Abstract
Introduction
Robotic inguinal hernia repair is growing in popularity among general surgeons despite little high-quality evidence supporting short- or long-term advantages over traditional laparoscopic inguinal hernia repair. The original RIVAL trial showed increased operative time, cost, and surgeon frustration for the robotic approach without advantages over laparoscopy. Here we report the 1- and 2-year outcomes of the trial.
Methods
This is a multi-center, patient-blinded, randomized clinical study conducted at six sites from 2016 to 2019, comparing laparoscopic versus robotic transabdominal preperitoneal (TAPP) inguinal hernia repair with follow-up at 1 and 2 years. Outcomes include pain (visual analog scale), neuropathic pain (Leeds assessment of neuropathic symptoms and signs pain scale), wound morbidity, composite hernia recurrence (patient-reported and clinical exam), health-related quality of life (36-item short-form health survey), and physical activity (physical activity assessment tool).
Results
Early trial participation included 102 patients; 83 (81%) completed 1-year follow-up (45 laparoscopic vs. 38 robotic) and 77 (75%) completed 2-year follow-up (43 laparoscopic vs. 34 robotic). At 1 and 2 years, pain was similar for both groups. No patients in either treatment arm experienced neuropathic pain. Health-related quality of life and physical activity were similar for both groups at 1 and 2 years. No long-term wound morbidity was seen for either repair type. At 2 years, there was no difference in hernia recurrence (1 laparoscopic vs. 1 robotic; P = 1.0).
Conclusions
Laparoscopic and robotic inguinal hernia repairs have similar long-term outcomes when performed by surgeons with experience in minimally invasive inguinal hernia repairs.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Laparoscopic inguinal hernia repair, introduced in 1991 [1], is an accepted alternative to open inguinal hernia repair [2]. Both approaches have similar hernia recurrence rates, but laparoscopic inguinal hernia repair also offers less short- and long-term postoperative pain compared to open repair [3]. The advantages of laparoscopic inguinal hernia repair have led to early enthusiasm for an alternative minimally invasive approach—robotic inguinal hernia repair.
Robotic inguinal hernia repair has grown exponentially since it was first described in the general surgery literature in 2015 [4, 5]. The reasons for this growth are not entirely clear, but may be partly due to the perceived advantages of the robot over traditional laparoscopy, including enhanced optics and wristed instruments with many degrees of freedom. Despite its perceived advantages, little evidence supports clinical or patient-reported benefits of the robot over laparoscopic inguinal hernia repair [6, 7]. Furthermore, robotic inguinal hernia repair is consistently associated with higher costs than traditional laparoscopy [8].
The RIVAL trial prospectively compared laparoscopic to robotic inguinal hernia repair and found similar clinical and patient-reported outcomes for both operations at 30 days postoperatively [9]. Here we compare the 1- and 2-year outcomes of the two approaches to inguinal hernia repair.
Methods
This study analyzed the 1- and 2-year outcomes of a multi-center, patient-blinded, randomized clinical study, which compared laparoscopic to robotic transabdominal preperitoneal (TAPP) inguinal hernia repair. Trial design and early outcomes were previously published [9]. The trial was registered at ClinicalTrials.gov as NCT #02816658. Institutional Review Board approval was granted at all participating sites, and all study participants provided written informed consent. The RIVAL trial was funded by an unrestricted grant from Intuitive Surgical, Inc.
All patients were at least 21 years old, had a primary or recurrent unilateral inguinal hernia, and a BMI ≤ 40 kg/m2. All surgeons were fellowship-trained in minimally invasive surgery (MIS) and had performed at least 25 robotic and 25 laparoscopic procedures before participating. The entire operation was performed by the attending surgeon. A flat heavy-weight polypropylene mesh at least 10 cm × 15 cm was used for all repairs. In the laparoscopic repairs, the mesh was fixated with permanent spiral tacks and the peritoneum was closed with permanent spiral tacks. In the robotic repairs, the mesh was fixated with permanent suture and the peritoneum was closed with running suture of the surgeon’s choice.
Baseline patient-reported details were captured during the preoperative clinic visit. Postoperative outcomes were captured at 1 year ± 1 month and 2 years ± 2 months. Pain was assessed with the visual analog scale (VAS), which is a pain scale from 0 to 100, with 0 representing no pain and 100 being the worst possible pain [10]. Neuropathic pain was measured by the Leeds assessment of neuropathic symptoms and signs (LANSS) pain scale, a validated 7-item, 24-point scale, with scores over 12 indicating neuropathic pain [11].
