Abstract
Currently hundreds of thousands of minor refugees entered Europe. This group has been exposed to traumatic events pre-, during, and post-migration and is at increased risk of developing psychiatric disorders. In this article, we describe the results of our literature search on screening and interventions for post-traumatic stress disorder (PTSD) in minor refugees, in order to make recommendations for clinical practice. Results show that studies on diagnostic accuracy of assessment instruments and efficacy of mental healthcare interventions in this population are lacking. Traumatic experiences pre-flight, during the flight and at resettlement, superimposed by parental PTSD, and other contextual factors, might lead to more than 25% of minor refugees developing PTSD.
Conclusion: To enhance the number of minor refugees recognized with PTSD, we recommend the use of a brief screening instrument. A public health approach, focusing on environmental supportive factors is the first step in treatment for this group, followed by short-term psychological group interventions focusing on psycho-education and stress reduction. Minor refugees with no improvement in PTSD symptoms by these interventions need referral to specialized mental health care services. Mental health providers should be culturally competent.
What is Known: |
• Post-traumatic stress disorder, anxiety, sleeping problems, and depression are the most common psychiatric disorders in minor refugees. |
• Evidence based methods on screening and interventions in minor refugees with psychiatric disorders are lacking. |
What is New: |
• In the absence of validated screening tools a best practice reliable, quick and child-friendly tool is presented. |
• A layered system for mental health care and psychosocial support in minor refugees is explained. |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
During the current refugee crisis, hundreds of thousands of minor refugees are entering Europe [19]. In 2015, more than 1.25 million refugees requested asylum in Europe, the majority was of Syrian nationality [46]. Nearly one third (29%) of these refugees were minors [3]. Almost a quarter (23%) of the group of minor refugees was traveling without their parents (unaccompanied minors) [3]. In the literature different terminology for minor refugees is used. An asylum seeker is a person who applies for the right to reside in a foreign country and to be protected as a refugee by that country, but who has not yet been approved as a refugee. When we speak of minor refugees in this article, we include forcibly displaced children, minor asylum seekers, and unaccompanied minor refugees.
Refugees are defined as having a “well-founded fear of being persecuted for reasons of race, religion, nationality, membership of a particular social group or political opinion in the country of their nationality” [42] and migrate for political reasons, whereas economic migrants may migrate for economic or educational reasons. Migration gives a higher risk of mental and physical health problems. Within the groups of migrants, refugees, especially women, elderly, and (unaccompanied) minors, are the most vulnerable to mental and physical health problems; common mental disorders are twice as high as in economic migrants [4]. In minor refugees, exposure to different kinds of traumatic events like war, torture, abuse, trafficking, the flight itself, and abduction of their parents, are associated with a variety of psychological problems. Besides the traumatic exposure, post-migration factors play an important role in the development of psychological symptoms [15]. Emotional and behavioral symptoms are common and mostly presented as a mixture of symptoms, not fitting in a single diagnostic category. Although there are no consistent prevalence rates of psychiatric symptoms in minor refugees, post-traumatic stress disorder (PTSD), anxiety, sleeping problems and depression are the most common and believed to be higher than in the general minor population [8, 14]. In this article, we will put the focus on screening and interventions on PTSD. Alisic et al. found in their meta-analysis that the PTSD rate in minors after an interpersonal traumatic experience was 25.2% [1]. Traumatic experiences pre-flight, during flight and at resettlement, sometimes superimposed by parental PTSD and complicating contextual factors (lack of family and social support and multiple relocations) might lead to a prevalence rate of more than 25% of minor refugees developing PTSD. This emphasizes the need for early screening and a timely intervention to prevent a cascade of developmental disruptions [1].
Only a small percentage of refugees with psychological problems seeks for help [28]. It is assumed that there is an underrepresentation of minor refugees with PTSD in mental health care practices, implying that a large amount of them is not being diagnosed or diagnosed after a delay and will not get a timely, efficient treatment. In this article, we describe the results of our literature search on screening and interventions for PTSD in minor refugees, in order to make recommendations for improvements in clinical practice.
