Abstract
Nephrin is a podocyte adhesion molecule located at the slit diaphragm between adjacent glomerular epithelial cells. Mutations in the gene encoding nephrin result in the absence of nephrin or alterations in nephrin causing massive proteinuria in patients with congenital nephrotic syndrome. Given the importance of nephrin to the structural integrity of the glomerular filtration barrier, we postulated that it might also be altered in acquired forms of nephrotic syndrome (NS). To test this hypothesis, frozen kidney biopsy sections from 29 pediatric patients with acquired NS and 5 controls were examined for expression of nephrin. The pathological diagnoses were minimal change disease (MCNS) (19) and focal segmental glomerulosclerosis (FSGS) (10). To determine if nephrin expression differed between children and adults with NS, 10 adult patients and 3 controls were also examined. Nephrin expression was evaluated by immunoperoxidase staining with a monoclonal antibody against the extracellular FnIII portion of human nephrin. In all cases, nephrin expression was seen along the glomerular basement membrane in a finely granular/linear pattern. Expression of nephrin was similar to controls in all 19 patients with MCNS and all 10 patients with FSGS. Areas of sclerosis in patients with FSGS did not demonstrate nephrin expression. A distinctly granular pattern to nephrin expression was seen in adult patients with NS as well as controls. These findings suggest that an alteration in nephrin expression is not a feature of acquired forms of NS in childhood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acquired nephrotic syndrome (NS) is characterized by proteinuria, hypoalbuminemia, edema, and hypercholesterolemia. The incidence of idiopathic NS is approximately 2–7 cases per 100,000 and it primarily affects children between the ages of 1 and 6 years [1, 2]. The two most common types of NS in children are minimal change nephrotic syndrome (MCNS) and focal segmental glomerulosclerosis (FSGS). The clinical and laboratory manifestations of edema, hypoalbuminemia, and proteinuria correlate with ultrastructural changes within the glomerulus, specifically of the glomerular visceral epithelial cells or podocytes. The glomerular filtration barrier consists of a fenestrated endothelial layer, an extracellular glomerular basement membrane, and overlying podocytes with their interdigitating foot processes and slit diaphragms [3]. The most characteristic pathological alteration is effacement and retraction of the foot processes with loss of the integrity of the filtration barrier and slit diaphragms (reviewed in [3]). The molecular mechanisms leading to podocyte effacement and loss of an intact filtration barrier remain unclear. However, recent studies have identified key components of the glomerular filtration barrier offering new insights into the pathogenesis of proteinuria.
Certain inherited diseases may be associated with NS. The prototype is congenital nephrotic syndrome of the Finnish type (CNF), an autosomal recessive disease that affects approximately 1 in 10,000 births in Finland. CNF is also characterized by fusion of foot processes. Studying 29 affected families, Tryggvason [4] identified a gene (NPHS1) that encodes nephrin, a protein that is altered in these patients. Nephrin is a 1,241-amino acid glycoprotein member of the immunoglobulin (Ig) superfamily consisting of eight extracellular Ig domains and one fibronectin-type III domain. Based on its structure, it is believed to be a podocyte adhesion molecule and it may play a role in signal transduction. Both immunofluorescence staining and immunoelectron microscopy have localized nephrin specifically to the area of the slit diaphragm [5]. Further ultrastructural studies in the CNF population confirmed the importance of nephrin in the development of the ladder-like structure of the slit diaphragm and filtration barrier [6]. Mutations in NPHS1, resulting in the absence of or alterations in the nephrin protein, are presumed to contribute to the lack of a slit diaphragm and massive proteinuria seen in patients with CNF. The sequence of cellular and molecular events between nephrin loss and proteinuria are currently under investigation in several laboratories.
Given the similar pathological findings between CNF and idiopathic NS and the importance of nephrin to the structural integrity of the glomerular filtration barrier, we hypothesized that nephrin expression may also be altered in idiopathic forms of childhood NS.
