Abstract
Background
Fibroblast activation protein-α (FAP-α), which is a serine protease specially expressed on the surface of the cancer stromal cells, plays an important role in the progression and prognosis in diverse malignancies. However, the role of FAP-α in non-small cell lung cancer (NSCLC) is still unknown.
Materials and methods
We enrolled 59 NSCLC patients who received complete resection. Sections of paraffin-embedded primary NSCLC specimens of all the patients were stained with antibody directed against FAP-α. Overall, percentage (Grade 0–3) and intensity (0–3+) of stromal FAP-α staining of the tumor were assessed.
Results
FAP-α was detected in >76 % of the specimens examined, and its high expression seemed to be correlated with poor tumor differentiation (P = 0.06). Furthermore, both increased FAP-α staining percentage and intensity were associated with worse overall survival of the patients (percentage, P = 0.0087; intensity, P = 0.05). Higher FAP-α staining percentage was observed in those patients with increased peripheral neutrophil and lymphocyte count ratio (P = 0.034).
Conclusions
FAP-α is highly expressed in cancer stroma and also a predictor of poor survival of NSCLC patients. Elevated FAP-α expression may be associated with inflammation and suppressed lymphocyte-dependent immune response, which then result in the tumor progression. Therefore, FAP-α plays an important role in the progression of NSCLC, and its high expression is a predictor of poor survival. Targeting FAP-α may be a novel strategy for NSCLC therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer is the most common cause of cancer-related death in men and women (Jemal et al. 2010; Ferlay et al. 2010). Non-small cell lung cancer (NSCLC) accounts for approximately 85 % of lung cancer cases. Despite the advancement in the introduction of multiple new therapeutic lung cancer agents, the dismal 5-year survival rate remains as low as 11–16 % (Holmberg et al. 2010; Jemal et al. 2010). Given the limited benefit of conventional chemotherapy in NSCLC, the identification of novel targets is critical (Henry et al. 2007).
The tumor microenvironment is increasingly recognized to be important in the proliferation, invasion, metastasis and chemoresistance of cancer cells (Östman and Augsten 2009; Saigusa 2011; Bhowmick et al. 2004). Recent evidence indicates that cancer cells are dependent on the reactive stroma for survival and growth signals as well as the nutritional support (Saigusa 2011; Cohen et al. 2008). Among stromal cells, activated fibroblasts which are also known as cancer-associated fibroblasts (CAF) have been shown to implicate nearly all stages of oncogenesis (Saigusa 2011; Franco et al. 2010). Specifically, CAF not only contribute to epithelial cell growth and tumorigenicity but also potentially drive the progression of cancerous cells into a highly aggressive and metastatic phenotype (Brennen et al. 2012).
Fibroblast activation protein-α (FAP-α), or seprase, is a type II integral membrane serine protease of the prolyl oligopeptidase family. Normally, there is no detectable FAP-α expression in healthy adult tissues outside areas of tissue remodeling or wound healing (Levy et al. 1999). However, recent studies indicate that FAP-α is selectively and highly expressed on the surface of CAF surrounding the examined epithelial cancers which includes breast, colorectal, ovarian, pancreatic and lung cancers (Garin-Chesa et al. 1990; Scanlan et al. 1994; Rettig et al. 1993). High FAP-α expression is associated with tumor re-growth, recurrence and poor clinical outcome in rectal and pancreatic cancer (Saigusa 2011; Cohen et al. 2008). More recently, Kraman et al. (2010) reported that FAP-α expressing cells were involved in the tumor immunosuppression. We hypothesized that high FAP-α expression contributes to poor prognosis and tumor immune system suppression in NSCLC patients. In the present study, we investigated the expression of FAP-α in NSCLC patients and its association with patients survival. Furthermore, we confirmed that its expression is associated with preoperative neutrophil/lymphocyte ratio (NLR), which is a widely available index of patients systemic inflammatory and immune response (Kao et al. 2010; Tomita et al. 2011; Walsh et al. 2005; Sarraf et al. 2009).