Mental health problems in minor refugees
Childhood trauma exposure has an impact on children’s development across a broad spectrum of functions and can lead to a variety of symptoms, for instance disturbed attachment patterns, shifts in emotional states, regulation problems, regressive behaviors, aggression, sleeping and eating problems, somatic symptoms, anticipatory anxiety, and lack of self-esteem [38]. Being exposed to violence is found to be the key risk factor for developing mental health problems in children [15]. Minor refugees, unaccompanied even more, are regularly exposed to violence and more often to several traumatic events, which puts them at high risk for developing mental health problems [9, 15]. Another risk factor is a pre-existing vulnerability for mental health problems. Compared to these pre-flight experiences, traumatic experiences during flight and resettlement have an even higher impact on developing mental health problems. [15]. These mental health problems occur based on complex interactions between the individual and the multiple systems which the individual is a part of. Factors that facilitate resilience in refugee minors such as high parental support and good parental mental health (particularly in mothers), peer support, adaptability, and self-esteem have a protective function in developing mental health problems [10, 15, 27, 39]. Parental exposure to traumatic events, for instance, shows a higher association with children’s mental health problems than the children’s own trauma exposure [15]. The parent-child interaction is affected in many traumatized parents in a way that makes the parents respond less sensitive, more hostile, and more aggressive towards their children. As a result, children of parents with PTSD show more behavioral problems, both internalizing and externalizing, than children of parents without PTSD [13, 15, 40]. Montgomery found that the PTSD criteria are insufficient when studying minor refugees’ psychological problems [27]. New conceptualizations have been suggested to define the complex psychopathological reactions that can arise after early initiated, long-lasting traumatic life experiences [27, 38], which lead to specifications in the criteria for PTSD for children above the age of six and separate specific criteria for children under the age of six in the recently published DSM-5 [2].
Assessment
Research shows that there is a gap between the need and the use of mental health services in the group of minor refugees [8]. They encounter various barriers affecting the accessibility, suitability, and acceptability of mental health services, including language barriers, stigma associated with mental health problems, low priority given to mental health compared to physical health, and lack of knowledge of the healthcare system in their host country, which emphasizes the need for appropriate assessment of mental health problems in this group [5, 8, 24]. Guidelines and research on early interventions after trauma advise a holistic comprehensive service to be able to recognize and treat mental health problems in the natural environment of the child, for instance the school, to lower these barriers [5, 6, 21, 22].
The NICE guideline on PTSD recommends to consider routinely use of a brief screening instrument on PTSD as part of the initial refugee healthcare assessment [30]. A systematic review by Gadeberg et al. shows a lack of validated screening tools on mental health and PTSD in minor refugees, especially below the age of six [17]. They state that because of the great variation in the use of informants and settings, a recommendation of a specific screening instrument is not possible [17]. Table 1 shows the available validated screening tools in minor refugees, based on the results of the systematic review of Gadeberg et al. [17]. At the moment, a “best practice” use of an (in)validated screening tool is advised [16]. The IES (impact of event scale) is one of the validated screening tools in minor refugees in Cambodia and in Croatia, Bosnia, and Herzegovina following two included articles in the review of Gadeberg et al. [12, 36]. Smith et al. show its validation in children in war in Bosnia and confirm the cross-cultural validity [41]. The CRIES (the Children’s Revised Impact of Event Scale), a children’s version of the Impact of Event Scale, was validated in the Dutch population by Verlinden et al. Because of the lack of a gold standard, we recommend the use of the CRIES as a best practice, because of its reliable, quick, and child-friendly way to screen for PTSD in minor refugees, which does not require additional training of professionals [45]. It can be used in children aged 8 years and above and is available in different languages [7]. The most appropriate timing for screening is still under debate. Stress reactions in the first 4 to 6 weeks after the traumatic event are considered a “normal reaction to abnormal events.” Screening in this period can bring the risk of “medicalizing” children with acute symptoms as part of the natural process. There is insufficient evidence for tracing latent symptoms in the first few weeks and minors with a delayed start of PTSD can be missed [30]. However, early screening and intervention can prevent problems from becoming chronic [29]. On top of that, in this population mostly multiple traumatic events occurred and the timeline of events and arrival can be undefinable. The abovementioned factors make a timely screening recommended in clinical practice. Moreover, since minor refugees growing up in families depend on parental support, mental health assessment of parents is also essential.
