Abstract
Background
Peroral endoscopic myotomy (POEM) is a novel, minimally invasive treatment for esophageal achalasia. We retrospectively examined and evaluated the results following POEM to verify the technique’s efficacy and safety.
Methods
We retrospectively analyzed data for patients who underwent POEM at eight Japanese facilities between September 2008 and October 2015. Pre- and postoperative assessments 3 months and 1 year after POEM included patient interviews, endoscopy, and manometry.
Results
A total of 1346 patients underwent POEM during the study period. Achalasia was the straight type in 1105 patients (82%) and the sigmoid type in 241 patients (18%). The average patient age was 47.2 years (range 3–95 years); 617 patients (46%) were men and 729 (54%) were women. Previous treatment included balloon dilatation in 381 patients (28%) and Heller–Dor operation in 43 patients (3%). The average operation time was 99.6 min. The mean length of the myotomy in the esophageal body was 10.8 cm, and the myotomy extended into the stomach a mean of 2.8 cm. The response rate (Eckardt score ≤ 3) was 95.1% 3 months postoperatively and 94.7% 1 year postoperatively. We noted 50 adverse events (3.7%) of Clavien–Dindo classification grade ≤ IIIa, and all resolved with conservative treatment. There were no Clavien–Dindo classification grade ≥ IIIb adverse events. After POEM, erosive esophagitis according to the Los Angeles classification was absent in 37% of the patients, grade A in 33%, B in 24%, C in 6%, and D in 0.2%. Symptomatic gastroesophageal reflux disease after POEM was confirmed in 14.8% of the patients; both erosive esophagitis and symptomatic gastroesophageal reflux disease responded to treatment with a proton-pump inhibitor.
Conclusion
Our results confirmed the safety and efficacy of POEM in a large patient series and support POEM as the first-line and standard treatment for esophageal achalasia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Esophageal achalasia is an esophageal motility disorder of unknown etiology [1,2,3]. The condition is characterized by failure of the lower esophageal sphincter (LES) to relax, along with impaired peristalsis of the esophageal body. Peroral endoscopic myotomy (POEM) is a novel, minimally invasive treatment for esophageal achalasia and related disorders, first reported by Inoue et al.; however, few subsequent reports have included more than 1000 patients [4, 5]. The purpose of our study was to retrospectively evaluate the results of POEM in a large patient cohort, and to verify the efficacy and safety of POEM.
Methods
We retrospectively analyzed data for patients undergoing POEM for esophageal achalasia at eight facilities in Japan between September 2008 and October 2015 (Table 1). All patients gave informed consent before undergoing POEM, and each institutional review board approved this study. The study met the Japanese governmental guidelines.
Preoperative patient evaluation
Patients’ clinical achalasia symptoms were assessed using Eckardt scores [6]. The Eckardt scores comprises four components: dysphagia, chest pain, regurgitation, and weight loss. Each component is assigned a score from 0 to 3 based on the patient’s self-reported assessment, with a total score ranging from 0 to 12. A higher Eckardt score reflects more severe symptoms of achalasia, whereas a lower score postoperatively indicates improvement in symptoms. Preoperative tests included manometry, endoscopy, barium swallow examination, and computed tomography. The type of achalasia was determined according to the findings from barium swallow examination and computed tomography. Each patient’s systemic function was also evaluated to determine whether general anesthesia was possible.
POEM procedure
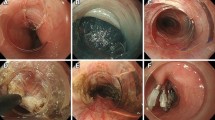
POEM was performed using the methods described by Inoue et al. (Fig. 1) [4, 7, 8]. All procedures were performed or supervised by surgeons from each of the eight study facilities who had learned the POEM procedure from Dr Inoue and who continued to use the same techniques. POEM was performed under general anesthesia with endotracheal intubation with patients in the supine position to be able to use preoperatively computed tomographic information. We used carbon dioxide exclusively to insufflate when using the endoscope. POEM was performed using a triangle-tip electrosurgical knife (KD-640L, Olympus, Tokyo, Japan).
Evaluation of the treatment effect
We evaluated patients’ results following POEM based on patient interviews, and endoscopy and manometry findings. We used patients’ Eckardt scores to evaluate the efficacy of POEM as follows: an Eckardt score ≦ 3 post-POEM was deemed a successful outcome. We assessed the safety of POEM using the Clavien–Dindo classification system to evaluate adverse events associated with the procedure [9]. For gastroesophageal reflux disease (GERD) after POEM, we evaluated the presence or absence of GERD, patients’ symptoms, and the degree of erosive esophagitis in endoscopy. Erosive esophagitis was evaluated according to the Los Angeles classification system [10].
