Abstract
Background
Bile duct injury in patients undergoing laparoscopic cholecystectomy is a rare but serious complication. Concomitant vascular injury worsens the outcome of bile duct injury repair. Near-infrared fluorescence imaging using indocyanine green (ICG) is a promising, innovative, and noninvasive method for the intraoperative identification of biliary and vascular anatomy during cholecystectomy. This study assessed the practical application of combined vascular and biliary fluorescence imaging in laparoscopic gallbladder surgery for early biliary tract delineation and arterial anatomy confirmation.
Methods
Patients undergoing elective laparoscopic cholecystectomy were enrolled in this prospective, single-institutional study. To delineate the major bile ducts and arteries, a dedicated laparoscope, offering both conventional and fluorescence imaging, was used. ICG (2.5 mg) was administered intravenously immediately after induction of anesthesia and in half of the patients repeated at establishment of critical view of safety for concomitant arterial imaging. During dissection of the base of the gallbladder and the cystic duct, the extrahepatic bile ducts were visualized. Intraoperative recognition of the biliary structures was registered at set time points, as well as visualization of the cystic artery after repeat ICG administration.
Results
Thirty patients were included. ICG was visible in the liver and bile ducts within 20 minutes after injection and remained up to approximately 2 h, using the ICG-filter of the laparoscope. In most cases, the common bile duct (83 %) and cystic duct (97 %) could be identified significantly earlier than with conventional camera mode. In 13 of 15 patients (87 %), confirmation of the cystic artery was obtained successfully after repeat ICG injection. No per- or postoperative complications occurred as a consequence of ICG use.
Conclusion
Biliary and vascular fluorescence imaging in laparoscopic cholecystectomy is easily applicable in clinical practice, can be helpful for earlier visualization of the biliary tree, and is useful for the confirmation of the arterial anatomy.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Bile duct injury is a rare but severe complication in patients undergoing laparoscopic cholecystectomy (0.3–0.7 %) [1–4]. Misidentification of the extrahepatic bile duct anatomy during this procedure is the main cause of such injury [5]. Concomitant vasculobiliary injury negatively affects the outcome of bile duct injury repair [6].
The critical view of safety (CVS) technique, which was first described by Strasberg et al. [7] and recommended by the SAGES Annual Meeting of 2005 [8], was introduced to reduce the risk of bile duct injury. To establish CVS, two windows need to be created during dissection of Calot’s triangle: one window between the cystic artery, cystic duct and gallbladder, another window between the cystic artery, gallbladder, and liver. The CVS technique is aimed especially at mobilizing the gallbladder neck from the liver to obtain a circumferential identification of the cystic duct.
Near-infrared fluorescence laparoscopy with preoperative intravenous injection of indocyanine green (ICG) is a promising, innovative, and noninvasive imaging method for enhanced intraoperative visualization of biliary anatomy. It has the potential to improve outcome of the laparoscopic cholecystectomy procedure [9, 10]. ICG is cleared quickly and exclusively by the liver after intravenous administration and has few, if any, side effects, making it an ideal fluorophore for this application.
Previous experience with intermittent fluorescence cholangiography during elective laparoscopic cholecystectomy showed that this technique can indeed accelerate biliary tract delineation [11]. In the present part of a larger feasibility study project on fluorescence laparoscopy technique, simultaneous fluorescence cholangiography and angiography at the moment of establishing CVS were conducted. The main objective of this study was to test the practical applicability of a newly developed laparoscopic fluorescence imaging system during elective laparoscopic cholecystectomy, regarding real-time intraoperative biliary, and arterial imaging.
Materials and methods
This study was performed at the Department of Surgery of the Maastricht University Medical Center (MUMC, Maastricht, The Netherlands) between December 2011 and October 2012. All operations were performed by a surgical resident and assisted by a surgeon with a track record of at least 150 laparoscopic cholecystectomies. The institutional review board (IRB) of the MUMC approved of this study. The study was registered in the Netherlands National Trial Register: http://www.trialregister.nl/trialreg/admin/rctview.asp?TC=3211, registration number NTR3211 (NIRFC-LC study).
