Abstract
Background and aim
To audit short- and long-term outcomes after laparoscopic common bile duct exploration (LCBDE) and factors influencing the success of the laparoscopic treatment.
Methods
From January 1999 to December 2011, 288 patients (93 males) underwent a single-stage laparoscopic cholecystectomy combined with LCBDE in two Finnish Hospitals. Short-term outcome data were collected prospectively. Long-term outcomes were examined retrospectively. The main measures of outcome were the success of laparoscopic CBD stone clearance and recurrence of CBD stones in the long-term, with 30-day mortality, morbidity, and the length of postoperative hospital stay as secondary outcome measures.
Results
CBD stones were successfully removed by one-stage laparoscopic procedure in 232 of the 279 patients (83.2 %) with verified CBD stones and after conversion to open surgery in additional 28 patients (93.2 %). Nineteen patients (6.8 %) having residual stones after surgery were successfully treated with postoperative ERCP. On multivariate analysis, the independent factors associated with a failed laparoscopic stone clearance were stone size over 7 mm [OR 3.51 (95 % CI 1.53–8.03), p = 0.003], difficult anatomy [OR 18.01 (5.03–64.49), p < 0.001] and transcholedochal approach [OR 2.98 (1.37–4.47), p = 0.006]. Laparoscopic stone clearance also failed in all 11 patients having impacted stones at the ampulla of Vater. Cumulative long-term recurrence rate was 3.6 % at 5 years and 6.0 % at 10 years. Thirty-day mortality was 0.3 % and morbidity 12.2 %. Postoperative hospital stay was median 2 (IQR 1–3) days after transcystic CBD removal and 4 (IQR 3–7) days after transcholedochal CBD removal, p < 0.001.
Conclusion
Our results show that one-stage LC combined with LCBDE stone clearance is safe and effective in most patients thus reducing the number of additional, potentially dangerous endoscopic procedures. Moreover, large or impacted stones are a risk factor for failed stone clearance.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
In the era of open cholecystectomy, open bile duct surgery was superior to preoperative endoscopic retrograde cholangiography (ERCP) in achieving common bile duct (CBD) stone clearance [1–5]. The introduction of laparoscopic cholecystectomy in the early 90’s was associated with increased use of ERCP and endoscopic sphincterotomy (ES) to treat CBD stones because operative clearance of CBD stones along with laparoscopic cholecystectomy was not considered technically possible [6]. Today, patients with CBD stones undergoing laparoscopic cholecystectomy can be managed by laparoscopic CBD exploration and stone removal at the time of surgery, or by pre-, intra or postoperative ERCP [7, 8].
The goal of therapy in choledocholithiasis is to achieve ductal clearance with the fewest number of interventions, least morbidity and lowest costs. Current evidence suggests that laparoscopic CBD stone clearance is as efficient as pre- or postoperative ERCP/ES resulting in a reduced number of total procedures, shorter hospital stay and similar mortality and morbidity [9–15]. Despite good short-term outcomes after laparoscopic CBD stone removal the management of CBD stones in patients who need to undergo cholecystectomy is still controversial and most surgeons prefer two-stage treatment strategy.
Long-term complications after laparoscopic CBD stone removal such as bile duct strictures and recurrent stones are scantily reported in the literature [16–18]. We therefore examined short and long-term results of one-stage laparoscopic cholecystectomy and CBD stone removal and factors influencing the success of the laparoscopic treatment.
