Abstract
Free fatty acids (FFA) have generally been proposed to regulate pancreatic insulin release by an intracellular mechanism involving inhibition of CPT-1. The recently de-orphanized G-protein coupled receptor, FFA1R/GPR40, has been shown to be essential for fatty-acid-stimulated insulin release in MIN6 mouse insulinoma cells. The CPT-1 inhibitor, 2-bromo palmitate (2BrP), was investigated for its ability to interact with mouse FFA1R/GPR40. It was found to inhibit phosphatidyl inositol hydrolysis induced by linoleic acid (LA) (100 μM in all experiments) in HEK293 cells transfected with FFA1R/GPR40 and in the MIN6 subclone, MIN6c4. 2BrP also inhibited LA-stimulated insulin release from mouse pancreatic islets. Mouse islets were subjected to antisense intervention by treatment with a FFA1R/GPR40-specific morpholino oligonucleotide for 48 h. Antisense treatment of islets suppressed LA-stimulated insulin release by 50% and by almost 100% when islets were pretreated with LA for 30 min before applying the antisense. Antisense treatment had no effect on tolbutamide-stimulated insulin release. Confocal microscopy using an FFA1R/GPR40-specific antibody revealed receptor expression largely localized to the plasma membrane of insulin-producing cells. Pretreating the islets with LA for 30 min followed by antisense oligonucleotide treatment for 48 h reduced the FFA1R/GPR40 immunoreactivity to background levels. The results demonstrate that FFA1R/GPR40 is inhibited by the CPT-1 inhibitor, 2BrP, and confirm that FFA1R/GPR40 is indeed necessary, at least in part, for fatty-acid-stimulated insulin release.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glucose and free fatty acids (FFAs) are the two most important regulators of insulin release. Medium-chain to long-chain fatty acids (FAs) are known to have pleiotropic effects on the pancreatic β-cell; while acute administration of FFAs stimulates insulin release (Haber et al. 2003), long-term exposure to high levels of FFAs results in impairment of the β-cell secretory capacity (Salehi et al. 2001, 2003; Bollheimer et al. 1998) often associated with type 2 diabetes. The secretory response is strongly dependent on the metabolic status of the β cell. Thus, in fasting rodents or humans, FFAs are essential to permit basal insulin secretion and to allow a secretory response to glucose on termination of the fasting period (Dobbins et al. 1998a). However, the mechanism by which FFAs potentiate insulin secretion is not fully understood. It has been generally proposed that in order to exert a stimulatory effect on insulin release, FFAs need to enter the cell and conjugate with coenzyme A, forming long-chain acyl-CoA (LC-CoA) (Corkey et al. 2000). According to the same proposed mechanism, LC-CoA then serves as a major effector molecule in the β cell, influencing a multitude of signaling pathways, including protein kinase C and the exocytotic machinery (Corkey et al. 2000).
Recently, we identified the orphan G-protein-coupled receptor (GPCR), previously known as GPR40, as a receptor of FFAs, and we tentatively named it FFA1R (Kotarsky et al. 2003b). The receptor couples to G-proteins of both the Gαq and to the pertussis-toxin-sensitive Gαi type, affecting several signaling pathways. GPR40 was “de-orphanized” simultaneously by another two groups (Briscoe et al. 2003; Itoh et al. 2003). The receptor is activated by medium- to long-chain FFAs and, quite notably, we also found that it responded to antidiabetic drugs of the thiazolidinedione type (Kotarsky et al. 2003b). All of the original three reports (Kotarsky et al. 2003b; Briscoe et al. 2003; Itoh et al. 2003) agree that a carbon chain of at least 10 atoms and a free carbonyl group seem to be major structural requirements for receptor activation. However, the conclusions concerning the degree of saturation differed. While our results (Kotarsky et al. 2003b) indicated a slight preference for saturated FAs, the reports of Briscoe et al. (2003) and Itoh et al. (2003) showed no differences between saturated and unsaturated FAs. The FFA1R/GPR40 transcript was found preferentially in β cells and in mouse insulinoma MIN6 cells, and also in monocytes (Kotarsky et al. 2003b; Briscoe et al. 2003; Itoh et al. 2003). We also observed that activation of the receptor resulted in an increase in cytosolic [Ca2+]. Since an increase in cytosolic calcium concentration is a prerequisite for insulin release, this observation strongly indicated that FFA1R/GPR40 activation is an important, if not necessary, component in this process. Our results were confirmed by Itoh et al. (2003), showing FFA1R/GPR40, indeed, to be necessary for FFA potentiation of insulin release in MIN6 cells.
The halogenated fatty acid 2-bromo palmitate (2BrP) originally described as an inhibitor of carnitine palmitoyl transferase 1 (CPT-1), has been shown to either potentiate glucose-stimulated insulin release (GSIS) (Prentki et al. 1992; Chen et al. 1994) or inhibit GSIS (Warnotte et al. 1994; Parker et al. 2003). The scope of the present study was to provide evidence that FA activation and 2BrP inhibition both modulate insulin release by interaction with FFA1R/GPR40, not only in MIN6 cells, but also in intact mouse pancreatic islets. The results obtained confirm earlier indications and show that FFA1R/GPR40 activation in intact mouse islets is, indeed, necessary for the FA-mediated potentiation of GSIS (Itoh et al. 2003).
