receptor pathway and mitochondrial pathway [5, 8, 36–38], the ERS pathway is also activated in cisplatin-induced kidney injury both in vivo and in vitro [39–43]. Therefore, the effect of p18 on the ERS pathway was further investigated to elucidate the actions of p18 in cisplatin-induced renal cell injury.
In ERS theory, the unfolded protein response (UPR) plays a central role in ERS-induced apoptosis [44–48]. It has been demonstrated that three transmembrane proteins are activated in UPR: inositol-requiring enzyme-1 (IRE1), pancreatic ER eukaryotic translation initiation factor (eIF)-2α kinase (PERK) and activating translation factor-6 (ATF6). Initially, UPR is an autoregulatory mechanism of the cellular response to ERS, whose purpose is to restore proper ER function. However, apoptosis is also induced once the level of ERS exceeds the self-regulatory ability of the cell [49–51]. It has been reported that activation of JNK and caspase 12 as well as increased expression of CCAAT/enhancer-binding protein homologous protein (CHOP) occur when the cell faces severe ERS [52–54]. In our experiments, the upregulation of molecular chaperone grp78, activation of caspase 12, and the PERK/eIF2α pathway were analyzed to evaluate the severity of ERS in cisplatin-induced LLC-PK1 cell injury.
As expected, p18 played an important role in cisplatin-induced LLC-PK1 cell injury. Overexpression of p18 significantly attenuated apoptosis in LLC-PK1 cells after cisplatin administration, although it did not affect necrosis, as demonstrated by flow cytometry analysis and LDH release respectively. The effect of p18 on apoptosis was also confirmed by analysis of the activity and cleavage of caspase 3 after cisplatin (100 μM) incubation for 24 h. The cleavage of PARP, a substrate of caspase 3, was also analyzed by western blot. The overexpression of p18 markedly decreased the activation of caspase 3 in cisplatin-injured LLC-PK1 cell injury, which confirms the protective effect of p18 in cisplatin-induced renal cell injury.
As demonstrated by MTT assay, overexpression of p18-inhibited cell cycle progression in LLC-PK1 cells, which implied that one mechanism of the p18 protective effect is related to its inhibition of the cell cycle in cisplatin-injured renal cells. Importantly, p18 also affects the ERS pathway, which plays an important role in cisplatin nephrotoxicity, although it is not clear exactly how. Overexpression of p18 markedly decreased the upregulation of chaperone grp78 and the activation of caspase 12. The PERK/eIF2α pathway, one component of the UPR, was inhibited by overexpression of p18 in cisplatin-injured LLC-PK1 cells. Together, these results indicate that the effect of p18 on cell death pathways, such as the ERS pathway, may be another facet of its protective mechanism in cisplatin-induced renal cell injury. Other classical death pathways affected by p18 in cisplatin-induced renal cell injury cannot be excluded because they were not investigated in our experiments.
Different concentrations of cisplatin used in our experiments were to further identify the effect of p18 on cisplatin-induced apoptosis and necrosis. It was apparent that there was no significant difference in the number of necrotic cells between vehicle- and p18-transfected cells after cisplatin (20 μM, 100 μM, and 500 μM) administration. The effect of p18 on apoptosis was more significant in cisplatin (20 μM and 100 μM) treatment than cisplatin (500 μM) treatment. From these results, we postulated that the actions of p18 in cisplatin-induced renal cell injury probably mainly lie in increasing the cells’ tolerance to cisplatin by alleviating to some extent the stress induced by cisplatin. Many of the molecular pathways leading to apoptotic cell death have been extensively studied, whereas those leading to cell death by necrosis are not yet as clear. The exact mechanism of the different effects of p18 on apoptosis and necrosis is unclear. One possible reason for this could be the model of renal injury induced in our experiments, and it will be interesting in our future studies to compare the effect of p18 on the factors associated with apoptosis and necrosis in the renal cell, including experiments on renal injury models induced by other causes, such as hypoxia or hyperoxia.
