Abstract
Purpose
Cervical cancer is the second most prevalent cancer in women worldwide. Survival of patients has been improved by cisplatin-based chemotherapy, but its effectiveness is limited due to its adverse effects on many tissues, especially nephrotoxicity. To optimize the efficacy of CDDP, we propose a combination therapy using natural products with minimal side effects. Vitamin C being a natural antioxidant is capable of selectively targeting cancer cells at pharmacological concentrations. Vitamin C synergistically enhances the activity of chemotherapeutic agents without increasing toxicity to normal cells. Therefore, we exploited co-therapy with cisplatin and vitamin C to kill cervical cancer cells.
Methods
We elucidated the role of CDDP and VC on cervical cancer cell line (SiHa) by using cell growth assays, DNA fragmentation analysis, comet assay, in vitro morphological assessment of apoptosis (AO/EB and DAPI staining), ROS analysis by DCFDA, flow cytometry, biochemical assays (GST, GSH, NO, catalase, TPA) and Western blotting.
Results
Our results clearly demonstrated that CDDP and VC treatment exhibited ameliorative effect on induction of cell death by p53 overexpression and generation of hydrogen peroxide in SiHa cells, thereby reducing the dosage of CDDP required to induce cell death in cancer cells.
Conclusions
These studies provide novel approaches to combat cisplatin resistance in cervical cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cervical cancer has a high mortality rate among women globally and is the most common cancer in many developing countries. Despite numerous advances in terms of early diagnosis and cervical cancer treatment in recent years, the prognosis of advanced-stage or recurrent cervical cancer is rather poor (Cuzick et al. 2008).
Cisplatin (CDDP) is used as a first-line anticancer drug for the treating epithelial malignancies, including ovarian, lung, cervical and testicular cancer. It exerts its anti-tumor effect by forming intra-strand crosslinks that inhibit replication and result in activation of cellular signaling pathways controlling cell death (Hernandez-Flores et al. 2011). However, CDDP chemotherapy has been associated with adverse side effects, including nephrotoxicity, neurotoxicity and hepatotoxicity. Furthermore, in advanced-stage cervical cancer patients, intrinsic resistance to CDDP also develops due to several factors (Kartalou and Essigmann 2001). Therefore, novel regimens or agents in combination with CDDP are essential to enhance anticancer activity with minimal adverse effects (Jurado et al. 2009).
In recent years, cancer therapies using chemotherapy, radiotherapy, hyperthermia and natural plant products that can induce p53-mediated apoptosis have received attention. A naturally occurring food supplement, vitamin C (VC), is a water-soluble vitamin with antioxidant properties. VC is an active reducing agent and plays a crucial role in the detoxification and metabolism of several exogenous and endogenous compounds (Henson et al. 1991). Various studies reported a good therapeutic potential of VC against cancer (Head 1998; Ohno et al. 2009). VC has been reported to enhance the efficacy of numerous chemotherapeutic drugs (Chiang et al. 1994; Kurbacher et al. 1996). Moreover, VC has been reported to stabilize the apoptosis-inducing p53 gene (Kim et al. 2012a). The reason for intrinsic resistance to chemotherapeutic drugs might be due to the altered p53 pathway in the majority of human cancers mostly by upregulation of MDM2, downregulation of p14ARF or mutation of p53 gene (Zilfou and Lowe 2009).
Some studies have examined the effect of VC on cancer and have elucidated some of the underlying mechanisms, and the available information is still debated on the utility of VC, especially in terms of its effect in cervical cancer. In addition, the aim of this study was to evaluate the cytotoxic effects of VC per se, CDDP per se and combination of both, in human cervical cancer cell line (SiHa) and human embryonic kidney cell line (HEK) and to see the mechanism involved. We have also examined the role of p53 as a sensitizer for VC cytotoxicity and hypothesize that p53 gene activation renders cells more sensitive to VC-induced oxidative stress. The findings exhibit that the use of VC with CDDP could be very useful in enhancing the therapeutic efficacy against cervical cancer cell line.
Materials and methods
Chemicals and reagents
RPMI 1640, fetal bovine serum, phosphate-buffered saline (PBS), paraformaldehyde, penicillin, streptomycin, acridine orange, ethidium bromide, 1-chloro, 2, 4-dinitrobenzene (CDNB), sodium bicarbonate, dimethyl sulfoxide (DMSO), HEPES (hydroxyl ethyl piperazine ethanesulfonic acid), vitamin C, cisplatin, propidium iodide, Triton X-100, RNase A, (3-(4, 5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide), DCFDA, DAPI, MTT reagent all were purchased from Sigma-Aldrich (USA). Trichloroacetic acid (TCA), paraformaldehyde, nitrobluetetrazolium, NADH, sulfanilamide, N-1-napthylethylenediamine dihydrochloride (NEDD), dithiobis-2-dinitrobenzoic acid (DTNB) orthophosphoric acid and ethylenediaminetetraacetic acid (EDTA) were purchased from SRL, India.