Materials and methods
Animals
Female mice of the NMRI strain (B&K, Sollentuna, Sweden), weighing 28–32 g, were used throughout the experiments. They were given a standard pellet diet (B&K) and tap water ad libitum. All animals used for preparation of pancreatic islets were killed by cervical dislocation. The experimental procedures were approved by the local Ethical Committee for Animal Research.
Drugs and chemicals
Collagenase and HRP-conjugated goat anti-rabbit IgG were from Sigma and Pierce Biotechnology (Rockford, IL. USA), respectively. Cy2-conjugated anti-rabbit IgG and Cy5-conjugated anti-guinea pig IgG were from Jackson Immunoresearch Laboratories (West Grove, PA, USA). Guinea-pig-raised anti-insulin antibody was from Eurodiagnostica (Malmö, Sweden). FA-free bovine serum albumin (BSA) was from Boehringer Mannheim. Triacsin C was from BIOMOL (Plymouth Meeting, PA, USA). FA-free BSA was from Roche. All other chemicals were from Merck or Sigma. Stock solutions of linoleic acid (LA) and 2BrP were made in 95% ethanol. Test substances were prepared in solution containing 1.0% (w/v) FA-free BSA, as previously described by Spector et al. (1971). Before the experiments, the stock solution was dissolved in the appropriate culture or incubation medium to achieve the desired concentrations of test substances.
Cell culture and transfection
A subclone of the MIN6 cell line, MIN6c4, was grown in Dulbecco's modified Eagle's medium (DMEM) with Glutamax-1 (Invitrogen, Paisley, UK) supplemented with 15% heat-inactivated FBS (Invitrogen), 60 μM β-mercaptothanol, 50 U/ml penicillin, and 50 μg/ml streptomycin. HeLa (Kotarsky et al. 2003a) and HEK293 cells were grown in DMEM with Glutamax-1 supplemented with 3% FBS, 50 U/ml penicillin and 50 μg/ml streptomycin. All cells were maintained in a 37°C incubator with 7% CO2. The mouse GPR40 ORF (Genbank accession number AB095745) was amplified with PCR (forward primer, 5′ GCCAAGCTTACCATGGACCTGCCCCCACAGCTCTCCTTCG 3′; reverse primer, 5′ GGCGAATTCCTACTTCTGAATTGTTCCTCTTTGAGTC 3′), subcloned into the pEAK12 expression vector (Edge BioSystems, Gaithersburg, MD), and then transfected into HEK293 cells using Lipofectamine 2000 (Invitrogen), according to the manufacturer's instructions. Total time of transfection was 6 h, and the cells were assayed 48–72 h later.
Phosphatidyl inositol hydrolysis
Receptor activation was assayed by measuring phosphatidyl inositol (PI) hydrolysis essentially as described by Kang and Leeb-Lundberg (2002). Briefly, MIN6c4 cells were preloaded with myo-[3H]inositol (Perkin Elmer, Boston, MA, USA) for 16–20 h and stimulated with LA, 2BrP, and/or tolbutamide for 30 min. The cells were lysed with formic acid on ice and the inositol phosphates were isolated using anion exchange chromatography. For ease of comparison, the results from repeated PI hydrolysis measurements were normalized against the mean basal hydrolysis activity of untreated cells (set to 1) and expressed as “relative PI hydrolysis.” The coefficient of variation (interassay differences) was 11% for the transfected HEK293 cells and 7% for MIN6c4 cells.
Insulin secretion from isolated islets
Preparation of pancreatic islets from mice was performed by retrograde injection of a collagenase solution via the bile-pancreatic duct. Islets were then isolated and hand picked under a stereomicroscope at room temperature (Gotoh et al. 1985). Thereafter, the islets were preincubated for 30 min at 37°C in Krebs-Ringer bicarbonate buffer, pH 7.4, supplemented with 10 mM HEPES, 1% FA-free BSA, and 1 mM glucose. After preincubation, the buffer was changed and the islets were incubated at 8.3 mM glucose with 1% FA-free BSA in the absence or presence of different test agents for 60 min at 37°C. In experiments including triacsin C, it was present at either 1 μM or 10 μM during both preincubation and incubation. Each incubation vial contained 8–12 islets in 1 ml of buffer solution and was gassed with 95% O2–5% CO2 to obtain a constant pH and oxygenation. All incubations were performed in a shaking incubator at 30 cycles/min. An aliquot of the medium was removed immediately after incubation and frozen for later assay of insulin. The radioimmunoassay kit used for insulin determination was obtained from Diagnostika (Falkenberg, Sweden). In experiments involving antisense intervention, islets were cultured for 48 h in RPMI 1640 (SVA, Uppsala, Sweden) supplemented with 10% calf serum, 100 U/ml penicillin, and 10 μg/ml streptomycin in the presence or absence of a mFFA1R/mGPR40-specific morpholino antisense oligonucleotide, M40 (Fig. 1) (Heasman 2002) (Gene Tools, Philomath, OR) at a concentration of 1.4 μM. A nonspecific random-sequence morpholino was used as control. Prior to addition to the incubation medium, the morpholinos were complexed with the manufacturer's special delivery system according to the instructions. To generate single β cells, the freshly isolated islets were shaken at low extracellular Ca2+, as previously described (Olofsson et al. 2004). The dispersed β cells were then plated on a plastic Petri dish (Nunc, Denmark) and maintained in culture for the same time period as for the islets (48 h).