Materials and methods
From January 1999 to December 2011, 288 patients with gallbladder stones and suspected CBD stones underwent laparoscopic cholecystectomy combined with laparoscopic CBD exploration (LCBDE) at the Central Hospital of Central Finland (N = 198) and at Hyvinkää Hospital in Hospital District of Helsinki and Uusimaa (N = 90). Central Hospital of Central Finland is a university affiliated to large teaching hospital. The technique of LCBDE was first adopted by IK after an appropriate training course in 1995. The study patients were operated by four experienced laparoscopic upper GI-surgeons trained by IK and having large experience in open and laparoscopic cholecystectomies. Included were patients undergoing elective or emergency laparoscopic cholecystectomy with preoperative or intraoperative confirmation of choledocholithiasis, as well as patients with gallbladder in situ having residual CBD stones after preoperative ERCP/ES. Excluded were patients with severe pancreatitis or cholangitis, as well as patients with significant comorbidity in whom a prolonged laparoscopic procedure would have been potentially harmful. Common bile duct stones were suspected on the basis of clinical, laboratory, ultrasonographic and since 2002 preoperative magnetic resonance cholangiopancreaticography (MRCP) findings in 288 patients and verified in 279 patients by intraoperative cholangiography (IOC) and choledochoscopy. Before the MRCP era ERCP was occasionally used to diagnose and treat CBD stones.
Preoperative and short-term outcome data were collected prospectively. Long-term outcome was investigated retrospectively using a mailed, self-completed questionnaire about jaundice, diagnosis and treatment of recurrent CBD stones, as well as the date of diagnosis of recurrent stones. Missing data were completed by phone calls. Hospital records were also carefully reviewed. The causes of death were obtained from the National Cause of Death Registry. The study was approved by the hospital administration.
Surgical technique
A standard operative technique was used as described earlier [19]. A 4-trocar technique was used for laparoscopic cholecystectomy. After verification of CBD stones by intraoperative cholangiography, a fifth 5 mm trocar was introduced under the right costal margin in midclavicular position for the choledochoscope. Transcystic (TC) CBD exploration was preferred for stones less than 7–8 mm in diameter, stone number ≤3, and if the cystic junction was lateral. Choledochotomy was chosen for large stones (>7–8 mm) causing ductal dilatation, multiple stones, if the CBD stones were situated above the cystic duct junction or the cystic junction was posterior, or if the TC approach failed. Stones were removed using Dormia basket, Fogarty balloon catheter or flushing and pushing techniques as described in the literature [20]. The cystic duct was not routinely dilated. Hyoscine butylbromide (Buscopan) was used to relax the sphincter of Oddi. The clearance of CBD was confirmed with choledochoscopy and/or cholangiography. If residual stones were detected intraoperatively they were removed by repeated choledochoscopy or conversion to open procedure in order to achieve one-stage clearance of the CBD stones. Choledochotomy was closed using 4-0 or 5-0 absorbable interrupted monofilament sutures. In the beginning of our series, T-tube was inserted routinely after choledochotomy. Later on T-tube was used selectively and the decision to insert a T-tube or to do a primary choledochotomy closure was left to the discretion of the operating surgeon. The cystic duct was closed by clips or sutured. Cholecystectomy was performed after laparoscopic CBD clearance with a diathermy hook in a retrograde manner. An abdominal drain was placed in the sub-hepatic space and removed postoperatively if no bilious drainage was detected. T-tube was removed 8–10 days after surgery in the outpatient department. The indications for postoperative ERCP were uncertainty about complete CBD stone clearance during the index operation, residual stones shown by postoperative T-tube cholangiography, or postoperative bile leakage or jaundice.
Definitions
Conversion to open surgery was defined as a necessity to interrupt the laparoscopic procedure and to proceed with open technique. Postoperative 30-day complications were classified according to the Dindo-Clavien classification [21]. Primary treatment failure was defined as a failure of CBD stone clearance by laparoscopic means and necessity to do a conversion to open surgery or postoperative ERCP in order to complete duct clearance. Retained CBD stones were defined as stones detected within 1 year after the index operation, and recurrent stones were defined as stones found 1 year after the index operation. Difficult anatomy was defined as an unclear anatomy in the hepatocystic triangle due to severe adhesions, fibrotic scarring, posterior insertion of the cystic duct to CBD or if the patient had a Mirizzi syndrome.
Statistical analysis
The data are presented as means with standard deviations (SD), medians with interquartile range (IQR) or counts with percentages. The 95 % confidence intervals (95 % CI) are given for the most important outcomes. The groups were compared using the Mann–Whitney U-test or the χ 2-test. Cumulative recurrence rate analysis was based on the product limit estimate (Kaplan–Meier) of the cumulative “survival “function. Binary logistic regression analysis was used to assess factors affecting the success of laparoscopic CBD clearance. Statistical analyses were performed using SPSS statistical software.
