Abstract
This tribute article presents selected immunocytochemical and transmission electron microscope data on the location of ATP-gated P2X receptor in the rat brain, as studied in the 1990s in Prof G. Burnstock’s laboratory at University College London. There are examples of immuno-ultrastructural findings and introductory information about pre- and post-synaptic location of P2X receptors in the rat cerebellum and endocrine hypothalamus to support the concept of purinergic transmission in the central nervous system. Then findings of diverse immunoreactivity for P2X1, P2X2, P2X4, and P2X6 receptors associated with brain microvessels are shown, including vascular endothelium and pericytes as well as perivascular astrocytes and neuronal components. These findings imply the involvement of P2X receptors and hence purinergic signalling in the neurovascular unit, at least in microvessels in the rat cerebellum and hypothalamic paraventricular and supraoptic nuclei examined here. Various aspects of P2X receptors in brain microvessels are discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In one of his last contributions to his legendary research on purinergic signalling, Prof Geoffrey Burnstock presented an overview of the role of a purine adenosine 5′-triphospate (ATP) as a cotransmitter with glutamate, noradrenaline (NA), gamma-aminobutyric acid, acetylcholine and dopamine in the brain. He highlighted the role of ATP-gated P2X ionotropic receptors, and their involvement in fast synaptic transmission and synaptic plasticity (Burnstock 2020). For the account of Prof G. Burnstock’s contribution to the field of purinergic signalling, see Verkhratsky et al. (2020).
In the late 1990s circumstances allowed morphologists to be involved in research into the purinergic system. The antibodies for the detection of purinergic P2 receptors had been developed and were made available for immunohistochemical research. Consequently, the first immunocytochemical findings from transmission electron microscope (TEM) examination of the distribution of ATP-gated P2X receptors in the central nervous system (CNS) were reported (Lê et al. 1998; Llewellyn-Smith and Burnstock 1998; Loesch and Burnstock 1998a). These included a study of rat brain, particularly of the cerebellum and the hypothalamo-neurohypophysial system (Loesch and Burnstock 1998a, 2000, 2001; Loesch et al. 1999). It was shown that the immunoreactivity for P2X1 receptors was localized in a subpopulation of synapses established by varicosities of parallel fibres of granule cells and dendritic spines of Purkinje cells, while P2X1-immunoreactivity also appeared in some astrocyte processes (Loesch and Burnstock 1998a). In the hypothalamo-neurohypophysial system, best known for its production of the hormones vasopressin and oxytocin (see Renaud and Bourquet 1991), immunoreactivity for P2X2 and P2X6 receptors was shown. The immunoreactivity for these receptors was associated with (i) hypothalamic supraoptic and paraventricular endocrine neurones, neurosecretory and non-neurosecretory axons and dendrites and (ii) neurohypophyseal pituicytes and neurosecretory axons (Loesch et al. 1999; Loesch and Burnstock 2001). Numerous asymmetric axo-dendritic synapses were commonly observed, which involved P2X2-positive axons and unlabelled dendrites or the contrary—involved P2X2-positive dendrites and unlabelled axons. Axo-somatic synapses established by P2X2-positive axons on P2X2-positive endocrine cell bodies as well as on P2X2-negative somata were also observed (Loesch et al. 1999). These data therefore demonstrated the fine morphological basis of P2X receptors distribution, at least P2X2 and P2X6 receptors, in the hypothalamo-neurohypophysial system (Loesch and Burnstock 2001).
A pioneering TEM-immunocytochemical study of P2X receptors in the rat also revealed an association of the P2X3 receptor with sensory neurons of (i) trigeminal ganglia; (ii) cervical and lumbar dorsal horn of the spinal cord, where the receptor appeared in scalloped presynaptic terminals; and (iii) the solitary nucleus and tract, where P2X3-labelled buttons synapsed on P2X3-negative dendrites or axons (Llewellyn-Smith and Burnstock 1998); these studies consequently suggested that ATP can influence sensory signalling within the CNS. At the same time TEM findings of presynaptic expression of P2X4 receptors in rat cerebellar cortex, olfactory bulb glomeruli, and substantia galatinosa of the spinal cord confirm the selective presynaptic role of ATP in the modulation of neurotransmitter release in central sensory nerves, and the involvement of the P2X4 receptor in fast excitatory purinergic transmission (Lê et al. 1998). In fact, evidence suggested that ATP may act not only as a fast transmitter or co-transmitter in autonomic and sensory nerves but may also play a modulatory role acting presynaptically rather than solely postsynaptically in the nervous system (Cunha and Ribeiro 2000).
Early TEM studies of the rat brain also showed that apart from neurons or their components displaying immunoreactivity for P2X receptors, hence histologically supporting the phenomenon of purinergic synaptic transmission in the brain (see Burnstock 2007), the endothelial cells of small calibre blood vessels can also express immunoreactive P2X receptors (Loesch and Burnstock 2000; Loesch 2002). Earlier, the possibility of the release of ATP by the endothelium was reported in the isolated microvessels of the rat brain (Milner et al. 1995).
This tribute article presents findings of P2X receptors: P2X1, P2X2, P2X4 and P2X6 in the rat brain microvessels. This is presented in the general context of the cerebrovascular mechanisms of the control of cerebral blood flow involving perivascular astrocytes and neuronal cell profiles as well as vascular endothelium and pericytes. It is well-established that these cells contribute to the histology and physiology of the functional neurovascular units (NVU) connecting brain parenchyma with cerebral vasculature (Dore-Duffy and Cleary 2011; Dalkara and Alarkon-Martinez 2015; Netto et al. 2018; Hayden 2019). Here, the data are extracted from the studies Prof G Burnstock and myself carried out in 1997–2001. Some TEM images of the vascular and perivascular immunoreactivity for purinergic receptors in rat cerebellum and hypothalamic paraventricular and supraoptic nuclei are shown here for the first time with the hope these might add to the general morphological aspects of purinergic signalling in relation to brain microcirculation.
Materials and methods
All data presented here were obtained by examination of the brains of 3–4-month old Sprague-Dawley and Wistar rats (in accordance with the ethical approval and UK Animals (Scientific Procedures) Act 1986) following application of relevant P2X antibodies and the pre-embedding immunocytochemistry protocols for TEM, details of which have been previously published (see Loesch and Burnstock 1998a, 2000, 2001; Loesch et al. 1999). In brief, rabbit polyclonal antibodies to P2X1, P2X2, P2X3, P2X4 and P2X6 receptors were generated and characterized by Roche Bioscience, Palo Alto, USA (Oglesby et al. 1999; also see Chan et al. 1998; Xiang et al. 1998). Antibodies were generated against unique peptide sequences of receptor subtypes. The receptors were visualized using ExtrAvidin-horseradish peroxidase conjugate protocol, which was followed by the step with 3,3′diaminobenzidine (DAB) and then standard procedures of osmication, dehydration, embedment in Araldite, ultracutting, contrasting with uranyl acetate and lead citrate and examination with a JEM-1010 TEM.