Cell culture and maintenance
HEK and SiHa cell lines were procured from National Cell Culture Science, Pune, India. The cell lines were maintained RPMI 1640 + 10 % FBS supplemented with l-glutamine and streptomycin/penicillin, 25 mM HEPES buffer) with 5 % CO2 at 37 °C.
In vitro biocompatibility evaluation
HEK and SiHa cell lines were treated with dose ranging between 200 and 5 µM CDDP for 24 h, 100 and 25 µg/ml VC for 24, 48 and 72 h, respectively. Combination study was done with different doses of CDDP and VC. Doses (100, 50, 5 and 1 µM) of CDDP were selected, and their combination effect with VC was observed at dose of 100 µg/ml VC for 24, 48 and 72 h. CDDP (50 µM) was also tested with 50 µg/ml VC for 24, 48 and 72 h. Percentage viability was calculated as per standard protocol described previously (Verma et al. 2005).
Apoptosis
CDDP in combination with VC induces apoptosis that is quantified by AO/EB double staining using standard protocol with slight modifications (Liu et al. 2015) by fluorescent microscopy.
DNA fragmentation assay
DNA fragmentation was performed according to previously published protocol (An et al. 2011).
DAPI staining
In vitro morphological assessment of apoptosis was performed according to the protocol of Kwon et al. (2016).
ROS analysis by DCFDA
Oxidative stress analysis using H2DCFDA dye was done as per previously published protocol (Ahamad et al. 2014).
Spectrofluorometric quantification of ROS generation
Quantification of H2O2 generation was done according to the protocol of Pajaniradje et al. (2014).
Cell cycle analysis by flow cytometry
Apoptosis detection by flow cytometry was carried out as per previously published protocol (Wlodkowic et al. 2009).
Comet assay
The comet assay was performed under alkaline conditions (pH > 13) according to the procedure of Singh et al. (1988). The images were analyzed using computer-based image analysis system CASP—Comet Assay Software Project by Końca et al. (2003). Visual image analyses of DNA damage were carried out in accordance with the protocol of Collins et al. (1996). Cells were visually assigned a score on an arbitrary scale of 0–4 (i.e., ranging from 0: no DNA damage to 4: extensive DNA damage) (Fig. 9) based on perceived comet tail length migration and relative proportion of DNA in the comet tail.
Western blotting
Expression of p53 protein was determined by the protocol of Blancher and Jones (2001). The bands were analyzed and quantified using an image scanner densitometer and normalized to an actin control. The density of the control was taken as 1, and results of the treatment were expressed in relative units (RU) compared to control.
Biochemical assays
GSH activity
Reduced glutathione estimation was performed by following the protocol of Moron et al. (1979).
Catalase assay
Catalase activity was estimated by the method of Aebi (1984) with minor modifications.
NO assay
NO assay was performed as per protocol of Griess (1879).
GST activity
The GST activity was performed as per previously published protocol (Habig and Pabst 1974).
Total peroxidase assay (TPA)
TPA was performed as per previously published protocol (Wolff 1994).
Statistical analysis
For most of the above experiments, statistical analysis among various treatment groups were done by comparing the untreated group with treated groups by applying one-way ANOVA test followed by Tukey’s test. Significant difference between the groups was found at p < 0.005. All results were done in triplicate.
Results and discussion
CDDP is a widely known anticancer drug employed for treating wide array of human cancers. CDDP exerts its anticancer action via the formation of DNA-platinum crosslinks, followed by DNA damage and activation of signal transduction pathways, culminating into cell cycle arrest at S, G1 or G2/M phases and finally leading to apoptosis (An et al. 2011). However, cisplatin possessed genotoxicity by inducing DNA damage of recombinational origin (Danesi et al. 2010) and anticipated to be human carcinogen (Waalkes et al. 2006). There are side effects from the use of cisplatin, such as nephrotoxicity, ototoxicity, nausea, vomiting and development of resistance in the cancer cells (Cepeda et al. 2007).
