Abstract
Periodontal ligament (PDL) cells exhibit several osteoblastic traits and are parathyroid hormone (PTH)-responsive providing evidence for a role of these cells in dental hard-tissue repair. To examine the hypothesis that PDL cells respond to PTH stimulation with changes in proliferation and apoptotic signaling through independent but convergent signaling pathways, PDL cells were cultured from human bicuspids obtained from six patients. PDL cells at different states of maturation were challenged with PTH(1–34) intermittently for 0, 1, or 24 h/cycle or exposed continuously. Specific inhibitors to protein kinases A and C (PKA, PKC) and the mitogen-activated protein kinase cascade (MAPK) were employed. At harvest, the cell number, BrdU incorporation, and DNA fragmentation were determined by means of cell counting and immunoassays. Intermittent PTH(1–34) caused a significant increase in cell number in confluent cells as opposed to a reduction in pre-confluent cells. In confluent cells, the effect resulted from a significant increase in proliferation, whereas DNA fragmentation was reduced when PTH(1–34) was administered for 1 h/cycle but increased after PTH(1–34) for 24 h/cycle. Inhibition of PKC inhibited PTH(1–34)-induced proliferation but enhanced apoptosis. Inhibition of PKA enhanced proliferation and DNA fragmentation. Similar results were obtained in less mature cells, although, in the presence of the PKA inhibitor, the PTH(1–34)-induced changes were more pronounced than in confluent cells. In the presence of the MAPK inhibitor, all of the parameters examined were reduced significantly in both maturation states. Thus, PTH(1–34) mediates proliferative and apoptotic signaling in human PDL cells in a maturation-state-dependent manner via PKC-dependent and PKA-dependent pathways.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tooth root resorption is a common side effect of orthodontic tooth movement. Although reparative cementum formation occurs occasionally, the underlying mechanisms at the cellular level remain to be elucidated. There is evidence that periodontal ligament (PDL) cells might be involved in the regulation of dental hard-tissue repair since they have been shown to exhibit several osteoblastic traits (Chou et al. 2002) indicating that they have the potential to differentiate into osteoblasts or cementoblasts (Basdra and Komposch 1997). Previously, PDL cells have been reported to respond to stimulation with parathyroid hormone (PTH) in an osteoblast-like manner with respect to differentiation and local factor production (Nohutcu et al. 1995; Ouyang et al. 2000; Lossdörfer et al. 2005). In several in vitro and in vivo model systems, intermittent low doses of PTH have been demonstrated to lead to an increase of skeletal mass as a result of accelerated bone formation (Yang et al. 1997; Iida-Klein et al. 2002) as opposed to a loss of bone through the stimulation of resorption in response to continuous administration (Lee and Lorenzo 1999). At the cellular level, increased numbers of osteoblasts have been observed following intermittent PTH(1–34) administration; this has been attributed, in part, to the stimulation of the proliferation of osteoblast precursor cells and to the prolonged survival of mature osteoblasts caused by the anti-apoptotic effect of an intermittent PTH(1–34) treatment regimen. The latter possibility is thought to be the predominant mechanism as supported by an increasing mass of literature pointing at prolonged cell survival via the inhibition of apoptosis in newly differentiated osteoprogenitor cells, as suggested by Jilka et al. (1999). The reported effects of PTH on apoptosis appear to be dependent upon the cell culture model (Zerega et al. 1999; Turner et al. 2000) and the differentiation state of the cells (Chen et al. 2002). PTH has been found to be anti-apoptotic in pre-confluent mesenchymal cells as opposed to its pro-apoptotic effects in more differentiated post-confluent cells (Chen et al. 2002). The interaction of PTH with its receptor activates several downstream signaling pathways in osteoblasts; this may, in part, account for the dual functionality of PTH. The predominant pathway seems to be the Gs-coupled activation of adenylate cyclase, resulting in increased cAMP and the activation of protein kinase A (PKA; Partridge et al. 1981). PTH also initiates Gq-coupled signaling, leading to activation of phospholipase C and the hydrolysis of phosphatidylinositol bisphosphate to inositol triphosphate and diacylglycerol, which in turn results in enhanced protein kinase C (PKC) activity (Babich et al. 1991; Civitelli et al. 1998). Whereas increases in proliferation in response to PTH at low concentrations have been linked to the PTH-dependent activation of PKC culminating in enhanced extracellular signal-regulated kinase signaling (Cole 1999; Swarthout et al. 2001), the growth arrest of UMR 106-01 cells as a consequence of continuous PTH administration has been attributed to the activation of the PKA pathway (Onishi and Hruska 1997). Other groups have found PKA activation to inhibit mitogen-activated protein kinase (MAPK) and proliferation, whereas the stimulation of ERK1/2 and proliferation by PTH has been demonstrated to be PKC-dependent in osteoblasts and kidney cells (Cole 1999; Swarthout et al. 2001).
The rationale for the present investigation has been to examine further the potential role of human PDL cells in the regulation of periodontal repair processes and to clarify whether human PDL cells respond to PTH(1–34) with changes in cell number as a result of altered proliferation and/or modified apoptotic signaling. The elucidation of the response of PDL cells to PTH stimulation, with special attention being directed to the intracellular signal transduction pathways involved, might improve our understanding of the mechanisms underlying periodontal repair and provide a potentially interesting target to influence, for example, reparative cementum formation following tooth root resorption induced by orthodontic tooth movement. We have hypothesized that PTH(1–34) exerts its effect on proliferation and apoptosis through independent but interconnected pathways involving PKC, PKA, and MAPK/ERK. We have also tested whether the maturation state of the cells and the mode of PTH(1–34) administration (pulsatile versus continuous) have an impact on the cellular response.
