Abstract
Purpose
We investigated the relationship between the effects of troglitazone (TGZ) on cellular growth, differentiation and apoptosis induction, and the induction of peroxisome proliferator-activated receptor (PPAR) γ in three human colon cancer cell lines, HCT-15, DLD-1and LoVo.
Methods
Viable cell number was evaluated by the Alamar blue assay and apoptotic cell death by TUNEL methods. Expression of PPARγ mRNA and protein was examined by reverse transcription-polymerase chain reaction (RT-PCR) and Western blot, respectively. The differentiation markers of colonic mucosa, villin and MUC2 mRNAs, were analyzed by real-time RT-PCR.
Results
HCT-15 and DLD-1 cells proliferated rapidly while LoVo cells grew slowly. TGZ dose-dependently inhibited the proliferation of all the cell lines, and also induced apoptotic cell death. High expression of PPARγ mRNA and protein was demonstrated in DLD-1 and LoVo cells before TGZ treatment. After the treatment, PPARγ mRNA and protein levels were increased in HCT-15 and LoVo cells. Villin and MUC2 mRNAs were increased by TGZ treatment in HCT-15 cells while villin mRNA was repressed in LoVo cells. Changes in expression of PPARγ, villin or MUC2 mRNAs were not observed in DLD-1 cells.
Conclusions
These results suggest that PPARγ levels are not correlated with the rates of cell proliferation. Differentiation induction by TGZ was only observed in the cell lines with enhanced PPARγ expression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Peroxisome proliferator-activated receptors (PPARs) are members of the nuclear hormone receptor gene superfamily, and regulate a number of genes predominantly associated with lipid metabolism through ligand-dependent transcriptional activation and repression (Willson et al. 2000). There are three different members in the PPAR family identified to date, encoded by separate genes: PPARα, PPARβ, and PPARγ (Willson et al. 2000). These isotypes exhibit distinct patterns of tissue distribution, and play fundamental roles in dietary fat storage and catabolism (Kersten et al. 2000). PPARγ is expressed at high levels in adipose tissue, and is an important regulator of adipocyte differentiation and lipid metabolism (Chawla et al. 1994; Tontonoz et al. 1994). PPARγ is also found in other cell types, such as hepatocytes, fibroblasts, and epithelial cells (Greene et al. 1995; Braissant et al. 1996). PPARγ mRNA level in the colon is near equivalent to that in adipocytes (Fajas et al. 1997), and the highest levels have been observed in post-mitotic and differentiated colonic epithelial cells (Mansén et al. 1996; Lefebvre et al. 1999).
Ligands for PPARγ include the natural prostanoid 15-deoxy-Δ12,14-prostaglandin J2, a variety of non-steroidal anti-inflammatory drugs, and the thiazolidinedione class of anti-diabetic drugs (Forman et al. 1995; Lehmann et al. 1995; Johnson et al. 1998). Troglitazone (TGZ), one of the thiazolidinediones, is used in the treatment of type 2 diabetes and is a potent and selective activator of PPARγ (Willson et al. 1996; Johnson et al. 1998). These ligands have been shown to mediate negative effects on the proliferation of malignant tumor cells, such as liposarcoma and breast cancer cells (Tontonoz et al. 1997; Mueller et al. 1998), and also to induce differentiation of adipose tissue, urothelium, and colonic epithelial cells (Guan et al. 1997; Sarraf et al. 1998; Kitamura et al. 1999; Lefebvre et al. 1999; Rosen et al. 1999), and apoptosis (Brockman et al. 1998; Mueller et al. 1998; Bishop-Bailey and Hla 1999; Yang and Frucht 2001). It was suggested that PPARγ could inhibit Bcl-2 through a NF-κB pathway (Chen et al. 2002) and activate c-myc or caspase (Miyashita et al. 1998; Keelan et al. 1999; Ohta et al. 2001; Shimada et al. 2002). On the other hand, PPARγ ligands are reported to enhance colon tumor formation in mice with mutation in APC gene (Lefebvre et al. 1998; Saez et al. 1998). However, other studies revealed that p53 or transcription factor co-activators are involved in TGZ-induced apoptosis rather than PPARγ activation (Kamei et al. 1996; Sheppard et al. 1998; Okura et al. 2000). It remains to be clarified whether the various effects of TGZ are mediated via PPARγ (Miyashita et al. 1998; Keelan et al. 1999; Ohta et al. 2001).