Results
Baseline characteristics of the 279 patients are shown in Table 1. The diagnostic work-up included preoperative MRCP in 153 (54.8 %), intraoperative cholangiography in 259 patients (92.8 %), and choledochoscopy in all patients. In addition, preoperative ERCP with CBD stone removal was done in 27 patients (9.7 %) still having CBD stones at the time of LC. Biliary pain was the most common presenting symptom (81.7 %) followed by jaundice (21.9 %), signs of acute cholecystitis (13.3 %), and history of previous biliary pancreatitis (10.4 %). Histopathological findings of the gallbladder are shown in Table 1.
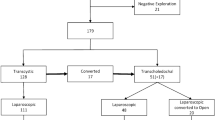
Intraoperative data are shown in Table 2. Common bile duct exploration was performed via the cystic duct in 177 of the 279 patients (63.4 %) and through a choledochotomy in 102 patients (36.6 %). Conversion to open surgery was necessary in 37 patients (13.3 %) because of failed laparoscopic stone clearance in 13 patients (35.1 %) and other causes (64.9 %) making the laparoscopic operation difficult (Table 2). In the emergency operations, the conversion rate to open surgery was significantly higher than conversion in the elective operations: 29.7 % (11 of 37 patients) versus 10.7 % (26 of 242 patients), p = 0.005, the main reason being difficult or unclear anatomy. Short-term outcome is shown in Table 3.
Success of laparoscopic CBD stone removal
Successful laparoscopic CBD stone clearance was achieved in 232 of the 279 (83.2 %) patients, and after conversion to open surgery in additional 28 patients with an overall success rate of 93.2 % for one-stage procedure. In elective operations, laparoscopic CBD stone clearance was successful in 206 of the 242 patients (85.1 %) and in emergency operations in 26 of the 37 patients (70.3 %), p = 0.025, and after conversion to open surgery in 93.8 versus 89.2 %, p = 0.300. T-tube was inserted in 57 patients. Retained stones after surgery were found in 19 of 279 patients (6.8 %) either by postoperative T-tube cholangiography in 10 patients (3.6 %) or ERCP in 9 patients (3.2 %). On multivariate analysis, the independent factors associated with a failed laparoscopic stone clearance were stone size over 7 mm [OR 3.51 (95 % CI 1.53–8.03), p = 0.003], difficult anatomy [OR 18.01 (5.03–64.49), p < 0.001], and transcholededochal approach [OR 2.98 (1.37 to 4.47), p = 0.006]. Laparoscopic CBD stone removal also failed in all 11 patients having impacted stones at the ampulla of Vater. All retained stones were removed by ERCP.
Postoperative ERCP was also performed in additional nine patients to confirm the complete clearance of CBD (four patients), and to treat bile leak (four patients) or to dilate a CBD stricture (one patient).
Long-term outcome
Long-term outcome data were available in 259 of 279 patients (response rate 92.8 %) having a median follow-up time 5.1 years (IQR 2.9–7.8 years). Of the 279 patients, 19 patients had died of the following reasons: coronary heart disease (10), pneumonia (3), ovarian cancer (1), herpes encephalitis (1), traffic accident (1), colon cancer (1), sepsis of unknown origin (1), and gallbladder cancer (1) in an 80-year-elderly patient having comorbid conditions and a with an incidental finding of T2 gallbladder cancer in the histopathological examination. One CBD stricture was observed during the index operation and was successfully treated with ERCP and balloon dilatation. The crude incidence of recurrent stones was 3.5 % (9 of 259 patients: one patient had cholangitis and 8 other had biliary pain with elevated liver tests). Recurrent ductal stones were verified with MRCP and successfully removed by ERCP. The cumulative 5-year and 10-year recurrence rates of CBD stones was 3.6 % (95 %CI 1.8–7.3 %) at 5 years and 6.0 % (2.5–14.0 %) at 10 years (Fig. 1). Median time to recurrence was 1.4 years (IQR 1.0–4.2 years).
