Abstract
Background
In the absence of facilities and expertise for laparoscopic bile duct exploration (LBDE), most patients with suspected ductal calculi undergo preoperative endoscopic duct clearance. Intraoperative cholangiography (IOC) is not performed at the subsequent laparoscopic cholecystectomy. This study aimed to investigate the rate of successful duct clearance after simple transcystic manipulations.
Methods
This prospective study investigated 1,408 patients over 13 years in a unit practicing single-session management of biliary calculi. For the great majority, IOC was attempted. Abnormalities were dealt with by flushing of the duct, glucagon injection, Dormia basket trawling, choledochoscopic transcystic exploration, or choledochotomy.
Results
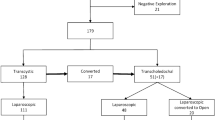
Of 1,056 cholangiograms performed (75%), 287 were abnormal (27.2%). Surgical trainees, operating under supervision, successfully performed 24% of all cholangiograms. Of 396 patients admitted with biliary emergencies, 94.1% had abnormal cholangiograms. Of the 287 patients with abnormal IOCs, 9.4% required no intervention, 18% were clear after glucagon and flushing, and 13% were cleared using Dormia basket trawling under fluoroscopy. A total of 95 patients required formal LBDE, and 2 required postoperative endoscopic retrograde cholangiopancreatography (ERCP). No postoperative ERCP for retained stones was required after simple transcystic manipulation. Eight conversions occurred, one during a transcystic exploration. Follow-up evaluation continued for as long as 6 years in some cases. Two patients had recurrent stones after LBDE and a clear postoperative tube cholangiogram.
Conclusion
In this series, 10% of the abnormal cholangiograms occurred in patients without preoperative risk factors for bile duct stones. Altogether, 88 IOCs (31%) were cleared after either simple flushing or trawling with a Dormia basket. Formal LBDE was not required for 40% of abnormal cholangiograms. Simple transcystic manipulations to clear the bile ducts justify the use of routine IOC in units without laparoscopic biliary expertise.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
The debate about the use of intraoperative cholangiography (IOC) continues, with recent reviews advocating a selective approach during laparoscopic cholecystectomy (LC) [1]. This is mainly because magnetic resonance cholangiopancreatography (MRCP) is emerging as the investigation of choice for patients with suspected ductal stones. In one study, MRCP demonstrated a sensitivity of 100% and a specificity of 96.3% [2]. Therapeutic endoscopic retrograde cholangiopancreatography (ERCP) may be required afterward to clear ductal stones before a LC. This two-session approach does not address some important issues such as clinically silent duct stones, spontaneous passage of stones found at MRCP during the wait for ERCP, or the likelihood of further stones passing into the bile duct between ERCP and LC or at the time of LC, because of excessive gallbladder handling before the cystic duct is secured. This approach is not necessary when IOC is performed for the great majority of patients treated in units practicing single-session laparoscopic management for all comers.
Although single-stage laparoscopic treatment of gallstones has been studied in prospective randomized trials [3, 4] and found to be superior to sequential endoscopic and laparoscopic treatment in terms of both clinical and economic outcome, many surgeons have been reluctant to adopt the procedure because it requires advanced levels of technical skills, availability of equipment, and logistic support. We aim to show that IOC is a useful tool, and that it can facilitate simple transcystic maneuvers used to clear the ducts in a proportion of patients who would otherwise have multiple diagnostic and therapeutic procedures and a longer hospital stay.
Patients and methods
Data and operative details were collected prospectively over a period of 13 years (1992–2004) in a unit practicing single-session management of all comers with gallstone disease. All the patients (n = 1,408) underwent surgery by a single consultant surgeon or in his presence. Both elective and emergency admissions were recruited. Hospital protocols were established to ensure that most emergency biliary admissions to any unit and all those with suspected bile duct stones were referred to the biliary unit after initial resuscitation and pain control.
Patients presented with biliary pain, acute cholecystitis, pancreatitis, obstructive jaundice, cholangitis, or a combination of these symptoms. All underwent preoperative investigations including an ultrasound scan and blood biochemistry assessment. Patient details were recorded on a proforma and entered into a Microsoft 2000 Access database. The use of MRCP was reserved for patients unfit for general anesthesia and those who showed no gallstones on ultrasound examination. Only those who had ductal calculi and remained unfit for surgery were referred for ERCP.