Materials and methods
Cell culture and PTH administration
Human periodontal ligament cells were scraped from the middle third of the roots of premolars of six different human donors, aged between 12 and 14 years, none of whom showed clinical signs of periodontitis. The teeth had been extracted for orthodontic reasons, with informed parental consent and following an approved protocol of the ethics committee of the University of Bonn. Prior to experimental use, the cells were characterized and demonstrated to express the osteoblastic markers alkaline phosphatase and osteocalcin at both the transcriptional and protein level. The cells from the six donors were not pooled. Fourth passage cells were plated in 96-well and 24-well plates (n=6), respectively, such that, at harvest, they either had reached a pre-confluent (~70%) or confluent state. Cells were cultured as described previously (Lossdörfer et al. 2006).
Previous experiments in our laboratory had shown no significant dose-dependence of the PTH effect on PDL cells (Lossdörfer et al. 2006). Thus, to assess whether PTH acted differently at different stages of maturation, pre-confluent and confluent cells were cultured in the presence of 10−12M PTH(1–34) (Sigma Aldrich, Germany) for 0, 1, and 24 h within a 48-h incubation cycle. For the remaining time, experimental media were replaced by tissue culture media without PTH(1–34). These cycles were carried out three times resulting in a total experimental period of 6 days. This intermittent treatment regimen was used to mimic the potentially anabolic effects of PTH. Additionally, cells were subjected to continuous PTH(1–34) challenge in order to investigate whether the mode of PTH administration affected the cellular response. In these cultures, the experimental media were replaced every 2 days to ensure that bioactive PTH(1–34) was continuously present in the culture system. Vehicle-treated cultures for each treatment group served as controls.
Inhibitor experiments
To examine whether changes in proliferative and apoptotic signaling in response to PTH(1–34) involved PKA, PKC, or MAPK, one of the following (Calbiochem, Germany) was added to the media for the entire experimental period: the PKC inhibitor RO-32-0432 (1 μM), the PKA inhibitor H8 (10 μM), or the inhibitor U0126 (20 μM), which inhibits the immediate upstream activators of MAPK, viz., mitogen-activated protein kinase kinase 1 and 2 (MEK1 and MEK2). The inhibitor concentrations used had been confirmed as being effective in PDL cells in preliminary experiments (data not shown). Vehicle-treated (ethanol for PTH(1–34); DMSO for RO-32-0432 and U0126; H2O for H8) cultures for each treatment group and cells cultured in the presence of the respective inhibitors but without PTH(1–34) served as controls.
Cell number
At harvest, cells were released from the culture surface by trypsinization for 10 min at 37°C. This reaction was terminated by the addition of DMEM containing 10% FBS. Thereafter, the cell suspension was centrifuged, and the cell pellet was resuspended in 0.9% NaCl. Finally, the cell number was determined by the use of a cell counter (Moelab, Hilgen, Germany). Cells harvested in this manner exhibited >95% viability based on Trypan-blue exclusion.
Proliferation assay
Cell proliferation was determined by measuring 5-bromo-2-deoxyuridine (BrdU) incorporation into the DNA of proliferating cells. The incorporation of BrdU into DNA over a time-period of 4 h was detected by enzyme-linked immunosorbent assay (ELISA; Roche, Germany). Absorbance was read with an ELISA reader at 450 nm and 690 nm as reference wavelengths.
DNA fragmentation assay
Since the biochemical hallmark of apoptosis is the fragmentation of the genomic DNA (an irreversible event committing the cell to die and occurring before changes in plasma membrane permeability), DNA fragmentation in cell lysates was determined by using a commercially available kit (Roche, Germany). This assay was based on a quantitative sandwich-enzyme-immunoassay principle with mouse monoclonal antibodies directed against DNA and histones, respectively, allowing the specific determination of mononucleosomes and oligonucleosomes in the cytoplasmic fraction of cell lysates. The amount of nucleosomes retained in the immunocomplex was determined photometrically with 2,2’-azino-di-(3-ethylbenzthiazoline sulfonate as substrate at 405 nm and 490 nm as reference wavelengths.
Calculation of results and statistical analysis
From all data obtained, the adsorption at the onset of PTH(1–34) administration (T0) was subtracted, and the mean value for the vehicle control at each maturation stage was set to 100% and served as a reference. For any given experiment, each data point represented the mean ±SEM of six independent cultures. Variance and statistical significance of data were analyzed by using Bonferroni’s modification of Student’s t-test. P-values of <0.05 were considered to be significant. Each set of experiments was repeated twice and analyzed separately, and both sets of experiments yielded comparable results. Only one set of results from the two sets of experiments are presented.
Results
Vehicle-treated cultures for each experimental group at a particular maturation state did not differ from each other or from untreated controls significantly and, therefore, in all of the figures only one vehicle-treated control for each maturation state is presented. At the beginning of PTH(1–34) exposure, in pre-confluent PDL cells, the cell number was 0.04±0.005×105 cells/well, whereas confluent contained 0.14±0.015×105 cells/well.
Effect of PTH(1–34) on cell number, proliferation, and apoptosis
In pre-confluent cultures, intermittent PTH(1–34) reduced the cell number significantly, and this effect was further pronounced when PTH(1–34) was administered continuously. In confluent cultures, intermittent PTH(1–34) for 1 h/cycle and 24 h/cycle induced a significant increase of the cell number. A similar trend was observed when PTH(1–34) was administered continuously, although the effect was less pronounced and not significant (Fig. 1a).
