Abstract
Background
Transanal endoscopic video-assisted (TEVA) excision represents an alternative approach for the surgical treatment of middle and upper rectal lesions not amenable to colonoscopic removal. Utilizing principles of single-incision laparoscopic surgery, this novel minimally invasive approach optimizes access for safe and complete removal of these lesions without the need for a formal rectal resection. We describe our technique and early outcomes with TEVA excision.
Methods
Between March 2010 and September 2011, TEVA excision was performed for patients presenting for management of rectal lesions not amenable to colonoscopic or standard transanal removal. Patients were selected if they presented with benign disease or superficial adenocarcinoma, and the proximal extent of the lesion extended beyond 8 cm from the anal verge. Demographic, intraoperative, and postoperative data were assessed. A SILS™ port was placed in the anal canal for access in all cases. Standard laparoscopic instruments were utilized for visualization, full-thickness transanal excision, and primary closure.
Results
Twenty patients (50 % male) with a mean age of 64.6 ± 10.9 years, mean body mass index of 28.2 ± 4.9 kg/m2, and median American Society of Anesthesiologist score of 2 underwent TEVA excision. Fourteen patients (70 %) presented with benign disease and six patients (30 %) presented with malignant disease. The mean size of the lesions was 3.0 ± 1.4 cm, and the mean distance from the anal verge was 10.6 ± 2.4 cm. All excisions were successfully completed with a mean operative time of 79.8 ± 25.1 (range, 45–135) min. The mean length of hospital stay was 1.1 ± 0.7 (range, 0-3) days.
Conclusions
TEVA excision is a safe and feasible approach for local excision of rectal lesions not otherwise amenable to standard techniques. Continued investigation and development will be important to establish its role in minimally invasive colorectal surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Although the majority of rectal polyps can be removed safely by using an array of polypectomy techniques during colonoscopy [1, 2], various factors, such as the size, location, and pathology of the lesion, may necessitate consideration of a surgical approach for definitive treatment [3–5]. Traditional transanal excision (TAE) is an important alternative for local removal of many of these lesions, because it avoids radical abdominal resection and is associated with low morbidity and mortality, expeditious recovery, and improved functional results [7, 8]. However, TAE is limited to lesions confined within 5–8 cm of the anal verge [6], primarily because those lesions of the middle or upper rectum cannot be readily accessed [9].
Traditionally, the majority of patients with middle or upper rectal lesions have required some form of radical abdominal surgery, such as low anterior resection (LAR) or abdominoperineal resection (APR), for early stage malignant disease (Tis and T1) and even large benign lesions [10–12]. These approaches are associated with significant morbidity, including anastomotic leak, pelvic sepsis, stenosis, and sexual or urinary dysfunction [13–17]. Furthermore, permanent colostomy may be necessary in up to 30 % of cases [18], even with the development of minimally invasive approaches and sphincter-preserving procedures.
More recently, the application of a single-incision laparoscopic access device for transanal excision has been assessed [19–26]. Labeled transanal endoscopic video-assisted (TEVA) excision by our group [27], this innovative approach facilitates surgical excision of middle and upper rectal lesions not amenable to standard transanal or colonoscopic removal. Combining the merits and technical skills of single-incision laparoscopic colectomy (SILC) [28–31] with the principles of TAE, TEVA excision optimizes access for safe and complete removal of these lesions without the need for a formal rectal resection. We describe our technique for TEVA excision and present our early outcomes with this novel minimally invasive surgical approach.
Materials and methods
Between March 2010 and September 2011, TEVA excision was performed for patients presenting for management of rectal lesions not amenable to colonoscopic or standard transanal removal. Patients were eligible for TEVA if (1) the proximal extent of the lesion extended beyond 8 cm from the anal verge, and (2) had benign disease, carcinoid, or early-stage adenocarcinomas (ultrasound stage: uTis or uT1N0). All procedures were performed by one of two board-certified colorectal surgeons (TBP and EMH). Demographic information, intraoperative parameters, and postoperative outcomes were assessed.