Consecutive male and female patients, aged 18 years and older, scheduled for elective laparoscopic cholecystectomy and with written, informed consent, were eligible for inclusion in this study. Indications for surgery were: cholecystolithiasis, cholecystitis, cholecystectomy after biliary pancreatitis. Patients were excluded in case of liver or renal insufficiency, known iodine or ICG hypersensitivity, and pregnancy (all are contraindications for the use of intravenous ICG).
Laparoscopic fluorescence imaging system
A novel, commercially available laparoscopic fluorescence imaging system (Karl Storz GmbH & CO. KG, Tuttlingen, Germany), including a plasma light guide and 30-degree, 10-mm laparoscope applicable for white light, autofluorescence, and ICG imaging, was used for intraoperative conventional imaging (WL-mode) and near-infrared fluorescence imaging (ICG-mode). The system is equipped with a foot pedal, allowing the surgeon to easily switch from WL-mode to ICG-mode, and back. Because of the instantaneous changing of images and the stable position of the laparoscope, anatomical orientation can be maintained. However, direct fluorescence image-overlay on the conventional anatomical image is not yet possible with this system.
ICG administration
In all patients, 2.5 mg of ICG (Infracyanine®; SERB, France) was injected intravenously directly after induction of anesthesia to obtain intraoperative near-infrared fluorescence illumination of the extrahepatic bile ducts. Half of the patients received a repeat intravenous injection of 2.5 mg of ICG at establishment of the CVS for concomitant arterial and biliary fluorescence delineation.
Fluorescence laparoscopy
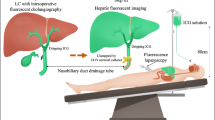
The operation was performed according to the Dutch Guidelines and best practice for laparoscopic cholecystectomy [12], which is based on the CVS technique. Initial fluorescence cholangiography was conducted at the first view of the liver hilum. Subsequently, fluorescence imaging was applied every 5–10 min until CVS was established by the surgeon. At establishment of CVS, simultaneous fluorescence angiography was obtained from 10 s up to ~1 min after repeat intravenous ICG injection. See Fig. 1 for a flowchart of the study procedure.
Data collection
Intraoperatively a researcher systematically registered on a paper form whether the localization of the common bile duct, cystic duct, and cystic artery could be identified at set time points, comparing the WL-camera mode to ICG-mode. For agreement on the identification of the aforementioned structures, the attending surgeon was consulted. A structure was scored as “identified” if its localization was confirmed with great certainty by the experienced surgeon. In case of the common bile duct, this does explicitly not mean that it was surgically exposed, as this is contradictory to the CVS technique.
During all laparoscopic cholecystectomies, the full surgical procedure was recorded on DVD, thereby collecting both conventional and fluorescence images. After completion of surgery, length of time between the introduction of the laparoscope until the first recognition of the following components were calculated based on the intraoperative registration: common bile duct (CBD), cystic duct (CD), cystic artery (CA), and CVS.
Using conventional imaging, the CBD is regularly not displayed; this is partly a result of the CVS technique. The mean “total fluorescence imaging time” during the laparoscopic procedures was calculated based on the video recordings to objectify how much longer the operation lasted due to application of the fluorescence technique.
Quantitative fluorescence image analysis
For objective assessment of the degree of fluorescence illumination in the extrahepatic bile ducts and artery, OsiriX 5.5.1 Imaging Software was used. The fluorescence images were analyzed by determining target-to-background ratio (TBR). TBR was defined as the mean fluorescence intensity (FI) of two point regions of interest (ROIs) in the target (i.e., CBD, CD, or CA) minus the mean FI of two background (BG) ROIs in the liver hilum, divided by the mean FI of the two BG ROIs in the liver hilum; in formula: TBR = (FI of target − FI of BG)/FI of BG.
