Abstract
Background
Endoscopic submucosal dissection (ESD) is a technically demanding procedure associated with a higher risk of complications. This study aimed to assess the difficulties and outcomes experienced by endoscopists beginning to perform ESD.
Methods
This prospective study investigated course participants in an ESD training workshop. The participants were asked at the end of the workshop about the ease of using various ESD knives, the occurrence of complications and their management, the procedural time, and the outcomes for the swine used for the procedure.
Results
For this study, 24 endoscopists were trained in performing gastric and esophageal ESD techniques using a porcine model. The mean size of the specimen retrieved was 2.66 ± 1.18 cm. The mean procedural times were 52.09 ± 24.67 min for gastric ESD and 32.50 ± 8.45 min for esophageal ESD. During gastric ESD, 15 participants (65.22%) encountered perforations, whereas bleeding occurred during 13 ESDs (56.52%). There were two procedure-related mortalities. Significantly, a higher proportion of perforations were encountered with the use of noninsulated knives. The perforated and nonperforated groups did not show a difference in prior endoscopic experience (P = 0.335). The majority of the participants agreed that the swine model is appropriate for simulating both human gastric (96%) and esophageal (96%) ESD.
Conclusions
The ESD procedure is technically challenging and associated with a high rate of complications for beginners. The use of noninsulated knives may increase the risk of perforations during the learning curve for gastric ESD, and future prospective trials must evaluate their use. The development of training models may augment the acquisition of skills in low-volume centers but will not replace a standardized patient-based training program.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Intramucosal neoplasias of the stomach, esophagus, and colon are associated with a low risk of lymph node metastasis. Recently, endoscopic submucosal dissection (ESD) has emerged as an appealing treatment method for these superficial lesions [1–6]. This has resulted from mounting evidence, mainly from Japan, of benefits including higher en bloc resection rates and the potential to decrease local recurrence over that of endoscopic mucosal resection (EMR) [7, 8]. Acquisition of ESD outside Japan, however, has been slow because the procedure requires a different set of endoscopic skills and is associated with a higher risk of complications than conventional EMR.
To master the techniques of ESD, particularly in areas with a low incidence of early gastrointestinal (GI) cancers, it is prudent that a standardized protocol for training be formulated. Currently, little literature exists regarding the difficulties and learning curves involved in performing the first ESDs. Thus, this study aimed to determine the factors contributing to the endoscopist’s performance during an ESD training workshop.
Materials and methods
This prospective study investigated course participants in an ESD training workshop in a University-affiliated unit during March 2008. The ESD training workshop was a tricomponent, 3-day, advanced endoscopic intensive course providing lectures on the basics of ESD; a live demonstration of ESD performed for gastric, esophageal, and colonic lesions; and a hands-on practical session of ESD using the porcine model. The course faculties included local and Japanese endoscopists highly experienced in ESD. The topics of discussion included recognition and diagnoses of early gastrointestinal neoplasms [9, 10], the Paris classification of superficial neoplastic lesions of the gastrointestinal tract [11], the basic setup required for ESD, the indications and techniques of ESD [12], the different types of knives used for ESD and their properties [1, 13–15], and management of complications [16].
During the hands-on practical session, course participants were allowed to practice gastric and esophageal ESDs under the supervision of local and overseas faculties. The participants then were required to complete a questionnaire regarding their experiences learning the procedure. Their prior experiences in endoscopy and their experience performing their first ESD were assessed. The questions evaluated the difficulties using various ESD knives rated on 10-cm unscaled visual analog scale with choices ranging from 0 (no difficulty) to 10 (extreme difficulty), the occurrence of complications and their management, the procedural time, and the outcome for the swine.
Instruments and technique of ESD
In performing gastric and esophageal ESDs, the instruments available for use included the insulated tip (IT) knife (KD-610L; Olympus Co. Ltd., Tokyo Japan.), the hook knife (KD-620LR; Olympus Co. Ltd.), the flex knife (KD-630L; Olympus Co. Ltd.), the triangular tip (TT) knife (KD-640L; Olympus Co. Ltd.), and the needleknife (KD-1L-1; Olympus Co. Ltd.). The electrosurgical generator used was the ESG-100 (Olympus Co. Ltd.), and the settings were changed according to the procedure being performed. For the initial marking, “force coagulation I” mode was used at power level 20. During submucosal dissection, “pulse cut slow” mode was used at power level 80. For coagulation with the ESD knives, “force coagulation II” mode was used at power level 50, and for coagulation with the coagulation grasper, “soft coagulation” mode was used at power level 80.
