Abstract
Introduction
Recent studies show contrasting data on the impact of laparoscopy on long-term complications such as the occurrence of small bowel obstruction (SBO) and incisional hernia (IH). The objective of the study was to assess the impact of the laparoscopic approach on the occurrence of SBO and IH after colorectal resection.
Methods
Two trained investigators independently searched MEDLINE, Embase, PubMed, and the Cochrane Central Register of clinical trials for studies comparing laparoscopy to open surgery for mid- to long-term outcomes after colorectal surgery. No language restriction was set. Sensitivity analyses for study design and quality, conversion rate, type of procedure (colon or rectal surgery), and length of follow-up were performed.
Results
Eleven RCTs and 14 non-RCT comparative studies for a total of 6540 patients were included in the analysis. Laparoscopy was associated with a significant reduction in the occurrence of SBO (RR 0.57, [95 %CI 0.42–0.76], 16 trials) and IH (RR 0.60, [95 %CI 0.50–0.72], 19 trials). Sensitivity analysis including only RCTs confirmed the reduction in SBO (RR 0.58, [95 %CI 0.39–0.87], 8 trials), while the difference was close to significance for IH (RR 0.76, [95 %CI 0.56–1.03], 7 trials). Sensitivity analysis including only studies with conversion rate lower than 15 % showed a significant protective effect of laparoscopy for both SBO (RR 0.53, [95 %CI 0.37–0.77], 11 trials) and IH (RR 0.58, [95 %CI 0.47–0.72], 12 trials). No significant difference between laparoscopy and open surgery was found when the analysis was limited to studies with conversion rate >15 % (SBO: RR 0.60 [0.32–1.12], IH: RR 0.70 [0.46–1.06]). Length of follow-up did not substantially impact on results.
Conclusion
Laparoscopic surgery is associated with a significant reduction in both SBO and IH compared to the open approach. A low conversion rate in the laparoscopic group plays a key role for reduction in both SBO and IH.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
It is well established that minimally invasive colorectal resection is associated with short-term benefits compared to traditional open surgery. Systematic reviews and meta-analyses have shown that laparoscopy (LPS) yields reduced postoperative analgesic requirements, lower morbidity, and faster recovery of gastrointestinal function resulting in reduced length of hospital stay [1]. In addition, oncologic non-inferiority of LPS has been reported in the setting of large multicenter trials for both colonic [2] and rectal cancers [3, 4].
The effect of LPS on long-term morbidity is still debated. Minimization of wound size and peritoneal trauma has the potential to protect from the occurrence of incisional hernia (IH) and small bowel obstruction (SBO), which are the most frequent late complications following colorectal resection. However, to our knowledge, no controlled trial has been specifically designed and powered to detect possible differences in long-term complications between minimally invasive and open surgery. Comparative studies including follow-ups of randomized controlled trials (RCTs) reported that LPS significantly reduced the incidence of IH and SBO [5], while other studies found no difference between surgical approaches [6, 7].
In the present meta-analysis, we aimed to summarize the available evidence and verify the effect of LPS on the occurrence of SBO and IH in patients undergoing elective colorectal resection.
Methods
Search strategy and study selection
This systematic review and meta-analysis was conducted according to the Cochrane Collaboration and the Preferred Reporting Items for Systematic reviews (PRISMA) guidelines [8]. Our search strategy followed the principles of the PICO (patient, intervention, comparison, outcomes) framework [9]. The objective was to evaluate in patients undergoing colorectal surgery (P) the impact of laparoscopy (I) compared with open surgery (C) on long-term morbidity (O).
A systematic database search was performed using MEDLINE (via OvidSP), Embase (via OvidSP), the Cochrane Library, and PubMed for articles up to January 2015. The search strategy was developed according to Robinson et al. [10], using text words and relevant indexing to capture the concepts of laparoscopic colorectal procedures (e.g., laparoscopy, colon resection, rectal resection, sigmoidectomy) and postoperative complications (e.g., intestinal obstruction, incisional hernia). No language restrictions were considered. The search strategy used for the MEDLINE database is described in Supplemental digital content 1.