Statistical analysis
Primary endpoint consisted of moment of clear visualization of the extrahepatic bile duct anatomy. Secondary endpoint was confirmation of the course of the CA at establishment of CVS. Regarding the primary endpoint, a paired t test was applied for determination of possible significant differences between the time measurements from “introduction of laparoscope” until “identification of CD/CBD”—comparing fluorescence imaging with conventional imaging.
Results
Thirty patients, undergoing an elective laparoscopic cholecystectomy, were included in this study. Before start of surgery no signs of biliary tract obstruction were present. Patient characteristics are shown in Table 1.
Fluorescence laparoscopy
The median time interval from preoperative ICG administration until first fluorescence imaging with the laparoscope was 34 (range 19–67) min. The time until first fluorescence imaging depended mainly on whether an adhesiolysis had to be conducted before initial exposure of the liver hilum could be obtained. After start of surgery, the CBD could be identified significantly earlier using fluorescence imaging compared with WL imaging (median 23 and 33 min respectively; P < 0.001). Using fluorescence laparoscopy, the CD was delineated after an average of 25 min, whereas using WL camera mode this took on average of 36 minutes (P < 0.001; see also Table 2 for intraoperative registration).
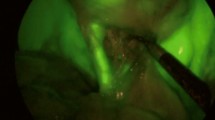
Using fluorescence cholangiography, the CBD and the CD could be clearly visualized and delineated before dissection of Calot’s triangle (Fig. 2A), respectively in 25 of 30 patients (83 %) and 29 of 30 patients (97 %). In four of five cases (17 %), in which the CBD could not be visualized using fluorescence imaging, a chronic inflammation of the gallbladder was present. One patient appeared to have a chronic, focally active cholecystitis. Body mass index (BMI) of these patients ranged from 26.35 to 31.14 kg/m2. However, in the 25 patients in whom the CBD could be delineated before dissection, there also were cases of chronic inflamed gallbladders and BMIs within the same range as these five patients.
A WL image (left) and corresponding fluorescence image (right) taken at initial exposure of the liver hilum. The liver and extrahepatic bile ducts are illuminated bright blue: cystic duct (continuous arrow) and common bile duct (interrupted arrow) are indicated. B WL image (left) and corresponding fluorescence image (right) at establishment of critical view of safety, snap-shots taken 10 s after repeat ICG injection. The cystic duct (continuous arrow) and cystic artery (interrupted arrow) are clearly exposed
Conventional laparoscopy provided certainty on the course of the CBD and the CD in respectively 22 of 30 patients and 29 of 30 patients. In one patient, conversion to open cholecystectomy followed, due to insufficient sight on the liver hilum after an early perforation of a very thin-walled gallbladder, causing persistent nuisance bile leakage.
CVS was obtained in a median of 45 min after incision. Concomitant fluorescence angiography of the CA (Fig. 2B) was successful in 13 of 15 patients (87 %). In two patients, the CA was already ligated in an earlier stage of dissection.
In the total operation time (median 90 min), 1–2 min was spent for the intraoperative use of the fluorescence technique.
As a preventive measure, in 3 of 30 patients the gallbladder was punctured and drained during surgery to facilitate manipulation; this did neither compromise fluorescence imaging of the biliary tract nor the postoperative course.
Target-to-background ratio
Mean TBR at establishment of CVS (median 63 minutes after ICG administration) amounted to 5.6 for the CD, 6.8 for the CBD, and 4.8 for the CA.
Complications
No per- or postoperative complications regarding the extrahepatic bile ducts occurred. There was one conversion from laparoscopic to open cholecystectomy. None of the patients developed any adverse reactions to the injected ICG.
Discussion
This prospective, single-institutional, clinical study showed that the near-infrared fluorescence imaging technique was useful for earlier bile duct delineation during laparoscopic cholecystectomy. Next, it was found that repeat ICG injection at establishment of CVS was helpful in the confirmation of arterial anatomy, in particular the course of the CA. The fluorescence technique provided a significantly earlier identification and a clear delineation (high TBR) of the CBD, the CD, and the CA, therewith assisting in safe and efficient dissection of the gallbladder according to the CVS technique.