Results
P2X receptors in the brain
In support of the immunocytochemical data described in the Introduction, here Fig. 1 demonstrates TEM examples of neural immunoreactivity for P2X receptors: P2X1, P2X2, P2X3, P2X4 and P2X6, and the involvement of these (or at least some) in the establishment of synaptic contacts. Apart from these findings, the focus of this article is on the distribution of P2X receptors: P2X1, P2X2, P2X4 and P2X6 in association with brain microvessels, here observed in the cerebellum and paraventricular and supraoptic nuclei.
TEM examples of neural immunoreactivity of P2X receptors in the rat brain. a A P2X1-positive postsynaptic dendritic spine (ds) in cerebellar molecular layer displaying immunoprecipitate (black) mostly at the postsynaptic density (arrow). Gl neuroglia processes, sv spherical agranular synaptic vesicles, pf parallel fibre. b A P2X2-positive presynaptic axon profile (Ax) adjacent to unlabelled dendrite (dn) in supraoptic nucleus; m mitochondrion. Note that obscuring effect of immunoprecipitate in Ax prevents clear identification of synaptic vesicles. c A P2X2-positive axon profile (Ax) with mostly agranular synaptic vesicles is establishing asymmetrical synapse with a P2X2-negative endocrine soma (black star) in supraoptic nucleus; Go Golgi complex, er endoplasmic reticulum. d A P2X3-positive dendrite (dn) in supraoptic nucleus is surrounded by P2X3-negative axon profiles (Ax) of which at least one is forming asymmetrical axo-dendritic synapse (arrow). e A P2X4-positive dendrite (dn) in cerebellar molecular layer is forming asymmetrical synapse with unlabelled axon profile (Ax). f A P2X6-positive dendrite (dn) in paraventricular nucleus is forming asymmetrical synapse with P2X6-negative axon profile; the latter displays small agranular synaptic vesicles and a few larger granular vesicles; m mitochondria. g Fragment of perivascular region of the neurohypophysis showing three neurosecretory axon profiles: P2X6-positive axon (Ax1) rich in microvesicles (a label mostly stains the membrane of the vesicles and axolemma), P2X6-partialy-stained axon (Ax2) filled with neurosecretory granules some of which are immunopositive (arrows), and one P2X6-negative axon (Ax3) containing mainly mitochondria (m). Also note a fragment of P2X6-positive pituicyte (P) with cytoplasm showing clusters of immunoprecipitate; ex extracellular matrix. Scale bars: a 100 nm, b, d–f 250 nm, c, g 0.5 μm. (Images adopted from a Loesch and Burnstock (1998a), with permission from Springer-Nature, Fig. 1c, p255; b, c Loesch et al. (1999), with permission from Springer-Nature, Fig. 2f, p498, Fig. 2j, p498; d-g A Loesch and G Burnstock unpublished studies performed in December 1997 and November 1998
P2X receptors and microvessels
P2X1. An example of the close relationship between immunoreactivity for P2X1 receptors and a microvessel of the rat cerebellar medulla is shown in Fig. 2a, b. Astrocyte processes are seen at the microvascular wall forming perivascular end-feet and displaying diffuse or patchy immunoreactivity for P2X1 receptor. Immunoreactive astroglia end-feet making tight overlap with no slits between them could be observed at higher TEM magnification (Fig. 2b). Microvascular endothelium and pericytes appeared to be immunonegative for P2X1 receptors.
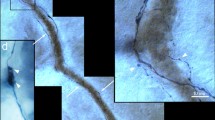
P2X1 receptor associated with rat brain microvessels seen at TEM level. a A microvessel in the cerebellar medulla displays immunoreactivity (black precipitate) for P2X1 receptor confined to perivascular astrocyte processes (As) end-feet, which embraces the capillary. Unlabelled endothelium (En), vessel lumen (lu), perivascular glial cell (Gl), and myelinated axons (mAx) can be seen; m mitochondria. b A microvessel in the cerebellar medulla shows an end-foot to end-foot overlap (a structure which helps seal the vessel) made by two astrocyte processes (As1 and As2); the overlap length of about 1.27 µm is demarcated by two black vertical arrows. Note that the astrocyte processes display clusters of P2X1-immunoreactivity (white short arrows); also note lightly labelled myelinated axons (mAx) and unmyelinated neural profiles (np), while endothelium (En), a fragment of a pericyte process (P), basement membrane (bm), mitochondria (m), and the vessel lumen (lu) are unlabelled. Scale bars: 0.5 µm. (Images from A Loesch and G Burnstock unpublished study performed in November 1998 (a, b))
P2X2. Perivascular regions of brain microvessels can display a rich presence of P2X2 receptor-immunoreactive neural and glial cells and/or their processes. In rat cerebellum, P2X2-immunoreactive dendrite profiles of Purkinje cells and astrocyte processes/end-feet can be seen contacting microvessels (Fig. 3a). Pericyte and endothelium of cerebellar microvessels showed no obvious immunoreactivity for P2X2 receptors. In contrast, some microvessels of the paraventricular and supraoptic nuclei of the hypothalamus showed endothelial immunoreactivity for P2X2 receptors, but P2X2-negative endothelial cells, pericytes, and astrocyte profiles were also observed (Fig. 3b, c). At times, however, immunoreactivity for P2X2 receptors could be seen in pericytes of microvessels in the paraventricular nucleus (Fig. 3d). In this case, a patchy distribution of P2X2-immunoreactivity seemed concentrated at the abluminal (adventitial) regions of the pericyte cytoplasm. This coincided with the presence of P2X2-negative perivascular axon terminals containing synaptic vesicles, including numerous small agranular and some granular vesicles.