Surgical technique
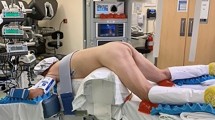
Our technique for TEVA excision has been described previously [27]. General endotracheal anesthesia is utilized to secure the airway and to facilitate the use of paralytics, which limits the loss of pneumorectum that tends to occur with changes in intra-abdominal pressure. The patient is always placed in supine position with legs elevated in candy-cane stirrups (independent of the location of the lesion). A SILS™ port (Covidien, Mansfield, MA) is inserted into the anal canal for access. A surgical clamp or sponge stick may be used to assist with port insertion (Fig. 1), and lateral fixation sutures may be placed to secure the port (Fig. 2).
The SILS™ port contains three cannulae for introduction of instrumentation into the lumen and a supplementary cannula that facilitates carbon dioxide (CO2) gas insufflation (Fig. 3). A maximum pressure of 15–18 mm Hg is used to maintain pneumorectum. Standard laparoscopic instrumentation, which includes an atraumatic bowel grasper, a hook Bovie electrocautery, and a 5-mm 30° camera, is utilized for all cases (Fig. 4). A right-angle light cord adaptor (KARL STORZ Endoscopy, El Segundo, CA) is essential to minimize external clashing between the instruments (Fig. 5).
The lesion is identified and the mucosa is scored by using the hook Bovie cautery in a circumferential fashion 1 cm from its edges to ensure gross-negative margins (Fig. 6). Attention is initially drawn to the proximal extent of the lesion, and a full-thickness excision is performed (Fig. 7). Systematic dissection continues in a tangential plane through the layers of the rectal tissue (confirmed with identification of the mesorectum). Once completely excised, the specimen is extracted transanally and hemostasis is achieved (Fig. 8).
Full-thickness excision. A Margins of excision outlined using score marks. B–D Systematic dissection in tangential plane through layers of rectal wall. Smoke accumulation may be eliminated with pulse suctioning. E Important to achieve full-thickness excision into perirectal adipose tissue. F Specimen extracted
The final stages of the procedure involve full-thickness primary closure of the rectal wall defect with interrupted 2.0 Vicryl sutures (Figs. 9, 10). Recently, we have adapted to using a V-Loc™ Absorbable Wound Closure Device (Covidien) for primary closure, which averts the need for intraluminal knot tying.
Results
Twenty patients (50 % male) with a mean age of 64.6 ± 10.9 (range, 40-86) years, mean body mass index of 28.2 ± 4.9 (range, 20.2–39) kg/m2, and median American Society of Anesthesiologist score of 2 (range, 1–3) underwent TEVA excision (Table 1). All patients had undergone previous colonoscopy with failed or incomplete polypectomy. All but six patients had a prior surgical history, including one patient who had undergone a previous transanal excision. Fourteen patients (70 %) presented with benign disease (adenoma), and six patients (30 %) presented with malignant disease (carcinoid or adenocarcinoma). The mean size of the lesions was 3.0 ± 1.4 (range, 1.3–5.5) cm, and the mean distance from the anal verge was 10.6 ± 2.4 (range, 6–15) cm.
All TEVA excisions were completed successfully, and there were no intraoperative complications. The mean operative time and length of hospital stay were 79.8 ± 25.1 (range, 45–135) min and 1.1 ± 0.7 (range, 0–3) days, respectively. A single postoperative complication occurred, which consisted of a patient who presented with vaginal drainage that spontaneously resolved. Repeat interval TEVA excision was required for two patients (10 %): one with inadequate surgical margins (within 1 mm) in a malignant lesion and another with recurrent villous adenoma 7 months after the index procedure. One patient underwent a formal oncologic LAR after TEVA excision revealed a T2 lesion on final pathology (preoperative stage: T1N0).
Discussion
Transanal endoscopic video-assisted excision is a safe and feasible approach for the treatment of benign polyps and early-stage rectal carcinoma. Merging the technical skill set of SILC with the principles of TAE optimizes access and visualization for safe and complete removal of these lesions when beyond the limits of TAE. Furthermore, the approach averts the need for a formal oncologic resection and the possible negative outcomes associated with a low colorectal anastomosis or definitive colostomy. Although early in our experience, the modality also has proven to be a viable option for excision of middle and upper rectal lesions.
Several case reports [20, 21, 25] and small case series [19, 22–24, 26] have been published describing similar experience utilizing the SILS™ port or other single-incision devices for transanal access and local excision. The first series reported by Atallah et al. [24] demonstrated excellent overall results for six patients. There were no conversions, morbidities or mortalities. Currently, the largest series published by van den Boezem et al. [26] includes 12 patients from the Netherlands. Ten cases were successfully completed using the SILS™ port. However, an open transanal approach was necessary for the remaining two cases, because there was insufficient distance between the port and target polyp in each case. Our operative time, length of stay, and complication rate is comparable to the current literature.
