Abstract
Introduction
The aim of this prospective controlled trial was the definition of the optimal timepoint for delayed closure after negative pressure wound therapy (NPWT) in the treatment of the open abdomen (OA) in septic patients after abdominal surgery. The delayed closure of the abdominal wall after abdominal NPWT treatment is often problematic due to the lateralization of the fascial edge leading to unfavorably high tensile forces of the adapting sutures in the midline. We present the results of an innovative combination of NPWT with a new fascial-approximation technique using dynamic fascial sutures (DFS) and delayed closure of the abdominal wall.
Methods
Eighty-seven patients subjected to OA therapy following surgery for secondary peritonitis were treated with NPWT and DFS. In all patients, a running suture of elastic vessel loops was used to approximate fascial edges. This procedure was continued for the duration of NPWT until final closure of the abdomen with running suture in 55 patients (63.2 %) and interrupted suture technique in eight patients (9.2 %). An anterior component separation was performed in seven patients.
Results
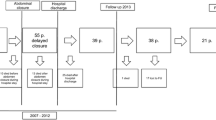
Delayed closure was achieved in 68 patients (78.2 %) after 12.6 days [mean (SD) 25.1 (2–204)] days and 4.3 re-operations [mean (SD) 6.0 (1–43)]. Fifteen (17.2 %) superficial and two (2.3 %) deep wound infections occurred. In three (3.4 %) cases, entero-atmospheric fistulas had to be treated. We recorded no technique-specific complications. Four (5.9 %) incisional hernia were detected in a mean follow-up of 40.5 months (16–65). Mortality rate was 55.2 %.
Conclusion
Using a new technique combining NPWT and DFS in the treatment of the OA, the delayed closure of the fascial edges by running suture can be achieved and the number of re-operations can be kept low. The technique was safe and led to a low incidence of incisional hernias. Extensive abdominal wall reconstruction was seldom required.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Since the introduction of negative pressure systems [negative pressure wound therapy (NPWT)] in the treatment of the open abdomen (OA) in septic patients [1] suffering from secondary peritonitis, morbidity and mortality has decreased significantly [2, 3]. The continuous negative pressure leads to a sufficient drainage of peritoneal fluids and prevents abdominal compartment syndrome. On the other hand, the perfusion of the intestinal and retroperitoneal organs is preserved. The most severe complications in the treatment of the OA are the frozen abdomen followed by entero-atmospheric fistulas [4]. The use of a special sheet for covering the intestine prevents these complications in the majority of the cases [5, 6]. The results of the literature suggest that NPWT is associated with the highest rates of fascial closure and the lowest mortality rates [2].
However, the primary delayed closure technique is one of the most discussed and predominantly complicated procedures after the successful treatment of the OA. The major obstacle to the closure is the lateralization of the rectus muscles, which should be avoided at all costs. Various approximation systems for this indication have been suggested and commercialized in the past [7–11]. The highest closure rates of 85–90 % are achieved by artificial burr and dynamic retention sutures [9–11]. Both techniques facilitate the delayed closures of the abdominal wall without high tension and the risk of acute and incisional hernia.
One of the crucial points is to determine the right time of primary delayed closure. In case of premature closure, the risk of a pertubated infection with the consequent need for a re-operation is high. On the other hand, a late closure is often associated with technical challenges and an inherent risk of high tension to the suture line. Therefore, the primary aims of this study were the prevention of the lateralization of the rectus muscles and the definition of the appropriate time to close the OA. Recurrences and other treatment-related complications were secondary parameters of interest.
