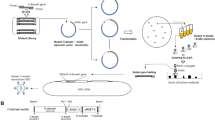
Abstract
Purpose
Newcastle disease virus (NDV) has been applied to oncolytic virotherapy for decades due to its naturally oncolytic property. In spite of the substantiation of the sialic acid receptors of NDV on host cells, knowledge of preference of sialic acid linkage in viral attachment and oncolytic effect is lacking and imperative to be elucidated.
Methods
Surface plasmon resonance analysis and competitive inhibition with sialylated glycan receptor analogues were used to determine the affinity and the preference of sialic acid receptor. Treatments of sialyltransferase inhibitors and linkage-specific sialidases and transfection with sialyltransferase expression vector were performed to regulate sialic acids levels.
Results
We demonstrated that sialic acid was essential for NDV binding and infection of tumor cells. α2,6-linked sialic acid served as a high-affinity receptor for NDV and the ST6Gal I sialyltransferase that synthesizes α2-6 linkage of sialylated N-linked glycans in CHO-K1 cells promoted NDV binding and cytopathic effect. More importantly, an enhanced antitumor effect of NDV on aggressive SW620 colorectal carcinoma cells with high-level of cell surface α2,6-sialylation, but not SW480 cells with relative low-level of α2,6-sialylation, was observed both in vitro and in vivo.
Conclusions
The study provides evidence of optimized therapeutic strategy in oncolytic virotherapy via partly defining α2,6-sialylated receptor as a “cellular marker” for NDV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The metastatic spread and apoptosis resistance are principal players in poor prognosis for cancer patients. Aberrant modification in glycosylation, particularly that in terminal sialylation correlates with tumorigenic transformation and progression, including proliferation, invasion and metastasis (Dube and Bertozzi 2005; Fuster and Esko 2005). Sialic acids (Sia) are nine-carbon backbone α-keto acidic sugars of approximately 50 different neuraminic acid derivatives with the most common variant referred to N-acetylneuraminic acid (Neu5Ac) (Schauer 2009). Sialyltransferases (STs) comprise a family of at least 20 different anabolic enzymes which are divided into three subfamilies according to the type of Sia linkage elaborated. The α2,3-ST, α2,6-ST and α2,8-ST mediate the transfer of Sia to terminals galactose (Gal; ST3Gal I–VI, ST6Gal I–II), N-acetylgalactosamine (GalNAc; ST6GalNAc I–VI) and the other Sia residues (ST8Sia I–VI) (Harduin-Lepers et al. 2001). Changes of selective ST have been described in cancer. Overexpression of ST3Gal I acts as a tumor promoter in a mouse model of breast cancer, while ST6Gal I promotes tumorigenesis and serves as a regulator of the stem cell phenotype (Picco et al. 2010; Swindall et al. 2013). Overexpression of ST8Sia I is restricted in neuroectoderm-derived malignant tumors and estrogen receptor-negative breast cancer (Steenackers et al. 2012). Correspondingly, Sia has been identified as a promising therapeutic target for cancer in several reports, in which sialidases, ST inhibitors and incorporation of Sia or non-natural Sia analogues were applied for the purpose of selectively blocking aberrant sialylation (O’Shea et al. 2014; Bull et al. 2015; Chen et al. 2011).
Oncolytic virus therapy has been intensively investigated and used as a promising alternative approach for treatment of cancer (Patel and Kratzke 2013). Newcastle disease virus (NDV), as an oncolytic virus, is a negative sense single-stranded RNA virus of Avulavirus genus of Paramyxoviridae family with a natural avian host range (Mayo 2002). Its natural oncolytic capability was first described during the 1960s (Cassel and Garrett 1965) and has been demonstrated in several cancer cell lines, animal tumor models and clinical trials (Sinkovics and Horvath 2000; Cheng et al. 2016; Schirrmacher 2015; Zamarin and Palese 2012). The viral infection is initiated by two surface glycoproteins, hemagglutinin-neuraminidase (HN) and fusion (F) proteins. HN binds to the Sia receptors for virus attachment to host cells and is of multifunction including F activation and hydrolyzation of Sia residues (neuraminidase activity) that facilitate progeny virus spreading (Ferreira et al. 2004; Villar and Barroso 2006). Both α2,3- and α2,6-linkage Sia are deployed to mediate NDV entry into host cells (Sanchez-Felipe et al. 2012). Spectacularly, NDV also exerts its oncolytic activity in apoptosis-resistant cancer cells by activation of the intrinsic or mitochondrial apoptosis pathway (Elankumaran et al. 2006; Mansour et al. 2011), which correlates with α2,6-hypersialylation (Swindall and Bellis 2011; Liu et al. 2011). Nevertheless, it is not known about the relation between hypersialylation and oncolytic therapeutic effect of NDV in tumor cells. In the present study, we aimed to clarify the expression level of Sia in various human cancer cells and its impact on virus attachment and infection via up-/down-regulation of Sia expression, and determine the preference of Sia linkage (α2,3- and α2,6-) in viral attachment and oncolytic effect for more effective utilization in anticancer therapy.