Inclusion and exclusion criteria
The following inclusion criteria were used for potentially relevant studies: (1) involves adult patients undergoing laparoscopic colorectal surgery, (2) a control group receiving open surgery, (3) random or non-random allocation to treatment, (4) reported at least one of the outcome measures of interest (see below) with no restriction on primary or secondary outcome. For the purpose of this review, we included both hand-assisted and conventional laparoscopic approaches. No language restrictions were set. Exclusion criteria were: (1) duplicate publications (in this case, only the article reporting the longest follow-up was abstracted), (2) non-human experimental studies, (3) more than 20 % of the cases were emergency surgeries, (4) patient follow-up was shorter than 12 months. The three investigators independently assessed compliance to selection criteria and selected studies for the final analysis with divergences finally being resolved by consensus.
Outcome measures
The primary outcome measures of interest were surgery-related SBO and IH occurring more than 30 days after surgery or after discharge from the primary admission. Secondary endpoints were reoperations due to surgery-related incisional hernia and small bowel obstruction occurring more than 30 days after surgery or after discharge from the primary admission.
Study selection, data extraction, and quality assessment
Two expert investigators (NP, SA) independently screened the articles identified by the search. Clearly irrelevant articles were excluded after examination of titles and abstracts. Non-English-language articles were translated before further analysis. Full-text versions of all articles potentially suitable for inclusion were retrieved and evaluated against the selection criteria. Divergences regarding eligibility were resolved by consensus or by consulting the senior investigator (MB). Data were extracted independently by two investigators (NP, SA) and crosschecked. In addition to the outcome measures of interest, the following variables were obtained from the selected papers: patient demographics and body mass index (BMI), diagnosis, type of resection (e.g., colonic resection, rectal resection), conversion rate, duration and modality of follow-up, definition of relevant endpoints.
The internal validity and the quality of each trial were evaluated independently by two investigators (MG, SA) using the Cochrane Collaboration’s tool [11] with divergences being resolved by consensus or by consulting a third investigator (MB). This tool appraises risk of bias across six domains: selection bias (random sequence generation and allocation concealment), performance bias (blinding of participants and personnel), detection bias (blinding of outcome assessment), attrition bias (incomplete outcome data), reporting bias (selective reporting), and other risks of bias. Because of the impossibility to blind assessors to the intervention in assessing the occurrence of incisional hernia, for the domain “detection bias,” we considered at low risk studies in which the clinical assessor was either independent (i.e., did not participate in the care of the patient) or was unaware of the type of surgery when reviewing questionnaire or radiological data. For the domain “other biases,” we considered any potential source of bias not included in the previous domains (e.g., extreme imbalance in baseline characteristics, trial was stopped early). The Cochrane Collaboration’s tool was originally designed to evaluate risk of bias in RCTs, but it has often been extended to non-randomized intervention studies [12]. Some domains of the tool are invariably negative in the absence of randomization (e.g., adequate sequence generation, allocation concealment). Studies with suboptimal scoring in up to three items were regarded at a moderate risk of bias, while studies with more than three suboptimal items and all non-randomized studies were qualified at high risk of bias.
Statistical analysis
Computations were performed with Stata 13 (StataCorp. 2013. Stata Statistical Software: Release 13. College Station, TX: StataCorp LP). Statistical heterogeneity and inconsistency were measured using Cochran’s Q tests and I2, respectively. Binary outcomes from individual studies were analyzed to compute individual and pooled risk ratios (RR) with pertinent 95 % confidence intervals (CI, with equivalence set at 1, RR < 1 favoring the first treatment, and RR > 1 favoring the second treatment), by means of a fixed effects method by inverse variance in the presence of low or moderate statistical inconsistency (I 2 ≤ 25 %), and by means of a random effects method (which considers clinical and statistical variations) by DerSimonian and Laird in the presence of high statistical inconsistency (I 2 > 25 %). Statistical significance was set at the two-tailed 0.05 level for measure of effect testing and for heterogeneity testing.