Effect of PTH(1–34) treatment on regulation of cell number (a), proliferation as determined by measuring BrdU-incorporation (b), and DNA fragmentation as determined by mononucleosomes and oligonucleosomes in the cytoplasmic fraction of cell lysates in pre-confluent and confluent PDL cells (c). Cells were either treated intermittently with 10−12 M PTH(1–34) for 0, 1, or 24 h during three cycles of 48 h each or were challenged continuously (cont). Vehicle-treated cultures for each experimental group served as controls (vehicle). Since control groups did not differ significantly from each other, only one control per maturation state is presented. At harvest, cells were counted with a cell counter. Adsorption at the onset of PTH(1–34) administration (T0) was subtracted from all data obtained for b, c, and the mean value for the vehicle control at each maturation stage was set to 100% and served as a reference. Data were acquired from one of two separate experiments, both yielding comparable results. Each value is the mean+SEM for six independent cultures. *P<0.05, experimental group vs. vehicle-treated control at a particular maturation state; ● P<0.05, experimental group vs. same treatment for 1 h/cycle at a particular maturation state
At all maturation states examined, intermittent PTH(1–34) for 24 h/cycle caused a significant increase in proliferative activity with the greatest effect in pre-confluent cultures. PTH(1–34) for 1 h/cycle and continuous exposure had no effect on proliferation except for confluent cultures in which continuous PTH(1–34) also enhanced proliferation (Fig. 1b). With regard to apoptosis, both intermittent PTH(1–34) for 24 h/cycle and continuous exposure enhanced DNA fragmentation significantly at all maturation stages examined. The effect was greater following intermittent PTH(1–34) as compared with continuous administration. In confluent cells, PTH(1–34) for 1 h/cycle resulted in a significant reduction in DNA fragmentation (Fig. 1c).
Effect of PKC inhibition
Inhibition of PKC significantly reduced the cell number in pre-confluent cultures. When pre-confluent cultures were challenged with PTH(1–34), the induced reduction in cell number was even more pronounced in the presence of the PKC inhibitor, regardless of the mode of PTH(1–34) administration. In more mature cells, inhibition of PKC itself had no effect on cell number. Mature cultures challenged with PTH(1–34) in the presence of the PKC inhibitor exhibited an inhibition of the induced increase in cell number (Fig. 2a).
Effect of PKC inhibitor on the regulation of cell number (a), proliferation as determined by measuring BrdU-incorporation (b), and DNA fragmentation as determined by mononucleosomes and oligonucleosomes in the cytoplasmic fraction of cell lysates in pre-confluent and confluent PDL cells (c). Cells were either cultured with control media or treated intermittently with 10−12 M PTH(1–34) for 0, 1, or 24 h during three cycles of 48 h each or challenged continuously (cont). Experimental media were supplemented with the PKC inhibitor RO-32-0432 (1 μM) for the entire experimental period. Vehicle-treated cultures served as controls (Control) as did cultures treated with the inhibitor alone (2nd, 4th bars of Control). Adsorption at the onset of PTH(1–34) administration (T0) was subtracted from all data obtained, and the mean value for the vehicle control at each maturation stage was set to 100% and served as a reference. Data were acquired from one of two separate experiments, both yielding comparable results. Each value is the mean+SEM for six independent cultures. *P<0.05, experimental group vs. control at the same maturation state; # P<0.05, experimental group vs. PTH(1–34) treated group at the same time point and maturation state; ● P<0.05, experimental group vs. same treatment for 1 h/cycle at a particular maturation state; $ P<0.05, experimental group vs. same treatment for 24 h/cycle at a particular maturation state
The PKC inhibitor alone had no effect on proliferation in pre-confluent cells, neither did it affect the increase in proliferative activity in response to intermittent PTH(1–34). However, when PTH(1–34) was administered continuously, proliferation was reduced significantly in the presence of the inhibitor. In confluent cells, BrdU-incorporation was reduced significantly in the presence of the PKC inhibitor, but the inhibitor was only weakly effective in reducing the increase in proliferation following intermittent PTH(1–34) administration. When cells were exposed to PTH(1–34) continuously, RO-32-0432 inhibited the induced increase in proliferation (Fig. 2b). With regard to DNA fragmentation, intermittent PTH(1–34) exposure of the cells in the presence of the PKC inhibitor led to a significant enhancement of DNA fragmentation as compared with PTH(1–34) alone, both in pre-confluent and in confluent cells. The effect of continuous PTH(1–34) exposure was not altered by inhibition of PKC (Fig. 2c).
Effect of PKA inhibition
Inhibition of PKA for the entire culture period had no effect on cell number in pre-confluent cells. When the cultures were challenged with intermittent PTH(1–34) in the presence of the PKA inhibitor, cell numbers increased significantly as compared with intermittent PTH(1–34) treatment alone. In cultures that were continuously exposed to PTH(1–34), inhibition of PKA resulted in a further reduction of the cell number as compared with PTH(1–34) alone. Similar observations were made in confluent cultures, although the changes in cell number in response to PTH(1–34) for 1 h/cycle in the presence of the PKA inhibitor displayed a trend rather than statistical significance (Fig. 3a). Inhibition of PKA resulted in an increase of proliferative activity at all maturation states examined and further enhanced the increase in proliferation in response to PTH(1–34), regardless of the mode of its administration. The effect was most obvious when the cultures were exposed to PTH(1–34) for 24 h/cycle (Fig. 3b). When the PKA inhibitor was present throughout the experimental period, DNA fragmentation was reduced in pre-confluent and confluent cells (Fig. 3c). Both intermittent PTH(1–34) for 1 h/cycle or continuous exposure in the presence of the PKA inhibitor resulted in an increase of DNA fragmentation as compared with PTH(1–34) alone. In contrast, PTH(1–34) for 24 h/cycle with simultaneous inhibition of PKA reduced DNA fragmentation (Fig. 3c).