Results
Patients’ demographics
POEM was performed in 1346 patients with achalasia (729 women and 617 men with a mean age of 47.2 ± 17.1 years) during the study period (Table 2). Achalasia was the straight type in 1105 (82%) patients and the sigmoid type in 241 (18%) patients; 381 (28%) patients had previously undergone pneumatic dilation, and 43 patients (3%) had previously undergone Heller–Dor operation.
POEM outcomes
The efficacy of POEM within 6 months after surgery was 95.1% and 94.7% 1 year postoperatively (Table 3). POEM was successfully completed (technical success) in all patients, with a mean procedural time of 99.6 ± 41.7 min (Table 4). Anterior myotomy was performed in 901 patients (67%), and posterior myotomy was performed in 445 (33%) patients. The mean length of the esophageal myotomies was 10.8 ± 3.8 cm, while the mean length of the gastric myotomies was 2.8 ± 1.1 cm.
Adverse events
Adverse events of Clavien–Dindo classification grade ≤ IIIa occurred in 50 patients (3.7%); five patients (0.4%) experienced mucosal perforation, 24 patients (1.8%) experienced mucosal injury without perforation, nine patients (0.7%) experienced submucosal hematoma, and two patients (0.1%) experienced major bleeding. There were no Clavien–Dindo classification grade ≥ IIIb adverse events.
GERD after POEM
Within 6 months after POEM, 1176 patients underwent endoscopic examination, and 63% had erosive esophagitis of Los Angeles classification grade A–D (Table 5). Severe erosive esophagitis (Los Angeles grade C or D) was observed in 6.2% of the patients. Symptomatic GERD was observed in 14.8% of patients; however, both erosive esophagitis and symptomatic GERD responded to treatment with a proton-pump inhibitor.
Discussion
POEM is a novel, minimally invasive treatment for esophageal achalasia and related disorders that was first reported by Inoue et al. in 2010 [4]. Many facilities worldwide have reported the therapeutic efficacy of POEM, but few reports have included more than 1000 patients [11,12,13,14,15]. In this study, we retrospectively examined the treatment results for > 1300 patients undergoing POEM at eight facilities in Japan, and we verified the efficacy and safety of POEM within 6 months and 1 year postoperatively.
The technical success of POEM in this study was 100%, and the efficacy of POEM was approximately 95% within 6 months and 1 year after POEM. Adverse events occurred in approximately 4% of our patients, half of which were associated with mucosal injury, but no patients suffered Clavien–Dindo classification grade ≥ IIIb adverse effects requiring surgical treatment. There are several possible reasons for the high efficacy and safety in this study. First, most surgeons in this study learned the POEM procedure during at least 1 year of study from its originator, Dr Inoue, and used the techniques consistently, thereafter. Second, all procedures were performed by these trained surgeons or under their supervision.
Regarding GERD after POEM, erosive esophagitis was observed in 63% of our patients; however, esophagitis of Los Angeles classification grade C and D occurred in only 6% of the patients. Additionally, the erosive esophagitis was mild in most patients, and all patients responded to a proton-pump inhibitor. Symptomatic GERD was recognized in 15% of patients, which also responded to treatment with a proton-pump inhibitor, similar to previous reports. We evaluated GERD after POEM in more than 1000 patients in this study, and no patients suffered refractory GERD requiring additional fundoplication. However, some reports have described patients requiring fundoplication after POEM [16, 17]. Therefore, long-term follow-up and reports of the clinical outcomes for patients with GERD after POEM are needed. Moreover, the risk factors for severe GERD after POEM must be defined.
The limitations of this study are the retrospective design, the relatively short-term follow-up, and that we did not include patients with other esophageal motility disorders. In the future, we plan to address these limitations by completing a prospective study or a retrospective study with a higher number of facilities and examination criteria.
In conclusion, our multicenter retrospective study confirmed the safety and efficacy of POEM in a large patient series. Our results support POEM as the first-line and standard treatment for esophageal achalasia.