A sensitivity analysis was performed by analyzing data from studies with low/intermediate risk of bias only. Subgroup analyses were planned a priori and performed, when possible, by clustering the studies according to whether they performed colon or rectal resection. Other subgroup analyses were also planned to verify the effect of conversion to open surgery and length of follow-up on the occurrence of SBO and IH. Studies reporting conversion to open surgery lower than 15 % were considered with low conversion rate, while trials with 15 % or higher conversion rate were considered with high conversion rate. Previous publications showed that more than one-third of IH are diagnosed 5 years or longer after open surgery [13]. Thus, we performed subgroup analyses for studies with duration of follow-up lower than 5 years and studies with follow-up time of at least 5 years.
Publication bias was assessed by visually inspecting funnel plots, by sequential removal of individual studies, by analytical appraisal based on the Egger’s regression test, and on the Peter test for publication bias [14]. According to the Egger or Peter methods for publication bias evaluation, a two-sided p value of 0.05 or less was regarded as significant.
Results
Literature search
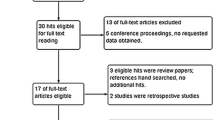
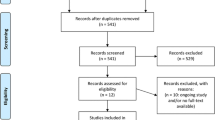
Database searches and scanning of references of retrieved articles yielded a total of 12,437 articles. Excluding non-pertinent titles or abstracts, we retrieved 76 studies in complete form, which we assessed according to the selection criteria. A total of 51 studies were further excluded due to: no reporting of long-term complications (n = 38), duplicate publication (n = 3), study from a population-based registry (n = 3), high amount of missing data (n = 3), short follow-up (n = 2), only emergency surgery (n = 1), insufficient information on timing of complications (n = 1). The excluded articles and reasons for exclusion are listed in Supplemental digital content 2. Finally, twenty-five full-text articles fulfilled our selection criteria and were included in the review. The flowchart of articles selection is shown in Fig. 1.
Characteristics of the included studies
The 25 studies analyzed in this review included 11 RCTs [5–7, 15–22] and 14 non-randomized trials [23–36]. Of the latter, 11 were retrospective cohort studies including 3 matched studies, and 3 were prospective cohort trials. Table 1 summarizes the methodological quality of the 25 studies. Fifteen studies were considered at high risk of bias.
Study characteristics are summarized in Table 2. Eleven RCTs totaling 2831 patients (1485 LPS, 1346 open) and 14 non-randomized trials totaling 3709 patients (1524 LPS, 2185 open) were included in the analysis for an overall pool of 6540 patients (3009 LPS, 3531 open). Overall, 21 studies included patients undergoing colectomy, and 14 studies included rectal resection patients. Median conversion to open surgery rate was 11 % (interquartile range 8–19 %), including 5 studies with conversion exceeding 15 %. Mean or median length of patient follow-up was 5 years or longer in 8 studies. Follow-up modality was heterogeneous between studies, including office visits, medical record review, patient telephone interview, or mailed questionnaires.
Table 3 reports baseline characteristics of the patients included in the studies. Detailed short-term postoperative morbidity and hospital readmission are listed in Table 4. The amount of missing data for short-term outcomes is significant. Two non-randomized studies reported increased wound infection in the open group, while a single RCT and a non-randomized study showed reduced incidence of postoperative ileus in the LPS group.
Small bowel obstruction
Sixteen trials reported on the occurrence of SBO, 8 RCTs [5–7, 15–17, 19, 20] and 8 non-RCTs [24, 25, 27, 29, 32, 33, 35, 36]. When all trials have been pooled together, LPS significantly reduced SBO rate (2.78 %, 68/2446) compared to the open group (5.53 %, 147/2657) (RR 0.57, [0.42, 0.76] p for effect < 0.0001, p for heterogeneity = 0.7, I 2 = 0 %) (Fig. 2). A significant difference in favor of LPS was found when the analysis was restricted to RCTs only (RR 0.58, [0.39, 0.87] p for effect < 0.008, p for heterogeneity = 0.3, I 2 = 4.2 %), whereas the difference was barely significant when the analysis was limited to non-RCTs (RR 0.61, [0.36, 1.02] p for effect = 0.057, p for heterogeneity = 0.86, I 2 = 0 %) (Fig. 3). SBO requiring surgery was comparable between patients undergoing LPS and open surgery (Supplemental digital content 3), also when RCTs and non-RCTs were considered separately (data not shown).