Previous studies have shown p21, a major effector of cell cycle arrest downstream of p53 activation, as either a negative or a positive regulator of apoptosis in a cell-specific manner. Overexpression of p21 has been shown to enhance the apoptotic response to cisplatin in glioma [55] and ovarian carcinoma [56] cell lines. In cisplatin-induced kidney injury, however, an antiapoptosis role for p21 was demonstrated in vivo and in vitro [18–21]. This effect is mainly due to p21 inhibiting CDK2 activity because the activation of CDK2 is an important factor in promoting apoptosis in cisplatin-induced AKI [22]. The effect of p21 on apoptosis and necrosis in cisplatin nephrotoxicity in previous studies was investigated through in vitro and in vivo experiments respectively. No similar difference in the effects of p21 on apoptosis and necrosis in cisplatin-induced renal cell injury was reported to compare with the effect of p18 found in our study.
INK4 family members have rarely been discussed in AKI, for which some of the possible reasons are the following. It was confirmed that INK4 members interact only with CDK4/6 and arrest the cell cycle in the early G1 phase, with no direct interaction with CDK2. INK4 family members are considered to be involved more in cell differentiation than CIP/KIP family members because no abnormality or defect exists in p21 gene knockout mice, whereas p18 gene knockout mice acquire pituitary tumors with age [13, 57]. However, some studies have reported the involvement of INK4 family members in the cellular response to genotoxic agents. P16 reduced apoptosis induced by ultraviolet light and cisplatin through the intrinsic mitochondrial cell death pathway [58, 59]. P19 overexpression also conferred resistance to cells exposed to UV irradiation [60, 61]. However, no effect of p16 or p19 on necrosis was evaluated through in vitro experiments in these studies. Therefore, apoptosis seems more important in cell injury induced by cisplatin or other genotoxic agents.
Indeed, INK4 proteins compete with D-type cyclins to bind CDK4/6, but studies have demonstrated that enforced expression of INK4 proteins can lead to G1 arrest by promoting the redistribution of CIP/KIP proteins and blocking cyclin E-CDK2 activity [62, 63]. Thus, it was possible that p18 overexpression indirectly inhibited the activity of CDK2 in cycling cells; however, results of the CDK assay in vitro in our study failed to find apparent inhibitory roles of p18 overexpression on CDK2 activity in the transfected cells, while inhibition of CDK4 and CDK6 activity was demonstrated, as shown in Fig. 3. This observation implied that p18 also exerted protection via regulating the cell cycle and cell death pathways in cisplatin-induced renal cell injury, although there are differences between p21 and p18.
As more protective roles for cell cycle regulatory proteins in cisplatin-induced AKI are discovered, it is promising that co-treatment with factors promoting cell cycle arrest and DNA repair may become a viable strategy for treating AKI. In future studies of cell cycle arrest in AKI, INK4 family members should no longer be ignored. Given that many questions remain regarding the ERS pathway during AKI induced by cisplatin nephrotoxicity or other toxic drugs, our study should be beneficial for future research on the ERS pathway.
In conclusion, we demonstrated that p18 overexpression significantly attenuated cisplatin-induced renal cell apoptosis, although it had no significant effect on necrosis. The highlights of our study are the discovery that p18 regulates the cell cycle and cell death pathways, such as the ERS pathway, against cisplatin-induced renal cell injury. However, the exact signal transduction pathways connecting p18 to cell death pathways still need to be investigated in detail.
