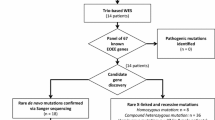
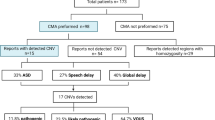
Abstract
While pathogenic copy number variations (CNVs) in 15q11.2 were recently identified in Caucasian patients with idiopathic generalized epilepsies (IGEs), the epilepsy-associated gene(s) in this region is/are still unknown. Our study investigated whether the CNVs in 15q11.2 are associated with childhood absence epilepsy (CAE) in Chinese patients and whether the selective magnesium transporter NIPA2 gene affected by 15q11.2 microdeletions is a susceptive gene for CAE. We assessed IGE-related CNVs by Affymetrix SNP 5.0 microarrays in 198 patients with CAE and 198 controls from northern China, and verified the identified CNVs by high-density oligonucleotide-based CGH microarrays. The coding region and exon–intron boundaries of NIPA2 were sequenced in all 380 patients with CAE and 400 controls. 15q11.2 microdeletions were detected in 3 of 198 (1.5%) patients and in no controls. Furthermore, we identified point mutations or indel in a heterozygous state of the NIPA2 gene in 3 out of 380 patients, whereas they were absent in 700 controls (P = 0.043). These mutations included two novel missense mutations (c.532A>T, p.I178F; c.731A>G, p.N244S) and one small novel insertion (c.1002_1003insGAT, p.N334_335EinsD). No NIPA2 mutation was found in 400 normal controls. We first identified that NIPA2, encoding a selective magnesium transporter, is a susceptible gene of CAE, and 15q11.2 microdeletions are important pathogenic CNVs for CAE with higher frequency in Chinese populations than that previously reported in Caucasians. The haploinsufficiency of NIPA2 may be a mechanism underlying the neurological phenotypes of 15q11.2 microdeletions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As one subtype of idiopathic generalized epilepsies (IGEs), childhood absence epilepsy (CAE) is also genetically determined (Jallon and Latour 2005). Recent studies of copy number variations (CNVs) in the human genome in patients with epilepsy have revealed recurrent microdeletions at 1q21.1, 15q11.2, 15q13.3, 16p11.2, 16p13.11, and 22q11.2. Among them, the common CNVs in 15q11.2 occurred in about 0.75–1.05% patients with IGEs (Helbig et al. 2009; Dibbens et al. 2009; de Kovel et al. 2010; Mefford et al. 2010). To elucidate whether these CNVs are consistently susceptible factors in Chinese patients with CAE, we assessed the reported IGEs-related CNVs using Affymetrix SNP 5.0 microarray in 198 patients and 198 controls, both from northern China. High-density oligonucleotide-based comparative genomic hybridization (CGH) microarrays and real-time quantitative PCR (RT-PCR) were employed to confirm the CNVs identified in 15q11.2 and 15q13. There are four highly conserved genes located in 15q11.2 that are expressed in the brain, including NIPA2, NIPA1, TUBGCP5, and CYFIP1 (Chai et al. 2003). Among them, NIPA2 and NIPA1 both encode magnesium transporter subtypes. Mutations in NIPA1 have been associated with autosomal dominant spastic paraplegia 6 (Zhao et al. 2008; Tsang et al. 2009), while the roles of NIPA2 mutations have not been assessed in any disease. We hypothesized that NIPA2 may be important in the etiology of epilepsy. Therefore, we conducted direct sequencing of entire coding regions and exon–intron boundaries of the NIPA2 gene in all 380 CAE patients (including the 198 cases studied by Affymetrix SNP 5.0 microarray) and 400 normal controls to investigate whether it could be a susceptible gene for CAE and might be the responsible gene for the CAE phenotypes manifested by 15q11.2 microdeletions.