In the present study, we investigated the relationship between the effects of TGZ on the cellular growth, differentiation and apoptosis induction, and the induction of PPARγ in three human colon cancer cell lines. To determine whether TGZ treatment could induce differentiation of colon cancer cell lines, the expression of villin and MUC2 mRNAs was examined as markers for differentiated epithelial cells. Villin was selected as a marker for enterocyte differentiation along the crypt-villous axis (Bretscher and Weber 1979; Robine et al. 1993), while MUC2 was selected for goblet cells (Chang et al. 1994; Tytgat et al. 1994). Inhibition of cell proliferation and apoptosis induction occurred in all the cell lines, irrespective of the presence or absence of PPARγ induction. Differentiation induction was only observed in cell lines with enhanced PPARγ expression.
Materials and methods
Cell culture
Human colonic cancer cell lines originated from adenocarcinoma, DLD-1, HCT-15, and LoVo, were obtained from the Cell Resource Center for Biomedical Research Institute of Development, Aging and Cancer, Tohoku University (Sendai, Japan, http://www.idac.tohoku.ac.jp/dep/ccr/). The cultures were incubated at 37 °C in a humidified atmosphere of 5% CO2, 95% air. A growth medium consisting of RPMI-1640 (Nissui Pharmaceutical, Tokyo, Japan) was supplemented with 10% heat-inactivated fetal bovine serum (JRH Biosciences, Lenexa, Kan., USA), 100 units/ml of penicillin, 100 µg/ml of streptomycin and 0.25 µg/ml amphotericin B (Invitrogen, Carlsbad, Calif., USA).
TGZ was kindly provided by Sankyo Pharmaceutical (Tokyo, Japan). TGZ was dissolved in dimethyl sulfoxide (DMSO) and stored at −20 °C as stock solution. Just before usage, the stock solution was incorporated with 20% bovine serum albumin (BSA). DMSO and BSA were used at final concentrations of 0.025% and 0.01%, respectively.
Cell proliferation assay
To study the effect of TGZ on proliferation of colon cancer cell lines, 90 µl aliquots of cell suspension (5,000 cells/well) in 96-well flat-bottomed microplates were incubated with 0 μM, 10 μM, 20 μM, or 50 μM TGZ. The experiments were carried out using triplicate plates except for 24 plates on the fifth day. Viable cell number was estimated by Alamar blue assay and the values were expressed as intensity of fluorescence (Ahmed et al. 1994). Ten microliters of Alamar blue working solution (Asahi Techno Glass, Tokyo, Japan) was added to each well and the plate was further incubated at 37 °C for 2 h. The fluorescence intensity was measured with excitation at 544 nm and emission at 590 nm using a Fluoroskan II (Thermo Labsystems, Vantaa, Finland). The reaction was linear in the range of 40−4,000 fluorescence units, corresponding to 5,000−500,000 viable cells/well.
TUNEL assay
To study apoptosis of cultured cells, TUNEL (terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end labeling of DNA fragmentation sites) assay was performed. 5.0×105 cells/slide were incubated in the presence or absence of 50 µM TGZ on Lab-Tek II chamber slides (Nalge Nunc International, Naperville, Ill., USA) for 4−7 days. Cells on chamber slides were then washed twice with phosphate-buffered saline (PBS), air-dried, and fixed with 4% paraformaldehyde at room temperature for 30 min. The TUNEL assay was performed using In Situ Cell Death Detection Kit (Roche Diagnostics, Mannheim, Germany), according to the manufacturer’s instructions. Peroxidase was detected by incubating with diaminobenzidine substrate solution for 10 min. The slides were counter-stained with light green (Merck, Darmstadt, Germany). Cells were viewed and photographed under a light microscopy with high-power magnification. Using an eyepiece grid, with one square measuring 0.1 mm2 when placed on an ocular lens, TUNEL-positive cells were counted and the values were expressed as numbers in ten randomly chosen squares. Positive and negative controls were performed using the cells treated with 1 μg/ml DNase I and cells without terminal deoxynucleotidyl transferase treatment, respectively.
Reverse transcription-polymerase chain reaction (RT-PCR)
Total RNAs were extracted from cultured cells using an RNeasy Kit (Qiagen, Hilden, Germany). RNA levels were quantified using a spectrophotometer at a wavelength of 260 nm. Each 1-µg RNA sample was converted to first strand cDNA by reverse transcription using a SuperScript Preamplification System (Invitrogen) with oligo (dT) priming methods in a volume of 20 µl. The resulting cDNA was stored at −20 °C.