Accumulating evidences have reported the anticancer activity of VC on tumor cells (Chen et al. 2005; Kim et al. 2012b). Hahm et al. reported anticancer effect of VC on melanoma cell proliferation. VC inhibited the melanoma cell proliferation in time- and dose-dependent manner that indicates the potential of VC in modulating tumor cell growth (Hahm et al. 2007). Combination chemotherapy or co-chemotherapy is an approach to increase the effectiveness of cisplatin as well as suppress its side effects. In our study, the percent cytotoxicity of CDDP and VC was assessed on SiHa and HEK cell lines in dose- and time-dependent manner. The anti-proliferative effects of CDDP and VC on human cervical cancer cells and HEK were determined by the cell toxicity evaluation based on MTT assay. The percent cytotoxicity of CDDP on SiHa cell line was assessed at dose ranging between 5 and 200 µM. The IC50 of CDDP on SiHa cell line is 145 µM. At 100 µM CDDP, 22.1 ± 0.88 % cytotoxicity was achieved post 24 h of treatment. Similarly, the percent toxicity of VC was assessed at doses of 25, 50 and 100 µg/ml for 24, 48 and 72 h and the percent cytotoxicity was observed to be 4.86 ± 0.23, 16.53 ± 1.22 and 26.50 ± 1.32, respectively, post 72 h of treatment. Therefore, 100 µg/ml dose of VC dose was taken as a referral to assess the cytotoxicity of CDDP (100 µM) with VC on SiHa and HEK cell lines (Fig. 1).
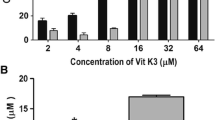
For the combination studies, SiHa and HEK cells were treated with varying concentrations of CDDP (100, 50, 5 and 1 µM) and/or VC (50, 100 μg/ml) for 24, 48 and 72 h. The percent cytotoxicity post-treatment with CDDP (100, 50, 5 and 1 µM) and 100 μg/ml of VC was observed to be 85.45 ± 3.6 %, 57.58 ± 4.2 %, 28.83 ± 3.5 % and 28.37 ± 2.4 %, respectively, and with 50 µg/ml VC and 50 µM CDDP, the cytotoxicity post 72 h was 58.41 ± 0.87 %, respectively. Hence, the treatment of 100 μg/ml of VC with 100 µM CDDP acted synergistically to enhance the cytotoxicity (Fig. 2). These results indicated that VC boosted the chemotherapeutic response of cervical cancer cells. But, in HEK cell line, VC and CDDP combination had negligible cytotoxicity that confirms the selective nature of VC in killing the cancer cells (Yun et al. 2015) (Fig. 3). Normal tissues have adequate blood flow that supplies antioxidant enzymes such as catalase and glutathione peroxidase to counter harmful hydroxyl radicals (Bao et al. 2013). Owing to this reason, CDDP and VC have negligible toxicity on HEK cell line.
These results were supported by the morphological changes occurring in SiHa cells post-treatments. It was found that the morphology of SiHa cells was distorted in cells treated with 100 µM of CDDP + 100 µg of VC (Fig. 4c).
Similarly, to visualize the morphological changes occurring in the nucleus of the SiHa cells post-treatments, in vitro DAPI staining was performed. As evident from the figure, maximum nuclear condensation and blebbing were observed in combination treatment, i.e., 100 µM CDDP + 100 µg/ml VC whereas intact nucleus was observed in untreated SiHa cells (Fig. 5).
To assess the fragmentation of DNA, DNA fragmentation assay was performed. The DNA degradation into numerous fragments comprising of 180–200 bp is considered as important hallmark of apoptosis (Hooker et al. 2012). DNA fragmentation assay has been used to study inter-nucleosomal DNase activity in apoptotic cells (Zhang and Xu 2000). Figure 6 shows the results of agarose gel electrophoresis of DNA extracted from the cells. Slight DNA fragmentation was seen in the presence of 100 μg/ml of VC (Fig. 6, Lane 1), indicating moderate DNA degradation. CDDP induced a characteristic DNA ladder pattern that is characteristic of apoptosis (Fig. 6, Lane 2). Moreover, an intensive pattern of apoptotic DNA fragmentation was visualized in combination treatments rather than in the individual ones (Fig. 6, Lane 3), confirming the synergistic action of CDDP and VC (Fig. 6).
AO/EB staining was performed to assess the mode of cell death. This staining identifies the different stages of cells that are undergoing apoptosis and necrosis. Increase in the number of apoptotic cells was observed when treated with the combination of VC and CDDP when compared to CDDP per se. Furthermore, upon VC treatment, slight increase was observed in the number of cells undergoing late apoptosis or necrosis. A green intact nuclear structure was seen in untreated SiHa cells (Fig. 7a), but with free CDDP and combination treatment, we observed nuclear margination and cell blebbing (Fig. 7c, d), chromatin condensation (e.g., in Fig. 7c) (early and moderate apoptosis), orange nuclei with normal distribution of chromatin (necrosis) (e.g., in Fig. 7d), as well as reddish-orange color indicating late apoptosis.