Materials and methods
Patient selection
Pediatric patients with a biopsy-proven diagnosis of MCNS or FSGS made between 1996 and 2001 at our institution were included in the study. Adults with MCNS and FSGS studied at the University of Washington between 2002 and 2003 were used for comparison. Percutaneous needle or open-wedge kidney biopsies were performed in children with NS that was unresponsive to an 8-week course of prednisone, or that followed a complicated clinical course with frequent relapses and/or steroid dependency. All biopsies were analyzed by light microscopy, immunofluorescence (IF), and electron microscopy (EM). The diagnosis was based on typical pathological, clinical, and laboratory data. Cases from the last 5 years were reviewed and those with adequate residual frozen tissue were selected for staining. Prior approval for these studies was obtained from our institutional review board.
Data collected from the pediatric patient charts included serum albumin and creatinine, urinalysis, quantification of proteinuria either by spot urinary protein/creatinine ratios or 24-h urine collections when available, and medications at the time of biopsy. Medications included prednisone, cyclosporine, and Cytoxan. Not all patients received therapy prior to the biopsy.
Kidney immunohistochemistry
OCT-embedded tissue was cut at 5 μm and fixed in cold acetone for 1 min. Two slides, each containing two tissue sections, were prepared for each case. Sections were air dried, washed in phosphate-buffered saline, and treated sequentially with 0.6% hydrogen peroxide/methanol and an avidin/biotin block (Avidin-Biotin Blocking Kit, Vector Laboratories, Burlingame, Calif., USA) to quench endogenous peroxidase and biotin and eliminate background staining. Blocking was achieved with mouse blocking serum (Vector Laboratories). Slides were incubated at room temperature for 2 h with a mouse monoclonal antibody (1:200 dilution) directed against the extracellular FnIII portion of human nephrin (gift from Dr. Vesa Ruotsalainen, Oulu, Finland). The antibody was detected using avidin-biotin-horseradish peroxidase (Vectastain ABC Immunoperoxidase Kit, Vector) followed by color visualization with 3,3′-diaminobenzidine tetrahydrochloride (DAB, Sigma, St. Louis, Mo., USA). Slides were counterstained with Gill’s hematoxylin. Negative controls, treated identically except for omission of the primary antibody, were run for each case. Test cases contained at least 2 glomeruli (range 2–26) on each section. Positive controls included the following: normal kidney tissue obtained at the time of nephrectomy for Wilms tumor (n=1), normal kidney tissue obtained at autopsy of patients without renal disease (n=2), and protocol allograft kidney biopsies from asymptomatic patients (n=2). A kidney biopsy obtained from a 6-week-old infant diagnosed with NS at 1 week of age whose light microscopic, IF, and EM pathology was consistent with congenital NS of the Finnish type was also stained.
Adult samples were handled in an identical manner, although some biopsies had been transported in tissue culture media and were washed in neutral phosphate buffer prior to freezing in OCT. Positive controls included allograft kidney biopsies from 3 asymptomatic patients.
Results
In total, 29 renal biopsies from 20 males and 9 females, ranging in age from 7 months to 18 years 10 months (mean age 7 years, 4 months) at the time of biopsy, were studied. The pathological diagnoses were MCNS in 19 cases and FSGS in 10 cases, based on standard pathological criteria by light microscopy, IF, and EM (Table 1). Ultrastructural examination revealed evidence of fused podocyte foot processes in all test specimens. Just prior to renal biopsy, the serum albumin levels ranged from 1.3 to 3.8 mg/dl and serum creatinine ranged from 0.3 to 1.7 mg/dl. All patients with FSGS had proteinuria. Proteinuria in patients with MCNS varied from negative to 3+ on dipstick prior to the biopsy.
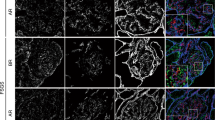
Immunoperoxidase staining of frozen tissue from patients with MCNS and FSGS detected expression for the extracellular domain of nephrin along the glomerular basement membrane in a linear to faintly granular pattern in all patients (Fig. 1a). Slight variability in staining intensity was noted. There was light staining of nephrin in the podocytes of some glomeruli, which was more obvious in the youngest patients. The expression of nephrin in controls was similar to the patients with MCNS and FSGS (Fig. 1b). Global or segmental absence of nephrin expression along the intact basement membrane was not observed in any patient. Although areas of sclerosis in patients with FSGS did not stain with nephrin, the non-sclerotic segments and other glomeruli from the same biopsy showed normal expression (Fig. 1c). Nephrin expression was not found in the glomerular basement membrane from the patient with congenital NS (Fig. 1d).