Secondary outcome measures
The 30-day morbidity was 12.2 %: surgical complications occurred in 18 patients (6.5 %) and general complications in 16 patients (5.7 %). There were no ERCP-related complications. Reoperation was done in 3 (1.1 %) patients: 2 for bile leak and 1 for hemorrhage. Severe (Dindo-Clavien IIIb-V) complications were observed in 12 patients (4.3 %). Bile leaks were observed in 7 (2.5 %) patients. One 73 -year-old female patient died of Clostridium perfringens sepsis. Postoperative hospital stay was median 3 days (IQR 2–5): transcystic group 2 days (IQR 1–3) and choledochotomy group 4 days (IQR 3–7). p < 0.001. One patient was readmitted because of fever of unknown origin.
Discussion
The ideal treatment for CBD stones is still controversial [8]. At present, CBD stones are commonly managed with preoperative or postoperative ERCP although one-stage laparoscopic cholecystectomy combined with laparoscopic CBD stone clearance is increasingly reported in the literature. According to a recent meta-analysis and randomized controlled trials successful laparoscopic CBD stone clearance has been reported in 75–100 % of the patients with an associated morbidity from 11 to 43 % [9–15, 22, 23]. In line with that our success rate of CBD stone removal was 83.2 % after laparoscopy alone and 93.2 % after conversion to open surgery. This was achieved with low 30-day morbidity (12.2 %), reoperation (1.1 %) and readmission (0.4 %) rates, short hospital stay (median 3 days), and a low incidence of retained stones (6.8 %) which were removed by postoperative ERCP. Independent determinants for failed laparoscopic CBD stone removal were stone size ≥7 mm, transductal approach and difficult anatomy of the cystohepatic triangle due to adhesions, scarring, and fibrosis. Moreover, the success rate of laparoscopic CBD stone clearance was lower in the emergency operations than in the elective operations.
It is well known that the success or failure of laparoscopic CBD stone clearance is related to patient selection, surgeon’s experience, and quality of surgery. Our conversion rate of 13.3 % is in agreement with previous studies reporting conversion rates from 3.5 to 25 % [9–13]. Of note, the main reasons for conversion in our study were severe adhesions and chronic inflammation in the cystohepatic triangle making laparoscopic surgery difficult. The high rate of acute and chronic cholecystitis in this study may explain the reason for conversion in the difficult anatomy group. Only 13 of the 37 patients (35.1 %) were converted because of an unsuccessful CBD removal. Patients with impacted stones at ampulla of Vater were all converted to open surgery because no mechanical, electrohydraulic, or laser lithotripsy was available. An improvement for CBD stone clearance has been reported when using electrohydraulic lithotripsy [24]. Moreover, it was our aim to do one-stage surgical procedure either laparoscopically or after conversion to avoid postoperative ERCPs, which also have a known morbidity and treatment failure rate [23].
Long-term ductal stone recurrence rates after laparoscopic CBD stone clearance are scantily reported in the literature [16, 17, 25, 26]. Our 5-year (3.6 %) and 10-year (6.0 %) recurrence rates compare favorably to previous long-term results reporting stone recurrence rates from 0 to 6.7 % [16, 17, 25, 26]. In comparison, long-term results after ERCP and ES have shown recurrent choledocholithiasis in 5.8–11 % [27–30]. Whether CBD stones detected after the index operation were retained or recurrent stones are uncertain. In our study retained CBD stones were diagnosed by a completion cholangiography and choledochoscopy during the index operation, and postoperative T-tube cholangiography or occasionally postoperative ERCP after surgery.
According to meta-analysis and randomized clinical trials [9–15, 22], the advantages of one-stage laparoscopic cholecystectomy and CBD stone clearance are a reduced number of total procedures, lower costs, shorter hospital stay, and similar morbidity and mortality when compared with 2-stage endo-laparoscopic approach [7, 23, 31–33]. In our series, the 30-day mortality and overall morbidity rates were low in agreement with previous studies [9–12, 15]. The number of major postoperative bile leaks (2.2 %) necessitating endoscopic (N = 4) or operative treatment (N = 2), as well as reoperation and readmission rates was very low. Similar outcomes and even greater bile leak rates have been published [13, 17, 24]. Thus, laparoscopic cholecystectomy combined with laparoscopic CBD stone clearance can be done without major risks in daily clinical practice. This finding is also supported by a large, Swedish population-based study comparing different management strategies for CBD stones during five decades [34].