Effect of PKA inhibitor on the regulation of cell number (a), proliferation as determined by measuring BrdU-incorporation (b), and DNA fragmentation as determined by mononucleosomes and oligonucleosomes in the cytoplasmic fraction of cell lysates in pre-confluent and confluent PDL cells (c). Cells were either cultured with control media or treated intermittently with 10−12 M PTH(1–34) for 0, 1, or 24 h during three cycles of 48 h each or challenged continuously (cont). Experimental media were supplemented with the PKA inhibitor H8 (10 μM) for the entire experimental period. Vehicle-treated cultures served as controls (Control) as did cultures treated with the inhibitor alone (2nd, 4th bars of Control). Adsorption at the onset of PTH(1–34) administration (T0) was subtracted from all data obtained, and the mean value for the vehicle-treated control at each maturation stage was set to 100% and served as a reference. Data were acquired from one of two separate experiments, both yielding comparable results. Each value is the mean+SEM for six independent cultures. *P<0.05, experimental group vs. control at a particular maturation state; # P<0.05, experimental group vs. PTH(1–34) treated group at the same time point and maturation state; ● P<0.05, experimental group vs. same treatment for 1h/cycle at a particular maturation state; $ P<0.05, experimental group vs. same treatment for 24 h/cycle at a particular maturation state
Effect of MAPK inhibition
Inhibition of MAPK/ERK1/2 resulted in a significant reduction in cell number, proliferative activity, and DNA fragmentation at all maturation states examined. When cells were challenged with PTH(1–34) in the presence of the ERK1/2 inhibitor, the PTH(1–34)-induced increase in cell number, proliferation, and apoptosis in pre-confluent cells was reduced to levels observed in cultures treated with the inhibitor alone. In confluent cells, the PTH(1–34) effect was also reduced but not to control levels (Fig. 4a–c).
Effect of MAPK/ERK inhibitor on the regulation of cell number (a), proliferation as determined by measuring BrdU-incorporation (b), and DNA fragmentation as determined by mononucleosomes and oligonucleosomes in the cytoplasmic fraction of cell lysates in pre-confluent and confluent PDL cells (c). Cells were either cultured with control media or treated intermittently with 10−12 M PTH(1–34) for 0, 1, or 24 h during three cycles of 48 h each or challenged continuously (cont). Experimental media were supplemented with the MAPK/ERK inhibitor U0126 (20 μM) for the entire experimental period. Vehicle-treated cultures served as controls (Control) as did cultures treated with the inhibitor alone (2nd, 4th bar of Control). Adsorption at the onset of PTH(1–34) administration (T0) was subtracted from all data obtained, and the mean value for the vehicle-treated control at each maturation stage was set to 100% and served as a reference. Data were acquired from one of two separate experiments, both yielding comparable results. Each value is the mean+SEM for six independent cultures. *P<0.05, experimental group vs. control at a particular maturation state; # P<0.05, experimental group vs. PTH(1–34) treated group at the same time point and maturation state; ● P<0.05, experimental group vs. same treatment for 1 h/cycle at a particular maturation state; $ P<0.05, experimental group vs. same treatment for 24 h/cycle at a particular maturation state
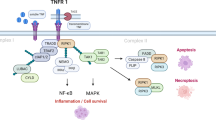
The results are summarized in Fig. 5, which illustrates the effect of PTH(1–34) on human periodontal ligament cells in vitro with respect to cell number, proliferation, and apoptosis (Fig. 5a) and to the intracellular signal transduction pathways involved in mediating the cellular response (Fig. 5b).
Representation of the effect of intermittent exposure of human PDL cells to PTH(1–34) in vitro with respect to cell number, proliferation, and apoptosis (a) with special consideration of the intracellular signal transduction pathways (b) involved (blue circles with + stimulation of a particular parameter in pre-confluent PDL cells, blue circles with − inhibition of a particular parameter in pre-confluent PDL cells, red circles with + stimulation of a particular parameter in confluent PDL cells, red circles with − inhibition of a particular parameter in confluent PDL cells)
Discussion
In this study, pre-confluent and confluent human PDL cells were employed in order to determine the cellular response to PTH(1–34) and the pathways involved. As one specific aim, we sought to elucidate the impact of the maturation state of the cells on the cellular response. Previously, we demonstrated that the degree of confluence of PDL cells was correlated with the expression of differentiation markers as evidenced by lower levels of alkaline phosphatase specific activity and osteocalcin expression in pre-confluent cells as opposed to higher levels in confluent cells (Lossdörfer et al. 2006). Thus, we consider it justified to regard pre-confluent cells as being less mature and confluent cells as being more mature. The term “pre-confluent” will therefore be used synonymously with “less mature”, and “confluent” as equivalent to “more mature”, throughout the following discussion of the results.
