Abstract
Background
Laparoscopic bile duct exploration (LBDE) is recommended in current treatment guidelines for the management of choledocholithiasis with gallbladder in situ. Failure of this technique is common as a consequence of large or impacted common bile duct (CBD) stones. In this series, we present our experience in using holmium laser lithotripsy as an adjunct to LBDE for the treatment of choledocholithiasis.
Methods
Between 2014 and 2016, eighteen laparoscopic bile duct explorations utilising holmium laser lithotripsy were performed after failure of standard retrieval techniques.
Results
Choledocholithiasis was successfully treated in 18 patients using laparoscopic holmium laser lithotripsy (transcystically in 14 patients). There was one failure where a CBD stricture prevented the scope reaching the stone. Two medical complications were recorded (Clavien–Dindo I and II). There were no mortalities or re-interventions.
Conclusions
LABEL technique is a successful and safe method to enhance LBDE in cases of impacted or large stones. In our experience, this approach increases the feasibility of the transcystic stone retrieval and may reduce overall operative time.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Choledocholithiasis has been reported in up to 18 % of patients undergoing cholecystectomy [1]. Endoscopic retrograde cholangiopancreatogram and endoscopic sphincterotomy (ERCP-ES) are widely performed in most hospitals as first-line treatment [2]. In contrast, as stated in current national and international guidelines [3, 4], LBDE (preferably by the transcystic route) is the gold-standard technique for the management of choledocholithiasis with gallbladder in situ (if the expertise is available) over ERCP-ES followed by laparoscopic cholecystectomy due to its lesser morbidity, hospital stay and cost [5–11]. Cystic duct (CD) size, stone size and the presence of impacted stones are factors favouring choledochotomy over the transcystic approach, and impacted stones are the main reason of failure of the technique. Holmium laser lithotripsy use has been already reported, with good results, for impacted CBD stone fragmentation in short series [12–14]. In this study, we describe our experience in the laparoscopic management of impacted and large biliary stones using holmium laser. To our knowledge, this is the largest reported series of laparoscopic holmium laser lithotripsy for choledocholithiasis.
Materials and methods
Patient selection
All patients admitted to our institution under the senior author (AI) with choledocholithiasis, gallstone pancreatitis or symptomatic cholelithiasis, and the suspicion of CBD stones are considered for laparoscopic cholecystectomy and intraoperative cholangiogram (IOC). LBDE is performed if choledocholithiasis is present. Since February 2014, laparoscopic holmium laser lithotripsy has been considered if routine basket retrieval was not possible because of impacted stones or when the size was too large for routine transcystic extraction.
Six patients were referred after failed ERCP with biliary stent insertion. One had a previous cholecystectomy. Twelve patients were admitted from the emergency department and referred to our unit for specialised single-stage surgical management on diagnosis of choledocholithiasis. One patient required cholecystostomy before laparoscopic holmium laser lithotripsy for severe acute cholecystitis.
Surgical technique
All patients underwent the formal informed consent process in line with our institution and National Medical Council guidelines. Additionally, all laser techniques were performed in a laser suitable theatre by experts officially trained in using the holmium laser in the operative field. All laser technology had undergone safety checks and been approved for use in human procedures. All precautionary steps were applied for the use of lasers in the operative environment.
All cases were performed in accordance with our previously described technique [14]. Our preferred technique is a transcystic approach to the bile duct, currently used in more than 75 % of our cases. Three main factors influenced our decision to perform choledochotomy in 5 patients in this series: (1) the diameter of the CD, (2) the stone size and (3) the presence of a CBD stricture.
Inclusion criteria for the use of laser lithotripsy were the presence of impacted CBD stones after unsuccessful retrieval attempts with Dormia basket, or a large non-impacted stone found through a transcystic approach unable to be extracted through the CD.
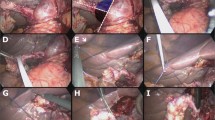
For the lithotripsy, a 200- to 365-µm holmium laser fibre (Optical Integrity ScopeSafe™) was introduced through the choledochoscope. After security measurements, the generator is initially set at 0.5 J and 5 Hz, and its frequency may then be increased according to the consistency of the stone. The coloured diode targets the point of the stone where the laser should be activated (Fig. 1). The stone is then fragmented (Fig. 2) until it can be extracted from the bile duct or through the cystic duct using a Dormia basket, or is small enough to be flashed down to the duodenum with the help of the water irrigation. In addition, the choledochoscope can be passed through the ampulla obtaining the view of the duodenum to reassure the surgeon that good drainage has been achieved. Once clearance of the biliary tree has been accomplished, if the transcystic route is not used, we favour primary closure of the choledochotomy with a 5/0 polyglactin running suture. A drain is left in place, and it is removed in 24 h. When the transcystic approach is performed, the cystic duct is tied using an endoloop or transfixed using a 3/0 polyglactin suture without the need of a drain.