The near-infrared fluorescence technique after local or intravenous administration of ICG has been evaluated in open, laparoscopic, single-incision laparoscopic and robotic single-site cholecystectomy [13–18]. Promising results were presented for successful intraoperative identification of the CBD and the CD compared with conventional laparoscopic imaging. The results of the present study showed moreover that fluorescence laparoscopy provided significantly earlier identification of the extrahepatic bile ducts during dissection.
Real-time simultaneous imaging of the bile ducts and the arterial anatomy (i.e., hepatic and cystic arteries) also can be obtained [13, 19–21]. This study confirmed the possibility of concomitant vascular (i.e., CA) and biliary (i.e., CD and CBD) imaging at establishment of CVS. Implementation of conducting both fluorescence cholangiography and angiography can be helpful in cases in which the establishment of CVS is challenging. Furthermore, it may facilitate the intraoperative detection of bile duct and possible concomitant vasculobiliary injury (e.g., hepatic artery). The latter is an increasingly recognized complication of laparoscopic cholecystectomy [22]. Such combined injury negatively affects the outcome of bile duct injury repair [6, 23]. Based on a review of vasculobiliary injury in laparoscopic and open cholecystectomy, routine arteriography in patients with biliary injury has been recommended [24].
The negligible extension of operation duration in this study, related to the use of the fluorescence technique, will probably further decrease with growing experience. Looking at the results of the quantitative fluorescence image analysis, the moment of ICG administration (directly after induction of anesthesia) seems appropriate for the laparoscopic cholecystectomy procedure: a timely and continuous intraoperative detection of biliary structures can be obtained. Also from a practical and logistical point of view, the applied timing of administration is appropriate.
In this study not only uncomplicated cholecystolithiasis patients, but also more complicated cases, such as cholecystitis or cholecystectomy after biliary pancreatitis, were included. Fluorescence cholangiography and angiography was successful in almost all cases, and no difference was found in image quality between the uncomplicated and complicated procedures. However, presence of factors, such as (either chronic or active) cholecystitis or obesity, might compromise the efficacy of the new imaging modality. The actual impact of such conditions should be further investigated by conducting a univariate and multivariate analysis in a study population (large enough for this kind of analysis) to determine the risk factors. This was not possible in the current group of patients.
The near-infrared fluorescence laparoscopy technique possesses potential to enter the clinical practice in the near future. However, optimization of the current laparoscopic imaging systems is needed to make them more easily applicable in the operating room. Current laparoscopic systems do not yet possess the ability to display the fluorescence image in anatomical context. Furthermore, penetration depth at which the imaging system can detect a fluorophore in tissues needs improvement (currently up to maximum of 1 cm). An increase in fluorescence capabilities of contrast agents also is desirable [25].
A comparison with conventional intraoperative cholangiography would be desirable. However, intraoperative cholangiography is only rarely applied in the Netherlands and many parts of the world. Intraoperative cholangiography has been suggested to reduce the risk of bile duct injury [1, 10]. However, this radiological imaging of the biliary tree is only used selectively, as the process takes time, radiation exposure is involved, and additional equipment and manpower for the procedure are required. Moreover, worldwide consensus about implementation of intraoperative cholangiography is still lacking [26].
It could be argued that the fluorescence laparoscopy technique is especially useful for the less experienced surgeon to perform safe laparoscopic gallbladder removal or in more complicated cholecystectomies. However, it may be most effective when performed routinely in all cases. Increased costs are involved in terms of the light source, camera, and fluorescent dye. However, it is anticipated that worldwide, standard application of this technique will be accompanied by cheaper devices and shorter operation duration, when proven that CVS actually can be obtained significantly earlier compared with conventional laparoscopic imaging.