P2X2 receptor associated with rat brain microvessels seen at TEM level. a Note that a microvessel in cerebellar cortex is accompanied by P2X2-immunoreactive (black immunoprecipitate), Purkinje cell proximal dendrite (Pd), and astrocyte end-feet (As), while vascular endothelium (En), pericyte (P), and axon profiles (Ax) are immunonegative; lu vessel lumen; m mitochondria; er endoplasmic reticulum. b A wall of microvessel in the paraventricular nucleus shows P2X2-immunoreactive (black stain) and P2X2-negative endothelial cells (En). Pericyte (P) with visible nucleus and astrocyte processes (As) are immunonegative; note that pericyte is surrounded by basement membrane (arrows); lu lumen. c A fragment of microvessel in the supraoptic nucleus displays P2X2-positive and P2X2-negative endothelial cells (En); immunoreactivity is also visible at the endothelial cells junction (arrow), while adjoining pericyte (P), astrocyte (As) and neural profiles (np) are immunonegative; lu lumen. d A fragment of microvessel in the paraventricular nucleus shows P2X2-positive pericyte with immunoprecipitate largely clustered at the cell abluminal site facing an immunonegative axon terminal (Ax) containing small agranular vesicle (av), a few granular vesicles (gv), and one mitochondrion (m); endothelium (En) appears to be P2X2-negative. Note a basement membrane (bm) around pericyte; lu lumen. Scale bars: a 0.5 μm, b, c 1 µm, and d 250 nm. (Images from A Loesch and G Burnstock unpublished data from a study performed in November 1998 (a–d))
P2X4. The appearance of immunoreactivity for P2X4 receptors appeared varied when comparing microvessels of cerebellum and hypothalamus. In the cerebellum both neural and glial perivascular components displayed P2X4-receptor immunoreactivity, while the endothelium and pericyte were unlabelled (Fig. 4a). In the hypothalamus, however, microvascular endothelium was immunoreactive for the P2X4 receptor, as also was the perivascular astrocyte; the immunoprecipitate was unevenly (in patches) distributed in these cells (Fig. 4b). No pericyte positive for the P2X4 receptor was observed.
P2X4 (a, b) and P2X6 (c, d) receptors associated with rat brain microvessels seen at TEM level. a Note P2X4-positive (black immunoprecipitate) astrocyte (As) embracing a microvessel wall in cerebellar cortex. Also note P2X4-positive neural profiles (np), while endothelium (En) and pericyte (P) are P2X4-negative; lu vessel lumen, m mitochondria. b A fragment of microvessel in the supraoptic nucleus shows P2X4-positive endothelium (En) with immunoprecipitate mostly clustered at the cell abluminal site (white arrows) facing an immunonegative pericyte (P) containing mitochondria (m); also note a cluster of P2X4-immunoprecipitate (black arrow) in astrocyte end-foot facing the pericyte; the latter is enveloped by a basement membrane (bm); lu lumen. c A microvessel in paraventricular nucleus displaying thin layer of intima; arrows point to junctions between P2X6-positive (right) and P2X6-negative (left) endothelial cells. Pericyte (P) containing dense body/lipofuscin granule (db) is P2X6-negative. d A fragment of microvessel in paraventricular nucleus shows juxtaposition of P2X6-positive astrocyte end-feet (As) with invaginated cell membrane facing immunonegative pericyte; also note P2X6-immunonegative endothelium (En), basement membrane (bm), mitochondria (m) and vessel lumen (lu). Scale bars: a 0.5 µm, b 250 nm, c 2 µm, and d 0.5 µm. (Images from A Loesch and G Burnstock unpublished studies performed in November and December 1997 (a, b), November 1998 (c), and February 2000 (d))
P2X6. Examples of immunoreactivity for P2X6 receptors were obtained from the study of the paraventricular nucleus. It was evident that the immunoreactivity for P2X6 receptors was confined to some of the microvascular endothelium (Fig. 4c) and perivascular astroglia end-feet (Fig. 4d). The cell membrane of P2X6-immunoreactive astrocyte end-feet could be invaginated; this was seen at the sites of presence of immuno-negative pericytes and/or endothelial cells (Fig. 4d).
Discussion
The immunocytochemical TEM data showed that P2X receptors are associated with brain microvessels. These findings extends the original TEM immunocytochemical observation of the P2X2 receptor in the rat brain microvessels (Loesch and Burnstock 2000) providing a further immuno-morphological basis for the diverse distribution of P2X receptors in the endothelium, pericyte and perivascular astroglia processes associated with brain microvessels. Here, some of the images disply a possible morphological relationship between the endothelium, pericyte, astrocyte and neural elements (as part of NVU), as well as the potential for purinergic signalling in and at the microvessels of rat brain. The possibility cannot be excluded that the immunoreactivity for either of P2X4 or P2X6 receptors observed in the present study might in fact indicate the presence of heteromeric P2X4/6 receptors. This is because P2X4 or P2X6 receptors are usually assembled as heteromeres P2X4/6 receptors and have trafficking properties (Collo et al. 1996). By the same token, immunoreactivity for P2X2 receptors might suggest the presence of heteromeric P2X2/6 receptors (Bobanovic et al. 2002; Robinson and Murrell-Lagnado 2013).
Endothelium
Here, endothelium showed a diverse, heterogeneous distribution of P2X receptors even within the same cross-sectional profile of a microvessel, where, for example, both P2X2-positive and P2X2-negative endothelial cells coexisted in microvessels of paraventricular and supraoptic nuclei. This heterogeneous distribution of P2X receptors might be related to the microvessel-specific role. It is now clear that the distribution of P2X receptors varies from vessel to vessel and also there are species-specific differences in receptor subtype expressions (Burnstock and Ralevic 2014; Burnstock 2017a). The initial studies of purinergic receptor distribution included immunofluorescence laser confocal microscopy of the P2X1 receptor in rat mesenteric artery and veins in urinary bladder, and of the P2X2 receptor in rat aorta (Hansen et al. 1999); the P2X3 receptor in endothelial cells of rat thymus (Glass et al. 2000), and the P2X3, P2X4 and P2X7 receptors in endothelial cells of rat thyroid blood vessels (Glass and Burnstock 2001). A co-labelling study of freshly harvested human umbilical vein endothelial cells (HUVECs) at the confocal microscope and TEM levels, as well as the application of Western blotting analysis revealed that the P2X4 and P2X6 receptors are strongly co-localized with the cell adhesion molecule VE-cadherin on plasma membranes at cellular adherens junctions. It also appeared that the receptors became internalized specifically after decreasing the extracellular calcium ([Ca2+]) level, therefore being involved in modulating adhesion junctions in human endothelial cells (Glass et al. 2002). Many more aspects of purinergic signalling in the cardiovascular system including the vasoactive role of ATP and purinoceptors can be found in the elegant publication by Ralevic and Burnstock (1998).