Health-related quality of life was evaluated with the 36-item short-form health survey (SF-36), which measures 8 health concepts on a scale from 0 to 100, with 0 representing the worst quality of life and 100 representing the best quality of life [12]. These 8 health concepts are often aggregated into 2 groups—physical and mental component summaries—to facilitate interpretation of SF-36 results [13]. The physical component summary is comprised physical functioning, limitations due to physical health, pain, and general health. The mental component summary is comprised vitality, social functioning, limitations due to emotional health, and mental health.
Physical activity was evaluated by the physical activity assessment tool, which measures the type, frequency, and duration of moderate and vigorous physical activity from four areas of physical activity (leisure, occupational, household, and transportation) in the last 7 days, compared to the usual level of activity [14]. Wound morbidity was defined in the original RIVAL trial [9]. Composite hernia recurrence was defined as a bulge on physical exam or a patient-reported bulge, using the validated Hernia Recurrence Inventory [15].
Statistical analysis
Student’s t-tests or Wilcoxon rank sum tests compared continuous variables, and Chi-squared tests or Fisher’s exact tests compared categorical variables. Composite hernia recurrence was classified as binary (yes/no). All analyses were performed using R software (version 4.0.0, Vienna, Austria), and were considered significant at a 5% level.
Results
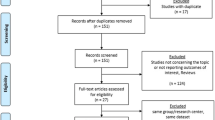
Of the 102 patients initially enrolled in the study, 54 (53%) underwent laparoscopic repair and 48 (47%) underwent robotic repair. At 1 year, 83 (81%) patients completed follow-up (45 laparoscopic and 38 robotic), and at 2 years, 77 (75%) patients completed follow-up (43 laparoscopic and 34 robotic). Overall pain measured by the VAS was similar for laparoscopic and robotic repairs at 1 year [5.68 (SD 11.1) vs. 3.50 (SD 5.55), respectively; P = 0.30] and 2 years [3.71 (SD 7.15) vs. 8.58 (SD 16.2), respectively; P = 0.17] (Fig. 1). The change from baseline pain (VAS) was also not significantly different between operative approaches [1-year laparoscopic: − 12.4 (SD 20.6) vs. 1-year robotic: − 14.16 (SD 19.8), P = 0.69; 2-year laparoscopic: − 2.30 (SD 12.6) vs. 2-year robotic: 0.71 (SD 16.6), P = 0.39]. Neuropathic pain was not present in either treatment arm at 1 year [33 laparoscopic: 0 (IQR 0;0) vs. 24 robotic: 0 (IQR 0;0)] or 2 years [17 laparoscopic: 0 (IQR 0;0) vs. 14 robotic: 0 (IQR 0;0)].
Health-related quality of life was similar for both treatment arms at 1 and 2 years for all categories assessed (Table 1). Physical component summaries were similar for laparoscopic and robotic repairs at 1 year [53.7 (SD 8.2) vs. 54.9 (SD 7.3), respectively; P = 0.51] and 2 years [54.2 (SD 6.1) vs. 53.1 (SD 8.1), respectively; P = 0.52]. Likewise, the long-term mental component summaries were similar for both repair types [1-year laparoscopic: 54.8 (SD 6.0) vs. 1-year robotic: 55.9 (SD 4.6), P = 0.38; 2-year laparoscopic: 53.4 (SD 5.6) vs. 2-year robotic: 53.9 (SD 6.8), P = 0.69].
Physical activity was similar for both operative approaches at 1 and 2 years (Table 2). Total time spent engaged in moderate physical activity (MPA) and vigorous physical activity (VPA) was not significantly different for laparoscopic and robotic repairs at 1 year [531 (SD 532) vs. 655 (SD 1127) minutes per week, respectively; P = 0.59] or 2 years [510 (SD 888) vs. 433 (SD 477) minutes per week, respectively; P = 0.68]. The long-term difference in MPA + VPA from baseline for both groups was also comparable [1-year laparoscopic: 141 (SD 838) vs. 1-year robotic: 384 (SD 1028), P = 0.25; 2-year laparoscopic: − 5.70 (SD 860) vs. 2-year robotic: 6.74 (SD 579), P = 0.94].
No long-term wound morbidity was seen in either group. At 2 years, there was no difference in inguinal hernia recurrence (1 laparoscopic vs 1 robotic; P = 1.0).
Discussion
The 1- and 2-year results of the RIVAL trial identified no significant long-term differences between laparoscopic and robotic inguinal hernia repair regarding pain, long-term health-related quality of life, or physical activity. No patients from either group developed neuropathic pain. At 2 years, hernia recurrence rates were the same for laparoscopic and robotic inguinal hernia repair.