Patients and methods
Choice of candidate CNV regions
The selection of microdeletions in 1q21.1, 15q11.2, 15q13.3, 16p11.2, 16p13.11, and 22q11.2 was based on previous large-scale CNV analysis (Helbig et al. 2009; Dibbens et al. 2009; de Kovel et al. 2010; Mefford et al. 2008, 2010; International Schizophrenia Consortium 2008; Sebat et al. 2007; Weiss et al. 2008; Hannes et al. 2009; Itsara et al. 2009) and a recent meta-analysis in neuropsychiatric disorders, which included autism, intellectual disability, and schizophrenia (Itsara et al. 2009). The following inclusion criteria for the selection of candidate CNVs were applied: (1) recurrent microdeletion with equal size and defined breakpoints generated by non-allelic homologous recombination (Stankiewicz and Lupski 2002); (2) previous association of microdeletion with neuropsychiatric disorders (P < 0.05); (3) size of microdeletion larger than 100 kb to ensure a reliable detection by the Affymetrix SNP 5.0 array (coverage: more than 100 probe sets).
Study participants
All participating patients were recruited from four hospitals in Beijing and were of Han ethnicity using the same criteria and protocol as that of our previous study (Chen et al. 2003). There were 380 patients who fulfilled our criteria for CAE. Informed consent was obtained from their parents. The 700 normal controls, also of Han ethnicity, were of normal gender-matched adults from northern China and without personal or family history of epilepsy. This study was approved by Medical Ethics Committee of Peking University First Hospital.
Genotyping and CNV detection
All genomic DNA was extracted from peripheral leukocytes. Among the participants, 198 patients and 198 controls were assessed by Affymetrix SNP 5.0 array. SNP genotyping was performed by the algorithm implemented in the Affymetrix Genotyping Console (version 3.0.2). CNV analysis was performed with CEL files of arrays using the hidden Markov model algorithm and the segmentation algorithm of Partek Genomics Suite (version 6.5).
Changes of the heterozygosity state and log2 ratios along with candidate microdeletion regions were visually inspected to exclude technical artifacts. The selected microdeletions were covered by more than 100 probe sets each on the Affymetrix SNP 5.0 array.
The high-density oligonucleotide-based CGH microarrays, including the Agilent SurePrint G3 Human High-Resolution Discovery Microarray (1x1M) and a customer-designed Agilent SurePrint G3 Microarray (8x60K) were used to verify CNVs. DNA digestion, Cy5-dUTP or Cy3-dUTP labeling, purification, array hybridization, washing, scanning, and data analysis were conducted by following the Agilent oligonucleotide aCGH protocol (version 6.3).
Microdeletions were considered to match the published deletions if they overlapped at least 70% of the genomic region of the candidate CNV (de Kovel et al. 2010). Microdeletions between breakpoints (BPs) 1 and 2 in 15q11.2 (Chai et al. 2003) were verified by real-time quantitative PCR (RT-PCR). RT-PCR was performed on the ABI StepOne™ Real-Time PCR System, using the SYBR® Green PCR Master Mix. Data were analyzed with StepOne™ Software (version 2.1).
Multiple SNPs located between BP1 and BP2 in 15q11.2 were used to analyze the heterozygosity state of the parents and the parental origin of microdeletions.
Statistical analysis
Association analysis of microdeletions between CAE patients and controls were carried out by one-sided χ2 tests or Fisher’s exact tests where appropriate.
NIPA2 mutation analysis
The sequence of NIPA2 was obtained from the UCSC Genome Bioinformatics database (NM_001184889). The primer sequences and PCR amplification conditions were available on request. All the primer sequences were shown in Table 1.
DNA sequencing was carried out using the ABI PRISM BigDye Terminator cycle Ready Reaction sequencing kit on an Applied Biosystems 3100 genetic analyzer (both from Applied Biosystems, Carlsbad, CA, USA). We conducted direct sequencing of entire coding regions and exon–intron boundaries of the NIPA2 gene in all 380 CAE patients (including the 198 cases for Affymetrix SNP 5.0 microarray study) and 400 normal controls. For the novel mutations found in patients, the corresponding amplicons from other 300 control samples were sequenced. Therefore, a total of 700 control samples were available for comparison in order to estimate a mutation rate from the 380 patient cases.