Interventions
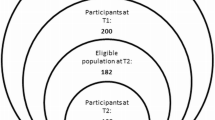
Various factors on different levels in the bio-ecological system, e.g., individual, family, community, and society factors, contribute to children’s development and their quality of life. In accordance with this, the Inter-agency Standing Committee (IASC) advises to develop a layered system for mental health care and psychosocial support in minor refugees, visually represented as a pyramid (see Fig. 1) [22]. The first layer consists of basic services and security. In the second layer, a smaller group is represented who needs help in accessing community and family supports. This is followed by a third layer of minors who require more focused non-specialized interventions. The top of the pyramid consists of individuals with the greatest need, who must have access to specialized mental health care services. Early psychosocial interventions, based on needs that are represented in the first and second layer of the pyramid, are applied to promote natural recovery and to prevent refugees from developing psychopathology [5, 15]. This means that successful interventions in minor refugees require not only psychotherapeutic treatment focusing on PTSD symptoms, instead they should consist of individual as well as supportive factors like (reuniting) family, having the possibility to go to school, integration of traditional health care, language training, and help with employment and housing for the parents, to improve outcome [15, 21, 24]. There is a definite correlation between indicators of mental health and social conditions in the host country; stable settlement and social support in the host country are the main protective factors for mental health outcomes in minor refugees [15]. Psychological functioning is improved by peer support; feeling safe at school, no discrimination, and low peer violence give a higher self-esteem. Programs focusing on improving basic needs and social support are an important part of mental health care for refugees to prevent them from developing psychiatric symptoms These preventive programs carry the advantage of reaching a wide range of minor refugees and the possibility of being carried out by paraprofessionals. Preventive interventions focusing on improving social conditions, like holistic interventions and family approaches, are described in the literature but research on effectiveness is limited [22, 24, 40]; however, there is general agreement on its necessity. Psycho-education is one of the main interventions in the third layer of the pyramid of “non-specialized interventions” and should consist of explanations on normal reactions to traumatic events, when to look for professional help and the importance on sticking to daily routines, adjusted to the age [21, 47]. Concerning decreased concentration levels of traumatized minors, information should be visual as well as verbal and short, structured, and accessible [21, 47].
Intervention pyramid for mental health care and psychosocial support in minor refugees, adapted from IASC guidelines on mental health and psychosocial support in emergency settings [22]
Most of the research on individual psychotherapy for children and adolescents with PTSD involves trauma-focused cognitive behavior therapy (TF-CBT). TF-CBT is an established treatment in children and adolescents with PTSD. Eye movement desensitization and reprocessing (EMDR) is not yet evidence-based but mentioned in guidelines as promising [11, 30, 44]. For minor refugees, only case reports or pilot studies are published about the effectiveness of TF-CBT, EMDR, and other psychotherapies like narrative exposure therapy for children (KIDNET) [31, 32, 34, 43], so the quality of the evidence base on psychotherapeutic interventions for this group is still low [33]. Questionable is if the literature found on trauma treatment in non-refugee minors is generalizable to this specific population. From pilot studies and case reports, there is a tendency that minor refugees can benefit from our known psychotherapeutic therapies. For psychotherapists, it is vital to only start individual trauma therapy in minor refugees when it can be completed, which might be a challenge because of the insecure status of the length of their stay at a specific location. In this situation, clinical practice can come in conflict with theoretical practice, for instance Morina and colleagues state that early interventions on PTSD in adults are highly recommended and significantly more effective than waiting lists [29]. The evidence for drug treatment for PTSD in children is very limited and no literature is available on this subject in minor refugees [30].
From literature no definite conclusion, it can be drawn on the optimal timing to start individual trauma treatments. Referrals to specialized mental health care services must be considered at any stage, when symptoms are apparent or do not respond to the public health interventions. Children’s mental health care centers need to have sufficient capacity to offer specialized mental health care to minor refugees and their families in which knowledge on transcultural psychiatry, trauma, and family treatment is essential. Besides that, specialists in children’s mental health care have an important role in consultation for local authorities, policy makers, teachers, social workers, youth care workers, and general health care workers, working with minor refugees [37].