PCR was performed with AmpliTaq Gold DNA polymerase (Applied Biosystems, Foster City, Calif., USA) using a GeneAmp PCR system 9600 (Applied Biosystems). According to the sequence of PPARγ cDNA (Kitamura et al. 1999), a combination of a forward primer, 5’-GAGATCACAGAGTATGCCAA-3’, and a reverse primer, 5’-CTGTCATCTAATTCCAGTGC-3’, were used for detection of PPARγ cDNA. A combination of a forward primer, 5’-CCATCACCATCTTCCAGGAG-3’, and a reverse primer, 5’-GCATGGACTGTGGTCATGAG-3’, were used for glyceraldehyde 3-phosphate dehydrogenase (GAPDH) cDNA as an internal control. Amplification conditions were as follows: initial denaturation at 95 °C for 10 min, and 35 cycles of denaturation at 95 °C for 30 s and annealing/extension at 60 °C for 1 min. After the completion of 35 cycles, the reaction mixtures were incubated at 60 °C for 10 min. The PCR products were subjected to electrophoresis on 2% agarose gels, and stained with ethidium bromide.
Quantitative RT-PCR
RNA extraction and cDNA synthesis were performed as described above. PPARγ, villin, and MUC2 mRNA levels were quantified by real-time RT-PCR using ABI PRISM 7000 (Applied Biosystems). All primers and probes were designed using sequence data from DDBJ sequences (DNA Database of Japan, http://www.ddbj.nig.ac.jp/) and the probe/primer design software (Primer Express, version 2.0, Applied Biosystems). The fluorogenic oligonucleotide probes (TaqMan probes, Applied Biosystems), forward and reverse primers were as follows: 6FAM-5’-CTGTTTGCCAAGCTGCTCCAGAAAATG-3’-TAMRA, 5’-TGAAGCTGAACCACCCTGAGT-3’, and 5’-GACCGTGTTCCGTGACAATC-3’ for PPARγ; 6FAM-5’-AGTCGGCCGTCTTTCAGCAGCTCTTC-3’-TAMRA, 5’-ACACAGGTGGAGGTGCAGAAT-3’, and 5’-GGTTGGACGCTGTCCACTTC-3’ for villin; 6FAM-5’-CAGCCAGAAGCCCGTTACCCACTG-3’-TAMRA, 5’-TGGGTGTCCTCGTCTCCTACA-3’, and 5’-TGTTGCCAAACCGGTGGTA-3’ for MUC2, respectively. We used the human GAPDH primers and probe set (Applied Biosystems) for internal calibration. PCR conditions were as follows: 1 μl cDNA solution synthesized from 200 ng RNA was added to 49 μl reaction mixture containing 25 μl 2× TaqMan Universal PCR Master Mix (Applied Biosystems), 0.4 μM each primer, 0.2 μM TaqMan probe. The thermal cycler conditions comprised an initial step of incubation at 50 °C for 2 min and at 95 °C for 10 min, and then 50 cycles of denaturation at 95 °C for 15 s and annealing/extension at 60 °C for 1 min.
Western blot analysis
Cells grown to subconfluence in 100-mm dishes were lysed in lysis buffer containing 20 mM Tris-HCl, pH 7.4, 150 mM NaCl, 2 mM EDTA, 1% Igepal CA-630, and 1% protease inhibitor cocktail (Sigma, St Louis, Mo., USA). This cell extract was electrophoresed in NuPAGE 4–12% Bis-Tris Gels (Invitrogen), and proteins were transferred to nitrocellulose membranes (Invitrogen). The membranes were blocked at room temperature for 1 h with 5% skimmed milk in PBS, and then with 0.01% goat serum in SuperBlock blocking buffer (Pierce, Rockford, Ill., USA), respectively. 0.05% Tween 20 was added in these buffers. The membranes were incubated at 4 °C overnight with rabbit polyclonal anti-human PPARγ antibody (Santa Cruz Biotechnology, Santa Cruz, Calif., USA) in SuperBlock blocking buffer, or mouse monoclonal anti-human β-actin antibody (Sigma), which was used as an internal control. After washing with PBS three times, the membranes were incubated at room temperature for 1 h with peroxidase-conjugated goat anti-rabbit IgG (Santa Cruz Biotechnology) or goat anti-mouse IgG antibodies (ICN Pharmaceuticals, Aurora, Ohio, USA). After being washed with the same buffer, peroxidase was detected with an enhanced chemiluminescence system (Pierce). The membranes were exposed to X-ray film (Fuji Photo Film, Tokyo, Japan) for 10 min. Quantitation of the results was performed by scanning the X-ray film with Photoshop software (version 5.5, Adobe Systems, San Jose, Calif., USA) followed by densitometry with the public domain software, NIH Image, version 1.62.