Results
Identification of microdeletions in patients with CAE and controls
We observed 15q11.2 microdeletions in 3 out of 198 (1.5%) patients with CAE and one large 15q13 microdeletion out of 198 (0.5%) patients with CAE (Table 2; Fig. 1), whereas neither was found in controls. One-sided Fisher test for 15q11.2 resulted in P = 0.12. No CNVs in 1q21.1, 16p11.2, 16p13.11, or 22q11.2 were identified in any participants. Two 15q11.2 microdeletions in Subjects 295 and 823 and one 15q13 microdeletion in Subject 289 were confirmed by high-density CGH microarray with resolution of <1 kb (Fig. 2). All these microdeletions were mediated between repeat sequences in 15q (BP1 and BP2 for the 15q11.2 microdeletions; BP3 and BP5 for the 15q13 microdeletion). Since the remaining DNA of Subject 170 was not sufficient for CGH assay, the 15q11.2 microdeletion identified in 170 was confirmed by RT-PCR assay of a test probe located in the common BP1–BP2 CNV region in 15q11.2. Multiple SNP analysis was also conducted in these three patients with 15q11.2 microdeletions and their parents. Heterozygous status in multiple SNPs in 15q11.2 was identified in Subject 170’s mother (170M), Subject 295’s father (295F), and Subject 823’s father (823F). The possibility of transmitting microdeletions from these subjects to the patients was thus excluded (Table 3). Then, we performed aCGH analysis in the remaining parents and showed that the 15q11.2 microdeletion in Subject 170 was de novo mutation and the 15q11.2 microdeletions in Subjects 295 and 823 were maternally inherited (Fig. 2). The large microdeletions mediated between BPs 3 and 5 in 15q13 were also maternally inherited (Fig. 2). There seemed no significant difference in clinical phenotypes between the CAE patients with and without the microdeletions (Table 2).
Results of Affymetrix SNP 5.0 microarray analysis. Each point represents the average of copy number values of five continuous probe sets. a–c Microdeletions in 15q11.2 in Subjects 170, 295, and 823, respectively. d Microdeletion in 15q13 in Subject 289. The CNV boundary was determined as the median of the marginal probe set of a CNV segment and its flanking copy number neutral probe set. Genomic coordinates of NCBI Build 36
Oligonucleotide aCGH analysis of 15q11.2 and 15q13 microdeletions in patients with CAE and their parents. a Locations of the four genes affected by 15q11.2 microdeletions, and two repeat sequences (BP1 and BP2) are shown. Above, for reference, is a horizontal line showing partial 15q11.2 region and Megabase (Mb) genomic coordinates (NCBI Build 37) below. b Three repeat sequences (BP3, BP4, and BP2) are shown. The 15q13 microdeletion was identified by Agilent 1 × 1 M genome-wide CGH microarray, whereas the CNV status of the parents was studied by customer-designed microarrays covering the common region (BP4–BP5) of 15q13 microdeletions. Above is a horizontal line showing partial 15q13 region and genomic coordinates below. The green (loss), black (neutral), and red (gain) dots show the relative intensities (deviation from the horizontal line of log2 ratio = zero) and genomic locations of the oligonucleotide probes employed in our aCGH assay. The regions that lack unique probes correspond to repeat sequences. The regions with copy number losses are shown in green bars (color figure online)
NIPA2 mutation analysis
NIPA2 mutations were identified in 3 of the 380 CAE patients, consisting of 2 novel missense mutations (c.532A>T, p.I178F; c.731A>G, p.N244S) and 1 small novel insertion (c.1002_1003insGAT, p.N334_335EinsD). All the NIPA2 mutations found in this study are heterozygous, as summarized in Table 4. These three novel mutations were all inherited from the patients’ fathers and not found in 700 normal controls. There was not any mutation in entire coding area and intron–exon boundaries of NIPA2 detected in the 400 normal controls. Amino acid alignment of NIPA2 orthologs from different species showed that these three rare variations affected the highly conserved amino acid (Fig. 3). There seemed to be no difference in the clinical manifestations between the CAE patients with and without these variations of NIPA2 (Table 4).