Incisional hernia
Nineteen studies reported on the incidence of incisional hernia, 7 RCTs [5, 7, 15–17, 20, 22] and 12 non-RCTs [23–25, 27–34, 36]. When all trials have been pooled together, LPS significantly reduced IH rate (7.08 %, 166/2345) compared to the open group (13.58 %, 379/2791) (RR 0.60, [0.50, 0.72] p for effect = 0.0001, p for heterogeneity = 0.19, I 2 = 21 %) (Fig. 4). A significant difference in favor of LPS was found when the analysis was restricted to non-RCTs only (RR 0.57, [0.45, 0.72] p for effect = 0.0001, p for heterogeneity = 0.53, I 2 = 0 %), whereas the difference was not significant when the analysis was limited to RCTs (RR 0.76, [0.56, 1.03] p for effect = 0.076, p for heterogeneity = 0.56, I 2 = 0 %) (Fig. 5). The need for surgery due to IH was comparable between LPS and open surgery (Supplemental digital content 4), also when RCTs and non-RCTs were considered separately (data not shown).
Sensitivity analyses and risk of bias
When the analysis was restricted to trials with low or intermediate risk of bias only, LPS significantly reduced SBO rate (RR 0.58, [0.39, 0.86] p for effect = 0.008, p for heterogeneity = 0.39, I 2 = 4 %), whereas no significant difference for IH rate was found (RR 0.76, [0.56, 1.03] p for effect = 0.076) (Supplemental digital contents 5 and 6).
A sensitivity analysis was performed according to the conversion rate in the LPS group. Studies were split into high conversion rate (i.e., 15 % or higher) or low conversion rate (i.e., lower than 15 %). The occurrence of SBO remained significantly lower in the LPS group considering the 11 studies reporting low conversion rates only (RR 0.53, [0.37, 0.77] p for effect = 0.001, p for heterogeneity = 0.9, I 2 = 0 %), whereas no difference was found between LPS and open surgery considering the 5 studies with high conversion rate only (RR 0.60, [0.32, 1.12] p for effect = 0.11, p for heterogeneity = 0.24, I 2 = 26 %) (Fig. 6). Similarly, the occurrence of IH remained significantly lower in the LPS group considering the 12 studies with low conversion rate only (RR 0.58, [0.47, 0.72] p for effect = 0.001, p for heterogeneity = 0.27, I 2 = 18 %), whereas a nonsignificant difference was found between LPS and open surgery considering the 7 studies where conversion rate exceed 15 % (RR 0.70, [0.46, 1.06] p for effect = 0.095, p for heterogeneity = 0.15, I 2 = 36 %) (Fig. 7).
LPS approach significantly reduced both SBO and IH considering studies with follow-up longer or shorter than 5 years (data not shown). Analyzing colonic and rectum resection separately, the occurrence of SBO was significantly lower in the LPS group considering 9 studies reporting data for colonic resection (RR 0.55, [0.38, 0.79] p for effect = 0.001, p for heterogeneity = 0.91, I 2 = 0 %), whereas the difference was not significant considering 7 studies that included data for rectal resection (RR 0.59, [0.34, 1.02] p for effect = 0.058, p for heterogeneity = 0.32, I 2 = 14 %) (Fig. 8). Conversely, the occurrence of IH was significantly different between LPS and open surgery for both colonic resection only (RR 0.54, [0.39, 0.76] p for effect < 0.001, p for heterogeneity = 0.15, I 2 = 34 %) and rectum resection only (RR 0.54, [0.38, 0.77] p for effect = 0.001, p for heterogeneity = 0.27, I 2 = 21 %) (Fig. 9). In studies reporting subgroup analysis for rectal resection [7, 17, 20, 29, 30, 35], median conversion rate was 16 % (interquartile range 8–22 %).