In the original RIVAL trial, we found increased operative time, cost, and surgeon frustration for robotic compared to laparoscopic inguinal hernia repair [9]. A critique of the RIVAL trial was that some of the surgeons were perhaps still on the robotic learning curve [16], although 5 of the surgeons participating in the study were also proctors for Intuitive Surgical, Inc. and taught robotic hernia repairs. Our long-term results suggest that the robotic repairs were performed competently—at least as well as the laparoscopic repairs—as no long-term outcome differences were observed to suggest a learning curve effect. This is not surprising because the operations were performed by surgeons with experience in MIS groin anatomy and surgical technique, and the two repair approaches are similar aside from mesh fixation. We do not know if similar outcomes can be expected from less experienced surgeons.
The technique for robotic mesh fixation—sewing instead of tacking—offers a possible benefit of less early postoperative pain compared to laparoscopy in inguinal hernia repair [17]. This is supported by Kleidari et al. who found less early (< 7 days) postoperative pain for laparoscopic inguinal hernia repair when fixating mesh with suture compared to tacks [18]. However, the original RIVAL trial did not find differences in early postoperative pain between robotic and laparoscopic inguinal hernia repairs [9], nor did we see differences in pain at 1 and 2 years between the two treatment arms. These findings have important implications because our trial suggests that long-term pain after MIS inguinal hernia repair might have less to do with mesh fixation methods than previously thought.
Although we found similar outcomes for both repair types in straightforward inguinal hernia repairs, the RIVAL trial did not investigate the utility of the robot for more complex cases, such as MIS inguinal hernia repairs with existing preperitoneal mesh. The robot has been used for inguinal hernia mesh explantations with acceptable outcomes [19], but this technique has not been compared to laparoscopic mesh excisions. Further study should be devoted to identifying clinical scenarios which may benefit from application of a robotic approach. There is also some conjecture that the robotic platform may facilitate skills acquisition for MIS inguinal hernia repair, allowing primarily open surgeons to adopt an MIS approach. Although there is some literature in inanimate or simulation models suggesting that robotic suturing can be learned more easily than laparoscopic suturing [20, 21], the learning curves for laparoscopic versus robotic inguinal hernia repair have not yet been defined or compared. Future head-to-head studies should assess whether it is easier for novices to overcome the learning curve of MIS inguinal hernia repairs when performed robotically versus laparoscopically.
This study is limited by missing long-term follow-up for 19% and 25% of patients at 1 and 2 years, respectively. Additionally, the RIVAL trial was not designed to identify small differences in long-term patient-reported outcomes. This is also a small sample size for long-term outcomes with low frequency event rates, like hernia recurrence. Finally, this study included only surgeons who were proficient with laparoscopic inguinal hernia repairs, which might limit the generalizability of our results.
In conclusion, our results indicate that laparoscopic and robotic TAPP inguinal hernia repairs have similar long-term outcomes when performed by surgeons with experience in MIS inguinal hernia repairs. The low rates of groin pain and hernia recurrence suggest that both approaches were performed competently. For surgeons already proficient with laparoscopic inguinal hernia repair, our findings do not support the adoption of the robotic technique for straightforward MIS inguinal hernia repairs. Future work should focus on defining and comparing the learning curve for laparoscopic and robotic inguinal hernia repair and comparing laparoscopic and robotic techniques in complex MIS inguinal operations.
References
Ger R (1991) Laparoscopic hernia operation. Chirurg 62(4):266–270 (Article in German)
HerniaSurge Group (2018) International guidelines for groin hernia management. Hernia 22:1–165
Bullen NL, Massey LH, Antoniou SA, Smart NJ, Fortelny RH (2019) Open versus laparoscopic mesh repair of primary unilateral uncomplicated inguinal hernia: a systematic review with meta-analysis and trial sequential analysis. Hernia 23:461–472
Escobar Dominguez JE, Gonzalez A, Donkor C (2015) Robotic inguinal hernia repair. J Surg Oncol 112(3):310–314
Sheetz KH, Claflin J, Dimick JB (2020) Trends in the adoption of robotic surgery for common surgical procedures. JAMA Netw Open. https://doi.org/10.1001/jamanetworkopen.2019.18911