Confocal microscopy
All incubations of freshly isolated islets were performed as above. The islets were then fixed in 4% formaldehyde and permeabilized with 5% Triton X-100. Mouse FFA1R/GPR40 was detected with a rabbit polyclonal antibody (1:100), raised against the C-terminal peptide NH2-CVTRTQRGTIQK-COOH in combination with Cy2-conjugated anti-rabbit IgG (1:150). Nonspecific binding was blocked with 5% normal donkey serum (Jackson Immunoresearch Laboratories). For staining of insulin, islets were incubated with the anti-insulin antibody (1:1,000) followed by an incubation with a Cy5-conjugated anti-guinea-pig IgG antibody (1:150). The fluorescence was visualized in a Pascal LSM510 confocal microscope by sequential scanning at the excitation/emission wavelengths 488/505–530 nm (Cy2) or 633/>650 nm (Cy5).
Statistics
The data are calculated as means ± SEM. The level of significance between groups was assessed using unpaired Student's t=test or analysis of variance followed by Tukey-Kramer's test whenever appropriate. In the figures, ***=p<0.001 and **=p<0.01.
Results
2-bromo palmitate (2BrP) inhibits mFFA1R/GPR40 in transfected HEK293 cells
The well described CPT-1 inhibitor, 2BrP (Chen et al. 1994; Chase and Tubbs 1972), has been reported also to inhibit FA-mediated potentiation of insulin release (Parker et al. 2003; Warnotte et al. 1994). In order to test if 2BrP also has effects on the FFA1R/GPR40, the mouse receptor was transiently expressed in HEK293 cells and challenged with LA, 2BrP, or with a mixture of both. LA (100 μM) activated the receptor as measured by the generation of IP3. However, while 100 μM 2BrP blocked the action of LA, 100 μM 2BrP alone also resulted in an activation, indicating partial agonism (Fig. 2a). Cells transfected with the pEAK12 expression vector without the FFA1R/GPR40 insert did not respond to LA stimulation (data not shown).
Phosphatidyl inositol (PI) hydrolysis in response to linoleic acid (LA) and 2-bromo palmitate (2BrP). a In transiently transfected HEK293 cells, LA increased the basal level of PI hydrolysis ten-fold. This increase was counteracted by 2BrP, which by itself caused a two-fold increase, indicating a partial agonism. b In MIN6c4 cells, stimulation with LA caused an almost six-fold increase in PI hydrolysis compared with basal levels. This effect was abolished by simultaneous addition of 2BrP. 2BrP alone lowered basal IP levels in MIN6c4 cells. Tolbutamide (tolb) had no effect, either on LA-induced or basal levels of IP production. All substances in these experiments were used at 100 μM. Data are means + SEM from representative experiments repeated on two occasions (n=3). ***=p<0.001, n.s not significant
2BrP inhibits mFFA1R/GPR40 in MIN6c4 cells
MIN6c4 is a subclone of the mouse insulinoma cell line MIN6 (Miyazaki et al. 1990), which expresses FFA1R/GPR40 endogenously (Kotarsky et al. 2003b; Briscoe et al. 2003; Itoh et al. 2003). This cell line has been selected because it retains the beta cell phenotype over repeated passages more consistently than the original MIN6 cells (JM unpublished data).
MIN6c4 cells were challenged with LA, 2BrP, and tolbutamide and assayed for receptor-mediated IP3 generation. The results were similar to those obtained in the HEK293 cells expressing the recombinant mouse receptor (Fig. 2b). LA (100 μM) generated an IP3 signal more than five times the basal level while 2BrP and tolbutamide alone were both essentially without stimulatory effect (Fig. 2b). Unlike tolbutamide, 100 μM 2BrP blocked the action of LA on IP3 generation.
2BrP inhibits LA-stimulated insulin release in mouse islets
The 2BrP experiment conducted on MIN6c4 cells was repeated in mouse islets followed by measurement of insulin release. The results, which were virtually identical to those obtained for PI hydrolysis in MIN6c4 cells, demonstrated that while 100 μM 2BrP alone had no significant effect on insulin release, it completely inhibited the release affected by LA (100 μM) (Table 1). Tolbutamide-stimulated insulin release was unaffected by the addition of 2BrP. In order to rule out the effects of FA metabolism, a follow-up experiment using the LC-CoA synthetase inhibitor triacsin C was performed. The LA-stimulated insulin secretion (1.91±0.15 ng/islet per hour) was not affected by the presence of triacsin C (1 μM, 1.95±0.16 ng/islet/h; 10 μM 1.93±0.19 ng/islet per hour; n=8 in all groups, p>0.89 for both concentrations of triacsin C versus LA).
