Abstract
Purpose
Androgen-independent prostate cancer (AI-PC) is characterized by a higher invasive potential compared to hormone-responsive prostate cancer. A therapeutic option for AI-PC should thus be targeted to suppress not only cell proliferation, but also the invasive ability of the cells. Here, we investigated the effect of the epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor gefitinib (‘IRESSA’, ZD1839) on EGF-stimulated invasion and proliferation in two androgen-independent prostate cancer cell lines PC3 and DU145. In addition, we determined the effect of the compound on EGF-stimulated PI3 K/AKT pathway activation, in view of the key role exerted by this pathway in carcinoma cell invasion.
Methods
Cell proliferation was determined by thymidine incorporation in the nuclei. Cell cycle analysis was performed by flow cytometry. Invasion through matrigel in vitro was measured by using Boyden chambers. PI3 K activity was measured by immunokinase assay and AKT phosphorylation was evaluated by Western blot analysis.
Results
Gefitinib inhibits invasion through matrigel and collagen in response to EGF in both cell lines. In addition, we confirm the inhibitory effect of the compound on basal and EGF-induced cell proliferation. Such an effect was accompanied by accumulation of the cells in the G0/G1 phase of the cell cycle. The effect of the compound is due, as expected, to suppression of EGF-induced autotransphosphorylation of EGFR. In addition, we demonstrate here that gefitinib inhibits EGF-induced activation of PI3 K/AKT pathway in both cell lines.
Conclusion
Overall, our results demonstrate that gefitinib is able to suppress invasion and proliferation of AI-PC cells by suppressing EGF-stimulated activation of the PI3 K/AKT pathway and support a possible use of the drug in the treatment of advanced PC to limit not only proliferation but also invasion to other districts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prostate cancer (PC) is the most common malignancy detected in men in western countries (Grönberg 2003). Early PC can be treated and cured either by radical prostatectomy or radiotherapy, whereas advanced metastatic PC can be treated only by pharmacological castration (endocrine therapy) often coupled to the peripheral blockage of androgen action. Although endocrine therapy leads to substantial periods of remission, once the tumor progresses from androgen dependence to independence, therapeutic alternatives are not available. Androgen-independent PC cells are indeed insensitive to endocrine treatment and continue to grow and invade.
One of the striking characteristics of androgen-independent PC is represented by its higher invasive potential (Bonaccorsi et al. 2000; Cinar et al. 2001), which, at least in part, can be explained by loss of androgen control of genes involved in limiting invasion (Baldi et al. 2003). In this situation, a therapeutic option for treatment of advanced PC should be targeted, in addition to proliferation, at the invasive ability of the cells.
Epidermal Growth Factor (EGF) and its receptor (EGFR) play an important role in the pathogenesis of different tumors, representing a promising therapeutic target (Normanno et al. 2003). In PC, both EGF and EGFR are up-regulated (Russell et al. 1998; Di Lorenzo et al. 2002). In particular, a change from paracrine to autocrine EGFR regulation has been shown in androgen-independent PC, suggesting increased EGF production by the tumors in advanced stages (Scher et al. 1995). Similarly, the percentage of prostate tumors expressing EGFR has been reported to increase during PC progression with a maximum (100% expression) in tumors from patients with androgen-refractory PC and metastasis (Di Lorenzo et al. 2002). Of interest, EGFR has a significant prognostic impact in PC patients, since its expression in the tumors is highly predictive of disease recurrence (Di Lorenzo et al. 2002). Inhibition of EGFR with monoclonal antibodies or with tyrosine kinase inhibitors inhibits growth both in androgen-dependent and independent PC (Mimeault et al. 2003).
Besides proliferation, EGFR plays a key role in invasion of cancer cells (Wells et al. 2002) participating, in association with integrins, in the formation of the structures (lamellipodia) that mediate migration through the basal membrane (Rabinovitz et al. 1999).
Recently, a new EGFR inhibitor, gefitinib, has been developed and entered clinical trials in cancer patients (Albanell et al. 2002; Blackledge et al. 2000). Gefitinib inhibits EGFR-associated tyrosine kinase and shows marked antiproliferative activity towards both androgen-dependent and -independent in vivo (Sirotnak et al. 2002) and in vitro (Vicentini et al. 2003) models of PC, thus representing a possible therapeutic alternative for the treatment of PC.
In this paper we investigated the effect of gefitinib on EGF-stimulated invasion in two androgen-refractory PC cell lines, namely PC3 and DU145. These two cell lines are characterized by high levels of expression of EGFR (Hofer et al. 1999; Peng et al. 1996), representing a valuable tool to investigate EGFR-mediated signaling as well as testing the effect of EGFR inhibitors. In view of the critical regulatory role of PI3 K/Akt pathway on cell survival/death decision (Cantley 2002) and invasion ability (Sotsios and Ward 2000) of carcinoma cells, we also evaluated the effect of gefitinib on this signal transduction pathway after stimulation with EGF. We observed that gefitinib markedly inhibits tyrosine autophosphorylation of EGFR, invasion, and proliferation in both cell lines. In addition, we show that gefitinib suppresses EGF-induced PI3 K/Akt activation in these cells.