a Minimal change disease. Antibodies directed against the extracellular portion of nephrin showed a linear to mildly granular pattern of expression. This glomerulus demonstrates uniform staining along the glomerular basement membrane [diaminobenzidine (DAB) original magnification, 400×]. b Normal control. Nephrin is demonstrated along the glomerular basement membrane in a smooth, slightly granular pattern (DAB, original magnification, 400×). c Focal segmental glomerulosclerosis (FSGS). The sclerotic segment of the glomerulus (arrowheads) shows no nephrin expression, while the basement membrane in the more-intact, although partially collapsed, region has obvious membrane staining (DAB, original magnification, 400×). d Congenital nephrotic syndrome. The glomeruli in this young infant showed no nephrin expression along the basement membrane, consistent with the Finnish type of congenital nephrotic syndrome (DAB, original magnification, 400×)
We included 4 adult patients with MCNS, 6 with FSGS and 3 adult controls. Immunoperoxidase staining for nephrin showed positivity along the glomerular basement membrane in all cases in a granular pattern that never achieved the smooth linear appearance seen in many of the children. There was no staining in the focally sclerotic regions, similar to the pediatric cases (Fig. 2), although intact segments of the glomerulus expressed nephrin. There was no significant difference in nephrin expression between adult patients with NS and the adult control samples.
Similar to FSGS in the child (Fig. 1c), there is no staining for nephrin in the sclerotic region of the glomerulus (arrow) from this adult patient. Undamaged areas of the glomerulus often showed a granular expression pattern along the basement membrane (DAB, original magnification, 400×)
Discussion
NS of childhood is a common illness that causes significant morbidity and mortality. The recent identification of mutations clustering within a single gene (NPHS1) in an inheritable form of NS (CNF) has provided the first insights into the molecular pathogenesis of proteinuria and resulted in a number of recent studies attempting to elucidate the role of nephrin in inherited and sporadic glomerular diseases.
This study focused on MCNS and FSGS, most common forms of acquired NS seen in the pediatric population. While these diseases also affect adults, they often follow different clinical courses in the two populations and respond differently to steroids. We found no difference in the expression of nephrin in 29 children with acquired NS compared with normal control kidneys. Immunohistochemical analyses showed a similar pattern of nephrin distribution along the glomerular capillary wall in both nephrotic patients and controls. The linear to slightly granular expression pattern and variable intensity was also similar in both groups. The single exception was the absence of nephrin in the regions of segmental glomerular sclerosis in patients with FSGS. Although we also noticed a uniformly more granular pattern of staining in adult patients with MCNS and FSGS, this was not significantly different from the adult controls. Our results are consistent with the findings of Patrakka et al. [7] who also reported no major alterations in the expression of nephrin using immunohistochemistry and in situ hybridization in MCNS, FSGS, and membranous nephropathy (MN). Although nephrin mRNA levels were not measured in our samples, Patrakka et al. [7] reported no major difference in the expression of nephrin mRNA in the samples from patients with MCNS and FSGS compared with controls.
However, other published studies report conflicting findings (Table 2). Decreased nephrin mRNA expression was found in an isolated glomerulus using the polymerase chain reaction from three adult patients with MCNS compared with controls [8]. Given the possibility of inter-glomerular heterogeneity and a sample of only 1 glomerulus per patient, the differences in results may be due to sampling bias. Doublier et al. [9] investigated the distribution of nephrin in the acquired proteinuric diseases MCNS, MN, and FSGS. Using indirect IF, they found a shift in the fluorescence pattern for nephrin from linear to granular and a loss of signal in patients with all types of NS compared with controls. Based on the relative diminution of the fluorescence intensity in proteinuric patients, the authors suggested that changes in nephrin expression are not specific to a particular disease but rather to the proteinuric state. Notably, however, there was no inverse correlation between the nephrin fluorescence intensity and degree of proteinuria. The variation in results may partly reflect different techniques for investigation.
Experimental animal models also support a role for nephrin in the primary pathogenesis of proteinuria [10, 11]. In an experimental rat model of MN, nephrin was shown to dissociate from actin at the onset of podocyte injury. There was progressive loss of nephrin from the foot process and changes in the morphology of the slit diaphragm [12].
