Abstract
Background
Single-port laparoscopic surgery is increasingly used to treat various types of diseases requiring surgical intervention. We present the technique and the results of our simple “cross and twine” intracorporeal knotting approach for treatment of a perforated duodenal ulcer.
Methods
From January 2009 to October 2009, 13 patients with perforated duodenal ulcers underwent single-port laparoscopic repair. The laparoscopic procedure included peritoneal lavage and suture of the perforation. The omentum above the repair site was then reinforced. After surgery, patients took an H2 receptor antagonist for 8 weeks and then underwent follow-up gastrofiberscopy.
Results
All procedures were completed under the conditions described. The mean operative time was 90.2 ± 24.2 min, and the mean hospital stay was 6.1 ± 0.5 days. The mean number of times that opiates were used for pain was 0.5 ± 1.0, and wound length was 1.9 ± 0.1 cm. There was no operation-related morbidity. Follow-up gastrofiberscopy revealed good lesion healing.
Conclusions
Single-port laparoscopic repair using the “cross and twine” knotting technique is a feasible and safe procedure, and it may be a less invasive laparoscopic surgical technique for scarless surgical treatment of perforated duodenal ulcers.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Perforated duodenal ulcers can be managed using various types of surgical options. However, as the efficacy of gastric antisecretory medication and eradication of Helicobacter pylori have improved [1, 2], the preferred surgical method for the treatment of perforated duodenal ulcers has shifted from definite ulcer surgery to primary repair of the perforation. Under this circumstance, laparoscopic primary repair was introduced for the repair of perforations and is now replacing the open procedure due to advantages such as less postoperative pain, faster recovery times, and shorter hospital stays [3, 4].
With advances in laparoscopic instruments and skills, laparoscopic single-port surgery (LSPS) has been developed and applied to many kinds of abdominal surgical procedures. This approach offers better cosmetic results (scarless abdominal surgery via umbilical incision), less incisional pain, and the capability to convert to multiport surgery if required [5–8]. However, making a “knot” when using the LSPS technique was more time-consuming and challenging than when using the conventional multiport laparoscopic technique to treat a perforated duodenal ulcer. This is the result of the limited freedom of movement when using the LSPS technique, which renders tool manipulation difficult.
In the present study we used LSPS to treat perforated duodenal ulcers with the simple “cross and twine” intracorporeal knotting technique, and then we evaluated the treatment results.
Materials and methods
Patients
From February 2009 to September 2009, 13 consecutive patients with perforated duodenal ulcers underwent LSPS. Each diagnosis was fundamentally based on the clinical presentation and the presence of subphrenic free air detected by chest radiography. Although the patient’s clinical presentation was adequate for a diagnosis of a perforated duodenal ulcer, abdominal computed tomography was performed to confirm the presence of free air around the duodenum if chest radiography presented obscure results. We did not perform LSPS for patients with previous upper abdominal surgery, gastric outlet obstruction, or history of gastric ulcers.
Surgical procedure
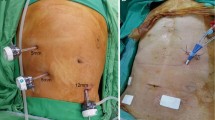
Before the operative procedure, a nasogastric tube was inserted in each patient, and prophylactic antibiotics were administered intravenously at the time of the incision. The single-port device was prepared before making a skin incision. The device comprised a surgical glove and three 5-mm trocars (Applied Medical, Rancho Santa Margarita, CA, USA). The trocars were inserted into the first, third, and fifth fingers of the glove and were then fastened with rubber bandages to prevent leakage of gas. A skin incision of about 20 mm was made in the patient’s umbilicus and carried down to the peritoneum. After a window had been made, a double-ring wound retractor (Alexis®, Applied Medical) was inserted through the incision and then rolled to cover and stretch the incision. The glove was then latched onto the wound retractor ring, which was rolled over it to provide a seal. Carbon dioxide was insufflated through the trocar at the first finger. After a pneumoperitoneum was established, a 5-mm 0° rigid videoscope was inserted into the first finger of the glove and the other two trocars were used for operating. After port access had been achieved, the operating table was tilted to the left and was placed in the reverse Trendelenberg position at angles of 15° and 25°, respectively. The abdominal cavity was examined and then the perforation site at the duodenum was identified. In case a perforation site was insufficiently exposed because of the liver or gallbladder, several pieces of surgical gauze were inserted between the liver bed and the upper border of the duodenum via a window to elevate the liver and gallbladder. Then the bulb of the duodenum was pulled downward by a laparoscopic instrument to secure the perforation site. The space around the perforation site was irrigated with warm normal saline. Then a 25-cm 3-0 polyglactin (Vicryl, Ethicon, Johnson & Johnson, Cincinnati, OH, USA) suture was inserted through the wall of the glove and introduced into the abdominal cavity with a laparoscopic needle holder (Fig. 1). During the suturing of the perforation site, the duodenum was pulled downward by one instrument and a double-stitch was simultaneously made on the perforation site with the other instrument (Fig. 2A). Each end of the thread was crossed on the liver surface (Fig. 2B). While holding the left end of the thread, the knot was produced by twining the right end of the thread through the space, which was created by crossing both ends of the thread (Fig. 2C). Then the knot was fastened using two instruments (Fig. 2D). A piece of the omentum was delivered into the perforation site, and then the perforation site was tied onto the omentum. The peritoneal cavity was massively irrigated with several liters of warm normal saline. At the end of the operation a closed suction drain was placed close to the repair site through the umbilicus.