Materials and methods
Antibodies and chemicals
Matrigel was obtained from Collaborative Biomedical Products (Bedford, Mass., USA). Mouse mAb Ab2 (anti EGFR) and mouse mAb Ab1 (anti EGFR) were from Oncogene (Cambridge, England, UK). Antiphosphotyrosine PY20 antibody was obtained from ICN (Costa Mesa, Calif., USA), antiphosphotyrosine PY99 antibody was purchased from Santa Cruz (Santa Cruz, Calif., USA). Antiphosphatidylinositol 3-kinase p85 (N-SH3) mouse monoclonal antibody was from Upstate Biotechnology (Lake Placid, N.Y., USA), antiphosphatidylinositol 3-kinase p110β (D-4) mouse monoclonal antibody from Santa Cruz Biotechnology, (Santa Cruz). Phospho-PKB/Akt (Ser473) rabbit polyclonal antibody from Cell Signalling Technology (Beverly, Mass., USA). AntiPKB/Akt rabbit polyclonal antibody from Cell Signalling Technology (Beverly). Recombinant human epidermal growth factor (EGF) was obtained from Pepro Tech EC (London, England, UK). The tyrosine kinase inhibitor gefitinib (‘IRESSA’, ZD1839) was a generous gift from AstraZeneca (London, England, UK). The antibiotic geneticin (G418), PD 098059 [2-(2’-amino-3’-methoxyphenyl)-oxanaphthalen-4-one], and LY294002 were obtained from Calbiochem (California, USA). Phosphoinositids, type IV collagen and other non-specified reagents were from SIGMA Chemical (St. Louis, Mo., USA).
Cell culture
Cell lines (DU145 and PC3) were obtained from American Tissue Culture Collection (Bethesda, Md., USA) and maintained respectively in DMEM and HAM-F12 Coon supplemented with 10% FBS, penicillin (100 UI/ml), streptomycin (10 mg/ml), and glutamine (2 mM) (growth medium) (SIGMA). PC3-AR and PC3-Neo cells were developed in our laboratory after transfection, respectively, with an androgen receptor expression vector or an empty vector and cultured as described previously (Bonaccorsi et al. 2000). Before any stimulation, cells were kept in serum-free medium for 1 night.
Immunoprecipitation and Western blot analysis
Protein extraction and immunoprecipitation were performed as previously described (Bonaccorsi et al.1997). Briefly, cells were scraped in PBS supplemented with 1 mM Na3VO4, centrifuged, and resuspended in lysis buffer (20 mM Tris, pH 7.4, 150 mM NaCl, 0.25% NP-40, 1 mM Na3VO4, 1 mM PMSF). After protein measurement, aliquots of cell lysates containing equal amount of proteins (500 μg) were incubated for 1 h with 30 μl of Protein A (or Protein G)-Sepharose for preclearing. Precleared lysates were then incubated for 1 h using 5 μg of specific antibodies on ice followed by overnight incubation at 4 °C with 30 μl of Protein A (or Protein G)-Sepharose. The immunobeads were washed three times in lysis buffer and then resuspended in 10 μl of 2× reducing sample buffer, boiled, and loaded onto 8% polyacrylamide-bisacrylamide gels. Proteins were transferred to nitrocellulose membrane and incubated with the specific primary antibodies for 2 h, washed, and incubated with peroxidase-conjugated relative secondary antibodies (1:4,000) for 2 h. After washing, the blots were incubated with enhanced chemiluminescence (BM, Roche) detection reagent and exposed to film. After the first blotting with peroxidase-conjugated secondary antibodies, nitrocellulose membranes were stripped at 50 °C for 30 min in stripping buffer (100 mM 2β-mercaptoethanol, 2% sodium dodecyl sulphate, 62.5 mM Tris-HCl pH 6.7) and re-probed with specific primary antibodies to detect different proteins.
PI3 K assay
Cells were stimulated with EGF (10 ng/ml 15 min) in the presence or absence of gefitinib, scraped in PBS supplemented with 1 mM Na3VO4, centrifuged, and extracted with lysis buffer (20 mM Tris, pH 7.4, 137 mM NaCl, 1 mM CaCl2, 1 mM MgCl2, 1% NP-40, 1 mM Na3VO4, 1 mM PMSF). PI3 K was determined as described (Luconi et al. 2004). Briefly, after measurement of proteins, the aliquots of cell extracts containing equivalent amount of proteins (500 μg) were incubated for 1 h with 50 μl of Protein G-Sepharose for preclearing. Precleared lysates were then incubated with an anti-phosphotyrosine mAb (PY99, Santa Cruz, Calif., USA) overnight at 4 °C with 50 μl of Protein G-Sepharose as described above. The Sepharose beads were washed twice with lysis buffer and twice with a 10 mM Tris-HCl (pH 7.4) containing 0.1 mM EGTA and 5 mM LiCl. After removal of the last wash, the beads were suspended in kinase buffer (10 mM Tris-HCl, 150 mM NaCl, 5 mM EDTA) containing 20 μg of L-α-phosphatidylinositol (Sigma) 25 mM MgCl2 and 10 μCi of [γ32P]ATP ICN (Costa Mesa, Calif., USA), and incubated for 20 min at room temperature. The reaction was stopped by the addition of 60 μl of 6 M HCl and 160 μl of a mixture of chloroform and methanol (1:1). Lipids were then resolved by thin layer chromatography plates (TLC silica gel 60) (Merck) in chloroform, methanol, water, and ammonium hydroxide (60:47:11,3:2). Dried TLC sheets were developed by autoradiography. Quantifications of the bands were performed using a Kodak image analysis system.