Since initially describing our technique [27], we have incorporated several modifications to enhance the procedure. For instance, the trocars are placed and positioned in a staggered fashion (Fig. 3B) to reduce potential instrument clashing. We also have utilized an extra-long camera as a method for limiting external collisions between the surgeon and assistant. A right-angle light cord adaptor (Fig. 5) is routinely used as well to limit external conflict. Even though intraluminal knot tying can be readily achieved by most experienced surgeon, the narrow confines of the rectal lumen can still be challenging. We have recently begun to use a V-Loc™ Absorbable Wound Closure Device for primary closure. This affords approximation with a running suture technique, obviating the need for intraluminal knot tying and reducing overall operative times.
Another alternative approach to avoid radical resection, transanal endoscopic microsurgery (TEM), was first introduced in the mid 1980s and has become a viable option for the management of lesions not suitable for TAE [32–34]. Studies have demonstrated TEM to be safe, feasible, and efficacious for the management of low-risk lesions, specifically large benign adenomas and early-stage carcinomas (T1 or T2 tumors) [35–37]. The technique provides enhanced visualization and precise excision, resulting in low morbidity and mortality rates for lesions located up to 25 cm from the anal verge [38, 39]. Nonetheless, TEM is not without its own inherent limitations. The high cost of instrumentation and extended learning curve for TEM has restricted its availability and curbed wider adaptation [40–43].
The cost of TEM is significant when taking into account the proctoscope and insufflation system [44], the optical and operative instrumentation, and the maintenance of the plugs and caps that help seal the closed system. Furthermore, the cost of training must be factored into the overall cost of the procedure. Compared with TEM, TEVA excision utilizes readily available surgical instrumentation, requires minimal set-up, and translates well to experienced laparoscopic surgeons. Furthermore, in the absence of a commercially available single-incision port, use of a “glove port,” such as previously used for SILC [45–47], may be considered for TEVA excision [48].
Transanal endoscopic video-assisted excision is a safe and feasible approach for local excision of benign and superficial malignant rectal lesions. The approach facilitates exposure and access to pathologies of the middle and upper rectum and averts the need for formal rectal resection. Continued investigation and development of this novel and innovative modality will be important to establish its role in minimally invasive colorectal surgery.
References
Waye JD (2000) Colonoscopic polypectomy. Diagn Ther Endosc 6:111–124
Cruz RA, Ragupathi M, Pedraza R, Pickron TB, Le AT, Haas EM (2011) Minimally invasive approaches for the management of “difficult” colonic polyps. Diagn Ther Endosc. doi:10.1155/2011/682793Jun28
Consolo P, Luigiano C, Strangio G, Scaffidi MG, Giacobbe G, Di Giuseppe G, Zirilli A, Familiari L (2008) Efficacy, risk factors and complications of endoscopic polypectomy: ten year experience at a single center. World J Gastroenterol 14:2364–2369
Pokala N, Delaney CP, Kiran RP, Brady K, Senagore AJ (2007) Outcome of laparoscopic colectomy for polyps not suitable for endoscopic resection. Surg Endosc 21:400–403
Caputi Iambrenghi O, Ugenti I, Martines G, Marino F, Francesco Altomare D, Memeo V (2009) Endoscopic management of large colorectal polyps. Int J Colorectal Dis 24:749–753
Casadesus D (2009) Surgical resection of rectal adenoma: a rapid review. World J Gastroenterol 15:3851–3854
Zorcolo L, Fantola G, Cabras F, Marongiu L, D’Alia G, Casula G (2009) Preoperative staging of patients with rectal tumors suitable for transanal endoscopic microsurgery (TEM): comparison of endorectal ultrasound and histopathologic findings. Surg Endosc 23:1384–1389