Role of intermittent PTH(1–34) in mediating changes in cell number, proliferation, and apoptosis
Our in vitro data show that PTH(1–34) modulates the cell number of human PDL cells as a result of altered proliferative and apoptotic signaling in a maturation-stage-dependent manner. Previous studies have demonstrated that low-dose PTH exposure results in increased proliferation of osteoprogenitor cells (Nakajima et al. 2002). This is in agreement with our observations of enhanced cell numbers as a result of enhanced proliferation together with reduced apoptosis following intermittent PTH(1–34) for 1 h/cycle and enhanced DNA fragmentation after PTH(1–34) for 24 h/cycle in confluent PDL cell cultures. Thus, PTH(1–34) might shift the balance between proliferation and apoptosis resulting in a dominance of mitosis over apoptosis, in turn leading to increased cell numbers in more mature cells. In less mature cells, similar changes in proliferation and apoptosis have been observed in response to PTH(1–34), although they are less pronounced in magnitude, resulting in a net decrease in cell number. In these pre-confluent cultures, PTH(1–34) might alter the ratio of proliferation over apoptosis in favor of DNA fragmentation. The simultaneous increase in proliferation and apoptosis at both maturation stages is not surprising, since proliferation has been found to be inevitably associated with apoptosis through the actions of tumor suppressor genes, such as p53, which controls key stages of the cell cycle to ensure that cells in which DNA becomes significantly flawed are eliminated through cell death (Evan and Littlewood 1998; Sheikh and Fornance 2000). Based on the data obtained in this study, the reason less mature PDL cells are apparently more susceptible to death signals than more mature cultures remains a matter of speculation. Since the ratio of the amount of anti-apoptotic to pro-apoptotic members of the Bcl-2 family expressed by cells has been found to determine their ability to resist death signals (Scorrano et al. 2003), one might hypothesize that less mature PDL cells express a smaller amount of anti-apoptotic survival genes. The PTH(1–34)-induced decrease in cell number in pre-confluent cells is accompanied by increased alkaline phosphatase specific activity and osteocalcin production (Lossdörfer et al. 2005, 2006), and therefore, the inhibition of proliferation has to be interpreted in the light of a simultaneous enhancement of differentiation.
Role of PKC, PKA, and MAPK/ERK in mediating PTH(1–34)-induced changes in proliferation
The present data also provide insight into the mechanisms involved in regulating the cell number of PDL cells. The PKC inhibitor RO-32-0432 decreases the cell number of pre-confluent cells and has no effect on this parameter in more mature cells. When PDL cells are challenged with intermittent PTH(1–34) in the presence of the PKC inhibitor, the cell number is further reduced in pre-confluent cells and in confluent cells as compared with treatment with the inhibitor alone. Thus, the PTH(1–34)-induced increase in cell number is inhibited. Similar observations have been made when BrdU incorporation is measured: the mitogenic activity of PTH(1–34) is reduced when PKC is inhibited. These results indicate that intermittent PTH(1–34) affects proliferative signaling of PDL cells through a PKC-dependent pathway, as PKC activity is necessary for pro-proliferative signaling. This finding is corroborated by several reports from other groups. Sömjen et al. (1987) have shown that the mitogenic activity of PTH can be mimicked by a variety of PKC activators. The same authors have subsequently demonstrated that fragments lacking the adenyl-cyclase-activating domain but retaining the PKC-activating domain can still stimulate the proliferation of rat osteoblastic cells (Sömjen et al. 1990). Further support comes from data presented by Sabatini et al. (1996) who have found that stimulation of PKC by phorbol 12-myristate-13-acetate results in enhanced proliferation of mouse calvaria cells. Additionally, the stimulation of ERK1/2 and proliferation by PTH has been demonstrated to be PKC-dependent in osteoblasts and kidney cells (Cole 1999; Swarthout et al. 2001). Interestingly, the PTH effect on proliferation seems to vary with the cell type studied, since PTH stimulates the proliferation of bone cells (MacDonald et al. 1996; Scutt et al. 1994), chondrocytes (Koike et al. 1990), and hypercalcemic carcinoma cells (Benitez-Verguizas and Esbrit 1994), whereas it inhibits the proliferation of keratinocytes (Kaiser et al. 1992) and lymphocytes (Adachi et al. 1990). Since the PDL cells employed in this study exhibit several osteoblastic traits, they respond to intermittent PTH(1–34) in an osteoblast-like manner with an increased proliferation; this increase is dependent on PKC signaling.
In contrast to the effect of inhibiting PKC, inhibition of PKA with H8 results in an increase in cell number at both maturation states examined. This observation is paralleled by an enhancement of proliferation following the inhibition of PKA. When cells are exposed to intermittent PTH(1–34) in the presence of H8, we have observed an even more pronounced increase in proliferation as compared with intermittent PTH(1–34) alone. These findings suggest that intermittent PTH(1–34) also activates the adenyl cyclase/PKA pathway in human PDL cells, resulting in an anti-mitogenic response and inhibition of proliferation. Our conclusion is supported by studies of various specific agonists of the PKA pathway indicating the role of the PKA pathway in inhibiting cell proliferation (Sabatini et al. 1996) by the inhibition of ERK1/2 (Siddhanti et al. 1995; Verheijen and Defize 1995). ERK1/2 is one of the components involved in the complex kinase cascade ultimately triggering the proliferative response, as has been shown, for example, in fibroblasts (Pages et al. 1993; Troppmair et al. 1994). ERK1/2 is activated by PKC in fibroblasts (Troppmair et al. 1994), whereas PKA interferes with the ERK1/2 pathway in fibroblasts, adipocytes, and smooth muscle cells (Burgering and Bos 1995). Consequently, although we have not measured ERK1/2 activity directly, the pro-proliferative role that we have demonstrated for PKC in response to PTH(1–34) stimulation probably also involves the activation of ERK1/2 in PDL cells, as opposed to the anti-proliferative effect of the PTH(1–34)-induced PKA signaling that might occur through the inhibition of ERK1/2. When we inhibited ERK1/2 with the specific inhibitor UO126, proliferation was reduced significantly. UO126 also inhibited the PTH(1–34)-induced increase in proliferation in pre-confluent cells and markedly reduced the increase in more mature cells, although BrdU incorporation was still above the levels observed for control cultures treated with the inhibitor alone. This might be explained by the concentration that we used for the inhibitor, which was comparatively low. The ERK1/2 inhibitor UO126 has been reported to require a concentration of at least 100 μM to interfere with proliferation. This certainly does not hold true for the cells that we have employed in our experiments but might explain why inhibition of ERK1/2 does not completely abolish either proliferation or the increase in proliferation following PTH(1–34) challenge in our PDL cell cultures.