Invasion assay
Invasion assays were performed as described previously (Bonaccorsi et al. 2000) according to Albini et al. (Albini et al. 1987) using the Boyden chambers equipped with 8-μm porosity polyvinylpyrrolidone-free polycarbonate filters. A thin layer of matrigel solution (50 μg/ml) was overlaid on the upper surface of the filter and allowed to gel by incubating the filters at 37 °C for 30 min. In some experiments type IV collagen (25 ug/ml in 10 mm acetic acid) was used instead of matrigel. Cell ability to invade the substrate was assessed by using epidermal growth factor (EGF). EGF (100 ng/ml in DMEM) was added to the bottom well of the Boyden chambers together with the inhibitor. We then added 105 cells to the top of the chambers and incubated for 24 h at 37 °C. Migrated cells were quantitated by counting cells with a Zeiss microscope (Oberkochen, Germany) equipped with brightfield optics (40× magnification). Results are expressed as the number of migrated cells per high-power field.
Mitogenic assays
[3H]thymidine (New England Nuclear, USA) incorporation was evaluated as described previously (Bonaccorsi et al. 1997; Bonaccorsi et al. 2000). Briefly, cells were plated in 24-well plates in complete culture medium. After 2 days of culture, cells were kept in serum-free medium for 24 h before treatments. Cells were then treated with stimuli or vehicles in serum-free medium at the indicated concentrations for the indicated times. All treatments were performed in triplicate. Cells were then incubated with [3H]-thymidine (1μCi/well) during the last 4 h of stimulation. Cells were then washed with TCA (5%) and solubilized with NaOH (0.25 N) in SDS (0.1%). Aliquots were transferred to plastic vials and counted by liquid scintillation. Since the effects of the different treatments were tested in cells maintained in serum-free medium for up to 72 h, the number of cells after such long serum deprivation conditions was evaluated. Cells were seeded at the density of 60,000/well and their number counted at the end of the period. We found 219,000±5,567 cells/well for DU145 and 96,500±1,454 for PC3 (mean±SEM, n=3 experiments).
Tunel assay
DNA fragmentation was assessed by Terminal deoxynucleotidyl transferase-mediated fluorescein-dUTP nick End Labeling (TUNEL) as described elsewhere (Muratori et al. 2000). Briefly, cells (2×106) were centrifuged at ×500 g (10 min) and fixed in paraformaldehyde (200 μl, 4% in PBS, pH 7.4) for 30 min, at room temperature. After two washes with 200 μl of PBS with 1% BSA, cells were permeabilized with 0.1% Triton X 100 in 0.1% sodium citrate (100 μl, for 2 min in ice). After washing twice, the labeling reaction was performed by incubating cells in 50 μl of labeling solution (supplied by “In Situ Cell Death Detection Kit, fluorescein”, Roche Molecular Biochemicals, Milan, Italy) containing the terminal deoxynucleotidyl transferase (TdT) enzyme for 1 h at 37 °C in the dark. For each experimental set, a negative control was prepared by omitting the TdT from the reaction mixture. After labeling, two subsequent washes were performed and sperm were resuspended in PBS for flow cytometry analysis. Positive controls were prepared as described before but with an additional treatment with DNAse I (Pharmacia Biotech Italia, Milan, Italy) 2 IU for 20 min at 37 °C, before the labeling reaction.
Green fluorescence was detected at 515–555 nm using a FL-1 detector of a FACScan flow cytometer (Becton Dickinson, Mountain View, Calif., USA) equipped with a 15-mW argon-ion laser for excitation. For each sample, 10,000 events were recorded at a flow rate of 200–300 cells/s. Debris were gated out by establishing a region around the population of interest, in the Forward Scatter/Side Scatter (FSC/SSC) dot plot.
Cell cycle analysis
Cell cycle studies were performed as previously described (Maggi et al. 1994; Muratori et al. 1997). Briefly, cells were cultured in 100 mm tissue culture plates in complete culture medium for 12 h. After culturing overnight in serum-free medium, cells were washed with PBS and incubated in presence or in absence of gefitinib (1 μM) for 24 h. Cells were then washed twice with cold PBS without calcium and magnesium, and 1 ml fluorochrome solution (propidium iodide, 0.05 mg/ml, dissolved in 0.1% sodium citrate and 0.1% Triton X-100) was added. Each experimental point was determined in triplicate. Dishes were kept for 60 min in the dark at 4 °C and cells were then detached by scraping and transferred to test tubes for cytofluorimetric analysis. Cell fluorescence was measured in a FACScan cytometer (Becton Dickinson). The LYSYS II software was used to determine the distribution of cells in the various cell cycle stages as G0 /G1, S, and G2.