In the original TEM study of P2X2 receptors in rat brain microvessels, we suggested the possibilities that these receptors may regulate the formation of endothelial gap and/or tight junctions influencing the blood-brain barrier (BBB) or modulate the contractility of capillary endothelial cells (Loesch and Burnstock 2000). Here, immunoreactivity for P2X2, P2X4 and P2X6 receptors detected in endothelial cells of hypothalamic microvessels also suggested that these receptors can interact with circulating ATP—possibly deriving from neighbouring endothelial cells (Burnstock 1990, 2010; also see Vanhoutte 2000).
It is now well-established that the endothelial distribution of P2 receptors is related to ATP effects on the vasculature and its involvement in control of vascular tone and remodelling (Burnstock and Ralevic 2014). In general terms, ATP released from perivascular sympathetic nerves causes vasoconstriction via the P2X1, 2 and 4 receptors on vascular smooth muscle of the media, while ATP released from endothelial cells during shear stress and hypoxia acts on P2X1, 2, 3 and 4 and P2Y1, 2, 4 or 11 receptors on nearby endothelial cells to stimulate the production of a potent vasorelaxant nitric oxide (NO) and endothelium-derived hyperpolarizing factor/s (EDHF), which subsequently dilate vessel/s (Burnstock and Ralevic 2014). It can be mentioned that a number of studies on ATP release from endothelial cells were performed in Prof Burnstock’s lab at UCL in the early 1990s. These studies have shown that ATP is released both from the in vivo and freshly isolated endothelial cells during hypoxia or changes of perfusion flow rate. Initially, release experiments were performed on freshly isolated rabbit aortic endothelial cells (Milner et al. 1990a, 1992; Bodin et al. 1991; Bodin and Burnstock 2001), freshly harvested HUVECs (Milner et al. 1990b; Bodin and Burnstock 1995), rat mesenteric arterial bed (Ralevic et al. 1992) and the rabbit cerebral vasculature perfused with a perfluorocarbon emulsion, a substitute for erythrocytes delivering oxygen to the brain (Domer et al. 1993). The latter study was particularly important in relation to the ATP system in the brain vasculature. It has supported the view that ATP and other vasoactive agents, such as substance P, endothelin-1 and arginine vasopressin, are released by vascular endothelial cells during changes in the rate of vascular perfusion, therefore contributing to changes in local cerebrovascular tone (Domer et al. 1993). Chronic sensory denervation of perivascular nerves with the neurotoxin capsaicin also leads to changes in the release of ATP, as well as substance P, endothelin and vasopressin of endothelial origin from rat brain microvessels during increased flow (Milner et al. 1995). Therefore, along with ATP other vasoactive substances also may play a role in maintaining cerebrovascular tone, and this includes NO generated by cerebrovascular endothelium and perivascular nerves and/or neuronal processes of central origin (Bredt et al. 1990; Iadecola et al. 1993; Nozaki et al. 1993; Loesch and Burnstock 1996, 1998b). Importantly, NO can also be released by brain glial cells including astrocytes (Murphy et al. 1993), as well as by the brain microvascular pericytes, particularly during inflammatory processes when these cells can secrete cytokines and chemokines (Kovac et al. 2011).
Astroglia and pericytes
Here, immunoreactivity for P2X receptors was displayed by perivascular astrocyte end-feet (P2X1,2,4 and 6) and to a lesser extent by pericytes (P2X2), suggesting that these cells are prepared for the action of extracellular ATP to influence intracellular Ca2+ concentration ([Ca2+]i). Hypothetically, the ATP action via P2X receptors could coexists with the action of glutamate that escaped from the synaptic clefts and interact with metabotropic glutamate receptors (mGluRs) on astrocytes increasing [Ca2+]i in these cells (Porter and McCarthy 1996). In fact, both ATP and glutamate can be released by astrocytes themselves as a part of the astrocytes-microglia signalling system (Verderio and Matteoli 2001), and also participating in astrocyte-neuron bidirectional cross-talk (Araque et al. 1999; Bezzi et al. 1999). Studies of primary cultures of hippocampal astrocytes of embryonic rat pups revealed two types of vesicles in the cells for storage and release of either: (i) ATP—stored in large dense-core vesicles of ~ 104 nm diameter or (ii) glutamate—stored in small agranular vesicles of ~ 56 nm diameter (Coco et al. 2003). Whether glutamate and ATP initiate relaxation or constriction of microvessels seems partially dependent on the pre-existing vascular tone (Blanco et al. 2008). Evidence also suggests that ATP acting on astrocytic P2X1 receptors evokes the release of prostaglandin E2 (PGE2), which subsequently relaxes pericytes (Mishra et al. 2016). Unfortunately, it is unknown in the present study whether P2X1-positive astrocytes of microvessels of cerebellar medulla were able to release PGE2 or any other agent. Complex morpho-functional studies of rat and mouse brain cortical slices, including whole-cell patch-clamp experiments, revealed that, for example, NA-stimulated elevations of [Ca2+]i in astrocytes can regulate arteriole diameter and that astrocyte Ca2+ waves cause vascular constrictions, the extent of which are related to astrocyte end-feet participation (Zonta et al. 2003; Mulligan and MacVicar 2004). As NA is a cotransmitter with ATP in central and autonomic sympathetic nerves (Sperlágh et al. 1997; Poelchen et al. 2001; Burnstock and Verkhratsky 2010; Burnstock 2020), here the possibility cannot be excluded that axon terminals observed close to pericyte might be a source of NA and ATP.
Here, the relatively modest expression of P2X receptors by pericytes, as only P2X2 immunoreactive receptors were observed in abluminal cytoplasm of pericytes of the hypothalamic microvessels, is nevertheless, worth to notice. This is because the close location of axon terminals to pericyte suggests that the axon terminals might be a source of ATP interacting with pericyte-associated P2X2-receptors. This is an interesting observation in the context of the elegant studies of the rat isolated retina and cerebellar slices by Peppiatt and colleagues (2006), showing that superfused ATP in the retina and NA in the cerebellum, resulted in constriction of capillaries by pericytes, while glutamate reversed the constriction produced by NA. Constriction of capillaries is caused when pericyte [Ca2+]i is elevated, which leads to activation of intracellular contractile proteins, hence causing constriction of pericyte processes around the capillary (Peppiatt et al. 2006; Chang et al. 2018). According to Peppiatt et al. (2006) the spread of constriction is not produced by a glial Ca2+ wave, but rather by a direct contact between neuropil elements and pericytes, which can render pericyte-capillary constriction. In light of the above data, the current finding of axon terminals close to the basement membrane covering P2X2 receptor-positive pericyte is interesting, as these terminals contain a number of synaptic vesicles, some of which perhaps store ATP (Fig. 3d). This histological feature might be of relevance to the purinergic involvement in local control of contractility of pericyte and the host microvessel. It can be noted, however, that pericytes display different sensitivities to purinergic stimulation (Peppiatt et al. 2006).