Role of PKC, PKA, and MAPK/ERK in mediating PTH(1–34)-induced changes in DNA fragmentation
In our hands, intermittent and continuous PTH(1–34) treatment results in enhanced apoptosis of human PDL cells at both maturation states examined. This contradicts other reports that intermittent PTH is anti-apoptotic (Jilka et al. 1999), whereas continuous PTH is pro-apoptotic (Bellido et al. 2003). Chen and coworkers (2002) have found that PTH exerts anti-apoptotic effects in pre-confluent cells as opposed to pro-apoptotic signaling in response to PTH in more differentiated post-confluent cells. As can be discussed for every other parameter examined in this study, part of our experimental results can be explained by the differences between our PDL cells and the osteoblasts employed in various other studies. Indeed, the cell lines and species employed and the different experimental conditions most likely play a significant role in the disparities of our experimental findings relative to previously published material. Additionally, the reported effects of PTH on apoptosis have been shown to be dependent on the cell culture system. PTH is reported to be anti-apoptotic in osteoblasts (Jilka et al. 1999) and chick embryo hypertrophic chondrocytes (Zerega et al. 1999), whereas it promotes apoptosis in 293 cells, a transformed primary embryonal kidney cell line (Turner et al. 2000). The similar response in apoptotic signaling in pre-confluent and confluent cells in our experiements might be explained by the degree of confluence that our pre-confluent cells have been allowed to reach (~70%). Had the cells been maintained in a less confluent stage, one might have observed a different response to PTH(1–34) with respect to apoptosis. In our experiments, inhibition of PKC did not affect DNA fragmentation in pre-confluent cells but reduced it significantly in more mature cells suggesting that PKC is involved in apoptotic signaling in confluent PDL cells. Additionally, inhibition of PKC further added to the pro-apoptotic effect of intermittent PTH(1–34) indicating that the pro-apoptotic effect of PTH(1–34) occurs not through PKC but by means of some other pathway. This finding is supported by the results of Turner et al. (2000) who have reported PKC inhibition to be only weakly effective in inhibiting PTH-induced cell death in 293 cells, suggesting a small contribution of PKC activation to apoptotic signaling, as has also been observed in other systems (Lucas and Sanchez-Margalet 1995). In human PDL cells, the PKA pathway seems to be involved in apoptotic signaling as evidenced by the significant reduction of DNA fragmentation when the PKA inhibitor is employed. However, inhibition of PKA failed to abrogate the PTH(1–34)-induced enhancement of DNA fragmentation, except in the 24 h/cycle group, but further augmented the effect seen for PTH(1–34) alone, indicating that the pro-apoptotic effect of intermittent PTH(1–34) for 24 h/cycle is mediated through PKA, whereas apoptotic signaling in response to PTH(1–34) for 1 h/cycle and continuous PTH(1–34) administration are not. Other studies have identified cAMP as part of the PKA pathway suppressing apoptosis in rat periosteal cells (Machwate et al. 1998) and human osteoblasts (Habener et al. 1984); this is in agreement with our observation of the impact of the PKA pathway in apoptosis following intermittent PTH(1–34) for 24 h/cycle.
Inhibition of the ERK1/2 pathway significantly reduced DNA fragmentation at both maturation states examined but did not completely abolish it and also proved effective in inhibiting the PTH(1–34)-induced increase in DNA fragmentation in pre-confluent cells. In more mature cultures, PTH(1–34)-induced apoptosis was also reduced but not to control levels, which, as discussed above, might be explained by the concentration of the inhibitor that we employed. These findings indicate that ERK1/2 is involved in the signaling cascade of the PTH(1–34) effect on PDL cell apoptosis.
Significance of the mode of PTH(1–34) administration
We have not observed any converse effects of continuous PTH(1–34) treatment as compared with intermittent exposure with respect to the pathways involved in the response of the cells. Ma and coworkers (2001) have observed continuous PTH effects as early as after 1 h in a rat model, with a peak after 6 h. Our measurements have been obtained after a culture period of up to 10 days. Although PTH receptor levels and responsiveness of the receptor to stimulation appear to increase during osteoblastic phenotypic maturation in vitro (McCauley et al. 1996; Bos et al. 1996; Kondo et al. 1997), sustained PTH stimulation for a culture period of 10 days might lead to a down-regulation of the number or sensitivity of PTH receptors in PDL cells as part of a feedback mechanism. This might at least in part explain our results. An explanation for the dual effects of continuous versus pulsatile PTH treatment regimens observed in vivo arises from the unresolved question of the way that the dynamic response of the PTH1 receptor (PTH1R) is related to PTH action on bone and to the differential effects of continuous versus pulsatile PTH dosing. Qin et al. (2004) propose that negative feedback loops in the PTH1R-mediated signaling networks lead to long-term desensitization of signal when dosing is continuous, whereas pulsatile doses achieve more signaling over time because the system resensitizes between doses.
Concluding remarks
The data presented in this study provide evidence that PTH(1–34) modifies proliferative and apoptotic signaling in human PDL cells via PKC-dependent and PKA-dependent pathways. In addition to the changes in local factor production in response to PTH(1–34), which we reported earlier, the present findings add further support to the assumption that PDL cells are regulatorily involved in dental hard-tissue repair and represent a potentially interesting target in order to influence reparative processes, such as reparative cementum formation following tooth root resorption induced by orthodontic tooth movement.
