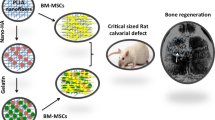
Abstract
Long bone defects comprise one of the most prevalent clinical problems worldwide and the current bone grafting materials have major limitations to repair them. Although tremendous efforts have been made to repair critical-sized long bone defects in animal models, designing an optimal bone tissue-engineered substitute remains one of the main challenges. Hence, this study aims to closely mimic a natural bone healing process by a tissue-engineered construct including osteoinductive materials pre-seeded with bone marrow-derived mesenchymal stem cells (BMSCs). Bioactive glass (BG) was incorporated into the gelatin/nano-hydroxyapatite (G/nHAp) scaffold (conventional one) to improve the bone regeneration process via its osteoinductivity and angiogenic activity. The fabricated G/nHAp and gelatin/nano-hydroxyapatite/bioactive glass (G/nHAp/BG) scaffolds were characterized by X-ray diffraction (XRD) and scanning electron microscopy (SEM) and analyzed for porosity and degradation rate. The osteogenic capability of fabricated scaffolds with or without BMSCs was then evaluated in vitro and in vivo. Critical-sized radial bone defects in rats were randomly filled with cell-free and BMSC-seeded scaffolds, autograft and a group left empty without any treatment. In vitro analysis showed that the G/nHAp/BG scaffold significantly increased the expression level of osteogenic and angiogenic markers in comparison to the G/nHAp-treated and control groups (P < 0.05). Moreover, the defects treated with the BMSC-seeded scaffolds showed superior bone formation and structural properties compared to the cell-free scaffolds 4 and 12 weeks post surgery. The radiological and histomorphological properties of defects treated by BMSC-seeded scaffolds, especially the BMSC-seeded G/nHAp/BG scaffold, were comparable to those of the autograft group. It is concluded that the combination of osteoconductive materials (i.e., nHAp) with the bioactive ones such as bioactive glass can effectively accelerate the bone regeneration process. In addition, our results demonstrated that the BMSCs have the potential to drastically increase the bone regeneration ability of osteoinductive scaffolds.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Critical-sized bone defects are the smallest-sized bone tissue defects that do not completely heal over a natural lifetime and often require medical intervention to promote bone regeneration (Oryan et al. 2016). Bone grafting procedure including autografts, allografts and xenografts is still the current therapeutic approach (Shibuya and Jupiter 2015). However, such a technique possesses some limitations such as lack of availability or donor site morbidity (Oryan et al. 2014c). Tissue engineering and regenerative medicine (TERM) has emerged since the last decade to develop novel strategies to the traditional ones (Fisher and Mauck 2013). It opens new horizons in repair and reconstruction of tissues and represents novel options to overcome the limitations of the traditional grafts, using a combination of cells, biomaterials and bioactive molecules (Howard et al. 2008). Selection of appropriate materials is crucial for fabrication of scaffolds in bone tissue engineering (BTE) (Zhang et al. 2017). Bioactivity, biocompatibility and biodegradability are three essential properties of biomaterials in BTE applications (Amini et al. 2012; Matassi et al. 2011; Oryan et al. 2017b; Yu et al. 2015). Hydroxyapatite (HAp) as a main inorganic component of hard tissues (bone and dental tissues) has been widely used alone or in composite form (i.e., gelatin (G)/HAp) for bone reconstruction (Dutta et al. 2015). It has been revealed that nano-HAp (nHAp) is a resource of free calcium and possesses higher osteoconductivity compared to micro-HAp, which makes it suitable for the osteogenic process (Pepla et al. 2014). Despite the excellent biocompatibility, availability and osteoconductivity, nHAp scaffolds have poor osteoinductivity or BTE application. Incorporation of osteoinductive materials would be an appealing strategy to improve osteogenic differentiation of HAp scaffolds (Friedlaender et al. 2013; Habibovic and de Groot 2007). Bioactive glass (BG) is one of the most popular osteoinductive biomaterials that enhances the expression of osteogenic-related markers and stimulates the secretion of angiogenic factors as well (Gorustovich et al. 2010; Xynos et al. 2001). Hence, incorporation of BG is proposed to overcome the drawbacks including lack of osteoinductivity and angiogenicity allocated to G/nHAp as a commercial product.
Cells (especially mesenchymal stem cells (MSCs) and progenitor cells) are the other key components of tissue engineering that have the ability to accelerate the bone healing process of critical-sized defects (Amini et al. 2012; Chan and Leong 2008). Differentiation of MSCs into the bone precursor cells is an important goal in BTE in order to successfully regenerate the critical-sized long bone defects in vivo without the need for growth-promotive factors. During the natural bone healing process, MSCs are recruited to the defect site and differentiate to form neo-bone (Knight and Hankenson 2013; Wang et al. 2013). MSCs are non-hematopoietic stromal stem cells that have a high capability for self-replication and the potential to differentiate into various lineages such as fibroblasts, osteoblasts, chondroblasts and adipocytes (Undale et al. 2009). Transplantation of undifferentiated MSCs has been extensively studied in previous investigations when MSCs have been proliferated by subculturing in vitro and usually seeded onto a carrier matrix or an osteoconductive scaffold. The transplanted MSCs then proliferate and differentiate into pre-osteoblastic cells in order to produce new functional bone tissue (Gao et al. 2012; Tortelli et al. 2010). However, the success of this strategy in the regeneration of large bone defects has not been proved yet and there are very few experimental reports on the MSC-induced repair of critical-sized long bone segmental defects (Cuomo et al. 2009).
This study aims to investigate the effect of BG incorporation on osteoinductivity and angiogenic activity of both bone marrow-derived mesenchymal stem cell (BMSC)-seeded and cell-free G/nHAp scaffolds in vitro and in the experimentally induced critical-sized radial bone defect (5 mm) in a rat model. The quantity and quality of new bone formation in different groups were comparatively evaluated, using imaging techniques (radiology and micro-CT scan), gross pathology, histopathology, immunohistochemistry, histomorphometry and biomechanical analysis.
Materials and methods
Materials
Gelatin (gel-bovine skin, type B, isoelectric point ~ 5) was purchased from Sigma-Aldrich (St. Louis, USA). BG 45S5 and n-HAp were obtained from the Pardis Pajouhesh Co. (Yazd, Iran). N-Hydroxysuccinimide (NHS) (97%) was purchased from Sigma-Aldrich (Wisconsin, USA). 1-Ethyl-3-(3-dimethylaminopropyl)carbodiimide hydrochloride (EDC) was obtained from Sigma-Aldrich (Milan, Italy).
Preparation of scaffolds
To fabricate the G/nHAp scaffold, 0.1 g nHAp was added to 5% w/v gelatin solution and stirred for 12 h at 37 °C. The G/nHAp/BG scaffold was prepared by dissolving 50:50 ratio of nHAp and BG (Bellucci et al. 2011) into the gelatin solution under agitation and then sonicated. The resultant gel was maintained at − 20 °C for 24 h and then freeze-dried. The scaffolds were chemically cross-linked with EDC and NHS (in a 5:1 ratio) (Liu and Ma 2009) in acetone/distilled water (DW) (90:10, v/v) for 12 h. The cross-linking reaction was stopped by adding 200 μM beta-mercaptoethanol. The cross-linked scaffolds were washed with DW (three times), freeze-dried and finally sterilized by 70% ethanol and UV light. They were kept in vacuumed packs until surgical application.