In fact, the vasoregulatory mechanisms involving ATP are complex, as it has been shown in the study of rat brain penetrating arterioles, which are precapillary microvessels. It has been shown that the microapplication of ATP to the cerebral penetrating arterioles produced a biphasic response, which in the first instance was constriction followed by dilatation, where the latter was dependent upon both the endothelium and cytochrome P450 metabolites (Dietrich et al. 2009; also see Jensen and Holstein-Rathlou 2013). Experiments with local injection of ATP into the somatosensory barrel cortex of transgenic NG2-DsRed mice showed that ATP-induced capillary constriction depends on the capillary order and the activation of purinergic P2 receptors, including those pericyte-associated P2 receptors (Cai et al. 2018).
Studies of adult rat retinal microvessels showed that extracellular ATP induces depolarizing changes in the ionic currents, increases calcium levels and causes pericytes to contract via functional pericyte-associated P2X7 receptors (Kawamura et al. 2003). The activation of P2X7 receptors not only alters the physiology of individual pericytes but also inhibits gap junction communication within the microvascular network, and therefore, it also regulates the spatial dynamics of the vasomotor response. However, the effects of ATP on pericytes appear to be mediated via multiple purinergic receptors, including P2X receptors and possibly also uridine-5′-triphosphate (UTP)-binding P2Y receptors (Kawamura et al. 2003; Peppiatt et al. 2006; Cai et al. 2018). Here, the detection of immunoreactivity of P2X2 receptors in pericytes, supports the evidence for pericyte-associated purinergic signalling.
But what role pericytes may play in the context of the P2X receptor-negative pericyte ‘sandwiched’ between the P2X4-positive perivascular astrocyte end-foot and the P2X4-positive intimal endothelium, an observation presented here in the hypothalamic supraoptic nucleus? Is it possible that in this case the P2X-negative pericyte is in fact able to release ATP to act on the adjacent P2X-positive end-foot and/or P2X-positive endothelium? So far there have been no reports of pericytes releasing ATP. However, studies of the metabolism of placental pericytes transiting from a quiescent to a proliferative state or during cell differentiation, which requires an increased uptake of glucose, showed that pericytes can produced ATP outside mitochondria through glycolysis; however, this ATP appears to primarily be used to meet pericyte energy demands (Cantelmo et al. 2016; Nwadozi et al. 2020)
Strikingly, pericytes in the brain seem to be more sensitive than endothelium to certain conditions. For instance, in rat ischemic cerebellum (evoked by the occlusion of the middle cerebral artery), a complex signalling can be observed leading to pericyte-elicited constriction of cerebellar microvessels, and subsequent death of the pericyte, which causes further and irreversible microvessel constriction and damage to the BBB (Hall et al. 2014). Here, there are no presentations of ischemic cerebrovascular pericyte or examples of pericytes immunolabelled either for the characteristic NG2 proteoglycan, or the platelet-derived growth factor receptor beta (PDGFRβ) involved in pericyte proliferation (Ozerdem et al. 2001; Armulik et al. 2005, 2010; Hall et al. 2014).
Finally, attention was given to the hypothalamo-neurohypophysial system, which is well-known to be influenced by ATP actions and P2X receptors (Mori et al. 1992; Chen et al. 1994; Sperlágh et al. 1997, 1999; Kapoor and Sladek 2000). The elegant fluorescence immunohistochemical study by Guo et al. (2009) showed that P2X2-6 receptors are richly but differentially expressed on vasopressin- and oxytocin-containing neurons in the paraventricular and supraoptic nuclei of rat hypothalamus. These immono-neuroanatomical findings provided valuable information on the possible functional interactions between the purinergic system and both vasopressinergic and oxytocinergic systems in the endocrine hypothalamus. For more details on purinergic signalling in the hypothalamo-neurohypophysial system, see Lemos et al. (2018).
Conclusions
This tribute article has focused on the description of immunoreactivity for P2X receptors associated with brain microvessels in the cerebellum and endocrine hypothalamus observed at TEM level. Immunoreactivity for P2X1, P2X2, P2X4 and P2X6 receptors was variously expressed in the endothelium, pericyte and perivascular astrocyte and neuronal elements. The possibility that microvessels of various orders from different regions of the brain are differently equipped in ATP mechanisms cannot be excluded. This perhaps depends on the presence or absence of specific P2X receptor subtypes on NVU involving vascular endothelium and pericytes as well as perivascular astroglia end-feet and neuronal components.
Reflections. It should be stressed that Professor Burnstock’s dedication to research on purinergic signalling did not focus on the research alone. He was also promoting the therapeutic potential of purinergic signalling and was involved in the development of new generation drugs for various diseases that involve dysregulation of the purinergic system. Prof G. Burnstock was very much interested in ATP signalling and its dysregulation in the brain in conditions like injury, stroke, ischemia, chronic pain, Alzheimer’s disease (AD), inflammation and many other conditions (the list is long) (Burnstock et al. 2011; Burnstock 2017b, c; Burnstock and Knight 2018).
To follow this interest, the question can be asked if the P2X receptors that have been identified on brain microvessels might be a potential therapeutic target, for example, in ischaemic stroke where mechanisms of vasoconstriction might dominate. In such conditions the persistent constriction and death of pericytes can occur, preventing blood flow and/or reflow (Cai et al. 2018). One of the possibilities is the selective targeting of the pericyte-associated P2X receptors to influence purinergic signalling initiated by NVU’s vasoconstrictor agents of perivascular nerves and glia (see Peppiatt et al. 2006). In fact, vasoactive properties of microvessels are complex involving all NVU components including microvascular endothelium. An earlier study in Prof G. Burnstock’s group at UCL showed that chronic depletion of sensory innervation leads to altered release of two endothelium-dependent vasodilators, ATP and substance P from the brain microvasculature including arterioles, venules and capillaries (Milner et al. 1995); no data on pericytes was presented there. But it is likely that any defect in microvasculature might affect pericytes and consequently the maintenance of BBB and blood flow (Armulik et al. 2010). Therefore, in some neurological diseases or stroke, pericytes can be a therapeutic target in order to preserve the BBB and to increase cerebral blood flow (Cheng et al. 2018). The relations between NVU components became more complex in pathology. For example, the most recent post-mortem study of various neurological stages of AD showed that there are distinct immuno-structural changes in NVU components in cortical and hippocampal samples suggesting functional deficits in the brain vasculature (Kirabali et al. 2020). But there are also some contradicting results. Stereological and two-photon imaging studies of post-mortem frozen AD brain samples revealed increased capillary density with a normal pericyte population at least in the frontal cortex (Fernandez-Klett et al. 2020). These examples of studies on AD show how difficult it would be to comprise various or even opposite research data when developing treatment to target pathological changes. Some advice on how to approach these difficult problems can be found in the scientific knowledge embedded in Prof Burnstock’s research publications.