Ptok H, Marusch F, Meyer F, Schubert D, Koeckerling F, Gastinger I, Lippert H, Colon/Rectal Cancer (Primary Tumor) Study Group (2007) Oncological outcome of local vs radical resection of low-risk pT1 rectal cancer. Arch Surg 142:649–656
Palma P, Freudenberg S, Samel S, Post S (2004) Transanal endoscopic microsurgery: indications and results after 100 cases. Colorectal Dis 6:350–355
MacFarlane JK, Ryall RD, Heald RJ (1993) Mesorectal excision for rectal cancer. Lancet 341:457–460
Aitken RJ (1996) Mesorectal excision for rectal cancer. Br J Surg 83:214–216
Enker WE, Havenga K, Polyak T, Thaler H, Cranor M (1997) Abdominoperineal resection via total mesorectal excision and autonomic nerve preservation for low rectal cancer. World J Surg 21:715–720
Longo WE, Virgo KS, Johnson FE, Wade TP, Vernava AM, Phelan MA, Henderson WG, Daley J, Khuri SF (1998) Outcome after proctectomy for rectal cancer in Department of Veterans Affairs Hospitals: a report from the National Surgical Quality Improvement Program. Ann Surg 228:64–70
Kasparek MS, Hassan I, Cima RR, Larson DR, Gullerud RE, Wolff BG (2012) Long-term quality of life and sexual and urinary function after abdominoperineal resection for distal rectal cancer. Dis Colon Rectum 55:147–154
Breukink SO, van der Zaag-Loonen HJ, Bouma EM, Pierie JP, Hoff C, Wiggers T, Meijerink WJ (2007) Prospective evaluation of quality of life and sexual functioning after laparoscopic total mesorectal excision. Dis Colon Rectum 50:147–155
Kumar A, Daga R, Vijayaragavan P, Prakash A, Singh RK, Behari A, Kapoor VK, Saxena R (2011) Anterior resection for rectal carcinoma: risk factors for anastomotic leaks and strictures. World J Gastroenterol 17:1475–1479
Lyall A, Mc Adam TK, Townend J, Loudon MA (2007) Factors affecting anastomotic complications following anterior resection in rectal cancer. Colorectal Dis 9:801–807
Morris E, Quirke P, Thomas JD, Fairley L, Cottier B, Forman D (2008) Unacceptable variation in abdominoperineal excision rates for rectal cancer: time to intervene? Gut 57:1690–1697
Michalik M, Bobowicz M, Orlowski M (2011) Transanal endoscopic microsurgery via TriPort Access System with no general anesthesia and without sphincter damage. Surg Laparosc Endosc Percutan Tech 21:e308–e310
Khoo RE (2010) Transanal excision of a rectal adenoma using single-access laparoscopic port. Dis Colon Rectum 53:1078–1079
Dardamanis D, Theodorou D, Theodoropoulos G, Larentzakis A, Natoudi M, Doulami G, Zoumpouli C, Markogiannakis H, Katsaragakis S, Zografos GC (2011) Transanal polypectomy using single incision laparoscopic instruments. World J Gastrointest Surg 3:56–58
Matz J, Matz A (2012) Use of a SILS port in transanal endoscopic microsurgery in the setting of a community hospital. J Laparoendosc Adv Surg Technol A 22:93–96
Lorenz C, Nimmesgern T, Back M, Langwieler TE (2010) Transanal single port microsurgery (TSPM) as a modified technique of transanal endoscopic microsurgery (TEM). Surg Innov 17:160–163
Atallah S, Albert M, Larach S (2010) Transanal minimally invasive surgery: a giant leap forward. Surg Endosc 24:2200–2205
Watts ES, Peacock O, Gupta A, Speake WJ, Lund JN (2012) Anyone for TAMIS? Tech Coloproctol. doi:10.1007/s10151-012-0806-9Feb18
van den Boezem PB, Kruyt PM, Stommel MW, Tobon Morales R, Cuesta MA, Sietses C (2011) Transanal single-port surgery for the resection of large polyps. Dig Surg 28:412–416
Ragupathi M, Haas EM (2011) Transanal endoscopic video-assisted excision: application of single-port access. JSLS 15:53–58
Ramos-Valadez DI, Patel CB, Ragupathi M, Bartley Pickron T, Haas EM (2010) Single-incision laparoscopic right hemicolectomy: safety and feasibility in a series of consecutive cases. Surg Endosc 24:2613–2616