Suppression of FFA1R/GPR40 in mouse islets decreases LA-stimulated insulin release
LA-induced potentiation of insulin secretion was studied in mouse islets. In order to discriminate between insulin release mediated by FFA1R/GPR40 and release caused by other mechanisms, we designed an antisense morpholino oligonucleotide (Heasman 2002) targeting the sequence between position −9 and −33 of the mFFA1R/GPR40 transcript (Fig. 1). Islets were cultured for 48 h with or without 1.4 μM of the M40 antisense oligonucleotide. Furthermore, one group of islets was challenged for 30 min with LA (100 μM) prior to the addition of the M40 oligonucleotide. After the culture period, the islets were washed and incubated for 60 min in 8.3 mM glucose with or without LA or 100 μM tolbutamide before samples were taken for measurement of the concentration of released insulin. A significant 62% attenuation of the LA-induced stimulatory effect on insulin secretion was observed for the group pretreated with the antisense oligonucleotide alone. The combined pretreatment with LA and then M40 caused a further reduction of the LA effect on insulin secretion down to control levels. In contrast, neither GSIS nor tolbutamide-boosted GSIS was affected by the antisense oligonucleotide, even after LA pretreatment (Fig. 3). To validate that the islets were still responsive after 48 h of culturing, insulin release was measured at 1 mM glucose (0.19±0.02 ng/islet per hour, n=6) and compared with the response at 8.3 mM glucose (0.72±0.04 ng/islet per hour, n=8, p<0.001).
Islets subjected to antisense treatment with the mFFA1R/GPR40-specific morpholino M40 exhibit a blunted response to linoleic acid (LA). Figure showing insulin release from islets in response to different stimulation; glucose (8.3 mM), glucose + LA (100 μM), and glucose + tolbutamide (100 μM). Prior to this stimulation, the islets received either a saline pretreatment (white bars), a 48-h pretreatment with the M40 antisense oligonucleotide (hashed bars), or a combination of a 30 min pretreatment with 100 μM LA followed by a 48-h incubation with the morpholino M40 (black bars). Insulin release in response to glucose stimulation alone remained unaffected by the changes in pretreatment whereas the M40 pretreatment significantly reduced the LA-mediated augmentation of GSIS. The combined LA+M40 pretreatment reduced the augmentation even further. The effect of tolbutamide is unaltered by the presence of the M40 oligonucleotide. Means + SEM for eight batches of islets per datapoint. Each batch contained eight to 12 islets incubated for 60 min in the presence of 8.3 mM glucose ± LA or tolbutamide. ***=p<0.001 and **=p<0.01
In the following experiment, the effect of increasing concentrations of LA on insulin secretion was studied in islets treated with the mFFA1R/GPR40 antisense nucleotide. Both untreated islets or islets treated with an unspecific morpholino-oligonucleotide were used as controls. Increasing the LA concentration from 1 μM to 1,000 μM caused a dose-dependent increase in insulin secretion in the untreated control group. The stimulatory effect of LA on insulin secretion from islets treated with the mFFA1R/GPR40 antisense probe was markedly reduced. No signficant difference was observed between the two control groups (with or without unspecific oligonucleotide treatment) (Fig. 4). This rules out nonspecific side effects caused by the morpholino oligonucleotide chemistry.
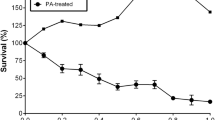
Treatment of islets with the M40 morpholino caused a marked reduction in linoleic acid (LA)-stimulated insulin secretion (white circles). The control morpholino failed to interfere with insulin secretion (black circles) compared with untreated islets (white boxes). Islets (12 in each vial) were incubated for 60 min in the presence of 8.3 mM glucose alone or 8.3 mM glucose and an increasing concentration of LA, as indicated in the figure. Values are means + SEM for six to eight different experiments performed at different occasions
Expression of mFFA1R/GPR40 in pancreatic islets
In order to investigate the distribution of mFFA1R/GPR40 within the pancreatic islet, a polyclonal antibody was raised against the C-terminal portion of mFFA1R/GPR40. The affinity-purified antibody was first tested by FITC labeling and confocal laser microscopy on HeLa cells stably expressing mFFA1R/GPR40. As illustrated in Fig. 5, cells expressing the receptor were stained primarily at the plasma membrane while nontransfected reporter cells only displayed background staining.