References
Adachi N, Yamaguchi K, Miyaki Y, Honda S, Nagasaki K, Akiyama Y, Adachi I, Abe K (1990) Parathyroid hormone related protein is a possible autocrine growth inhibitor for lymphocytes. Biochem Biophys Res Commun 166:1088–1094
Babich M, Choi H, Johnson RM, King KL, Alford NE, Nissenson RA (1991) Thrombin and parathyroid hormone mobilize intracellular calcium in rat osteosarcoma cells by distinct pathways. Endocrinology 129:1463–1470
Basdra EK, Komposch G (1997) Osteoblast-like properties of human periodontal ligament cells: an in vitro analysis. Eur J Orthod 19:615–621
Bellido T, Ali AA, Plotkin LI, Fu Q, Gubrij I, Roberson PK, Weinstein RS, O’Brien CA, Manolagas SC, Jilka RL (2003) Proteasomal degradation of Runx2 shortens parathyroid hormone-induced anti-apoptotic signaling in osteoblasts. A putative explanation for why intermittent administration is needed for bone anabolism. J Biol Chem 278:50259–50272
Benitez-Verguizas J, Esbrit P (1994) Proliferative effect of parathyroid hormone-related protein on the hypercalcemic walker 256 carcinoma cell line. Biochem Biophys Res Commun 198:1281–1289
Bos MP, Meer JM van der, Feyen JH, Herrmann-Erlee MP (1996) Expression of the parathyroid hormone receptor and correlation with other osteoblastic parameters in fetal rat osteoblasts. Calcif Tissue Int 58:95–100
Burgering BMT, Bos JL (1995) Regulation of ras-mediated signaling: more than one way to skin a cat. Trends Biochem Sci 20:18–22
Chen H, Demiralp B, Schneider A, Koh A, Silve C, Wang C, McCauley LK (2002) Parathyroid hormone and parathyroid hormone-related protein exert both pro- and anti-apoptotic effects in mesenchymal cells. J Biol Chem 277:19374–19381
Chou AM, Sae-Lim V, Lim T, Schantz J, Teoh S, Chew A (2002) Culturing and characterization of human periodontal ligament fibroblasts—a preliminary study. Mater Sci Eng 20:77–83
Civitelli R, Reid IR, Westbrook S, Avioli LV, Hruska KA (1998) PTH elevates inositol polyphosphates and diacylglycerol in a rat osteoblast-like cell line. Am J Physiol 255:E660–E667
Cole JA (1999) Parathyroid hormone activates mitogen-activated protein kinase in opossum kidney cells. Endocrinology 140:5771–5779
Evan G, Littlewood T (1998) A matter of life and cell death. Science 281:1317–1321
Habener JF, Rosenblatt M, Potts JT Jr (1984) Parathyroid hormone: biochemical aspects of biosynthesis, secretion, action on anabolism. Physiol Rev 64: 984–1053
Iida-Klein A, Zhou H, Lu S, Levine LR, Ducayen-Knowles M, Dempster DW, Nieves J, Lindsay R (2002) Anabolic action of parathyroid hormone is skeletal site specific at the tissue and cellular levels in mice. J Bone Miner Res 17:808–816
Jilka RL, Weinstein RS, Bellido T, Roberson P, Parfitt AM, Manolagas SC (1999) Increased bone formation by prevention of osteoblast apoptosis with parathyroid hormone. J Clin Invest 104:439–446
Kaiser SM, Laneauville P, Bernier SM, Rhim JS, Kremer R, Goltzman D (1992) Enhanced growth of a human keratinocyte cell line induced by antisense RNA for parathyroid hormone-related peptide. J Biol Chem 267:13623–13628
Koike T, Iwamoto M, Shimazu A, Nakashima K, Suzuki F, Kato Y (1990) Potent mitogenic effects of parathyroid horone (PTH) on embryonic chick and rabbit chondrozytes. J Clin Invest 85:626–631
Kondo H, Ohyama T, Ohya K, Kasugai S (1997) Temporal changes of mRNA expression of matrix proteins and parathyroid hormone and parathyroid hormone-related protein (PTH/PTHrP) receptor in bone development. J Bone Miner Res 12:2089–2097
Lee SK, Lorenzo JA (1999) Parathyroid hormone stimulates TRANCE and inhibits osteoprotegerin messenger ribonucleic acid expression in murine bone marrow cultures: correlation with osteoclast-like cell formation. Endocrinology 140:3552–3561
Lossdörfer S, Götz W, Jäger A (2005) PTH(1–34) affects OPG production in human PDL cells in vitro. J Dent Res 84:634–638
Lossdörfer S, Stier S, Götz W, Jäger A (2006) Maturation-state dependent response of human periodontal ligament cells to an intermittent parathyroid hormone exposure in vitro. J Periodontal Res 41:62–72
Lucas M, Sanchez-Margalet V (1995) Protein kinase C involvement in apoptosis. Gen Pharmacol 26:881–887
Ma YL, Cain R, Halladay D, Yang X, Zeng Q, Miles R, Chandrasekhar S, Martin TJ, Onyia JE (2001) Catabolic effects of continuous human PTH (1–38) in vivo is associated with sustained stimulation of RANKL and inhibition of osteoprotegerin and gene-associated bone formation. Endocrinology 142:4047–4054
MacDonald BR, Gallagher JA, Russell RGG (1996) Parathyroid hormone stimulates the proliferation of cells derived from human bone. Endocrinology 118:2445–2449
Machwate M, Rodan SB, Rodan GA, Harada SI (1998) Sphingosine kinase mediates cyclic AMP suppression of apoptosis in rat periosteal cells. Mol Pharmacol 54:70–77
McCauley LK, Koh AJ, Beecher CA, Cui Y, Rosol TJ, Franceschi RT (1996) PTH/PTHrP receptor is temporally regulated during osteoblast differentiation and is associated with collagen synthesis. J Cell Biochem 61:638–647