Postoperative course
H2 receptor antagonist was intravenously injected during the fasting periods and then was orally administered after starting a meal. If a patient complained of pain at the operation site, 25 mg of pethidine was injected intramuscularly. The patients resumed oral intake after passing the first flatus and were discharged when they were able to tolerate an oral diet. An H2 receptor antagonist was prescribed for 8 weeks, and follow-up gastrofiberscopy was performed to assess the healing status of the ulcer and to identify whether the patient was affected by Helicobacter pylori. The patients infected with Helicobacter pylori were given triple therapy, including a proton pump inhibitor, amoxicillin, and clarithromycin for 1 week.
Results
Patient characteristics are listed in Table 1. All ulcer perforation sites were located in the duodenal bulb region and were less than 5 mm long. For four patients, no free air was observed by chest radiography; this observation was confirmed by abdominal computed tomography. The mean body mass index (BMI) was 22.4 ± 3.2.
There was no conversion to an open procedure or addition of a trocar (Table 2). The mean intracorporeal repair with omentopexy time was 20.7 ± 4.9 min; mean hospital stay was 6.1 ± 0.5 days. There were no operation-related morbidities, including dehiscence of the perforation site, intra-abdominal abscess, wound infection, or incisional hernia (especially at the umbilicus).
Discussion
Laparoscopic surgery is now replacing laparotomy for the treatment of various types of gastrointestinal problems and has been proven as a safe procedure. Laparoscopic surgery has several advantages, including less postoperative pain, shorter hospital stays, less scarring, and early recovery [9, 10]. Since Nathanson et al. [11] first reported laparoscopic management of a perforated duodenal ulcer in 1990, perforated duodenal ulcers have been managed with laparoscopic repair unless the ulcer is accompanied by a large perforation. With advances in instrumentation and surgical experience, many laparoscopic surgeons have attempted to minimize the number of ports to reduce traces of the operation, and LSPS was borne of these efforts. Various surgical procedures, including appendectomy, cholecystectomy, and adrenalectomy, have been attempted with LSPS, which presents certain advantages such as minimal scarring, less incisional pain, and the ability to add another trocar to perform multiport surgery [5–8]. The technique has attracted many laparoscopic surgeons. However, the previously described procedures were limited to resection procedures, and there was a hidden pitfall. We observed a “clashing” of instruments resulting from the restricted freedom of movement, the proximity of the instruments, and the parallel use of multiple instruments. These factors increased the complexity and technical challenges of the operation. For this reason, LSPS was believed to be a relatively more time-consuming procedure than multiport surgery, requiring extensive surgical skills and therefore limiting its application. To make up for these disadvantages, the articulated laparoscopic instrument was developed and is currently used in some institutes. However, it might take time for surgeons to acclimate themselves to this new technique, and the approach may increase costs. Patients with perforated duodenal ulcers usually undergo emergency operations because they feel poorly and run the risk of contracting sepsis. A surgical procedure, if it were applicable to this situation, should be simple. Unlike multiport laparoscopic surgery, LSPS does not provide sufficient triangulation for the simultaneous manipulation of instruments in order to make a “knot.” Therefore, a simple and less time-consuming technique was needed to treat perforated duodenal ulcer.
Taking these problems into consideration, we worked out a way to make a knot intracorporeally using the “cross and twine” method. This technique was simple and did not require the simultaneous manipulation of specialized instruments to make a “knot.” This technique is well suited to the conditions of the abdominal cavity. In general, the liver surface is wet. If suture threads are placed on the liver surface, they adhere to it easily; the moisture is sufficient to maintain the frame of the loop. We took advantage of this natural condition. The first step was to cross each end of the thread over the liver surface to build a loop after suturing the perforated site. The next step was insertion of the instrument through the loop, which was followed by pulling one end of the thread through the loop. Then, the knot was fastened with two instruments. After these procedures, the omentum was pulled at the repair site and fixed with the same threads used previously. Even if the surgeon was somewhat lacking in experience with LSPS, as long as s/he had a chance to obtain moderate laparoscopic experience, this “knotting” process could be performed without any challenges. The liver bed or gallbladder might occasionally inhibit sufficient exposure of perforation site, making the repair process more difficult. In that case, we inserted surgical gauzes between the liver bed and upper border of the duodenum to expose the operative field, and we tilted the operation table more vertically to secure an operative field. Various laparoscopic techniques have been designed to repair the perforated site and their usefulness has been evaluated [9, 12–14]. Since the edge of the perforation site is characterized by inflammation and friableness, a minor fissure of the repair site resulting from tight fastening might result in an unsatisfactory closure. To strengthen the weak point, we extended the omentum over the perforated site once more. As a result, there was no leakage at the perforation site or conversion to multiport surgery. Placement of a drain should be considered cautiously because there is no other puncture site except for the umbilicus. In that circumstance, we placed drains via the umbilicus without suturing the skin, and no wound infection has occurred. Nevertheless, careful wound management will be required.