Confocal immunofluorescence microscopy with insulin antibodies (labeled with Texas red) and mFFA1R/GPR40 antibodies (labeled with FITC) showed that the two antigens were coexpressed in β cells whether viewed in intact islets (Fig. 6a–c) or in dispersed cell groups (Fig. 6d–f). Analysis of single cells (Fig. 6g) confirmed that mFFA1R/GPR40 expression was primarily localized to the plasma membrane (cf. Fig. 5).
Confocal microscopy images of an intact islet (a–c) or dispersed islet cells (d–f) demonstrating the expression of mFFA1R/GPR40 (a and d), insulin (b and e), and coexpression of both (c and f). An increased magnification shows that mFFA1R/GPR40 is expressed on the β-cell surface (g). Arrowheads (d) illustrate sites of FFA1R/GPR40 expression in the membrane of one β cell. Scale bars are 10 μM
In order to verify that the observed reduction in LA-mediated insulin release was actually the consequence of a suppressed mFFA1R/GPR40 translation, islets were subjected to LA challenge followed by antisense intervention. The islets were then visualized by confocal immunofluorescence using FFA1R/GPR40 and insulin antibodies. The results showed that a reduction in LA-mediated insulin release was, indeed, correlated with a lower cellular expression of mFFA1R/GPR40 (Fig. 7a and b). The insulin staining was not affected by the antisense oligonucleotide treatment (c and d).
Confocal microscopy images of mouse islets. The top panels show islets stained for mFFA1R/GPR40 expression, both untreated (a) and treated for 30 min with 100 μM LA and then for 48 h with the morpholino, M40 (b). The bottom panels show the same islets, either untreated (c) or subjected to identical LA/M40 treatment (d) stained for insulin. Scale bars are 10 μM
Discussion
The mechanism generally proposed for FA-induced potentiation of insulin secretion involves metabolic coupling (Prentki et al. 1992; Corkey et al. 2000), where anaplerotic input into the tricarboxylic acid cycle generates an excess of the regulatory signaling molecule malonyl-CoA. An increase in malonyl-CoA levels inhibits CPT-1, causing the concentration of the FA metabolite LC-CoA to increase. LC-CoA has been reported to affect cellular processes involved in insulin release, either directly on exocytosis (Deeney et al. 2000) or indirectly by activation of protein kinase C (Yaney et al. 2000).
Although plenty of evidence favors the “malonyl-CoA hypothesis,” arguments have also been presented against it. For example, it has been shown that neither inhibition of LC-CoA synthetase in rat islets nor a reduction of malonyl-CoA in INS-1 cells has any effect on insulin secretion (Antinozzi et al. 1998). Intracellular application of palmitoyl-CoA has been reported unable to mimic the action of palmitate on Ca2+ currents and on exocytosis (Olofsson et al. 2004). Also, it has been demonstrated that FAs are capable of increasing the secretory response to nonglucose activators, such as amino acids (Dobbins et al. 1998b). When the previously unknown receptor GPR40 was identified as a receptor for FFAs—with a high expression in β cells and functional involvement in insulin release—it became evident that the mechanism of FA-mediated insulin release is more complex.
One of the arguments for the idea that accumulation of LC-CoA is directly involved in the potentiation mechanism of GSIS has been the finding that 2BrP stimulates insulin secretion in HIT-T15 cells (Prentki et al. 1992) and in perfused rat pancreas (Chen et al. 1994), thus supporting the “malonyl-CoA hypothesis” by linking CPT-1 inhibition to insulin release. Originally described as an inhibitor of CPT-1 and therefore of mitochondrial long-chain FA oxidation (Chase and Tubbs 1972), 2BrP has since proven to have multiple effects on the β-cell metabolism, including inhibition of FA esterification (Parker et al. 2003). However, some authors have reported that 2BrP is unable to potentiate GSIS and also that 2BrP rather attenuates FA-mediated stimulation of insulin secretion in mouse islets (Warnotte et al. 1994) and in HIT-T15 cells (Parker et al. 2003). In view of the contradictory reports regarding the effect of 2BrP on insulin secretion, it must be concluded that the mechanism of action of this substance is far from understood and, consequently, cannot be used as an argument for the malonyl-CoA hypothesis.