Patients are routinely kept in hospital overnight and discharged the following day.
Results
Over a period of 26 months, between February 2014 and June 2016, eighteen patients [10 males; mean age 53 (21–84)] underwent LABEL procedure (Table 1). Over the same period, a total of 87 LBDE were performed in our institution. The diameter of the CBD varied from 8 to 24 mm (mean 13.3 mm). The number of stones ranged from 1 to 5 with a median diameter of 10.3 mm (5–20 mm). All procedures were accomplished laparoscopically. A transcystic approach was performed in 14 patients, whereas 5 patients underwent choledochotomy. Both approaches were used in one patient (the only unsuccessful laser lithotripsy stone retrieval) due to the choledocholithiasis being beyond an inflammatory CBD stricture unable to be passed by the scope. Closure over a T-tube was decided in this case to alleviate biliary obstruction, and the procedure was completed with a postoperative ERCP confirming the stricture. Sphincterotomy was performed, the three stones retrieved and a biliary stent placed. The T-tube was uneventfully removed after normal T-tube cholangiogram (Fig. 3) 1 month after the procedure and, at this time, the stricture had settled.
In one case (patient 14), four large stones were found within the CBD, and the Dormia basket became lodged during a standard transcystic basket removal. This was managed by removing the Dormia handle and then the basket from the scope followed by a transcystic laser fragmentation of the impacted stone within the basket, allowing the release of the Dormia basket. The remaining 3 stones were also fragmented to allow completion of the transcystic removal.
In another case (patient 11), the patient had undergone a previous cholecystectomy. In this case, we were unable to pass the papilla after successfully completing the laser lithotripsy of a large CBD stone. Due to the patient’s age (84 years) and the size of CBD (20 mm), a laparoscopic choledochoduodenostomy was decided to ensure adequate biliary drainage. The remaining 3 patients requiring choledochotomy underwent an uncomplicated primary closure without complications.
Five patients underwent preoperative placement of a biliary stent, 3 of whom had the stent removed during surgery. The remaining 2 patients underwent endoscopic removal of the stent postoperatively.
There was no mortality, and no reoperations were required. No patients had retained stones, and there have been no recurrences to date. Postoperative complications were observed in 2 patients. The first was a 71-year-old patient with hypertension and atrial fibrillation who developed pulmonary oedema that resolved with diuretics (Clavien–Dindo I). The second was an 84-year-old patient who underwent choledochoduodenostomy. This was complicated with an episode of maelena that was treated conservatively (Clavien–Dindo II); his overall length of stay was 30 days.
The mean postoperative stay was 5.3 days (1–30). Patients undergoing surgery via a transcystic approach were discharged earlier (mean length of stay (LOS) was 2.3 days) than those undergoing choledochotomy (mean LOS was 13 days) (p = 0.0025).
Discussion
Laser lithotripsy has been widely used for ureteric stones with high success and a low complication rate [16, 17]. Different lasers are currently used for stone fragmentation: KTP:YAG, LBO:YAG, diode lasers, holmium:YAG and thulium:YAG lasers [18], but holmium laser lithotripsy has the advantage of increased flexibility, which improves the access to previously unreachable areas, and its visible diode facilitates targeting stones with minimal collateral damage [19, 20]. The good outcomes achieved with the use of lasers in urological procedures prompted their adoption in the treatment of biliary stones. First described by Orii et al. [21], laser lithotripsy was initially used to fragment intrahepatic and choledochal stones using a choledochoscope through a T-tube or percutaneous transhepatic fistula.
In the present era, treatment of choledocholithiasis classically includes ERCP, which forms the standard technique in most hospitals [2]. In our institution, we favour single-stage laparoscopic management of choledocholithiasis and gallstone pancreatitis in the case of concomitant biliary stones [22], in accordance with the current National Institute for Health and Care Excellence (NICE) guidelines for gallstone disease [3]. After its introduction in 1998, our management of access and closure of the CBD evolved from choledochotomy and closure over a T-Tube into a choledochorraphy over an anterograde biliary endoprosthesis. This technique was later abandoned due to a high incidence of stent-related pancreatitis [15, 23, 24]. Currently, our preferred technique for CBD closure when choledochotomy is performed is primary choledochorraphy using a running 5/0 polyglactin suture [15]. In recent years, we are increasingly favouring the transcystic route (>75 % of cases) due to its excellent safety profile and the availability of 3-mm choledochoscopes. Furthermore, the advantages of single-stage management and the use of a transcystic approach in terms of lower hospital stay, need of fewer procedures, reduced bile leak, lower overall complication rate and a decrease in hospital costs have now been reported by a number of groups [5–11].