We use a standard four-port cholecystectomy. Intraoperative cholangiography is performed after preparation and distal intracorporeal ligation of the cystic duct to prevent stone migration and incision of its anterior wall. The cannulation unit comprises a 4-Fr ureteric catheter threaded through a cholangiography cannula. The unit is introduced into the abdomen via the right subcostal port, and the ureteric catheter then is advanced into the cystic duct incision without clamping, clipping, or ligating of the cystic duct around it (Fig. 1). Occasional resistance offered by valves in the cystic duct can, in most cases, be overcome by injecting saline or by gentle stretching using a “duckbill” or curved grasper to enable introduction of the catheter. It also is important to ensure that there are no stones in the proximal cystic duct. Cholangiography is obtained by injecting diluted contrast material under fluoroscopic control. Complete assessment of the biliary tree is almost always possible before any contrast leaks from the cystic duct incision. A cholangiography clamp is used only when the catheter cannot be passed into the common bile duct (CBD) or when obvious extravasation of the contrast occurs.
Initial attempts at transcystic duct clearance were performed when CBD stones were discovered at IOC, unless it was obvious from the size of the stone that a choledochotomy would be required to retrieve it. Saline flushing after glucagon injection was attempted first, followed by trawling with a Dormia basket either blindly or under fluoroscopic control. Flushing of the CBD, used in the case of single or multiple relatively small stones, was facilitated by the administration of glucagon.
Care was taken to avoid high-pressure flushing because this could have resulted in displacement of lower bile duct stones into the intrahepatic ducts. If duct clearance was unsuccessful, transcystic choledochoscopic examination using a 2.8-mm choledochoscope was attempted. The indications and the technique of choledochoscopic bile duct exploration are not the subject of this report.
Cholangiography was repeated to confirm duct clearance. Transcystic biliary drains were inserted after exploration for multiple stones, when stone fragmentation had occurred, or when repeated manipulation including passage of the Dormia basket through the papilla was necessary.
Results
In this study, 77% of the patients undergoing IOC were women. The median age was 51 years (mean, 51.3 years; range, 14–89 years). Of the 1,408 patients, 390 (28%) were emergency admissions.
Of the 1,056 patients (75%) who underwent IOC, 467 had risk factors for ductal stones. The threshold for performing an IOC was very low and based on preoperative and intraoperative findings. Most of the patients who did not undergo a cholangiogram had no clinical, biochemical, or radiologic evidence of CBD stones. In some cases, cystic duct cannulation was difficult, and no further attempts were made to obtain an IOC. In a small number of patients with strong evidence of a CBD stone or previously failed ERCP and stone extraction, the decision to progress to CBD exploration was made from the start without resort to a cholangiogram. Altogether, 287 cholangiograms were reported as abnormal (Table 1). Preoperative ultrasound evidence of duct dilation, ductal stones, or both seemed to be the factor most predictive of a positive IOC (50.8%) (Table 2).
Cholangiograms were considered abnormal if they showed any of five characteritistics: filling defects, no contrast flowing to the duodenum, anatomic variation, strictures, or a dilated duct.
Abnormal cholangiograms attributable to anatomic variation, CBD stricture, or dilated CBD without any filling defects did not require any intraoperative intervention and were labeled as such. There were 396 emergency admissions in the whole series. A total of 373 patients underwent IOC (94.1%). Of the 1,056 cholangiograms, more highly trained surgical trainees successfully managed 253, which represented 100% of those they attempted and 24% of all the cholangiograms performed.
In some cases, the decision to perform an IOC was made intraoperatively. The finding of wide cystic ducts in 56 patients without preoperative risk factors prompted cholangiography, and 14 were found to have filling defects in the CBD. The presence of cystic duct stones in 102 cases with no suspicion of choledocholithiasis was associated with 31 bile duct filling defects observed on cholangiography.
Clinically, silent duct stones were detected in 59 (10%) of 589 IOCs performed with no preoperative risk factors such as jaundice, history of jaundice, deranged liver function tests (LFTs), or ultrasound evidence (Table 3). This group, however, had intraoperative risk factors including wide cystic ducts in 56 cases and cystic duct stones in 86 cases.