There may be age-dependent differences in glomerular expression of nephrin, as has been suggested for glomerular endothelial cell expression of the Gb3 shiga toxin receptor [13, 14, 15]. The different staining patterns, linear versus granular, in the pediatric and adult patients with NS and controls in this study may reflect differential expression or distribution of nephrin. It is difficult to comment on variation of expression of nephrin with age using immunohistochemistry alone. Various studies of adult patients with NS describe a granular pattern of nephrin staining compared with the linear pattern of their normal controls [9, 16, 17]. Wernerson et al. [17] found a direct correlation between the degree of foot process effacement and nephrin granularity using IF. Using immunoelectron microscopy and gold-labeled antibodies, proportionally more nephrin was located in the cytoplasm than the slit diaphragm in patients with NS compared with controls . Nephrin redistribution from the plasma membrane has also been reported by others [9]. These investigators postulated that this granular pattern represents a dislocation or displacement of nephrin from the slit diaphragm [9, 17]. Perhaps the altered distribution of nephrin in adults with NS reflects a more severe disease process or different pathophysiology than in children. This possibility deserves further investigation given that only 3 of 32 previously published MCNS patients with decreased nephrin expression were children and 11 of 14 children had normal expression, whereas all 18 adults had decreased expression (summarized in Table 2). In previously published studies of patients with FSGS, only 3 of 5 children had abnormal nephrin expression compared with 18 of 18 adults with abnormal expression. Once podocytes are lost as the glomerulus scars in FSGS, nephrin immunoreactivity disappears in all patients.
Our findings suggest that a significant reduction in nephrin expression is not the primary mechanism underlying proteinuria in idiopathic forms of NS in childhood. It is still possible that altered nephrin distribution (not identifiable by light microscopy) or altered nephrin function could play an important pathogenetic role. Single gene mutations in nephrin can lead to profound nephrosis. Such ‘missense’ mutations can lead to misfolding of the mutant nephrin and cause its retention in the endoplasmic reticulum rather than transport to the cell membrane [18]. Based on its structure, nephrin is also thought to play a role in signal transduction, so it is feasible that alterations in the downstream signaling pathways lead to podocyte effacement and proteinuria rather than alterations in the protein itself [19]. Interactions between nephrin, podocin, and CD2AP have also been demonstrated in rat models [20]. Huber et al. [21] demonstrated that nephrin stimulates mitogen-activated protein kinases. This signaling pathway is further enhanced by interaction with podocin. They suggest that appropriate function of nephrin depends not only on it being present, but also on proper localization to the foot processes and efficient signaling.
The recent identification of podocin and alpha actinin mutations in familial forms of FSGS, as well as the localization of CD2AP in the glomerular filtration barrier, raises the question of whether interactions and alterations in the podocyte cytoskeleton, rather than exclusively in nephrin, contribute to the pathogenesis of proteinuria [22, 23, 24, 25]. CD2AP is an adapter protein thought to anchor nephrin to the cytoskeleton of the podocyte [24]. Mice deficient in CD2AP have congenital NS, although the human homologue of this disease has not yet been reported. Perturbations in the normal dynamic interactions between CD2AP, podocin, nephrin, and the podocyte cytoskeleton may also lead to proteinuria [20, 26]. By immunoelectron microscopy using a gold-conjugated polyclonal antibody against nephrin, Huh et al. [27] found that gold particles were absent in areas of podoctye effacement but preserved in areas with normal podocyte appearance. This further supported the idea that changes in the podocyte structure lead to alterations in nephrin expression. We attempted to stain kidney specimens from pediatric patients for CD2AP but were unsuccessful (data not shown).
Additional immunoelectron microscopic studies are needed to extend the observations of Huh et al. [27] and determine if subtle differences in nephrin distribution occur in pediatric idiopathic MCNS and FSGS. While future cell biological studies should delineate the functional role of nephrin in podocyte effacement and pathological proteinuria, the findings of the present study suggest that loss of nephrin protein is neither a prerequisite nor a common finding in idiopathic childhood NS.