Statistical analysis
Data are expressed as mean±SD. All statistical comparisons were analyzed using SPSS software (version 10.0, SPSS, Chicago, Ill., USA). Analysis of variance (ANOVA) was performed when more than two groups were compared, and when significant (P<0.05), Sheffé’s multiple comparison test was applied to test for differences between individual groups. The Mann Whitney’s U-test was used for statistical analyses of inter-group comparison. A P-value less than 0.05 was considered to be significant.
Results
Effect of TGZ on cell numbers of colon cancer cell lines
In the absence of TGZ, both HCT-15 and DLD-1 cells proliferated rapidly, reaching a plateau on day 5, whereas LoVo cells continued to grow up to day 8 with a slower rate. Addition of TGZ in culture medium inhibited the increases of these cells in a dose-dependent manner (Fig. 1). Alamar blue fluorescence values of respective cell lines cultured for 5 days with 0 μM, 10, 20 μM, and 50 μM TGZ were as follows: 2,580±260 (mean±SD), 2,110±150, 1,510±270, and 820±60 in HCT-15; 2,840±520, 2,550±400, 2,170±350, and 1,360±230 in DLD-1; 640±100, 540±100, 400±70, and 210±40 in LoVo. The values treated with 50 μM TGZ for 5 days were decreased to one-third to a half of the values of the respective cell line without treatment. The growth of HCT-15 and LoVo cells was significantly inhibited by treatment with 10 μM, 20 μM, and 50 μM TGZ, compared with DMSO alone (P<0.01). TGZ treatment for 8 days completely repressed the increase of LoVo cells at a 50-μM concentration. Treatment with 20 μM and 50 μM TGZ inhibited the proliferation of DLD-1 cells (P<0.01).
Effects of troglitazone (TGZ) on cell numbers for human colon cancer cell lines, A HCT-15, B DLD-1, and C LoVo. The same cell numbers of each cell line were cultured in the presence of 0 (■), 10 (●), 20 (▲), and 50 (□) μM TGZ. At the indicated time points, cell numbers were estimated by arbitrary units of fluorescence intensity using Alamar blue assay. Each point and bar represent the mean and SD, respectively, from triplicate assays
Effects of TGZ on apoptosis induction in colon cancer cell lines
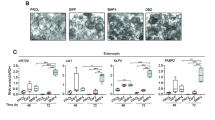
TUNEL-positive cells were increased after TGZ treatment (Fig. 2), although a small amount of positive cells were observed in cells without TGZ treatment. Most of the nuclei were not stained in the negative control, but small numbers of nuclei were stained. The numbers of TUNEL-positive cells in individual cell lines are presented in Table 1. Treatment with TGZ resulted in 2.8-, 2.3-, and 2.4-fold increases of apoptotic cells in HCT-15, DLD-1, and LoVo cells, respectively, as compared with the respective values without TGZ treatment. The values of positive cells were higher in HCT-15 and LoVo cells after treatment than that for DLD-1 cells.
Effect of troglitazone (TGZ) on apoptosis induction in A HCT-15, B DLD-1, and C LoVo. After treatment with (+, in each panel) or without (−) 50 μM TGZ for 5−7 days, cells were stained for apoptotic cells and photographed under a light microscopy. Cells containing black nuclei are positive for TUNEL assay. Bar =20 μm
Effects of TGZ on PPARγ mRNA and protein levels in colon cancer cell lines
Before TGZ treatment, PPARγ mRNA was detected in all cell lines by RT-PCR (Fig. 3A), and PPARγ protein, a band with a subunit molecular mass of approximately 40 kD, was also observed by Western blot (Fig. 3B). PPARγ protein levels were almost proportional with its mRNA levels in the individual cell lines. The protein level in HCT-15 cells was less than those in DLD-1 and LoVo cells.