I believe that the light and electron microscopy combined with immunohistochemical methods were very much appreciated by Professor G. Burnstock. This is evident in many of his publications showing structural and immunohistochemical details relevant to our better understanding of biological functions, including of the cells associated with purinergic system.
References
Araque A, Parpura V, Sanzgiri RP, Haydon PG (1999) Tripartite synapses: glia, the unacknowledged partner. Trends Neurosci 22:208–215
Armulik A, Abramsson A, Betsholtz C (2005) Endothelial/pericyte-interactions. Circ Res 97:512–523
Armulik A, Genove G, Mäe M, Nisancioglu MH, Wallgard E, Niaudet C, He L, Norlin J, Lindblom P, Strittmatter K, Johansson BR, Betsholtz C (2010) Pericytes regulate the blood–brain barrier. Nature 468:557–561
Bezzi P, Domercq M, Vesce S, Volterra A (1999) Neuron-astrocyte cross-talk during synaptic transmission: physiological and neuropathological implications. Progr Brain Res 132:255–265
Blanco VM, Stern JE, Filosa J (2008) Tone-dependent vascular responses to astrocyte-derived signals. Am J Physiol Heart Circ Physiol 294:H2855–H2863
Bobanovic LK, Royle SL, Murrell-Lagnado RD (2002) P2X receptor trafficking in neurons is subunit specific. J Neurosci 22:4814–4824
Bodin P, Burnstock G (1995) Synergistic effect of acute hypoxia on flow-induced release of ATP from cultured endothelial cells. Experientia 51:256–259
Bodin P, Burnstock G (2001) Evidence that release of adenosine triphosphate from endothelial cells during increased shear stress is vesicular. J Cardiovasc Pharmacol 38:900–908
Bodin P, Bailey DJ, Burnstock G (1991) Increased flow-induced ATP release from isolated vascular endothelial but not smooth muscle cells. Br J Pharmacol 103:1203–1205
Bredt DS, Hwang PM, Snyder SH (1990) Localization of nitric oxide synthase indicating a neural role for nitric oxide. Nature 347:768–770
Burnstock G (1990) Dual control of local blood flow by purines. Ann NY Acad Sci 603:31–44
Burnstock G (2007) Physiology and pathophysiology of purinergic neurotransmission. Physiol Rev 67:659–797. https://doi.org/10.1152/physrev.00043.2006
Burnstock G (2010) Control of vascular tone by purines and pyrimidines. Br J Pharmacol 161:527–529
Burnstock G (2017a) Purinergic signaling in the cardiovascular system. Circ Res 120:207–228
Burnstock G (2017b) Purinergic signalling and neurological diseases: an update. CNS Neurol Disord Drug Targets 16:257–265
Burnstock G (2017c) Purinergic signalling: therapeutic developments Front Pharmacol 8:661. https://doi.org/10.3389/fphar.2017.00661
Burnstock G (2020) Introduction to purinergic signalling in the brain. In: Barańska J (ed) Glioma signaling. Advances in experimental medicine and biology, vol 1202. Springer, Cham, pp 1–12 https://doi.org/10.1007/978-3-030-30651-9_1
Burnstock G, Knight G (2018) The potential of P2X7 receptors as a therapeutic target, including inflammation and tumour progression. Purinergic Signal 14:1–18
Burnstock G, Ralevic V (2014) Purinergic signaling and blood vessels in health and disease. Pharmacol Rev 66:102–192
Burnstock G, Krugel U, Abbracchio MP, Illes P (2011) Purinergic signalling: from normal behaviour to pathological brain function. Prog Neurobiol 95:229–274
Burnstock G, Verkhratsky A (2010) Vas deferens - a model used to establish sympathetic cotransmission. Trends Pharmacol Sci 31:131–139
Cai C, Fordsmann JC, Jensen SH, Gesslein B, Lønstrup M, Hald BO, Zambach SA, Brodin B, Lauritzen MJ (2018) Stimulation-induced increases in cerebral blood flow and local capillary vasoconstriction depend on conducted vascular responses. PNAS 115:E5796–E5804
Cantelmo AR, Conradi L-C, Brajic A, Goveia J, Kalucka J, Pircher A, Chaturvedi P, Hol J, Thienpont B, Teuwen L-A, Schoors S, Boeckx B, Vriens J, Kuchnio A, Veys K, Cruys B, Finotto L, Treps L, Stav-Noraas TE, Bifari F, Stapor P, Decimo I, Kampen K, De Bock K, Haraldsen G, Schoonjans L, Rabelink T, Eelen G, Ghesquière B, Rehman J, Lambrechts D, Malik AB, Dewerchin M, Carmeliet P (2016) Inhibition of the glycolytic activator PFKFB3 in endothelium induces tumor vessel normalization, impairs metastasis, and improves chemotherapy. Cancer Cell 30:968–985
Chan CM, Unwin RJ, Oglesby IB, Ford APDW, Townsend-Nicholson A, Burnstock G (1998) Localization of the P2X1purinoceptors by autoradiography and immunochistochemistry in rat kid-neys. Am J Physiol 274:F799–F804
Chen ZP, Levy A, Lightman SL (1994) Activation of specific ATP receptors induces a rapid increase in intracellular calcium ions in rat hypothalamic neurons. Brain Res 641:249–256
Cheng J, Korte N, Nortley R, Sethi H, Tang Y, Attwell D (2018) Targeting pericytes for therapeutic approaches to neurological disorders. Acta Neuropathol 136:507–523
Coco S, Calegari F, Pravettoni E, Pozzi D, Taverna E, Rosa P, Matteoli M, Verderio C (2003) Storage and release of ATP from astrocytes in culture. Biol Chem 278:1354–1362. https://doi.org/10.1074/jbc.m209454200
Collo G, North RA, Kawashima E, Merlo-Pich E, Neidhart S, Surprenant A, Buell G (1996) Cloning of P2X5 and P2X6 receptors and the distribution and properties of an extended family of ATP-gated ion channels. J Neurosci 16:2495–2507
Cunha RA, Ribeiro JA (2000) ATP as a presynaptic modulator. Life Sci 68:119–137
Dalkara T, Alakron-Martinez L (2015) Cerebral microvascular pericytes and neurogliovascular gnaling in health and disease. Brain Res 1623:3–17