In summary, in the present study, nephrin immunohistochemical studies did not detect significant differences in glomerular nephrin protein expression or localization patterns between normal kidneys and the kidneys of children with NS due to MCNS or FSGS. Complete absence of glomerular nephrin expression appears to be restricted to patients with congenital NS due to inherited NPHS mutations. Further studies are indicated to determine if alterations in nephrin function or distribution rather than its expression levels represent a common pathway to proteinuria in acquired forms of idiopathic NS in childhood.
References
Chesney RW (1999) The idiopathic nephrotic syndrome. Curr Opin Pediatr 11:158–161
McKinney PA, Feltbower RG, Brocklebank JT, Fitzpatrick MM (2001) Time trends and ethnic patterns of childhood nephrotic syndrome in Yorkshire, UK. Pediatr Nephrol 16:1040–1044
Smoyer WE, Mundel P (1998) Regulation of podocyte structure during the development of nephrotic syndrome. J Mol Med 76:172–183
Tryggvason K (1999) Unraveling the mechanisms of glomerular ultrafiltration: nephrin, a key component of the slit diaphragm. J Am Soc Nephrol 10:2440–2445
Ruotsalainen V, Ljungberg P, Wartiovaara J, Lenkkeri U, Kestila M, Jalanko H, Holmberg C, Tryggvason K (1999) Nephrin is specifically located at the slit diaphragm of glomerular podocytes. Proc Natl Acad Sci U S A 96:7962–7967
Ruotsalainen V, Patrakka J, Tissari P, Reponen P, Hess M, Kestila M, Holmberg C, Salonen R, Heikinheimo M, Wartiovaara J, Tryggvason K, Jalanko H (2000) Role of nephrin in cell junction formation in human nephrogenesis. Am J Pathol 157:1905–1916
Patrakka J, Ruotsalainen V, Ketola I, Holmberg C, Heikinheimo M, Tryggvason K, Jalanko H (2001) Expression of nephrin in pediatric kidney diseases. J Am Soc Nephrol 12:289–296
Furness PN, Hall LL, Shaw JA, Pringle JH (1999) Glomerular expression of nephrin is decreased in acquired human nephrotic syndrome. Nephrol Dial Transplant 14:1234–1237
Doublier S, Ruotsalainen V, Salvidio G, Lupia E, Biancone L, Conaldi PG, Reponen P, Tryggvason K, Camussi G (2001) Nephrin redistribution on podocytes is a potential mechanism for proteinuria in patients with primary acquired nephrotic syndrome. Am J Pathol 158:1723–1731
Luimula P, Aaltonen P, Ahola H, Palmen T, Holthofer H (2000) Alternatively spliced nephrin in experimental glomerular disease of the rat. Pediatr Res 48:759–762
Rantanen M, Palmen T, Patari A, Ahola H, Lehtonen S, Astrom E, Floss T, Vauti F, Wurst W, Ruiz P, Kerjaschki D, Holthofer H (2002) Nephrin TRAP mice lack slit diaphragms and show fibrotic glomeruli and cystic tubular lesions. J Am Soc Nephrol 13:1586–1594
Yuan H, Takeuchi E, Taylor G A, McLaughlin M, Brown D, Salant DJ (2002) Nephrin dissociates from actin, and its expression is reduced in early experimental membranous nephropathy. J Am Soc Nephrol 13:946–956
Mobassaleh M, Donohue-Rolfe A, Jacewicz M, Grand RJ, Keusch GT (1988) Pathogenesis of shigella diarrhea: evidence for a developmentally regulated glycolipid receptor for shigella toxin involved in the fluid secretory response of rabbit small intestine. J Infect Dis 157:1023–1031
Mobassaleh M, Gross SK, McCluer RH, Donohue-Rolfe A, Keusch GT (1989) Quantitation of the rabbit intestinal glycolipid receptor for Shiga toxin. Further evidence for the developmental regulation of globotriaosylceramide in microvillus membranes. Gastroenterology 97:384–391
Mobassaleh M, Koul O, Mishra K, McCluer RH, Keusch GT (1994) Developmentally regulated Gb3 galactosyltransferase and alpha-galactosidase determine Shiga toxin receptors in intestine. Am J Physiol 267:G618–G624