The course participants were advised to follow a stepwise approach in performing ESD. This approach was illustrated during the lectures, then reinforced through a demonstration by the local and overseas faculties during a hands-on practical session. The study participants were divided into groups of two, each assisting the other during the procedure. They also had a choice of completing the procedure with a single knife or a combination of knives.
An imaginary lesion was first made by suctioning the mucosa using the endoscope or markings by the instructors. In the stomach, the imaginary lesions were created at the posterior wall of the antrum, whereas in the esophagus, the lesions were created at the posterior wall anywhere between the cricopharyngeus and the esophagogastric junction. The mucosa was lifted by submucosal injection of a hyaluronic acid–adrenaline–indigocarmine mixture [2]. It then was marked with a non-insulated-tip knife, and a circumferential incision was made with a knife according the endoscopist’s choice. A lateral margin at least 1 or 2 mm from the imaginary lesion was obtained. The submucosa then was dissected under direct vision by stretching the submucosal connective tissue using a transparent hood attached to the tip of the endoscope. Hemostasis was achieved using the ESD knives or the coagulation grasper for small vessels and hemoclips for larger vessels. The specimen retrieved was pinned to a foam board to avoid curling of the specimen and to allow for measurement of the size. The specimen size was taken as the maximum diameter of the specimen.
Statistical analyses
Statistical analyses were performed using Student’s t-test, Fisher’s exact test, and the chi-square test where appropriate. Comparison between groups was performed using the Kruskal–Wallis one-way test of variance. Statistical analyses of the data were performed using the SPSS 11.0 statistical software (SPSS, Chicago, IL, USA). A two-sided P value less than 0.05 was considered statistically significant.
Results
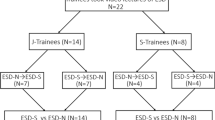
In March 2008, a total of 140 delegates participated in the ESD training workshop. Of these participants, 24 took part in the hands-on practical session, with 23 returning their questionnaires. The demographics of the participants are shown in Table 1. The 23 returned questionnaires showed that 16 participants (69.56%) had prior experience in endoscopic retrograde cholangiopancreatography (ERCP). A total of 23 gastric ESDs and 9 esophageal ESDs were performed. All the participants performed at least one gastric ESD. The procedural details are shown in Table 2. There were no significant differences between gastroenterologists and surgeons.
The majority of the participants completed the procedures with a combination of knives. The mean size of the specimen retrieved was 2.66 ± 1.18 cm. The mean procedural times were 52.09 ± 24.67 min for the gastric ESDs and 32.50 ± 8.45 min for the esophageal ESDs. There was a high incidence of associated complications. Perforations occurred during gastric ESDs for 15 participants (65.22%), and attempted closure with endoclips was successful in 13 cases (85.71%). Perforations occurred for five participants (55.56%) who underwent esophageal ESDs, and closure was successful in two cases (22.22%). Bleeding was encountered by 13 participants (56.52%), and all achieved successful hemostasis with either the ESD knives or the coagulation grasper. Two procedure-related mortalities occurred among the swine with gastric perforations.
The groups with and without perforations during gastric ESDs were further compared (Table 3). No significant differences were found related to years of medical (P = 0.960) or endoscopic (P = 0.335) experience. The numbers of endoscopic procedures performed per year did not differ significantly among the two groups, although the nonperforated group (P = 0.079) showed a trend of performing more endoscopic retrograde cholangiopancreatographies (ERCPs).
In terms of ESD instruments, the two groups showed significant differences in the types of knives used. More noninsulated knives were used in the perforated group including the TT knife (P = 0.089), the hook knife (P = 0.039), and the needleknife (P = 0.039), although no significant difference in usage between the insulated knives was observed (IT knife, P = 1.00; Flex knife, P = 0.269). In addition, no significant differences were found in terms of specimen size (P = 0.204), procedural time (P = 0.510), or procedure-related mortality (P = 1.00).
Regarding the difficulties using the various knives, the median difficulty scores for the various knives were 4.9 (range, 0.7–8) for the IT knife, 3.85 (range, 0.5–8) for the TT knife, 5 (range, 2–7) for the hook knife, 5.25 (range, 1.7–9) for the flex knife, and the 5 (range, 2–8) for the needleknife. The differences were not statistically significant (P = 0.466) (Fig. 1).
The participants also were questioned on the suitability of using the animal model as a simulation for human ESD. The majority of the participants agreed that the porcine model is appropriate for simulation of both gastric (96%) and esophageal (96%) ESD.
Discussion
For treatment of early gastric cancers, ESD is gaining popularity over endoscopic mucosal resection (EMR), and its use for esophageal and colonic lesions is increasingly reported [1–8]. The proposed advantages are that larger lesions can be resected en bloc, complete resection rates are higher, and local recurrence rates may be reduced [7]. However, obvious concerns surround the introduction of the procedure because it is technically more demanding and may potentially increase the risk of complications.