Patel CB, Ramos-Valadez DI, Ragupathi M, Haas EM (2010) Single incision laparoscopic-assisted right hemicolectomy: technique and application (with video). Surg Laparosc Endosc Percutan Tech 20:e146–e149
Ragupathi M, Ramos-Valadez DI, Yaakovian MD, Haas EM (2011) Single-incision laparoscopic colectomy: a novel approach through a Pfannenstiel incision. Tech Coloproctol 15:61–65
Ramos-Valadez DI, Patel CB, Ragupathi M, Bokhari MB, Pickron TB, Haas EM (2011) Single-incision laparoscopic colectomy: outcomes of an emerging minimally invasive technique. Int J Colorectal Dis 26:761–767
Buess G, Theiss R, Günther M, Hutterer F, Pichlmaier H (1985) Endoscopic surgery in the rectum. Endoscopy 17:31–35
Buess G, Kipfmüller K, Naruhn M, Braunstein S, Junginger T (1987) Endoscopic microsurgery of rectal tumors. Endoscopy 19:38–42
Allaix ME, Arezzo A, Caldart M, Festa F, Morino M (2009) Transanal endoscopic microsurgery for rectal neoplasms: experience of 300 consecutive cases. Dis Colon Rectum 52:1831–1836
de Graaf EJ, Doornebosch PG, Tetteroo GW, Geldof H, Hop WC (2009) Transanal endoscopic microsurgery is feasible for adenomas throughout the entire rectum: a prospective study. Dis Colon Rectum 52:1107–1113
Christoforidis D, Cho HM, Dixon MR, Mellgren AF, Madoff RD, Finne CO (2009) Transanal endoscopic microsurgery versus conventional transanal excision for patients with early rectal cancer. Ann Surg 249:776–782
de Graaf EJ, Doornebosch PG, Tollenaar RA, Meershoek-Klein Kranenbarg E, de Boer AC, Bekkering FC, van de Velde CJ (2009) Transanal endoscopic microsurgery versus total mesorectal excision of T1 rectal adenocarcinomas with curative intention. Eur J Surg Oncol 35:1280–1285
Guerrieri M, Baldarelli M, de Sanctis A, Campagnacci R, Rimini M, Lezoche E (2010) Treatment of rectal adenomas by transanal endoscopic microsurgery: 15 years’ experience. Surg Endosc 24:445–449
Floyd ND, Saclarides TJ (2006) Transanal endoscopic microsurgical resection of pT1 rectal tumors. Dis Colon Rectum 49(2):164–168
Platell C, Denholm E, Makin G (2004) Efficacy of transanal endoscopic microsurgery in the management of rectal polyps. J Gastroenterol Hepatol 19:767–772
Maslekar S, Pillinger SH, Sharma A, Taylor A, Monson JR (2007) Cost analysis of transanal endoscopic microsurgery for rectal tumours. Colorectal Dis 9:229–234
Cataldo PA (2006) Transanal endoscopic microsurgery. Surg Clin North Am 86:915–925
Koebrugge B, Bosscha K, Ernst MF (2009) Transanal endoscopic microsurgery for local excision of rectal lesions: is there a learning curve? Dig Surg 26:372–377
Denk PM, Swanström LL, Whiteford MH (2008) Transanal endoscopic microsurgical platform for natural orifice surgery. Gastrointest Endosc 68:954–959
Baig MN, Moftah M, Deasy J, McNamara D, Cahill RA (2012) Implementation and usefulness of single access laparoscopic segmental and total colectomy. Colorectal Dis. doi:10.1111/j.1463-1318.2012.02966.xFeb6
Ishida H, Okada N, Ishibashi K, Ohsawa T, Kumamoto K, Haga N (2011) Single-incision laparoscopic-assisted surgery for colon cancer via a periumbilical approach using a surgical glove: initial experience with 9 cases. Int J Surg 9:150–154
Choi SI, Lee KY, Park SJ, Lee SH (2010) Single port laparoscopic right hemicolectomy with D3 dissection for advanced colon cancer. World J Gastroenterol 16:275–278
Cahill RA, Hompes R, Cunningham C, Mortensen NJ (2011) Sealed Orifice Laparoscopic or Endoscopic (SOLE) surgery: technology and technique convergence for next-step colorectal surgery. Colorectal Dis 13:3–7
Disclosures
Drs. Ragupathi, Vande Maele, Nieto, Pickron, and Haas have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ragupathi, M., Maele, D.V., Nieto, J. et al. Transanal endoscopic video-assisted (TEVA) excision. Surg Endosc 26, 3528–3535 (2012). https://doi.org/10.1007/s00464-012-2399-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-012-2399-9