Several port access techniques have been designed to carry out LSPS. For example, a combination of the Gelport and the Alexis double-ring wound retractor [5] and the use of port devices including the Unix-XTM (Pnavel Systems, Brooklyn, NY, USA) [15] and the R-portTM (Advanced Surgical Concepts, Wicklow, Ireland) [16] have been developed. However, there is still no standard method for single-port access. Because these port devices are not commonly supplied, we did not use commercial instruments; instead, we used devices that are commonly available in the operating room. Our port device was able to increase the diameter of the incision and protect the incised wound. If an additional trocar or instrument is needed, this could be accomplished by using the remaining two fingers of the glove without requiring a supplementary puncture.
In conclusion, LSPS for the treatment of a perforated duodenal ulcer using the “cross and twine” technique can be performed successfully without technical challenges and does not require any specialized instruments. In addition, even though there were a small number of patients included in this study, the results from treating the perforated duodenal ulcer with LSPS and the cross and twine technique demonstrated its safety and feasibility. Thus, LSPS might be an alternative means for treating perforated duodenal ulcers if the “cross and twine” method is used.
References
Chung SC, Li AK (1997) Helicobacter pylori and peptic ulcer surgery. Br J Surg 84:1489–1490
Hopkins RJ, Girardi LS, Turney EA (1996) Relationship between Helicobacter pylori eradication and reduced duodenal and gastric ulcer recurrence: a review. Gastroenterology 110:1244–1252
Kathouda N, Mouiel J (1998) Laparoscopic treatment of peptic ulcer disease. In: Hunter JG, Sackie JM (eds) Minimally invasive surgery. McGraw-Hill, New York, pp 123–130
Lunevicius R, Morkevicius M (2005) Systematic review comparing laparoscopic and open repair for perforated peptic ulcers. Br J Surg 92:1195–1207
Merchant AM, Cook MW, White BC, Davis SS, Sweeney JF, Lin E (2009) Transumbilical gelport access technique for performing single incision laparoscopic surgery (SILS). J Gastrointest Surg 13:159–162
Hong TH, You YK, Lee KH (2009) Transumbilical single-port laparoscopic cholecystectomy: scarless cholecystectomy. Surg Endosc 23(6):1393–1397
Pappalepore N, Tursini S, Marino N, Lisi G, Lelli Chiesa P (2002) Transumbilical laparoscopy-assisted appendectomy (TULAA): a safe and useful alternative for uncomplicated appendicitis. Eur J Pediatr Surg 12:383–386
Castellucci SA, Curcillo PG, Ginsberg PC, Saba SC, Jaffe JS, Harmon JD (2008) Single port access adrenalectomy. J Endourol 22:1573–1576
Bhogal RH, Athwal R, Durkin D, Deakin M, Cheruvu CNV (2008) Comparison between open and laparoscopic repair of perforated ulcer disease. World J Surg 32:2371–2374
Nelson H, Sargent DJ, Wieand HS, Fleshman J, Anvari M, Stryker SJ, Beart RW, Hellinger M, Flanagan R, Peters W, Ota D (2004) A comparison of laparoscopically assisted and open colectomy for colon cancer. N Engl J Med 350:2050–2059
Nathanson LK, Easter DW, Cushieri A (1990) Laparoscopic repair peritoneal toilet of perforated duodenal ulcer. Surg Endosc 4:232–233
Palanivelu C, Jani K, Senthilnathan P (2007) Laparoscopic management of duodenal ulcer perforation: is it advantageous? Indian J Gastroenterol 26(2):64–66
Song KY, Kim TH, Kim SM, Park CH (2008) Laparoscopic repair of perforated duodenal ulcers: the simple “one-stitch” suture with omental patch technique. Surg Endosc 22:1632–1635
Atea M, Sevil S, Bakircioglu E, Colak C (2007) Laparoscopic repair of peptic ulcer perforation without omental patch versus conventional open repair. J Laparoendosc Adv Surg Technol A 17:615–619
Remzi FH, Kirat HT, Kaouk JH, Geisler DP (2008) Single-port laparoscopy in colorectal surgery. Colorectal Dis 10:823–826
Rane A, Rao P, Bonadio F, Rao P (2007) Single port laparoscopic nephrectomy using a novel laparoscopic port (R-port) and evolution of single laparoscopic port procedure (SLIPP). J Endourol 21:A287
Disclosures
Drs. J. Lee, K. Sung, D. Lee, W. Lee, and W. Kim have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, J., Sung, K., Lee, D. et al. Single-port laparoscopic repair of a perforated duodenal ulcer: intracorporeal “cross and twine” knotting. Surg Endosc 25, 229–233 (2011). https://doi.org/10.1007/s00464-010-1164-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-1164-1