After a positive IOC, simple initial attempts at transcystic clearance were made. In the early years of the study (1992–1995), six patients had IOCs showing suspected small filling defects, but no attempt was made at clearance either because transcystic exploration facilities were lacking or because the filling defects were small. Open exploration followed one failed transcystic choledochoscopic exploration (stone-impacted lower CBD) and four failed choledochotomies. Bypass procedures were necessary for four patients with impacted stones or anatomic abnormalities (Fig. 2). No intervention was required intraoperatively for a group of patients with anatomic variations, dilated ducts, and strictures (n = 27).
A total of 238 patients with abnormal cholangiography underwent laparoscopic exploration of the bile duct, 95 through dochotomies and 143 transcystically. Only 20% of the transcystic exploration group required the insertion of a choledochoscope. Abnormal cholangiograms were cleared in 31% of the patients either by flushing and glucagon injection (F&G) or by Dormia trawling with or without fluoroscopic guidance.
There were no bile duct injuries in the series. Four patients had documented bile leaks into subhepatic drains, all after laparoscopic bile duct exploration and dochotomies. All the patients were seen in the outpatient clinic 6 weeks and 12 months after discharge. Four postoperative ERCPs were necessary. Two ERCPs were required for retained stones identified during surgery that could not be removed with laparoscopic or open attempts. One ERCP was performed as a prophylactic measure after a laparoscopic bile duct exploration in which multiple intrahepatic stones were removed and clearance confirmed with a T-tube cholangiogram. The last ERCP in this group of patients was performed after the discovery of a lower CBD stricture on the IOC, which was subsequently diagnosed as pancreatic cancer.
After long-term follow-up assessment, two more ERCPs were required: the one performed 9 months and the other more than 2 years after surgery for recurrent stones. Both patients had undergone successful ductal explorations and normal postoperative tube cholangiography.
Discussion
In the past, routine intraoperative cholangiogram has been advocated for the diagnosis of unsuspected ductal stones and for aid in delineating the biliary anatomy [5, 6]. The adoption of a two-session approach for the management of suspected ductal stones, the perception that IOC is difficult and time consuming, and advances in preoperative detection of ductal stones in recent years have led to the relative decline in IOC. Virtual reality cholangioscopy using software to reconstruct magnetic resonance images has shown 71% sensitivity and 91% specificity for ductal stones [7]. Ultrasound [8] and more recently magnetic resonance cholangiography (MRC) [2, 9] have become increasingly reliable in detecting bile duct stones. There can be no doubt that the future holds even greater advances in the accuracy of imaging techniques, but all said, IOC and ERCP will continue to have a dominant role in the management of ductal stones.
Despite its potential for serious complications, ERCP continues to play a role [10, 11]. This has led to the emergence of MRC as the tool of choice for suspected ductal stones, followed by ERCP for the clearance of confirmed ductal stones before surgery. In our series, 10% of the patients had no preoperative evidence of ductal stones, which compares with reports in the literature [12, 13], one of which documented 11% silent CBD stones detected on IOC [14]. This remains a significant percentage of hospital admissions for calculus biliary disease and represents a failure in terms of preoperative CBD stone prediction and clearance.
In this series, routine IOC was performed during LC, followed by ERCP for those with abnormal IOC results. False-positive IOC in 0.8% of the cases [15] and spontaneous passage of stones before ERCP (∼25%) [16, 17] were found to be the reasons for the absence of stones at ERCP. In a review of nine series [1] involving 5,179 laparoscopic cholecystectomies performed without IOC, problems related to retained stones developed for 15% of the patients. We found that almost 80% of silent stones in our series occurred in cases of elective admissions, which may lend support to the theory that only a small proportion of silent CBD stones become symptomatic. However, it could be argued that, from a medicolegal point of view and to help facilitate follow-up planning, it is much better to know which patients harbor silent CBD stones.
Advocates of selective IOC for ductal stones argue that it is possible to predict the presence of ductal stones at the preoperative investigation for most patients. A second argument is that in the absence of preoperative risk factors for ductal stones, the small number of undetected ductal stones will remain asymptomatic or pass spontaneously in a majority of cases. However, in the absence of facilities for MRCP/ERCP, those who require an IOC during LC would not benefit much from the procedure because it would be only diagnostic. To clear the duct in a unit without laparoscopic bile duct exploration expertise would entail a postoperative ERCP or open bile duct surgery.