Materials and methods
Patients
The study was conducted in Provincial Hospital Affiliated to Shandong University from 2008 to 2009. It included 59 NSCLC patients who received either a lobectomy or a pneumonectomy plus regional lymph nodes dissection. All the patients were diagnosed as NSCLC, and no metastasis was detected before surgeries. Resected specimens were assessed with immunohistochemistry (IHC) analysis. Postoperative staging of all patients was determined according to the tumor-node-metastasis (TNM) classification of the Union for International Cancer Control, ver. 7, 2009. Peripheral blood samples were obtained at hospitalization, and NLR was calculated as neutrophil count divided by lymphocyte count. Patients who underwent preoperative chemotherapy and/or radiation therapy were excluded from the present study. The study was approved by the Ethical Committee of Provincial Hospital affiliated to Shandong University.
Immunohistochemistry
Formalin-fixed, paraffin-embedded specimens were sliced into 4 μm sections. After deparaffinization and dehydration, specimens were brought to a boil in 10 mM sodium citrate buffer (PH 6.0) for antigen unmasking. Specimens were then blocked by 3 % hydrogen peroxide and incubated with rabbit polyclonal antibody against human FAP-α (ab53066, Abcam, diluted 1:200) overnight at 4 °C. Specific biotinylated-secondary anti-rabbit antibodies were then added and incubated. After incubation, slides were again washed and developed with 3,3′ diaminobenzidine substrate. All sections were counterstained with hematoxylin and were dehydrated and mounted. Negative controls were also run simultaneously.
Intensity and percent of stroma staining were evaluated independently by two pathologists. For each section of specimens, every pathologist picked 8 random fields to assess the expression levels of FAP-α then calculated an average score. In addition, they were kept blind to the clinical status of the patients. For each patient specimen, FAP-α staining was assessed by both percent of staining in stroma (Grade 0, absent or <1 %; Grade 1, 1–10 %; Grade 2, 11–50 %; Grade 3, >50 %) and intensity (0, none; +1, light; +2, moderate; +3, intense) (Henry et al. 2007).
Statistical analysis
The overall survival of the patients was defined from the time of surgery and estimated by the Kaplan–Meier method. Patient alive at the time of last follow-up was censored. Spearman’s rank correlation was used to test the relationship among FAP-α expression and peripheral neutrophil, lymphocyte count and NLR. Fisher’s exact test was applied to assess the correlations among FAP-α expression and categorical variants, including gender, age, histology, differentiation, pT (tumor progression status), pN (lymph node metastasis) and TNM stage. All tests were conducted with a 5 % type I error. To further investigate the relationship between overall survival and these prognostic factors, we apply a Cox proportional hazard model. Statistical analyses were carried out by using SAS statistical software version 9.2.
Results
Patient and tumor characteristics
For all 59 patients in the study, the median age at cancer diagnosis was 63.5 years (range: 43–75 years) and 47 patients were male (79.6 %). Table 1 lists the patient characteristics and pathological findings. Most of the tumors (69.5 %) were well or moderate differentiated. The most common histology was squamous cell carcinoma (29, 49.1 %), followed by adenocarcinoma (27, 45.7 %) and other types (3, 5.2 %). The number of patients in Stage I, II and III was 25, 21 and 13, respectively. The median follow-up for all patients was 30 months (range from 8 to 40 months).
Immunohistochemistry results
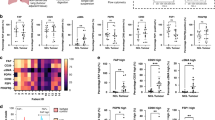
In all, we detected the expression of FAP-α in 45 of 59 (76.2 %) specimens. The percentage of FAP-α staining in stroma was scored as Grade 0 in 14 (23.7 %), Grade 1 in 12 (20.3 %), Grade 2 in 26 (44.0 %) and Grade 3 in 7 (11.9 %) (Fig 1). Staining intensity was assessed as light in 14 (23.7 %), moderate in 16 (27.1 %) and intense in 15 (25.4 %).