Recently, it was reported that a palmitate-induced rise in cytosolic-free [Ca2+] in mouse primary β cells and of HIT-T15 cells was reversibly inhibited by either 100 μM 2BrP or 100 μM methyl palmoxirate (Remizov et al. 2003). An increase in cytosolic [Ca2+] is an accepted secretion signal required for palmitate-induced insulin release (Warnotte et al. 1994; Deeney et al. 2000); it is also the common signal generated by Gαq-coupled receptors such as FFA1R/GPR40. Our results agree well with the reports describing 2BrP as an inhibitor of FA-mediated insulin release, and they also point out FFA1R/GPR40 as a likely target. In the first part of the present study, we showed that 2BrP acts as an antagonist of mFFA1R/GPR40 by blocking the LA-mediated PI hydrolysis in experiments where receptors were expressed either transiently in HEK293 cells or endogenously in MIN6c4 cells. The discrepancy between 2BrP effects on PI hydrolysis between the cell lines can be explained by the difference in receptor densities obtained in a recombinant compared with an endogenous system. The agonist properties of partial agonists, such as 2BrP, will appear more pronounced in a recombinant system with higher receptor density (Kenakin 1997). We were also able to confirm earlier reports (Parker et al. 2003; Warnotte et al. 1994) showing that while 2BrP inhibits LA-stimulated insulin release in mouse islets, the LC-CoA synthetase inhibitor triacsin C was without effect. The fact that 2BrP not only appears as an inhibitor of FA-mediated insulin release but has now also been identified as an antagonist/partial agonist of FFA1R/GPR40 provides a pharmacological support for our view that FFA1R/GPR40 is an essential link in the mechanism underlying the FA-mediated potentiation of insulin secretion. However, although 2BrP acts as an antagonist on FFA1R/GPR40, it is also a toxic substance reported to have a multitude of effects on the cell, including effects on FA metabolism and signaling. The pharmacological characterization alone is therefore not sufficient to link FFA1R/GPR40 to FA-mediated potentiation of insulin secretion.
It has been argued that palmitate stimulation of GSIS proceeds by increasing [Ca2+] via an IP3-independent mechanism involving enhanced Ca2+ influx through L-type channels (Olofsson et al. 2004). This view is not in contradiction with the concept of FFA1R/GPR40 being essential for the mechanism of FA potentiation of insulin secretion since the signaling pathway does not necessarily include a calcium mobilization step. It has been shown by Scholze et al. that Gαi/Gαo-coupled receptors are capable of stimulating pancreatic voltage-gated CaV1.3 channels via a mechanism probably involving diacylglycerol acting on phorbol-acivated protein kinases (Scholze et al. 2001). Another possible pathway is through Gαq-mediated inhibition of G-protein-coupled inwardly rectifying K+ channels (Lei et al. 2003), which are known to be expressed in pancreatic tissue (Smith et al. 2001; Vaughn et al. 2000).
In the second part of the present report, pancreatic islets subjected to mFFA1R/GPR40 antisense intervention displayed an attenuated LA-induced potentiation of GSIS, thus confirming earlier results on MIN6 insulinoma cells (Itoh et al. 2003). However, suppression of the receptor mRNA translation alone did not completely abolish the insulin secretory response of islets to LA. It is possible that this remaining secretory response is due to non-receptor-mediated mechanisms. Another likely explanation is that, due to the slow turnover of membrane receptors, there are still enough receptors on the plasma membrane to trigger an insulin release (cf. Fig. 3). It is a well-studied fact that stimulation of a GPCR generally triggers an internalization procedure removing the receptor from the plasma membrane (Lefkowitz 2004; Gaborik and Hunyady 2004). We therefore assumed that a brief prestimulation with LA would enhance the effect of the antisense intervention. Accordingly, the remaining part of the LA-induced stimulatory effect completely disappeared when the islets were challenged for 30 min with LA prior to the 48-h antisense exposure period. The fact that a tolbutamide-induced insulin release (Proks et al. 2002) was unaffected by both antisense oligonucleotide and LA indicates that the suppressive effect was specific.
In the final part of our study, the distribution of mFFA1R/GPR40 within the islet was established using confocal immunofluorescence microscopy. It was found that the receptor distribution to a great extent overlapped with the distribution of insulin immunoreactivity. This agrees with the observations of both Briscoe et al. (2003) and Itoh et al. (2003). An important observation in our antisense interventions was that a decrease in islet mFFA1R/GPR40 immunostaining strongly correlated with the reduction in LA-stimulated insulin secretion.
An argument that has been raised against a functional relevance of FFA1R/GPR40 (Poitout 2003) has been that receptor activation in the presence of albumin has not yet been demonstrated. It should be noted that all our experiments on mouse islets included 1% FA-free BSA in the culture as well as incubation media. In addition, a recent study of FFA1R/GPR40 in human breast cancer cells demonstrated that receptor-mediated calcium activation occurs in the presence of 0.5% albumin (Yonezawa et al. 2004).
Long-term elevation of FA levels has a deleterious effect on β-cell function, often referred to as lipotoxicity (Robertson et al. 2004). An important question is whether FFA1R/GPR40 is involved also in the long-term lipotoxic effect of FAs. In the lipotoxicity research, there is an increasing interest in the control of the β cell lipid metabolism by lipid-sensing transcription factors such as PPARα, PPARδ, PPARγ, and SREBP-1c (Fatehi-Hassanabad and Chan 2005). An important future task will be to show how the membrane-bound lipid receptor FFA1R/GPR40 interrelate with the nuclear PPAR and SREBP-1c receptors.
Taken together, our results show that activation of FFA1R/GPR40 constitutes an important, if not essential, part of FA-mediated stimulation of insulin secretion. The emerging picture of the mechanism indicates a complex process involving both metabolic coupling and receptor-mediated events where we believe that the latter is of the utmost importance. It is obvious that more research is needed to determine exactly how these components relate to each other.