Evaluation of the porosity
The porosity of all scaffolds was determined using a liquid displacement method (Torres et al. 2013). Briefly, the scaffolds with known dry weight were immersed in a graduated cylinder containing a known volume of absolute ethanol (AE) for 5 min (V 1). The scaffolds were then pressed to force out air from them and allow the AE to permeate and fill the pores. The total volume of AE and the saturated scaffold with AE was then recorded (V 2). The saturated scaffold with AE was removed from the graded cylinder and the residual AE volume was recorded (V 3). The porosity of the scaffolds was calculated by the following equation:
Three replicates were analyzed for each bioscaffold.
Biodegradation analysis
Degradation of scaffolds was assessed through monitoring the scaffold weight loss. The scaffolds were cut into uniform sizes (1.5 × 1.5 cm) and fully immersed in the simulated body fluid (SBF; 0.2 ml of SBF/mm3 of the scaffold) solution for 21 days at 37 °C. The scaffolds were taken out from the SBF medium at different time points (7, 14, 21 and 28 days), washed with DW and freeze-dried to assess the morphological changes and weight loss. The biodegradability ratio was calculated using the following equation:
where D 1 denotes the original weight of scaffolds and D 2 is the weight of the freeze-dried scaffolds after immersing in SBF. Three samples of each group were analyzed to determine the mean biodegradation rate (percentage).
Scanning electron microscopy
Scanning electron microscopy (SEM; Crossbeam®, 1540XB, Zeiss) was performed to assess the surface and internal 3D architecture of the fabricated scaffolds. Attachment and morphological features of the cultured BMSCs on the scaffolds were also observed at days 1, 14 and 28 post seeding. For both experiments, the scaffolds were fixed in 2.5% glutaraldehyde (GA); dehydrated in graded concentrations of ethanol, followed by processing with osmium tetroxide; and finally, gold coated under vacuum and kept in proper storage conditions for further SEM analysis. Pore sizes were measured at least in 100 pores in each scaffold (Meimandi-Parizi et al. 2013; Oryan et al. 2014b).
X-ray diffraction analysis
Phase analysis of the composite scaffolds was determined, using a PANalytical X’Pert PRO powder diffractometer with monochromatic Cu-Kα radiation, operating at a voltage of 40 kV and 30 mA. XRD was taken at a 2θ angle range of 5°–80°. In order to identify the crystalline phases, the XRD patterns were compared with JCPDS standards.
Isolation and culture of BMSCs
Mesenchymal stem cells were isolated from the bone marrow of 4-week-old male Wistar rats and cultured in Dulbecco’s modified Eagle’s medium (DMEM; Gibco BRL, Life Technologies, Grand Island, NY, USA) supplemented with 15% fetal bovine serum (FBS) and antibiotics (100 units/ml penicillin G and 100 mg/ml streptomycin; Gibco BRL, Life Technologies). The culture flasks were then incubated in a 5% CO2 humidified atmosphere at 37 °C. Non-adherent cells were removed 3 days after seeding and the medium was replaced with fresh culture medium. When the culture reached approximately 90% confluency, the cells were passaged. BMSCs at passage 3 were used for further experiments.
Differentiation of BMSCs into mesenchymal lineages
The isolated cells were evaluated for their differentiation potential to mesodermal lineages. To induce the osteogenic differentiation, the cells were seeded in six-well culture plates and incubated in osteogenic medium (DMEM supplemented with 15% FBS, 10 mM β-glycerophosphate, 10 nM dexamethasone, and 0.2 mM ascorbic acid) for 21 days. Osteogenesis and the subsequent calcium mineral deposition were examined by 1% alizarin red S (ARS) (pH 6.0). Adipogenic differentiation was induced by incubating the cells in an adipogenic medium including DMEM supplemented with 10% FBS, 1 μM dexamethasone, 0.5 mM indomethacin and 1 mM ascorbic acid for 3 weeks. Lipid droplets were visualized with 4% oil red O staining for 15 min at room temperature (RT).
Flow cytometry
Flow cytometry was used to assess the expression of the cell surface marker of isolated cells. Briefly, 1 × 105 cells were incubated with phycoerythrin (PE)-conjugated anti-mouse CD11b and CD34 (Abcam, USA) and fluorescein isothiocyanate (FITC)-conjugated anti-mouse CD90 and CD25 (Abcam, USA) at 4 °C in a dark place for 30 min. As isotype controls, murine FITC-conjugated IgG1 and PE-conjugated IgG2b (eBioscience) were substituted for primary antibodies. Data from all samples were collected using a FACScan™ flow cytometer (BD FACSCalibur; BD Biosciences, San Jose, CA, USA) and analyzed by Flowing software, version 2.5.
Cell labeling
BMSCs were labeled with superparamagnetic iron oxide (SPIO) nanoparticles known as Feridex IV (Sigma) prior to seeding onto the scaffolds. The cells were incubated with a mixture of Feridex IV (100 μg/ml) and protamine sulfate (45 μg/ml) prepared in serum-free culture medium for 2 h at 37 °C. Subsequently, the medium was enriched with 10% FBS, 1% l-glutamine and 1% penicillin/streptomycin and then incubated for 48 h. Prussian blue staining was used to locate the SPIO-labeled BMSCs and labeling efficacy.
Cell seeding onto scaffolds
The sterilized scaffolds were washed twice in phosphate-buffered saline (PBS) and then placed in 24-well tissue culture plates. The BMSC suspension (50 μl; 1.0 × 106 cells/scaffold) for the 5-mm scaffold blocks was added onto the upper surface of each scaffold and incubated for 2 h to allow the BMSCs to adhere to the scaffolds.
Cytotoxicity assay
3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT; Sigma, USA) assay was performed to measure the viability of BMSCs and their proliferation rate after 1, 3 and 7 days (n = 3). The BMSC-seeded scaffolds were placed in 500 μl culture medium (DMEM) containing 100 μl MTT and incubated in a humidified atmosphere (5% CO2) at 37 °C for 3 h. The supernatant was then removed and the insoluble formazan salt crystals were dissolved in dimethyl sulfoxide (DMSO, 150 μl; Sigma, USA) and the optical density was measured at 570 nm, using a microplate reader (Thermo Scientific, USA).
Quantitative real-time PCR analysis
Osteogenic induction of the fabricated scaffolds (BMSC-seeded scaffolds: G/nHAp, G/nHAp/BG) was evaluated by quantitative real-time PCR (qRT-PCR) at day 21. Total RNA was extracted from the cells, using the RNeasy Micro Kit (74004; Qiagen). Complementary DNA (cDNA) was synthesized using the RevertAid First Strand cDNA Synthesis Kit (k1632; Fermentas, Sankt Leon-Rot, Germany) according to the manufacturer’s instructions. The qRT-PCR reaction was performed with SYBR® Green PCR Master Mix (Ref. 4367659; Applied Biosystems Life Technologies, Inc.) with a real-time PCR system (ABI StepOnePlus; Applied Biosystems Life Technologies, Inc.) and analyzed with StepOne software (version 2.1; Applied Biosystems). Relative quantification was performed, using a comparative CT method (also known as the 2−ΔΔCt method), where a number of target genes were normalized to an endogenous control (B2m) and relative to the calibrator group (control group, 2D culture flask). All reactions were performed in duplicate and all samples were collected from three biological replicates. Table 1 lists the primers.