Relationship of FAP-α and clinicopathological variables
There was a significant positive association between staining percentage and peripheral NLR (P = 0.034). We also find FAP-α staining percentage was positively associated with peripheral neutrophil counts (P = 0.07). Then, all patients were divided into two groups (FAP-α positive group: Staining Grade 1, 2, 3 and FAP-α negative group: Staining Grade 0) based on the percent of staining. Then, we assessed the differences of gender, age, histology, differentiation, pT, pN and TNM stage between the two groups. FAP-α seemed to be negatively associated with tumor differentiation (P = 0.06). However, there was no significant correlation between FAP-α expression and clinicopathological variables, including age, gender, histology, pT, pN, TNM stage and peripheral lymphocyte counts. These results were not statistically significant, potentially due to the small sample size.
Higher expression of FAP-α was associated with poorer overall survival
As shown in Fig. 2, overall survival showed to be worse for patients with positively expressed stromal FAP-α (P = 0.027). From the output of Cox regression, we found that larger staining percentage of stromal FAP-α tends to predict poor overall survival (P = 0.0087; hazard ratio, 2.49; 95 % confidence interval (CI), 1.26–4.94). Also, higher FAP-α staining grade was associated with worse survival (P = 0.05; hazard ratio, 2.49; 95 % CI 0.29–1.02). Moreover, tumor differentiation has a significant negative association with overall survival (P = 0.0056; hazard ratio, 0.16; 95 % CI 0.04–0.59). All the above results are listed in Table 2.
Discussion
Despite the vast knowledge about cancer biology and the introduction of multiple new therapeutic NSCLC agents, the survival rate remains relatively low (Jemal et al. 2010). The clinical benefits of current therapies targeting cancer cells for NSCLC are limited. Consequently, there is an increasing importance to understand the cancer within its surrounding context (tumor microenvironment). Experimental evidences show that cancer cells communicate with surrounding stromal cells, inflammatory cells and immune cells directly or indirectly. This is pivotal to provide the appropriate microenvironment to support tumorigenesis, angiogenesis and metastasis (Bhowmick et al. 2004; Tlsty and Coussens 2006; Rasanen et al. 2009). CAF, the activated fibroblasts in stroma of cancer, have been identified to be crucial to regulate the dynamic reactions between cancer cells and numerous non-cancerous cells in the tumor microenvironment (Franco et al. 2010). A key characteristic of CAF is the expression of FAP-α (Garin-Chesa et al. 1990; O’Brien and O’Connor 2008).
In the current study, FAP-α was detected in >76 % NSCLC samples. In a small study, it was reported that FAP-α expressed fibroblasts were detected in all 13 primary lung carcinomas specimens examined (Garin-Chesa et al. 1990). Our results confirmed the high expression of FAP-α in the stroma of NSCLCs. Certain studies have suggested that FAP-α expressions are associated with aggressive disease and poorer overall prognosis in multiple cancer types (Henry et al. 2007; Cohen et al. 2008; Peng et al. 2013). However, the association between the FAP-α expression and clinicopathological variables plus overall survivals in patients with resectable NSCLC both has not been previously reported. Our results indicated that higher expression of FAP-α was related to worse overall survival in NSCLC patients. Although Ariga et al. (2001) reported that increased FAP-α in tumor stroma was associated with improved prognosis in breast cancer, some groups evaluated this relationship in other malignancies. In contrast, elevated FAP-α expression was found to correlate with decreased survival in colon cancer (Henry et al. 2007). Similar trend was also observed in multiple other malignancies including rectal (Saigusa 2011), pancreatic (Cohen et al. 2008), hepatocellular (Ju et al. 2009) and ovarian carcinomas (Zhang et al. 2007). Therefore, the role of FAP-α in tumorigenesis and progression in different types of cancers is still controversial. The mechanisms underlying this phenomenon are unknown, but it is plausible that the functions of FAP-α are related to differences in the tumor microenvironment among different tumor types.