Potential disadvantages of ERCP/ES include the risk of serious complications, costs, and the inconvenience of undergoing a subsequent laparoscopic cholecystectomy for gallbladder stones. Besides, about 2–15 % of patients who undergo preoperative ERCP and sphincterotomy have residual ductal stones at intraoperative cholangiogram as shown also here. Post-procedural mortality is <1 % and morbidity from 5 to 11 % including post-ERCP pancreatitis, duodenal perforation, sepsis, and bleeding [8]. Endoscopic sphincterotomy also causes bacterobilia in all patients and predisposes the CBD to the increased risk of recurrent bilirubinate stones in the long term. An advantage of surgical CBD exploration is that the sphincter anatomy is not distorted. Moreover, the incidence of postoperative pancreatitis after LCBDE is rare (0.4–0.5 %) [16, 25] and was here 0 %. Postoperative recovery after transcystic CBD stone clearance was similar to that reported after laparoscopic cholecystectomy alone [16, 35] and significantly shorter than after transcholedochal clearance.
A major challenge with this study and other similar studies was the lack of randomization which may have caused some selection bias. For logistic reasons, some patients with CBD stones, as well as elderly high-risk patients with comorbidities have been managed by 2-stage endo-laparoscopic approach instead of one-stage laparoscopic approach or by ERCP alone leaving the gallbladder in situ. The learning curve and evolving laparoscopic technique may have played a role as well. On the other hand, the long-term outcome was investigated in 259 of the 279 eligible patients. The compliance in this study compares favorably with earlier studies with some 93 % of the patients returning the questionnaire for long-term evaluation. The economical impact of laparoscopic CBD stone clearance compared to 2-stage endo-laparoscopic treatment remains to be analyzed in the future.
Conclusion
Our results show that laparoscopic cholecystectomy combined with laparoscopic CBD stone clearance is safe and effective method of treating CBD stones in most patients both in elective and emergency situations, thus reducing the number of additional, potentially dangerous endoscopic procedures. Moreover, large or impacted stones at the ampulla of Vater are risk factors for failed stone clearance.
References
Stiegmann GV, Goff JS, Mansour A, Pearlman N, Reveille RM, Norton L (1992) Precholecystectomy endoscopic cholangiography and stone removal is not superior to cholecystectomy, cholangiography, and common duct exploration. Am J Surg 163:227–230
Hammarstrom LE, Holmin T, Stridbeck H, Ihse I (1995) Long-term follow-up of a prospective randomized study of endoscopic versus surgical treatment of bile duct calculi in patients with gallbladder in situ. Br J Surg 82:1516–1521
Kapoor R, Kaushik SP, Saraswat VA, Choudhuri G, Sikora SS, Saxena R, Kapoor VK (1996) Prospective randomized trial comparing endoscopic sphincterotomy followed by surgery with surgery alone in good risk patients with choledocholithiasis. HPB Surg 9:145–148
Targarona EM, Ayuso RM, Bordas JM, Ros E, Pros I, Martinez J, Teres J, Trias M (1996) Randomised trial of endoscopic sphincterotomy with gallbladder left in situ versus open surgery for common bileduct calculi in high-risk patients. Lancet 347:926–929
Suc B, Escat J, Cherqui D, Fourtanier G, Hay JM, Fingerhut A, Millat B (1998) Surgery vs endoscopy as primary treatment in symptomatic patients with suspected common bile duct stones: a multicenter randomized trial. French Associations for Surgical Research. Arch Surg 133:702–708