We recommend short-term group interventions for minor refugees suffering from PTSD. Group interventions have the advantage of being supportive in a way that problems are identifiable, recognizable, and minors can be an example for each other. Besides that, they are less time-consuming and more cost-effective compared to individual treatments. The group interventions can be based on the first phases of TF-CBT, which include psycho-education, relaxation, affect regulation, and cognitive coping. Parents can be (partially) involved in these group sessions and can have parallel sessions with the other parents. Clustering groups by specific ages or ethnicity may be preferable. Culturally sensitive social workers can be trained by mental health professionals to lead these intervention groups. A short-term intervention is needed to prevent minor refugees from not being able to complete the treatment. An incomplete treatment might make people not to search for treatment later during the course of their symptoms.
Policies of deterrence
A threat to the humanitarian needs of minor refugees and thereby their mental health are governmental and society concerns about uncontrolled migration. Host countries adopt policies of deterrence with increasingly restrictive measures, resulting in restricted access to education, housing, welfare, more stringent refugee determinations procedures, temporary forms of asylum, and so on [37]. The asylum procedure with many relocations and restrictive policies opposes to the basics of preventive programs, adding to the effect of post-migration stress, leading to disadvantages and negative influence on mental health and ongoing PTSD [18, 23, 26, 37]. Mental health providers have a role in educating society and governments on the risks of these policies of deterrence [37].
Transcultural issues
There are arguments against a universality of mental illness, which raises the question if a Western treatment model can be applied to cultures where their relevance has not been validated yet [8]. A common understanding of the concept of child development and mental health is needed in ensuring engagement in diagnosis and treatment. Diagnostic systems based on Western culture might generate misdiagnoses in minor refugees resettling in the host countries [20, 24, 25]. Mental health providers should be culturally sensitive of the diversity in different ethnical populations and culturally competent to be able to provide effective services in the group of minor refugees [8, 30]. Lack of trust, inadequate communication, including language barriers, and cultural differences between the mental health care worker and the minor refugees are challenges to obtain an appropriate history [35]. To be able to understand the full trauma story, including the personal and cultural relevance, it is needed to seek information about conditions in the minor refugee’s country of origin, to listen attentive, and have empathy and respect [35]. Culturally sensitive mental health providers should know that communication styles, for instance eye contact or shaking hands with opposite sex, may differ between different ethnic groups and the host country [35]. Expectations of psychiatric treatment may differ between the minor refugees (and their parents) and the mental health care workers [15, 40]. Research on the views and perceptions of unaccompanied minors in the UK, for example, showed that there was a mistrust in mental health services, especially in doctors. The intentions, motives, and future actions of mental health care workers were uncertain, as, in the minor’s opinion, they were part of the state [25]. Minor refugees may fear arrest and deportation if they are in the asylum process [35]. Talking therapy remains one of the most common treatments for trauma in the Western European countries, while pharmacological treatment is in general more accepted in this population [20, 25] (although there is no evidence PTSD in minor refugees). In talking, a therapy the language barrier can make subtle nuances in communication get lost. Besides that, non-talking, silencing, and containment are normal responses to traumatic experiences in some other parts of the world [20]. To optimize the quality of the communication and minimize the risk of misunderstanding, professional interpreters should be involved in cases with a language barrier. The gender and ethnicity of the interpreter may be important [35]. Mediation, by people in whom this group of minor refugees have, trust might be helpful to access and engage in mental health services [5, 25].
Conclusion
Development of mental health problems and in particular PTSD in minor refugees is a major problem. We estimate that more than 25% of the minor refugees develop PTSD. The asylum procedure, resettlement, and transcultural issues cause that only a small proportion of this group is being recognized with PTSD and receiving treatment.
To enhance the number of minor refugees recognized with PTSD, we recommend the use of a brief screening instrument for minors on PTSD in the health care assessment at the host country. Furthermore, assessment of the mental health of parents is essential.