ClustalW alignment of NIPA2 orthologs from human (NCBI accession number NM_001184889), mouse (NCBI accession number CH466599), chicken (NCBI accession number NM_001030809), Xenopus (NCBI accession number CR760985), and Rattus (NCBI accession number NM_001107518). The transmembrane areas are shown in red. Arrows indicate heterozygous point mutation sites and the insertion mutation site (color figure online)
Discussion
Recurrent CNVs in 15q have been reported to be associated with IGEs including CAE. However, to our knowledge, there has been no pathogenic 15q CNV reported in an Asian CAE patient cohort. In this study, we identified 15q11.2 microdeletions in 3 cases and a 15q13.3 microdeletion in 1 case from our 198 Chinese CAE patients. Altogether, microdeletions were present in 2.02% of 198 CAE patients (4/198) versus none of 198 population controls. Our study thus suggests that CNV is an important risk factor for Chinese CAE patients, especially regarding 15q11.2 microdeletions, even though the P value is not significant enough due to the limited sample size of case and control cohort.
We showed that the frequency of 15q11.2 microdeletions in CAE patients (1.5%) was much higher than that of 15q13.3 microdeletion (0.5%) in our patients’ cohort. Additionally, no microdeletion was found in other loci previously reported to be associated with IGEs in Caucasians. Published data for CAE/JAE demonstrated the CNVs in 15q13.3 (0.87–4.5%), 15q11.2 (0.87%), and 16p13.11 (0.69%) were more common than those in other regions (Dibbens et al. 2009; de Kovel et al. 2010). The difference in the CNV configuration in CAE/JAE between our study in Chinese and previous studies in Caucasians may be due to the more restricted recruiting criteria of our study or racial differences of the patient cohorts. We need to collect more patient data to clarify that in the future. Another interesting finding was the microdeletion we found in 15q13.3, which was a large deletion spanning from BP3 to BP5 (~3.3 Mb). Only five subjects were previously reported to have this large deletion in 15q13.3 (Helbig et al. 2009; Sharp et al. 2008; Ben-Shachar et al. 2009; van Bon et al. 2009). Among them, only one German patient had a phenotype (JAE, with generalized seizure later) similar to that of our patient (CAE, no other seizure type). The remaining four subjects had epilepsy together with mental retardation or only mental retardation/autistic behavior. All these previous cases were Caucasian. Thus, the 15q13.3 microdeletion that we found was the first Asian case with a larger BP3–BP5 microdeletion in 15q13.3.
We also conducted direct sequencing in the coding regions of the NIPA2 gene and identified three mutations that existed only in the 380 patients with CAE but not in the 700 controls. All these rare variations affect conserved residues in NIPA2 proteins across species (Fig. 3). In contrast, there were no mutations within the entire coding regions and exon–intron boundaries of NIPA2 detected in the 400 normal controls. These results suggest that the NIPA2 gene may be an important susceptible gene in CAE. NIPA2 was located at the common area of the three microdeletions in 15q11.2 (Fig. 2) and encodes a selective magnesium transporter (Goytain et al. 2008). Phylogenetic analysis showed that NIPA2 was highly conserved in vertebrate species and expressed in the brain (Chai et al. 2003). The NIPA2 gene includes ten exons, with a coding region from exon 6 to exon 10, which encodes a putative polypeptide with nine transmembrane domains (Fig. 4). Ion channel genes have been proved to be the most important susceptibility genes of idiopathic epilepsy, especially IGEs. For CAE, the CACNA1H gene encoding low-threshold T-type Ca2+ channels is an important susceptible gene first reported by our group and confirmed by other centers later (Chen et al. 2003; Lacinova 2004). Mg2+ and Ca2+ reinforce each other’s actions. The precise adjustment of the both intra- and extracellular levels of Ca2+ and Mg2+ is crucial in the functioning of excitable tissues. The central nervous system (CNS) is very sensitive to the level of magnesium as well as calcium. Excitability and synaptic transmission are both affected by the level of magnesium (Rausche et al. 1990; Czéh and Somjen 1989). Hypermagnesemia can induce CNS neuronal depression with encephalopathy, while hypomagnesaemia causes mainly CNS neuronal irritability with seizures (Cao et al. 2003; Riggs 2002; Castilla-Guerra et al. 2006). Brain slices obtained from both a genetic rat model of absence seizures and a non-epileptic control rat could produce synchronous epileptiform discharges during prolonged application of zero [Mg2+] medium which closely resembled electrographic seizures (D’Arcangelo et al. 2002).