Animals and surgical procedure
A total of 45 adult male Sprague Dawley rats (200–250 g) were purchased from the Razi Institute, Karaj, Iran. The animals received ad libitum access to standard chow pellets and water throughout the duration of the study. For general anesthesia in rats, 50 mg/kg ketamine hydrochloride (Ketamine 10%; Alfasan Co., Woerden, Holland), 2 mg/kg xylazine (Xylazine 2%; Alfasan Co., Woerden, Holland) and 1 mg/kg acepromazine maleate (Alfasan Co., Woerden, Holland) were injected intramuscularly. After shaving off the hair on the forelimbs, the radial bones were exposed via an appropriate 3-cm incision that was bilaterally made over the forelimbs. Complete bilateral 5-mm bone defects were then made in the middle of each radius, using an electrical bone saw (Strong Co., Seoul, South Korea) under physiological saline irrigation. The ulnar bones were left intact for mechanical stability of the defect site. The bone defects (15 defects/group) were either left empty or treated with autograft, G/nHAp and G/nHAp/BG with and without MSCs in the defect areas (2 × 2 × 5 mm3). After implantation, the incision was sutured in a routine fashion. Postoperative pain relief and antibiotic therapy were then provided by subcutaneous (SC) administration of 1 mg/kg meloxicam (Meloxivet 2%; Razak Co., Tehran, Iran) and intramuscular (IM) administration of enrofloxacin (Enron 5%; Irfan, Tehran, Iran), respectively, for 5 days. The number of animals examined in each group is shown in Fig. 1. All animals received humane care in compliance with the Guide for care and use of laboratory animals published by the National Institutes of Health (NIH; Publication No. 85-23, revised 1985). This experiment was approved by the local ethics committee of regulations for using animals in scientific procedures in the Cell Science Research Center, Royan Institute for Stem Cell Biology and Technology, Tehran, Iran. The rats were euthanized 4 and 12 weeks post surgery by IM injection of 50 mg/kg ketamine hydrochloride and 2 mg/kg xylazine hydrochloride. Then, 1 mg/kg gallamine triethiodide (Specia, Paris, France) was injected intracardially to stop breathing of the anesthetized animals.
Schematic presentation of different groups and subsequent treatment protocols (six groups). a Untreated defect (left forelimb, group 1) and autograft (right forelimb, group 2). b Radial bone segmental defect (5 mm). c Implantation of scaffolds (Sc). d G/nHAp scaffold-treated group (left forelimb, group 3) and G/nHAp/BG scaffold-treated group (right forelimb, group 4). e G/nHAp scaffold. f G/nHAp/BG scaffold. g G/nHAp-MSC scaffold-treated group (left forelimb, group 5) and G/nHAp/BG-MSC scaffold-treated group (right forelimb, group 6). h G/nHAp-MSC scaffold. i G/nHAp/BG-MSC scaffold
Gross evaluation
Macroscopic evaluation and scoring of bone repair for each radial bone sample were blindly done as follows: no union instability at the defect site (0 score), incomplete union with presence of fibrous connective tissue (+ 1 score) or cartilage (+ 2 score) within the defect site and complete union and presence of the bridging bone (+ 3 score; Oryan et al. 2014a)).
Radiological evaluation
Plain X-ray images were provided from the lateral surface of the radial bones from the anesthetized animals at 35 kV and 1.5 mA for 3 s. To evaluate the healing process of the radial bone defects, each digital radiograph was scored according to the previously described scoring system (Oryan et al. 2014a).
Micro-computed tomography testing
Micro-computed tomograms of the harvested radial bones were acquired at 70 kVp and 114 μA for 800 ms, using a SCANCO μCT35 scanner (SCANCO, Wangen-Brüttisellen, Switzerland). Bone volume (BV), total volume (TV) and the BV/TV were evaluated according to the micro-computed tomography (m-CT) scan results.
Histopathology and histomorphometry analysis
The radial bones were dissected free from soft tissue, fixed in 10% neutral buffered formalin solution for 48 h and decalcified with 10% EDTA (pH 7.4) for 25 days. The decalcified bone samples were then dehydrated in a gradient series of ethanol (70–100%), cleared in xylene and embedded in paraffin and finally, 5-μm-thick sections were prepared and stained with hematoxylin and eosin (H&E). The histological sections were examined, using a light microscope (Olympus BX51; Olympus, Tokyo, Japan) and blindly scored by an independent pathologist. For histomorphometric analysis, the number of cells including chondroblasts, chondrocytes, osteoblasts, osteocytes, fibroblasts, fibrocytes and other constituents, such as neo-vascularization and formation of new cartilage and bone and fibrous connective tissues, was calculated and analyzed, using the computer software Image-Pro Plus® V.6 (Media Cybernetics, Inc., Silver Spring, USA). Magnification × 400 was employed for counting the cells. In MSC-seeded scaffold groups, tissue sections were also stained with Prussian blue in order to localize the iron particles in SPIO-labeled MSCs within the repaired bone (Reddy et al. 2010).
Immunohistochemical analysis
Tissue sections from the lesions were also analyzed for expression of the following primary antibodies: CD31 (ab119339; Abcam, MA, USA), osteocalcin (OCN) (ab13420; Abcam, MA, USA), osteopontin (OPN) (ab8448; Abcam, MA, USA), and collagen type 1 (sc-59772; Santa Cruz Biotechnology, CA, USA). Antigen retrieval was performed by incubation of tissue sections with proteinase K (Dako, Glostrup, Denmark) for 6 min at RT. The tissue sections were blocked with 1% hydrogen peroxide/methanol (Sigma-Aldrich, St. Louis, MO, USA) for 30 min at RT, followed by an overnight incubation with primary antibodies at 4 °C. The color reaction was developed with diaminobenzidine (DAB) kit (Dako) and the slides were then counterstained with hematoxylin. The results were visualized by an ordinary light microscope (Olympus, Japan).
Biomechanical evaluation
The bone samples (n = 5 for each group) were firstly removed from the soft tissues, wrapped in gauze dampened with PBS in order to prevent dehydration and frozen at − 20 °C until biomechanical evaluation. The biomechanical analysis was performed on the radius–ulna complexes as have previously been described (Oryan et al. 2014a; Shafiei-Sarvestani et al. 2012). The bone specimens were subjected to destructive three-point bending, using a universal tensile testing machine (Instron, London, UK). The bone samples were placed horizontally on two rounded supporting bars separated at a distance of 16 mm. The third bar was carefully positioned at the midpoint of the defect (bone implanting) site. The rate of loading on the bone specimen was 2 mm/min until fracturing. The load–deformation curve was recorded for each sample by the machine. The maximum load (N), stress (N/mm2), strain (%) and stiffness (N/mm) were then calculated from the load–deformation curve and analyzed for each specimen. The biomechanical results calculated from the load–deformation curve were presented as the mean ± standard deviation (SD).