Materials and methods
Cell culture and virus
The cell lines, A549, NCI-H460, SW480, SW620 and CHO-K1 were purchased from the Cell Bank of Shanghai Institute of Biochemistry and Cell Biology, Chinese Academy of Sciences (Shanghai, China). The cells were maintained in Roswell Park Memorial Institute-1640 medium (RPMI-1640) supplemented with 10% fetal bovine serum (FBS), 100 U/ml penicillin and 100 μg/ml streptomycin at 37 °C in a 5% CO2 incubator under a humidified atmosphere. Prior to treatment with ST inhibitor, cells were cultured in minimum essential medium RPMI-1640 containing 5% FBS. The NDV Italien strain and recombinant NDV carrying luciferase (rNDV-Luci) were prepared in embryonated specific-pathogen-free chicken eggs and stored in our laboratory. Virus titration was measured by end-point dilution assay with eight replicates for each dilution and expressed in 50% tissue culture infective dose (TCID50) per milliliter, which was calculated by the method of Reed and Muench as previously reported (Wei et al. 2012).
NDV binding tests
When 90% confluency was reached, cells were harvested with cell dissociation buffer (Invitrogen, Carlsbad, CA, USA) and washed with serum-free medium, then infected with NDV Italien strain at a multiplicity of infection (MOI) of 100. After 1 h of incubation at 4 °C, the cells were rinsed three times with cold medium to remove unbound virus.
Competition experiments were performed by preincubating NDV at a low concentration (MOI 10) with either 3′-sialyl-N-acetyllactosamine (3′SLN) (Sigma-Aldrich, St Louis, MO, USA) or 6′-sialyl-N-acetyllactosamine (6′SLN) (Sigma-Aldrich) in a series of doses ranging from 1 to 3 mM. The resultant mixture was added to cells cultured in RPMI-1640 containing 5% FBS and maintained at 4 °C for 1 h after chilling on ice. Then, the cells were rinsed three times with cold medium and assayed for virus binding tests.
For virus binding tests, the cells were incubated at 4 °C for 1 h with chicken polyclonal anti-NDV antibody (Abcam, Cambridge, UK), washed and subsequently incubated at 4 °C for another hour with rabbit fluorescein isothiocyanate (FITC) labeled-anti-chicken IgG antibody (Jackson immunoResearch, West Grove, PA, USA). A chicken IgY (Abcam) was used as isotype control. Cells were washed and fixed with 4% paraformaldehyde. FITC signals were detected using a FACSCalibur flow cytometer (BD, San Jose, CA, USA) and FACS data were analyzed using FlowJo software.
Detection of sialic acid by lectin staining assay
After harvesting, cells were blocked with 1% bovine serum albumin at room temperature for 30 min. Lectin staining was performed by incubation with FITC-labeled Maackia amurensis lectin (MAA; EY Laboratories Inc., San Mateo, CA, USA), Sambucus nigra lectin (SNA; Vector Laboratories, Burlingame, CA, USA) or Maackia amurensis lectin II (MAL II; Vector Laboratories) labeled with fluorescent dye Cy3 (GE Healthcare, Little Chalfont, Buckinghamshire, UK) according to the instructions. MAA and MAL II appear to bind Sia in an α2,3-linkage, while SNA binds α2,6-linkage Sia. The respective lectin was added to the cell cultures and incubated at room temperature for 30 min, rinsed three times with phosphate buffered saline (PBS), and then fixed with 4% paraformaldehyde. Binding of lectin to cells was detected using flow cytometry.
ST inhibitor treatment
A549 and NCI-H460 cells cultured in RPMI-1640 containing 5% FBS were incubated with 128 μmol/L P-3Fax-Neu5Ac. Cells were harvested after 3 days of culture and washed extensively with serum-free medium for the assay of sialylation status using specific carbohydrate-binding lectins MAA and SNA or virus binding test.
Sialidase treatment
The confluent cells were harvested by cell dissociation buffer (Invitrogen), washed with serum-free medium and divided into aliquots of 1 × 106 cells. Then, either specific α2,3-sialidase from Salmonella typhimurium LT2 or bispecific α2,3/6-sialidase from Clostridium perfringens (New England Biolabs, Beverly, MA, USA) was added at 5 units per aliquot and incubated with cells for 3 h at 37 °C. Cells untreated were used as control. Following chilling at 4 °C for 15 min, cells were washed twice with serum-free medium for lectin staining or virus binding test.