The current study demonstrated that the initial performances of ESD are associated with a high incidence of complications, the risk of which is not dependent on previous experience in endoscopy. This may indicate a significant difference between the techniques of ESD and other endoscopic procedures. It also highlights the need for a standardized patient-based training program that involves adequate observation and stepwise introduction of the procedure to allow safe performance of ESD by a beginner.
In major series, a perforation rate of 3% to 6% and an immediate bleeding rate of 7% have been reported, and most authors have indicated that the majority of perforations occurred in the early phase of their series [1, 3, 4, 7, 15]. Similar findings were noted for colorectal ESDs, with the rate of perforations decreasing markedly as experience is acquired [5]. On the other hand, Kakushima et al. [3] found that the endoscopist’s experience with ESD was not a determinant of treatment efficacy or safety. These authors found no significant difference in the rates for bleeding and perforation between cases managed early and late in the series. Rather, with increasing experience and proficiency of the technique, the procedural time decreased and lesion size increased.
The types of instruments used also appeared to affect the likelihood of perforation, with significantly more participants using noninsulated knives in the perforation group. In theory, a noninsulated knife is in direct contact with submucosal tissue, which could induce more tissue injury and diathermy penetration to the muscular layer during dissection. This increases the risk of perforation with the misjudgment of tissue depth. On the other hand, the IT knife was found to be associated with an increased risk of perforations during colorectal ESD [5]. This appears to be associated with the anatomic limitation of the colon, which is a cylindrical tubular structure, thus making the IT knife’s typical action of lateral dissection difficult (Fig. 2).
Furthermore, the ease of performing ESD also is determined by the part of the gastrointestinal tract involved as well as the location of the lesion within the organ. The difficulty performing gastric ESD was found to be dependent on the location and size of the lesion [4]. Ulcerative lesions larger than 20 mm in the upper third of the stomach were the most difficult lesions to be resected by ESD, whereas nonulcerated lesions at the antrum were the easiest to perform. This was partly because of the difficulty manipulating the partially dissected specimen in the upper third of the stomach due to a retroflexed endoscope and the effect of gravity. Control of the endoscope during esophageal ESD is limited by the confined cylindrical space within the esophagus, which is more susceptible to perforations due to a thinner muscularis propria [1, 2]. Large bowel ESDs located in the proximal large bowel (cecum and transverse colon) are more demanding to perform due to difficulty maintaining the position of the endoscope and also a thinner muscle layer [5, 8].
For the preceding reasons, the use of simulation models may be helpful in attaining the skills required for safe performance of ESD in areas that have a low volume of ESDs. The live porcine ex vivo or computer simulation models have gained much acceptance for training in upper endoscopy ESD, and some evidence suggests that prior training with these simulation models enhances skill acquisition [17, 18]. The majority of the participants in our workshop found the porcine model to be an appropriate simulation of human ESDs, and future studies should aim to assess whether training models can be developed for ESDs and comparisons between them. Nevertheless, it should be recognized that these simulation workshops are a means for augmenting training in skills and will not replace patient-based training [17].
Those who interpret the data in this study must recognize a number of potential biases and limitations. Selection bias may have occurred because only a small proportion of endoscopists were enrolled in the hands-on session. The participants not reporting on the occurrence of perforations may have contributed to a nonresponse bias. The participants with a particular preference for noninsulated knives may have caused a response style bias. Completion of the questionnaires at the end of the session posed the potential for a recall bias. The small group of participants in this study may have predisposed it to both type 1 and type 2 errors. Furthermore, it was difficult to assess the relative risk of various knives because the participants were not restricted to using only one knife throughout the procedure. Thus, evaluation of insulated versus noninsulated knives will be required in future prospective trials.
In conclusion, ESD is a technically challenging procedure that may be associated with a high rate of complications for beginners. The use of noninsulated knives may increase the risk of perforations during the learning curve for gastric ESD, and this should be evaluated in prospective trials. The development of training models may augment the acquisition of skills in low-volume centers, but these will not replace a standardized patient-based training program.