Statistical analysis
Quantitative data were presented as the mean ± SD and one-way ANOVA with subsequent Tukey’s post hoc tests were used to compare data between the groups. Kruskal–Wallis H and non-parametric ANOVA were used for statistical analysis of the qualitative data obtained from the scored values and if the differences were significant (P < 0.05), the data were analyzed by the Mann–Whitney U test. All statistical analyses were performed by GraphPad Prism software, version 6.00 (GraphPad Prism, Inc., San Diego, CA, USA).
Results
Characterization of scaffolds
SEM micrographs of the fabricated G/nHAp and G/nHAp/BG scaffolds are shown in Fig. 2. Porous structures with large-sized pores and proper interconnectivity were seen. The G/nHAp scaffolds showed high porosity (83%) with mean pore sizes of 355 μm. The G/nHAp/BG had suitable (81%) porosity with mean pore sizes of 323 μm. The fabricated scaffolds containing nHAp and BG were soaked in SBF solution at different periods of time (7, 14, 21 and 28 days) to evaluate their biodegradation rate (Fig. 3a). The biodegradation rate clearly diminished and gradually slowed down by increasing the BG content. Phase analyses of the fabricated scaffolds are shown in Fig. 3(b). The CaP-based scaffolds exhibited sharp diffraction peaks and had a similar XRD pattern to the standard patterns for nHAp. Analysis of all the XRD patterns, except for the BG powder-fabricated scaffold, revealed the presence of crystalline phases. These phases were consistent with the phases listed in the ICDD database. The characteristic diffraction peaks for both nHAp and gelatin were suppressed by the amorphous peak of BG observed in the range between 2θ angles equal to 20°–40°.
Macroscopic images of fabricated scaffold including G/nHAp (a) and G/nHAp/BG (a’). Scanning ultramicrographs of the G/nHAp (b, d) and G/nHAp/BG (c, e) scaffolds prepared via the freeze-drying method. The G/nHAp and G/nHAp/BG scaffolds show a homogeneous porous structure. nHAp nano-hydroxyapatite, G gelatin, BG bioactive glass
Attachment, viability, and morphology of BMSCs on scaffolds
To confirm the mesenchymal phenotype, the isolated cells underwent differentiation into osteogenic and adipogenic lineages (Supplementary Fig. S1, a–d). In addition, they were analyzed against various surface markers. As expected, the majority of BMSCs were positive for CD90 (> 90%) and CD25 (75%). In addition, 20% of the BMSCs expressed CD34, whereas 5% expressed CD11b (Supplementary Fig. S1, e–h).
The viability of the BMSCs on both G/nHAp and G/nHAp/BG scaffolds was examined after 1, 3 and 7 days (Fig. 4a). Based on MTT assay, there was no cytotoxicity associated with G/nHAp and G/nHAp/BG. A number of the cells on G/nHAp were slightly lower in comparison with the controls but this difference was not significant.
In vitro analysis. a MTT assay. b Tracking of the seeded BMSCs via SPIO nanoparticles (arrows). The SPIO-labeled MSCs (blue cytoplasm) showing clusters of iron-positive blue cells in vitro (Prussian blue staining). c–g Effects of the scaffolds on mRNA expression of CD31, Runx2, OCN, ALP and Col1 on day 21. The G/nHAp/BG scaffold could promote expression of OCN, Col1 and CD31 genes, which were expressed higher compared with the control group and other scaffolds. nHAp nano-hydroxyapatite, G gelatin, BG bioactive glass, Runx2 Runt-related transcription factor 2, OCN osteocalcin, ALP alkaline phosphatase, Col1 collagen type 1
The SEM ultramicrographs showed that the BMSCs were successfully attached on the scaffold surfaces at 2 h post seeding (Fig. 5a, b). After 1 day of BMSC seeding, the cells strongly adhered over the surface of the porous scaffold via their pseudopodia and cell processes (Fig. 5c, d). BMSCs were elongated, originating from the pseudopodia extending along the surface and the new organization of the cytoskeleton structure at day 14 (Fig. 5e, f). This preliminary experiment also confirmed the cytocompatibility of the fabricated scaffold for BMSC attachment.
SEM ultramicrographs of BMSC-seeded bioscaffolds. BMSCs have successfully attached at 2 h (a, b). BMSCs attached onto the scaffolds via their pseudopods (c, d) at 1 day post seeding. Fourteen days after seeding, the BMSCs showed morphological changes that indicate their differentiation (e, f). nHAp nano-hydroxyapatite, G gelatin, BG bioactive glass
In vitro cell labeling
To visualize the SPIO-labeled BMSCs through in vitro analysis, Prussian blue staining was used to detect internalization of iron nanoparticles and it revealed that almost all the cells were labeled efficiently with SPIO particles (Fig. 4b).
qRT-PCR analysis
qRT-PCR was performed to analyze the expression level of angiogenic- and osteogenic-related genes of BMSCs seeded on the scaffolds at day 21. Both BMSC-loaded G/nHAp and G/nHAp/BG showed a higher expression level of CD31 and Alp compared to the control group (2D culture flask). Similarly, the Alp expression level (Fig. 3d) was also higher in the G/nHAp/BG scaffold than in the G/nHAp one (P < 0.05). BMSCs cultured in the G/nHAp/BG expressed a higher level of CD31 (Fig. 3g) and OCN (Fig. 3c) than those in other groups (P < 0.05). The Runt-related transcription factor 2 (Runx2) expression level (Fig. 3e) decreased in both G/nHAp- and G/nHAp/BG-treated groups in comparison to the control, while the statistical analysis showed no obvious differences (P > 0.05). Col1 expressed higher in the G/nHAp/BG followed by the G/nHAp ones (Fig. 3f) in comparison to the control group (P < 0.05).
Pre-clinical evaluations
All animals survived until the end of experiments without any complication. The forelimbs of the treated groups with cell-free scaffolds showed obvious hyperemia, edema and swelling, while those with BMSCs had milder signs during the first 1 to 2 weeks post implantation. In addition, the non-treated and autograft-treated groups showed mild to moderate postsurgical inflammation. However, these signs were gradually diminished to normal in these groups 4 weeks after surgery. The defect sites of the untreated group still remained empty on digital palpation, whereas in the treated groups, the defects were filled with new soft fibrous connective tissues and further with hard tissues, at 5–7 weeks after injury induction. The animals in the treated and autograft groups had better weight-bearing in comparison to those in the untreated group in which the defect sites were less developed. Moreover, the BMSC-seeded G/nHAp/BG scaffold groups demonstrated the best weight-bearing and gait ability when compared to the other groups.