Interventions should start with a public health approach, focusing on basic security, environmental and supportive factors. Participation and integration of parents is part of this approach. Short term group interventions based on the first phases of TF-CBT are recommended as a next step before specialized psychotherapeutic interventions. Mental health care professionals need to be culturally sensitive and competent and have a role in emphasizing and advising on the importance of the above mentioned factors to policy makers.
There is a lack of research on screening and interventions in this specific population. From pilot studies and case reports, there is a tendency that minor refugees can benefit from our known psychotherapeutic therapies. Research in this specific population is needed to draw a conclusion on this matter.
Abbreviations
- CRIES:
-
Children’s Revised Impact of Event Scale
- DSM-5:
-
diagnostic and statistical manual of mental disorders-5
- EMDR:
-
eye movement desensitization and reprocessing
- IASC:
-
Inter-agency Standing Committee
- IES:
-
impact of event scale
- KIDNET:
-
narrative exposure therapy for children
- NICE:
-
National Institute for Health and Care Excellence
- PTSD:
-
post-traumatic stress disorder
- TF-CBT:
-
trauma focused-cognitive behavior therapy
References
Alisic E, Zalta AK, Wesel F Van, Larsen SE, Hafstad GS, Hassanpour K et al (2014) Rates of posttraumatic stress disorder in trauma-exposed children and adolescents: meta-analysis. Br J Psychiatry 204; 335–340.
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. Washington, DC. http://dsm.psychiatryonline.org/doi/book/10.1176/appi.books.9780890425596
Asylum statistics (2016) http://ec.europa.eu/eurostat/statistics-explained/index.php/Asylum_statistics
Bhugra D, Gupta S, Bhui K, Craig TOM, Dogra N, Ingleby JD et al (2011) WPA guidance on mental health and mental health care in migrants. World Psychiatry 10(1):2–10. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3048516/
Birman D, Ho J, Pulley E, Batia K, Everson ML, Ellis H et al (2005) Mental Health Interventions for Refugee Children in Resettlement II. Natl Child Trauma Stress Netw. 1–29. http://www.nctsnet.org/nctsn_assets/pdfs/promising_practices/MH_Interventions_for_Refugee_Children.pdf
Brymer M, Steinberg A, Sornborger J, Layne C, Pynoos R (2008) Acute interventions for refugee children and families. Child Adolesc Psychiatr Clin N Am 17(3):625–640
Children’s Revised Impact of Event Scale. http://www.childrenandwar.org/measures
de Anstiss H, Ziaian T, Procter N, Warland J, Baghurst P (2009) Help-seeking for mental health problems in young refugees: a review of the literature with Implications for Policy, Practice, and Research. Transcult Psychiatry 46(4):584–607. http://tps.sagepub.com/content/46/4/584%5Cn http://tps.sagepub.com.ezproxy.welch.jhmi.edu/content/46/4/584%5Cn http://www.ncbi.nlm.nih.gov/pubmed/20028678
Derluyn I, Broekaert E, Schuyten G (2008) Emotional and behavioural problems in migrant adolescents in Belgium. European Child and Adolescence Psychiatry 54–62.