In our series, it was shown that the practice of IOC can be combined with simple transcystic manipulation such as flushing or trawling with a Dormia basket to obtain duct clearance. More highly trained surgical trainees successfully cleared the CBD in 14 patients by trawling the stones through the sphincter with the use of a Dormia basket. The judicious use of a Dormia basket combined with fluoroscopic guidance makes this technique a safe practice in the hands of trained surgeons. The safety and efficacy of Dormia baskets have been well demonstrated by their similar use in ERCP stone extraction. A total of 88 patients (31%) with filling defects shown on IOC were clear after simple maneuvers without the need for a choledochoscope. These simple techniques, based on the basic skill of cystic duct cannulation, should be mastered by any laparoscopic surgeon, who could effectively clear the ducts, avoiding further hospital admissions and interventions.
Findings have shown that flushing effectively clears retained stones through a transcystic T-tube (after the administration of glucagon) under radiologic control [18]. The same concept can be applied intraoperatively by trawling with a Dormia basket under fluoroscopy as presented in this series. In a similar series of laparoscopic bile duct explorations [19], nine patients had stones cleared from the CBD by flushing only, although there seemed to be no intent to pursue transcystic clearance by simple maneuvers, which could have led to a higher rate of duct clearance with the use of trawling under fluoroscopy. Cystic duct dilation over a guidewire with a combination of flushing, basket manipulation, retrieval, fragmentation, or advancement of stones through the ampulla has been advocated in the past [20]. A recent published series reported a 71% clearance rate with transcystic exploration and without the use of a choledochoscope. The same report also concluded that long-term outcomes after laparoscopic ductal clearance are similar to those for ERCP clearance [25].
Centers that perform selective IOC have success rates of 75% to 100%, as compared with success rates of 95% to 100% for patients in centers practicing routine cholangiography [21]. Surgical trainees successfully performed cystic duct access and cholangiography in 7% of the cases in this series, indicating the importance of overcoming the technical and interpretative learning curve of IOC for the investigation to be of practical use. Performance of an IOC leads to the development of skills that are useful in the context of the diagnostic and subsequent therapeutic advantage of single-stage management. A strong case can therefore be made for the routine use of IOC.
The use of IOC helped to identify aberrant anatomy and strictures in 13 patients. There were no bile duct injuries. Proponents of IOC argue that its main advantage is the immediate recognition of bile duct injuries although it does little to prevent them [22]. It has been suggested that unclear anatomy would render the placement of a cholangiogram catheter unsafe because it could directly injure the bile duct [1]. In our experience, this has never occurred due to meticulous dissection in Calot’s triangle, adequate management of cystic duct stones [23] and Hartman’s pouch stones, and fundus-first LC [24] to help in cystic duct identification.
Conclusion
Intraoperative cholangiogram remains a useful investigation even in units without full facilities for laparoscopic bile duct exploration. It allows single-session management of suspected bile duct stones in a proportion of patients who would otherwise require MRCP and/or ERCP, with the potential for complications and a longer hospital stay. When bile duct stones are confirmed, simple transcystic maneuvers may clear the ducts in up to one-third of those with a positive IOC. This gives IOC an edge over alternative preoperative diagnostic methods. The skills developed during routine IOC are the mainstay of those required to perform most bile duct explorations carried out through the transcystic approach.