Gross pathology
The defect sites were filled with fibrous connective tissue or remained empty in the untreated group (Fig. 6a, a’) while the autograft was integrated to both old radial bone edges in the defect area via the newly formed hard tissue (Fig. 6b, b’). The scaffolds in the MSC-seeded G/nHAp- and G/nHAp/BG-treated groups were almost completely degraded at 4 weeks after surgery (Fig. 6e, f) and the defects were replaced by the newly regenerated tissue including cartilaginous, osteochondral, or bone tissue at 12 weeks post surgery (WPS) (Fig. 6e’, f’). However, the defect sites were partially filled with bony-like tissues in the cell-free scaffold groups 12 WPS (Fig. 6c’, d’) and the scaffolds were partially degraded over 4 weeks (small segments of the scaffolds were still present in tissue sections) (Fig. 6c, d). Each group was macroscopically scored based on the newly formed tissue after 12 weeks (Table 2). The defects in the BMSC-seeded scaffolds and autograft groups were filled with hard tissues and gained higher scores in comparison with the untreated group (negative control) in which the lesions were either empty or filled with fibrous connective tissues (P < 0.01). There was no significant difference between the autograft and BMSC-seeded scaffold groups in terms of microscopic union scores (P > 0.05).
Radiology
In order to follow the progress of new bone formation in the defect sites, radiographs were taken from the experimental and control groups at 4 and 12 WPS. The X-ray images and the results for different experimental groups at sequential intervals during the study are shown in Fig. 6g, g’, h, h’, i, i’, j, j’, k, k’, l, l’ and Table 3, respectively. The X-ray scores revealed that new bone formation and union of the BMSC-seeded scaffolds and autograft groups were significantly superior compared to the other groups at 4 and 12 weeks (P < 0.05) post operation. The lesions in G/nHAp/BG pre-seeded with BMSCs showed more significant bone formation in comparison to the untreated defect group at 4 weeks (P = 0.007). There were significant differences between the X-ray scores of the BMSC-free G/nHAp and G/nHAp/BG groups with the untreated defect group at 4 weeks (P < 0.05). Additionally, the lesions in the BMSC-seeded scaffold groups demonstrate more significant bone union than the cell-free G/nHAp- and G/nHAp/BG-treated groups (P < 0.05). After 12 weeks, the bone gap in the autograft and BMSC-seeded scaffold groups was radiopaque, whereas those in the BMSC-free scaffolds and untreated groups were radiolucent.
Micro-CT scan
For 3D characterization of new bone formation, micro-CT scan analysis was utilized 12 WPS (Table 4). Micro-CT scans of different groups are presented in Fig. 6g”, g”’, h”, h”’, i”, i”’, j”, j”’, k”, k”’, l”, l”’. The micro-CT results were reported as BV, TV and percentage of BV/TV for all the radial bone defects, after 12 weeks of implantation. BV/TV, as an index of new bone formation, was significantly higher in the autograft and all the treated groups in comparison to the untreated group (P < 0.01). BV/TV in the autograft and the MSC-seeded scaffold-treated groups was significantly superior to the other groups (P < 0.05). Over 81% of the bone gaps in the BMSC-seeded G/nHAp scaffolds were filled with new bone tissue. The new bone formation was less than 10% in the untreated defect group, while the BMSC-free G/nHAp- and G/nHAp/BG-treated groups showed approximately 37 and 51% new bone formation, respectively. Moreover, the autograft and the BMSC-seeded G/nHAp/BG-treated groups achieved almost a complete union and remodeling (96 and 92%, respectively).
Histopathologic, histomorphometric and immunohistochemical findings
To assess the progress of new bone formation and regeneration in the radial defects, longitudinal sections were harvested at 4 WPS (Fig. 7) and 12 WPS (Fig. 8). The tissue sections were prepared and examined histopathologically, histomorphometrically and immunohistochemically (Fig. 9). Based on the microscopic scores (Table 2), the injured radial bones in the autograft and BMSC-seeded scaffold-treated groups had significantly superior scores compared to those of the untreated defect and BMSC-free scaffold groups at 4 and 12 weeks after surgical operation (P < 0.05). However, there was no significant difference in microscopic scores of the BMSC-seeded scaffold and autograft group (P > 0.05).
Histopathological sections from radial bone defects in rats at 4 weeks post operation. There are still some remnants of cell-free G/nHAp and G/nHAp/BG scaffolds, while the BMSC-seeded bioscaffolds were completely degraded and replaced mostly with new bone and cartilage tissue. Minimum healing of the defect site was seen in the untreated defect group. nHAp nano-hydroxyapatite, G gelatin, BG bioactive glass, LACT loose areolar connective tissue, DCT dense connective tissue, FT fibrous connective tissue, FCT fibrocartilage tissue, OB old bone, BM bone marrow, Ag angiogenesis, G gap, NBF new bone formation, NBM new bone marrow, CT cartilaginous tissue, SC scaffold, HC hyaline cartilage, WB woven bone, RS remnants of the scaffold, OC osteocytes. a–a”’ Untreated defect. b–b”’ Autograft. c–c”’ G/nHAp. d–d”’ G/nHAp/BG. e–e”’ G/nHAp-MSCs. f–f”’ G/nHAp/BG-MSCs. Stained with H&E
Histopathological sections from radial bone defects in rats at 12 weeks post operation. The cell-free G/nHAp and G/nHAp/BG scaffolds were degraded over time and replaced by new tissues (fibrous, cartilage, and osseous tissues). Maximum similarity to the autograft was seen in the BMSC-seeded bioscaffolds, especially in the BMSC-seeded G/nHAp/BG scaffold in which the defect site was completely filled with new bone and cartilage tissue. nHAp nano-hydroxyapatite, G gelatin, BG bioactive glass, LACT loose areolar connective tissue, DCT dense connective tissue, FT fibrous connective tissue, FCT fibrocartilage tissue, OB old bone, BM bone marrow, Ag angiogenesis, G gap, NBF new bone formation, NBM new bone marrow, CT cartilaginous tissue, SC scaffold, HC hyaline cartilage, WB woven bone, RS remnants of the scaffold, OC osteocytes. a–a”’ Untreated defect. b–b”’ Autograft. c–c”’ G/nHAp. d–d”’ G/nHAp/BG. e–e”’ G/nHAp-MSCs. f–f”’ G/nHAp/BG-MSCs. Stained with H&E
Immunostaining of the injured area in different treatment groups for bone regeneration and angiogenesis. Immunohistochemical analysis of Col1, OCN, OPN and CD31 was used to determine the osteogenesis and angiogenesis in samples. The brown color represents positive staining of Col1, OCN, OPN and CD31. a–a”’ Untreated defect. b–b”’ Autograft. c–c”’ G/nHAp. d–d”’ G/nHAp/BG. e–e”’ G/nHAp-MSCs. f–f”’ G/nHAp/BG-MSCs. g Double asterisks, untreated vs. autograft, G/nHAp, G/nHAp/BG, G/nHAp-MSCs, and G/nHAp/BG-MSCs. Single asterisk, G/nHAp vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. Single asterisk, G/nHAp/BG vs. autograft and G/nHAp/BG-MSCs. g’ Double asterisks, untreated vs. autograft and G/nHAp/BG. Double asterisks, G/nHAp vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. Single asterisk, untreated vs. G/nHAp. Single asterisk, G/nHAp vs. G/nHAp/BG. Single asterisk, G/nHAp/BG vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. g” Double asterisks, untreated vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. Double asterisks, G/nHAp vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. Double asterisks, G/nHAp/BG vs. autograft, G/nHAp-MSCs and G/nHAp/BG-MSCs. g”’ Double asterisks, untreated vs. autograft, G/nHAp and G/nHAp/BG. Double asterisks, G/nHAp-MSCs vs. autograft, G/nHAp and G/nHAp/BG. Double asterisks, G/nHAp/BG-MSCs vs. autograft, G/nHAp, and G/nHAp/BG. Single asterisk, untreated vs. G/nHAp-MSCs and G/nHAp/BG-MSCs. Single asterisk, G/nHAp vs. autograft and G/nHAp/BG. **P < 0.01; *P < 0.05