Derluyn I, Broekaert E, Schuyten G, Temmerman DE (2004) Post-traumatic stress in former Ugandan child. Soldiers 363:861–863
Diehle J, Opmeer BC, Boer F, Mannarino AP, Lindauer RJL (2015) Trauma-focused cognitive behavioral therapy or eye movement desensitization and reprocessing: what works in children with posttraumatic stress symptoms? A randomized controlled trial. Eur Child Adolesc Psychiatry 24(2):227–236
Dyregrov A, Kuterovac G, Baráth Á (1996) Factor analysis of the Impact of Event Scale with children in war. Scand J Psychol 37:339–350
Ee van E, Hein I, Bala J, Mooren T (2014) Multi Family Therapy met vluchtelingengezinnen: van oorlog naar veiligheid. Kind Adolesc 35(3):205–2015
Fazel M, Stein A (2002) The mental health of refugee children. Arch Dis Child 87(5):366–370. http://www.ncbi.nlm.nih.gov/pubmed/12390902%5Cn http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=PMC1763071
Fazel M, Reed RV, Panter-Brick C, Stein A (2012) Mental health of displaced and refugee children resettled in high-income countries: risk and protective factors. Lancet 379(9812):266–282. https://doi.org/10.1016/S0140-6736(11)60051-2
Gadeberg AK, Norredam M (2016) Urgent need for validated trauma and mental health screening tools for refugee children and youth. Eur Child Adolesc Psychiatry 25(8):929–931. http://www.ncbi.nlm.nih.gov/pubmed/27043846
Gadeberg AK, Montgomery E, Frederiksen HW, Norredam M. (2016) Assessing trauma and mental health in refugee children and youth: a systematic review of validated screening and measurement tools. European Journal of Public Health 27(3): 439–446
Goosen S, Stronks K, Kunst AE (2014) Frequent relocations between asylum-seeker centres are associated with mental distress in asylum-seeking children: a longitudinal medical record study. Int J Epidemiol 43(1):94–104
Hebebrand J, Anagnostopoulos D, Eliez S, Linse H, Pejovic-Milovancevic M, Klasen H (2016) A first assessment of the needs of young refugees arriving in Europe: what mental health professionals need to know. Eur Child Adolesc Psychiatry 25(1):1–6
Hjern A, Jeppsson O (2005) Sociale steun adequater dan traumagerichte aanpak. Phaxx, kwartaalblad vluchtelingen en gezondheid. http://www.pharos.nl/documents/doc/Phaxx/2005_3_Ggz_kinderen.pdf
Impact (2007) Multidisciplinary Guideline: Early psychosocial interventions after disasters, terrorism and other shocking events. https://www.escap.eu/bestanden/Care(38)/Refugees/multidisciplinary_guideline_english_complete.pdf
Inter-Agency Standing Committee (2007) Iasc Guidelines on Mental Health and Psychosocial Support in Emergency Settings. http://www.who.int/mental_health/emergencies/guidelines_iasc_mental_health_psychosocial_june_2007.pdf
Laban CJ, Komproe IH, Gernaat HBPE, Jong JTVM (2008) The impact of a long asylum procedure on quality of life, disability and physical health in Iraqi asylum seekers in the Netherlands. Soc Psychiatry Psychiatr Epidemiol 43(7):507–515
Lustig SL, Kia-Keating M, Knight WG, Geltman P, Ellis H, Kinzie D et al (2004) Review of child and adolescent refugee mental health. J Am Acad Child Adolesc Psychiatry 43(1):24–36. https://doi.org/10.1097/00004583-200401000-00012
Majumder P, O’Reilly M, Karim K, Vostanis P (2015) “This doctor, I not trust him, I”m not safe’: the perceptions of mental health and services by unaccompanied refugee adolescents. Int J Soc Psychiatry 61(2):129–136. http://www.scopus.com/inward/record.url?eid=2-s2.0-84924759283&partnerID=tZOtx3y1
Malmusi D (2015) Immigrants’ health and health inequality by type of integration policies in European countries. Eur J Pub Health 25(2):293–299
Montgomery E (2011) Trauma, exile and mental health in young refugees. Acta Psychiatr Scand 124(SUPPL. S440):1–46
Soydaş S, Mooren T (2015) Verkenning van noden en mogelijkheden voor hulpverlening aan mensen die asiel aanvragen in Nederland. Nederlands instituut voor psychologen. https://www.kenniscentrum-kjp.nl/app/webroot/files/tmpwebsite/downloadables_publicaties/onderzoek-nip-23-11-final.pdf
Morina N, Wicherts JM, Lobbrecht J, Priebe S (2014) Clinical psychology review remission from post-traumatic stress disorder in adults: a systematic review and meta-analysis of long term outcome studies. Clin Psychol Rev 34(3):249–255. https://doi.org/10.1016/j.cpr.2014.03.002