Barwood NT, Valinsky LJ, Hobbs MS, Fletcher DR, Knuiman MW, Ridout SC (2002) Changing methods of imaging the common bile duct in the laparoscopic cholecystectomy era in Western Australia: implications for surgical practice. Ann Surg 235:41–50
Martin DJ, Vernon DR, Toouli J (2006) Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev. doi:10.1002/14651858.CD003327.pub2
Dasari BV, Tan CJ, Gurusamy KS, Martin DJ, Kirk G, McKie L, Diamond T, Taylor MA (2013) Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev 9:CD003327. doi:10.1002/14651858.CD003327.pub3
Cuschieri A, Lezoche E, Morino M, Croce E, Lacy A, Toouli J, Faggioni A, Ribeiro VM, Jakimowicz J, Visa J, Hanna GB (1999) EAES multicenter prospective randomized trial comparing two-stage vs single-stage management of patients with gallstone disease and ductal calculi. Surg Endosc 13:952–957
Rogers SJ, Cello JP, Horn JK, Siperstein AE, Schecter WP, Campbell AR, Mackersie RC, Rodas A, Kreuwel HT, Harris HW (2010) Prospective randomized trial of LC + LCBDE vs ERCP/S + LC for common bile duct stone disease. Arch Surg 145:28–33. doi:10.1001/archsurg.2009.226
Noble H, Tranter S, Chesworth T, Norton S, Thompson M (2009) A randomized, clinical trial to compare endoscopic sphincterotomy and subsequent laparoscopic cholecystectomy with primary laparoscopic bile duct exploration during cholecystectomy in higher risk patients with choledocholithiasis. J Laparoendosc Adv Surg Tech A 19:713–720. doi:10.1089/lap.2008.0428
Nathanson LK, O’Rourke NA, Martin IJ, Fielding GA, Cowen AE, Roberts RK, Kendall BJ, Kerlin P, Devereux BM (2005) Postoperative ERCP versus laparoscopic choledochotomy for clearance of selected bile duct calculi: a randomized trial. Ann Surg 242:188–192
Bansal VK, Misra MC, Garg P, Prabhu M (2010) A prospective randomized trial comparing two-stage versus single-stage management of patients with gallstone disease and common bile duct stones. Surg Endosc 24:1986–1989. doi:10.1007/s00464-010-0891-7
Rhodes M, Sussman L, Cohen L, Lewis MP (1998) Randomised trial of laparoscopic exploration of common bile duct versus postoperative endoscopic retrograde cholangiography for common bile duct stones. Lancet 351:159–161
Sgourakis G, Karaliotas K (2002) Laparoscopic common bile duct exploration and cholecystectomy versus endoscopic stone extraction and laparoscopic cholecystectomy for choledocholithiasis. A prospective randomized study. Minerva Chir 57:467–474
Paganini AM, Guerrieri M, Sarnari J, De Sanctis A, D’Ambrosio G, Lezoche G, Perretta S, Lezoche E (2007) Thirteen years’ experience with laparoscopic transcystic common bile duct exploration for stones Effectiveness and long-term results. Surg Endosc 21:34–40. doi:10.1007/s00464-005-0286-3
Waage A, Stromberg C, Leijonmarck CE, Arvidsson D (2003) Long-term results from laparoscopic common bile duct exploration. Surg Endosc 17:1181–1185. doi:10.1007/s00464-002-8937-0
Campbell-Lloyd AJ, Martin DJ, Martin IJ (2008) Long-term outcomes after laparoscopic bile duct exploration: a 5-year follow up of 150 consecutive patients. ANZ J Surg 78:492–494. doi:10.1111/j.1445-2197.2008.04541.x
Overby DW, Apelgren KN, Richardson W, Fanelli R, Society of American Gastrointestinal and Endoscopic Surgeons (2010) SAGES guidelines for the clinical application of laparoscopic biliary tract surgery. Surg Endosc 24:2368–2386. doi:10.1007/s00464-010-1268-7
Petelin JB (2003) Laparoscopic common bile duct exploration. Surg Endosc 17:1705–1715. doi:10.1007/s00464-002-8917-4