Although the mutations identified in the 3 CAE patients were not found in any of the 700 controls, they were all inherited from their fathers, and none of these fathers reported a history of CAE. In addition, two out of three 15q11.2 microdeletions and one 15q13 microdeletion were also inherited (all maternal transmissions), but such large microdeletions were absent in the controls. The possible explanations may include the following. First, considering the location of NIPA2 is adjacent to the imprinted region of Prader-Willi/Angelman syndrome (Chai et al. 2003), one might suspect that only the paternal NIPA2 allele is normally expressed due to imprinting; therefore, mutated paternal NIPA2 allele may lead to abnormal phenotype. However, like the other three genes located between breakpoint hotspots BP1 and BP2 of the Prader-Willi/Angelman syndrome’s deletion region, NIPA2 is reported to be non-imprinted in human blood and mouse brain samples, although it is only ∼2 Mb from the imprinted domain (Chai et al. 2003). Also, expression analysis of cultured human cells and brain tissues showed that NIPA2 are biallelically expressed (Jiang et al. 2008). These evidences deny the possibility of brain-specific imprinting in the pathogenesis of our cases. Second, it is possible that allelic imbalance (AI) expression of NIPA2 could cause a significant distortion in the ratio of expression level between two NIPA2 alleles. AI could decrease the level of transcripts and thus contribute to an increased susceptibility of developing CAE phenotype in offsprings, while not in their parents. The mutated allele may have a minor effect in the father, while having a major effect in the offspring. This phenomenon has been proved widely and has attracted much attention recently (Pastinen 2010). Third, current evidence suggests that CAE is a multifactorial disease, and many factors might be involved in the expression of the CAE genotype. Therefore, the NIPA2 functional abnormality itself may only increase the risk of CAE and may not be sufficient to cause the CAE phenotype on its own, similar to the findings in CACNA1H (Hughes 2009). Finally, the mechanism of phenotypic differences is still unclear. The previous 15q11.2 deletion study for epilepsy showed the parents (father or mother) and offspring with the same deletion had different phenotypes (de Kovel et al. 2010).
In summary, our findings show the associations between 15q11.2 microdeletions and child absence epilepsy, which is the first time in Asian populations. Furthermore, we present evidence supporting that the mutations in NIPA2 gene were associated with CAE, which also indicated that the haploinsufficiency of NIPA2 might be a candidate mechanism underlying the IGE/CAE phenotypes caused by 15q11.2 microdeletions or rare mutations in NIPA2. Further studies with more cases and functional analysis of the NIPA2 mutations are warranted.