The bone gap in the untreated group was replaced with a loose areolar fibrous connective tissue at 4 weeks after bone surgery so that the gap was empty from the new bone tissue and did not bridge. At 12 weeks post operation, the gap was completely filled by fibrovascular tissue with a narrow ridge of fibrocartilage tissue at the edges of old radial bones. Four weeks following surgery, only one end of the implanted autograft was integrated to the edge of the old bones by cartilaginous and osseous tissues. Finally, the histopathological findings showed that this integration was fully achieved at 12 weeks. Some remnants of the cell-free G/nHAp scaffold remained in the defect area surrounded by fibrous connective tissue. In the cell-free G/nHAp-treated group, the radial bone gap was filled with a mixed tissue consisting of woven bone, hyaline cartilage and fibrous connective tissue. In the cell-free G/nHAp/BG-treated group, the residue of the scaffold was seen in the defect area at 4 weeks; however, this scaffold was fully degraded at 12 weeks post operation and the defects were filled with new bone and loose areolar connective tissue. In the BMSC-seeded G/nHAp scaffolds, most of the scaffold degraded over 4 weeks and the gap was filled with fibrocartilage and woven bone. In the BMSC-seeded G/nHAp-treated group, the scaffold was completely degraded over 12 weeks and totally replaced with woven bone. In the BMSC-seeded G/nHAp/BG-treated group, the scaffold was totally degraded over 4 weeks after surgery and replaced with woven bone and hyaline cartilage. The defects in the BMSC-seeded G/nHAp/BG-treated group were totally filled with woven and compact bone, at 12 weeks post operation.
The histopathologic findings of the BMSC-seeded G/nHAp/BG scaffold were more close to autograft than the other groups (i.e., cell-free scaffolds and untreated defect). Both the autograft and BMSC-seeded G/nHAp/BG-treated groups showed hypertrophic bone edges, and neo-bone was formed in the BMSC-seeded G/nHAp/BG-treated group through endochondral ossification. The woven bone formation was considerably higher in the BMSC-seeded scaffold groups when compared to the cell-free scaffold groups. In addition, the SPIO-labeled MSCs after staining with Prussian blue were demonstrated by blue cytoplasm, showing clusters of iron-positive blue cells in paraffin sections of the defect site in the BMSC-seeded scaffold groups (Fig. 8).
Histomorphometric findings of bone regeneration related to different experimental groups in 12 weeks after bone surgery are shown in Table 5. Accordingly, the density of newly formed tissues including cartilaginous (C), osseous (O) and fibrous (F) connective tissues in each group was respectively as follows: 3.43 ± 0.45C%, 0.00O% and 96.57 ± 1.85F% for the untreated defect; 20.97 ± 2.74C%, 71.99 ± 1.69O% and 7.04 ± 8.26F% for the autograft; 33.98 ± 3.21C%, 27.16 ± 2.97O% and 38.86 ± 3.34F% for the cell-free G/nHAp; 36.19 ± 2.41C%, 31.37 ± 3.55O% and 32.44 ± 3.14F% for the cell-free G/nHAp/BG; 33.30 ± 3.16C%, 55.21 ± 2.54O%, and 11.49 ± 1.28F% for the BMSC-seeded G/nHAp-treated group; and 19.87 ± 2.26C%, 73.13 ± 3.25O% and 7.00 ± 1.03F% for the BMSC-seeded G/nHAp/BG-treated group. Based on these data, the density of cartilage and osseous tissues in the autograft and BMSC-seeded G/nHAp/BG-treated groups was highest than that in the other groups (P < 0.05), followed by the BMSC-seeded G/nHAp, cell-free G/nHAp/BG and cell-free G-nHAp-treated and untreated defects. On the other hand, the density of fibrous connective tissues was significantly higher in the untreated defects in comparison to the other treatments (P < 0.01) (Table 5).
The autograft and BMSC-seeded scaffold groups had the greatest immunostaining for collagen type 1 (Col1), a typical marker of matrix maturation, indicating that the bone formation and maturation rate was higher in these groups compared to that in the other groups (P < 0.05). The untreated defects showed the lowest expression level of Col1 at 12 weeks after bone injury (P < 0.01) (Fig. 9). Immunohistochemical (IHC) analysis of OPN, a protein that is involved in bone remodeling, showed a very strong signal in autograft and BMSC-seeded scaffolds at 4 weeks (P < 0.05). OCN, as a specific marker of mature osteoblasts, exhibited no signal in the untreated defects at 4 weeks. On the other hand, a very strong signal of OCN was seen in the autograft and BMSC-seeded scaffold groups 4 weeks post implantation. The expression level of OCN protein was lower in the cell-free scaffold groups in comparison to the autograft and BMSC-seeded scaffold groups (P < 0.05). Moreover, a significant difference was observed in cell-free G/nHAp/BG- and G/nHAp-treated groups in terms of OCN expression level (P < 0.05). IHC analysis of the BMSC-seeded scaffolds showed higher expression of the endothelial marker CD31 when compared to the other treatments, showing more angiogenesis in the BMSC-seeded scaffold groups. However, the highest expression of CD31 marker was seen in the untreated defects (P < 0.01). The expression of CD31 was considerably higher in the cell-free G/nHAp/BG- than in the G/nHAp-treated groups (P < 0.05).
Biomechanical performance
The data achieved from the biomechanical testing are available in Table 6. The autograft and BMSC-seeded scaffold groups demonstrated significantly higher maximum load (N), stress (N/mm2) and stiffness (N/mm) when compared with the cell-free scaffolds (P < 0.01) and untreated defect groups (P < 0.01). The defects in the cell-free scaffold groups had a significantly greater ultimate load, stress and stiffness when compared to those of the untreated group (P < 0.05). On the other hand, the untreated group had the greatest strain (%) as compared with that of the autograft, BMSC-seeded and cell-free scaffold groups (P < 0.05). In addition, the cell-free scaffolds demonstrated a significantly higher strain in comparison to the autograft and the BMSC-seeded scaffold-treated groups (P < 0.05).
Discussion
This study was aimed to understand the effect of BG on osteoinductivity and angiogenic activity of the G/nHAp scaffold with and without incorporation of BMSCs. More recently, it has been reported that grafting different scaffolds with pre/differentiated MSCs into critical-sized defects resulted in enhanced bone formation compared to cell-free scaffolds (Harada et al. 2014; Maiti et al. 2016). Osteogenic/chondrogenic differentiation of BMSCs is still an expensive and time-consuming approach requiring specific growth factors and differentiation media (Welter et al. 2007). Hence, we evaluated the osteogenic effects of G/nHAp/BG (as an optimized scaffold) and G/nHAp (as a conventional option) with or without BMSCs in 5-mm critical-sized radial bone defects in rats. The defects were created as the smallest gap that is not able to heal naturally throughout the duration of the experiment (Harada et al. 2014). The therapeutic effects of different scaffolds seeded with undifferentiated BMSCs in the critical-sized rat radial bone defects were then assessed.