Kim KB, Hong KH, Kim HJ, Lee SH (2002) Differential expression of nephrin in acquired human proteinuric diseases. Am J Kidney Dis 40:964–973
Wernerson A, Dunér F, Pettersson E, Widholm SM, Berg U, Ruotsalainen V, Tryggvason K, Hultenby K, Söderberg M (2003) Altered ultrastructural distribution of nephrin in minimal change nephrotic syndrome. Nephrol Dial Transplant 18:70–76
Liu L, Done SC, Khoshnoodi J, Bertorello A, Wartiovaara J, Berggren PO, Tryggvason K (2001) Defective nephrin trafficking caused by missense mutations in the NPHS1 gene: insight into the mechanisms of congenital nephrotic syndrome. Hum Mol Genet 10:2637–2644
Tryggvason K (2001) Nephrin: role in normal kidney and in disease. Adv Nephrol Necker Hosp 31:221–234
Schwarz K, Simons M, Reiser J, Saleem M A, Faul C, Kriz W, Shaw AS, Holzman LB, Mundel P (2001) Podocin, a raft-associated component of the glomerular slit diaphragm, interacts with CD2AP and nephrin. J Clin Invest 108:1621–1629
Huber TB, Kottgen M, Schilling B, Walz G, Benzing T (2001) Interaction with podocin facilitates nephrin signaling. J Biol Chem 276:41543–41546
Tsukaguchi H, Yager H, Dawborn J, Jost L, Cohlmia J, Abreu PF, Pereira AB, Pollak MR (2000) A locus for adolescent and adult onset familial focal segmental glomerulosclerosis on chromosome 1q25-31. J Am Soc Nephrol 11:1674–1680
Boute N, Gribouval O, Roselli S, Benessy F, Lee H, Fuchshuber A, Dahan K, Gubler MC, Niaudet P, Antignac C (2000) NPHS2, encoding the glomerular protein podocin, is mutated in autosomal recessive steroid-resistant nephrotic syndrome. Nat Genet 24:349–354
Shih NY, Li J, Karpitskii V, Nguyen A, Dustin ML, Kanagawa O, Miner JH, Shaw AS (1999) Congenital nephrotic syndrome in mice lacking CD2-associated protein. Science 286:312–315
Kaplan JM, Kim SH, North KN, Rennke H, Correia LA, Tong HQ, Mathis BJ, Rodriguez-Perez JC, Allen PG, Beggs AH, Pollak MR (2000) Mutations in ACTN4, encoding alpha-actinin-4, cause familial focal segmental glomerulosclerosis. Nat Genet 24:251–256
Lehtonen S, Zhao F, Lehtonen E (2002) CD2-associated protein directly interacts with the actin cytoskeleton. Am J Physiol Renal Physiol 283:F734–F743
Huh W, Kim DJ, Kim MK, Kim YG, Oh HY, Ruotsalainen V, Tryggvason K (2002) Expression of nephrin in acquired human glomerular disease. Nephrol Dial Transplant 17:478–484
Srivastava T, Whiting JM, Garola RE, Dasouki MJ, Ruotsalainen V, Tryggvason K, Hamed R, Alon US (2001) Podocyte proteins in Galloway-Mowat syndrome. Pediatr Nephrol 16:1022–1029
Wang SX, Rastaldi MP, Patari A, Ahola H, Heikkila E, Holthofer H (2002) Patterns of nephrin and a new proteinuria-associated protein expression in human renal diseases. Kidney Int 61:141–147
Acknowledgements
The antibodies used in this study were kindly provided by Dr. Vesa Ruotsalainen, Oulu, Finland. This work was supported in part by grants from the National Institutes of Health DK07662 (S.R.H.), DK54500 (A.A.E.), and DK4757 (A.A.E.), the National Kidney Foundation and American Society of Nephrology and Renal Physicians Association (S.R.H.). We would also like to thank Marena Hawk for her administrative assistance in preparing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hingorani, S.R., Finn, L.S., Kowalewska, J. et al. Expression of nephrin in acquired forms of nephrotic syndrome in childhood. Pediatr Nephrol 19, 300–305 (2004). https://doi.org/10.1007/s00467-003-1346-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-003-1346-3