References
Ben-Shachar S, Lanpher B, German JR, Qasaymeh M, Potocki L, Nagamani SC, Franco LM, Malphrus A, Bottenfield GW, Spence JE, Amato S, Rousseau JA, Moghaddam B, Skinner C, Skinner SA, Bernes S, Armstrong N, Shinawi M, Stankiewicz P, Patel A, Cheung SW, Lupski JR, Beaudet AL, Sahoo T (2009) Microdeletion 15q13.3: a locus with incomplete penetrance for autism, mental retardation, and psychiatric disorders. J Med Genet 46:382–388
Cao H, Jiang Y, Liu Z, Wu X (2003) The effect of magnesium-free treatment induced recurrent epileptiform discharges on developing cortical neuron in vitro. Dev Brain Res 142:1–6
Castilla-Guerra L, del Carmen Fernández-Moreno M, López-Chozas JM, Fernández-Bolaños R (2006) Electrolytes disturbances and seizures. Epilepsia 47:1990–1998
Chai JH, Locke DP, Greally JM, Knoll JH, Ohta T, Dunai J, Yavor A, Eichler EE, Nicholls RD (2003) Identification of four highly conserved genes between breakpoint hotspots BP1 and BP2 of the Prader-Willi/Angelman syndromes deletion region that have undergone evolutionary transposition mediated by flanking duplicons. Am J Hum Genet 73:898–925
Chen Y, Lu J, Pan H, Zhang Y, Wu H, Xu K, Liu X, Jiang Y, Bao X, Yao Z, Ding K, Lo WH, Qiang B, Chan P, Shen Y, Wu X (2003) Association between genetic variation of CACNA1H and childhood absence epilepsy. Ann Neurol 54:239–243
Czéh G, Somjen GG (1989) Changes in extracellular calcium and magnesium and synaptic transmission in isolated mouse spinal cord. Brain Res 486:274–285
D’Arcangelo G, D’Antuono M, Biagini G, Warren R, Tancredi V, Avoli M (2002) Thalamocortical oscillations in a genetic model of absence seizures. Eur J Neurosci 16:2383–2393
de Kovel CG, Trucks H, Helbig I, Mefford HC, Baker C, Leu C, Kluck C, Muhle H, von Spiczak S, Ostertag P, Obermeier T, Kleefuss-Lie AA, Hallmann K, Steffens M, Gaus V, Klein KM, Hamer HM, Rosenow F, Brilstra EH, Trenité DK, Swinkels ME, Weber YG, Unterberger I, Zimprich F, Urak L, Feucht M, Fuchs K, Møller RS, Hjalgrim H, De Jonghe P, Suls A, Rückert IM, Wichmann HE, Franke A, Schreiber S, Nürnberg P, Elger CE, Lerche H, Stephani U, Koeleman BP, Lindhout D, Eichler EE, Sander T (2010) Recurrent microdeletions at 15q11.2 and 16p13.11 predispose to idiopathic generalized epilepsies. Brain 133(Pt 1):23–32
Dibbens LM, Mullen S, Helbig I, Mefford HC, Bayly MA, Bellows S, Leu C, Trucks H, Obermeier T, Wittig M, Franke A, Caglayan H, Yapici Z, EPICURE Consortium, Sander T, Eichler EE, Scheffer IE, Mulley JC, Berkovic SF (2009) Familial and sporadic 15q13.3 microdeletions in idiopathic generalized epilepsy: precedent for disorders with complex inheritance. Hum Mol Genet 18:3626–3631
Goytain A, Hines RM, Quamme GA (2008) Functional characterization of NIPA2, a selective Mg2+ transporter. Am J Physiol Cell Physiol 295(4):C944–C953
Hannes FD, Sharp AJ, Mefford HC, de Ravel T, Ruivenkamp CA, Breuning MH, Fryns JP, Devriendt K, Van Buggenhout G, Vogels A, Stewart H, Hennekam RC, Cooper GM, Regan R, Knight SJ, Eichler EE, Vermeesch JR (2009) Recurrent reciprocal deletions and duplications of 16p13.11: the deletion is a risk factor for MR/MCA while the duplication may be a rare benign variant. J Med Genet 46:223–232