Fluorescence laparoscopy also could be implemented as a final check of the liver hilum before closing the pneumoperitoneum to rule out or to detect bile duct or vasculobiliary injury. This could be checked through the presence or absence of fluorescence contrast leakage into the abdomen.
Conclusions
Both biliary and vascular fluorescence imaging in laparoscopic cholecystectomy are easily applicable, can be helpful for earlier identification of the extrahepatic bile ducts, and are useful for the confirmation of the arterial anatomy.
Abbreviations
- ICG:
-
Indocyanine green
- CVS:
-
Critical view of safety
References
Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T (2003) Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. JAMA 289:1639–1644
Fletcher DR, Hobbs MS, Tan P, Valinsky LJ, Hockey RL, Pikora TJ, Knuiman MW, Sheiner HJ, Edis A (1999) Complications of cholecystectomy: risks of the laparoscopic approach and protective effects of operative cholangiography: a population-based study. Ann Surg 229:449–457
Nuzzo G, Giuliante F, Giovannini I, Ardito F, D’Acapito F, Vellone M, Murazio M, Capelli G (2005) Bile duct injury during laparoscopic cholecystectomy: results of an Italian national survey on 56 591 cholecystectomies. Arch Surg 140:986–992
Waage A, Nilsson M (2006) Iatrogenic bile duct injury: a population-based study of 152 776 cholecystectomies in the Swedish Inpatient Registry. Arch Surg 141:1207–1213
Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K, Hunter JG (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237:460–469
Sarno G, Al-Sarira AA, Ghaneh P, Fenwick SW, Malik HZ, Poston GJ (2012) Cholecystectomy-related bile duct and vasculobiliary injuries. Br J Surg 99:1129–1136
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180:101–125
Kuwada T (2005) Highlights of the society of American gastrointestinal and endoscopic surgeons 2005, Annual Meeting April 13–16, 2005; Ft Lauderdale, Florida. Medscape General Surgery: Conference reports. http://wwwmedscapecom/viewarticle/506432. Accessed 14 Feb 2013
Agarwal BB (2009) Patient safety in laparoscopic cholecystectomy. Arch Surg 144:979
Buddingh KT, Nieuwenhuijs VB, van Buuren L, Hulscher JB, de Jong JS, van Dam GM (2011) Intraoperative assessment of biliary anatomy for prevention of bile duct injury: a review of current and future patient safety interventions. Surg Endosc 25:2449–2461
Schols RM, Bouvy ND, Masclee AA, van Dam RM, Dejong CH, Stassen LP (2012) Fluorescence cholangiography during laparoscopic cholecystectomy: a feasibility study on early biliary tract delineation. Surg Endosc 27(5):1530–1536
Lange JF, Stassen LPS (2006) Best practice in verband met de techniek van laparoscopische cholecystectomie (critical view of safety [CVS] in 7 stappen). Werkgroep Endoscopische Chirurgie van de Nederlandse vereniging voor Heelkunde. http://wwwheelkundenl/uploads/_6/re/_6reZZkgrYUAuCG6uvcN-A/richtlijn_galsteenpdf. Accessed 14 Feb 2013
Tagaya N, Shimoda M, Kato M, Nakagawa A, Abe A, Iwasaki Y, Oishi H, Shirotani N, Kubota K (2010) Intraoperative exploration of biliary anatomy using fluorescence imaging of indocyanine green in experimental and clinical cholecystectomies. J Hepatobiliary Pancreat Sci 17:595–600
Ishizawa T, Bandai Y, Ijichi M, Kaneko J, Hasegawa K, Kokudo N (2010) Fluorescent cholangiography illuminating the biliary tree during laparoscopic cholecystectomy. Br J Surg 97:1369–1377