CCK-8 assay
Cells were seeded in 96-well plates and infected with NDV Italien at an MOI of 0.1. After 1 h of adsorption, the cells were washed once and refed with RPMI-1640 supplemented with 10% FBS and incubated at 37 °C. Cell viability was assayed after 36 h post-infection. According to the manufacturer’s instructions, 10% CCK-8 solution (Engreen, Beijing, China) was added to each well and absorbance was determined at 450 nm after 2 h of incubation using ELISA microplate readers (BioTek Instruments, Winooski, VT, USA). Uninfected cells were used as the negative control group, and the assay was repeated at least three times.
Surface plasmon resonance (SPR) analysis of glycan–NDV interactions
Biotinylated glycans were obtained from GlycoTech (Rockville, MD, USA). A NLC chip (Bio-Rad Laboratories, Hercules, CA, USA) was used for glycan–NDV interaction analysis on ProteOn XPR36 protein interaction array system (Bio-Rad Laboratories). The channels were regenerated with 1 M NaCl and 50 mM NaOH in horizontal and vertical directions, respectively, for 60 s at 30 μl/min before coupling with glycans. To immobilize the biotinylated glycans onto the streptavidin surface of the NLC chip, 16 µg/ml Neu5Acα2-3GalNAcα-PAA-biotin (01-109; GlycoTech) and 0.2 µg/ml Neu5Acα2-6GalNAcα-PAA-biotin (01-059; GlycoTech) in PBS containing 0.05% Tween 20 (pH 7.4) were injected at a flow rate of 25 μl/min. HOCH2(HOCH)4CH2NH-PAA-biotin (01-000; GlycoTech) without glycan was used as a control. The glycans (01-109 and 01-059) and the glycan-free compound (01-000) were immobilized onto chip in separate flow channels. One channel was left unmodified to provide an additional reference surface. Once the glycan surface on the NLC chip was prepared, the twofold serial dilutions of NDV Italien were injected at a flow rate of 50 μl/min, with 0.506 × 107–8.1 × 107 plaque forming unit (pfu) for 01-109 and 01-000, and 1.5 × 107–16 × 107 pfu for 01-059. For each analyte concentration, association was performed for 180 s and dissociation was monitored for 720 s. Surface was regenerated with 10 mM Gly-HCl by multiple 15 s pulses so that the experiment could be reproduced. After the sensorgrams were processed for baseline alignment and reference channel subtraction, kinetic analysis was performed by globally fitting curves based on a simple 1:1 biomolecular reaction model.
Transfection of CHO-K1 cells with expression vector pcDNA3.1-ST6GAL1
The cDNA of human 2,6-sialyltransferase (ST6GAL1) was obtained from A549 cells under the guidelines of total RNA extraction kit (Omega, Riverside, CA, USA) and PrimeScript RT reagents kit (TaKaRa, Otsu, Japan). The full-length open reading frame of ST6GAL1 was amplified with primers 5′-GGCCGATATGGATCCGCCACCATGATTCACACCAACCTGAAG-3′ and 5′-GGCGCAATAGCGGCCGCTTAGCAGTGAATGGTCCGGAAGCCAG-3′, incorporating BamH I and Not I sites, respectively. The amplified fragment was digested with BamH I and Not I, then cloned into the eukaryotic expression vector pcDNA3.1(+), sequenced and named as pcDNA3.1-ST6GAL1. CHO-K1 cells were transiently transfected with pcDNA3.1-ST6GAL1 using Lipofectamine 2000 Reagent (Invitrogen) according to the manufacturer’s instructions.
Animal studies
Nude mice aged 4–6 weeks (Experimental Animal Centre of Fourth Military Medical University, Xi’an, China) were subcutaneously implanted with either SW480 or SW620 cells (1 × 107 cells in 100 μl PBS). When tumors reached a size of 5–8 mm in diameter, mice were intratumorally injected with PBS or 5 × 107 pfu of rNDV-Luci (in 100 μl PBS) every other day for ten injections in total. The condition of the mice was monitored and the tumor diameter was measured using a digital caliper every other day. The tumor volume was calculated using the formula: width2 × length/2. Tumor growth inhibition rate was calculated as: (1 − tumor volume of treated group/tumor volume of control group) × 100%. Mice were humanely euthanized when tumor size reached 18 mm in any dimension. All mice received humane care and all animal procedures were performed in accordance with Laboratory Animal Ethics Committee of Fourth Military Medical University.
Bioluminescence imaging
rNDV-Luci replication in vivo was monitored by IVIS imaging system (Caliper Life Sciences, Hopkinton, MA) with Living Image acquisition and analysis software (Living Image 3.2, Caliper). The mice were injected intraperitoneally with D-luciferin potassium salt (Yeasen, Shanghai, China) at a dose of 150 mg/kg and anesthetized with isoflurane-mixed oxygen. After 10 min, the bioluminescence of mice was assayed and captured in photos.