To visualize and assess the DNA damage in single cell, single-cell gel electrophoresis (comet assay) was done. The damaged DNA releasing from the nucleus under applied voltage forms a comet that provides us with the percent damage (Fig. 8). In addition, it has been employed in assessing double- and single-strand breaks, alkali-labile sites (Garaj-Vrhovac and Kopjar 2003).
After incubation of SiHa cells with 100 µM CDDP, it was observed that the DNA content in comet tails (30.25 ± 3.54 %) was increased. At the concentration of 100 µg/ml VC, slight increase in DNA migration by 16.48 ± 2.73 % in comet tails was reported whereas negative control exhibited percent tail damage of 3.26 ± 0.41 %. Maximum DNA damage, with an increase of DNA by 50.52 ± 5.9 % in comet tails, was noted after the exposure of SiHa cells to 100 µM CDDP + 100 µg/ml VC. Enhanced DNA damage post-incubation with VC and CDDP was partly associated with pro-oxidant effect of VC leading to H2O2 production that facilitates apoptosis (Kim et al. 2012a), thereby enhancing the chemotherapeutic effect of CDDP (Fig. 9).
DNA fragment migration patterns by alkaline comet assay taken with a fluorescence microscope (with excitation filter 420–490 nm). a Intact cells (control); most of the DNA is located in the head of the comet, b cell line treated by 100 µM CDDP, c 100 µg VC, d 100 µM CDDP + 100 µg VC; the presence of the tail reflects the DNA damage
To confirm the results obtained from MTT, DAPI staining, comet assay, DNA fragmentation assay, FACS analysis was performed. Elevated proportions of sub-G1 and apoptotic cells were respectively found in the combinative treatments in comparison with hypothetic values of additive effects (Fig. 10). In SiHa cells, apoptosis was induced by VC and CDDP, which was detected by annexin V and PI. In the contour plots, X axis reflects the annexin V FITC staining and Y axis corresponds to PI staining in logarithmic scale (Fig. 11). Annexin V FITC versus PI contour plots with quadrant gates shows four populations. The annexin V+/PI– is early apoptotic cells, and annexin V+/PI+ is late apoptotic cells (Fig. 11). The percent of apoptotic cells are 4.12, 4.27, 4,18, 18.71, 19.58 and 21.58 in untreated cells, treated with 50 μg/ml VC, 100 μg/ml VC, 100 μM CDDP, 50 μg/ml VC + 100 μM CDDP and 100 μg/ml VC + 100 μM CDDP, respectively, post 2 h of treatment. Therefore, combined treatment of the VC and CDDP increases the apoptosis in dose-dependent manner. Cell cycle analysis post 12 h treatment confirmed the initiation of synergistic action of CDDP and VC.
Oxidative stress (OS) results from an imbalance between the generation of reactive oxygen species (O·2− and H2O2) and ability of the biological system to repair oxidative damage or to neutralize the free radicals and peroxides (Rahman et al. 2012). VC has been known to induce the oxidation of GSH to GSSG leading to hydrogen peroxide accumulation in concentration-dependent manner culminating into apoptosis (Park et al. 2004). The VC is preferentially taken up by the cancer cell, thereby modulating the redox-active compounds by reducing them into quinines leading to a disturbed redox cycle impairing the oxidant–antioxidant balance unbearable by malignant cells that are already facing high constitutive oxidative stress. It has been reported that cancer cells are more sensitive to oxidative stress than normal cells. In addition, energy crisis occurs in cancer cells due to enhanced oxidant level which strongly inhibits the glycolysis (Verrax et al. 2007) resulting in cell death of cancer cells.
Therefore, to assess the generation of H2O2 in malignant cells, CM-H2DCFDA staining was performed that is specific for hydrogen peroxide generation. CDDP enhanced the cellular H2O2 level as evident by enhanced green fluorescence in the cells. More striking extent of H2O2 induction by combination treatments with CDDP and VC was observed (Fig. 12), indicating that VC modifies the cellular redox status. These results suggested that VC in combination with CDDP strongly induces the cellular ROS, proving that VC at pharmacological concentrations works as pro-oxidant in cancer cell (Kim et al. 2012a).