Helbig I, Mefford HC, Sharp AJ, Guipponi M, Fichera M, Franke A, Muhle H, de Kovel C, Baker C, von Spiczak S, Kron KL, Steinich I, Kleefuss-Lie AA, Leu C, Gaus V, Schmitz B, Klein KM, Reif PS, Rosenow F, Weber Y, Lerche H, Zimprich F, Urak L, Fuchs K, Feucht M, Genton P, Thomas P, Visscher F, de Haan GJ, Møller RS, Hjalgrim H, Luciano D, Wittig M, Nothnagel M, Elger CE, Nürnberg P, Romano C, Malafosse A, Koeleman BP, Lindhout D, Stephani U, Schreiber S, Eichler EE, Sander T (2009) 15q13.3 microdeletions increase risk of idiopathic generalized epilepsy. Nat Genet 41:160–162
Hughes JR (2009) Absence seizures: a review of recent reports with new concepts. Epilepsy Behav 15:404–412
International Schizophrenia Consortium (2008) Rare chromosomal deletions and duplications increase risk of schizophrenia. Nature 455:237–241
Itsara A, Cooper GM, Baker C, Girirajan S, Li J, Absher D, Krauss RM, Myers RM, Ridker PM, Chasman DI, Mefford H, Ying P, Nickerson DA, Eichler EE (2009) Population analysis of large copy number variants and hotspots of human genetic disease. Am J Hum Genet 84:148–161
Jallon P, Latour P (2005) Epidemiology of idiopathic generalized epilepsies. Epilepsia 46(Suppl 9):10–14
Jiang YH, Wauki K, Liu Q, Bressler J, Pan Y, Kashork CD, Shaffer LG, Beaudet AL (2008) Genomic analysis of the chromosome 15q11-q13 Prader-Willi syndrome region and characterization of transcripts for GOLGA8E and WHCD1L1 from the proximal breakpoint region. BMC Genomics 9:50
Lacinova L (2004) Pharmacology of recombinant low-voltage activated calcium channels. Curr Drug Targets CNS Neurol Disord 3:105–111
Mefford HC, Sharp AJ, Baker C, Itsara A, Jiang Z, Buysse K, Huang S, Maloney VK, Crolla JA, Baralle D, Collins A, Mercer C, Norga K, de Ravel T, Devriendt K, Bongers EM, de Leeuw N, Reardon W, Gimelli S, Bena F, Hennekam RC, Male A, Gaunt L, Clayton-Smith J, Simonic I, Park SM, Mehta SG, Nik-Zainal S, Woods CG, Firth HV, Parkin G, Fichera M, Reitano S, Lo Giudice M, Li KE, Casuga I, Broomer A, Conrad B, Schwerzmann M, Räber L, Gallati S, Striano P, Coppola A, Tolmie JL, Tobias ES, Lilley C, Armengol L, Spysschaert Y, Verloo P, De Coene A, Goossens L, Mortier G, Speleman F, van Binsbergen E, Nelen MR, Hochstenbach R, Poot M, Gallagher L, Gill M, McClellan J, King MC, Regan R, Skinner C, Stevenson RE, Antonarakis SE, Chen C, Estivill X, Menten B, Gimelli G, Gribble S, Schwartz S, Sutcliffe JS, Walsh T, Knight SJ, Sebat J, Romano C, Schwartz CE, Veltman JA, de Vries BB, Vermeesch JR, Barber JC, Willatt L, Tassabehji M, Eichler EE (2008) Recurrent rearrangements of chromosome 1q21.1 and variable pediatric phenotypes. N Engl J Med 359:1685–1699
Mefford HC, Muhle H, Ostertag P, von Spiczak S, Buysse K, Baker C, Franke A, Malafosse A, Genton P, Thomas P, Gurnett CA, Schreiber S, Bassuk AG, Guipponi M, Stephani U, Helbig I, Eichler EE (2010) Genome-wide copy number variation in epilepsy: novel susceptibility loci in idiopathic generalized and focal epilepsies. PLoS Genet 6(5):e1000962
Pastinen T (2010) Genome-wide allele-specific analysis: insights into regulatory variation. Nat Rev Genet 11:533–538
Rausche G, Igelmund P, Heinemann U (1990) Effects of changes in extracellular potassium, magnesium and calcium concentration on synaptic transmission in area CA1 and the dentate gyrus of rat hippocampal slices. Pflugers Arch 415:588–593
Riggs JE (2002) Neurological manifestations of electrolyte disturbances. Neurol Clin 20:227–239
Sebat J, Lakshmi B, Malhotra D, Troge J, Lese-Martin C, Walsh T, Yamrom B, Yoon S, Krasnitz A, Kendall J, Leotta A, Pai D, Zhang R, Lee YH, Hicks J, Spence SJ, Lee AT, Puura K, Lehtimäki T, Ledbetter D, Gregersen PK, Bregman J, Sutcliffe JS, Jobanputra V, Chung W, Warburton D, King MC, Skuse D, Geschwind DH, Gilliam TC, Ye K, Wigler M (2007) Strong association of de novo copy number mutations with autism. Science 316:445–449
