Abstract
Background
Mesh-assisted hiatal closure during foregut surgery is increasing. Our aim was to evaluate the complications that follow revisional foregut surgery. Specifically, we compared surgical indications and perioperative outcomes between patients with and without prior hiatal mesh (PHM).
Methods
We conducted an institutional review board (IRB)-approved retrospective cohort study from a single tertiary-care referral center. Over 37 months, 91 patients underwent revisional foregut surgery. We excluded 13 cases including operations performed primarily for obesity or achalasia. Of the remaining 78 patients, 10 had PHM and 68 were nonmesh patients (NM).
Results
The groups were similar in terms of age, body mass index (BMI), American Society of Anesthesiologists (ASA) classification, and rates and types of anatomic failure. Compared with NM patients, PHM patients had increased estimated blood loss (410 vs. 127 ml, p < 0.01) and operative time (4.07 vs. 2.89 h, p < 0.01). The groups had no difference in perioperative blood transfusion or length of stay. Complete fundoplication was more commonly created in NM patients (2/10 vs. 42/68, p = 0.03). Three of the 10 PHM patients and 3 of the 68 NM patients required major resection. Therefore, PHM patients had 6.8-fold increased risk of major resection compared with NM patients [95% confidence interval (CI) = 1.585, 29.17; p = 0.05]. The NM patients with multiple prior hiatal operations had 4.6-fold increased risk of major resection compared with those with one prior operation (95% CI = 2.919, 7.384; p = 0.03). In PHM patients, however, the number of prior hiatal operations was not associated with major resection.
Conclusions
PHM is associated with increased risk of major resection at revision. The pattern of failure was not different in patients with hiatal mesh, suggesting that hiatal mesh does not eliminate the potential for revision. When performing hiatal herniorrhaphy, the increased risk of recurrence without mesh must be weighed against the potential risk for subsequent major resection when using mesh.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Surgeons generally agree upon specific key components for successful paraesophageal hernia (PEH) repair. Those components include visceral reduction, sac excision, obtaining adequate intraabdominal esophageal length, crural reapproximation, and fundoplication. There is debate, however, as to how to manage the hiatal opening after hernia reduction. To address these issues, Targarona published a review looking at strategies in using mesh for hiatal repair, not all of which are tension-free [1]. Options for primary repair include the use of continuous [2] or interrupted sutures, with or without synthetic pledgets [3, 4]. Options for mesh repair include placement of an anterior triangular [5], posterior triangular [6], or square piece of mesh [7]. The mesh can also be fashioned in a keyhole configuration [8, 9], or the mesh can be used as a buttress reinforcement of the pillars using an onlay technique [10]. Alternatively, a relaxing incision lateral to the right crura can be performed, with mesh coverage of the subsequent diaphragmatic defect [11, 12]. Finally, the mesh itself may be fully synthetic, biological, or semisynthetic.
Those who believe in the use of hiatal mesh cite the need for a secure tension-free repair that is sometimes impossible without mesh because of a large defect, poor crural strength, and/or a fibrotic and tense diaphragm. Opponents of mesh realize that the esophagus is a dynamic structure that moves during breathing and swallowing and may therefore suffer adverse inflammation and erosion caused by apposition of mesh to the esophageal adventitia. Therefore, controversy exists as to the best means of repair.
Despite the fact that both methods of repair have known rates of recurrence, reintervention required in a patient with fundoplication failure following prior hiatal mesh may involve a separate set of challenges, not seen during a reintervention in a patient without prior hiatal mesh.
In this study, our aim is to evaluate the complications that follow revisional surgery for fundoplication failure and/or recurrent hiatal hernia. In particular, we compared the indications for surgery and the perioperative outcomes between those patients with and without a prior mesh repair of the esophageal hiatus.