The pro-oxidant function of VC has been verified by our studies. But there are other mechanisms that remain to be clarified. They include degradation of hypoxia-inducible factor 1 alpha (HIF-1 alpha) and maintenance of the extracellular matrix (Mikirova et al. 2008; Verrax and Buc Calderon 2008; Du et al. 2012). Although the underlying mechanisms triggered by VC remain to be clarified, numerous biochemical changes occur due to oxidative stress. Therefore, it was necessary to evaluate the antioxidant enzyme assay (GST, GSH, TPA, catalase) in the SiHa cells as it would provide us with the alterations occurring in biochemical mechanisms post-treatment with CDDP per se, VC per se and their combination on SiHa cells.
GSTs are enzymes that aid in catalyzing the conjugation of electrophilic substitution to GSH, which protects cells by regenerating S-thiolated proteins and removing reactive oxygen species (van Bladeren 2000). To minimize the deleterious effects of oxidative stress in the organelle, mitochondria possess antioxidants that are present on both sides of membrane. They include GSH, SOD and GPx (Cadenas and Davies 2000).
The values of all biochemical assays are presented in Table 1. From the results, it was concluded that post CDDP + VC treatment, the levels of antioxidants were reduced. As per reports, decrease in antioxidant enzyme activities has been associated with enhanced generation of reactive oxygen species resulting in protein, lipid and DNA damage leading to disruption of cellular processes (Udensi and Tchounwou 2014). These findings were in unison with our experimental results, as decreased GSH levels were reported in all the experimental groups. This decrease could be due to the increasing levels of lipid oxidation products that may be associated with reduced availability of NADPH required for the GR activity to convert GSSG to GSH (Pias and AW 2002). GSH depletion and reduced GSH/GSSG ratio were marked as indicators of oxidative stress in different types of cancer (Zitka et al. 2012).
Moreover, biotoxicity of CDDP and VC was assessed on SiHa cells by evaluating the level of RNS. From our studies, we have observed high RNS level (Table 1) post CDDP and VC treatment when compared to control that further depicts constitutive oxidative stress in cancer cells.
In addition, we have examined that VC cytotoxicity is partially due to the upregulation of p53 gene as reactivation of p53 in cancer cells enhances chemotherapeutic potential of VC by enhancing ROS generation via transcriptional network of p53 (Kim et al. 2012b). Our study was in line with the published evidences. In 2001, Reddy and colleagues showed that VC stabilizes p53 gene involved in cancer progression. As per reports, exposure of p53-deficient cancer cells to DNA damaging agents and ionizing radiation leads to termination of apoptosis. p53 accumulation sensitizes the cells to cell cycle arrest, induced by chemotherapy agents such as cisplatin and etoposide (Reddy et al. 2001). Susceptibility of cancer cells to undergo apoptosis increases due to increased level of p53 protein. Accumulating evidences reported loss of p53 results in resistance to DNA damage, thereby failing to undergo apoptosis (Céraline et al. 1998; Attardi and Jacks 1999). Treatment of VC and CDDP resulted in apoptosis of cancer cells that could be explained by the overexpression of p53 gene.
To confirm the effect of VC on expression of p53, Western blot analysis was performed. Combined treatments of 100 µM CDDP + 100 µg VC markedly raised p53 expression when compared to untreated control (Lane 1), CDDP (Lane 2) and VC (Lane 3). Therefore, our data suggested that VC + CDDP enhanced the p53 accumulation. Similar observations were reported in B16F10 murine melanoma cells (Hahm et al. 2007). Collectively, our results confirmed that a combination of CDDP and VC makes SiHa cells more sensitive to apoptosis. These results strongly supported a new strategy for cervical cancer chemotherapy.
Besides preventing direct damage to the DNA caused by chemotherapy, VC can also maintain antioxidant levels in the body after a chemotherapy treatment (Ratnam et al. 2006). This could make VC a better choice for chemotherapy treatment than CDDP, which is currently one of the most effective chemotherapeutic agents used to treat cancerous tumors (Weijl et al. 2004). While it has many positive attributes including its ability to effectively attack cancer cells without many negative side effects, one of the CDDP’s side effects is the extent to which it decreases plasma concentrations of antioxidants in the body, a result that is almost nonexistent when VC is used (Ratnam et al. 2006).
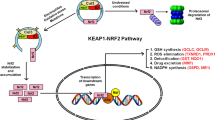
Therefore, CDDP and VC combination has provided a good therapeutic potential in inducing apoptosis in cervical cancer cells through a p53-mediated pathway (Fig. 13).
Conclusions
An ideal anticancer agent should be lethal to malignant cells but only minimally toxic to normal cells. In this regard, VC acted as a good cancer therapeutic agent. However, more basic work should be done before using it as a common anticancer drug as the information available on VC is still debatable. In addition, future studies will be focussed on determining whether VC is useful in reducing the side effects of cisplatin chemotherapy in the in vitro and in vivo systems as it is known that CDDP causes nephrotoxicity, one of the major side effects. Based on these results, oncologists could begin to prescribe VC therapy as a primary form of treatment. While the extent to which VC can affect tumors and the dosage of VC most useful to cancer treatment has yet to be precisely determined, the strong evidence of VC’s benefits, combined with its abilities to keep natural cells from harm, makes VC a valuable supplement for cancer treatment.