Despite technical improvements over our 326 case experience of LBDE, impacted stones (both intrahepatic and in the distal bile duct) had remained the main cause of procedural failure before the introduction of the laser [25]. Similar to reports from other groups [26, 27], we have also found the presence of large-sized stones to be the main reason for choledochotomy after failure of the transcystic approach. The LABEL procedure now allows impacted CBD stones to be fragmented into smaller pieces, which may then either be grabbed by the Dormia basket or passed through the ampulla, with the help of water irrigation. As a consequence, we are now able to perform transcystic extraction in the majority of cases.
Holmium laser lithotripsy can be used for the management of impacted CBD stones either endoscopically, percutaneously or surgically [12–14, 28–31]. It may also be applied to facilitate complicated mechanical stone extraction. The advantage of laparoscopic holmium laser lithotripsy is that it reduces the number of the choledochotomies required by fragmenting CBD stones into small pieces that may be mechanically retrieved transcystically. The availability of 3-mm choledochoscopes has facilitated increased uptake of this technique as these may more easily be passed through the cystic duct.
The only technical limitation of the holmium laser lithotripsy encountered in our series was the presence of a CBD inflammatory stricture, where we were unable to pass the choledochoscope to reach the impacted distal CBD stone. This was not seen in the preoperative MRCP; otherwise, intraoperative balloon dilatation would have been planned preoperatively. Finally, after choledochotomy and closure over a T-tube, choledocholithiasis was removed by ERCP and the inflammatory stricture settled.
Conclusions
To our knowledge, this is the largest reported series of laparoscopic holmium laser lithotripsy for biliary calculi. These results demonstrate the feasibility and reproducibility of the technique once experience for LBDE is gained. Holmium laser lithotripsy increases facilitates a transcystic approach, reduces failure related to impacted biliary stones and may also be used in cases of complicated mechanical extraction. As such, we believe that there is now a role for a more widespread uptake of LABEL procedure in the first-line management of impacted CBD stones.
References
Martin DJ, Vernon DR, Toouli J (2006) Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev 2:CD003327
Puig I, Calvet X, Baylina M, Isava Á, Sort P, Llaó J, Porta F, Vida F (2014) How and when should NSAIDs be used for preventing post-ERCP pancreatitis? A systematic review and meta-analysis. PLoS One 9(3):e92922
Internal Clinical Guidelines Team (UK) (2014). National Institute for Health and Care Excellence: Clinical Guidelines. Gallstone disease: diagnosis and management of cholelithiasis, cholecystitis and choledocholithiasis. National Institute for Health and Care Excellence, London
Overby DW, Apelgren KN, Richardson W, Fanelli R (2010) Society of American Gastrointestinal and Endoscopic Surgeons. SAGES guidelines for the clinical application of laparoscopic biliary tract surgery. Surg Endosc 24(10):2368–2386
Reinders JS, Gouma DJ, Ubbink DT, van Ramshorst B, Boerma D (2014) Transcystic or transductal stone extraction during single-stage treatment of choledochocystolithiasis: a systematic review. World J Surg 38(9):2403–2411
Bansal VK, Misra MC, Rajan K, Kilambi R, Kumar S, Krishna A, Kumar A, Pandav CS, Subramaniam R, Arora MK, Garg PK (2014) Single-stage laparoscopic common bile duct exploration and cholecystectomy versus two-stage endoscopic stone extraction followed by laparoscopic cholecystectomy for patients with concomitant gallbladder stones and common bile duct stones: a randomized controlled trial. Surg Endosc 28(3):875–885
Zhu JG, Han W, Zhang ZT, Guo W, Liu W, Li J (2014) Short-term outcomes of laparoscopic transcystic common bile duct exploration with discharge less than 24 h. J Laparoendosc Adv Surg Tech A 24(5):302–305
Zhang WJ, Xu GF, Huang Q, Luo KL, Dong ZT, Li JM, Wu GZ, Guan WX (2015) Treatment of gallbladder stone with common bile duct stones in the laparoscopic era. BMC Surg 26(15):7
Petersson U, Johansen D, Montgomery A (2015) Laparoscopic transcystic laser lithotripsy for common bile duct stone clearance. Surg Laparosc Endosc Percutan Tech 25(1):33–36
Hongjun H, Yong J, Baoqiang W (2015) Laparoscopic common bile duct exploration: Choledochotomy versus transcystic approach? Surg Laparosc Endosc Percutan Tech 25(3):218–222