References
Antinozzi PA, Segall L, Prentki M, McGarry JD, Newgard CB (1998) Molecular or pharmacologic perturbation of the link between glucose and lipid metabolism is without effect on glucose-stimulated insulin secretion. A re-evaluation of the long-chain acyl-CoA hypothesis. J Biol Chem 273:16146–16154
Bollheimer LC, Skelly RH, Chester MW, McGarry JD, Rhodes CJ (1998) Chronic exposure to free fatty acid reduces pancreatic beta cell insulin content by increasing basal insulin secretion that is not compensated for by a corresponding increase in proinsulin biosynthesis translation. J Clin Invest 101:1094–1101
Briscoe CP, Tadayyon M, Andrews JL, Benson WG, Chambers JK, Eilert MM, Ellis C, Elshourbagy NA, Goetz AS, Minnick DT, Murdock PR, Sauls HR Jr, Shabon U, Spinage LD, Strum JC, Szekeres PG, Tan KB, Way JM, Ignar DM, Wilson S, Muir AI (2003) The orphan G protein-coupled receptor GPR40 is activated by medium and long chain fatty acids. J Biol Chem 278:11303–11311
Chase JF, Tubbs PK (1972) Specific inhibition of mitochondrial fatty acid oxidation by 2-bromopalmitate and its coenzyme A and carnitine esters. Biochem J 129:55–65
Chen S, Ogawa A, Ohneda M, Unger RH, Foster DW, McGarry JD (1994) More direct evidence for a malonyl-CoA-carnitine palmitoyltransferase I interaction as a key event in pancreatic beta-cell signaling. Diabetes 43:878–883
Corkey BE, Deeney JT, Yaney GC, Tornheim K, Prentki M (2000) The role of long-chain fatty acyl-CoA esters in beta-cell signal transduction. J Nutr 130:299S–304S
Deeney JT, Gromada J, Hoy M, Olsen HL, Rhodes CJ, Prentki M, Berggren PO, Corkey BE (2000) Acute stimulation with long chain acyl-CoA enhances exocytosis in insulin-secreting cells (HIT T-15 and NMRI beta-cells) J Biol Chem 275:9363–9368
Dobbins RL, Chester MW, Daniels MB, McGarry JD, Stein DT (1998a) Circulating fatty acids are essential for efficient glucose-stimulated insulin secretion after prolonged fasting in humans. Diabetes 47:1613–1618
Dobbins RL, Chester MW, Stevenson BE, Daniels MB, Stein DT, McGarry JD (1998b) A fatty acid- dependent step is critically important for both glucose- and non-glucose-stimulated insulin secretion. J Clin Invest 101:2370–2376
Fatehi-Hassanabad Z, Chan CB (2005) Transcriptional regulation of lipid metabolism by fatty acids: a key determinant of pancreatic beta-cell function. Nutr Metab (Lond) 2:1
Gaborik Z, Hunyady L (2004) Intracellular trafficking of hormone receptors. Trends Endocrinol Metab 15:286–293
Gotoh M, Maki T, Kiyoizumi T, Satomi S, Monaco AP (1985) An improved method for isolation of mouse pancreatic islets. Transplantation 40:437–438
Haber EP, Ximenes HM, Procopio J, Carvalho CR, Curi R, Carpinelli AR (2003) Pleiotropic effects of fatty acids on pancreatic beta-cells. J Cell Physiol 194:1–12
Heasman J (2002) Morpholino oligos: making sense of antisense? Dev Biol 243:209–214
Itoh Y, Kawamata Y, Harada M, Kobayashi M, Fujii R, Fukusumi S, Ogi K, Hosoya M, Tanaka Y, Uejima H, Tanaka H, Maruyama M, Satoh R, Okubo S, Kizawa H, Komatsu H, Matsumura F, Noguchi Y, Shinohara T, Hinuma S, Fujisawa Y, Fujino M (2003) Free fatty acids regulate insulin secretion from pancreatic beta cells through GPR40. Nature 422:173–176
Kang DS, Leeb-Lundberg LM (2002) Negative and positive regulatory epitopes in the C-terminal domains of the human B1 and B2 bradykinin receptor subtypes determine receptor coupling efficacy to G(q/11)-mediated [correction of G(9/11)-mediated] phospholipase Cbeta activity. Mol Pharmacol 62:281–288
Kenakin T (1997) Differences between natural and recombinant G protein-coupled receptor systems with varying receptor/G protein stoichiometry. Trends Pharmacol Sci 18:456–464
Kotarsky K, Antonsson L, Owman C, Olde B (2003a) Optimized reporter gene assays based on a synthetic multifunctional promoter and a secreted luciferase. Anal Biochem 316:208–215
Kotarsky K, Nilsson NE, Flodgren E, Owman C, Olde B (2003b) A human cell surface receptor activated by free fatty acids and thiazolidinedione drugs. Biochem Biophys Res Commun 301:406–410
Lefkowitz RJ (2004) Historical review: a brief history and personal retrospective of seven-transmembrane receptors. Trends Pharmacol Sci 25:413–422