Dietrich HH, Horiuchi T, Xiang C, Hongo K, Falck JR, Dacey RG Jr (2009) Mechanism of ATP-induced local and conducted vasomotor responses in isolated rat cerebral penetrating arterioles. J Vasc Res 46:253–264
Domer FR, Alexander B, Milner P, Bodin P, Burnstock G (1993) Effect of changes in rate of vascular perfusion on release of substances into the effluent from the brain of the rabbit. Brain Res 630:88–94
Dore-Duffy P, Cleary K (2011) Morphology and properties of pericytes. Methods Mol Biol 686:49–68
Fernandez-Klett F, Brandt L, Fernández-Zapata C, Abuelnor B, Middeldorp J, Sluijs JA, Curtis M, Faull R, Harris LW, Bahn S, Hol EM, Prille J (2020) Denser brain capillary network with preserved pericytes in Alzheimer’s disease. Brain Pathol 2020:1–1. https://doi.org/10.1111/bpa.12897
Glass R, Burnstock G (2001) Immunohistochemical identification of cells expressing ATP-gated cation channels (P2X receptors) in the adult rat thyroid. J Anat 198:569–579
Glass R, Townsend-Nicholson A, Burnstock G (2000) P2 receptors in the thymus: expression of P2X and P2Y receptors in adult rats, an immunohistochemical and in situ hybridisation study. Cell Tissue Res 300:295–306
Glass R, Loesch A, Bodin† P, Burnstock G, (2002) P2X4 and P2X6 receptors associate with VE-cadherin in human endothelial cells. CMLS, Cell Mol Life Sci 59:870–881
Guo W, Sun J, Xu X, Bunstock G, He C, Xiang Z (2009) P2X receptors are differentially expressed on vasopressin and oxytocin-containing neurons in the supraoptic and paraventricular nuclei of rat hypothalamus. Histochem Cell Biol 131:29–41
Hall CN, Reynell C, Gesslein B, Hamilton NB, Mishra A, Sutherland BA, O’Farrell FM, Buchan AM, Lauritzen M, Attwell D (2014) Capillary pericytes regulate cerebral blood flow in health and disease. Nature 508:55–60
Hansen MA, Dutton JL, Barden BVJ, JA, Bennett MR, (1999) P, (purinergic) receptor distributions in rat blood vessels. J Anat Nerv Syst 75:147–155. https://doi.org/10.1016/S0165-1838(98)00189-1
Hayden MR (2019) Hypothesis: astrocyte foot processes detachment from the neurovascular unit in female diabetic mice may impair modulation of information processing-six degrees of separation. Brain Sci 9:83. https://doi.org/10.3390/brainsci9040083
Iadecola C, Beitz AJ, Renno W, Xu X, Mayer B, Zhang F (1993) Nitric oxide synthase-containing neural processes on large cerebral arteries and cerebral microvessels. Brain Res 606:148–155
Jensen LJ, Holstein-Rathlou NH (2013) The vascular conducted response in cerebral blood flow regulation. J Cereb Blood Flow Metab 33:649–656
Kapoor JR, Sladek CD (2000) Purinergic and adrenergic agonists synergize in stimulating vasopressin and oxytocin release. J Neurosci 20:8868–8875
Kawamura H, Sugiyama T, Wu DM, Kobayashi M, Yamanishi S, Katsumura K, Puro DG (2003) ATP: a vasoactive signal in the pericyte-containing microvasculature of the rat retina. J Physiol 551(Pt 3):787–799
Kirabali T, Rust R, Rigorri S, Siccoli A, Nitsch RM, Kulic L (2020) Distinct changes in all major components of the neurovascular unit across different neuropathological stages of Alzheimer’s disease. Brain Pathol. https://doi.org/10.1111/bpa.12895
Kovac A, Erickson MA, Banks WA (2011) Brain microvascular pericytes are immunoactive in culture: cytokine, chemokine, nitric oxide, and LRP-1 expression in response to lipopolysaccharide. J Neuroinflammation 8:139. https://doi.org/10.1186/1742-2094-8-139
Lê KT, Villeneuve P, Ramjaun AR, Mcpherson PS, Beaudet A, Séguéla P (1998) Sensory presynaptic and widespread somatodendritic immunolocalization of central ionotropic P2X ATP receptors. Neuroscience 83:177–190
Lemos JR, Custer EE, Ortiz-Miranda S (2018) Purinergic receptor types in the hypothalamic-neurohypophysial system. J Neuroendorrinol 30:1–8
Llewenllyn-Smith IJ, Burnstock G (1998) Ultrastructural localization of P2X3 receptors in rat sensory neurons. NeuroReport 9:2545–2550
Loesch A (2002) Perivascular nerves and vascular endothelium: recent advances. Histol Histopathol 17:591–597
Loesch A, Burnstock G (1996) Ultrastructural study of perivascular nerve fibres and endothelial cells of the rat basilar artery immunolabelled with monoclonal antibodies to neuronal and endothelial nitric oxide synthase. J Neurocytol 25:525–534
Loesch A, Burnstock G (1998a) Electron-immunocytochemical localization of P2X1 receptors in the rat cerebellum. Cell Tissue Res 294:253–260
Loesch A, Burnstock G (1998b) Perivascular nerve fibres and endothelial cells of the rat basilar artery: immuno-gold labelling of antigenic sites for type I and type III nitric oxide synthase. J Neurocytol 27:197–204
Loesch A, Burnstock G (2000) Ultrastructural localisation of ATP-gated P2X2 receptor immunoreactivity in vascular endothelial cells in rat brain. Endothelium 7:93–98
Loesch A, Burnstock G (2001) Immunoreactivity to P2X6 receptors in the rat hypothalamo-neurohypophysial system: An ultrastructural study with extravidin and colloidal gold-silver labelling. Neuroscience 106:621–631
Loesch A, Miah S, Burnstock G (1999) Ultrastructural localisation of ATP-gated P2X2 receptor immunoreactivity in the rat hypothalamo-neurohypophysial system. J Neurocytol 28:495–504
Milner P, Bodin P, Loesch A, Burnstock G (1990) Rapid release of endothelin and ATP from isolated aortic endothelial cells exposed to increased flow. Biochem Biophys Res Commun 170:649–656