Statistical analysis
All the data are shown as mean±SEM of the indicated number of experiments. Statistical analysis was performed with ANOVA and Student’s t-test for unpaired and, when applicable, for paired data. The IC50 was calculated with the programme ALLFIT.
Results
Gefitinib inhibits EGFR autotransphosphorylation
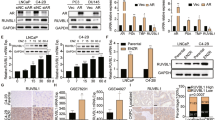
Figure 1 illustrates the effect of gefitinib (ZD, 1 μΜ) on EGF-induced tyrosine phosphorylation of EGFR in PC3 (parts A and B) and DU145 (parts C and D) cells. In both cases, cells were stimulated with EGF (10 ng/ml) for 10 min in the presence or absence of gefitinib or LY294002 as control. The experiment was performed in total lysates (parts A and C) and following immunoprecipitation of EGFR (parts B and D). As shown in Fig. 1, EGF-induced tyrosine phosphorylation of a band of 180 kDa corresponding to EGFR, is totally blunted by the inhibitor in both cell lines. On the other hand, the PI3 K inhibitor LY294002 (LY, 10 μM) does not affect basal levels and slightly increases EGF-stimulated tyrosine phosphorylation of EGFR (Fig. 1), in both cell lines. In agreement with our results, Zi et al. (Zi et al. 2000) reported that inhibition of PI3 K by using inositol hexaphosphate leads to increased EGFR phosphorylation in response to TGFα in DU145 cells. The authors hypothesize that such an effect is due to an impairment of endocytosis of the receptor at the cell surface leading to increased activation. Indeed, inositol hexaphosphate inhibits the binding of EGFR to AP2, thus blocking receptor internalization.
Effect of gefitinib (ZD, 1 μM) and LY294002 (LY, 10 μM) on EGF (10 ng/ml)-induced tyrosine phosphorylation of EGFR. SDS-PAGE of total protein lysates of A PC3 and C DU145 cell lines were performed. After protein transfer, the membranes were blotted first with the anti-phosphotyrosine antibody PY20 and then, after stripping, with an anti-EGFR antibody. To confirm that the 180 kDa band phosphorylated in tyrosine in response to EGF corresponds to EGFR, proteins from both cell lines were immunoprecipitated with an anti-EGFR antibody and revealed using PY20 antibody (for B PC3 and D DU145 cell lines). C basal conditions. Representative of three similar experiments
Gefitinib inhibits PC3 and DU145 cell proliferation by promoting G1 cell cycle arrest
We next evaluated the effects of gefitinib on cell proliferation. Table 1 presents the effect of gefitinib at 12 h, 24 h, and 36 h compared to basal thymidine incorporation in DU145. The inhibitory effect of the compound was observed at all time points (Table 1) although it was greater at 24 h and 36 h compared to 12. According to this result, subsequent experiments were performed at 24 h. As shown in Fig. 2A, the compound is able to inhibit basal and EGF (10 ng/ml)-stimulated thymidine incorporation in the two cell lines in a dose-dependent manner with an IC50 of 0.9±0.2 μM for PC3 cells and of 0.8±0.1 μM for DU145. We also evaluated the effect of the PI3 K inhibitor LY294002 on basal thymidine incorporation in PC3 cells. As shown in Fig. 2A (inset), the compound is able to inhibit PC3 cell proliferation in a dose-response manner. We also tested the effect of the compound on basal and EGF-stimulated thymidine incorporation in PC3-AR cells. This cell line, developed in our laboratory few years ago by transfection of PC3 cells with a full-length androgen receptor expression vector, retains androgen sensitivity and is characterized by reduced invasion ability compared to the parental and the mock-transfected PC3-Neo cell lines (Bonaccorsi et al. 2000). As shown in Fig. 2B, ZD1839 inhibited both basal and EGF-stimulated proliferation in PC3-AR cells to a similar extent as that in PC3-Neo and parental cells (Fig. 2A), confirming that the compound is effective also in androgen-sensitive PC cell lines, as already reported for LNCaP (Vicentini et al. 2003). To investigate whether the effect of ZD1839 on thymidine incorporation is due to inhibition of cell cycle progression the latter was evaluated by flow cytometry. As shown in Fig. 3A and Fig. 3B, treatment of PC3 and DU145 cells with gefitinib for 24 h induces accumulation of cells in G0/G1 phase with a decrease in the percentage of cells in S-phase respect to controls. In addition gefitinib is also able to slightly induce apoptosis as demonstrated by the increase of DNA fragmentation observed by Tunel coupled to flow cytometry analysis in both PC3 and DU145 cells (Fig. 3C).