Abbreviations
- CDDP:
-
Cisplatin
- VC:
-
Vitamin C
- GST:
-
Glutathione S-transferase
- GSH:
-
Reduced glutathione
- TPA:
-
Total peroxidase assay
- GPx:
-
Glutathione peroxidase
- ROS:
-
Reactive oxygen species
- AO:
-
Acridine orange
- EB:
-
Ethidium bromide
References
Aebi H (1984) [13] Catalase in vitro. Methods Enzymol 105:121–126. doi:10.1016/S0076-6879(84)05016-3
Ahamad MS, Siddiqui S, Jafri A et al (2014) Induction of apoptosis and antiproliferative activity of naringenin in human epidermoid carcinoma cell through ROS generation and cell cycle arrest. PLoS ONE. doi:10.1371/journal.pone.0110003
An SH, Kang JH, Kim DH, Lee MS (2011) Vitamin C increases the apoptosis via up-regulation p53 during cisplatin treatment in human colon cancer cells. BMB Rep 44:211–216. doi:10.5483/BMBRep.2011.44.3.211
Attardi DL, Jacks T (1999) The role of p53 in tumour suppression: lessons from mouse models. Cell Mol Life Sci C 55:48–63. doi:10.1007/s000180050269
Bao J, Haldane C, Lee Y et al (2013) Effectiveness of intravenous Vitamin C in combination with conventional chemotherapy in cancer treatment : a review. J IHP-Contin Educ 1:72–80
Blancher C, Jones A (2001) SDS -PAGE and Western Blotting techniques. In: Brooks SA, Schumacher U (eds) Metastasis research protocols: volume I: analysis of cells and tissues, vol I. Humana Press, Totowa, pp 145–162
Cadenas E, Davies KJA (2000) Mitochondrial free radical generation, oxidative stress, and aging. Free Radic Biol Med 29:222–230. doi:10.1016/S0891-5849(00)00317-8
Cepeda V, Fuertes MA, Castilla J, Alonso C, Quevedo CPJ (2007) Biochemical mechanisms of cisplatin cytotoxicity. Anticancer Agents Med Chem 7:3–18
Céraline J, Deplanque G, Duclos B et al (1998) Inactivation of p53 in normal human cells increases G2/M arrest and sensitivity to DNA-damaging agents. Int J Cancer 75:432–438. doi:10.1002/(SICI)1097-0215(19980130)75:3<432:AID-IJC17>3.0.CO;2-A
Chen Q, Espey MG, Krishna MC et al (2005) Pharmacologic ascorbic acid concentrations selectively kill cancer cells: action as a pro-drug to deliver hydrogen peroxide to tissues. Proc Natl Acad Sci USA 102:13604–13609. doi:10.1073/pnas.0506390102
Chiang CD, Song EJ, Yang VC, Chao CC (1994) Ascorbic acid increases drug accumulation and reverses vincristine resistance of human non-small-cell lung-cancer cells. Biochem J 301:759–764
Collins AR, Dusinská M, Gedik CM, Stĕtina R (1996) Oxidative damage to DNA: do we have a reliable biomarker? Environ Health Perspect 104:465–469. doi:10.1289/ehp.96104s3465
Cuzick J, Arbyn M, Sankaranarayanan R et al (2008) Overview of human papillomavirus-based and other novel options for cervical cancer screening in developed and developing countries. Vaccine 26:K29–K41. doi:10.1016/j.vaccine.2008.06.019
Danesi CC, Bellagamba BC, Dihl RR et al (2010) Evaluation of the genotoxicity of cisplatin, paclitaxel and 5-fluorouracil combined treatment in the Drosophila wing-spot test. Food Chem Toxicol 48:3120–3124. doi:10.1016/j.fct.2010.08.005
Du J, Cullen JJ, Buettner GR (2012) Ascorbic acid: chemistry, biology and the treatment of cancer. Biochim Biophys Acta Rev Cancer 1826:443–457. doi:10.1016/j.bbcan.2012.06.003
Garaj-Vrhovac V, Kopjar N (2003) The alkaline Comet assay as biomarker in assessment of DNA damage in medical personnel occupationally exposed to ionizing radiation. Dans les dernières années, l’électrophorèse sur gel de cellule unique (SCGE) ou test des comètes a été largement utilisé po. Mutagenesis 18:265–271
Griess P (1879) Bemerkungen zu der abhandlung der H.H. Weselsky und Benedikt Ueber einige azoverbindungen. Chem Ber 12:426–428
Habig WH, Pabst MJJW (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249:7130–7139. doi:10.14026/j.cnki.0253-9705.2010.23.013