Sharp AJ, Mefford HC, Li K, Baker C, Skinner C, Stevenson RE, Schroer RJ, Novara F, De Gregori M, Ciccone R, Broomer A, Casuga I, Wang Y, Xiao C, Barbacioru C, Gimelli G, Bernardina BD, Torniero C, Giorda R, Regan R, Murday V, Mansour S, Fichera M, Castiglia L, Failla P, Ventura M, Jiang Z, Cooper GM, Knight SJ, Romano C, Zuffardi O, Chen C, Schwartz CE, Eichler EE (2008) A recurrent 15q13.3 microdeletion syndrome associated with mental retardation and seizures. Nat Genet 40:322–328
Stankiewicz P, Lupski JR (2002) Genome architecture, rearrangements and genomic disorders. Trends Genet 18(2):74–82
Tsang HT, Edwards TL, Wang X, Connell JW, Davies RJ, Durrington HJ, O’Kane CJ, Luzio JP, Reid E (2009) The hereditary spastic paraplegia proteins NIPA1, spastin and spartin are inhibitors of mammalian BMP signaling. Hum Mol Genet 18:3805–3821
van Bon BW, Mefford HC, Menten B, Koolen DA, Sharp AJ, Nillesen WM, Innis JW, de Ravel TJ, Mercer CL, Fichera M, Stewart H, Connell LE, Ounap K, Lachlan K, Castle B, van der Aa N, van Ravenswaaij C, Nobrega MA, Serra-Juhé C, Simonic I, de Leeuw N, Pfundt R, Bongers EM, Baker C, Finnemore P, Huang S, Maloney VK, Crolla JA, van Kalmthout M, Elia M, Vandeweyer G, Fryns JP, Janssens S, Foulds N, Reitano S, Smith K, Parkel S, Loeys B, Woods CG, Oostra A, Speleman F, Pereira AC, Kurg A, Willatt L, Knight SJ, Vermeesch JR, Romano C, Barber JC, Mortier G, Pérez-Jurado LA, Kooy F, Brunner HG, Eichler EE, Kleefstra T, Kleefstra T, de Vries BB (2009) Further delineation of the 15q13 microdeletion and duplication syndromes: a clinical spectrum varying from non-pathogenic to a severe outcome. J Med Genet 46:511–523
Weiss LA, Shen Y, Korn JM, Arking DE, Miller DT, Fossdal R, Saemundsen E, Stefansson H, Ferreira MA, Green T, Platt OS, Ruderfer DM, Walsh CA, Altshuler D, Chakravarti A, Tanzi RE, Stefansson K, Santangelo SL, Gusella JF, Sklar P, Wu BL, Daly MJ (2008) Association between microdeletion and microduplication at 16p11.2 and autism. N Engl J Med 358:667–675
Zhao J, Matthies DS, Botzolakis EJ, Macdonald RL, Blakely RD, Hedera P (2008) Hereditary spastic paraplegia-associated mutations in the NIPA1 gene and its Caenorhabditis elegans homolog trigger neural degeneration in vitro and in vivo through a gain-of-function mechanism. J Neurosci 28:13938–13951
Acknowledgments
This study was supported by grants from the Ministry of Science and Technology of China (2006AA02A408, 2006CB500701, 2008ZX09312-014, 2011CBA00401). The authors thank Dr. Alexander Merkle and Dr. Yan Dong from Medical school of University of Minnesota, USA and BoldFace Editors, Inc., USA for help with manuscript preparation. We highly appreciate our patients and their families for their participation.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Y. Jiang, Y. Zhang, and P. Zhang contributed equally to the manuscript.
Our experiments comply with the current laws of the country in which they were performed.
Rights and permissions
About this article
Cite this article
Jiang, Y., Zhang, Y., Zhang, P. et al. NIPA2 located in 15q11.2 is mutated in patients with childhood absence epilepsy. Hum Genet 131, 1217–1224 (2012). https://doi.org/10.1007/s00439-012-1149-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00439-012-1149-3