Statistical analysis
Comparison between two groups was conducted by unpaired two-tailed Student’s t test using GraphPad Prism version 5.01. Three independent experiments were presented as mean ± SEM. The level of significance was considered at P < 0.05.
Results
Attachment of NDV required sialic acids of host cells
To determine if Sia was necessary for efficient attachment of NDV, two lung cancer cell lines (A549, NCI-H460) were treated with an inhibitor of sialyltransferases, P-3Fax-Neu5Ac (Calbiochem, Darmstadt, Germany) which could selectively inhibit sialylation. The cells were incubated with a high concentration of P-3Fax-Neu5Ac (128 μmol/L) for 3 days, and the α2,3- and α2,6-sialylations were assessed using specific carbohydrate-binding lectins MAA and SNA, respectively. As shown in Fig. 1a, the inhibitor dramatically blocked the expression of α2,3- and α2,6-linked Sia by 90 and 76% on A549 cells, 88 and 78% on NCI-H460 cells. Accordingly, virus attachment was strongly reduced to 5 and 7% on A549 and NCI-H460 cells (Fig. 1b). The results indicated that NDV attachment required Sia of host cells.
Higher affinity of NDV for sialylated glycan motifs with terminal Neu5Acα-2,6 than Neu5Acα-2,3
Although both α2,3- and α2,6-linked Sia were known to act as receptors for NDV binding (Sanchez-Felipe et al. 2012), the interaction of NDV with the two linkages remains to be compared. Therefore, an SPR-based analysis of glycan–virus interactions was developed to monitor and evaluate the receptor binding preference of NDV between α2,3- and α2,6-linked Sia in real-time. The α2,3-sialyl glycan (NeuAcα-2,3GalNAc), α2,6-sialyl glycan (NeuAcα-2,6GalNAc) and glycan-free biotinylated compound [HOCH2(HOCH)4CH2NH] were sequentially immobilized onto the streptavidin surface of the NLC chip; HOCH2(HOCH)4CH2NH was used as a negative control. Five different concentrations of NDV Italien strain were injected into the flow channels which were coated with NeuAcα-2,3GalNAc, NeuAcα-2,6GalNAc or HOCH2(HOCH)4CH2NH. Specific binding responses of NDV to both NeuAcα-2,3GalNAc and NeuAcα-2,6GalNAc were observed and the equilibrium dissociation constant (K D) was calculated based on the association constant (Ka) and the dissociation constant (K d) which demonstrated a tenfold higher affinity of NDV for α2,6-linkage than α2,3-linkage. No signal showed in the negative control (Fig. 2).
α2,6-linked sialic acid displayed a preferred specificity for NDV binding
To further identify which specific linkage NDV utilized for binding, A549 cells were pretreated with specific α2,3-sialidase (from Salmonella typhimurium LT2) to reduce α2,3-linkage level or bispecific α2,3/6-sialidase (from Clostridium perfringens) to reduce both α2,3- and α2,6-linkage levels. No specific α2,6-sialidase was commoditized, so that the individual reduction of α2,6-linkage level was unavailable. The specificity of both sialidases hydrolyzing α2,3- and α2,3/6-glycosidic linkages of terminal Sia residues was confirmed by flow cytometry with linkage-specific lectins (Fig. 3a). Although treatment with the two sialidases decreased α2,3- and α2,6-linkages to approximately equal level (Fig. 3a), α2,3-sialidase caused minor reduction in NDV binding and α2,3/6-sialidase dramatically inhibited virus binding (Fig. 3b), which indicated a more important role of α2,6-linkage for NDV binding. Furthermore, the sialylated trisaccharides 3′SLN and 6′SLN describing the features of authentic sialylated receptors in nature were used as potential receptor analogues in attachment assays. Preincubation of NDV (MOI 10) with 3′SLN and 6′SLN inhibited viral attachment in a dose-dependent manner while 6′SLN was more competitive for NDV binding than 3′SLN (Fig. 3c). Taken together, these data suggest that both α2,3- and α2,6-linked Sia act as functional receptors for NDV and the virus preferentially utilizes α2,6-sialylated glycans for binding.
The effects of sialidases and sialyl-N-acetyllactosamine (SLN) on sialic acid expression and NDV binding were detected by FACS analysis in A549 cells. The inhibiting efficiency of sialidases on α2,3- and α2,6-linked sialic acid expressions (a) and virus binding (b). Untreated cells were used as control and unstained cells were as background. c Suppression effects of 3′SLN and 6′SLN on virus binding. *P < 0.05, **P < 0.01, ***P < 0.001
Ectopic expression of ST6Gal I sialyltransferase increased the α2,6-linkage level leading to enhanced NDV binding and cytopathic effect
To further test the role of α2,6-linkage in NDV binding, we used CHO-K1 cells which lack a functional copy of the gene encoding α2,6-sialyltransferase leading to a lower level of α2,6-linkage (Fig. 4a). The ST6Gal I sialyltransferase can catalyze the transfer of Sia from cytidine monophosphate-sialic acid in an α2,6-linkage to the termini of N-glycans. To ectopically express ST6Gal I in CHO-K1 cells, an expression plasmid containing ST6Gal I was constructed (Fig. 4b). Subsequently, transient transfection of CHO-K1 cells with the plasmid resulted in a twofold increase of α2,6-linked Sia and decrease of α2,3-linked Sia by half (Fig. 4c), and the virus binding increased more than twofold compared with the mock control (Fig. 4d). Accordingly, NDV showed an enhanced killing effect in ST6Gal I-transfected cells after 36 h post-infection compared with mock control (Fig. 4e).