Hahm E, Jin D-H, Kang JS et al (2007) The molecular mechanisms of Vitamin C on cell cycle regulation in B16F10 murine melanoma. J Cell Biochem 102:1002–1010. doi:10.1002/jcb.21336
Head KA (1998) Ascorbic acid in the prevention and treatment of cancer. Altern Med Rev 3:174–186
Henson DE, Block G, Levine M (1991) Ascorbic acid: biologic functions and relation to cancer. J Natl Cancer Inst 83:547–550. doi:10.1093/jnci/83.8.547
Hernandez-Flores G, Ortiz-Lazareno PC, Lerma-Diaz JM et al (2011) Pentoxifylline sensitizes human cervical tumor cells to cisplatin-induced apoptosis by suppressing NF-kappa B and decreased cell senescence. BMC Cancer 11:483. doi:10.1186/1471-2407-11-483
Hooker DJ, Mobarok M, Anderson JL et al (2012) A new way of measuring apoptosis by absolute quantitation of inter-nucleosomally fragmented genomic DNA. Nucleic Acids Res. doi:10.1093/nar/gks334
Jurado R, Lopez-Flores A, Alvarez A, García-López P (2009) Cisplatin cytotoxicity is increased by mifepristone in cervical carcinoma: an in vitro and in vivo study. Oncol Rep 22:1237–1245
Kartalou M, Essigmann JM (2001) Mechanisms of resistance to cisplatin. Mutat Res Mol Mech Mutagen 478:23–43. doi:10.1016/S0027-5107(01)00141-5
Kim J, Lee S-D, Chang B et al (2012a) Enhanced antitumor activity of Vitamin C via p53 in cancer cells. Free Radic Biol Med 53:1607–1615. doi:10.1016/j.freeradbiomed.2012.07.079
Kim J, Lee S-D, Chang B et al (2012b) Enhanced antitumor activity of Vitamin C via p53 in cancer cells. Free Radic Biol Med 53:1607–1615. doi:10.1016/j.freeradbiomed.2012.07.079
Końca K, Lankoff A, Banasik A et al (2003) A cross-platform public domain PC image-analysis program for the comet assay. Mutat Res Toxicol Environ Mutagen 534:15–20. doi:10.1016/S1383-5718(02)00251-6
Kurbacher CM, Wagner U, Kolster B et al (1996) Ascorbic acid (Vitamin C) improves the antineoplastic activity of doxorubicin, cisplatin, and paclitaxel in human breast carcinoma cells in vitro. Cancer Lett 103:183–189. doi:10.1016/0304-3835(96)04212-7
Kwon S-B, Kim M-J, Yang JM et al (2016) Cudrania tricuspidata Stem Extract Induces Apoptosis via the Extrinsic Pathway in SiHa Cervical Cancer Cells. PLoS ONE 11:e0150235. doi:10.1371/journal.pone.0150235
Liu K, Liu P-C, Liu R, Wu X (2015) Dual AO/EB staining to setect apoptosis in osteosarcoma cells compared with flow cytometry. Med Sci Monit Basic Res 21:15–20. doi:10.12659/MSMBR.893327
Mikirova Na, Ichim TE, Riordan NH (2008) Anti-angiogenic effect of high doses of ascorbic acid. J Transl Med 6:50. doi:10.1186/1479-5876-6-50
Moron MS, Kepierre JW, Mannervick B (1979) Levels of glutathione, glutathione reductase and glutathione S-transferase activities in rat lung and liver. Biochim Biophys Acta Gen Subj 582:67–78. doi:10.1016/0304-4165(79)90289-7
Ohno S, Ohno Y, Suzuki N et al (2009) High-dose Vitamin C (ascorbic acid) therapy in the treatment of patients with advanced cancer. Anticancer Res 29:809–815
Pajaniradje S, Mohankumar K, Pamidimukkala R et al (2014) Antiproliferative and apoptotic effects of sesbania grandiflora leaves in human cancer cells. Biomed Res Int. doi:10.1155/2014/474953
Park S, Han S-S, Park CH et al (2004) L-Ascorbic acid induces apoptosis in acute myeloid leukemia cells via hydrogen peroxide-mediated mechanisms. Int J Biochem Cell Biol 36:2180–2195. doi:10.1016/j.biocel.2004.04.005
Pias EKAT, AW TY (2002) Apoptosis in mitotic competent undifferentiated cells is induced by cellular redox imbalance independent of reactive oxygen species production. FASEB J 16:781–790. doi:10.1096/fj.01-0784com