National Institute for Health and Care Excellence (2005) Post-traumatic stress disorder: management. Clinical guideline
Onyut LP, Neuner F, Schauer E, Ertl V, Odenwald M, Schauer M et al (2005) Narrative Exposure Therapy as a treatment for child war survivors with posttraumatic stress disorder: two case reports and a pilot study in an African refugee settlement. BMC Psychiatry 5:7
Oras R, de Ezpeleta SC, Ahmad A (2004) Treatment of traumatized refugee children with eye movement desensitization and reprocessing in a psychodynamic context. Nord J Psychiatry 58(3):199–203
Pacione L, Measham T, Rousseau C (2013) Refugee children: Mental health and effective interventions. Curr Psychiatry Rep 15:341
Robjant K, Fazel M (2010) The emerging evidence for Narrative Exposure Therapy: a review. Clin Psychol Rev Elsevier Ltd 30(8):1030–1039. https://doi.org/10.1016/j.cpr.2010.07.004
Crosby SS (2013) Primary Care Management of non–english-speaking refugees who have experienced trauma: a clinical review. JAMA 310(5):519–528
Sack W, Seeley J, Him C, Clarke G (1998) Psychometric properties of the Impact of Event Scale in traumatized Cambodian refugee youth. Personal Individ Differ 25:57–67
Silove D, Steel Z, Watters C (2000) Policies of deterrence and the mental health of asylum seekers. JAMA 284(5):604–611
Simonelli A (2013) Posttraumatic stress disorder in early childhood: classification and diagnostic issues. Eur J Psychotraumatol 4(1):21357. http://doi.org/10.3402/ejpt.v4i0.21357
Sleijpen M, ter Heide FJJ, Mooren T, Boeije HR, Kleber RJ (2013) Bouncing forward of young refugees: a perspective on resilience research directions. European Journal of Psychotraumatology 4(1):20124. http://doi.org/10.3402/ejpt.v4i0.20124
Slobodin O, de Jong JT (2015) Family interventions in traumatized immigrants and refugees: a systematic review. Transcult Psychiatry 52(6):723–742
Smith P, Perrin S, Dyregrov A, Yule W (2003) Principal components analysis of the impact of event scale with children in war. Personal Individ Differ 34(2):315–322
United Nations High Commissioner for Refugees. www.unhcr.org
Unterhitzenberger J, Eberle-Sejari R, Rassenhofer M, Sukale T, Rosner R, Goldbeck L (2015) Trauma-focused cognitive behavioral therapy with unaccompanied refugee minors: a case series. BMC Psychiatry 15(1):260. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=4619299&tool=pmcentrez&rendertype=abstract
Verlinden E, Lindauer RJL (2015) Trauma bij kinderen en adolescenten: screening, diagnostiek en behandeling. Tijdschr Psychiatr 57(12):912–916
Verlinden E, Opmeer BC, Van Meijel EPM, Beer R, De Roos C, Bicanic IAE et al (2015) Enhanced screening for posttraumatic stress disorder and comorbid diagnoses in children and adolescents. Eur J Psychotraumatol 26661. http://www.ncbi.nlm.nih.gov/pubmed/26320743%5Cn http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=PMC4553265
Vluchtelingen in getallen (2016) VluchtelingenWerk Nederland, pp 1–50. https://www.vluchtelingenwerk.nl/sites/public/u895/Vluchtelingeningetallen2016_nieuw.pdf
Zurek G, Schedlich C, Bering R (2006) Manual for trauma-based psychoeducation for victims of disasters. European Network for Psychosocial Aftercare in Case of Disaster. Target Group Intervention Programme Manual III
Funding
This study has not been funded.
Author information
Authors and Affiliations
Contributions
Study design: Horlings AH, Hein IM
Literature search: Horlings AH, Hein IM
Drafting the article: Horlings AH
Figures, tables: Horlings AH
Critical revision: Hein IM
Final approval of the version to be published: Horlings AH, Hein IM
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval/informed consent
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Communicated by Nicole Ritz
This article refers to the Editiorial https://doi.org/10.1007/s00431-017-3019-4
Rights and permissions
About this article
Cite this article
Horlings, A., Hein, I. Psychiatric screening and interventions for minor refugees in Europe: an overview of approaches and tools. Eur J Pediatr 177, 163–169 (2018). https://doi.org/10.1007/s00431-017-3027-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-017-3027-4