A second observation in this study is the relationship between FAP-α expression and clinicopathological variables of the patients. Elevated FAP-α expression seemed to be associated with poor tumor differentiation (P = 0.06). It is plausible that poorly differentiated cancer cells recruited more FAP-α positive stromal cells for the cancer progression, which also indicted the differences of the tumor microenvironment among diverse differentiated NSCLC. Interesting, higher FAP-α expression is not correlated with the neutrophils or lymphocytes count alone in peripheral blood but with increased NLR. Increased NLR has been demonstrated to be an independent predictor of survival in NSCLC patients (Sarraf et al. 2009; Yao et al. 2012; Tomita et al. 2012). Compared with neutrophils count or lymphocytes count alone, NLR reflects inflammation and immune in tumor progression together. Recently, Kraman et al. (2010) showed that depletion of FAP-α expressing cells caused rapid hypoxic necrosis of cancer cells and permitted immunological control of tumor growth in the models of Lewis lung carcinomas and pancreatic ductal adenocarcinoma. FAP-α positive cells were a non-redundant, immune-suppressive component of the tumor microenvironment. Inflammation has been shown to play an important role in the progression of NSCLC, and the host’s immune response to the tumor is mainly lymphocyte dependent (Al-Shibli et al. 2008; O’Callaghan et al. 2010). Taken together, our results suggested that increased expression of FAP-α may be associated with inflammation and suppressed lymphocyte-dependent immune response, which then results in the progression and worse survival of NSCLC patients. Therefore, the mechanism of FAP-α positive stromal cells which affect host inflammation and immunity deserves further research. Moreover, one shortcoming of the study is the small sample size, so it would be necessary to enroll more patients for further research in the future.
In conclusion, for the first time, we explored the expression of FAP-α and showed its association with poor overall survival in NSCLC patients. Higher FAP-α staining percentage was correlated with increased NLR, which is an index of host inflammation and lymphocyte immunity. FAP-α may result in the progression and poor prognosis of lung cancer by affecting the host inflammation and lymphocyte-dependent immunity. Targeting FAP-α can be a possible novel strategy for NSCLC therapy.
References
Al-Shibli KI, Donnem T, Al-Saad S, Persson M, Bremnes RM, Busund LT (2008) Prognostic effect of epithelial and stromal lymphocyte infiltration in non-small cell lung cancer. Clin Cancer Res 14(16):5220–5227. doi:10.1158/1078-0432.ccr-08-0133
Ariga N, Sato E, Ohuchi N, Nagura H, Ohtani H (2001) Stromal expression of fibroblast activation protein/seprase, a cell membrane serine proteinase and gelatinase, is associated with longer survival in patients with invasive ductal carcinoma of breast. Int J Cancer 95(1):67–72
Bhowmick NA, Neilson EG, Moses HL (2004) Stromal fibroblasts in cancer initiation and progression. Nature 432(7015):332–337. doi:10.1038/nature03096
Brennen WN, Isaacs JT, Denmeade SR (2012) Rationale behind targeting fibroblast activation protein-expressing carcinoma-associated fibroblasts as a novel chemotherapeutic strategy. Mol Cancer Ther 11(2):257–266. doi:10.1158/1535-7163.mct-11-0340