Materials and methods
The institution’s institutional review board approved this retrospective cohort study (IRB no. 09-006300). Data were collected from the electronic medical record of a single tertiary-care referral center. Between December 2006 and December 2009, 91 patients were identified as having had revisional foregut surgery. Patients undergoing planned operations for obesity (n = 2) or achalasia (n = 11) were excluded from analysis. From the records of the remaining 78 patients, we determined the number of patients that had previous hiatal mesh, and then gathered demographic data including age, gender, BMI, ASA classification, number of prior foregut operations (dichotomized into one or multiple), and reason for fundoplication failure. Reasons for fundoplication failure were based on patients’ presenting symptoms, radiographic studies, and intraoperative findings.
The operative records for the previous procedures were reviewed to determine the preoperative approach and type of procedure performed. Of the 10 patients with prior mesh, 7 had operative reports that described the mesh placement. Two of the seven had interpositional polytetrafluoroethylene (PTFE) mesh. The remaining five patients had an onlay mesh placed; three were biologic mesh and two were PTFE mesh. Intraoperative outcomes from our institution included estimated blood loss, operative time, creation of fundoplication, and whether or not major resection was required. In addition, postoperative records were reviewed to determine quantity of blood transfused and length of hospital stay.
The primary outcomes were the need for major esophagogastric resection requiring anastomosis and the ability to create a fundoplication. Secondary outcomes were length of stay (LOS), operative time, estimated blood loss (EBL), laparoscopic approach, rate of conversion to open procedure, and amount of blood transfused. To compare the primary outcome of major resection between the exposed and unexposed groups, a rate of major resection was calculated. These rates were then used to determine a rate ratio, describing the relative rate of major resection between those with prior mesh and those without. Further analysis was performed on each of the exposure groups, exploring the association between multiple previous operations and the need for major resection at revision.
For continuous data, including age, BMI, operative time, EBL, and LOS, a two-sample t test was used to compare differences between the two groups. For ordinal data, as with the number of units of blood transfused, the Mann–Whitney U test was used. For dichotomous data, including gender, anatomic failure, multiple previous operations, laparoscopic approach, conversion to open procedure, major resection, and ability to create a fundoplication, Fisher’s exact test was used to analyze difference between the two groups. For categorical data, including ASA score, Kruskal–Wallis test was performed.
Statistical analysis was performed using SAS 9.1.3 and OpenEpi, with p < 0.05 considered statistically significant. Confidence intervals (95%) were calculated where appropriate.
Results
Patients in each exposure group [nonmesh (NM) and prior hiatal mesh (PHM)] were similar with regard to age, gender, BMI, and ASA classification. In addition, the groups had similar rates of anatomic and functional failure and similar background regarding the number of prior operations, as shown in Table 1. The specific mechanisms of fundoplication failure are presented in Table 2. With regard to intraoperative and perioperative outcomes, there were no significant differences in operative approach between groups (e.g., laparoscopic, open, or conversion to open). Based on intention-to-treat analysis, complete fundoplication was more commonly created in those patients with NM than in those with PHM (n = 0.03). We also found differences between PHM and NM patients involving operative time (p < 0.01), EBL (p < 0.01), and need for major resection (p = 0.05), as shown in Table 3. No difference between groups was seen regarding LOS, transfusion requirements, or creation of a partial fundoplication.
In the 68 patients in the NM group, 3 required major resection at reoperation. The first patient required thoracoabdominal esophagogastrectomy, the second patient underwent esophagogastrectomy with Roux-en-Y esophagojejunostomy, and the third patient had takedown of a NF with subtotal gastrectomy and uncut Roux-en-Y reconstruction. In the 10 patients with PHM, 3 required major resection. The first patient required left thoracotomy with mesh removal and esophagogastrectomy, the second patient underwent thoracoabdominal esophagogastrectomy with mesh removal, and the third patient had open esophagogastrectomy with pyloroplasty and mesh removal. Therefore, the relative risk of requiring major resection is 6.8 times as likely in PHM patients as compared with NM patients (95% CI = 1.585, 29.17; p = 0.05). The incidence of major resection was similar between those patients with biological mesh (one of four) and permanent mesh (two of six).