We also examined whether TGZ treatment could induce alterations in PPARγ mRNA and protein levels in the cell lines. The quantitative RT-PCR analysis demonstrated that PPARγ mRNA levels were increased by 50-μM TGZ treatment 2.2-fold and 1.7-fold in HCT-15 and LoVo cells, respectively, compared with untreated cells (Fig. 4A). Western blot revealed that 50 μM TGZ increased 1.6-fold and 3.4-fold PPARγ protein levels in HCT-15 and LoVo cells, respectively, compared with untreated cells, but it did not alter the mRNA and protein levels in DLD-1 cells (Fig. 4A, B). The extent of increased protein level was proportional to that of mRNA level in HCT-15 cells whereas a higher increase in protein level was observed in LoVo cells.
Effects of troglitazone (TGZ) on peroxisome proliferator-activated receptor (PPAR) γ mRNA and protein levels in three cell lines. A After treatment with 50 μM TGZ for 5−7 days, PPARγ mRNA levels were quantified by a real-time RT-PCR method. After normalization to glyceraldehyde 3-phosphate dehydrogenase, the results (closed bar) are expressed as the fold increase of expression with relation to vehicle-treated control (open bar), and shown as the mean from 4–6 independent determinations. B PPARγ protein levels after treatment with (+, 50 μM) or without (−) TGZ for 5−7 days were measured by Western blot. β-actin was used as control for the amount of loading protein. Signal densities were measured by NIH image, and after normalization to β-actin, the results are shown at the bottom as the fold increase of expression with respect to vehicle-treated control
Effects of TGZ on villin and MUC2 mRNA levels in colon cancer cell lines
The results demonstrated that TGZ induced a 2.0-fold increase in villin mRNA in HCT-15 cells, whereas there was a 90% decrease in LoVo cells (Fig. 5A), as compared with the respective cell lines without TGZ treatment. Addition of the drug induced 2.8-fold and 3.8-fold increases of MUC2 mRNA levels in HCT-15 and LoVo cells, respectively (Fig. 5B). DLD-1 cells did not exhibit alterations in villin or MUC2 mRNA levels after TGZ treatment.
Effects of troglitazone (TGZ) on expression of differentiation markers in three cell lines. After treatment with 50 μM TGZ for 5−7 days, A villin and B MUC2 mRNA levels were quantified by a real-time RT-PCR method. After normalization to glyceraldehyde 3-phosphate dehydrogenase, the results (closed bar) are expressed as the fold increase of expression with relation to vehicle-treated control (open bar), and shown as the mean from 4−6 independent determinations
Discussion
In the present study, TGZ inhibited the cell proliferation and also induced apoptosis of human colon cancer cell lines, HCT-15, DLD-1, and LoVo in a dose-dependent manner (Fig. 1, Fig. 2). Recent reports indicated that TGZ inhibited cell proliferation in several carcinoma cell lines and their inhibition was mainly due to apoptosis (Elstner et al. 1998; Kubota et al. 1998; Takahashi et al. 1999). Although treatment of LoVo cells with 50 μM TGZ for 5 days resulted in almost complete inhibition of cell proliferation and a 2.5-fold increase in apoptotic cell death, TUNEL assay demonstrated that many cells survived (Fig. 2). The present study revealed that apoptosis is not a sole reason for inhibition of cell proliferation due to TGZ in some cell lines. In response to treatment with a ligand for PPARγ, prostate cancer cells are reported to exhibit autophagic cell death (Butler et al. 2000). This type of cell death is characterized by the formation of autophagic vacuoles and does not show the features of apoptosis such as DNA fragmentation (Bursch et al. 1996). When autophagic activity is inhibited, apoptotic cell death induced by an anti-inflammatory drug is increased in colon cancer cells (Bauvy et al. 2001). Although apoptosis induction was demonstrated in this study, occurrence of autophagic cell death in the cells treated with TGZ remained to be clarified.
Expression of PPARγ mRNA and protein was demonstrated in the three cell lines before TGZ treatment, consistent with previous reports that PPARγ was expressed at high levels in colon epithelium and cancer cells (Sarraf et al. 1998; Kitamura et al. 1999). TGZ treatment resulted in increases of PPARγ mRNA and protein levels in HCT-15 and LoVo cells, whereas the increase in DLD-1 cells was minimal, possibly because of a high basal level (Fig. 3).