Cohen SJ, Alpaugh RK, Palazzo I, Meropol NJ, Rogatko A, Xu Z, Hoffman JP, Weiner LM, Cheng JD (2008) Fibroblast activation protein and its relationship to clinical outcome in pancreatic adenocarcinoma. Pancreas 37(2):154–158. doi:10.1097/MPA.0b013e31816618ce
Ferlay J, Parkin DM, Steliarova-Foucher E (2010) Estimates of cancer incidence and mortality in Europe in 2008. Eur J Cancer 46(4):765–781. doi:10.1016/j.ejca.2009.12.014
Franco OE, Shaw AK, Strand DW, Hayward SW (2010) Cancer associated fibroblasts in cancer pathogenesis. Semin Cell Dev Biol 21(1):33–39. doi:10.1016/j.semcdb.2009.10.010
Garin-Chesa P, Old LJ, Rettig WJ (1990) Cell surface glycoprotein of reactive stromal fibroblasts as a potential antibody target in human epithelial cancers. Proc Natl Acad Sci USA 87(18):7235–7239
Henry LR, Lee HO, Lee JS, Klein-Szanto A, Watts P, Ross EA, Chen WT, Cheng JD (2007) Clinical implications of fibroblast activation protein in patients with colon cancer. Clin Cancer Res 13(6):1736–1741. doi:10.1158/1078-0432.ccr-06-1746
Holmberg L, Sandin F, Bray F, Richards M, Spicer J, Lambe M, Klint A, Peake M, Strand TE, Linklater K, Robinson D, Moller H (2010) National comparisons of lung cancer survival in England, Norway and Sweden 2001-2004: differences occur early in follow-up. Thorax 65(5):436–441. doi:10.1136/thx.2009.124222
Jemal A, Siegel R, Xu J, Ward E (2010) Cancer statistics, 2010. CA Cancer J Clin 60(5):277–300. doi:10.3322/caac.20073
Ju MJ, Qiu SJ, Fan J, Xiao YS, Gao Q, Zhou J, Li YW, Tang ZY (2009) Peritumoral activated hepatic stellate cells predict poor clinical outcome in hepatocellular carcinoma after curative resection. Am J Clin Pathol 131(4):498–510. doi:10.1309/ajcp86ppbngohnnl
Kao SC, Pavlakis N, Harvie R, Vardy JL, Boyer MJ, van Zandwijk N, Clarke SJ (2010) High blood neutrophil-to-lymphocyte ratio is an indicator of poor prognosis in malignant mesothelioma patients undergoing systemic therapy. Clin Cancer Res 16(23):5805–5813. doi:10.1158/1078-0432.ccr-10-2245
Kraman M, Bambrough PJ, Arnold JN, Roberts EW, Magiera L, Jones JO, Gopinathan A, Tuveson DA, Fearon DT (2010) Suppression of antitumor immunity by stromal cells expressing fibroblast activation protein-α. Science 330(6005):827–830. doi:10.1126/science.1195300
Levy MT, McCaughan GW, Abbott CA, Park JE, Cunningham AM, Muller E, Rettig WJ, Gorrell MD (1999) Fibroblast activation protein: a cell surface dipeptidyl peptidase and gelatinase expressed by stellate cells at the tissue remodelling interface in human cirrhosis. Hepatology 29(6):1768–1778. doi:10.1002/hep.510290631
O’Brien P, O’Connor BF (2008) Seprase: an overview of an important matrix serine protease. Biochim Biophys Acta 1784(9):1130–1145. doi:10.1016/j.bbapap.2008.01.006
O’Callaghan DS, O’Donnell D, O’Connell F, O’Byrne KJ (2010) The role of inflammation in the pathogenesis of non-small cell lung cancer. J Thorac Oncol 5(12):2024–2036
Östman A, Augsten M (2009) Cancer-associated fibroblasts and tumor growth—bystanders turning into key players. Curr Opin Genet Dev 19(1):67–73. doi:10.1016/j.gde.2009.01.003
Peng Q, Zhao L, Hou Y, Sun Y, Wang L, Luo H, Peng H, Liu M (2013) Biological characteristics and genetic heterogeneity between carcinoma-associated fibroblasts and their paired normal fibroblasts in human breast cancer. PLoS ONE 8(4):e60321. doi:10.1371/journal.pone.0060321