Effect of gefitinib (ZD, 0.1–5 μM) on basal and EGF (10 ng/ml)-stimulated thymidine incorporation in A PC3 and DU145 cells and in B PC3-Neo and PC3-AR cells. Cells were treated for 24 h with the different agonists. The inset shows the effect of LY294002 (0.1–10 μM) on basal thymidine incorporation in PC3 cells. Data are means±SEM of three different experiments
Effect of gefitinib (ZD, 1 μM) on cell cycle progression in A PC3 and B DU145 cell lines. Cells were treated for 24 h with gefitinib. C shows the effect of the compound on DNA fragmentation in the two cell lines as evaluated by Tunel coupled to Flow cytometry. Representative of three different experiments
Gefitinib inhibits EGF-induced invasion of PC3 and DU145 cells
Next, we evaluated the effect of the compound on EGF-stimulated invasion through a reconstituted membrane (matrigel) in the two cell lines. The effect of the EGFR inhibitor was tested at the concentration of 1 μM, in agreement with the calculated IC50 of its antiproliferative effect. As shown in Fig. 4, EGF-stimulated invasion is totally blunted by treatment with gefitinib (ZD) in both cell lines. As control, we tested the effect of the PI3 K inhibitor LY294002 on EGF-stimulated invasion in PC3 cells. As expected, LY294002 (LY, 10 μM) suppresses EGF-stimulated invasion (Fig. 4) confirming the involvement of PI3K-mediated pathways in EGF-stimulated invasion. The effect of gefitinib on EGF-stimulated invasion was also evaluated in DU145 by using type IV collagen instead of matrigel. The results of these experiments (Fig. 4, inset) substantially confirmed the ability of the compound to inhibit EGF-stimulated invasion ability of the cells.
Effect of gefitinib (ZD, 1 μM) on EGF (50 ng/ml)-stimulated matrigel invasion of PC3 and DU145 cells. As control, the effect of LY294002 (LY, 10 μM) on EGF (50 ng/ml)-stimulated matrigel invasion of PC3 cells is shown. Data are means±SEM of mean number of three different stimulated experiments. The inset shows the effect of gefitinib (ZD, 1 μM) on EGF-stimulated invasion through type IV collagen in DU145 cells
Gefitinib inhibits EGF-stimulated activation of PI3 K pathway in prostate cancer cells
As mentioned above, PI3 K plays a key role both in the control of proliferation and in invasion and migration mechanisms of carcinoma cells (Cantley 2002), as also documented by the inhibitory effect of LY294002 on EGF-mediated proliferation (Fig. 2, inset) and invasion (Fig. 4) of PC3 cells. To investigate whether the inhibitory effects of gefitinib on invasion were due to inhibition of the PI3 K signalling cascade, we evaluated PI3 K activity in the cells by immunokinase assay (Cantley 2002). As shown in Fig. 5, gefitinib totally suppressed PI3 K activation stimulated by EGF in PC3 and DU145 cells (parts A and B).
Effect of gefitinib (ZD, 1 μM) on EGF (10 ng/ml)-stimulated PI3 K activity in PC3 and DU145 cell lines. PI3 K assay was performed on the immunoprecipitates with an anti-phosphotyrosine mAb (PY99), followed by TLC analysis of the reaction products. A shows a representative experiment and illustrates the portions of the TLC autoradiographs that correspond to the locations of PIP (phosphatidylinositolphosphate); B shows mean±SEM of data quantification of three different experiments
Next, we evaluated the effect of the compound on the downstream PI3 K effector serine/threonine kinase AKT (Cantley 2002). It is well-known that serine/threonine phosphorylation of AKT following PI3 K activation, is essential for AKT activation, and that AKT promotes invasion in carcinoma cells (Grille et al. 2003). Thus, we evaluated serine phosphorylation of AKT by Western blot analysis employing a specific anti-ser phosphorylated AKT antibody. We found that gefitinib was able to inhibit EGF-stimulated AKT serine phosphorylation in PC3 (Fig. 6A) and in DU145 cells (Fig. 6B). As expected, EGF-stimulated AKT phosphorylation was also totally blunted by the PI3 K inhibitor LY294002 (10 μM) used as control in PC3 cells (Fig. 6A).
Effect of gefitinib (ZD, 1 μM) on EGF (E, 10 ng/ml)-stimulated phosphorylation of AKT/PKB in A PC3 and B DU145 cells as determined by Western blot analysis of total protein lysates. After protein transfer, the membranes were blotted first with the anti-phosphoserine AKT antibody (P ser-AKT) and then, after stripping, with an anti-AKT antibody. In PC3 cells the effect of LY294002 (LY, 10 μM) was also evaluated. Representative of three similar experiments. C PTEN expression in PC3 and DU145 cells determined by Western blot analysis of total lysates. C control conditions
AKT activation is downregulated by PTEN, a lipid phosphatase that catalyzes the dephosphorylation of PIP3 (Cantley 2002). PTEN is considered a tumor suppressor and its expression is often lost or reduced in cancer cells, including PC-3 cells (Huang et al. 2001) but not DU145 (Huang et al. 2001; Bastola et al. 2002). In agreement with these results, we found that PTEN expression is reduced in PC3 cells compared to DU145 cells (Fig. 6C).