Ishizawa T, Kaneko J, Inoue Y, Takemura N, Seyama Y, Aoki T, Beck Y, Sugawara Y, Hasegawa K, Harada N, Ijichi M, Kusaka K, Shibasaki M, Bandai Y, Kokudo N (2011) Application of fluorescent cholangiography to single-incision laparoscopic cholecystectomy. Surg Endosc 25:2631–2636
Aoki T, Murakami M, Yasuda D, Shimizu Y, Kusano T, Matsuda K, Niiya T, Kato H, Murai N, Otsuka K, Kusano M, Kato T (2010) Intraoperative fluorescent imaging using indocyanine green for liver mapping and cholangiography. J Hepatobiliary Pancreat Sci 17:590–594
Spinoglio G, Priora F, Bianchi PP, Lucido FS, Licciardello A, Maglione V, Grosso F, Quarati R, Ravazzoni F, Lenti LM (2013) Real-time near-infrared (NIR) fluorescent cholangiography in single-site robotic cholecystectomy (SSRC): a single-institutional prospective study. Surg Endosc 27(6):2156–2162
Buchs NC, Hagen ME, Pugin F, Volonte F, Bucher P, Schiffer E, Morel P (2012) Intra-operative fluorescent cholangiography using indocyanine green during robotic single site cholecystectomy. Int J Med Robot 8:436–440
Ashitate Y, Stockdale A, Choi HS, Laurence RG, Frangioni JV (2012) Real-time simultaneous near-infrared fluorescence imaging of bile duct and arterial anatomy. J Surg Res 176(1):7–13
Mitsuhashi N, Kimura F, Shimizu H, Imamaki M, Yoshidome H, Ohtsuka M, Kato A, Yoshitomi H, Nozawa S, Furukawa K, Takeuchi D, Takayashiki T, Suda K, Igarashi T, Miyazaki M (2008) Usefulness of intraoperative fluorescence imaging to evaluate local anatomy in hepatobiliary surgery. J Hepatobiliary Pancreat Surg 15:508–514
Kaneko J, Ishizawa T, Masuda K, Kawaguchi Y, Aoki T, Sakamoto Y, Hasegawa K, Sugawara Y, Kokudo N (2012) Indocyanine green reinjection technique for use in fluorescent angiography concomitant with cholangiography during laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 22:341–344
Pulitano C, Parks RW, Ireland H, Wigmore SJ, Garden OJ (2011) Impact of concomitant arterial injury on the outcome of laparoscopic bile duct injury. Am J Surg 201:238–244
Schmidt SC, Langrehr JM, Raakow R, Klupp J, Steinmuller T, Neuhaus P (2002) Right hepatic lobectomy for recurrent cholangitis after combined bile duct and right hepatic artery injury during laparoscopic cholecystectomy: a report of two cases. Langenbecks Arch Surg 387:183–187
Strasberg SM, Helton WS (2011) An analytical review of vasculobiliary injury in laparoscopic and open cholecystectomy. HPB (Oxford) 13:1–14
Schols RM, Bouvy ND, van Dam RM, Stassen LP (2013) Advanced intraoperative imaging methods for laparoscopic anatomy navigation: an overview. Surg Endosc 27(6):1851–1859
Ford JA, Soop M, Du J, Loveday BP, Rodgers M (2012) Systematic review of intraoperative cholangiography in cholecystectomy. Br J Surg 99:160–167
Acknowledgments
The authors thank Karl Storz GmbH & Co. KG (Tuttlingen, Germany) for providing the laparoscopic fluorescence imaging system and for technical assistance during the study. Furthermore, they acknowledge the surgeons and resident surgeons who performed the laparoscopic cholecystectomies in this study, and the patients who gave consent to participate in the study.
Disclosures
R.M. Schols, N.D. Bouvy, R.M. van Dam, A.A.M. Masclee, C.H.C. Dejong, and L.P.S. Stassen have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schols, R.M., Bouvy, N.D., van Dam, R.M. et al. Combined vascular and biliary fluorescence imaging in laparoscopic cholecystectomy. Surg Endosc 27, 4511–4517 (2013). https://doi.org/10.1007/s00464-013-3100-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-013-3100-7