The effects of ectopic presence of α2,6-linked sialic acid on NDV binding and virus-induced cytopathic effect. a The presences of Sia linkages were detected by FACS analysis in CHO-K1 cells. b The pcDNA3.1(+) plasmid expressing the sialyltransferase gene ST6GAL1 was constructed and validated by colony PCR. c Sialic acid expression was detected in CHO-K1 cells transfected with ST6Gal I expression vector. d, e NDV binding and cytopathic effect in ST6Gal I-transfected cells were detected by FACS analysis and CCK-8 assay, respectively. Cells transfected with pcDNA3.1(+) plasmid were used as mock and unstained cells were as background. *P < 0.05, **P < 0.01
Therapeutic antitumor efficacy of NDV correlated with expression of α2,6-sialic acid in colon tumors
To explore the link between antitumor efficacy of NDV and α2,6-Sia expression level of tumor cells, we tested the Sia linkages on the surfaces of two colon cancer (SW620, SW480) cell lines. According to the American Type Culture Collection information, SW620 cell line was derived from a metastasis of the same colorectal adenocarcinoma from which the SW480 was derived. Interestingly, flow cytometry analysis showed that SW480 and SW620 cells displayed higher levels of α2,3- and α2,6-linkages, respectively (Fig. 5a), thus we used the two cell lines to perform the virus replication-induced cytotoxicity assay. The cell mortality rates of NDV infection in SW620 cells were higher than that of SW480 cells after 36 h post-infection (Fig. 5b). To assess the in vivo therapeutic efficacy of NDV, nude mice were engrafted with SW480 and SW620 cells subcutaneously, and then intratumorally treated with 5 × 107 pfu of rNDV-Luci, which was a recombinant NDV Italien strain expressing firefly luciferase for visualization of virus distribution with similar replicative properties as its wild-type (Wei et al. 2012). As shown in Fig. 5c, inoculation of SW620 cells induced a higher propagation rate of tumor than that of SW480 cells, indicating the more aggressiveness of SW620. The application of rNDV-Luci was able to reduce both tumor burdens as illustrated by tumor volume measurements compared with control mice treated with PBS. However, the rNDV-Luci exhibited a considerable tumor growth inhibitory effect in SW620 cells than SW480 cells. Thirty days after treatment, luciferase expression and therapeutic efficacy of rNDV-Luci were visualized in vivo by IVIS imaging. As seen in Fig. 5d, virus was able to express luciferase only within tumor and the signal intensity was consistent with tumor volume. Taken together, these data highlight that NDV can be used as an effective and safe oncolytic virotherapy for human cancer with higher α2,6-sialylation.
Correlation of α2,6-linked sialic acid expression and antitumor effect of NDV in vitro and in vivo. a Expression of α2,3- and α2,6-linked sialic acids in two colon cancer cell lines detected by FACS analysis. b Cell mortality rates of two colon cancer cell lines after infection of NDV Italien were determined with CCK-8 assay. c Nude mice were subcutaneously implanted with SW480 and SW620 cells. Then the mice were intratumorally treated with 5 × 107 pfu rNDV-Luci every other day for a total of ten injections. Mice that received PBS were used as control. n = 10. d Luciferase expression of rNDV-Luci in tumor-bearing mice at 30 days post-intratumoral injection by IVIS imaging. *P < 0.05, **P < 0.01, ***P < 0.001
Discussion
We intensively investigated here the possible effects of sialylation modification on cell entry and infection of oncolytic NDV in the human non-small cell lung carcinomas (A549 and NCI-H460) and colorectal carcinoma cell lines (SW480 and SW620), in which SW620 is more tumourigenic and metastatic potentials than SW480 as demonstrated previously (Hewitt et al. 2000). We further analyzed the receptor binding preference of NDV between two primary α2,3- and α2,6-linked sialylation.