Nakajima A, Shimoji N, Shiomi K, Shimizu S, Moriya H, Einhorn TA, Yamazaki M (2002) Mechanisms for the enhancement of fracture healing in rats treated with intermittent low-dose human parathyroid hormone (1–34). J Bone Miner Res 17:2038–2047
Nohutcu RM, Somerman MJ, McCauley LK (1995) Dexamethasone enhances the effects of parathyroid hormone on human periodontal ligament cells in vitro. Calcif Tissue Int 56:571–577
Onishi T, Hruska K (1997) Expression of p27Kip1 in osteoblast-like cells during differentiation with parathyroid hormone. Endocrinology 138:1995–2004
Ouyang H, McCauley L, Berry J, D’Errico J, Strayhorn C, Somerman M (2000) Response of immortalized murine cementoblasts/periodontal ligament cells to parathyroid hormone and parathyroid hormone related protein in vitro. Arch Oral Biol 45:293–303
Pages G, Lenormand P, L’Allemain G, Chambard JC, Meloche S, Pouyssegur J (1993) Mitogen-activated protein kinase p42mapk and p44mapk are required for fibroblast proliferation. Proc Natl Acad Sci USA 90:8319–8323
Partridge NC, Alcorn D, Michelangeli VP, Kemp BE, Ryan GB, Martin TJ (1981) Functional properties of hormonally responsive cultured normal and malignant rat osteoblastic cells. Endocrinology 108:213–219
Qin L, Raggatt LJ, Partridge NC (2004) Parathyroid hormone: a double-edged sword for bone metabolism. Trends Endocrinol Metab 15:60–65
Sabatini M, Lesur C, Pacherie M, Pastoureau P, Kucharczyk N, Fauchiere JL, Bonnet J (1996) Effects of parathyroid hormone and agonists of the adenyl cyclase and protein kinase C pathways on bone cell proliferation. Bone 18:59–65
Scorrano L, Oakes SA, Opferman JT, Cheng EH, Sorcinelli MD, Pozzan T, Korsmeyer SJ (2003) BAX and BAK regulation of endoplasmic reticulum Ca2+: a control point for apoptosis. Science 300:135–139
Scutt A, Duvos C, Lauber J, Mayer H (1994) Time-dependent effects of parathyroid hormone and prostaglandin E2 on DNA synthesis by periosteal cells from embryonic chick calvariae. Calcif Tissue Int 55:208–215
Sheikh M, Fornance A (2000) Death and decoy receptors and p53-mediated apoptosis. Leukemia 14:1509–1513
Siddhanti SR, Hartle JE 2nd, Quarles LD (1995) Forskolin inhibits protein kinase C-induced mitogen activated protin kinase activity in MC3T3-E1 osteoblasts. Endocrinology 136:4834–4841
Sömjen D, Zor U, Kaye AM, Harell A, Binderman I (1987) Parathyroid hormone induction of creatine kinase activity and DNA synthesis is mimicked by phospholipase C, diacyglycerol and phorbol ester. Biochim Biophys Acta 931:215–223
Sömjen D, Binderman I, Schlüter KD, Wingender F, Mayer H, Kaye AM (1990) Stimulation by defined parathryoid hormone fragments of cell proliferation in skeletal-derived cell cultures. Biochem J 272:781–785
Swarthout JT, Doggett TA, Lemker JL, Partridge NC (2001) Stimulation of extracellular signal-regulated kinases and proliferation in rat osteoblastic cells by parathyroid hormone is protein kinase C-dependent. J Biol Chem 276:7586–7592
Troppmair J, Bruder JT, Munoz H, Lloyd PA, Kyriakis J, Banerjee P, Avruch J, Rapp UR (1994) Mitogen-activated protein kinase/extracellular signal-regulated protein kinase activation by oncogenes, serum, and 12-O-tetradecanoylphorbol-13-acetate requires raf and is necessary for transformation. J Biol Chem 269:7030–7035
Turner PR, Mefford S, Christakos S, Nissenson RA (2000) Apoptosis mediated by activation of the G protein-coupled receptor for parathyroid hormone (PTH)/PTH-related protein (PTHrP). Mol Endocrinol 14:241–254
Verheijen MH, Defize LH (1995) Parathyroid hormone inhibits mitogen-activated protein kinase activation in osteosarcoma cells via a protein kinase A-dependent pathway. Endocrinology 136:3331–3337
Yang ZJ, Cheng V, Barnes S, Cavalho L, Sindrey D (1997) Pulsatile parathyroid hormone (PTH) treatment increases bone formation in vitro in fetal rat calvarial cell (FRCC) culture system. J Bone Miner Res 12 (Suppl 1):S317
Zerega B, Cermelli S, Bianco P, Cancedda R, Cancedda FD (1999) Parathyroid hormone [PTH(1–34)] and parathyroid hormone-related protein [PTHrP(1–34)] promote reversion of hypertrophic chondrocytes to a prehypertrophic proliferating phenotype and prevent terminal differentiation of osteoblast-like cells. J Bone Miner Res 14:1281–1289
Acknowledgements
The authors thank K. Hoffmann for technical assistance and C. Maelicke for her help in preparing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
This research was supported by research grants from the BONFOR program (O-135.0006) of the University of Bonn, Bonn, Germany and the Deutsche Forschungsgemeinschaft (DFG; LO-1181/1-1).
Rights and permissions
About this article
Cite this article
Lossdörfer, S., Götz, W., Rath-Deschner, B. et al. Parathyroid hormone(1–34) mediates proliferative and apoptotic signaling in human periodontal ligament cells in vitro via protein kinase C-dependent and protein kinase A-dependent pathways. Cell Tissue Res 325, 469–479 (2006). https://doi.org/10.1007/s00441-006-0198-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-006-0198-0