Methods
Between September 2007 and December 2012, all consecutive patients undergoing emergent laparotomy and OA treatment were enrolled in this prospective study. Inclusion criteria were advanced peritonitis in more than one quadrant. Because of the prospective but non-randomized and non-comparative character of the study, the local ethical committee waived responsibility. Exclusion criteria for OA treatment with negative pressure were hemorrhage, localized peritonitis, or the ability to perform sufficient source control during the initial procedure in stable patients. The Mannheim Peritonitis Index (MPI), as well as the American Society of Anesthesiologists (ASA) score, was calculated at timepoint of the NPWT treatment and related to the different sources of sepsis in upper and lower gastrointestine (GI). For a comparison of the general infection score at the beginning of the OA therapy and closure of the abdomen, the C-reactive protein (CRP) [mg/dl] data and leukocyte number (g/μl) were recorded.
CRP and leukocyte data were compared between patients with wound infection and bland wound healing. Minimum follow-up was 10 days after abdominal closure. Technique of fascia closure and wound infection was compared in groups with and without incisional hernia.
The number of NPWT re-operations was assessed and different variables compared between ≤4 and >4 re-operations until delayed fascial closure: death during hospital stay, incisional hernia, complications, and wound infection. Further predictive data for death during hospital stay were evaluated.
Patient demographics
A total of 87 patients—39 (44.8 %) women and 48 (55.2 %) men; median age 69 years (range 25–93 years)—were included (Table 1). Indications were sepsis from an intra-abdominal infection. Source of infection was the upper GI (stomach, duodenum, small bowel) in 29.9 % of patients, the lower GI (large bowel, rectum) in 58.6 % of patients, and others in 11.5 % of patients (Table 1). Co-morbidities at the time of starting treatment of the OA using ASA score was a median of 2 (1–4), and the MPI median was 15 (5–29) (Table 1).
Surgical technique
Source control
The aim of primary surgical intervention was a rapid source control. Surgical intervention implied an extended lavage, especially in cases of widely-spread fecal contamination of the abdominal cavity.
Negative pressure wound therapy: technique
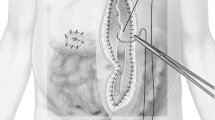
The surgical procedure always included a covering of the intestinal block using a sheet of vacuum dressing (VAC®; KCI, San Antonio, TX, USA). To achieve sufficient prevention of the fascial and muscle retention, dynamic fascial sutures (DFS) using elastic vessel loops were applied to the anterior sheet of the rectus muscle in a running technique. To achieve a safe approximation of the external aponeurosis, a bilateral dissection of 4–5 cm was performed (Fig. 1). The sutures were placed at least 2 cm apart from the midline to preserve the fascia for the delayed closure, and included only the aponeurosis without the rectus muscles. Only two long vessel loops in an uninterrupted suture technique were used to close the gap to a distance of 2 cm for assuring a sufficient suction of the dressing system and an elastic permanent approximation. The overlaps of the loops were fixed with a re-useable clip which enabled re-operation by loosening the two loops avoiding fascia resuturing with the drawback of repeated impairment of the fascial tissue (Fig. 2). Preserving the tissue of the linea alba, external aponeurosis and rectus muscle is crucial for later physiological safe closure of the abdomen. Finally, the OA was temporarily closed by a vacuum dressing using a continuously negative pressure of 90–125 mmHg. Postoperatively, patients were admitted to the intensive care unit (ICU) for further advanced treatment. The planned re-operation took place after 24 h and up to 48 h in an elective setting. In case of insufficient clearance of the peritoneal cavity, a reapplication of the abdominal vacuum dressing was performed.
Delayed primary fascial closure technique
After successful treatment of the OA by NPWT, the external fascia was prepared for a tension-free closure technique. In the beginning of the study, the closures were performed by non-resorbable running sutures (Prolene®, Ethicon, Norderstedt, Germany) and late resorbable sutures (PDS®, Ethicon, Norderstedt, Germany; MaxonPlus®, MonoMax®, Braun, Melsungen, Germany). In order to, in particular, minimize the risk of acute hernia due to a high tension, the suture technique at the start of the prospective study changed from ‘large bites’ to ‘small bites’, as recommended by Israelsson et al. [12–14]. In the large bites technique, the suture-to-wound length ratio was higher, at least 4:1, whereas in the small bites technique the ratio was at least 6:1 (Fig. 3). If a tension-free closure could not be achieved, additional anterior component separation (ACS), as described by Ramirez et al. [15], was performed (Fig. 3). In some cases a bulging on the site of ACS appeared. In these cases a prophylactic onlay mesh reinforcement was accomplished (Fig. 4).