Zhu JG, Han W, Guo W, Su W, Bai ZG, Zhang ZT (2015) Learning curve and outcome of laparoscopic transcystic common bile duct exploration for choledocholithiasis. Br J Surg 102(13):1691–1697
Teichman JM, Schwesinger WH, Lackner J, Cossman RM (2001) Holmium: YAG laser lithotripsy for gallstones. A preliminary report. Surg Endosc 15(9):1034–1037
Healy K, Chamsuddin A, Spivey J, Martin L, Nieh P, Ogan K (2009) Percutaneous endoscopic holmium laser lithotripsy for management of complicated biliary calculi. JSLS 13(2):184–189
Varban O, Assimos D, Passman C, Westcott C (2010) Laparoscopic common bile duct exploration and holmium laser lithotripsy: a novel approach to the management of common bile duct stones. Surg Endosc 24(7):1759–1764
Abellán Morcillo I, Qurashi K, Abrisqueta Carrión J, Martínez Isla A (2014) Exploración laparoscópica de la vía biliar, lecciones aprendidas tras más de 200 casos. Cir Esp 92:341–347
Bader MJ, Eisner B, Porpiglia F, Preminger GM, Tiselius HG (2012) Contemporary management of ureteral stones. Eur Urol 61:672–764
Khoder WY, Bader M, Sroka R, Stief C, Waidelich R (2014) Efficacy and safety of Ho:YAG laser lithotripsy for ureteroscopic removal of proximal and distal ureteral calculi. BMC Urol 14:62
Dołowy Ł, Krajewski W, Dembowski J, Zdrojowy R, Kołodziej A (2015) The role of lasers in modern urology. Cent Eur J Urol 68(2):175–182
Xu G, Wen J, Li Z et al (2015) A comparative study to analyze the efficacy and safety of flexible ureteroscopy combined with holmium laser lithotripsy for residual calculi after percutaneous nephrolithotripsy. Int J Clin Exp Med 8(3):4501–4507
Nazif OA, Teichman JM, Glickman RD, Welch AJ (2004) Review of laser fibers: a practical guide for urologists. J Endourol 18(9):818–829
Orii K, Ozaki A, Takase Y, Iwasaki Y (1983) Lithotomy of intrahepatic and choledochal stones with Yag laser. Surg Gynecol Obstet 156(4):485–488
Griniatsos J, Karvounis E, Isla A (2005) Early versus delayed single-stage laparoscopic eradication for both gallstones and common bile duct stones in mild acute biliary pancreatitis. Am Surg 71(8):682–686
Isla AM, Griniatsos J, Wan A (2002) A technique for safe placement of a biliary endoprosthesis after laparoscopic choledochotomy. J Laparoendosc Adv Surg Tech 12(3):207–211
Isla AM, Griniatsos J, Karvounis E, Arbuckle JD (2004) Advantages of laparoscopic stented choledochorrhaphy over T-tube placement. Br J Surg 91(7):862–866
Karvounis E, Griniatsos J, Arnold J, Atkin G, Isla AM (2006) Why does laparoscopic common bile duct exploration fail? Int Surg 91(2):90–93
Lee SH, Park JK, Yoon WJ, Lee JK, Ryu JK, Kim YT, Yoon YB (2007) How to predict the outcome of endoscopic mechanical lithotripsy in patients with difficult bile duct stones? Scand J Gastroenterol 42(8):1006–1010
Gupta N, Poreddy V, Al-Kawas F (2008) Endoscopy in the management of choledocholithiasis. Curr Gastroenterol Rep 10(2):169–176
Shamamian P, Grasso M (2004) Management of complex biliary tract calculi with a holmium laser. J Gastrointest Surg 8(2):191–199
Day A, Sayegh ME, Kastner C, Liston T (2009) The use of holmium laser technology for the treatment of refractory common bile duct stones, with a short review of the relevant literature. Surg Innov 16(2):169–172
Heller SJ (2013) Endoscopic removal of large common bile duct stones: Time to arm the laser? Dig Dis Sci 58(1):17–19
Sauer BG, Cerefice M, Swartz DC, Gaidhane M, Jain A, Haider S, Kahaleh M (2013) Safety and efficacy of laser lithotripsy for complicated biliary stones using direct choledochoscopy. Dig Dis Sci 58(1):253–256
Author contribution
ANS, HA, JJSS and AI made substantial contributions to design, acquisition of data, analysis and interpretation of data. All authors participated in drafting the article and revising it critically for important intellectual content. All authors gave final approval of the version to be submitted.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Drs. Antonio Navarro-Sánchez, Hutan Ashrafian, Juan José Segura-Sampedro and Alberto Isla have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Navarro-Sánchez, A., Ashrafian, H., Segura-Sampedro, J.J. et al. LABEL procedure: Laser-Assisted Bile duct Exploration by Laparoendoscopy for choledocholithiasis: improving surgical outcomes and reducing technical failure. Surg Endosc 31, 2103–2108 (2017). https://doi.org/10.1007/s00464-016-5206-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5206-1