In PHM patients, the number of prior hiatal operations was not associated with need for resection. The NM patients having multiple prior hiatal operations were 4.6 times as likely to require resection as those with only one prior operation, which was statistically significant (95% CI = 2.919, 7.384; p = 0.03).
Discussion
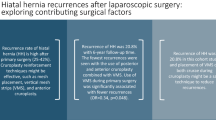
The reported use of hiatal mesh has increased, based on reports of high radiologic recurrence following primary hiatal herniorrhaphy and the reduction of this rate when using mesh. Complete analysis of the costs and benefits of hiatal mesh can only be performed with additional data, including the likelihood of patients with radiologic hiatal hernia recurrence to become symptomatic and require revisional operation, and the morbidity of revisional operation. It should be clear from the high-quality studies that have been performed, comparing mesh and nonmesh repair, that radiologic recurrence of hiatal hernia is reduced with mesh.
In 2005, Granderath and colleagues published results from a prospective trial showing that intrathoracic wrap migration occurred more frequently following primary crural closure than following closure with a heavyweight polypropylene mesh pledget technique (26 vs. 8%, respectively) [13]. Also by randomized trial, Frantzides compared key-holed PTFE buttress with no-mesh closure and showed benefit in reduction of radiological recurrence (0 vs. 22%, respectively) [14]. Due to concern over using prosthetic mesh at the esophageal hiatus, Oelschlager and colleagues performed a multicenter, prospective, randomized trial investigating the use of a U-shaped, small intestine submucosal (SIS)-based hiatal mesh as an onlay buttress, in comparison with primary suture approximation during laparoscopic paraesophageal hernia (PEH) repair. Similar to outcomes from studies investigating permanent mesh, those authors noted that four patients (9%) developed a recurrent hernia (>2 cm) in the mesh group, while 12 patients (24%) developed a hernia in the primary repair group at 6-month follow-up [15].
Laparoscopic repair of PEH is associated with up to a 42% hernia recurrence rate at 27–37 months median follow-up, based on esophagram [16, 17], though there appears to be little correlation between recurrent hernia and recurrent symptoms. Hashemi’s series of 41 patients showed reherniation in 12 patients, but 7 of the 12 were asymptomatic [16]. In Luostarinen’s study, only 5 of 16 patients had recurrent PEH following hiatal repair, with few patients having symptoms [17]. In the multicenter SIS study, however, patients with recurrent hernia had significantly more chest pain, early satiety, and worse physical functioning [15].
Most studies point to a very low rate of symptoms in patients with nonmesh repair of PEH, even in those patients with radiologic recurrence. In 1999, Hunter and colleagues published results from 99 patients who underwent laparoscopic fundoplication and PEH repair. Based on median follow-up of 34 months, revision was required in only three patients, and this was similar to their rate of revision (3.6%) for patients who underwent laparoscopic fundoplication for gastroesophageal reflux disease (GERD) [18]. Terry and colleagues looked at 1,000 patients at 27-month median follow-up, and they reported a reoperative rate of 3.5% for all-comers. Despite the acknowledged higher rate of recurrent hiatal hernia after PEH repair, the rate of symptomatic fundoplication failure requiring reoperation was lower when compared with fundoplication for GERD (reoperation rate: PEH 1.7%, GERD 4.2%, p < 0.01) [19]. A subsequent publication of 1,892 patients at the same institution showed a similarly low 2.8% rate of reoperation after laparoscopic PEH repair [20]. This suggests that the quality of the fundoplication may play a greater role in postoperative symptoms than the presence of recurrent hiatal hernia.