To clarify the effects of TGZ upon differentiation of colon cancer cell lines, we examined the expression of villin and MUC2 mRNAs. Villin is a major cytoskeletal protein of the brush border in epithelial cells of the digestive and urogenital tracts (Bretscher and Weber 1979; Robine et al. 1993), and hence considered as a marker for enterocyte differentiation along the crypt-villous axis. MUC2 is a major mucin peptide expressed in goblet cells in the intestine (Chang et al. 1994; Tytgat et al. 1994; Sylvester et al. 2001). In this study, the villin mRNA level was increased in HCT-15 cells while markedly repressed in LoVo cells, and MUC2 was induced in HCT-15 and LoVo cells after TGZ treatment but not in DLD-1 cells. These results suggested that HCT-15 cells may be differentiated to enterocytes along the villous axis and LoVo cells are also differentiated but may be withdrawn from the villous axis. DLD-1 cells did not exhibit alterations in villin mRNA or PPARγ mRNA levels. On the other hand, the two cell lines that showed differentiation after TGZ treatment exhibited increased PPARγ mRNA and protein levels. Thus, differentiation induction may be dependent on the enhanced PPARγ level due to TGZ treatment. In this context, inhibition of cell proliferation and apoptosis induction occurred in the three cell lines, irrespective of the presence or absence of PPARγ induction by the drug. Both DLD-1 cells expressing a high amount of PPARγ and HCT-15 cells with a low expression grew at a similar rate. Thus, PPARγ levels in these cell line before TGZ treatment were not correlated with the rates of cell proliferation. These results suggest that the rate of cell proliferation might be independent of PPARγ level. Differentiation induction by TGZ was only observed in the cell lines with enhanced PPARγ expression.
References
Ahmed SA, Gogal RM Jr, Walsh JE (1994) A new rapid and simple non-radioactive assay to monitor and determine the proliferation of lymphocytes: an alternative to [3H]thymidine incorporation assay. J Immunol Methods 170:211−224
Bauvy C, Gane P, Arico S, Codogno P, Ogier-Denis E (2001) Autophagy delays sulindac sulfide-induced apoptosis in the human intestinal colon cancer cell line HT-29. Exp Cell Res 268:139−149
Bishop-Bailey D, Hla T (1999) Endothelial cell apoptosis induced by the peroxisome proliferator-activated receptor (PPAR) ligand 15-deoxy-Δ12, 14-prostaglandin J2. J Biol Chem 274:17042−17048
Braissant O, Foufelle F, Scotto C, Dauca M, Wahli W (1996) Differential expression of peroxisome proliferator-activated receptors (PPARs): tissue distribution of PPAR-α, -β, and -γ in the adult rat. Endocrinology 137:354−366
Bretscher A, Weber K (1979) Villin: the major microfilament-associated protein of the intestinal microvillus. Proc Natl Acad Sci USA 76:2321−2325
Brockman JA, Gupta RA, DuBois RN (1998) Activation of PPARγ leads to inhibition of anchorage-independent growth of human colorectal cancer cells. Gastroenterology 115:1049−1055
Bursch W, Ellinger A, Kienzl H, Torok L, Pandey S, Sikorska M, Walker R, Hermann RS (1996) Active cell death induced by the anti-estrogens tamoxifen and ICI 164384 in human mammary carcinoma cells (MCF-7) in culture: the role of autophagy. Carcinogenesis 17:1595−1607
Butler R, Mitchell SH, Tindall DJ, Young CYF (2000) Nonapoptotic cell death associated with S-phase arrest of prostate cancer cells via the peroxisome proliferator-activated receptor γ ligand, 15-deoxy-Δ12,14-prostaglandin J2. Cell Growth Differ 11:49−61
Chang SK, Dohrman AF, Basbaum CB, Ho SB, Tsuda T, Toribara NW, Gum JR, Kim YS (1994) Localization of mucin (MUC2 and MUC3) messenger RNA and peptide expression in human normal intestine and colon cancer. Gastroenterology 107:28−36
Chawla A, Schwarz EJ, Dimaculangan DD, Lazar MA (1994) Peroxisome proliferator-activated receptor (PPAR) γ: adipose-predominant expression and induction early in adipocyte differentiation. Endocrinology 135:798−800