References
Chiu PW, Chan KF, Lee YT, Sung JJ, Lau JY, Ng EK (2008) Endoscopic submucosal dissection used for treating early neoplasia of the foregut using a combination of knives. Surg Endosc 22:777–783
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Yamamichi N, Tateishi A, Shimizu Y, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2006) Endoscopic submucosal dissection of esophageal squamous cell neoplasms. Clin Gastroenterol Hepatol 4:688–694
Kakushima N, Fujishiro M, Kodashima S, Muraki Y, Tateishi A, Omata M (2006) A learning curve for endoscopic submucosal dissection of gastric epithelial neoplasms. Endoscopy 38:991–995
Imagawa A, Okada H, Kawahara Y, Takenaka R, Kato J, Kawamoto H, Fujiki S, Takata R, Yoshino T, Shiratori Y (2006) Endoscopic submucosal dissection for early gastric cancer: results and degrees of technical difficulty as well as success. Endoscopy 38:987–990
Tanaka S, Oka S, Kaneko I, Hirata M, Mouri R, Kanao H, Yoshida S, Chayama K (2007) Endoscopic submucosal dissection for colorectal neoplasia: possibility of standardization. Gastrointest Endosc 66:100–107
Kodama M, Kakegawa T (1998) Treatment of superficial cancer of the esophagus: a summary of responses to a questionnaire on superficial cancer of the esophagus in Japan. Surgery 123:432–439
Oka S, Tanaka S, Kaneko I, Mouri R, Hirata M, Kawamura T, Yoshihara M, Chayama K (2006) Advantage of endoscopic submucosal dissection compared with EMR for early gastric cancer. Gastrointest Endosc 64:877–883
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Yamamichi N, Tateishi A, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2007) Outcomes of endoscopic submucosal dissection for colorectal epithelial neoplasms in 200 consecutive cases. Clin Gastroenterol Hepatol 5:678–683
Okabayashi T, Gotoda T, Kondo H, Ono H, Oda I, Fujishiro M, Yachida S (2000) Usefulness of indigo carmine chromoendoscopy and endoscopic clipping for accurate preoperative assessment of proximal gastric cancer. Endoscopy 32:S62
Uedo N, Iishi H, Tatsuta M, Yamada T, Ogiyama H, Imanaka K, Sugimoto N, Higashino K, Ishihara R, Narahara H, Ishiguro S (2005) A novel videoendoscopy system by using autofluorescence and reflectance imaging for diagnosis of esophagogastric cancers. Gastrointest Endosc 62:521–528
Participants of the Paris Workshop (2003) The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, 2002. Gastrointest Endosc 58:S3–S43
Gotoda T, Yanagisawa A, Sasako M, Ono H, Nakanishi Y, Shimoda T, Kato Y (2000) Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 3:219–225
Gotoda T (2005) A large endoscopic resection by endoscopic submucosal dissection procedure for early gastric cancer. Clin Gastroenterol Hepatol 3:S71–S73
Inoue H, Satoh Y, Kazawa T, Sugaya S, Usui S, Satodate H, Kudo S (2004) Endoscopic submucosal dissection using a newly developed triangle-tip knife. Stomach Intest 39:73–75
Kodashima S, Fujishiro M, Yahagi N, Kakushima N, Ichinose M, Omata M (2006) Endoscopic submucosal dissection for gastric neoplasia: experience with the flex-knife. Acta Gastroenterol Belg 69:224–229
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Kobayashi K, Hashimoto T, Yamamichi N, Tateishi A, Shimizu Y, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2006) Successful nonsurgical management of perforation complicating endoscopic submucosal dissection of gastrointestinal epithelial neoplasms. Endoscopy 38:1001–1006
Nelson DB, Bosco JJ, Curtis WD, Faigel DO, Kelsey PB, Leung JW, Mills MR, Smith P, Tarnasky PR, VanDam J, Wang KK, Wassef WY (1999) ASGE technology evaluation report: endoscopy simulators, May 1999. American Society for Gastrointestinal Endoscopy. Gastrointest Endosc 50:935–937
Sedlack R, Petersen B, Binmoeller K, Kolars J (2003) A direct comparison of ERCP teaching models. Gastrointest Endosc 57:886–890
Acknowledgments
We express our deepest appreciation for all the overseas faculties from Japan involved in organizing the ESD workshop including Professor Haruhiro Inoue, Digestive Disease Centre, Showa University; Dr. Takuji Gotoda, National Cancer Center Hospital; Dr Noriya Uedo, Osaka Medical Center for Cancer and Cardiovascular Diseases; and Dr. Naohisa Yahagi, Toranomon Hospital. We also thank Olympus Co. Ltd., Hong Kong, and Olympus Tokyo, Japan, for sponsoring the training workshop.
Disclosures
Anthony Y. B. Teoh, Philip W. Y. Chiu, Simon K. H. Wong, Joseph J. Y. Sung, James Y. W. Lau, and Enders K. W. Ng have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Teoh, A.Y.B., Chiu, P.W.Y., Wong, S.K.H. et al. Difficulties and outcomes in starting endoscopic submucosal dissection. Surg Endosc 24, 1049–1054 (2010). https://doi.org/10.1007/s00464-009-0724-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0724-8