It is apparent from analysis of the reports of hiatal mesh that GERD-related symptoms are adversely affected by use of hiatal mesh. Patients with hiatal mesh had a higher rate of dysphagia at 3 months when compared with those without mesh (12 vs. 4%), although there was no difference at 1-year follow-up [13]. More recent data also showed a higher rate of dysphagia in the mesh group at 3 months (15 vs. 5%), with the 1-year follow-up again showing no difference. Although the dysphagia appears to resolve, a statistically significant decreased lower esophageal sphincter (LES) pressure is noted in the nonmesh group compared with the mesh group (8.9 ± 3.7 vs. 13.9 ± 4.9 mmHg, respectively, p < 0.01) [21]. In the multicenter SIS study, although not powered to reveal a difference in GERD-related symptom control, patients with a mesh repair had a trend towards increased heartburn, regurgitation, dysphagia, chest pain, and bloating scores, in comparison with patients repaired without mesh [15].
Evidence points toward an increased rate of symptoms in patients with both hiatal mesh and anatomic failure. Soricelli reports that all patients with both mesh repair and demonstrated anatomic failure required reoperation. Luketich and colleagues reported their 10-year experience with laparoscopic repair of giant PEH with selective use of biologic mesh. Based on a total of 662 patients, 445 had a follow-up barium esophagram after 3 months postoperatively, and 70 patients (15.7%) had radiographic recurrence. Interestingly, the incidence of radiographic recurrence was actually similar between those patients with and without hiatal mesh. In addition, there was no difference in the rate of symptoms between those patients with and without radiographic recurrence. It was apparent that hiatal mesh did not prevent radiographic recurrence, nor did it prevent the need for reoperation, as there was a higher rate of reoperation after mesh was used than when no mesh was used (9.1 vs. 2.3%; p = 0.0007). The authors state that the failure of mesh to show a decreased recurrence rate may have to do with selective use of mesh for only those patients in whom crural closure was compromised [22].
While mesh may reduce recurrent hernia, this may be reduced at the cost of GERD-related symptoms that are, at least, transiently increased. And in the presence of mesh, anatomic failure may be more likely to require reoperation. This report demonstrates that reoperation in the setting of prior mesh is associated with increased morbidity and increased rate of requiring major esophagogastric resection. Those prior hiatal mesh patients who did not require resection were also less likely to have complete fundoplication. The goals of reoperation in the setting of prior hiatal mesh are more remedial than in patients without mesh, due to the difficulty of managing the fibrosis and adhesions caused by the mesh.
We explored the possibility that the number of previous operations was confounding the relationship between prior mesh and major resection. However, there was no significant association between the exposure of interest (mesh) and the confounder (number of previous operations), and therefore the number of previous operations was not a confounder. Additionally, we investigated the relationship between the primary outcome (major resection) and the number of prior operations (one vs. two or more). While the NM patients who had multiple previous hiatal operations were statistically more likely to require resection than those with only one prior operation [relative risk (RR) = 4.6], the number of prior hiatal operations in PHM patients had no association with major resection. Therefore, if we compare the relative risk of major resection in PHM patients versus NM patients (RR = 6.8) with the relative risk of major resection for NM patients with multiple prior operation versus NM patients with one prior operation (RR = 4.6), it appears that prior mesh is more problematic than having had multiple previous operations.
Mesh-associated complications have been published in numerous case reports and case series. Based on 15 patients who had crural repair with expanded PTFE mesh, Griffith and colleagues presented a 20% complication rate. Dysphagia resulted within 7–34 months postoperatively, secondary to LES stenosis, and was amenable to minimally invasive techniques that resolved the dysphagia. Procedures included endoscopic mesh removal, endoscopic placement of a covered stent, and laparoscopic drainage of a periesophageal fluid collection and removal of mesh [23]. Additionally, Rumstadt described a patient who had successful endoscopic removal of a titanium-covered polypropylene mesh that had eroded intraluminally at the gastroesophageal junction (GEJ) [24]. Finally, Tatum reported two more cases involving mesh complication. While one patient had successful removal of a PTFE mesh, the other patient required gastrectomy to remove a mesh that had eroded into the GEJ and gastric cardia [25].