Chen GG, Lee JFY, Wang SH, Chan UPF, Ip PC, Lau WY (2002) Apoptosis induced by activation of peroxisome proliferator-activated receptor-gamma is associated with Bcl-2 and NF-kB in human colon cancer. Life Sci 70:2631−2646
Elstner E, Müller C, Koshizuka K, Williamson EA, Park D, Asou H, Shintaku P, Said JW, Heber D, Koeffler HP (1998) Ligands for peroxisome proliferator-activated receptor γ and retinoic acid receptor inhibit growth and induce apoptosis of human breast cancer cells in vitro and in BNX mice. Proc Natl Acad Sci USA 95:8806−8811
Fajas L, Auboeuf D, Raspé E, Schoonjans K, Lefebvre AM, Saladin R, Najib J, Laville M, Fruchart JC, Deeb S, Vidal-Puig A, Flier J, Briggs MR, Staels B, Vidal H, Auwerx J (1997) The organization, promoter analysis, and expression of the human PPARγ gene. J Biol Chem 272:18779−18789
Forman BM, Tontonoz P, Chen J, Brun RP, Spiegelman BM, Evans RM (1995) 15-Deoxy-Δ12, 14-prostaglandin J2 is a ligand for the adipocyte determination factor PPARγ. Cell 83:803−812
Greene ME, Blumberg B, McBride OW, Yi HF, Kronquist K, Kwan K, Hsieh L, Greene G, Nimer SD (1995) Isolation of the human peroxisome proliferator activated receptor γ cDNA: expression in hematopoietic cells and chromosomal mapping. Gene Expr 4:281−299
Guan Y, Zhang Y, Davis L, Breyer MD (1997) Expression of peroxisome proliferator-activated receptors in urinary tract of rabbits and humans. Am J Physiol 273:F1013−F1022
Johnson MD, Campbell LK, Campbell RK (1998) Troglitazone: review and assessment of its role in the treatment of patients with impaired glucose tolerance and diabetes mellitus. Ann Pharmacother 32:337−348
Kamei Y, Xu L, Heinzel T, Torchia J, Kurokawa R, Gloss B, Lin SC, Heyman RA, Rose DW, Glass CK, Rosenfeld MG (1996) A CBP integrator complex mediates transcriptional activation and AP-1 inhibition by nuclear receptors. Cell 85:403−414
Keelan JA, Sato TA, Marvin KW, Lander J, Gilmour RS, Mitchell MD (1999) 15-Deoxy-Δ12,14-prostaglandin J2, a ligand for peroxisome proliferator-activated receptor-γ, induces apoptosis in JEG3 choriocarcinoma cells. Biochem Biophys Res Commun 262:579−585
Kersten S, Desvergne B, Wahli W (2000) Roles of PPARs in health and disease. Nature 405:421−424
Kitamura S, Miyazaki Y, Shinomura Y, Kondo S, Kanayama S, Matsuzawa Y (1999) Peroxisome proliferator-activated receptor γ induces growth arrest and differentiation markers of human colon cancer cells. Jpn J Cancer Res 90:75−80
Kubota T, Koshizuka K, Williamson EA, Asou H, Said JW, Holden S, Miyoshi I, Koeffler HP (1998) Ligand for peroxisome proliferator-activated receptor γ (troglitazone) has potent antitumor effect against human prostate cancer both in vitro and in vivo. Cancer Res 58:3344−3452
Lefebvre AM, Chen I, Desreumaux P, Najib J, Fruchart J-C, Geboes K, Brigges M, Heyman R, Auwerx J (1998) Activation of the peroxisome proliferator-activated receptor γ promotes the development of colon tumors in C57BL/6J-APCMin/+mice. Nat Med 4:1053−1057
Lefebvre AM, Paulweber B, Fajas L, Woods J, McCary C, Colombel JF, Najib J, Fruchart J-C, Datz C, Vidal H, Desreumaux P, Auwerx J (1999) Peroxisome proliferator-activated receptor gamma is induced during differentiation of colon epithelium cells. J Endocrinol 162:331−340
Lehmann JM, Moore LB, Smith-Oliver TA, Wilkison WO, Willson TM, Kliewer SA (1995) An antidiabetic thiazolidinedione is a high affinity ligand for peroxisome proliferator-activated receptor γ (PPARγ). J Biol Chem 270:12953−12956
Mansén A, Guardiola-Diaz H, Rafter J, Branting C, Gustafsson JÅ (1996) Expression of the peroxisome proliferator-activated receptor (PPAR) in the mouse colonic mucosa. Biochem Biophys Res Commun 222:844−851