Visual inspection of funnel plots did not identify a skewed or asymmetrical shape (Supplemental digital contents 7–8). Sequential removal of individual studies did not identify any study with excessive influence on results. Quantitative evaluation did not suggest the presence of publication bias, as measured by the Peter test (p = 0.74 for SBO analysis and p = 0.14 for IH analysis) and the Egger test (p = 0.60 for SBO analysis and p = 0.59 for IH analysis) on the overall complication rate.
Discussion
The present meta-analysis found that laparoscopic colorectal surgery is associated with a significant reduction in SBO and IH compared to the open approach. Limiting the analysis to RCTs only, the incidence of SBO was significantly lower in patients treated with laparoscopy, while the reduction in IH only approached statistical significance. Sensitivity analyses showed that the laparoscopic approach is associated with a significant reduction in both SBO and IH only in studies with low conversion rate.
The growing popularity of colorectal laparoscopic approach among surgeons and patients is due to its demonstrated advantages in the short term [1]. Moreover, RCTs confirmed that LPS did not adversely affect the chance of cure for colonic cancer [2]. Among the potential long-term advantages of LPS, a reduction in SBO and IH rates has been hypothesized in several comparative studies with contrasting results [5–7, 16]. The present meta-analysis explores this issue and represents a substantial update from a previous Cochrane review [37] in terms of number of studies and patients included. To clarify the effect of factors potentially influencing the occurrence of SBO and IH such as conversion to open surgery, length of follow-up, and type of procedure (colonic or rectal resection), specific sensitivity and subgroup analyses were performed.
SBO is a frequent cause of hospital admission and eventually late reoperation after colorectal surgery [38, 39]. Postoperative adhesion formation takes place in response to injury of the peritoneal surfaces involving a complex interaction of many factors secreted by cells proximate to the traumatized areas [40]. The minimally invasive approach has the potential to reduce adhesion formation because of attenuated surgical trauma, less tissue handling, and smaller scars [41]. Our analysis found that LPS significantly reduced SBO by almost half when compared to open surgery. This was confirmed when limiting the analysis to RCTs and to trials at low risk of bias. Sensitivity analyses confirmed the reduction in SBO in LPS when considering subgroups with low conversion rate and colon resection, whereas no significant reduction was found including studies with high conversion rate and rectal resection.
Incisional hernia occurs in up to 30 % patients receiving a laparotomy and often enlarges over time leading to pain and potentially serious complication such as bowel obstruction, incarceration and strangulation [30, 31]. The possible reduction in IH in LPS surgery could derive from smaller incisions, better preservation of the abdominal wall, and lower wound infection rate compared to open approach. In the analysis we performed, LPS significantly reduced the risk of IH by 40 % when compared with open surgery. However, this effect was not confirmed when the analysis was limited to RCTs or when trials at high risk of bias were excluded. Sensitivity analyses confirmed the reduction in IH by LPS when considering studies with low conversion rate, whereas no difference was found including the studies with a high conversion rate only.
The impact of different factors on the occurrence of SBO and IH has been investigated by specifically focused sensitivity analyses. Conversion to open surgery was a key effect modifier when analyzing the impact of laparoscopy on both SBO and IH. When the analysis was limited to studies with conversion rate higher than 15 %, no advantage from the laparoscopic approach was found. In fact, as conversion rate increases, the number of patients initially allocated to the LPS group who really benefit from the minimally invasive approach is reduced. Moreover, previous research has shown that patients converted from laparoscopic to open surgery experience more complications than those operated with a straightforward open approach [7]. A per-protocol analysis, which includes in the LPS arm only those patients who had a successful laparoscopic resection, would better ascertain the impact of the minimally invasive technique on long-term morbidity, but it would not reflect real-life clinical practice. Length of follow-up did not substantially impact on results, despite studies suggesting that long-term morbidity can occur several years after the primary surgery [13, 16].