In the largest series of mesh-related hiatal complications, Stadlhuber and colleagues described 28 patients with PHM that presented with a variety of foregut-related symptoms, and 23 of the 28 ultimately required surgery. Intraoperative findings included intraluminal mesh erosion (n = 17), esophageal stenosis (n = 6), and dense fibrosis (n = 5). Of the 23 patients who underwent surgery, 6 required esophagectomy, 2 required partial gastrectomy, and 1 had a total gastrectomy. Although there were no immediate postoperative mortalities, one patient had severe gastroparesis and five patients became dependent on tube feeding [26]. Therefore, mesh-based hiatal repair can create an unmanageable problem that may lead to major resection. Consistent with Stadlhuber’s finding of a 32% incidence of major resection, our results demonstrate a 30% incidence of major resection in the face of PHM, significantly higher than the 4.3% incidence of major resection during revisional surgery on NM.
In addition to the increased risk of major resection in patients with PHM, our secondary outcomes demonstrate that patients with PHM had increased EBL and operative time, relative to those patients with NM. We saw no difference between groups with regard to LOS and need for blood transfusion. The increased operative time and EBL in patients with PHM are likely explained by the obscured tissue planes and inflammatory changes often associated with mesh, as well as the degree of difficulty involved in the dissection around biological mesh or in the careful removal of permanent mesh.
Fortunately, successful revisional surgery has been done with highly selective or no use of mesh. Based on the revision of 104 patients with fundoplication failure, 24 of whom had crural disruption, Iqbal and colleagues used mesh in only four patients. Despite both the prevalence of crural disruption (n = 24) and the infrequent use of mesh, 74% of patients had resolution of symptomatic dysphagia at mean follow-up of 38 months. Similarly, the majority of patients had resolution of heartburn (75%), regurgitation (85%), and chest pain (94%) [27].
There are several limitations to our report. Although this represents a large volume of revisional fundoplications over a 3-year period, there are few prior hiatal mesh patients, and they could result from referral bias. With such small numbers, it would be difficult to determine if biologic meshes were associated with different outcomes at reoperation as compared with permanent mesh. As none of the ten patients with prior hiatal mesh had their initial surgery at our institution, we cannot determine if the prior fundoplication was altered by mediastinal herniation, inflammation caused by mesh, or if the fundoplication was initially misplaced. As we report only perioperative data, we cannot be certain of the efficacy of our revisional operation. Finally, as more experience is gained with revisional surgery in the face of hiatal mesh, it is possible that the rate of major resection could improve.
In conclusion, this study demonstrates that presence of mesh at the esophageal hiatus is associated with increased risk of requiring major resection during a revisional procedure. Our finding is independent of the mechanism of fundoplication failure. Both the PHM and NM groups had high incidence of anatomical failure (80 and 72%, respectively), with symptomatic PEH being the most common indication for reoperation. Although mesh decreases hiatal hernia recurrence, this decrease is based more on radiographic data than on symptomatic data. We believe that GERD-specific symptomatic outcomes are more dependent on the quality of the fundoplication and less dependent on the quality of the hiatal repair. Furthermore, mesh does not eliminate recurrence. Mesh does, however, create a significantly morbid path to remediation. Therefore, because of the increased complexity, time required, and chance for major resection when operating in the setting of prior hiatal mesh, the stakes are higher for both the surgeon and patient.
Looking closely at the seven patients with prior mesh for whom preoperative procedural notes were available, we noted that five had an onlay mesh and two had mesh interposition, with one patient from each group having had major resection. Because the number of patients with prior mesh was relatively small, these data afford us no opportunity to present techniques of mesh placement that could minimize the need for reoperation or resection at reoperation. However, based on senior author experience, we anecdotally advise surgeons to avoid the following if possible: use of permanent mesh at the hiatus, use of interpositional mesh as a “bridge” to closure, and having mesh in contact with the esophagus. Alternatively, one might consider a right lateral relaxing incision on the diaphragm, which allows crural approximation without tension. This can be followed by placement of a biologic or semisynthetic mesh that bridges the neodiaphragmatic defect and buttresses the crural closure posteriorly, with tissue interposition that prevents mesh from contacting the esophagus.