Previous studies have shown that biphasic calcium phosphate strut coating with bioactive glass materials could significantly increase the compressive strength and differentiation of BMSCs through upregulation of Runx2, osteopontin and sialoprotein genes (Yi et al. 2016). Similarly, in our study, the bioactive glass composite (with nHAp and gelatin) showed superior outcomes in repairing long bone defects in comparison to the G/nHAp. Moreover, BMSCs significantly enhanced the regeneration process during a similar treatment time.
Radiology and m-CT results indicated that bone healing and union occurred in the BMSC-seeded scaffold groups, while incomplete and no union was observed in cell-free scaffold and untreated defect groups, respectively. Furthermore, the in vivo biodegradation rate of the scaffolds and their potential in stimulating bone regeneration were considerably higher in BMSC-seeded scaffolds compared to cell-free groups. Biodegradation occurred in BMSC-seeded scaffolds as early as 4 weeks after the implantation. One of the most important factors in long bone regeneration and repair is whether the newly formed bone has adequate strength to carry out their load-bearing functions. Moreover, cancellous bone regeneration is a necessary process to maintain hematopoiesis, tissue perfusion and lightness. The BMSC-seeded G/nHAp/BG scaffold provides all these requirements. In our study, the biomechanical tests showed that there was no significant difference between the maximum load of the repaired bone in the BMSC-seeded scaffolds and the autograft, at 12 weeks after surgery, while the cell-free scaffolds had a mean ultimate load that was 64% of the autograft.
The differentiation process of BMSCs into osteogenic lineage is usually divided into three phases including differentiation into osteoblasts, synthesis of bone matrix and matrix mineralization (Beck Jr 2003). The Runx2 gene expression, as an early marker and essential transcriptional factor for osteogenic lineage commitment and osteoblastic differentiation, was lower in all experimental groups in comparison to the control group at 4 weeks after in vitro culture, which might result from its gene expression reduction over time. On the other hand, the highest expression of late osteoblastic markers such as ALP (as an important factor in osteoid formation and bone mineralization) and OCN and Col1 (as the essential bone proteins produced by osteoblasts) found with the BMSC-seeded G/nHAp/BG scaffold was consistent their higher bone formation and matrix mineralization in vivo. CD31 is another important endothelial marker, whose expression level increases in bone regeneration, especially at an early phase of regeneration (Yang et al. 2012). the CD31 expression level was significantly elevated in the BMSC-seeded G/nHAp/BG scaffold at day 21 as evidenced by immunohistochemical analysis in vivo. Taken together, qRT-PCR results demonstrated that the G/nHAp/BG scaffold increased the expression level of angiogenic- and osteogenic-related genes of BMSCs, indicating the beneficial effects of BG incorporation into G/nHAp.
It should be pointed out that the rate of new bone formation (92.7%) and biomechanical performance (ultimate load, 36.4 N) of the regenerated bone tissue in our study were much more promising than those reported earlier (new bone formation, 67.9, 61.6, 46.38 and 80.29%; ultimate load, 27.3, 28.6, 31.2 and 28.2 N) (Alidadi et al. 2017a; Alidadi et al. 2017b; Oryan et al. 2017a; Oryan et al. 2017b). Based on our results, it can be figured out that the fabricated scaffold in terms of its materials, porosity, pore size and shape can successfully induce osteogenic differentiation of exogenous and host-recruited MSCs and a promising alternative to autograft can be established. However, further experiments are necessary to clearly elucidate the exact cellular and molecular mechanisms underlying this process.
Conclusion
This study revealed an optimized therapeutic modality for regeneration of critical-sized bone defects in large bones that havehas two major advantages including acceptable therapeutic efficacy and reliability. If these encouraging results observed in the animal model affirm to be consistent in human and other mammals, this could open new horizons to the development of clinical applications. The present study suggests that the osteoinductive scaffolds, especially G/nHAp/BG with the incorporation of BMSCs, enhance angiogenesis and bone repair in comparison to conventional scaffolds (G/nHAp), which were proved by in vivo and in vitro analyses. Therefore, due to perfect new bone formation along with high in vivo biodegradability of this scaffold, it can be introduced as a promising alternative to autografts. It can also be concluded that the BMSC-seeded scaffolds rather than the ones without BMSCs are more promising scaffolds for bone reconstruction programs.
Change history
23 August 2021
A Correction to this paper has been published: https://doi.org/10.1007/s00441-021-03520-w
References
Alidadi S, Oryan A, Bigham-Sadegh A, Moshiri A (2017a) Comparative study on the healing potential of chitosan, polymethylmethacrylate, and demineralized bone matrix in radial bone defects of rat. Carbohydr Polym 166:236–248
Alidadi S, Oryan A, Bigham-Sadegh A, Moshiri A (2017b) Role of platelet gel embedded within gelatin scaffold on healing of experimentally induced critical-sized radial bone defects in rats. Int Orthop 41:805–812
Amini AR, Laurencin CT, Nukavarapu SP (2012) Bone tissue engineering: recent advances and challenges. Crit Rev Biomed Eng 40:363–408
Beck GR Jr (2003) Inorganic phosphate as a signaling molecule in osteoblast differentiation. J Cell Biochem 90:234–243
Bellucci D, Cannillo V, Sola A (2011) A new highly bioactive composite for scaffold applications: a feasibility study. Materials 4:339
Chan BP, Leong KW (2008) Scaffolding in tissue engineering: general approaches and tissue-specific considerations. Eur Spine J 17:467–479
Cuomo AV, Virk M, Petrigliano F, Morgan EF, Lieberman JR (2009) Mesenchymal stem cell concentration and bone repair: potential pitfalls from bench to bedside. J Bone Joint Surg Am 91:1073–1083
Dutta SR, Passi D, Singh P, Bhuibhar A (2015) Ceramic and non-ceramic hydroxyapatite as a bone graft material: a brief review. Ir J Med Sci 184:101–106
Fisher MB, Mauck RL (2013) Tissue engineering and regenerative medicine: recent innovations and the transition to translation. Tissue Eng B Rev 19:1–13
Friedlaender GE, Lin S, Solchaga LA, Snel LB, Lynch SE (2013) The role of recombinant human platelet-derived growth factor-BB (rhPDGF-BB) in orthopaedic bone repair and regeneration. Curr Pharm Des 19:3384–3390