No significant advantage from laparoscopic approach on SBO rates was found in patients who underwent rectal surgery. However, only few studies, most of which were non-randomized, reported subgroup data for rectal surgery. This limited the power of our analysis and increased the risk of bias. In addition, half of these trials [7, 29, 30] had conversion rates for rectal resection >20 %, which significantly reduces the protective effect of LPS. It should also be noted that rectal cancer patients are routinely undergoing neoadjuvant or adjuvant radiotherapy, which may have facilitated the occurrence of postoperative pelvic adhesions and SBO in both groups. Thus, to correctly identify the influence of the surgical approach on long-term complications following rectal resection, additional data from novel and specifically designed prospective studies accounting for confounding factors are required.
A limitation of our meta-analysis is that several included trials are of suboptimal quality especially non-randomized trials, carrying a high risk of bias. To avoid possible influences due to the poor quality of some studies, separate sensitivity analyses focused on RCTs and excluding trials at high risk of bias were performed. In addition, no risk of small studies bias or publication bias was detected, and no single study was identified as excessively influencing overall results. Another limitation concerning all studies included is that none of them was primarily designed and powered to detect possible differences in long-term complications between minimally invasive and open surgery, rather it represented a secondary analysis of studies powered on short-term results or cancer survival. Furthermore, subgroup analysis for colon and rectal resection were limited because of reduced sample size and a significant amount of missing data. Finally, it should also be noted that, although outcome measures and sensitivity analyses were planned ahead before pooling the data, the study protocol was not registered in a systematic review database (e.g., PROSPERO).
In conclusion, this meta-analysis found that laparoscopic colorectal surgery is associated with a significant reduction in SBO and IH compared to the open approach. When conversion rate is high, the protective role of laparoscopy for the occurrence of both SBO and IH disappears.
References
Schwenk W, Haase O, Neudecker J, Muller JM (2005) Short term benefits for laparoscopic colorectal resection. Cochrane Database Syst Rev. doi:10.1002/14651858.CD003145.pub2
Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol 10:44–52
Bonjer HJ, Deijen CL, Abis GA, Cuesta MA, van der Pas MH, de Lange-de Klerk ES, Lacy AM, Bemelman WA, Andersson J, Angenete E, Rosenberg J, Fuerst A, Haglind E, Group CIS (2015) A randomized trial of laparoscopic versus open surgery for rectal cancer. N Engl J Med 372:1324–1332
Jeong SY, Park JW, Nam BH, Kim S, Kang SB, Lim SB, Choi HS, Kim DW, Chang HJ, Kim DY, Jung KH, Kim TY, Kang GH, Chie EK, Kim SY, Sohn DK, Kim DH, Kim JS, Lee HS, Kim JH, Oh JH (2014) Open versus laparoscopic surgery for mid-rectal or low-rectal cancer after neoadjuvant chemoradiotherapy (COREAN trial): survival outcomes of an open-label, non-inferiority, randomised controlled trial. Lancet Oncol 15:767–774
Bartels SA, Vlug MS, Hollmann MW, Dijkgraaf MG, Ubbink DT, Cense HA, van Wagensveld BA, Engel AF, Gerhards MF, Bemelman WA, Collaborative LSG (2014) Small bowel obstruction, incisional hernia and survival after laparoscopic and open colonic resection (LAFA study). Br J Surg 101:1153–1159
Scholin J, Buunen M, Hop W, Bonjer J, Anderberg B, Cuesta M, Delgado S, Ibarzabal A, Ivarsson ML, Janson M, Lacy A, Lange J, Pahlman L, Skullman S, Haglind E (2011) Bowel obstruction after laparoscopic and open colon resection for cancer: results of 5 years of follow-up in a randomized trial. Surg Endosc 25:3755–3760