References
Metcalfe MS, Ong T, Bruening MH, Iswariah H, Wemyss-Holden SA, Maddern GJ (2004) Is laparoscopic intraoperative cholangiogram a matter of routine? Am J Surg 187: 475–481
Wei KZ, Zhu ZC, Hui LJ, Kai Y, De HJ (2003) Prospective evaluation of magnetic resonance cholangiography in patients with suspected common bile duct stones before laparoscopic cholecystectomy. Hepatobiliary Pancreat Dis Int 2: 576–580
Cuschieri A, Lezoche E, Morino M, Croce E, Lacy A, Toouli J, Faggioni A, Riberio VM, Jakimowicz J, Visa J, Hanna GB (1999) EAES multicenter prospective randomized trial comparing two-stage vs single-stage management of patients with gallstone disease and ductal calculi. Surg Endosc 13: 952–957
Rhodes M, Sussman L, Cohen L, Lewis MP (1995) Randomized trial of laparoscopic exploration of common bile duct versus postoperative endoscopic retrograde cholangiography for common bile duct stones. Lancet 351: 159–161
Corbitt JD, Leonetti LA (1997) One thousand and six consecutive laparoscopic intraoperative cholangiograms. JSLS 1: 13–16
Kitahama A, Kerstein MD, Overby JL, Kappelman MD, Webb WR (1986) Routine intraoperative cholangiogram. Surg Gynecol Obstet 162: 317–322
Simone M, Mutter D, Rubino F, Dutson E, Roy C, Soler L, Marescaux J (2004) Three dimensional virtual cholangioscopy: a reliable tool for the diagnosis of common bile duct stones. Ann Surg 240: 82–88
Hunt DR, Reiter L, Scott AJ (1990) Preoperative ultrasound measurement of bile duct diameter: basis for selective cholangiography. Aust N Z J Surg 60: 189–192
Gautier G, Frank P, Crombe TA, Gruner L, Ponchon T, Barth X, Valette PJ (2004) Contribution of magnetic resonance cholangiopancreatography to the management of patients with suspected common bile duct stones. Gastroenterol Clin Biol 28: 129–134
Arvanitidis-Dimitrios G, Pantes A, Agaritsi R, Margantinis G, Tsiakos S, Sakorafas G, Kostopoulos P (2004) Can somatostatin prevent post-ERCP pancreatitis? Results of a randomized controlled trial. J Gastroenterol Hepatol 19: 278–282
Cotton PB, Lehman G, Vennes J, Geenen J, Russell RC, Meyers WC, Liquory C, Nickl N (1991) Endoscopic sphincterotomy complications and their management: an attempt at consensus. Gastrointest Endosc 37: 383–393
Corbitt JD, Yusem SO (1994) Laparoscopic cholecystectomy with operative cholangiogram. Surg Endosc 8: 292–295
Sabharwal EJ, Minford EJ, Marson LP, Muir IM, Hill D, Auld CD (1998) Laparoscopic cholangiography: a prospective study. Br J Surg 85: 624–626
Duensing RA, Williams R, Collins JC, Wilson SE (1995) Managing choledocholithiasis in the laparoscopic era. Am J Surg 170: 619–623
Grace PA, Qureshi A, Burke P (1993) Selective cholangiography in laparoscopic cholecystectomy. Br J Surg 80: 244–246
Kelly TR (1980) Gallstone pancreatitis: the timing of surgery. Surgery 88: 345–350
Acosta MJ, Rossi R, Ledesma CL (1977) The usefulness of stool screening for diagnosing cholelithiasis in acute pancreatitis: a description of the technique. Am J Dig Dis 22: 168–172
Mahmud S, McGlinchey I, Kasem H, Nassar AH (2001) Radiological treatment of retained bile duct stones following recent surgery using glucagon. Surg Endosc 15: 1359–1360
Thompson MH, Tranter SE (2002) All-comers policy for laparoscopic exploration of the common bile duct. Br J Surg 89: 1608–1612
Hyser MJ, Chaudhry V, Byrne MP (1999) Laparoscopic transcystic management of choledocholithiasis. Am Surg 65: 606–609
Lorimer JW, Fairfull-Smith RJ (1995) Intraoperative cholangiography is not essential to avoid duct injuries during laparoscopic cholecystectomy. Am J Surg 169: 344–347
Davidoff AM, Pappas TN, Murray EA (1992) Mechanisms of major biliary injury during laparoscopic cholecystectomy. Ann Surg 215: 196–202
Mahmud S, Hamza Y, Nassar AH (2001) The significance of cystic duct stones encountered during laparoscopic cholecystectomy. Surg Endosc 15: 460–462
Mahmud S, Masaud M, Canna K, Nassar AHM (2002) Fundus-first laparoscopic cholecystectomy. Surg Endosc 16: 581–584
Wagner AJ, Sobrino MA, Traverso LW (2004) The long-term follow-up of patients with positive intraoperative cholangiograms during laparoscopic cholecystectomy. Surg Endosc 18: 1762–1765
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hamouda, A.H., Goh, W., Mahmud, S. et al. Intraoperative cholangiography facilitates simple transcystic clearance of ductal stones in units without expertise for laparoscopic bile duct surgery. Surg Endosc 21, 955–959 (2007). https://doi.org/10.1007/s00464-006-9127-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-006-9127-2