Data collection and statistical analysis
Data collection included patients’ demographics, peritonitis score (MPI), inflammation scores (CRP, leukocytes), number of NPWT changes, duration of OA therapy, days in the ICU, fascial closure, complications, patient survival, incidence of incisional hernia, wound infections and clinically relevant events.
Results are represented as median and range, unless otherwise stated. Statistical testing was carried out using the Kolmogorov–Smirnov Test for Gaussian distribution. t-Test was used when comparing two groups and when data were normally distributed, or Mann–Whitney test when data were not normally distributed. Contingency testing was completed using Chi-square (>2 variables) and Fisher’s test (two variables, low n). p-Values of <0.05 were considered to indicate statistical significance.
Results
Delay of closure
Delayed closure was achieved in 68 patients (78.2 %) after 12.6 days [mean (SD) 25.1 (2–204)] and 4.3 re-operations [mean (SD) 6.0 (1–43)]. Mortality rate was 55.2 %, whereas 23 (26.4 %) patients died during hospital stay. The mean time between fascia closure and death was 140.6 (SD 241.4). Median stay at the ICU was 13 days (1–123).
In order to receive information about the optimal timepoint of delayed fascial closure, different analyses were performed. Factors hypothetically influencing the outcome (wound infection, incisional hernia) were assessed. Different variables were compared between ≤4 and >4 planned re-operations until delayed fascial closure. Further predictive data for hospital morbidity were evaluated.
Wound infection
Superficial wound infection was observed in 17.2 %. Seroma and hematoma were found in 5.7 and 2.3 % of patients, respectively. Two patients experienced deep wound infection (2.3 %), and in three (3.4 %) cases entero-atmospheric fistulas had to be treated. CRP (mg/dl) data and leukocyte number (g/μl) did not differ between beginning of abdominal vacuum therapy and the closure of the abdomen. CRP and leukocyte data did not influence wound infection.
Incisional hernia
A total of 55 patients (63.2 %) achieved fascial closure with running suture: 11 closures with Prolene® 0, 14 with PDS® 1, 3 with MaxonPlus® 1, 18 with MonoMax® 0, and 9 with MonoMax® 1. Seven patients received ACS, two patients with an additional onlay mesh. In eight patients, fascial closure was achieved with interrupted suture (9.2 %).
Technique of fascia closure and wound infection was compared in groups with and without incisional hernia. Four incisional hernias were observed in 68 patients with delayed closure (5.9 %), all with running suture after a mean follow-up of 40.5 months (16–65).
One fascial closure was achieved with MonoMax® 1, one with MaxonPlus® 1 and two with PDS® 1. No wound infection was detected in all fascial closure techniques.
≤4 and >4 planned re-operations
Overall, 63 patients had ≤4 planned re-operations and 20 had >4 planned re-operations. Incisional hernias were found in 3 of 43 patients with ≤4 re-operations (4.8 %), and 1 of 15 patients with >4 re-operations (7 %) [Table 2]. Patients with a follow-up less than 1 year were excluded. Death during hospital occurred in 12 of 63 patients with ≤4 planned reoperations (20 %), and 1 of 20 patients in >4 re-operations (5 %). Mortality in patients with ≤4 re-operations was significantly higher than in patients with >4 re-operations. Complications (abscess formation, fistulation) were found in 10 of 63 patients (15.8 %) and 6 of 20 patients (30 %). In 11 of 47 patients (23.4 %) and 4 of 16 patients (4 %) wound infection occurred (Table 2). No significant differences could be observed in all groups by contingency testing.