Gao C, Seuntjens J, Kaufman GN, Tran-Khanh N, Butler A, Li A, Wang H, Buschmann MD, Harvey EJ, Henderson JE (2012) Mesenchymal stem cell transplantation to promote bone healing. J Orthop Res 30:1183–1189
Gorustovich AA, Roether JA, Boccaccini AR (2010) Effect of bioactive glasses on angiogenesis: a review of in vitro and in vivo evidences. Tissue Eng B Rev 16:199–207
Habibovic P, de Groot K (2007) Osteoinductive biomaterials—properties and relevance in bone repair. J Tissue Eng Regen Med 1:25–32
Harada N, Watanabe Y, Sato K, Abe S, Yamanaka K, Sakai Y, Kaneko T, Matsushita T (2014) Bone regeneration in a massive rat femur defect through endochondral ossification achieved with chondrogenically differentiated MSCs in a degradable scaffold. Biomaterials 35:7800–7810
Howard D, Buttery LD, Shakesheff KM, Roberts SJ (2008) Tissue engineering: strategies, stem cells and scaffolds. J Anat 213:66–72
Knight MN, Hankenson KD (2013) Mesenchymal stem cells in bone regeneration. Adv Wound Care 2:306–316
Liu X, Ma PX (2009) Phase separation, pore structure, and properties of nanofibrous gelatin scaffolds. Biomaterials 30:4094–4103
Maiti SK, Ninu AR, Sangeetha P, Mathew DD, Tamilmahan P, Kritaniya D, Kumar N, Hescheler J (2016) Mesenchymal stem cells-seeded bio-ceramic construct for bone regeneration in large critical-size bone defect in rabbit. J Stem Cells Regen Med 12:87–99
Matassi F, Nistri L, Chicon Paez D, Innocenti M (2011) New biomaterials for bone regeneration. Clinical cases in mineral and bone. Metabolism 8:21–24
Meimandi-Parizi A, Oryan A, Moshiri A (2013) Tendon tissue engineering and its role on healing of the experimentally induced large tendon defect model in rabbits: a comprehensive in vivo study. PLoS One 8:e73016
Oryan A, Alidadi S, Bigham-Sadegh A, Meimandi-Parizi A (2017a) Chitosan/gelatin/platelet gel enriched by a combination of hydroxyapatite and beta-tricalcium phosphate in healing of a radial bone defect model in rat. Int J Biol Macromol 101:630–637
Oryan A, Alidadi S, Bigham-Sadegh A, Moshiri A (2016) Comparative study on the role of gelatin, chitosan and their combination as tissue engineered scaffolds on healing and regeneration of critical sized bone defects: an in vivo study. J Mater Sci Mater Med 27:155
Oryan A, Alidadi S, Bigham-Sadegh A, Moshiri A, Kamali A (2017b) Effectiveness of tissue engineered chitosan-gelatin composite scaffold loaded with human platelet gel in regeneration of critical sized radial bone defect in rat. J Control Release 254:65–74
Oryan A, Bigham-Sadegh A, Abbasi-Teshnizi F (2014a) Effects of osteogenic medium on healing of the experimental critical bone defect in a rabbit model. Bone 63:53–60
Oryan A, Moshiri A, Meimandi-Parizi A (2014b) In vitro characterization of a novel tissue engineered based hybridized nano and micro structured collagen implant and its in vivo role on tenoinduction, tenoconduction, tenogenesis and tenointegration. J Mater Sci Mater Med 25:873–897
Oryan A, Moshiri A, Meimandi-Parizi A (2014c) In vitro characterization of a novel tissue engineered based hybridized nano and micro structured collagen implant and its in vivo role on tenoinduction, tenoconduction, tenogenesis and tenointegration. J Mater Sci Mater Med 25:873–897
Pepla E, Besharat LK, Palaia G, Tenore G, Migliau G (2014) Nano-hydroxyapatite and its applications in preventive, restorative and regenerative dentistry: a review of literature. Annali di Stomatologia 5:108–114
Reddy AM, Kwak BK, Shim HJ, Ahn C, Lee HS, Suh YJ, Park ES (2010) In vivo tracking of mesenchymal stem cells labeled with a novel chitosan-coated superparamagnetic iron oxide nanoparticles using 3.0T MRI. J Korean Med Sci 25:211–219
Shafiei-Sarvestani Z, Oryan A, Bigham AS, Meimandi-Parizi A (2012) The effect of hydroxyapatite-hPRP, and coral-hPRP on bone healing in rabbits: radiological, biomechanical, macroscopic and histopathologic evaluation. Int J Surg (London, England) 10:96–101
Shibuya N, Jupiter DC (2015) Bone graft substitute: allograft and xenograft. Clin Podiatr Med Surg 32:21–34
Torres AL, Gaspar VM, Serra IR, Diogo GS, Fradique R, Silva AP, Correia IJ (2013) Bioactive polymeric-ceramic hybrid 3D scaffold for application in bone tissue regeneration. Mater Sci Eng C Mater Biol Appl 33:4460–4469
Tortelli F, Tasso R, Loiacono F, Cancedda R (2010) The development of tissue-engineered bone of different origin through endochondral and intramembranous ossification following the implantation of mesenchymal stem cells and osteoblasts in a murine model. Biomaterials 31:242–249
Undale AH, Westendorf JJ, Yaszemski MJ, Khosla S (2009) Mesenchymal stem cells for bone repair and metabolic bone diseases. Mayo Clin Proc 84:893–902
Wang X, Wang Y, Gou W, Lu Q, Peng J, Lu S (2013) Role of mesenchymal stem cells in bone regeneration and fracture repair: a review. Int Orthop 37:2491–2498
Welter JF, Solchaga LA, Penick KJ (2007) Simplification of aggregate culture of human mesenchymal stem cells as a chondrogenic screening assay. BioTechniques 42:732–737
Xynos ID, Edgar AJ, Buttery LD, Hench LL, Polak JM (2001) Gene-expression profiling of human osteoblasts following treatment with the ionic products of bioglass 45S5 dissolution. J Biomed Mater Res 55:151–157
Yang YQ, Tan YY, Wong R, Wenden A, Zhang LK, Rabie ABM (2012) The role of vascular endothelial growth factor in ossification. Int J Oral Sci 4:64–68
Yi H, Ur Rehman F, Zhao C, Liu B, He N (2016) Recent advances in nano scaffolds for bone repair. Bone Res 4:16050
Yu X, Tang X, Gohil SV, Laurencin CT (2015) Biomaterials for bone regenerative engineering. Adv Healthc Mater 4:1268–1285
Zhang X-Y, Fang G, Zhou J (2017) Additively manufactured scaffolds for bone tissue engineering and the prediction of their mechanical behavior: a review. Materials 10:50
Acknowledgement
The authors wish to thank Miss F.A. Sayahpour (Royan Institute, Tehran, Iran) for the valuable help with the quantitative real-time PCR analysis.
Funding
This work was supported by the Veterinary School, Shiraz University, Shiraz, Iran–Royan Institute, Tehran, Iran–Iran National Science Foundation (INSF) (Grant number 96006039), Tehran, Iran.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Supplementary Figure S1
(JPEG 3363 kb)
About this article
Cite this article
Oryan, A., Baghaban Eslaminejad, M., Kamali, A. et al. RETRACTED ARTICLE: Mesenchymal stem cells seeded onto tissue-engineered osteoinductive scaffolds enhance the healing process of critical-sized radial bone defects in rat. Cell Tissue Res 374, 63–81 (2018). https://doi.org/10.1007/s00441-018-2837-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-018-2837-7