Discussion
Blockade of EGF-mediated signalling pathways represents a promising new strategy for anticancer therapy. Indeed, EGF and its receptors are negative prognostic factors in several different tumors including PC, where they have been found to be elevated in advanced and metastatic tumors (Russell et al. 1998; Di Lorenzo et al. 2002). In androgen-independent PC (AI-PC) in particular, where endocrine therapy is no longer possible and other therapies are not available, blockade of EGFR with a specific inhibitor may be particularly useful, since it may be valuable both for suppressing proliferation and invasion of PC cells. Our results clearly demonstrate that the EGFR tyrosine kinase inhibitor gefitinib, which is an orally active compound with anti-tumor activity in a wide range of tumors (Albanell et al. 2002; Blackledge et al. 2000), is able to inhibit EGF-stimulated invasion and proliferation in vitro in two different AI-PC cell lines. The compound effectively suppresses EGF-mediated EGFR autotransphosphorylation in both cell lines and inhibits the EGF-stimulated downstream signalling pathway PI3 K, as demonstrated both by suppression of PI3 K activation and of phosphorylation of the PI3 K effector AKT. Blockade of EGF-mediated PI3 K signaling appears to be fundamental both for the antiproliferative and the anti-invasive effect of gefitinib, as already reported for other cell lines (Rodrigues et al. 2003). Indeed, it is well-known that PI3 K/AKT activation regulates both proliferation and invasion/migration of carcinoma cells (Cantley 2002; Grille et al. 2003). The finding that anti-proliferative and anti-invasive effects similar to those obtained with gefitinib were obtained with the PI3 K inhibitor LY294002, further indicate that suppression of EGF-induced PI3 K/AKT activation is responsible for these inhibitory effects.
Interestingly, the inhibitory effect of gefitinib on proliferation, invasion, and EGF-induced PI3 K activation/AKT phosphorylation was observed both in the PTEN-mutated PC3 cell line (Huang et al. 2001) and in the DU145 cell line, which shows normal values and activity of PTEN (Huang et al. 2001; Bastola et al. 2002), as also confirmed in the present paper (Fig. 6C). These results are in agreement with recent results obtained, in both cell lines, by another group (Vicentini et al. 2003). PTEN, a tumor suppressor involved in de-phosphorylation of its downstream substrate AKT (Cantley 2002), is often found inactivated by somatic mutations in a wide range of tumors including PC (Mareel and Leroy 2003). PTEN mutations have been associated with insensitivity to antitumoral therapies because of constitutive AKT activation (Chen et al. 2001), and recent results show that PTEN-mutated MDA-468 cells are relatively resistant to the antiproliferative effect of gefitinib compared to A431 (which express normal PTEN levels) despite suppression of EGFR autotransphosphorylation in both cell lines with low concentrations of the inhibitor (Bianco et al. 2003). Our results suggest that, at least in vitro, the effect of gefitinib can be obtained both in PTEN-mutated and non-mutated PC cell lines, providing a rationale for its use in vivo also in PTEN-mutated tumors. The mechanism(s) by which gefitinib is effective also in PTEN-mutated PC3 cells is not clear and has not been investigated in the present paper. We speculate that EGF and its receptor represent one of the main pathways supporting proliferation in these two cells lines and thus the inhibitor, by suppressing activation of EGFR, inhibits all the downstream pathways activated by the receptor partially overcoming the effects of constitutive AKT activation.
The effect of gefitinib is observed at relatively low concentrations. Indeed, the inhibitory effect on proliferation shows an IC50 of about 1 μM, in agreement with its inhibitory effect on proliferation of other cell lines (Vicentini et al. 2003). At the concentration of 5 μM, the growth inhibitory effect of the compound on both basal and EGF-stimulated thymidine incorporation was approaching 100%. This result is of particular interest in view of the fact that this effect was not due to toxicity of the compound, but rather to induction of cell cycle arrest in the G0/G1 phase of the cell cycle. These results are in agreement with previously published results in PC cells (Vicentini et al. 2003), where, however, the effect of gefitinib on apoptosis and cell cycle regulation was measured in the presence of EGF and not in basal conditions. On the other hand, a small apoptotic effect of the compound in unstimulated conditions has been observed also in human squamous carcinoma cell lines (Huang et al. 2002). The presence of an inhibitory effect on basal proliferation in PC3 and DU145 cell lines, supports the evidence for the presence of an EGF/TGFα autocrine loop mediating proliferation of these cells (Peng et al. 1996; Hofer et al. 1991).
In conclusion, our results demonstrate that the EGFR tyrosine kinase inhibitor gefitinib is able to suppress both invasion ability and proliferation of PC cell lines in vitro. These results suggest the use of the drug during the androgen-independent phase of PC to limit not only proliferation of the tumor but also invasion to other districts.