Altered sialylation is associated with various aspects of malignant transformation (Yogeeswaran and Salk 1981; Kim and Varki 1997). Elevated cell surface sialylation is a common characteristic of tumor cells and attributed to dysregulation of selected sialyltransferases (Dall’Olio and Chiricolo 2001; Harduin-Lepers et al. 2012). Evidences are accumulating that overexpression of α2,6-Sia occurs in many different cancers, including breast (Alley and Novotny 2010), ovarian (Christie et al. 2008), lung (Vasseur et al. 2012), gastric (Ozaki et al. 2012) and colon (Seales et al. 2005), which corresponds to the up-regulation of ST6Gal I (Gessner et al. 1993) or ST6GalNAc STs (Marcos et al. 2004). In this study, the hypersialylation of α2,6-linkage was detected in SW620 cell lines and oncolytic NDV killed SW620-derived tumors much more effectively than SW480, suggesting an advantage of oncolytic virotherapy using NDV in lysing α2,6-hypersialylated cancerous cells.
We also clarified the direct effect of sialylation in viral attachment by ST inhibitor and sialidase treatment. P-3Fax-Neu5Ac is a fluorinated Sia analogue that globally blocks sialylation via inhibiting STs and preventing the synthesis of Sia with high potency and long-term effect. The blockage of sialylation with P-3Fax-Neu5Ac strongly prevented viral attachment accompanied with the depletion of α2,3- or α2,6-linked Sia in A549 and NCI-H460 cells. Likewise, linkage-specific sialidase treatment resulted in defective sialylation of α2,3- or α2,6-linkage and reduced virus binding of A549 cells. Moreover, the results implied that α2,6-linkage is a major contributor to virus binding relative to α2,3-linkage.
The advancements of SPR technology have facilitated the analyses of virus and glycan interactions. By this method, NDV Italien strain showed a preference affinity ratio of about 10 between α2,3- and α2,6-linkages. In competition assay, 6′SLN inhibited NDV attachment more efficiently than 3′SLN did in A549 cells. Taken together, these findings indicate that NDV preferentially recognizes Sia receptor with an α2,6-linkage.
The α2,6-hypersialylation correlates with not only increased metastasis and enhanced tumor cell survival, but also a less differentiated phenotype (Hedlund et al. 2008). The present study applied forced overexpression of ST6Gal I that up-regulated α2,6-linked Sia level in a cell model, CHO-K1 which is naturally lack of α2,6-linked Sia. As expected, the decreased expression of α2,3-linked Sia in ST6Gal I-transfected cells by approximately 50% due to the competition between α2,6-ST and α2,3-ST which utilized the same substrate. But the status did not impair the enhanced binding of NDV to ST6Gal I-transfected cells, which further suggested the more defined role of α2,6-sialylation in viral attachment and infection. Furthermore, it was confirmed that therapeutic effect of oncolytic NDV was in agreement with high levels of α2,6-linked Sia in xenografted colon tumors. Accordingly, the data available so far may be developing a novel treatment strategy that define α2,6-linked Sia as a potential target in oncolytic virotherapy with NDV.
Abbreviations
- F:
-
Fusion
- FBS:
-
Fetal bovine serum
- FITC:
-
Fluorescein isothiocyanate
- Gal:
-
Galactose
- GalNAc:
-
N-acetylgalactosamine
- HN:
-
Hemagglutinin-neuraminidase
- K a :
-
Association constant
- K d :
-
Dissociation constant
- K D :
-
Equilibrium dissociation constant
- MAA:
-
Maackia amurensis lectin
- MAL II:
-
Maackia amurensis lectin II
- MOI:
-
Multiplicity of infection
- NDV:
-
Newcastle disease virus
- Neu5Ac:
-
N-acetylneuraminic acid
- Pfu:
-
Plaque forming unit
- RPMI-1640:
-
Roswell Park Memorial Institute-1640 medium
- Sia:
-
Sialic acids
- ST6GAL1:
-
2,6-sialyltransferase
- 3′SLN:
-
3′-sialyl-N-acetyllactosamine
- 6′SLN:
-
6′-sialyl-N-acetyllactosamine
- SNA:
-
Sambucus nigra
- STs:
-
Sialyltransferases
References
Alley WJ, Novotny MV (2010) Glycomic analysis of sialic acid linkages in glycans derived from blood serum glycoproteins. J Proteome Res 9:3062–3072. doi:10.1021/pr901210r