Hospital mortality
Mann–Whitney test showed significant higher MPI in patients who died during hospital stay. No significant differences could be shown in CRP/leukocytes.
Discussion
In the management of secondary peritonitis, treatment by NPWT techniques changed the outcome of these critically ill patients significantly [2]. In a retrospective multicenter study the advantage of the NPWT treatment revealed a reduction in mortality rate of 40 % [16]. The reduction of the bacterial contamination of the abdominal cavity and the edema of the bowel by this special treatment provides the pathophysiological background for a successful closure of the abdominal wall. Another important aspect is the morbidity of the fascial closure procedure and the incidence of incisional hernia. Several techniques have been described to achieve a delayed closure by means of mesh [8] or even by split-thickness skin grafts to the bowel [17]. Preventing retraction of the rectus muscles the NPWT treatment is sometimes insufficient by itself. Pliakos et al. [18] demonstrated a significantly better sequential closure rate by the use of additional retention sutures in a double-blinded study with and without sutures. The most successful methods [1] seem to be the approximation by means of a patch technique [9] or mediated by mesh [2, 7] or sutures [11, 18–21]. The use of an elastic suture material (e.g. vessel loops) to obtain a dynamic approximation of the fascia without the risk of high tension to the tissue and rupture seems to be consequentially better. In the technique presented in this study, preserving the fascial tissue by performing the suture stitches of these sutures at a ‘safe’ distance of the midline and leaving them in place during all of the OA period are key elements for then performing a small bite suture repair for final closure.
To reduce the high risk of incisional hernia in patients treated for secondary peritonitis with OA, which is reportedly as high as 50 % [22], the initial closure should be optimized in terms of technique.
In the beginning of our study, the small bites technique was not established in clinical routine. Based on the excellent results of the study group of Israelsson et al. [12], we adopted this technique for primary midline closure of the abdominal wall. Afterwards we extended the small bites closure technique in these NPWT patients. The risk of a burst abdomen was not increased with this technique in primary midline closure nor in delayed closure of the abdominal wall.
Based on the high evidence level IA, the primary midline closure should be performed with a late resorbable suture material [23] and, accordingly, this suture material was implemented during the observation period.
In the first prospective, randomized, multicenter trial (ISSAAC) using a new ultra-long-term absorbable, elastic monofilament suture material (MonoMax®) for the closure of primary midline laparotomy, the 1-year results showed an incisional hernia rate of 14.0 % versus 21.3 % in comparison with the control group (MonoPlus® or PDS®;) [24]. Regarding the wound infection or burst abdomen, there was no significant difference in both groups (13.1 vs. 17.8 %). Thus, because this study was performed in patients without previous treatment with NPWT, we decided to change the suture material in our study.
In case of high tension of the midline closure despite all efforts mentioned, an ACS should preferably be performed. In our study, four patients were treated in this way without any complications. In two cases, the Ramirez incisions were reinforced by an onlay mesh using a macroporous lightweight polypropylene mesh. Even in this potentially contaminated field, the synthetic mesh application caused no infection-related complications and did not result in incisional hernia. Taking into account the ongoing discussion of the indication for the use of biological meshes in this special field [25, 26], our experiences with macroporous synthetic meshes were convincing.
Our policy of early closure after NPWT treatment is based on the findings of correlation of mechanical ventilation and OA. At the time of delayed fascial closure, weaning from mechanical ventilation was started in most patients. Consequently, an early closure implies a reduction of ventilation time and stay at the ICU. Furthermore, an early-performed delayed fascial closure implies generally better conditions for preserved tissue of the abdominal wall, less lateralization of the fascia and rectus muscle, and, at the end, less risk of frozen abdomen and other severe complications such as entero-atmospheric fistula. Thus, following this policy we had two patients suffering from ‘frozen abdomen’ and three patients suffering from entero-atmospheric fistula.