Abbreviations
- EGF:
-
Epidermal growth factor
- EGFR:
-
Epidermal growth factor receptor
- AI-PC:
-
Androgen-independent prostate cancer
- PI3 K:
-
Phosphatidylinositol 3-kinase
References
Albanell J, Rojo F, Averbuch S, Feyereislova A, Mascaro JM, Herbst R, LoRusso P, Rischin D, Sauleda S, Gee J, Nicholson RI, Baselga J (2002) Pharmacodynamic studies of the epidermal growth factor receptor inhibitor ZD1839 in skin from cancer patients: istopathologic and molecular consequences of receptor inhibition. J Clin Oncol 20:110–124
Albini A, Iwamoto Y, Kleinman HK, Martin GR, Aaronson S A, Kozlowski JM, McEwan RN (1987) A rapid in vitro assay for quantitating the invasive potential of tumor cells. Cancer Res 47:3239–3245
Baldi E, Bonaccorsi L, Forti G (2003) Androgen receptor: good guy or bad guy in prostate cancer invasion? Endocrinology 144:1653–1655
Bastola DR, Pahwa GS, Lin MF, Cheng PW (2002) Downregulation of PTEN/MMAC/TEP1 expression in human prostate cancer cell line DU145 by growth stimuli. Mol Cell Biochem 236:75–81
Bianco R, Shin I, Ritter CA, Yakes FM, Basso A, Rosen N, Tsurutani J, Dennis PA, Mills GB, Arteaga CL (2003) Loss of PTEN/MMAC1/TEP in EGF receptor-expressing tumor cells counteracts the antitumor action of EGFR tyrosine kinase inhibitors. Oncogene 22:2812–2822
Blackledge G, Averbuch S, Kay A, Barton J (2000) Anti-EGF receptor therapy. Prostate Cancer Prostatic Dis 3:296–302
Bonaccorsi L, Luconi M, Maggi M, Muratori M, Forti G, Serio M, Baldi E (1997) Protein tyrosine kinase, mitogen-activated protein kinase and protein kinase C are involved in the mitogenic signaling of platelet-activating factor (PAF) in HEC-1A cells. Biochim Biophys Acta 1355:155–166
Bonaccorsi L, Carloni V, Muratori M, Salvatori A, Giannini A, Carini M, Serio M, Forti G, Baldi E (2000) Androgen receptor expression in prostate carcinoma cells suppresses alpha6beta4 integrin-mediated invasive phenotype. Endocrinology 141:3172–3182
Cantley LC (2002) The phosphoinositide 3-kinase pathway. Science 296:1655–1657
Chen X, Thakkar H, Tyan F, Gim S, Robinson H, Lee C, Pandey SK, Nwokorie C, Onwudiwe N, Srivastava RK (2001) Constitutively active Akt is an important regulator of TRAIL sensitivity in prostate cancer. Oncogene 20:6073–6083
Cinar B, Koeneman KS, Edlund M, Prins GS, Zhau HE, Chung LW (2001) Androgen receptor mediates the reduced tumor growth, enhanced androgen responsiveness, and selected target gene transactivation in a human prostate cancer cell line. Cancer Res 61:7310–7317
Di Lorenzo G, Tortora G, D’Armiento FP, De Rosa G, Staibano S, Autorino R, D’Armiento M, De Laurentiis M, De Placido S, Catalano G, Bianco AR, Ciardiello F (2002) Expression of epidermal growth factor receptor correlates with disease relapse and progression to androgen-independence in human prostate cancer. Clin Cancer Res 8:3438–3444
Grille SJ, Bellicosa A, Upson J, Klein-Szanto AJ, van Roy F, Lee-Kwon W, Donowitz M, Tsichlis PN, Larue L (2003) The protein kinase Akt induces epithelial mesenchymal transition and promotes enhanced motility and invasiveness of squamous cell carcinoma lines. Cancer Res 63:2172–2178
Grönberg H (2003) Prostate cancer epidemiology. Lancet 361:859–864
Hofer DR, Sherwood ER, Bromberg WD, Mendelsohn J, Lee C, Kozlowski JM (1991) Autonomous growth of androgen-independent human prostatic carcinoma cells: role of transforming growth factor alpha. Cancer Res 51:2780–2785
Huang H, Cheville JC, Pan Y, Roche PC, Schmidt LJ, Tindall DJ (2001) PTEN induces chemosensitivity in PTEN-mutated prostate cancer cells by suppression of Bcl-2 expression. J Biol Chem 276:38830–38836
Huang S-M, Jing L, Armstrong EA, Harari PM (2002) Modulation of radiation response and tumor-induced angiogenesis after epidermal groath factor receptor inhibition by ZD1839 (Iressa). Cancer Res 62:4300–4306
Luconi M, Carloni V, Marra F, Ferruzzi P, Forti G, Baldi E (2004) Increased phosphorylation of AKAP by inhibition of phosphatidylinositol 3-kinase enhances human sperm motility through tail recruitment of protein kinase A. Journal Cell Sci 117:1235–1246