References
Waikar SS, Liu KD, Chertow GM (2008) Diagnosis, epidemiology and outcomes of acute kidney injury. Clin J Am Soc Nephrol 3:844–861
Okusa MD (2002) The inflammatory cascade in acute ischemic renal failure. Nephron 90:133–138
Ramesh G, Reeves WB (2002) TNF-α mediates cytokine and cytokine expression and renal injury in cisplatin nephrotoxicity. J Clin Invest 110:835–842
Oh DJ, Dursun B, He Z, Lu L, Hoke TS, Ljubanovic D, Faubel S, Edelstein CL (2008) Fractalkine receptor (CX3CR1) inhibition is protective against ischemic acute renal failure in mice. Am J Physiol Renal Physiol 294:F264–F271
Del Rio M, Imam A, DeLeon M, Gomez G, Mishra J, Ma Q, Parikh S, Devarajan P (2004) The death domain of kidney ankyrin interacts with Fas and promotes Fas-mediated cell death in renal epithelia. J Am Soc Nephrol 15:41–51
Devarajan P (2006) Update on mechanisms of ischemic acute kidney injury. J Am Soc Nephrol 17:1503–1520
Burne MJ, Daniels F, El Ghandour A, Mauiyyedi S, Colvin RB, O'Donnell MP, Rabb H (2001) Identification of the CD4+ T cell as a major pathogenic factor in ischemic acute renal failure. J Clin Invest 108:1283–1290
Jiang M, Pabla N, Murphy RF, Yang T, Yin XM, Degenhardt K, White E, Dong Z (2007) Nutlin-3 protects kidney cells during cisplatin therapy by suppressing Bax/Bak activation. J Biol Chem 282:2636–2645
Wei Q, Dong G, Yang T, Megyesi J, Price PM, Dong Z (2007) Activation and involvement of p53 in cisplatin-induced nephrotoxicity. Am J Physiol Renal Physiol 293:F1282–F1291
Cummings BS, Schnellmann RG (2002) Cisplatin-induced renal cell apoptosis: caspase 3-dependent and -independent pathways. J Pharmacol Exp Ther 302:8–17
Kroemer G, Galluzzi L, Vandenabeele P, Abrams J, Alnemri ES, Baehrecke EH, Blagosklonny MV, El-Deiry WS, Golstein P, Green DR, Hengartner M, Knight RA, Kumar S, Lipton SA, Malorni W, Nuñez G, Peter ME, Tschopp J, Yuan J, Piacentini M, Zhivotovsky B, Melino G (2009) Classification of cell death: recommendations of the nomenclature committee on cell death 2009. Cell Death Differ 16:3–11
Periyasamy-Thandavan S, Jiang M, Wei Q, Smith R, Yin XM, Dong Z (2008) Autophagy is cytoprotective during cisplatin injury of renal proximal tubular cells. Kidney Int 74:631–640
Shankland SJ, Wolf G (2000) Cell cycle regulatory proteins in renal disease: role in hypertrophy, proliferation, and apoptosis. Am J Physiol Renal Physiol 278:F515–F529
Morgan DO (1995) Principles of CDK regulation. Nature 374:131–134
Peter M, Herskowitz I (1994) Joining the complex: cyclin-dependent kinase inhibitory proteins and the cell cycle. Cell 79:181–184
Weinert T (1998) DNA damage and checkpoint pathways: molecular anatomy and interactions with repair. Cell 94:555–558
Price PM, Safirstein RL, Megyesi J (2009) The cell cycle and acute kidney injury. Kidney Int 76:604–613
Megyesi J, Safirstein RL, Price PM (1998) Induction of p21WAF1/CIP1/SDI1 in kidney tubule cells affects the course of cisplatin-induced acute renal failure. J Clin Invest 101:777–782
Nowak G, Price PM, Schnellmann RG (2003) Lack of a functional p21WAF1/CIP1 gene accelerates caspase-independent apoptosis induced by cisplatin in renal cells. Am J Physiol Renal Physiol 285:F440–F450
Yu F, Megyesi J, Safirstein RL, Price PM (2005) Identification of the functional domain of p21(WAF1/CIP1) that protects cells from cisplatin cytotoxicity. Am J Physiol Renal Physiol 289:F514–F520
Megyesi J, Andrade L, Vieira JM Jr, Safirstein RL, Price PM (2002) Coordination of the cell cycle is an important determinant of the syndrome of acute renal failure. Am J Physiol Renal Physiol 283:F810–F816