Milner P, Kirkpatrick KA, Ralevic V, Toothill V, Pearson JD, Burnstock G (1990) Endothelial cells cultured from human umbilical vein release ATP, substance P and acetylcholine in response to increased flow. Proc Roy Soc B 241:245–248
Milner P, Bodin P, Loesch A, Burnstock G (1992) Increased shear stress leads to differential release of endothelin and ATP from isolated endothelial cells from 4- and 12-month-old male rabbit aorta. J Vasc Res 29:420–425
Milner P, Bodin P, Loesch A, Burnstock G (1995) Interactions between sensory perivascular nerves and the endothelium in brain microvessels. Int J Microcirc 15:1–9
Mishra A, Reynolds JP, Chen Y, Gourine AV, Rusakov DA, Attwell D (2016) Astrocytes mediate neurovascular signaling to capillary pericytes but not to arteriols. Nat Neurosci 19:1619–1627
Mori M, Tsushima H, Matsuda T (1992) Antidiuretic effects of purinoceptor agonists injected into the hypothalamic paraventricular nucleus of water-loaded, ethanol-anesthetized rats. Neuropharmacol 31:585–592
Mulligan SJ, MacVicar BA (2004) Calcium transients in astrocyte endfeet cause cerebrovascular constrictions. Nature 431:195–199
Murphy S, Simmons ML, Agullo L, Garcia A, Feinstein DL, Galea E, Reis DJ, Minc-Golomb D, Schwartz JP (1993) Synthesis of nitric oxide in CNS glial cells. Trends Neurosci 16:323–328
Netto JP, Iliff J, Stanimirovic D, Krohn KA, Hamilton B, Varallyay C, Gahramanov S, Daldrup-Link H, d’Esterre C, Zlokovic B, Sair H, Lee Y, Taheri S, Jain R, Panigrahy A, Reich DS, Drewes LR, Castillo M, Neuwelt EA (2018) Neurovascular unit: basic and clinical imaging with emphasis on advantages of ferumoxytol. Neurosurgery 82:770–780
Nozaki K, Moskowitz MA, Maynard KI, Koketsu N, Dawson TM, Bredt DS, Snyder SH (1993) Possible origins and distribution of immunoreactive nitric oxide synthase-containing nerve fibers in cerebral arteries. J Cereb Blood Flow Metab 13:70–79
Nwadozi E, Rudnicki M, Haas TL (2020) Metabolic coordination of pericyte phenotypes: therapeutic implications. Front Cell Dev Biol 8:77. https://doi.org/10.3389/2Ffcell.2020.00077
Oglesby IB, Lachnit WG, Burnstock G, Ford APDW (1999) Subunit specificity of polyclonal antisera to the carboxy terminal regions of the P2X receptors, P2X1 through P2X7. Drug Dev Res 47:189–195
Ozerdem U, Grako KA, Danhil-Huppe K, Monsov E, Stallcup WB (2001) NG2 proteoglycan is expressed exclusively by mural cells during vascular morphogenesis. Dev Dyn 222:218–227
Peppiatt CM, Howarth C, Mobbs P, Attwell D (2006) Bidirectional control of CNS capillary diameter by pericytes. Nature 443:700–704
Poelchen W, Sieler D, Wirkner K, Illes P (2001) Co-transmitter function of ATP in central catecholaminergic neurons of the rat. Neuroscience 102:593–602
Porter JT, McCarthy KD (1996) Hippocampal astrocytes in situ respond to glutamate released from synaptic terminals. J Neurosci 16:5073–5081
Ralevic V, Burnstock G (1998) Receptors for purines and pyrimidines. Pharmacol Rev 50:413–492
Ralevic V, Milner P, Kirkpatrick KA, Burnstock G (1992) Flow-induced release of adenosine 5’-triphosphate from endothelial cells of the rat mesenteric arterial bed. Experientia 48:31–34
Renaud LP, Bourquet CW (1991) Neurophysiology and neuropharmacology of hypothalamic magnocellular neurons secreting vasopressin and oxytocin. Progr Neurobiol 36:131–169
Robinson LE, Murrell-Lagnado R (2013) The trafficking and targeting of P2X receptors. Front. Cell. Neurosci., 22 November 2013 https://doi.org/10.3389/fncel.2013.00233
Sperlágh B, Sershen H, Lajtha A, Vizi ES (1997) Co-release of endogenous ATP and [3H]noradrenaline from rat hypothalamic slices: origin and modulation by α2-adrenoceptors. Neuroscience 82:511–520
Sperlágh B, Mergl Z, Juranyi Z, Vizi ES, Makara GB (1999) Local regulation of vasopressin and oxytocin secretion by extracellular ATP in the isolated posterior lobe of the rat hypophysis. J Endocrinol 160:343–350
Vanhoutte PM (2000) Say NO to ET. J Auton Nerv Syst 81:271–277
Verderio C, Matteoli M (2001) ATP Mediates calcium signaling between astrocytes and microglial cells: modulation by IFN-gamma. J Immunol 166:6383–6391
Verkhratsky A, Zimmermann H, Abbracchio MP, Illes P, Di Virgilio F (2020) Invited Obituary. In memoriam Geoffrey Burnstock: Creator of purinergic signaling. FUNCTION, 2020, 1(1): zqaa006. https://doi.org/10.1093/function/zqaa006
Xiang Z, Bo ZX, Burnstock G (1998) Localization of ATP-gated P2X receptor immunoreactivity in rat sensory and sympathetic ganglia. Neurosci Lett 256:105–108
Zonta M, Angulo MC, Gobbo S, Rosengarten B, Hossmann KA, Pozzan T, Carmignoto G (2003) Neuron-to-astrocyte signaling is central to the dynamic control of brain microcirculation. Nature Neurosci 6:43–50
Acknowledgments
I would like to thank Ms Tania Raquel Assuncao Martins for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that there is no conflict of interest.
Ethical approval
The studies described were carried following ethical approval. All rats were treated in accordance with the UK Animals (Scientific Procedures) Act 1986.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Loesch, A. On P2X receptors in the brain: microvessels. Dedicated to the memory of the late Professor Geoffrey Burnstock (1929–2020). Cell Tissue Res 384, 577–588 (2021). https://doi.org/10.1007/s00441-021-03411-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-021-03411-0