In our study, the number of incisional hernias in a follow-up of at least 1 year in surviving patients detected no significantly different results in patients with ≤4 or >4 NPWT planned re-operations. In particular, the group of patients treated by component separation with and without onlay mesh reinforcement, as well as patients with a small bites closure technique by elastic suture material, exhibited no incisional hernia up to now. On the other hand, the mortality rate of our patients correlated significantly with a high MPI score. The obvious limitations of this study are its non-randomized, non-comparative design, as well as the expectedly high mortality in this specific patient population. Nevertheless, we are optimistic that the treatment regimen presented will help to further reduce planned re-operations, consecutive ICU stay, and the rate of incisional hernias. Randomized controlled studies, together with other high-volume centers, are planned.
Conclusions
In our experience, the first aim in the treatment of an OA is, beside the initial source control, to prevent lateralization of the rectus muscles by means of NPWT in combination with DFS from the very beginning. Following this strategy, an early successful delayed fascial closure by elastic, late resorbable, running suture in small bites technique, with low risk of burst abdomen and incisional hernia, can be achieved.
References
Bjorck M, Bruhin A, Cheatham M, Hinck D, Kaplan M, Manca G, Wild T, Windsor A (2009) Classification: important step to improve management of patients with an open abdomen. World J Surg 33:1154–1157
van Boele HP, Wind J, Dijkgraaf MG, Busch OR, Goslings JC (2009) Temporary closure of the open abdomen: a systematic review on delayed primary fascial closure in patients with an open abdomen. World J Surg 33:199–207
Miller PR, Meredith JW, Johnson JC, Chang MC (2004) Prospective evaluation of vacuum-assisted fascial closure after open abdomen: planned ventral hernia rate is substantially reduced. Ann Surg 239:608–614
Latifi R, Joseph B, Kulvatunyou N, Wynne JL, O’Keeffe T, Tang A, Friese R, Rhee PM (2012) Enterocutaneous fistulas and a hostile abdomen: reoperative surgical approaches. World J Surg 36:516–523
Barker DE, Green JM, Maxwell RA, Smith PW, Mejia VA, Dart BW, Cofer JB, Roe SM, Burns RP (2007) Experience with vacuum-pack temporary abdominal wound closure in 258 trauma and general and vascular surgical patients. J Am Coll Surg 204:784–792
Bjarnason T, Montgomery A, Hlebowicz J, Lindstedt S, Petersson U (2011) Pressure at the bowel surface during topical negative pressure therapy of the open abdomen: an experimental study in a porcine model. World J Surg 35:917–923
Petersson U, Acosta S, Bjorck M (2007) Vacuum-assisted wound closure and mesh-mediated fascial traction: a novel technique for late closure of the open abdomen. World J Surg 31:2133–2137
Dietz UA, Wichelmann C, Wunder C, Kauczok J, Spor L, Strauss A, Wildenauer R, Jurowich C, Germer CT (2012) Early repair of open abdomen with a tailored two-component mesh and conditioning vacuum packing: a safe alternative to the planned giant ventral hernia. Hernia 16:451–460
Keramati M, Srivastava A, Sakabu S, Rumbolo P, Smock M, Pollack J, Troop B (2008) The Wittmann Patch s a temporary abdominal closure device after decompressive celiotomy for abdominal compartment syndrome following burn. Burns 34:493–497
Koniaris LG, Hendrickson RJ, Drugas G, Abt P, Schoeniger LO (2001) Dynamic retention: a technique for closure of the complex abdomen in critically ill patients. Arch Surg 136:1359–1362