Taylor GW, Jayne DG, Brown SR, Thorpe H, Brown JM, Dewberry SC, Parker MC, Guillou PJ (2010) Adhesions and incisional hernias following laparoscopic versus open surgery for colorectal cancer in the CLASICC trial. Br J Surg 97:70–78
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6:e1000100
Schardt C, Adams MB, Owens T, Keitz S, Fontelo P (2007) Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inform Decis Mak 7:16
Robinson KA, Dickersin K (2002) Development of a highly sensitive search strategy for the retrieval of reports of controlled trials using PubMed. Int J Epidemiol 31:150–153
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ (Clinical research ed) 343:d5928
Savovic J, Weeks L, Sterne JA, Turner L, Altman DG, Moher D, Higgins JP (2014) Evaluation of the Cochrane Collaboration’s tool for assessing the risk of bias in randomized trials: focus groups, online survey, proposed recommendations and their implementation. Syst Rev 3:37
Mudge M, Hughes LE (1985) Incisional hernia: a 10 year prospective study of incidence and attitudes. Br J Surg 72:70–71
Peters JL, Sutton AJ, Jones DR, Abrams KR, Rushton L (2006) Comparison of two methods to detect publication bias in meta-analysis. JAMA 295:676–680
Ng SS, Lee JF, Yiu RY, Li JC, Hon SS, Mak TW, Ngo DK, Leung WW, Leung KL (2014) Laparoscopic-assisted versus open total mesorectal excision with anal sphincter preservation for mid and low rectal cancer: a prospective, randomized trial. Surg Endosc 28:297–306
Ng SS, Leung KL, Lee JF, Yiu RY, Li JC, Hon SS (2009) Long-term morbidity and oncologic outcomes of laparoscopic-assisted anterior resection for upper rectal cancer: ten-year results of a prospective, randomized trial. Dis Colon Rectum 52:558–566
Braga M, Pecorelli N, Frasson M, Vignali A, Zuliani W, Carlo VD (2011) Long-term outcomes after laparoscopic colectomy. World J Gastrointest Oncol 3:43–48
Eshuis EJ, Slors JF, Stokkers PC, Sprangers MA, Ubbink DT, Cuesta MA, Pierik EG, Bemelman WA (2010) Long-term outcomes following laparoscopically assisted versus open ileocolic resection for Crohn’s disease. Br J Surg 97:563–568
Gervaz P, Mugnier-Konrad B, Morel P, Huber O, Inan I (2011) Laparoscopic versus open sigmoid resection for diverticulitis: long-term results of a prospective, randomized trial. Surg Endosc 25:3373–3378
Polle SW, Dunker MS, Slors JF, Sprangers MA, Cuesta MA, Gouma DJ, Bemelman WA (2007) Body image, cosmesis, quality of life, and functional outcome of hand-assisted laparoscopic versus open restorative proctocolectomy: long-term results of a randomized trial. Surg Endosc 21:1301–1307
Stocchi L, Milsom JW, Fazio VW (2008) Long-term outcomes of laparoscopic versus open ileocolic resection for Crohn’s disease: follow-up of a prospective randomized trial. Surgery 144:622–627 (discussion 627–628)
Winslow ER, Fleshman JW, Birnbaum EH, Brunt LM (2002) Wound complications of laparoscopic vs open colectomy. Surg Endosc 16:1420–1425
Andersen LP, Klein M, Gogenur I, Rosenberg J (2008) Incisional hernia after open versus laparoscopic sigmoid resection. Surg Endosc 22:2026–2029
Champault GG, Barrat C, Raselli R, Elizalde A, Catheline JM (2002) Laparoscopic versus open surgery for colorectal carcinoma: a prospective clinical trial involving 157 cases with a mean follow-up of 5 years. Surg Laparosc Endosc Percutan Tech 12:88–95
Duepree H-J, Senagore AJ, Delaney CP, Fazio VW (2003) Does means of access affect the incidence of small bowel obstruction and ventral hernia after bowel resection? J Am Coll Surg 197:177–181