Rahman T, Hosen I, Islam MMT, Shekhar HU (2012) Oxidative stress and human health. Adv Biosci Biotechnol 03:997–1019. doi:10.4236/abb.2012.327123
Ratnam DV, Ankola DD, Bhardwaj V et al (2006) Role of antioxidants in prophylaxis and therapy: a pharmaceutical perspective. J Control Release 113:189–207. doi:10.1016/j.jconrel.2006.04.015
Reddy VG, Khanna N, Singh N (2001) Vitamin C augments chemotherapeutic response of cervical carcinoma HeLa cells by stabilizing P53. Biochem Biophys Res Commun 282:409–415. doi:10.1006/bbrc.2001.4593
Singh NP, McCoy MT, Tice RR, Schneider EL (1988) A simple technique for quantitation of low levels of DNA damage in individual cells. Exp Cell Res 175:184–191. doi:10.1016/0014-4827(88)90265-0
Udensi UK, Tchounwou PB (2014) Dual effect of oxidative stress on leukemia cancer induction and treatment. J Exp Clin Cancer Res 33:106. doi:10.1186/s13046-014-0106-5
van Bladeren PJ (2000) Glutathione conjugation as a bioactivation reaction. Chem Biol Interact 129:61–76. doi:10.1016/S0009-2797(00)00214-3
Verma AK, Sachin K, Saxena A, Bohodar HB (2005) Release kinetics from bio polymeric nanoparticles encapsulating protein synthesis inhibitor-cycloheximide, for possible therapeutic applications. Curr Pharm Biotech 6:121–130
Verrax J, Buc Calderon P (2008) The controversial place of Vitamin C in cancer treatment. Biochem Pharmacol 76:1644–1652
Verrax J, Vanbever S, Stockis J et al (2007) Role of glycolysis inhibition and poly(ADP-ribose) polymerase activation in necrotic-like cell death caused by ascorbate/menadione-induced oxidative stress in K562 human chronic myelogenous leukemic cells. Int J Cancer 120:1192–1197. doi:10.1002/ijc.22439
Waalkes MP, Liu J, Kasprzak KS, Diwan BA (2006) Hypersusceptibility to cisplatin carcinogenicity in metallothionein-I/II double knockout mice: production of hepatocellular carcinoma at clinically relevant doses. Int J Cancer 119:28–32. doi:10.1002/ijc.21245
Weijl N, Elsendoorn T, Lentjes EGW et al (2004) Supplementation with antioxidant micronutrients and chemotherapy-induced toxicity in cancer patients treated with cisplatin-based chemotherapy: a randomised, double-blind, placebo-controlled study. Eur J Cancer 40:1713–1723. doi:10.1016/j.ejca.2004.02.029
Wlodkowic D, Skommer J, Darzynkiewicz Z (2009) Flow cytometry-based apoptosis detection. Methods Mol Biol 559:1–14. doi:10.1007/978-1-60327-017-5
Wolff SP (1994) Ferrous ion oxidation in presence of ferric ion indicator xylenol orange for measurement of hydroperoxides [J]. Methods Enzymol 233:182–189
Yun J, Mullarky E, Lu C et al (2015) Vitamin C selectively kills KRAS and BRAF mutant colorectal cancer cells by targeting GAPDH. Science 350:1391–1396. doi:10.1126/science.aaa5004
Zhang JH, Xu M (2000) DNA fragmentation in apoptosis. Cell Res 10:205–211. doi:10.1038/sj.cr.7290049
Zilfou JT, Lowe SW (2009) Tumor suppressive functions of p53. Cold Spring Harb Perspect Biol 1:1–12. doi:10.1101/cshperspect.a001883
Zitka O, Skalickova S, Gumulec J et al (2012) Redox status expressed as GSH:GSSG ratio as a marker for oxidative stress in paediatric tumour patients. Oncol Lett 4:1247–1253. doi:10.3892/ol.2012.931
Acknowledgments
Ankita Leekha is thankful to Jamia Millia Islamia for providing her Non-Net fellowship.
Funding
The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript, and this is purely academic research work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Leekha, A., Gurjar, B.S., Tyagi, A. et al. Vitamin C in synergism with cisplatin induces cell death in cervical cancer cells through altered redox cycling and p53 upregulation. J Cancer Res Clin Oncol 142, 2503–2514 (2016). https://doi.org/10.1007/s00432-016-2235-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-016-2235-z