Kafka-Ritsch R, Zitt M, Schorn N, Stroemmer S, Schneeberger S, Pratschke J, Perathoner A (2012) Open abdomen treatment with dynamic sutures and topical negative pressure resulting in a high primary fascia closure rate. World J Surg 36:1765–1771
Millbourn D, Cengiz Y, Israelsson LA (2009) Effect of stitch length on wound complications after closure of midline incisions: a randomized controlled trial. Arch Surg 144:1056–1059
Millbourn D, Cengiz Y, Israelsson LA (2011) Risk factors for wound complications in midline abdominal incisions related to the size of stitches. Hernia 15:261–266
Israelsson LA, Millbourn D (2012) Closing midline abdominal incisions. Langenbecks Arch Surg 397:1201–1207
Ramirez OM, Ruas E, Dellon AL (1990) “Components separation” method for closure of abdominal-wall defects: an anatomic and clinical study. Plast Reconstr Surg 86:519–526
Wild T, Stortecky S, Stremitzer S, Lechner P, Humpel G, Glaser K, Fortelny R, Karner J, Sautner T (2006) Abdominal dressing – a new standard in therapy of the open abdomen following secondary peritonitis? [in German]. Zentralbl Chir 131(Suppl 1):S111–S114
Jernigan TW, Fabian TC, Croce MA, Moore N, Pritchard FE, Minard G, Bee TK (2003) Staged management of giant abdominal wall defects: acute and long-term results. Ann Surg 238:349–355
Pliakos I, Papavramidis TS, Mihalopoulos N, Koulouris H, Kesisoglou I, Sapalidis K, Deligiannidis N, Papavramidis S (2010) Vacuum-assisted closure in severe abdominal sepsis with or without retention sutured sequential fascial closure: a clinical trial. Surgery 148:947–953
Verdam FJ, Dolmans DE, Loos MJ, Raber MH, de Wit RJ, Charbon JA, Vroemen JP (2011) Delayed primary closure of the septic open abdomen with a dynamic closure system. World J Surg 35:2348–2355
Salman AE, Yetisir F, Aksoy M, Tokac M, Yildirim MB, Kilic M (2012) Use of dynamic wound closure system in conjunction with vacuum-assisted closure therapy in delayed closure of open abdomen. Hernia. Epub 30 Oct 2012
Brandl A, Laimer E, Perathoner A, Zitt M, Pratschke J, Kafka-Ritsch R (2013) Incisional hernia rate after open abdomen treatment with negative pressure and delayed primary fascia closure. Hernia. Epub 2 Mar 2013
Mingoli A, Puggioni A, Sgarzini G, Luciani G, Corzani F, Ciccarone F, Baldassarre E, Modini C (1999) Incidence of incisional hernia following emergency abdominal surgery. Ital J Gastroenterol Hepatol 31:449–453
Diener MK, Voss S, Jensen K, Buchler MW, Seiler CM (2010) Elective midline laparotomy closure: the INLINE systematic review and meta-analysis. Ann Surg 251:843–856
Albertsmeier M, Seiler CM, Fischer L, Baumann P, Husing J, Seidlmayer C, Franck A, Jauch KW, Knaebel HP, Buchler MW (2012) Evaluation of the safety and efficacy of MonoMax(R) suture material for abdominal wall closure after primary midline laparotomy-a controlled prospective multicentre trial: ISSAAC [NCT005725079]. Langenbecks Arch Surg 397:363–371
Regner JL, Kobayashi L, Coimbra R (2012) Surgical strategies for management of the open abdomen. World J Surg 36:497–510
Canda AE, Karaca A (2009) Incisional hernia in action: the use of vacuum-assisted closure and porcine dermal collagen implant. Hernia 13:651–655
Disclosures
The authors thank Ilse Jung for statistical analysis. None of the authors has any commercial interest in publishing this review.
Conflict of interest
Drs. R.H. Fortelny, A. Hofmann, S. Gruber Blum, A.H. Petter Puchner and K.S. Glaser have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fortelny, R.H., Hofmann, A., Gruber-Blum, S. et al. Delayed closure of open abdomen in septic patients is facilitated by combined negative pressure wound therapy and dynamic fascial suture. Surg Endosc 28, 735–740 (2014). https://doi.org/10.1007/s00464-013-3251-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3251-6