Eshuis EJ, Polle SW, Slors JF, Hommes DW, Sprangers MA, Gouma DJ, Bemelman WA (2008) Long-term surgical recurrence, morbidity, quality of life, and body image of laparoscopic-assisted vs. open ileocolic resection for Crohn’s disease: a comparative study. Dis Colon Rectum 51:858–867
Franklin ME Jr, Rosenthal D, Abrego-Medina D, Dorman JP, Glass JL, Norem R, Diaz A (1996) Prospective comparison of open vs. laparoscopic colon surgery for carcinoma. Five-year results. Dis Colon Rectum 39:S35–S46
Ihedioha U, Mackay G, Leung E, Molloy RG, O’Dwyer PJ (2008) Laparoscopic colorectal resection does not reduce incisional hernia rates when compared with open colorectal resection. Surg Endosc 22:689–692
Kellokumpu IH, Kairaluoma MI, Nuorva KP, Kautiainen HJ, Jantunen IT (2012) Short- and long-term outcome following laparoscopic versus open resection for carcinoma of the rectum in the multimodal setting. Dis Colon Rectum 55:854–863
Laurent C, Leblanc F, Bretagnol F, Capdepont M, Rullier E (2008) Long-term wound advantages of the laparoscopic approach in rectal cancer. Br J Surg 95:903–908
Llaguna OH, Avgerinos DV, Lugo JZ, Matatov T, Abbadessa B, Martz JE, Leitman IM (2010) Incidence and risk factors for the development of incisional hernia following elective laparoscopic versus open colon resections. Am J Surg 200:265–269
Makni A, Chebbi F, Ksantini R, Fetirich F, Bedioui H, Jouini M, Kacem M, Ben Mami N, Filali A, Ben Safta Z (2013) Laparoscopic-assisted versus conventional ileocolectomy for primary Crohn’s disease: results of a comparative study. J Visc Surg 150:137–143
Patankar SK, Larach SW, Ferrara A, Williamson PR, Gallagher JT, DeJesus S, Narayanan S (2003) Prospective comparison of laparoscopic vs. open resections for colorectal adenocarcinoma over a ten-year period. Dis Colon Rectum 46:601–611
Pereira JA, Pera M, Grande L (2013) Incidence of incisional hernia after open and laparoscopic colorectal cancer resection. Cir Esp 91:44–49
Saklani AP, Naguib N, Shah PR, Mekhail P, Winstanley S, Masoud AG (2013) Adhesive intestinal obstruction in laparoscopic vs open colorectal resection. Colorectal Dis 15:80–84
Vignali A, De Nardi P, Ghirardelli L, Di Palo S, Staudacher C (2013) Short and long-term outcomes of laparoscopic colectomy in obese patients. World J Gastroenterol WJG 19:7405–7411
Kuhry E, Schwenk WF, Gaupset R, Romild U, Bonjer HJ (2008) Long-term results of laparoscopic colorectal cancer resection. Cochrane Database Syst Rev. doi:10.1002/14651858.CD003432.pub2
Lee L, Mappin-Kasirer B, Sender Liberman A, Stein B, Charlebois P, Vassiliou M, Fried GM, Feldman LS (2012) High incidence of symptomatic incisional hernia after midline extraction in laparoscopic colon resection. Surg Endosc 26:3180–3185
Parker MC, Wilson MS, Menzies D, Sunderland G, Clark DN, Knight AD, Crowe AM, Surgical Clinical Adhesions, Research G (2005) The SCAR-3 study: 5-year adhesion-related readmission risk following lower abdominal surgical procedures. Colorectal Dis 7:551–558
Holmdahl L, Eriksson E, Eriksson BI, Risberg B (1998) Depression of peritoneal fibrinolysis during operation is a local response to trauma. Surgery 123:539–544
Rosin D, Zmora O, Hoffman A, Khaikin M, Zakai BB, Munz Y, Shabtai M, Ayalon A (2007) Low incidence of adhesion-related bowel obstruction after laparoscopic colorectal surgery. J Laparoendosc Adv Surg Tech 17:604–607
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Nicolò Pecorelli, Massimiliano Greco, Salvatore Amodeo, and Marco Braga have no conflict of interest to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pecorelli, N., Greco, M., Amodeo, S. et al. Small bowel obstruction and incisional hernia after laparoscopic and open colorectal surgery: a meta-analysis of comparative trials. Surg Endosc 31, 85–99 (2017). https://doi.org/10.1007/s00464-016-4995-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-4995-6