Abbreviations
- POEM:
-
Peroral endoscopic myotomy
- LES:
-
Lower esophageal sphincter
- GERD:
-
Gastroesophageal reflux disease
References
Richter JE (2001) Oesophageal motility disorders. Lancet 358:823–828
Japan Esophageal S (2017) Descriptive rules for achalasia of the esophagus, June 2012: 4th edn. Esophagus 14:275–289
Vaezi MF, Pandolfino JE, Vela MF (2013) ACG clinical guideline: diagnosis and management of achalasia. Am J Gastroenterol 108:1238–1249 (Quiz 1250)
Inoue H, Minami H, Kobayashi Y et al (2010) Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy 42:265–271
Haito-Chavez Y, Inoue H, Beard KW et al (2017) Comprehensive analysis of adverse events associated with per oral endoscopic myotomy in 1826 patients: an international multicenter study. Am J Gastroenterol 112:1267–1276
Eckardt VF (2001) Clinical presentations and complications of achalasia. Gastrointest Endosc Clin N Am 11(281–92):vi
Inoue H, Tianle KM, Ikeda H et al (2011) Peroral endoscopic myotomy for esophageal achalasia: technique, indication, and outcomes. Thorac Surg Clin 21:519–525
Inoue H, Shiwaku H, Iwakiri K et al (2018) Clinical practice guidelines for peroral endoscopic myotomy. Dig Endosc 30:563–579
American Society of Anesthesiologists (2014) ASA physical status classification system. https://www.asahq.org/standards-and-guidelines/asa-physical-status-classification-system
Armstrong D, Bennett JR, Blum AL et al (1996) The endoscopic assessment of esophagitis: a progress report on observer agreement. Gastroenterology 111:85–92
Minami H, Inoue H, Haji A et al (2015) Per-oral endoscopic myotomy: emerging indications and evolving techniques. Dig Endosc 27:175–181
Shiwaku H, Inoue H, Yamashita K et al (2016) Peroral endoscopic myotomy for esophageal achalasia: outcomes of the first over 100 patients with short-term follow-up. Surg Endosc 30:4817–4826
Sato H, Takahashi K, Mizuno KI et al (2018) A clinical study of peroral endoscopic myotomy reveals that impaired lower esophageal sphincter relaxation in achalasia is not only defined by high-resolution manometry. PLoS ONE 13:e0195423
Tanaka S, Toyonaga T, Kawara F et al (2017) Peroral endoscopic myotomy using FlushKnife BT: a single-center series. Endosc Int Open 5:E663–E669
Von Renteln D, Fuchs KH, Fockens P et al (2013) Peroral endoscopic myotomy for the treatment of achalasia: an international prospective multicenter study. Gastroenterology 145(309–11):e1–e3
Zak Y, Meireles OR, Rattner DW (2018) Laparoscopic toupet fundoplication for GERD after POEM. https://www.sages.org/meetings/annual-meeting/abstracts-archive/laparoscopic-toupet-fundoplication-for-gerd-after-poem/
Tyberg A, Choi A, Gaidhane M et al (2018) Transoral incisional fundoplication for reflux after peroral endoscopic myotomy: a crucial addition to our arsenal. Endosc Int Open 6:E549–E552
Acknowledgements
The authors would like to thank Dr. Toshihiro Ohmiya (Digestive Disease Center of Showa University Northern Yokohama Hospital and Department of Gastroenterological Surgery, Fukuoka University Faculty of Medicine), Dr. Masaki Ominami (Digestive Diseases Center, Showa University Koto-Toyosu Hospital and Department of Gastroenterology, Osaka City University Graduate School of Medicine), Dr. Shin Kono (Digestive Diseases Center, Showa University Koto-Toyosu Hospital and Department of Gastroenterology and Hepatology, Tokyo Medical University), and Dr. Masayuki Nishimoto (Digestive Diseases Center, Showa University Koto-Toyosu Hospital and Department of Gastroenterology, Wakayama Medical University) for their contribution to data acquisition of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
The authors state that this manuscript is being submitted as an accompaniment to a podium presentation at SAGES 2018, held in Seattle, WA, USA. Dr Haruhiro Inoue reports grants from Olympus Co. and grants from Boston Scientific Co. outside the submitted work. Hironari Shiwaku, Manabu Onimaru, Hitomi Minami, Hiroki Sato, Chiaki Sato, ShinwaTanaka, Ryo Ogawa, and Norihiko Okushima have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shiwaku, H., Inoue, H., Onimaru, M. et al. Multicenter collaborative retrospective evaluation of peroral endoscopic myotomy for esophageal achalasia: analysis of data from more than 1300 patients at eight facilities in Japan. Surg Endosc 34, 464–468 (2020). https://doi.org/10.1007/s00464-019-06833-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06833-8