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196. doi:10.1097/SLA.0b013e3181b13ca2
Alexakis N, Connor S (2012) Meta-analysis of one- vs. two-stage laparoscopic/endoscopic management of common bile duct stones. HPB (Oxford) 14:254–259. doi:10.1111/j.1477-2574.2012.00439.x;10.1111/j.1477-2574.2012.00439.x
Tranter SE, Thompson MH (2002) Comparison of endoscopic sphincterotomy and laparoscopic exploration of the common bile duct. Br J Surg 89:1495–1504. doi:10.1046/j.1365-2168.2002.02291.x
Noble H, Whitley E, Norton S, Thompson M (2011) A study of preoperative factors associated with a poor outcome following laparoscopic bile duct exploration. Surg Endosc 25:130–139. doi:10.1007/s00464-010-1146-3
Berthou JC, Dron B, Charbonneau P, Moussalier K, Pellissier L (2007) Evaluation of laparoscopic treatment of common bile duct stones in a prospective series of 505 patients: indications and results. Surg Endosc 21:1970–1974. doi:10.1007/s00464-007-9387-5
Bove A, Bongarzoni G, Palone G, Di Renzo RM, Calisesi EM, Corradetti L, Di Nicola M, Corbellini L (2009) Why is there recurrence after transcystic laparoscopic bile duct clearance? Risk factor analysis. Surg Endosc 23:1470–1475. doi:10.1007/s00464-009-0377-7
Pereira-Lima JC, Jakobs R, Winter UH, Benz C, Martin WR, Adamek HE, Riemann JF (1998) Long-term results (7 to 10 years) of endoscopic papillotomy for choledocholithiasis. Multivariate analysis of prognostic factors for the recurrence of biliary symptoms. Gastrointest Endosc 48:457–464
Schreurs WH, Juttmann JR, Stuifbergen WN, Oostvogel HJ, van Vroonhoven TJ (2002) Management of common bile duct stones: selective endoscopic retrograde cholangiography and endoscopic sphincterotomy: short- and long-term results. Surg Endosc 16:1068–1072. doi:10.1007/s00464-001-9104-8
Ando T, Tsuyuguchi T, Okugawa T, Saito M, Ishihara T, Yamaguchi T, Saisho H (2003) Risk factors for recurrent bile duct stones after endoscopic papillotomy. Gut 52:116–121
Kim KH, Rhu JH, Kim TN (2012) Recurrence of bile duct stones after endoscopic papillary large balloon dilation combined with limited sphincterotomy: long-term follow-up study. Gut Liver 6:107–112. doi:10.5009/gnl.2012.6.1.107;10.5009/gnl.2012.6.1.107
Poulose BK, Arbogast PG, Holzman MD (2006) National analysis of in-hospital resource utilization in choledocholithiasis management using propensity scores. Surg Endosc 20:186–190. doi:10.1007/s00464-005-0235-1
Williams EJ, Green J, Beckingham I, Parks R, Martin D, Lombard M, British Society of Gastroenterology (2008) Guidelines on the management of common bile duct stones (CBDS). Gut 57:1004–1021. doi:10.1136/gut.2007.121657
Kharbutli B, Velanovich V (2008) Management of preoperatively suspected choledocholithiasis: a decision analysis. J Gastrointest Surg 12:1973–1980. doi:10.1007/s11605-008-0624-6
Stromberg C, Nilsson M (2011) Nationwide study of the treatment of common bile duct stones in Sweden between 1965 and 2009. Br J Surg 98:1766–1774. doi:10.1002/bjs.7690;10.1002/bjs.7690
Topal B, Aerts R, Penninckx F (2007) Laparoscopic common bile duct stone clearance with flexible choledochoscopy. Surg Endosc 21:2317–2321. doi:10.1007/s00464-007-9577-1
Disclosures
A Mattila, J Luhtala, J Mrena, I Kellokumpu and H Kautiainen have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mattila, A., Luhtala, J., Mrena, J. et al. An audit of short- and long-term outcomes after laparoscopic removal of common bile duct stones in Finland. Surg Endosc 28, 3451–3457 (2014). https://doi.org/10.1007/s00464-014-3620-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3620-9