Bull C, Boltje TJ, van Dinther EA, Peters T, de Graaf AM, Leusen JH, Kreutz M, Figdor CG, den Brok MH, Adema GJ (2015) Targeted delivery of a sialic acid-blocking glycomimetic to cancer cells inhibits metastatic spread. ACS Nano 9:733–745. doi:10.1021/nn5061964
Cassel WA, Garrett RE (1965) Newcastle disease virus as an antineoplastic agent. Cancer 18:863–868
Chen JY, Tang YA, Huang SM, Juan HF, Wu LW, Sun YC, Wang SC, Wu KW, Balraj G, Chang TT, Li WS, Cheng HC, Wang YC (2011) A novel sialyltransferase inhibitor suppresses FAK/paxillin signaling and cancer angiogenesis and metastasis pathways. Cancer Res 71:473–483. doi:10.1158/0008-5472.CAN-10-1303
Cheng X, Wang W, Xu Q, Harper J, Carroll D, Galinski MS, Suzich J, Jin H (2016) Genetic modification of oncolytic Newcastle disease virus for cancer therapy. J Virol 90:5343–5352. doi:10.1128/JVI.00136-16
Christie DR, Shaikh FM, Lucas JT, Lucas JR, Bellis SL (2008) ST6Gal-I expression in ovarian cancer cells promotes an invasive phenotype by altering integrin glycosylation and function. J Ovarian Res 1:3. doi:10.1186/1757-2215-1-3
Dall’Olio F, Chiricolo M (2001) Sialyltransferases in cancer. Glycoconj J 18:841–850
Dube DH, Bertozzi CR (2005) Glycans in cancer and inflammation–potential for therapeutics and diagnostics. Nat Rev Drug Discov 4:477–488. doi:10.1038/nrd1751
Elankumaran S, Rockemann D, Samal SK (2006) Newcastle disease virus exerts oncolysis by both intrinsic and extrinsic caspase-dependent pathways of cell death. J Virol 80:7522–7534. doi:10.1128/JVI.00241-06
Ferreira L, Villar E, Munoz-Barroso I (2004) Gangliosides and N-glycoproteins function as Newcastle disease virus receptors. Int J Biochem Cell Biol 36:2344–2356. doi:10.1016/j.biocel.2004.05.011
Fuster MM, Esko JD (2005) The sweet and sour of cancer: glycans as novel therapeutic targets. Nat Rev Cancer 5:526–542. doi:10.1038/nrc1649
Gessner P, Riedl S, Quentmaier A, Kemmner W (1993) Enhanced activity of CMP-neuAc: Gal beta 1–4GlcNAc:alpha 2,6-sialyltransferase in metastasizing human colorectal tumor tissue and serum of tumor patients. Cancer Lett 75:143–149
Harduin-Lepers A, Vallejo-Ruiz V, Krzewinski-Recchi MA, Samyn-Petit B, Julien S, Delannoy P (2001) The human sialyltransferase family. Biochimie 83:727–737
Harduin-Lepers A, Krzewinski-Recchi MA, Colomb F, Foulquier F, Groux-Degroote S, Delannoy P (2012) Sialyltransferases functions in cancers. Front Biosci (Elite Ed) 4:499–515
Hedlund M, Ng E, Varki A, Varki NM (2008) alpha 2-6-Linked sialic acids on N-glycans modulate carcinoma differentiation in vivo. Cancer Res 68:388–394. doi:10.1158/0008-5472.CAN-07-1340
Hewitt RE, McMarlin A, Kleiner D, Wersto R, Martin P, Tsokos M, Stamp GW, Stetler-Stevenson WG (2000) Validation of a model of colon cancer progression. J Pathol 192:446–454
Kim YJ, Varki A (1997) Perspectives on the significance of altered glycosylation of glycoproteins in cancer. Glycoconj J 14:569–576
Liu Z, Swindall AF, Kesterson RA, Schoeb TR, Bullard DC, Bellis SL (2011) ST6Gal-I regulates macrophage apoptosis via alpha2-6 sialylation of the TNFR1 death receptor. J Biol Chem 286:39654–39662. doi:10.1074/jbc.M111.276063
Mansour M, Palese P, Zamarin D (2011) Oncolytic specificity of Newcastle disease virus is mediated by selectivity for apoptosis-resistant cells. J Virol 85:6015–6023. doi:10.1128/JVI.01537-10
Marcos NT, Pinho S, Grandela C, Cruz A, Samyn-Petit B, Harduin-Lepers A, Almeida R, Silva F, Morais V, Costa J, Kihlberg J, Clausen H, Reis CA (2004) Role of the human ST6GalNAc-I and ST6GalNAc-II in the synthesis of the cancer-associated sialyl-Tn antigen. Cancer Res 64:7050–7057. doi:10.1158/0008-5472.CAN-04-1921
Mayo M (2002) A summary of taxonomic changes recently approved by ICTV. Arch Virol 147:1655–1663. doi:10.1007/s007050200039
O’Shea LK, Abdulkhalek S, Allison S, Neufeld RJ, Szewczuk MR (2014) Therapeutic targeting of Neu1 sialidase with oseltamivir phosphate (Tamiflu(R)) disables cancer cell survival in human pancreatic cancer with acquired chemoresistance. Onco Targets Ther 7:117–134. doi:10.2147/OTT.S55344
Ozaki H, Matsuzaki H, Ando H, Kaji H, Nakanishi H, Ikehara Y, Narimatsu H (2012) Enhancement of metastatic ability by ectopic expression of ST6GalNAcI on a gastric cancer cell line in a mouse model. Clin Exp Metastasis 29:229–238. doi:10.1007/s10585-011-9445-1