Miyashita T, Nagao K, Krajewski S, Salvesen GS, Reed JC, Inoue T, Yamada M (1998) Investigation of glucocorticoid-induced apoptotic pathway: processing of caspase-6 but not caspase-3. Cell Death Differ 5:1034−1041
Mueller E, Sarraf P, Tontonoz P, Evans RM, Martin KJ, Zhang M, Fletcher C, Singer S, Spiegelman BM (1998) Terminal differentiation of human breast cancer through PPARγ. Mol Cell 1:465−470
Ohta K, Endo T, Haraguchi K, Hershman JM, Onaya T (2001) Ligands for peroxisome proliferator-activated receptor γ inhibit growth and induce apoptosis of human papillary thyroid carcinoma cells. J Clin Endocrinol Metab 86:2170−2177
Okura T, Nakamura M, Takata Y, Watanabe S, Kitami Y, Hiwada K (2000) Troglitazone induces apoptosis via the p53 and Gadd45 pathway in vascular smooth muscle cells. Eur J Pharmacol 407:227−235
Robine S, Sahuquillo-Merino C, Louvard D, Pringault E (1993) Regulatory sequences on the human villin gene trigger the expression of a reporter gene in a differentiating HT29 intestinal cell line. J Biol Chem 268:11426−11434
Rosen ED, Sarraf P, Troy AE, Bradwin G, Moore K, Milstone DS, Spiegelman BM, Mortensen RM (1999) PPARγ is required for the differentiation of adipose tissue in vivo and in vitro. Mol Cell 4:611−617
Saez E, Tontonoz P, Nelson MC, Alvarez JGA, Tze MU, Baird SM, Thomazy VA, Evans RM (1998) Activators of the nuclear receptor PPARγ enhance colon polyp formation. Nat Med 4:1058−1061
Sarraf P, Mueller E, Jones D, King FJ, DeAngelo DJ, Partridge JB, Holden SA, Chen LB, Singer S, Fletcher C, Spiegelman BM (1998) Differentiation and reversal of malignant changes in colon cancer through PPARγ. Nat Med 4:1046−1052
Sheppard KA, Phelps KM, Williams AJ, Thanos D, Glass CK, Rosenfeld MG, Gerritsen ME, Collins T (1998) Nuclear integration of glucocorticoid receptor and nuclear factor-κB signaling by CREB-binding protein and steroid receptor coactivator-1. J Biol Chem 273:29291−29294
Shimada T, Kojima K, Yoshiura K, Hiraishi H, Terano A (2002) Characteristic of the peroxisome proliferator activated receptor γ (PPARγ) ligand induced apoptosis in colon cancer cells. Gut 50:658−664
Sylvester PA, Myerscough N, Warren BF, Carlstedt I, Corfield AP, Durdey P, Thomas MG (2001) Differential expression of the chromosome 11 mucin genes in colorectal cancer. J Pathol 195:327−335
Takahashi N, Okumura T, Motomura W, Fujimoto Y, Kawabata I, Kohgo Y (1999) Activation of PPARγ inhibits cell growth and induces apoptosis in human gastric cancer cells. FEBS Lett 455:135−139
Tontonoz P, Hu E, Spiegelman BM (1994) Stimulation of adipogenesis in fibroblasts by PPARγ2, a lipid-activated transcription factor. Cell 79:1147−1156
Tontonoz P, Singer S, Forman BM, Sarraf P, Fletcher JA, Fletcher CDM, Brun RM, Mueller E, Altiok S, Oppenheim H, Evans RH, Spiegelman BM (1997) Terminal differentiation of human liposarcoma cells induced by ligands for peroxisome proliferator γ and the retinoid X receptor. Proc Natl Acad Sci USA 94:237−241
Tytgat KMAJ, Büller HA, Opdam FJM, Kim YS, Einerhand AWC, Dekker J (1994) Biosynthesis of human colonic mucin: Muc2 is the prominent secretory mucin. Gastroenterology 107:1352−1363
Willson TM, Lehmann JM, Kliewer SA (1996) Discovery of ligands for the nuclear peroxisome proliferator-activated receptors. Ann NY Acad Sci 804:276−283
Willson TM, Brown PJ, Stermbach DD, Henke BR (2000) The PPARs: from orphan receptors to drug discovery. J Med Chem 43:527−550
Yang WL, Frucht H (2001) Activation of the PPAR pathway induces apoptosis and COX-2 inhibition in HT-29 human colon cancer cells. Carcinogenesis 22:1379−1383
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kato, M., Kusumi, T., Tsuchida, S. et al. Induction of differentiation and peroxisome proliferator-activated receptor γ expression in colon cancer cell lines by troglitazone. J Cancer Res Clin Oncol 130, 73–79 (2004). https://doi.org/10.1007/s00432-003-0510-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-003-0510-2