Maggi M, Bonaccorsi L, Finetti G, Carloni V, Muratori M, Laffi G, Forti G, Serio M, Baldi E (1994) Platelet-activating factor mediates an autocrine proliferative loop in the endometrial adenocarcinoma cell line HEC-1A. Cancer Res 54:4777–4784
Mareel M, Leroy A (2003) Clinical, cellular, and molecular aspects of cancer invasion. Physiol Rev 83:337–376
Mimeault M, Pommery N, Henichart JP (2003) New advances on prostate carcinogenesis and therapies: involvement of EGF-EGFR transduction system. Growth Factors 21:1–14
Muratori M, Nicoletti I, Vannelli GB, Luconi M, Macorsini E, Serio M, Forti G, Maggi M (1997) Genistein induces a G(2)/M block and apoptosis in human uterine adenocarcinoma cell lines. Endocr Relat Cancer 4:203–218
Muratori M, Piomboni P, Baldi E, Filimberti E, Pecchioli P, Moretti E, Gambera L, Baccetti B, Biagiotti R, Forti G, Maggi M (2000) Functional and ultrastructural features of DNA-fragmented human sperm. J Androl 21:903–912
Normanno N, Bianco C, De Luca A, Maiello MR, Salomon DS (2003) Target-based agents against ErbB receptors and their ligands: a novel approach to cancer treatment. Endocr Relat Cancer 10:1–21
Peng D, Fan Z, Lu Y, DeBlasio T, Scher H, Mendelsohn J (1996) Anti-epidermal growth factor receptor monoclonal antibody 225 up-regulates p27KIP1 and induces G1 arrest in prostatic cancer cell line DU145. Cancer Res 56:3666–3669
Rabinovitz I, Toker A, Mercurio AM (1999) Protein kinase C-dependent mobilization of the alpha6beta4 integrin from hemidesmosomes and its association with actin-rich cell protrusions drive the chemotactic migration of carcinoma cells. J Cell Biol 146:1147–1160
Rodrigues S, Attoub S, Nguyen QD, Bruyneel E, Rodrigue CM, Westley BR, May FE, Thim L, Mareel M, Emami S, Gespach C (2003) Selective abrogation of the proinvasive activity of the trefoil peptides pS2 and spasmolytic polypeptide by disruption of the EGF receptor signaling pathwaysin kidney and colonic cancer cells. Oncogene 22:4488–4497
Russell PJ, Bennett S, Stricker P (1998) Growth factor involvement in progression of prostate cancer. Clin Chem 44:705–723
Scher HI, Sarkis A, Reuter V, Cohen D, Netto G, Petrylak D, Lianes P, Fuks Z, Mendelsohn J, Cordon-Cardo C (1995) Changing pattern of expression of the epidermal growth factor receptor and transforming growth factor alpha in the progression of prostatic neoplasms. Clin Cancer Res 1:545–550
Sirotnak FM, She Y, Lee F, Chen J, Scher HI (2002) Studies with CWR22 xenografts in nude mice suggest that gefitinib may have a role in the treatment of both androgen-dependent and androgen-independent human prostate cancer. Clin Cancer Res 8:3870–3876
Sotsios Y, Ward SG (2000) Phosphoinositide 3-kinase: a key biochemical signal for cell migration in response to chemokines. Immunol Res 177:217–235
Vicentini C, Festuccia C, Gravina GL, Angelucci A, Marronaro A, Bologna M (2003) Prostate cancer cell proliferation is strongly reduced by the epidermal growth factor receptor tyrosine kinase inhibitor ZD1839 in vitro on human cell lines and primary cultures. J Cancer Res Clin Oncol 129:165–174
Wells A, Kassis J, Solava J, Turner T, Lauffenburger DA (2002) Growth factor-induced cell motility in tumor invasion. Acta Oncol 41:124–130
Zi X, Singh RP, Agarwal R (2000) Impairment of erbB1 receptor and fluid-phase endocytosis and associated mitogenic signaling by inositol hexaphosphate in human prostate carcinoma DU145 cells. Carcinogenesis 21:2225–2235
Acknowledgements
We thank Prof. Mario Maggi (Endocrine Unit, University of Florence) and Dr. Clara Crescioli (Endocrine Unit, University of Florence) for helpful advice. Supported by Associazione Italiana Ricerca sul Cancro (AIRC, Milan), University of Florence, Ministry of University and Scientific Research (Programmi di Ricerca Scientifica di Rilevante Interesse Nazionale, COFIN), and AstraZeneca Spa (Basiglio, Milan, Italy).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bonaccorsi, L., Marchiani, S., Muratori, M. et al. Gefitinib (‘IRESSA’, ZD1839) inhibits EGF-induced invasion in prostate cancer cells by suppressing PI3 K/AKT activation. J Cancer Res Clin Oncol 130, 604–614 (2004). https://doi.org/10.1007/s00432-004-0581-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-004-0581-8