When performing an initial hiatal hernia repair, we agree that an ideal tension-free primary crural repair involves maintenance of the peritoneal lining over the crura and complete division of all attachments from the diaphragm to the stomach and spleen [22]. We suggest that mesh be considered when concern for recurrence is especially high. Such patients may include those that require an esophageal lengthening procedure or have flimsy crura, as well as those with large hiatal defects or prior hiatal recurrences. Therefore, prior to repairing a hiatal hernia with mesh, the surgeon must weigh the potential benefit of a decreased rate of recurrence against the potential risk of a subsequent major resection.
References
Targarona EM, Bendahan G, Balague C, Garriga J, Trias M (2004) Mesh in the hiatus: a controversial issue. Arch Surg 139:1286–1296 (discussion 1296)
Cuschieri A, Shimi S, Nathanson LK (1992) Laparoscopic reduction, crural repair, and fundoplication of large hiatal hernia. Am J Surg 163:425–430
van der Peet DL, Klinkenberg-Knol EC, Alonso Poza A, Sietses C, Eijsbouts QA, Cuesta MA (2000) Laparoscopic treatment of large paraesophageal hernias: both excision of the sac and gastropexy are imperative for adequate surgical treatment. Surg Endosc 14:1015–1018
Jobe BA, Aye RW, Deveney CW, Domreis JS, Hill LD (2002) Laparoscopic management of giant type III hiatal hernia and short esophagus. Objective follow-up at three years. J Gastrointest Surg 6:181–188 (discussion 188)
Luketich JD, Raja S, Fernando HC, Campbell W, Christie NA, Buenaventura PO, Weigel TL, Keenan RJ, Schauer PR (2000) Laparoscopic repair of giant paraesophageal hernia: 100 consecutive cases. Ann Surg 232:608–618
Kuster GG, Gilroy S (1993) Laparoscopic technique for repair of paraesophageal hiatal hernias. J Laparoendosc Surg 3:331–338
Basso N, De Leo A, Genco A, Rosato P, Rea S, Spaziani E, Primavera A (2000) 360 degrees laparoscopic fundoplication with tension-free hiatoplasty in the treatment of symptomatic gastroesophageal reflux disease. Surg Endosc 14:164–169
Athanasakis H, Tzortzinis A, Tsiaoussis J, Vassilakis JS, Xynos E (2001) Laparoscopic repair of paraesophageal hernia. Endoscopy 33:590–594
Oelschlager BK, Barreca M, Chang L, Pellegrini CA (2003) The use of small intestine submucosa in the repair of paraesophageal hernias: initial observations of a new technique. Am J Surg 186:4–8
Kamolz T, Granderath FA, Bammer T, Pasiut M, Pointner R (2002) Dysphagia and quality of life after laparoscopic Nissen fundoplication in patients with and without prosthetic reinforcement of the hiatal crura. Surg Endosc 16:572–577
Horgan S, Eubanks TR, Jacobsen G, Omelanczuk P, Pellegrini CA (1999) Repair of paraesophageal hernias. Am J Surg 177:354–358
Huntington TR (1997) Laparoscopic mesh repair of the esophageal hiatus. J Am Coll Surg 184:399–400
Granderath FA, Schweiger UM, Kamolz T, Asche KU, Pointner R (2005) Laparoscopic Nissen fundoplication with prosthetic hiatal closure reduces postoperative intrathoracic wrap herniation: preliminary results of a prospective randomized functional and clinical study. Arch Surg 140:40–48