Patel MR, Kratzke RA (2013) Oncolytic virus therapy for cancer: the first wave of translational clinical trials. Transl Res 161:355–364. doi:10.1016/j.trsl.2012.12.010
Picco G, Julien S, Brockhausen I, Beatson R, Antonopoulos A, Haslam S, Mandel U, Dell A, Pinder S, Taylor-Papadimitriou J, Burchell J (2010) Over-expression of ST3Gal-I promotes mammary tumorigenesis. Glycobiology 20:1241–1250. doi:10.1093/glycob/cwq085
Sanchez-Felipe L, Villar E, Munoz-Barroso I (2012) alpha2-3- and alpha2-6- N-linked sialic acids allow efficient interaction of Newcastle disease virus with target cells. Glycoconj J 29:539–549. doi:10.1007/s10719-012-9431-0
Schauer R (2009) Sialic acids as regulators of molecular and cellular interactions. Curr Opin Struct Biol 19:507–514. doi:10.1016/j.sbi.2009.06.003
Schirrmacher V (2015) Oncolytic Newcastle disease virus as a prospective anti-cancer therapy. A biologic agent with potential to break therapy resistance. Expert Opin Biol Ther 15:1757–1771. doi:10.1517/14712598.2015.1088000
Seales EC, Jurado GA, Brunson BA, Wakefield JK, Frost AR, Bellis SL (2005) Hypersialylation of beta1 integrins, observed in colon adenocarcinoma, may contribute to cancer progression by up-regulating cell motility. Cancer Res 65:4645–4652. doi:10.1158/0008-5472.CAN-04-3117
Sinkovics JG, Horvath JC (2000) Newcastle disease virus (NDV): brief history of its oncolytic strains. J Clin Virol 16:1–15
Steenackers A, Vanbeselaere J, Cazet A, Bobowski M, Rombouts Y, Colomb F, Le Bourhis X, Guerardel Y, Delannoy P (2012) Accumulation of unusual gangliosides G(Q3) and G(P3) in breast cancer cells expressing the G(D3) synthase. Molecules 17:9559–9572. doi:10.3390/molecules17089559
Swindall AF, Bellis SL (2011) Sialylation of the Fas death receptor by ST6Gal-I provides protection against Fas-mediated apoptosis in colon carcinoma cells. J Biol Chem 286:22982–22990. doi:10.1074/jbc.M110.211375
Swindall AF, Londono-Joshi AI, Schultz MJ, Fineberg N, Buchsbaum DJ, Bellis SL (2013) ST6Gal-I protein expression is upregulated in human epithelial tumors and correlates with stem cell markers in normal tissues and colon cancer cell lines. Cancer Res 73:2368–2378. doi:10.1158/0008-5472.CAN-12-3424
Vasseur JA, Goetz JA, Alley WJ, Novotny MV (2012) Smoking and lung cancer-induced changes in N-glycosylation of blood serum proteins. Glycobiology 22:1684–1708. doi:10.1093/glycob/cws108
Villar E, Barroso IM (2006) Role of sialic acid-containing molecules in paramyxovirus entry into the host cell: a minireview. Glycoconj J 23:5–17. doi:10.1007/s10719-006-5433-0
Wei D, Sun N, Nan G, Wang Y, Liu HQ, Peeters B, Chen ZN, Bian H (2012) Construction of recombinant Newcastle disease virus Italien strain for oncolytic virotherapy of tumors. Hum Gene Ther 23:700–710. doi:10.1089/hum.2011.207
Yogeeswaran G, Salk PL (1981) Metastatic potential is positively correlated with cell surface sialylation of cultured murine tumor cell lines. Science 212:1514–1516
Zamarin D, Palese P (2012) Oncolytic Newcastle disease virus for cancer therapy: old challenges and new directions. Future Microbiol 7:347–367. doi:10.2217/fmb.12.4
Acknowledgments
The authors thank Prof. Volker Schirrmacher (German Cancer Research Center, Germany) for the gift of NDV Italien.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
This work was supported by grants from the National Natural Science Foundation of China (31571434, 81172144, 81201776) and the National Science and Technology Major Project (2015CB553701, 2012ZX10002-015, 2012AA020806).
Conflict of interest
All authors have read the journal’s policy on disclosure of potential conflicts of interest and have none to declare. All authors have read the journal’s authorship agreement, and the manuscript has been reviewed and approved by all named authors.
Rights and permissions
About this article
Cite this article
Li, Q., Wei, D., Feng, F. et al. α2,6-linked sialic acid serves as a high-affinity receptor for cancer oncolytic virotherapy with Newcastle disease virus. J Cancer Res Clin Oncol 143, 2171–2181 (2017). https://doi.org/10.1007/s00432-017-2470-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-017-2470-y