Ye L, Tang AB, Shenoy R, Mederos MA, Mak SS, Booth MS, Wilson M, Gunnar W, Girgis MD, Maggard-Gibbons M, GLA ESP Team (2021) Clinical and cost outcomes of robot-assisted inguinal hernia repair: a systematic review. J Am Coll Surg 232(5):746–763
LeBlanc K, Dickens E, Gonzalez A, Gamagami R, Pierce R, Balentine C, Voeller G (2020) Prospective, multicenter, pairwise analysis of robotic-assisted inguinal hernia repair with open and laparoscopic inguinal hernia repair: early results from the prospective hernia study. Hernia 24:1069–1081
Abdelmoaty WF, Dunst CM, Neighorn C, Swanstrom L, Hammil CW (2019) Robotic-assisted versus laparoscopic unilateral inguinal hernia repair: a comprehensive cost analysis. Surg Endosc 33(10):3436–3443
Prabhu AS, Carbonell A, Hope W, Warren J, Higgins R, Jacob B, Blatnik J, Haskins I, Alkhatib H, Tastaldi L, Fafaj A, Tu C, Rosen MJ (2020) Robotic inguinal vs transabdominal laparoscopic inguinal hernia repair: the RIVAL randomized clinical trial. JAMA Surg 155(5):380–387
Huskisson EC (1974) Measurement of pain. Lancet 2(7889):1127–1131
Bennett M (2001) The LANSS pain scale: the Leeds assessment of neuropathic symptoms and signs. Pain 92:147–157
Ware JE Jr, Sherbourne CD (1992) The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med Care 30(6):473–483
Ware JE, Keller SD, Kosinski M (1994) SF-36 physical and mental health summary scales: a user’s manual. The Health Institute, New England Medical Center, Boston
Meriwether RA, McMahon PM, Islam N, Steinmann WC (2006) Physical activity assessment: validation of a clinical assessment tool. Am J Prev Med 31(6):484–491
Tastaldi L, Barros PHF, Krpata DM, Prabhu AS, Rosenblatt S, Petro CC, Alkhatib H, Szutan LA, Silva RA, Olson MA, Stewart TG, Roll S, Rosen MJ, Poulose BK (2020) Hernia recurrence inventory: inguinal hernia recurrence can be accurately assessed using patient-reported outcomes. Hernia 24(1):127–135
Liu N, Greenberg JA (2020) Robotics vs laparoscopy—are they truly rivals? JAMA Surg 155(5):388
Waite KE, Herman MA, Doyle PA (2016) Comparison of robotic versus laparoscopic trans abdominal preperitoneal (TAPP) inguinal hernia repair. J Robot Surg 10:239–244
Kleidari B, Mahmoudieh M, Yaribakht M, Homaei Z (2014) Mesh fixation in TAPP laparoscopic hernia repair: introduction of a new method in a prospective randomized trial. Surg Endosc 28:531–536
Mandujano CC, Tchokouani L, Lima DL, Malcher F, Jacob B (2021) Robotic mesh explanation (RoME): a novel approach for patients with chronic pain following hernia repair. Surg Endosc. https://doi.org/10.1007/s00464-021-08835-x
Yohannes P, Rotariu P, Pinto P, Smith AD, Lee BR (2002) Comparison of robotic versus laparoscopic skills: is there a difference in the learning curve? Urology 60(1):39–45
Leijte E, de Blaauw I, Van Workum F, Rosman C, Botden S (2020) Robot assisted versus laparoscopic suturing learning curve in a simulated setting. Surg Endosc 34(8):3679–3689
Funding
This study was funded by a Grant from Intuitive Surgical (IUSI1602MR).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Ajita S. Prabhu is a consultant for Verb Surgical and CMR Surgical. She has also been a speaker for and has received grant support from Intuitive Surgical (IUSI1602MR). Dr. Alfredo M. Carbonell has received speaking fees from Intuitive Surgical and has been a consultant for Ethicon and WL Gore. He received grant support from WL Gore and is an advisory board member for Medtronic. Dr. William Hope has been a consultant for Medtronic and BD and has received honoraria from Medtronic, WL Gore, Intuitive Surgical, and BD. He has also received research support from WL Gore, Intuitive Surgical, and BD. Dr. Jeremy Warren has received honoraria from Intuitive Surgical. Dr. Rana M. Higgins has received speaking fees from WL Gore and speaking fees and honoraria from Intuitive Surgical. Dr. Brian Jacob and received honoraria from Medtronic. He is also a founder and has equity in the International Hernia Collaboration. Dr. Jeffrey Blatnik has been a consultant for Intuitive Surgical and BD and has received grant support from Cook Biomedical. Dr. Michael J. Rosen receives salary support as medical director of the Abdominal Core Health Quality Collaborative and is a board member of Ariste Medical with stock options. Dr. Benjamin T. Miller, Dr. Clayton C. Petro, Dr. Lucas R. A. Beffa, Dr. David M. Krpata, Chao Tu, and Adele Constanzo have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Miller, B.T., Prabhu, A.S., Petro, C.C. et al. Laparoscopic versus robotic inguinal hernia repair: 1- and 2-year outcomes from the RIVAL trial. Surg Endosc 37, 723–728 (2023). https://doi.org/10.1007/s00464-022-09320-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09320-9