Rasanen K, Virtanen I, Salmenpera P, Grenman R, Vaheri A (2009) Differences in the nemosis response of normal and cancer-associated fibroblasts from patients with oral squamous cell carcinoma. PLoS ONE 4(9):e6879. doi:10.1371/journal.pone.0006879
Rettig WJ, Garin-Chesa P, Healey JH, Su SL, Ozer HL, Schwab M, Albino AP, Old LJ (1993) Regulation and heteromeric structure of the fibroblast activation protein in normal and transformed cells of mesenchymal and neuroectodermal origin. Cancer Res 53(14):3327–3335
Saigusa S, Toiyama Y, Tanaka K, Yokoe T, Okugawa Y, Fujikawa H, Matsusita K, Kawamura M, Inoue Y, Miki C, Kusunoki M (2011) Cancer-associated fibroblasts correlate with poor prognosis in rectal cancer after chemoradiotherapy. Int J Oncol 38(3):655–663. doi:10.3892/ijo.2011.906
Sarraf KM, Belcher E, Raevsky E, Nicholson AG, Goldstraw P, Lim E (2009) Neutrophil/lymphocyte ratio and its association with survival after complete resection in non-small cell lung cancer. J Thorac Cardiovasc Surg 137(2):425–428. doi:10.1016/j.jtcvs.2008.05.046
Scanlan MJ, Raj BK, Calvo B, Garin-Chesa P, Sanz-Moncasi MP, Healey JH, Old LJ, Rettig WJ (1994) Molecular cloning of fibroblast activation protein alpha, a member of the serine protease family selectively expressed in stromal fibroblasts of epithelial cancers. Proc Natl Acad Sci USA 91(12):5657–5661
Tlsty TD, Coussens LM (2006) Tumor stroma and regulation of cancer development. Annu Rev Pathol 1:119–150. doi:10.1146/annurev.pathol.1.110304.100224
Tomita M, Shimizu T, Ayabe T, Yonei A, Onitsuka T (2011) Preoperative neutrophil to lymphocyte ratio as a prognostic predictor after curative resection for non-small cell lung cancer. Anticancer Res 31(9):2995–2998
Tomita M, Shimizu T, Ayabe T, Onitsuka T (2012) Elevated preoperative inflammatory markers based on neutrophil-to-lymphocyte ratio and C-reactive protein predict poor survival in resected non-small cell lung cancer. Anticancer Res 32(8):3535–3538
Walsh SR, Cook EJ, Goulder F, Justin TA, Keeling NJ (2005) Neutrophil-lymphocyte ratio as a prognostic factor in colorectal cancer. J Surg Oncol 91(3):181–184. doi:10.1002/jso.20329
Yao Y, Yuan D, Liu H, Gu X, Song Y (2012) Pretreatment neutrophil to lymphocyte ratio is associated with response to therapy and prognosis of advanced non-small cell lung cancer patients treated with first-line platinum-based chemotherapy. Cancer Immunol Immunother. doi:10.1007/s00262-012-1347-9
Zhang MZ, Qiao YH, Nesland JM, Trope C, Kennedy A, Chen WT, Suo ZH (2007) Expression of seprase in effusions from patients with epithelial ovarian carcinoma. Chin Med J (Engl) 120(8):663–668
Acknowledgments
The work was supported by Provincial Science and Technology Development Planning of Shandong (2011GGH21819) and Provincial Science and Technology Development Planning of Shandong (2012G0021836).
Conflict of interest
The authors have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Additional information
Yida Liao and Yang Ni contributed equally to this work.
Rights and permissions
About this article
Cite this article
Liao, Y., Ni, Y., He, R. et al. Clinical implications of fibroblast activation protein-α in non-small cell lung cancer after curative resection: a new predictor for prognosis. J Cancer Res Clin Oncol 139, 1523–1528 (2013). https://doi.org/10.1007/s00432-013-1471-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-013-1471-8