Price PM, Yu F, Kaldis P, Aleem E, Nowak G, Safirstein RL, Megyesi J (2006) Dependence of cisplatin-induced cell death in vitro and in vivo on cyclin-dependent kinase 2. J Am Soc Nephrol 17:2434–2442
Yu F, Megyesi J, Price PM (2008) Cytoplasmic initiation of cisplatin cytotoxicity. Am J Physiol Renal Physiol 295:F44–F452
Price PM, Safirstein RL, Megyesi J (2004) Protection of renal cells from cisplatin toxicity by cell cycle inhibitors. Am J Physiol Renal Physiol 286:F378–F384
Hengst L, Reed SI (1998) Inhibitors of the Cip/Kip family. Curr Top Microbiol Immunol 227:25–41
Sherr CJ, Roberts JM (1995) Inhibitors of mammalian G1 cyclin-dependent kinases. Genes Dev 9:1149–1163
Cordon-Cardo C (1995) Mutation of cell cycle regulators. Biological and clinical implications for human neoplasia. Am J Pathol 147:545–560
Cánepa ET, Scassa ME, Ceruti JM, Marazita MC, Carcagno AL, Sirkin PF, Ogara MF (2007) INK4 proteins, a family of mammalian CDK inhibitors with novel biological functions. IUBMB Life 59:419–426
Guan KL, Jenkins CW, Li Y, Nichols MA, Wu X, O’Keefe CL, Matera AG, Xiong Y (1994) Growth suppression by p18, a p16INK4/MTS1- and p14INK4B/MTS2-related CDK6 inhibitor, correlates with wild-type pRb function. Genes Dev 8:2939–2952
Hirai H, Roussel MF, Kato JY, Ashmun RA, Sherr CJ (1995) Novel INK4 proteins, p19 and p18, are specific inhibitors of the cyclin D-dependent kinases CDK4 and CDK6. Mol Cell Biol 15:2672–2681
Choi KS, Eom YW, Kang Y, Ha MJ, Rhee H, Yoon JW, Kim SJ (1999) Cdc2 and Cdk2 kinase activated by transforming growth factor-beta1 trigger apoptosis through the phosphorylation of retinoblastoma protein in FaO hepatoma cells. J Biol Chem 274:31775–31783
Wang D, Lippard SJ (2005) Cellular processing of platinum anticancer drugs. Nat Rev Drug Discov 4:307–320
Siddik ZH (2003) Cisplatin: mode of cytotoxic action and molecular basis of resistance. Oncogene 22:7265–7279
Pabla N, Dong Z (2008) Cisplatin nephrotoxicity: mechanisms and renoprotective strategies. Kidney Int 73:994–1007
Lieberthal W, Triaca V, Levine J (1996) Mechanisms of death induced by cisplatin in proximal tubular epithelial cells: apoptosis vs. necrosis. Am J Physiol 270:F700–F708
Razzaque MS, Koji T, Kumatori A, Taguchi T (1999) Cisplatin-induced apoptosis in human proximal tubular epithelial cells is associated with the activation of the Fas/Fas ligand system. Histochem Cell Biol 111:359–365
Seth R, Yang C, Kaushal V, Shah SV, Kaushal GP (2005) p53-dependent caspase-2 activiation in mitochondrial release of apoptosis-inducing factor and its role in renal tubular epithelial cell injury. J Biol Chem 280:31230–31239
Park MS, De Leon M, Devarajan P (2002) Cisplatin induces apoptosis in LLC-PK1 cells via activation of mitochondrial pathways. J Am Soc Nephrol 13:858–865
Huang Q, Dunn RT 2nd, Jayadev S, DiSorbo O, Pack FD, Farr SB, Stoll RE, Blanchard KT (2001) Assessment of cisplatin-induced nephrotoxicity by microarray technology. Toxicol Sci 63:196–207
Muruganandan S, Cribb AE (2006) Calpain-induced endoplasmic reticulum stress and cell death following cytotoxic damage to renal cells. Toxicol Sci 94:118–128
Cribb AE, Peyrou M, Muruganandan S, Schneider L (2005) The endoplasmic reticulum in xenobiotic toxicity. Drug Metab Rev 37:405–442
Peyrou M, Hanna PE, Cribb AE (2007) Cisplatin, gentamicin, and p-aminophenol induce markers of endoplasmic reticulum stress in the rat kidneys. Toxicol Sci 99:346–353