Lei Q, Jones MB, Talley EM, Garrison JC, Bayliss DA (2003) Molecular mechanisms mediating inhibition of G protein-coupled inwardly-rectifying K+ channels. Mol Cells 15:1–9
Miyazaki J, Araki K, Yamato E, Ikegami H, Asano T, Shibasaki Y, Oka Y, Yamamura K (1990) Establishment of a pancreatic beta cell line that retains glucose-inducible insulin secretion: special reference to expression of glucose transporter isoforms. Endocrinology 127:126–132
Olofsson CS, Salehi A, Holm C, Rorsman P (2004) Palmitate increases L-type Ca2+ currents and the size of the readily releasable granule pool in mouse pancreatic beta-cells. J Physiol 557:935–948
Parker SM, Moore PC, Johnson LM, Poitout V (2003) Palmitate potentiation of glucose-induced insulin release: a study using 2-bromopalmitate. Metabolism 52:1367–1371
Poitout V (2003) The ins and outs of fatty acids on the pancreatic beta cell. Trends Endocrinol Metab 14:201–203
Prentki M, Vischer S, Glennon MC, Regazzi R, Deeney JT, Corkey BE (1992) Malonyl-CoA and long chain acyl-CoA esters as metabolic coupling factors in nutrient-induced insulin secretion. J Biol Chem 267:5802–5810
Proks P, Reimann F, Green N, Gribble F, Ashcroft F (2002) Sulfonylurea stimulation of insulin secretion. Diabetes Suppl 3
Remizov O, Jakubov R, Dufer M, Krippeit Drews P, Drews G, Waring M, Brabant G, Wienbergen A, Rustenbeck I, Schofl C (2003) Palmitate-induced Ca2+-signaling in pancreatic beta-cells. Mol Cell Endocrinol 212:1–9
Robertson RP, Harmon J, Tran PO, Poitout V (2004) Beta-cell glucose toxicity, lipotoxicity, and chronic oxidative stress in type 2 diabetes. Diabetes 53(Suppl 1):S119–S124
Salehi A, Ekelund M, Henningsson R, Lundquist I (2001) Total parenteral nutrition modulates hormone release by stimulating expression and activity of inducible nitric oxide synthase in rat pancreatic islets. Endocrine 16:97–104
Salehi A, Ekelund M, Lundquist I (2003) Total parenteral nutrition-stimulated activity of inducible nitric oxide synthase in rat pancreatic islets is suppressed by glucagon-like peptide-1. Horm Metab Res 35:48–54
Scholze A, Plant TD, Dolphin AC, Nurnberg B (2001) Functional expression and characterization of a voltage-gated CaV1.3 (alpha1D) calcium channel subunit from an insulin-secreting cell line. Mol Endocrinol 15:1211–1221
Smith PA, Sellers LA, Humphrey PP (2001) Somatostatin activates two types of inwardly rectifying K+ channels in MIN-6 cells. J Physiol 532:127–142
Spector AA, Fletcher JE, Ashbrook JD (1971) Analysis of long-chain free fatty acid binding to bovine serum albumin by determination of stepwise equilibrium constants. Biochemistry 10:3229–3232
Warnotte C, Gilon P, Nenquin M, Henquin JC (1994) Mechanisms of the stimulation of insulin release by saturated fatty acids. A study of palmitate effects in mouse beta-cells. Diabetes 43:703–711
Vaughn J, Wolford JK, Prochazka M, Permana PA (2000) Genomic structure and expression of human KCNJ9 (Kir3.3/GIRK3) Biochem Biophys Res Commun 274:302–309
Yaney GC, Korchak HM, Corkey BE (2000) Long-chain acyl CoA regulation of protein kinase C and fatty acid potentiation of glucose-stimulated insulin secretion in clonal beta-cells. Endocrinology 141:1989–1998
Yonezawa T, Katoh K, Obara Y (2004) Existence of GPR40 functioning in a human breast cancer cell line, MCF-7. Biochem Biophys Res Commun 314:805–809
Acknowledgements
The technical help of Britt-Marie Nilsson is greatly appreciated. We also thank professor Patrik Rorsman for making available the confocal microscope. This work was supported in part by grants from the Swedish Segerfalk Foundation, GS Development, Crafoord Foundation, Kock Foundation, Royal Physiographic Society, Lund, The Swedish Diabetes Foundation, The Diabetes Programme at the Medical Faculty of Lund University, and the Swedish National Council for Medical Research.
Author information
Authors and Affiliations
Corresponding author
Additional information
A. Salehi and E. Flodgren contributed equally to this work
Rights and permissions
About this article
Cite this article
Salehi, A., Flodgren, E., Nilsson, N.E. et al. Free fatty acid receptor 1 (FFA1R/GPR40) and its involvement in fatty-acid-stimulated insulin secretion. Cell Tissue Res 322, 207–215 (2005). https://doi.org/10.1007/s00441-005-0017-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-005-0017-z