Frantzides CT, Madan AK, Carlson MA, Stavropoulos GP (2002) A prospective, randomized trial of laparoscopic polytetrafluoroethylene (PTFE) patch repair vs simple cruroplasty for large hiatal hernia. Arch Surg 137:649–652
Oelschlager BK, Pellegrini CA, Hunter J, Soper N, Brunt M, Sheppard B, Jobe B, Polissar N, Mitsumori L, Nelson J, Swanstrom L (2006) Biologic prosthesis reduces recurrence after laparoscopic paraesophageal hernia repair: a multicenter, prospective, randomized trial. Ann Surg 244:481–490
Hashemi M, Peters JH, DeMeester TR, Huprich JE, Quek M, Hagen JA, Crookes PF, Theisen J, DeMeester SR, Sillin LF, Bremner CG (2000) Laparoscopic repair of large type III hiatal hernia: objective followup reveals high recurrence rate. J Am Coll Surg 190:553–560 (discussion 560–561)
Luostarinen M, Rantalainen M, Helve O, Reinikainen P, Isolauri J (1998) Late results of paraoesophageal hiatus hernia repair with fundoplication. Br J Surg 85:272–275
Hunter JG, Smith CD, Branum GD, Waring JP, Trus TL, Cornwell M, Galloway K (1999) Laparoscopic fundoplication failures: patterns of failure and response to fundoplication revision. Ann Surg 230:595–604 (discussion 604–606)
Terry M, Smith CD, Branum GD, Galloway K, Waring JP, Hunter JG (2001) Outcomes of laparoscopic fundoplication for gastroesophageal reflux disease and paraesophageal hernia. Surg Endosc 15:691–699
Smith CD, McClusky DA, Rajad MA, Lederman AB, Hunter JG (2005) When fundoplication fails: redo? Ann Surg 241:861–869 (discussion 869–871)
Granderath FA, Kamolz T, Schweiger UM, Pointner R (2006) Impact of laparoscopic nissen fundoplication with prosthetic hiatal closure on esophageal body motility: results of a prospective randomized trial. Arch Surg 141:625–632
Luketich JD, Nason KS, Christie NA, Pennathur A, Jobe BA, Landreneau RJ, Schuchert MJ (2010) Outcomes after a decade of laparoscopic giant paraesophageal hernia repair. J Thorac Cardiovasc Surg 139:395–404, 404.e1
Griffith PS, Valenti V, Qurashi K, Martinez-Isla A (2008) Rejection of goretex mesh used in prosthetic cruroplasty: a case series. Int J Surg 6:106–109
Rumstadt B, Kahler G, Mickisch O, Schilling D (2008) Gastric mesh erosion after hiatoplasty for recurrent paraesophageal hernia. Endoscopy 40 Suppl 2:E70
Tatum RP, Shalhub S, Oelschlager BK, Pellegrini CA (2008) Complications of PTFE mesh at the diaphragmatic hiatus. J Gastrointest Surg 12:953–957
Stadlhuber RJ, Sherif AE, Mittal SK, Fitzgibbons RJ Jr, Brunt LM, Hunter JG, DeMeester TR, Swanstrom LL, Smith CD, Filipi CJ (2009) Mesh complications after prosthetic reinforcement of hiatal closure: a 28-case series. Surg Endosc 23:1219–1226
Iqbal A, Awad Z, Simkins J, Shah R, Haider M, Salinas V, Turaga K, Karu A, Mittal SK, Filipi CJ (2006) Repair of 104 failed anti-reflux operations. Ann Surg 244:42–51
Disclosures
Authors Parker, Bowers, Bray, Harris, Belli, Pfluke, Preissler, Asbun, and Smith, have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parker, M., Bowers, S.P., Bray, J.M. et al. Hiatal mesh is associated with major resection at revisional operation. Surg Endosc 24, 3095–3101 (2010). https://doi.org/10.1007/s00464-010-1095-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-010-1095-x