Liu H, Baliga R (2005) Endoplasmic reticulum stress-associated caspase 12 mediates cisplatin-induced LLC-PK1 cell apoptosis. J Am Soc Nephrol 16:1985–1992
Bernales S, Papa FR, Walter P (2006) Intracellular signaling by the unfolded protein response. Annu Rev Cell Dev Biol 22:487–508
Lin JH, Walter P, Yen TS (2008) Endoplasmic reticulum stress in disease pathogenesis. Annu Rev Pathol 3:399–425
Malhotra JD, Kaufman RJ (2007) The endoplasmic reticulum and the unfolded protein response. Semin Cell Dev Biol 18:716–731
Mori K (2000) Tripartite management of unfolded proteins in the endoplasmic reticulum. Cell 101:451–454
Kleizen B, Braakman I (2004) Protein folding and quality control in the endoplasmic reticulum. Curr Opin Cell Biol 16:343–349
Zhang K, Kaufman RJ (2006) The unfolded protein response: a stress signaling pathway critical for health and disease. Neurology 66:S102–S109
Marciniak SJ, Ron D (2006) Endoplasmic reticulum stress signaling in disease. Physiol Rev 86:1133–1149
Szegezdi E, Logue SE, Gorman AM, Samali A (2006) Mediators of endoplasmic reticulum stress-induced apoptosis. EMBO Rep 7:880–885
Nakagawa T, Zhu H, Morishima N, Li E, Xu J, Yankner BA, Yuan J (2000) Caspase 12 mediates ER-specific apoptosis and cytotoxicity by amyloid-β. Nature 403:98–103
Kalai M, Lamkanfi M, Denecker G, Boogmans M, Lippens S, Meeus A, Declercq W, Vandenabeele P (2003) Regulation of the expression and processing of caspase 12. J Cell Biol 162:457–467
Oyadomari S, Mori M (2004) Role of CHOP/GADD153 in endoplasmic reticulum stress. Cell Death Differ 11:381–389
Kondo S, Barna BP, Kondo Y, Tanaka Y, Casey G, Liu J, Morimura T, Kaakaji R, Peterson JW, Werbel B, Barnett GH (1996) WAF1/CIP1 increases the susceptibility of p53 non-functional malignant glioma cells to cisplatin-induced apoptosis. Oncogene 13:1279–1285
Lincet H, Poulain L, Remy JS, Deslandes E, Duigou F, Gauduchon P, Staedel C (2000) The p21(cip1/waf1) cyclin-dependent kinase inhibitor enhances the cytotoxic effect of cisplatin in human ovarian carcinoma cells. Cancer Lett 161:17–26
Franklin DS, Godfrey VL, Lee H, Kovalev GI, Schoonhoven R, Chen-Kiang S, Su L, Xiong Y (1998) CDK inhibitors p18INK4c and p27Kip1 mediate two separate pathways to collaboratively suppress pituitary tumorigenesis. Genes Dev 12:2899–2911
Al-Mohanna MA, Manogaran PS, Al-Mukhalafi Z, A Al-Hussein K, Aboussekhra A (2004) The tumor suppressor p16(INK4a) gene is a regulator of apoptosis induced by ultraviolet light and cisplatin. Oncogene 23:201–212
Le HV, Minn AJ, Massagué J (2005) Cyclin-dependent kinase inhibitors uncouple cell cycle progression from mitochondrial apoptotic functions in DNA-damaged cancer cells. J Biol Chem 280:32018–32025
Scassa ME, Marazita MC, Ceruti JM, Carcagno AL, Sirkin PF, González-Cid M, Pignataro OP, Cánepa ET (2007) Cell cycle inhibitor, p19INK4d, promotes cell survival and decreases chromosomal aberrations after genotoxic insult due to enhanced DNA repair. DNA Repair 6:626–638
Tavera-Mendoza LE, Wang TT, White JH (2006) p19INK4D and cell death. Cell Cycle 5:596–598
Massagué J (2004) G1 cell-cycle control and cancer. Nature 432:298–306
Trimarchi JM, Lees JA (2002) Sibling rivalry in the E2F family. Nat Rev Mol Cell Biol 3:11–20
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, Y., Yuan, L., Fu, L. et al. Overexpression of p18INK4C in LLC-PK1 cells increases resistance to cisplatin-induced apoptosis. Pediatr Nephrol 26, 1291–1301 (2011). https://doi.org/10.1007/s00467-011-1877-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-011-1877-y